Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Davi Vieira Teixeira da Silva | -- | 5265 | 2023-06-06 16:02:18 | | | |
| 2 | Rita Xu | Meta information modification | 5265 | 2023-06-07 03:49:01 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Da Silva, D.V.T.; Baião, D.D.S.; Almeida, C.C.; Paschoalin, V.M.F. Endothelial Dysfunction and Arterial Stiffness under Cardiovascular Risk. Encyclopedia. Available online: https://encyclopedia.pub/entry/45249 (accessed on 24 May 2026).
Da Silva DVT, Baião DDS, Almeida CC, Paschoalin VMF. Endothelial Dysfunction and Arterial Stiffness under Cardiovascular Risk. Encyclopedia. Available at: https://encyclopedia.pub/entry/45249. Accessed May 24, 2026.
Da Silva, Davi Vieira Teixeira, Diego Dos Santos Baião, Cristine Couto Almeida, Vania Margaret Flosi Paschoalin. "Endothelial Dysfunction and Arterial Stiffness under Cardiovascular Risk" Encyclopedia, https://encyclopedia.pub/entry/45249 (accessed May 24, 2026).
Da Silva, D.V.T., Baião, D.D.S., Almeida, C.C., & Paschoalin, V.M.F. (2023, June 06). Endothelial Dysfunction and Arterial Stiffness under Cardiovascular Risk. In Encyclopedia. https://encyclopedia.pub/entry/45249
Da Silva, Davi Vieira Teixeira, et al. "Endothelial Dysfunction and Arterial Stiffness under Cardiovascular Risk." Encyclopedia. Web. 06 June, 2023.
Copy Citation
Pathophysiological conditions such as endothelial dysfunction and arterial stiffness, characterized by low nitric oxide bioavailability, deficient endothelium-dependent vasodilation and heart effort, predispose individuals to atherosclerotic lesions and cardiac events. Nitrate (NO3−), L-arginine, L-citrulline and potassium (K+) can mitigate arterial dysfunction and stiffness by intensifying NO bioavailability. Dietary compounds such as L-arginine, L-citrulline, NO3− and K+ exert vasoactive effects as demonstrated in clinical interventions by noninvasive flow-mediated vasodilation (FMD) and pulse-wave velocity (PWV) prognostic techniques.
L-arginine
L-citrulline
Potassium ions
NO bioavailability
dietary interventions
1. Introduction
Blood vessels are constituted of connective tissue, fibroblasts, vascular smooth muscle cells (VSMCs) and endothelial cells (ECs). The endothelium is a semipermeable layer located between the bloodstream and blood vessel wall, comprising a barrier that selectively limits macromolecule movements and guarantees host defense [1]. Endothelial cells, the main endothelium components, play an important role in cardiovascular homeostasis by regulating vascular tone, blood flow, angiogenesis, monocyte/leukocyte adhesion and platelet aggregation [2]. In response to different stimuli, the endothelium maintains the balance between vasoconstriction and vasodilation through the release of both autocrine and paracrine substances, including angiotensin II, endothelin-1, thromboxane A2 and prostacyclin H2, all of which participate in vasoconstriction, while nitric oxide (NO), bradykinin, and hyperpolarizing factors act on vasodilation [3]. The endothelium thus maintains vessel integrity and hemodynamic functions through this self-regulation mechanism [3][4].
Endothelium dysfunctions represent EC failure in maintaining cardiovascular homeostasis, caused by imbalances between endothelium-derived relaxing and contracting factors and leading to deficient vasodilation and low NO synthesis and/or bioavailability in favor of vasoconstrictor elements [5]. Loss of vascular tonus homeostasis can be triggered by several cardiovascular risk factors, such as diabetes mellitus, hypertension, hypercholesterolemia, obesity, aging and chronic smoking, which lead to EC injury and activation [6][7][8][9][10][11][12]. Activated ECs acquire proinflammatory and prothrombotic phenotypes in response to injury, comprising an innate and adaptive immunity mechanism characterized by the overexpression of adhesion molecules and inflammatory cytokines, as well as platelet activation [12]. Endothelial cell activation and dysfunction are important contributors to increased arterial stiffness, atherosclerosis, and cardiovascular events [13][14].
Arterial stiffness is another clinical condition that may contribute to the pathogenesis of atherosclerosis, naturally increasing with age and commonly observed as a complication of endothelial dysfunction in individuals with risk factors for CVD [14][15]. Stiffening of the large arteries can impose extra cardiac muscle effort, leading to heart failure. The pathophysiological mechanisms that lead to arterial stiffness induced by cardiovascular risk factors are numerous, complex and do not result exclusively from endothelial dysfunction, as vessel stiffness can also alter endothelial function [16]. Some of these proposed mechanisms will be briefly discussed below. Aging is associated with lower vessel wall elastin-to-collagen ratios, due to progressive elastic fiber degeneration and increased collagen synthesis [17]. Hyperglycemia induces VSMC proliferation and enhances the formation of advanced glycation products and collagen crosslinking [18]. High blood pressure increases collagen deposition and leads to biomechanical wall fatigue and stiffness in response to repeated pulsatile stress [19]. LDL cholesterol and oxidized-LDL (oxLDL) both increase the production of reactive oxygen species (ROS) via NADPH oxidases (NOX) isoforms such as NOX 1, NOX 2, NOX 4 and NOX 5 expressed in vascular cells, and are the major ROS sources in CVD, resulting in oxidative injury and vessel stiffness [20]. Furthermore, oxLDL triggers VSMC autophagy and apoptosis, with defective autophagy leading to Ca2+ homeostasis alterations, enhancing osteogenic differentiation and VSMC calcification [21].
Recent clinical trials, meta-analyses and prospective multicenter observational studies have demonstrated that endothelial dysfunction is closely associated with abnormal arterial stiffness and the development of atherosclerosis, leading to cardiovascular complications. Therefore, early hemodynamic abnormality detection is paramount and depends on the application of reliable and non-invasive techniques, valuable as routine diagnostic procedures. Non-invasive methods, such as flow-mediated vasodilation (FMD) and pulse wave velocity (PWV) measurements, particularly the carotid–femoral (cfPWV) and brachial–ankle (baPWV) pulse wave velocities, which are recognized as indexes of arterial stiffness and the speed at which the arterial pulse propagates along the arterial wall, with cfPWV being considered the gold standard for measuring large artery stiffness, have been employed to assess endothelial function and arterial stiffness, respectively, as cardiovascular event predictors [2][22][23][24].
FMD measures endothelial function through the brachial artery diameter. As NO is the only vasodilatation mediator at this site, FMD brachial artery assessments provide a non-invasive and accurate method to measure endothelial NO production, using imaging to measure arterial dilation following post-occlusive reactive hyperemia. Together, these noninvasive methods can be applied as reliable tools for cardiovascular disease prognostics [25].
Regular fruit and vegetable consumption is associated with decreased CVD. As an example, the Mediterranean diet, characterized by a combination of antioxidant-enriched foods, confers a protective effect against CVD, where dietary compounds may maintain and/or restore cardiovascular homeostasis by increasing NO production, suppressing ROS overproduction and controlling anti-inflammatory activity [26][27]. Therefore, healthy eating patterns can reduce the global burden arising from cardiovascular disease management [28][29].
The current human lifestyle often does not allow for the adoption of healthy diets. Thus, dietary supplementation employing compounds extracted from certain food matrices, as well as new foodstuffs formulated with high concentrations of certain bioactive compounds, may comprise a convenient alternative for human health maintenance.
Several preclinical and clinical trials have highlighted the potential of certain dietary compounds as vasoactive agents, restoring endothelial function through increased NO synthesis, reversing artery stiffness and reinstating endothelial function. Dietary NO3−, L-arginine, L-citrulline and the mineral potassium (K+) are vasoactive compounds acclaimed for their beneficial effects on critical cardiovascular parameters, demonstrated in both animal models and humans [30][31][32][33][34][35][36][37]. L-arginine and NO3− are direct precursors of enzymatic and non-enzymatic NO biosynthesis, respectively [38], L-citrulline is a precursor of the endogenous L-arginine synthesis and, at the same time, an NO biosynthesis product, contributing to the de novo L-arginine-NO synthesis [39]; while K+ ions are required for normal body fluid volume maintenance, cell membrane potential and the balance between intracellular sodium (Na+) and calcium (Ca2+) ions, with beneficial effects on vascular smooth muscle relaxation and endothelium-dependent vasodilation [40][41].
2. Nitrate
Nitrate (NO3−) is a negatively charged nitric acid salt formed by a single nitrogen atom bound to three oxygen atoms, while nitrite (NO2−) is a nitrous acid salt formed by a single nitrogen atom bound to two oxygen atoms. Both can be obtained from endogenous and/or exogenous sources [42]. Endogenous NO3− and NO2− formation occurs by NO metabolism through the L-arginine/NO pathway [3]. Once in the intracellular medium, the amino acid L-arginine undergoes five-electron oxygen-dependent oxidation catalyzed by the nitric oxide synthase enzyme (NOS) and its cofactors, such as calmodulin, Ca2+, BH4, NAD, NADPH, FAD, FMN and O2, forming NO and L-citrulline [43]. In addition, shear stress (the blood flow shear force exerted on endothelial cells) can activate NOS to form NO. Once synthesized, NO is rapidly transformed to NO2− by auto-oxidation or through ceruloplasmin, a protein that plays a role in plasma copper transport. The formed NO2− can also undergo the action of oxyhemoglobin (oxyHb), generating NO3− [44].
The acquisition of exogenous NO3− takes place from drinking water and green and leafy vegetables, in addition to vegetables grown in low-light environments, as NO3− is stored and not reduced to form amino acids. Some tubers, mainly beetroot, store high NO3− content. In addition, NO2− is added to cured meat as a preservative additive [45]. The NO3− ingested by the NO3−-NO2−/NO pathway is absorbed in the proximal portion of the small intestine, possibly the jejunum, into the bloodstream or tissues, where it accumulates intracellularly as NO3−. Dietary NO3− increases quickly in plasma in about 30 min, peaking at 90 min. About 60% of the absorbed NO3− is excreted in urine and 25% is extracted by the salivary glands, concentrated in saliva through the entero-salivary cycle [46]. Concerning the salivary route, NO3− in the oral cavity is reduced to NO2− by nitrate-reductase expressed by oral commensal bacteria, such as Streptococcus salivarius, S. mitis, S. bovis and Veillonella spp., identified as the most prevalent nitrate-reductive microbiota on the tongue that use NO3− as a terminal electron acceptor to generate ATP or incorporate it into their biomass [47][48][49]. This NO2− mouth generation is sensitive to antibiotics or mouthwash, which can inactivate bacteria, compromising the conversion of NO3− to NO2− [50]. Furthermore, the metabolic activities of commensal microorganisms that inhabit the oral cavity, such as Granulicatella spp., Actinomyces, Prevotella spp., Neisseria spp., Haemophilus spp. and those belonging to the Rothia genera, can also significantly influence NO3− to NO conversion [51][52]. Subsequently, NO2− is protonated upon reaching the gastric acid, forming nitrous acid (HNO2), which spontaneously decomposes to NO and other bioactive nitrogen oxides, such as nitrogen dioxide (NO2), dinitrogen trioxide (N2O3) and the nitrosonium ion (NO+). Furthermore, HNO2 may also be decomposed to NO by ascorbic acid and polyphenols [48][49]. In the jejunum, the remaining NO3− and NO2− are rapidly absorbed into the bloodstream or tissues. Therefore, NO2− levels are considerably delayed in circulation, reaching a maximum peak after 2.5–3 h of ingestion [53], the time required for oral cavity NO3− to NO2− conversion (Figure 1).
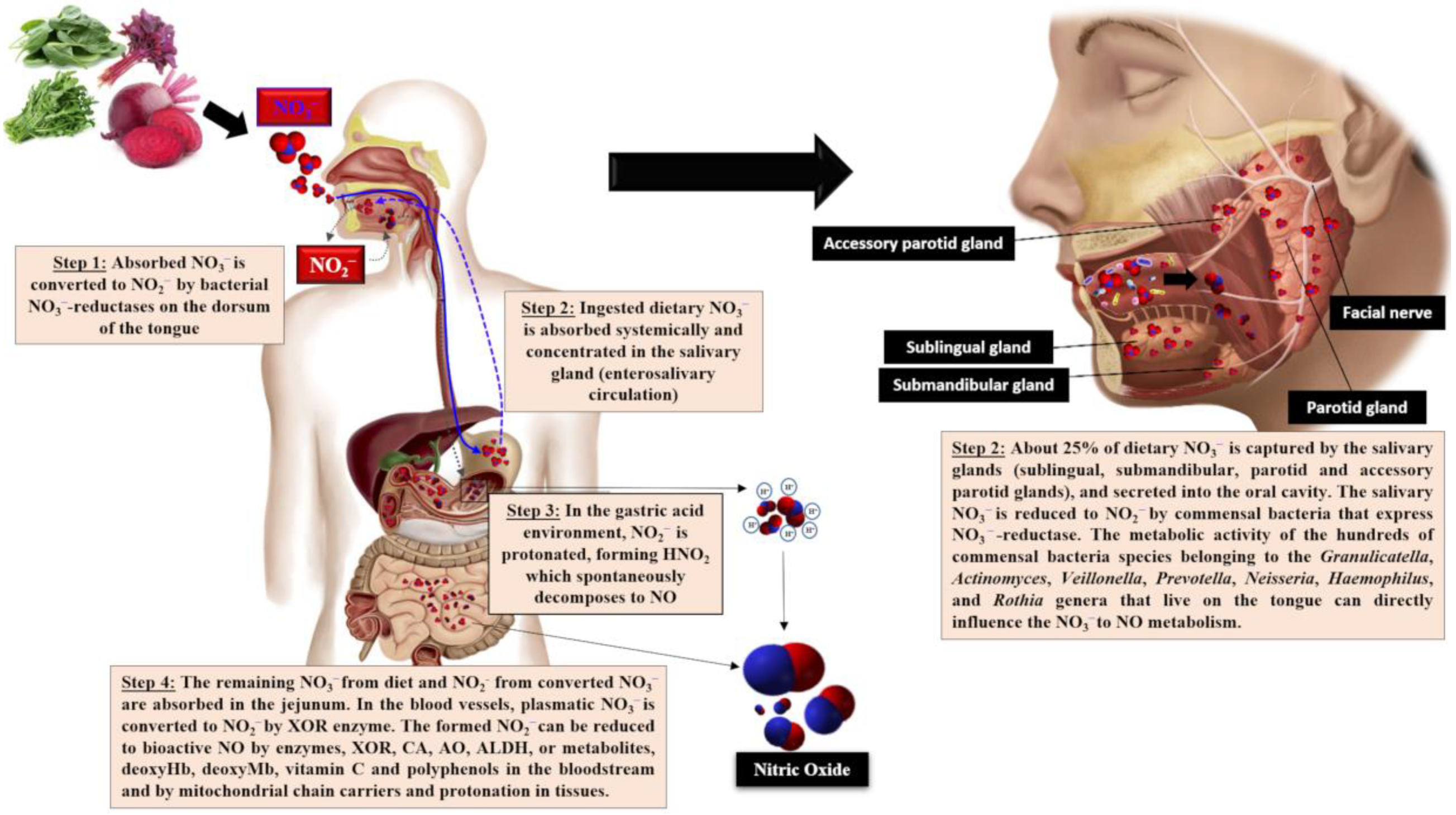
Figure 1. Triggering of the NO3−-NO2−/ NO pathway following the ingestion of NO3−-rich foods. XOR, xanthine oxidoreductase; AO, aldehyde oxidase; ALDH, aldehyde dehydrogenase; deoxyHb, deoxyhemoglobin; deoxyMb, deoxymyoglobin; CA, carbonic anhydrase.
Dietary NO3− and NO2− accumulation occurs by endogenous synthesis through the L-arginine/NO pathway. As mentioned previously, most NO3− is lost by renal clearance and a small part is extracted by the salivary glands, concentrating in the saliva, to continue the entero-salivary cycle [54][55][56]. Additionally, a small amount of plasmatic NO3− and NO2− may be reduced by xanthine oxidoreductase (XOR), which displays similar enzymatic activity to salivary nitrate reductase. Xanthine oxidoreductase catalyzes NO synthesis from the remaining NO3− and NO2−, albeit in the absence of O2. Thus, NO can be formed under both hypoxic and ischemic conditions, with increased XOR expression and activity. In addition, NO2− can be reduced to NO by deoxyhemoglobin (deoxyHb) and deoxymyoglobin (deoxyMb), especially under low O2 levels [49][53]. Other enzymes, such as aldehyde oxidase (AO), aldehyde dehydrogenase (ALDH) and carbonic anhydrase (CA), as well as antioxidant compounds, i.e., vitamin C and polyphenols, display the ability to reduce plasmatic NO2− to NO, the bioactive form [54][55].
As NO2− is not naturally found in food matrices, due to its instability and quick oxidation to NO3−, 70 to 80% of NO2− exposure originates from food additives mixed with foodstuffs. These compounds are used to improve food taste, color and appearance and prevent food oxidation, as well as the growth of foodborne pathogens and secretion of harmful compounds, such as the botulinum toxin, during meat and baked goods and cereal processing [57]. Thus, plasma NO reflects dietary NO3− intake, with 85% originating from vegetables in Western diets, although the content of this anion varies between edible plants from distinct botanical families [50]. Indeed, NO3− content in vegetables depends on their genetic background or environmental factors such as atmospheric humidity, temperature, water content and exposure to sunlight and irradiation, as well as agricultural practices, i.e., crop type, fertilization, soil conditions, the use of fertilizers and herbicides, the amounts of available nitrogen and the availability of other nutrients, and, finally, post-harvest conditions, such as transportation and storage conditions [50][58]. The NO3− contents in plant organs also differ, classified from the highest to the lowest contents as petiole > leaf > stem > root > tuber > bulb > fruit > seed. Among vegetables considered the richest NO3− food sources, beetroot (1300 mg of NO3−·kg−1), arugula (4677 mg of NO3−·kg−1) and spinach (2500 mg of NO3−·kg−1) are the most popular with respect to dietary interventions, all resulting in effective cardiovascular performance improvements estimated through blood pressure decreases and vascular function improvements [49][50][58]. Furthermore, a single serving portion of any of these vegetables contains more NO3− than is formed through internal human body processes per day. However, it is important to note that NO3− supplementation from leafy greens has been tested only in healthy individuals, and it is unknown whether its effects can be extended to individuals displaying cardiovascular risk factors. Although the protective cardiovascular effects of NO3−-enriched vegetables have been clearly demonstrated in clinical trials with healthy subjects, the large vegetable serving portions to be ingested to achieve effective NO3− plasma concentrations may comprise a limiting factor in ensuring adherence to long-term nutritional interventions [3]. In this regard, the low NO3− content in serving portions has been overcome by developing different beetroot formulations that concentrate pharmacological NO3− doses in small serving portions of an attractive food product, favoring continuous intake and better adherence to a non-drug strategy therapy in order to improve endothelial function in individuals at cardiovascular risk [3].
However, strict standards regarding the levels of these anions in foods and drinks have been established in the past. Until a decade ago, NO3− was considered a toxic compound derived from unfavorable diets, as it was mistakenly associated with the development of certain malignancies, such as metglobinemia (MetHba) and gastric cancer [59][60][61]. Therefore, the Food and Agriculture Organization of the United Nations/World Health Organization (FAO/WHO) defined an acceptable daily intake of 3.7 mg of NO3−·kg−1 of body weight in 1962, the same level adopted by the European Food Safety Authority [62][63]. For a healthy 80 kg adult, this content is the equivalent of ~300 mg NO3−·day−1. However, the adoption of vegetarian diets, in general, increases NO3− consumption in 80 kg adults to over 350 mg.day−1, well above the stipulated acceptable daily intake [64]. The association between NO3− and NO2− and MetHba in adults and children, however, has not been proven in the literature [61][65]. Furthermore, several studies have failed to demonstrate a link between dietary NO3− and NO2− ingestion and the production of N-nitrosamines, carcinogenic compounds that can lead to tumor development [66]. This evidence supports a significant link between cancer and red processed meat, with little knowledge of the effects of vegetables and drinking water available. In this regard, the inorganic NO3− and, particularly, inorganic NO2− added during meat processing may contribute to cancer development [67]. Nonetheless, the hypothesis that both dietary NO3− and NO2− from foods, mainly from plant origin, are toxic has been established based merely on conjecture.
Health organizations have established an adequate NO3− intake of around 40–185 mg·day−1 (1 to 3 mmol·day−1) in Europe and 40–100 mg·day−1 (1 to 1.6 mmol·day−1) in the USA, considering 100% NO3− bioavailability following dietary intake [68]. However, considering the role of NO3− on cardiovascular system function, none or minimal beneficial hemodynamic and vascular effects have been observed following acute NO3− administration or short-period administration for under 14 days [3][58]. Increases in plasmatic NO3− levels, from 31 to 150 μM, as well as NO2−, from 0.23 to 0.40 μM, have been observed, but no improvements were detected in SBP and FMD following 14 days of supplementation with 7.5 mmol NO3− from beetroot juice in elderly patients with type 2 diabetes mellitus [69]. No changes in arterial stiffness, assessed by PWV and AIx, or in blood pressure were observed in normotensive individuals after a 7-day intake of 6.4 mmol NO3− from green leafy vegetables, although increased plasmatic NO3− levels, from 23.4 to 152 μM, and NO2−, from 2.0 to 8.0 μM, were observed [70]. Furthermore, Bondonno et al. [71] did not observe modifications in domestic BP, and ambulatory 24 h SBP and DBP in hypertensive individuals supplemented for 7 days with 7.0 mmol NO3− from beetroot juice, although increased NO synthesis was observed, assessed through NO3− and NO2− determinations in plasma, urine, and saliva.
On the other hand, when NO3− is provided as a chronic dietary supplementation, the beneficial effects on vascular function are more consistents. Kapil et al. [72] observed a decrease in systolic (SBP) and diastolic blood pressure (DBP), decrease in PWV, and an increase and improvement of AIx and FMD, respectively, of hypertensive volunteers after supplementation with 6.4 mmol NO3− during 28 days, corresponding to 400 mg/day of beetroot juice. Endothelial function and arterial stiffness improvements and decreased blood pressure were observed simultaneously with increased NO synthesis, estimated by increased NO3− plasma levels, from ≈40 to ≈200 μM, as well as higher NO2− levels, from ≈0.4 to ≈0.9 µM. Rammos et al. [73] administered 150 µmol·kg−1 of NaNO3−, at least 10.5 mmol for a 70 kg individual, for 28 days to elderly patients presenting moderate CVD risks, also describing increases in average NO3− plasma concentrations, varying from 32 to 263 μM, and NO2− concentrations, ranging from 0.08 to 0.33 μM, alongside improved FMD and decreased SBP, DBP, PWV and AIx. Recent systematic reviews and meta-analysis studies have evaluated vascular responses to dietary NO3− and confirmed BP decreases and endothelial dysfunction amelioration. A systematic review conducted by Bahadoran et al. [74] demonstrated that beetroot juice intake reduces SBP [−3.55 mm Hg; 95% CI: −4.55, −2.54 mm Hg] and DBP [−1.32 mm Hg; 95% CI: −1.97, −0.68 mm Hg]. Furthermore, decreased SBP depends on the amount of beetroot juice intake, where comparisons between 500 mL and 70 mL and 140 mL·day−1 indicate −4.78 vs. −2.37 mm Hg decreases. Longer supplementation periods compared to shorter ones (≥14 days vs. <14 days of treatment) led to a −5.11 vs. −2.67 mm Hg decrease. In another systematic review and meta-analysis, randomized controlled trials indicated that NO3− supplementation from beetroot juice for longer than 14 days reduced both SBP (−3.55 mm Hg; 95% CI: −4.55, −2.54 mm Hg) and DBP (−1.32 mm Hg; 95% CI: −1.97, −0.68 mm Hg). Furthermore, beneficial dietary NO3− effects on endothelial function are associated with dose, age, and body mass index (BMI), where chronic beet juice supplementation improved FMD and endothelium function according to the administered NO3− dose (β = 0.04, SE = 0.01, p < 0.001), age (β = −0.01, SE = 0.004, p = 0.02) and BMI (β = −0.04, SE = 0.02, p = 0.05) [75].
3. L-Arginine
L-arginine (2-amino-5-guanidinopentanoic acid) is a semi-essential cationic amino acid obtained through dietary intake, protein turnover, and/or de novo synthesis from L-citrulline in liver, and from the kidney urea cycle [76]. Oral L-arginine undergoes gastrointestinal and hepatic extractions before reaching portal circulation, where arginases from enterocytes and liver catalyze the hydrolysis of L-arginine into L-ornithine and urea, which limits systemic L-arginine levels (Figure 2A). L-arginine is also biosynthesized in the kidneys through L-citrulline metabolism following the conversion of exogenous L-citrulline (not metabolized in the liver first-pass) to the precursor arginosuccinate, catalyzed by arginosuccinate synthase, and then converted to L-arginine by arginosuccinate lyase in the urea cycle [76].
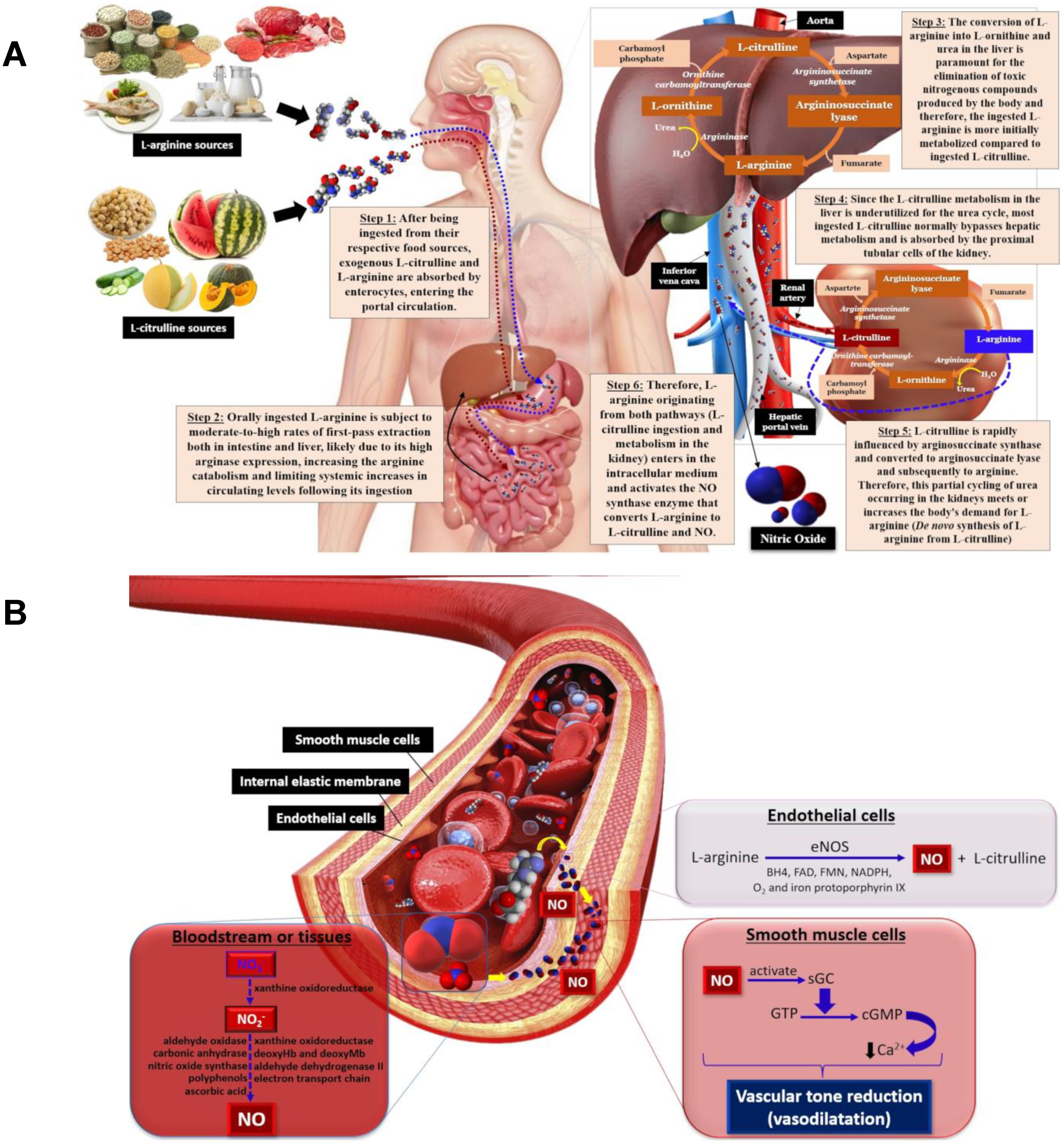
Figure 2. The metabolic pathway for L-arginine and L-citrulline obtained from food sources, urea cycle and NO biosynthesis (A); NO biosynthesis from L-arginine by eNOS promotes vasodilation by activating guanylate cyclase to form cGMP that, in turn, decreases Ca2+ within smooth muscle cells, diminishing vascular tone and leading to vasodilation (B). eNOS—endothelial nitric oxide synthase, BH4—tetrahydrobiopterin, FAD—flavin adenine dinucleotide, FMN—flavin mononucleotide, GC—guanylate cyclase, GTP—guanosine triphosphate, cGMP—cyclic guanosine monophosphate, Ca2+—calcium ions.
L-arginine is involved in NO synthesis, and is employed as a substrate for nitric oxide synthase (NOS) class enzymes, comprising neuronal (nNOS), inducible (iNOS) and endothelial (eNOS) isoforms. As mentioned previously, L-arginine, the substrate, adenine dinucleotide phosphate (NADPH) as the electron cofactor, and O2 are involved in NO synthesis, forming citrulline and NADP+. Tetrahydrobiopterin (BH4), flavin adenine dinucleotide (FAD), flavin mononucleotide (FMN) and iron protoporphyrin IX are all cofactors involved in this reaction [77]. Once synthesized, NO diffuses from endothelial cells to smooth muscle cells in blood vessels and activates the soluble guanylate cyclase (GC) enzyme that, in turn, catalyzes the conversion of guanosine triphosphate (GTP) to cyclic guanosine monophosphate (cGMP) and pyrophosphate (PPi) [78]. Subsequently, cGMP decreases intracellular Ca2+ concentrations by activating the calcium pump within smooth muscle cells, inducing vasodilation through reduced vascular tone [79][80][81] (Figure 2B).
L-arginine is found in nuts, such as peanuts and walnuts, but also in foods of animal origin, such as meats, poultry, fish and dairy products, providing an intake of about 4.4 g/day of this amino acid in Western diets [82]. Considering that L-arginine is the NO substrate for NO synthesis and its involvement in endothelium-dependent dilatation, the beneficial effects of L-arginine supplementation on endothelial dysfunction and arterial stiffness have attracted attention for some time, aiming to overcome hemodynamic abnormalities and risk factors, thus avoiding cardiovascular events.
In a prospective, double-blind, randomized crossover trial with elderly healthy individuals (age 73.8 ± 2.7 years), the L-arginine supplementation of 16 g/day for 2 weeks increased L-arginine plasma levels from 57.4 ± 5.0 mM to 114.9 ± 11.6 mM, improving endothelial-dependent vasodilation [34]. Similar to aging, smoking represents a harmful condition leading to endothelial dysfunction and decreased NO biosynthesis alongside inflammatory responses caused by endothelium injury, which can be counteracted by L-arginine supplementation. Six grams/day of L-arginine administered for 3 days to 10 healthy smokers in a randomized, placebo-controlled, double-blind, and cross-over clinical trial led to an improvement on FMD baseline and prevented smoking-induced FMD decreases at day 1. The supplementation was, however, unable to sustain this up to day 3. On the other hand, L-arginine decreased both PWV and AIx at days 1 and 3 compared to the placebo [83]. In a similar study, L-arginine supplemented at 21 g/day for 3 days to 12 healthy smokers improved FMD baselines, but did not cease smoking effects, while smoking-induced PWV and AIx increases were inhibited by L-arginine supplementation [84]. L-arginine may, therefore, be considered a very promissory positive effector, able to prevent the arterial stiffness increment associated with smoking behavior. L-arginine also seems to improve endothelial function in subjects presenting coronary artery disease (CAD) [85]. Following an intake of 21 g of L-arginine for 10 days resulted in an FMD improvement by 4.7 ± 1.1 vs. 1.8 ± 0.7% (p < 0.04). Similarly, the intake of 10 g of L-arginine by stable CAD patients for a longer period of time of 4 weeks reduced endothelial dysfunction, as demonstrated by changes in FMD diameter, increasing the diameter by 4.87% (p < 0.0001) compared to baseline values. The conclusions from that study, however, were limited, due to its open-label clinical trial character, as the placebo group received vitamin C, which is also an active compound [86]. On the other hand, in a similar clinical double-blind and placebo-controlled trial, chronic L-arginine therapy was shown to increase the reactive hyperemia of the forearm blood flow by employing venous occlusion plethysmography in individuals displaying stable CAD for 6 months. The hyperemic flow of the forearm is considered an endothelial-mediated vasodilation marker and has been shown to depend on NO synthesis. The positive correlation between the 6.4 g/day L-arginine supplementation, c-GMP and reactive hyperemia increments reinforces the role of L-arginine in NO synthesis enhancement and consequent endothelial function improvement [87]. Coronary endothelial dysfunction has been proposed to predict the progression of atherosclerotic disease and cardiovascular event rates [88], and, although the clinical trials presented in this research have not evaluated the effect of L-arginine on the coronary artery, the findings presented herein indicate that L-arginine supplementation may comprise a promising alternative against endothelial function impairment in CAD patients and be able to inhibit unfavorable cardiovascular outcomes.
L-arginine intake for 28 days or more has also been shown to protect against others chronic pathologies deleterious to vascular function. The daily ingestion of 8 g L-arginine improved endothelial function in 28 women with polycystic ovary syndrome (PCOS) who were making use of oral contraceptives. PCOS is a pathological condition associated with low NO bioavailability due to its inadequate release, production, or degradation. This results in endothelium-dependent vasodilatation impairment and cardiovascular risks that may be exacerbated by oral contraceptives [89][90]. For the treatment of PCOS, ultrasonographic and Doppler flow evaluations revealed that L-arginine supplementation promoted a significant improvement in brachial artery diameter and pulsatility index at 15 s after reactive hyperemia, compared to the baseline. This effect was not observed in contraceptive plus placebo group. L-arginine supplementation did not lead to any blood pressure variations, whereas the placebo group displayed increases for 24 h, both during the day and during the night. Increased plasma NO3− and NO2− following L-arginine intake confirmed NO availability and endothelial function improvements. However, the most important finding in this intervention comprised the fact that endothelial function and NO production effects were extended for 6 months following L-arginine supplementation, demonstrating a sustained effect following 28 days of L-arginine administration [90].
Oral administration of 8 g L-arginine to 15 congestive heart failure patients for 60 days led to endothelial function improvements, evaluated through the maximum amplitude time (MAT), total wave time (TT) and MAT/TT ratio obtained through photoplethysmography following forearm blood flow occlusion and reactive hyperemia in comparison to pre-ischemia levels [91]. Photoplethysmography can be used to indirectly evaluate endothelial function in peripheral vessels by sensing vasodilatation in the index finger, since changes in blood flow and pulse wave amplitude are the result of flow-mediated vasodilatation following NO synthesis [92]. Although the dietary intervention was limited due to the low number of patients, the absence of a control group, and the method reflecting only the microvascular status, L-arginine supplementation decreased MAT/TT values to under 30, similar to values observed in healthy individuals, demonstrating its modulation on NO-mediated vasodilation [93]. Likewise, a 12-week supplementation with 9 g of L-arginine was able to circumvent the PWV ≥ 900 cm/s commonly found in chronic kidney disease (CKD) patients. Clinical CKD manifestations increase the risks for CAD, heart failure and cardiac death due to the pathological vascular remodeling, calcification and arterial stiffness that underly kidney disease [93]. The chronic intake of L-arginine promoted a significant increase in NO levels and decreased aortic stiffness, overcoming NO baseline levels and PWV, confirming vascular damage caused by kidney impairment and the effectiveness of L-arginine supplementation in reversing hemodynamic abnormalities in CKD patients, probably caused by a defective L-arginine/NO biosynthesis [94].
Postprandial endothelial dysfunction is a clinically important condition and has been reported following high-fat meals in both healthy subjects and in those with risk factors for CVD. Postprandial endothelial dysfunction has been proposed to be triggered through oxidative stress induced by hypertriglyceridemia, where NO bioavailability is reduced by the superoxide anion (O2−), resulting in the generation of the highly reactive and cytotoxic peroxynitrite [95][96][97]. In overweight adults with high triglyceride plasma levels and waist circumference measurements, L-arginine supplementation was able to overcome cardiovascular risk factors following 4.5 g supplementation for 4 weeks, where an inhibition of the decrease in postprandial endothelial function induced by a high-fat meal was observed, demonstrated by a 29% reduction in FMD when compared to a 50% reduction in FMD in placebo-treated subjects. In this clinical trial, a 5% increase in reactive hyperemia was also observed, while there was a 49% reduction in placebo treatment [98]. Similarly, a single dose of 15 g of L-arginine attenuated the FMD reduction promoted by high-fat meals compared with a placebo treatment in forty healthy men (from 10.3 ± 1.3 to 9.3 ± 0.9% in the L-arginine supplementation group and from 10.5 ± 1.2% to 6.8 ± 1.4%, in the placebo group) [99]. These findings indicate that L-arginine may increase NO bioavailability and reduce endothelial dysfunction induced by postprandial hypertriglyceridemia.
4. L-Citrulline
L-citrulline, a non-essential amino acid not commonly found in proteins, is involved in nitrogen homeostasis and shows promising vascular benefits in promoting endothelial vasodilation. L-citrulline is efficiently converted to L-arginine, the endogenous NO biosynthesis precursor that acts in reducing arterial stiffness, as discussed previously (Figure 2B) [35][100][101]. Dietary L-citrulline passes through the liver to the kidneys, where it is converted to L-arginine via the argininosuccinate biosynthesis in the urea cycle, producing extra NO (Figure 2A). Studies have reported that L-citrulline can indirectly reduce blood pressure by increasing NO biosynthesis, improving arterial function, blood flow and circulation and, thus, reducing the risk of heart disease [102][103].
L-citrulline is found in legumes, fruits, and grains, such as onions, garlic, chickpeas, peanuts, and soy, and the highest concentrations of this amino acid are found in watermelon pulp and rinds in concentrations ranging between 0.7 and 3.6 g.kg−1 of fresh weight depending on the type of cultivar [101][104][105]. L-citrulline has been widely commercialized as a supplement, and is available at higher doses than those found in natural foods. Marketed L-citrulline is mainly consumed by athletes to assist in sports performance and muscle mass gain [106][107].
Although L-citrulline was for many years considered simply a metabolic intermediate of little biological interest, studies have confirmed that it increases circulating L-arginine levels more efficiently than L-arginine supplementation, the final product formed during L-citrulline metabolization. A large amount of the ingested L-arginine is degraded during the extensive pre-systemic metabolism by intestinal bacteria and by arginase found in the liver and gut mucosa. In contrast, L-citrulline is preserved during the pre-systemic metabolism, effectively transported across the intestinal luminal membrane and then converted to L-arginine in the kidneys. Subsequently, L-arginine is converted to L-citrulline and NO by eNOS in endothelial cells [35][54][76][103][108]. The absorption characteristics of oral L-citrulline indicate that the use of this amino acid comprises an attractive non-pharmacological approach that may counteract cardiovascular pathophysiological conditions.
The endothelial function effects of watermelon ingestion for seven consecutive days were investigated on the basis of FMD measurements. Six healthy overweight/obese adults received 100 kcal serving portions prepared from watermelon pulp, rind, and seeds, while the control group received flour. FMD reactivity assessed in the brachial artery after 7 h intake showed no differences, with the authors ascribing the inconclusive results to a low sample number [109]. When evaluating the supplementation of eleven young adults with 30 g of microencapsulated watermelon rind (MWR) containing 4 g of L-citrulline, improved endothelial function assessed by FMD was observed alongside with increased L-citrulline and L-arginine plasma levels [110].
One hypothesis postulate that postprandial hyperglycemia and acute hyperlipidemia both induce endothelial dysfunction as measured by FMD throughout oxidative stress induction, since free radicals quench NO, disrupting endothelial-dependent vasodilation [96]. In a randomized, placebo-controlled, double-blind, crossover trial, 17 healthy young adults from 21 to 25 years old, 6 males and 11 females, were supplemented with 500 mL of watermelon juice for 2 weeks and underwent an oral glucose tolerance test followed by postprandial FMD, to evaluate endothelial function following hyperglycemia induction and L-citrulline supplementation effects. Although no significant effects were observed on plasma L-citrulline and L-arginine, the latter showed a tendency to increase compared to placebo and the postprandial FMD area AUC was higher after juice supplementation when compared with the placebo group (838 ± 459% vs. 90 min compared with 539 ± 278% vs. 90 min). [111]. In this way, supplementation with L-citrulline, as a precursor of L-arginine and consequently of nitric oxide, seems to have the potential to attenuate the endothelial dysfunction induced by high glucose levels, but more studies need to be carried out.
Another randomized, double-blind, placebo-controlled trial study was performed to evaluate the effects of watermelon juice on vascular health, albeit in 21 healthy postmenopausal women. Subjects were randomized to consume two 360 mL servings of 100% watermelon juice ingested daily or an isocaloric placebo for 4 weeks. Vascular function assessments included pulse pressure, PWV, 24 h ambulatory BP, and FMD. In contrast to the findings of previous clinical trials in younger adults, the watermelon juice supplementation did not affect vascular parameters compared to the placebo, indicating that a 720 mL dosage/day of watermelon juice is insufficient to alter serum L-arginine in postmenopausal women, possibly explaining the unchanged vascular function [112]. On the other hand, watermelon supplementation (L-citrulline/L-arginine 6 g/d) to twelve obese, hypertensive postmenopausal women for 6 weeks significantly lowered baPWV, aortic SBP and DBP compared to placebo [113], which suggests that the vascular effects of watermelon L-citrulline may be more pronounced when the individual has some cardiovascular risk factor.
Following randomized crossover studies, watermelon intake enriched in L-citrulline promoted aortic blood pressure and arterial function amelioration in hypertensive individuals. The pilot study assessed nine participants, four men and five women aged 54 ± 3 years, who were diagnosed with pre-hypertension and consumed 2.7 g/day of watermelon or placebo for 6 weeks. Both the AIx and AIx adjusted for an HR of 75 beats/min (AIx 75) decreased in the watermelon-supplemented group (−6.0 ± 3% and −4.0 ± 2%, respectively). At the same time, no PWV carotid–femoral or reflected wave (Tr) transit time effects were noted [114]. In another study, carotid AIx (cAIx) measures were performed instead of aortic AIx, since the former can more precisely reflect the central AIx. After 6 weeks of watermelon supplementation containing 6 g of L-citrulline/L-arginine administered daily, decreased cAlx values (−8.8 ± 2.6%) were observed in 14 obese middle-aged adults presenting prehypertension or stage 1 hypertension, reflecting artery endothelium function improvements [103].
Acute ingestion of L-citrulline (3 g) effectively increases the availability of L-arginine and NO in both young and elderly adults with heart failure. L-citrulline supplementation increased NO synthesis 10-fold, but was ineffective at promoting endothelium-mediated vasodilation in the two CVD subject groups. These results imply that other factors besides NO may play a role in vascular dysfunction. In addition, longer-term L-arginine or L-citrulline supplementation is required to reverse peripheral vascular function impairment in older adults with heart failure. Younger adults are more sensitive to the acute ingestion of L-citrulline compared to the elderly, due to the efficacy in converting this compound to L-arginine. Older adults present a higher L-arginine to ornithine conversion rate via arginase in the urea cycle, illustrating NO synthesis differenced with aging [115].
References
- Rahimi, N. Defenders and Challengers of Endothelial Barrier Function. Front. Immunol. 2017, 8, 1847.
- Sun, Y.; Liu, F.; Zhang, Y.; Lu, Y.; Su, Z.; Ji, H.; Cheng, Y.; Song, W.; Hidru, T.H.; Yang, X.; et al. The Relationship of Endothelial Function and Arterial Stiffness with Subclinical Target Organ Damage in Essential Hypertension. J. Clin. Hypertens. 2022, 24, 418–429.
- dos Santos Baião, D.; Vieira Teixeira da Silva, D.; Margaret Flosi Paschoalin, V. A Narrative Review on Dietary Strategies to Provide Nitric Oxide as a Non-Drug Cardiovascular Disease Therapy: Beetroot Formulations—A Smart Nutritional Intervention. Foods 2021, 10, 859.
- Lai, W.K.; Kan, M.Y. Homocysteine-Induced Endothelial Dysfunction. Ann. Nutr. Metab. 2015, 67, 1–12.
- Ghosh, A.; Gao, L.; Thakur, A.; Siu, P.M.; Lai, C.W.K. Role of Free Fatty Acids in Endothelial Dysfunction. J. Biomed. 2017, 24, 50.
- Ohsugi, M.; Adachi, K.; Horai, R.; Kakuta, S.; Sudo, K.; Kotaki, H.; Tokai-Nishizumi, N.; Sagara, H.; Iwakura, Y.; Yamamoto, T. Kid-mediated Chromosome Compaction Ensures Proper Nuclear Envelope Formation. Cell 2008, 132, 771–782.
- Blumenthal, J.A.; Hinderliter, A.L.; Smith, P.J.; Mabe, S.; Watkins, L.L.; Craighead, L.; Ingle, K.; Tyson, C.; Lin, P.H.; Kraus, W.E.; et al. Effects of Lifestyle Modification on Patients with Resistant Hypertension: Results of the TRIUMPH Randomized Clinical Trial. Circulation 2021, 144, 1212–1226.
- Ozkor, M.A.; Hayek, S.S.; Rahman, A.M.; Murrow, J.R.; Kavtaradze, N.; Lin, J.; Manatunga, A.; Quyyumi, A.A. Contribution of Endothelium-Derived Hyperpolarizing Factor to Exercise-induced Vasodilation in Health and Hypercholesterolemia. Vasc. Med. 2015, 20, 14–22.
- Seals, D.R.; Jablonski, K.L.; Donato, A.J. Aging and Vascular Endothelial Function in Humans. Clin. Sci. 2011, 120, 357–375.
- Virdis, A. Endothelial Dysfunction in Obesity: Role of Inflammation. High Blood Press. Cardiovasc. Prev. 2016, 23, 83–85.
- Messner, B.; Bernhard, D. Smoking and Cardiovascular Disease: Mechanisms of Endothelial Dysfunction and Early Atherogenesis. Arterioscler. Thromb. Vasc. Biol. 2014, 34, 509–515.
- Pober, J.S.; Min, W.; Bradley, J.R. Mechanisms of Endothelial Dysfunction, Injury, and Death. Annu. Rev. Pathol. 2009, 4, 71–95.
- Daiber, A.; Steven, S.; Weber, A.; Shuvaev, V.V.; Muzykantov, V.R.; Laher, I.; Li, H.; Lamas, S.; Münzel, T. Targeting vascular (endothelial) dysfunction. Br. J. Pharmacol. 2017, 174, 1591–1619.
- Oliver, J.J.; Webb, D.J. Noninvasive Assessment of Arterial Stiffness and Risk of Atherosclerotic Events. Arterioscler. Thromb. Vasc. Biol. 2003, 23, 554–566.
- Cavalcante, J.L.; Lima, J.A.; Redheuil, A.; Al-Mallah, M.H. Aortic Stiffness: Current Understanding and Future Directions. J. Am. Coll. Cardiol. 2011, 57, 1511–1522.
- Zieman, S.J.; Melenovsky, V.; Kass, D.A. Mechanisms, Pathophysiology, and Therapy of Arterial Stiffness. Arterioscler. Thromb. Vasc. Biol. 2005, 25, 932–943.
- Kohn, J.C.; Lampi, M.C.; Reinhart-King, A. Age-Related Vascular Stiffening: Causes and Consequences. Front. Genet. 2015, 6, 112.
- Schram, M.T.; Schalkwijk, C.G.; Bootsma, H.A.; Fuller, J.H.; Chaturvedi, N.; Stehouwer, C.D.A. Advanced Glycation end Products are Associated with Pulse Pressure in Type 1 Diabetes. Hypertension 2005, 46, 232–237.
- Laurent, S.; Boutouyrie, P. The Structural Factor of Hypertension: Large and Small Artery Alterations. Circ. Res. 2015, 116, 1007–1021.
- Zhang, Y.; Murugesan, P.; Huang, K.; Cai, H. NADPH Oxidases and Oxidase Crosstalk in Cardiovascular Diseases: Novel Therapeutic Targets. Nat. Rev. Cardiol. 2020, 17, 170–194.
- Lacolley, P.; Regnault, V.; Laurent, S. Mechanisms of Arterial Stiffening: From Mechanotransduction to Epigenetics. Arterioscler. Thromb. Vasc. Biol. 2020, 40, 1055–1062.
- Segers, P.; Rietzschel, E.R.; Chirinos, J.A. How to Measure Arterial Stiffness in Humans. Arterioscler. Thromb. Vasc. Biol. 2020, 40, 1034–1043.
- Tršan, J.; Košuta, D.; Rajkovič, U.; Fras, Z.; Jug, B.; Novaković, M. Vascular Function in Patients after Myocardial Infarction: The Importance of Physical Activity. Front. Physiol. 2021, 12, 763043.
- Maruhashi, T.; Soga, J.; Fujimura, N.; Idei, N.; Mikami, S.; Iwamoto, Y.; Iwamoto, A.; Kajikawa, M.; Matsumoto, T.; Oda, N.; et al. Endothelial Dysfunction, Increased Arterial Stiffness, and Cardiovascular Risk Prediction in Patients with Coronary Artery Disease: FMD-J (Flow-Mediated Dilation Japan) Study A. J. Am. Heart Assoc. 2018, 7, e008588.
- Chia, P.Y.; Teo, A.; Yeo, T.W. Overview of the Assessment of Endothelial Function in Humans. Front. Med. 2020, 7, 542567.
- Yubero-Serrano, E.M.; Fernandez-Gandara, C.; Garcia-Rios, A.; Rangel-Zuñiga, O.A.; Gutierrez-Mariscal, F.M.; Torres-Peña, J.D.; Marin, C.; Lopez-Moreno, J.; Castaño, J.P.; Delgado-Lista, J.; et al. Mediterranean Diet and Endothelial Function in Patients with Coronary Heart Disease: An Analysis of the CORDIOPREV Randomized Controlled Trial. PLoS Med. 2020, 17, e1003282.
- Baião, D.D.S.; de Freitas, C.S.; Gomes, L.P.; da Silva, D.; Correa, A.C.N.T.F.; Pereira, P.R.; Aguila, E.M.D.; Paschoalin, V.M.F. Polyphenols from Root, Tubercles and Grains Cropped in Brazil: Chemical and Nutritional Characterization and Their Effects on Human Health and Diseases. Nutrients 2017, 9, 1044.
- Yu, E.; Malik, V.S.; Hu, F.B. Cardiovascular Disease Prevention by Diet Modification: JACC Health Promotion Series. J. Am. Coll. Cardiol. 2018, 72, 914–926.
- Roth, G.A.; Mensah, G.A.; Johnson, C.O.; Addolorato, G.; Ammirati, E.; Baddour, L.M.; Barengo, N.C.; Beaton, A.Z.; Benjamin, E.J.; Benziger, C.P.; et al. Global Burden of Cardiovascular Diseases and Risk Factors, 1990-2019: Update from the GBD 2019 Study. J. Am. Coll. Cardiol. 2020, 76, 2982–3021.
- Carlström, M.; Larsen, F.J.; Nyström, T.; Hezel, M.; Borniquel, S.; Weitzberg, E.; Lundberg, J.O. Dietary Inorganic Nitrate Reverses Features of Metabolic Syndrome in Endothelial Nitric Oxide Synthase-Deficient Mice. Proc. Natl. Acad. Sci. USA 2010, 107, 17716–17720.
- Zhao, Y.X.; Tong, L.; Zhang, G.M.; Zhao, X.H.; Sa, Y.P.; Liu, Y.; Lu, D.X.; Ga, Q.; Wu, P. L-Arginine Supplementation Improves Vascular Endothelial Dysfunction Induced by High-Fat Diet in Rats Exposed to Hypoxia. Wilderness Environ. Med. 2020, 31, 400–406.
- Tsuboi, T.; Maeda, M.; Hayashi, T. Administration of L-Arginine Plus L-Citrulline or L-Citrulline Alone Successfully Retarded Endothelial Senescence. PLoS ONE 2018, 13, e0192252.
- Zhou, M.S.; Kosaka, H.; Yoneyama, H. Potassium Augments Vascular Relaxation Mediated by Nitric Oxide in The Carotid Arteries of Hypertensive Dahl Rats. Am. J. Hypertens. 2000, 13, 666–672.
- Bode-Böger, S.M.; Muke, J.; Surdacki, A.; Brabant, G.; Böger, R.H.; Frölich, J.C. Oral L-Arginine Improves Endothelial Function in Healthy Individuals Older than 70 Years. Vasc. Med. 2003, 8, 77–81.
- Allerton, T.D.; Proctor, D.N.; Stephens, J.M.; Dugas, T.R.; Spielmann, G.; Irving, B.A. L-Citrulline Supplementation: Impact on Cardiometabolic Health. Nutrients 2018, 10, 921.
- Raubenheimer, K.; Hickey, D.; Leveritt, M.; Fassett, R.; Ortiz de Zevallos Munoz, J.; Allen, J.D.; Briskey, D.; Parker, T.J.; Kerr, G.; Peake, J.M.; et al. Acute Effects of Nitrate-Rich Beetroot Juice on Blood Pressure, Hemostasis and Vascular Inflammation Markers in Healthy Older Adults: A Randomized, Placebo-Controlled Crossover Study. Nutrients 2017, 22, 1270.
- Blanch, N.; Clifton, P.M.; Petersen, K.S.; Keogh, J.B. Effect of Sodium and Potassium Supplementation on Vascular and Endothelial Function: A Randomized Controlled Trial. Am. J. Clin. Nutr. 2015, 101, 939–946.
- Lundberg, J.O.; Weitzberg, E.; Gladwin, M.T. The Nitrate-Nitrite-Nitric Oxide Pathway in Physiology and Therapeutics. Nat. Rev. Drug Discov. 2008, 7, 156–167.
- Nyawose, S.; Naidoo, R.; Naumovski, N.; McKune, A.J. The Effects of Consuming Amino Acids L-Arginine, L-Citrulline (and Their Combination) as a Beverage or Powder, on Athletic and Physical Performance: A Systematic Review. Beverages 2022, 8, 48.
- Nomura, N.; Shoda, W.; Uchida, S. Clinical Importance of Potassium Intake and Molecular Mechanism of Potassium Regulation. Clin. Exp. Nephrol. 2019, 23, 1175–1180.
- Ekmekcioglu, C.; Elmadfa, I.; Meyer, A.L.; Moeslinger, T. The Role of Dietary Potassium in Hypertension and Diabetes. J. Physiol. Biochem. 2016, 72, 93–106.
- Omar, S.A.; Artime, E.; Webb, A.J. A Comparison of Organic and Inorganic Nitrates/Nitrites. Nitric Oxide 2012, 26, 229–240.
- Alzahrani, H.S.; Jackson, K.G.; Hobbs, D.A.; Lovegrove, J.A. The Role of Dietary Nitrate and the Oral Microbiome on Blood Pressure and Vascular Tone. Nutr. Res. Rev. 2020, 34, 222–239.
- Reina-Torres, E.; De Leso, M.L.; Pasquale, L.R.; Madekurozwa, M.; van Batenburg-Sherwood, J.; Overby, D.R.; Daniel Stamer, W. The Vital Role for Nitric Oxide in Intraocular Pressure Homeostasis. Prog. Retin. Eye Res. 2021, 83, 100922.
- Gilchrist, M.; Winyard, P.G.; Benjamin, N. Dietary Nitrate—Good or Bad? Nitric Oxide 2010, 22, 104–109.
- Baião, D.S.; da Silva, D.V.T.; Del Aguila, E.M.; Paschoalin, V.M.F. Nutritional, Bioactive and Physicochemical Characteristics of Different Beetroot Formulations. In Food Additives; Intech Open: London, UK, 2017; Volume 2, pp. 20–44.
- González-Soltero, R.; Bailén, M.; de Lucas, B.; Ramírez-Goercke, M.I.; Pareja-Galeano, H.; Larrosa, M. Role of Oral and Gut Microbiota in Dietary Nitrate Metabolism and Its Impact on Sports Performance. Nutrients 2020, 12, 3611.
- Lidder, S.; Webb, A.J. Vascular Effects of Dietary Nitrate (as Found in Green Leafy Vegetables and Beetroot) via the Nitrate-Nitrite-Nitric Oxide Pathway. Br. J. Clin. Pharmacol. 2013, 75, 677–696.
- Blekkenhorst, L.C.; Bondonno, N.P.; Liu, A.H.; Ward, N.C.; Prince, R.L.; Lewis, J.R.; Devine, A.; Croft, K.D.; Hodgson, J.M.; Bondonno, C.P. Nitrate, the Oral Microbiome, and Cardiovascular Health: A Systematic Literature Review of Human and Animal Studies. Am. J. Clin. Nutr. 2018, 107, 504–522.
- Burleigh, M.; Liddle, L.; Muggeridge, D.J.; Monaghan, C.; Sculthorpe, N.; Butcher, J.; Henriquez, F.; Easton, C. Dietary Nitrate Supplementation Alters the Oral Microbiome but Does Not Improve the Vascular Responses to an Acute Nitrate Dose. Nitric Oxide 2019, 89, 54–63.
- Karwowska, M.; Kononiuk, A. Nitrates/Nitrites in Food-Risk for Nitrosative Stress and Benefits. Antioxidants 2020, 9, 241.
- McDonagh, S.T.J.; Wylie, L.J.; Webster, J.M.A.; Vanhatalo, A.; Jones, A.M. Influence of Dietary Nitrate Food Forms on Nitrate Metabolism and Blood Pressure in Healthy Normotensive Adults. Nitric Oxide 2018, 72, 66–74.
- Weitzberg, E.; Lundberg, J.O. Novel Aspects of Dietary Nitrate and Human Health. Annu. Rev. Nutr. 2013, 33, 129–159.
- Lundberg, J.O.; Gladwin, M.T.; Weitzberg, E. Strategies to Increase Nitric Oxide Signalling in Cardiovascular Disease. Nat. Rev. Drug Discov. 2015, 14, 623–641.
- Woessner, M.N.; Levinger, I.; Neil, C.; Smith, C.; Allen, J.D. Effects of Dietary Inorganic Nitrate Supplementation on Exercise Performance in Patients with Heart Failure: Protocol for a Randomized, Placebo-Controlled, Cross-Over Trial. JMIR Res. Protoc. 2018, 7, e86.
- Koch, C.D.; Gladwin, M.T.; Freeman, B.A.; Lundberg, J.O.; Weitzberg, E.; Morris, A. Enterosalivary nitrate metabolism and the microbiome: Intersection of microbial metabolism, nitric oxide and diet in cardiac and pulmonary vascular health. Free Radic Biol Med. 2017, 105, 48–67.
- Tamme, T.; Reinik, M.; Püssa, T.; Roasto, M.; Meremäe, K.; Kiis, A. Dynamics of Nitrate and Nitrite Content During Storage of Home-Made and Small-Scale Industrially Produced Raw Vegetable Juices and Their Dietary Intake. Food Addit. Contam. Part A Chem. Anal. Control Expo. Risk Assess. 2010, 27, 487–495.
- Baião, D.S.; da Silva, D.V.T.; Paschoalin, V.M.F. Beetroot, a Remarkable Vegetable: Its Nitrate and Phytochemical Contents Can Be Adjusted in Novel Formulations to Benefit Health and Support Cardiovascular Disease Therapies. Antioxidants 2020, 9, 960.
- Spiegelhalder, B.; Eisenbrand, G.; Preussman, R. Influence of Dietary Nitrate on Nitrite Content of Human Saliva: Possible Relevance to In-Vivo Formation of N-Nitroso Compounds. Food Cosmet. Toxicol. 1976, 14, 545–548.
- Tannenbaum, S.R.; Weisman, M.; Fett, D. The Effect of Nitrate Intake on Nitrite Formation in Human Saliva. Food Cosmet. Toxicol. 1976, 14, 549–552.
- Powlson, D.S.; Addiscott, T.M.; Benjamin, N.; Cassman, K.G.; de Kok, T.M.; van Grinsven, H.; L’Hirondel, J.L.; Avery, A.A.; van Kessel, C. When Does Nitrate Become a Risk For Humans? J. Environ. Qual. 2008, 37, 291–295.
- Food and Agriculture Organization of the United Nations and World Health Organization (FAO/WHO). Evaluation of Certain Food Additives and Contaminants; WHO: Geneva, Switzerland, 1995; Available online: https://apps.who.int/iris/bitstream/handle/10665/42849/WHO_TRS_922.pdf;sequence=1 (accessed on 30 January 2023).
- European Food Safety Authority. Opinion of the Scientific Panel on Contaminants in the Food Chain on a Request from the European Commission to Perform a Scientific Risk Assessment on Nitrate in Vegetables. EFSA J. 2008, 6, 689. Available online: https://www.efsa.europa.eu/en/efsajournal/pub/689 (accessed on 30 January 2023).
- Katan, M.B. Nitrate in Foods: Harmful or Healthy? Am. J. Clin. Nutr. 2009, 90, 11–12.
- Dejam, A.; Hunter, C.J.; Tremonti, C.; Pluta, R.M.; Hon, Y.Y.; Grimes, G.; Partovi, K.; Pelletier, M.M.; Oldfield, E.H.; Cannon, R.O., III; et al. Nitrite Infusion in Humans and Nonhuman Primates: Endocrine Effects, Pharmacokinetics, and Tolerance Formation. Circulation 2007, 116, 1821–1831.
- Hord, N.G.; Tang, Y.; Bryan, N.S. Food Sources of Nitrates and Nitrites: The Physiologic Context for Potential Health Benefits. Am. J. Clin. Nutr. 2009, 90, 1–10.
- Chazelas, E.; Pierre, F.; Druesne-Pecollo, N.; Esseddik, Y.; Szabo de Edelenyi, F.; Agaesse, C.; De Sa, A.; Lutchia, R.; Gigandet, S.; Srour, B.; et al. Nitrites and Nitrates from Food Additives and Natural Sources and Cancer Risk: Results from the Nutrinet-Santé Cohort. Int. J. Epidemiol. 2022, 51, 1106–1119.
- Van Velzen, A.G.; Sips, A.J.; Schothorst, R.C.; Lambers, A.C.; Meulenbelt, J. The Oral Bioavailability of Nitrate from Nitrate-Rich Vegetables in Humans. Toxicol. Lett. 2008, 181, 177–181.
- Gilchrist, M.; Winyard, P.G.; Aizawa, K.; Anning, C.; Shore, A.; Benjamin, N. Effect of Dietary Nitrate on Blood Pressure, Endothelial Function, and Insulin Sensitivity in Type 2 Diabetes. Free Radic. Biol. Med. 2013, 60, 89–97.
- Bondonno, C.P.; Liu, A.H.; Croft, K.D.; Ward, N.C.; Yang, X.; Considine, M.J.; Puddey, I.B.; Woodman, R.J.; Hodgson, J.M. Short-Term Effects of Nitrate-Rich Green Leafy Vegetables on Blood Pressure and Arterial Stiffness in Individuals with High-Normal Blood Pressure. Free Radic. Biol. Med. 2014, 77, 353–362.
- Bondonno, C.P.; Liu, A.H.; Croft, K.D.; Ward, N.C.; Puddey, I.B.; Woodman, R.J.; Hodgson, J.M. Short-Term Effects of a High Nitrate Diet on Nitrate Metabolism in Healthy Individuals. Nutrients 2015, 7, 1906–1915.
- Kapil, V.; Khambata, R.S.; Robertson, A.; Caulfield, M.J.; Ahluwalia, A. Dietary Nitrate Provides Sustained Blood Pressure Lowering in Hypertensive Patients: A Randomized, Phase 2, Double-Blind, Placebo Controlled Study. Hypertension 2015, 65, 320–327.
- Rammos, C.; Hendgen-Cotta, U.B.; Sobierajski, J.; Bernard, A.; Kelm, M.; Rassaf, T. Dietary Nitrate Reverses Vascular Dysfunction in Older Adults with Moderately Increased Cardiovascular Risk. J. Am. Coll. Cardiol 2014, 63, 1584–1585.
- Bahadoran, Z.; Mirmiran, P.; Kabir, A.; Azizi, F.; Ghasemi, A. The Nitrate-Independent Blood Pressure-Lowering Effect of Beetroot Juice: A Systematic Review and Meta-Analysis. Hypertension 2015, 65, 320–327.
- Lara, J.; Ashor, A.W.; Oggioni, C.; Ahluwalia, A.; Mathers, J.C.; Siervo, M. Effects of Inorganic Nitrate and Beetroot Supplementation on Endothelial Function: A Systematic Review and Meta-Analysis. Eur. J. Nutr. 2016, 55, 451–459.
- Wijnands, K.A.; Meesters, D.M.; van Barneveld, K.W.; Visschers, R.G.; Briedé, J.J.; Vandendriessche, B.; Van Eijk, H.M.; Bessems, B.A.; van den Hoven, N.; Von Wintersdorff, C.J.; et al. Citrulline Supplementation Improves Organ Perfusion and Arginine Availability Under Conditions with Enhanced Arginase Activity. Nutrients 2015, 7, 5217–5238.
- Alderton, W.K.; Cooper, C.E.; Knowles, R.G. Nitric Oxide Synthases: Structure, Function and Inhibition. Biochem. J. 2001, 357, 593–615.
- Ataabadi, A.E.; Golshiri, K.; Jüttner, A.; Krenning, G.; Danser, A.H.J.; Roks, A.J. Nitric Oxide-cGMP Signaling in Hypertension: Current and Future Options for Pharmacotherapy. Hypertension 2020, 76, 1055–1068.
- Blatter, L.A.; Wier, W.G. Nitric Oxide Decreases in Vascular Smooth Muscle by Inhibition of the Calcium Current. Cell Calcium 1994, 15, 122–131.
- Vtolix, M.L.; Raeymaeken, F.; Wuytack, F.; Hofmann, F.; Casteels, R. Cyclic GMP-dependent protein kinase stimulates the plasmalemmal Ca2+ pump of smooth muscle via phosphorylation of phosphatidylinositol. Biochem. J. 1988, 255, 855–863.
- Münzel, T.; Daiber, A.; Ullrich, V.; Mülsch, A. Vascular consequences of endothelial nitric oxide synthase uncoupling for the activity and expression of the soluble guanylyl cyclase and the cGMP-dependent protein kinase. Arterioscler Thromb Vasc Biol. 2005, 25, 1551–1557.
- King, D.E.; Mainous, A.G., 3rd; Geesey, M.E. Variation in L-Arginine Intake Follow Demographics and Lifestyle Factors That May Impact Cardiovascular Disease Risk. Nutr. Res. 2008, 28, 21–24.
- Siasos, G.; Tousoulis, D.; Vlachopoulos, C.; Antoniades, C.; Stefanadi, E.; Ioakeimidis, N.; Andreou, I.; Zisimos, K.; Papavassiliou, A.G.; Stefanadis, C. Short-Term Treatment with L-Arginine Prevents the Smoking-Induced Impairment of Endothelial Function and Vascular Elastic Properties in Young Individuals. Int. J. Cardiol. 2008, 126, 394–399.
- Siasos, G.; Tousoulis, D.; Vlachopoulos, C.; Antoniades, C.; Stefanadi, E.; Ioakeimidis, N.; Zisimos, K.; Siasou, Z.; Papavassiliou, A.G.; Stefanadis, C. The impact of oral L-arginine supplementation on acute smoking-induced endothelial injury and arterial performance. Am. J. Hypertens. 2009, 22, 586–592.
- Adams, M.R.; McCredie, R.; Jessup, W.; Robinson, J.; Sullivan, D.; Celermajer, D.S. Oral L-Arginine Improves Endothelium-Dependent Dilatation and Reduces Monocyte Adhesion to Endothelial Cells in Young Men with Coronary Artery Disease. Atherosclerosis 1997, 129, 261–269.
- Yin, W.H.; Chen, J.W.; Tsai, C.; Chiang, M.C.; Young, M.S.; Lin, S.J. L-Arginine Improves Endothelial Function and Reduces LDL Oxidation in Patients with Stable Coronary Artery Disease. Clin. Nutr. 2005, 24, 988–997.
- Lucotti, P.; Monti, L.; Setola, E.; La Canna, G.; Castiglioni, A.; Rossodivita, A.; Pala, M.G.; Formica, F.; Paolini, G.; Catapano, A.L.; et al. Oral L-Arginine Supplementation Improves Endothelial Function and Ameliorates Insulin Sensitivity and Inflammation in Cardiopathic Nondiabetic Patients after an Aortocoronary Bypass. Metabolism 2009, 58, 1270–1276.
- Schächinger, V.; Britten, M.B.; Zeiher, A.M. Prognostic Impact of Coronary Vasodilator Dysfunction on Adverse Long-Term Outcome of Coronary Heart Disease. Circulation 2000, 101, 1899–1906.
- Osibogun, O.; Ogunmoroti, O.; Michos, E.D. Polycystic Ovary Syndrome and Cardiometabolic Risk: Opportunities for Cardiovascular Disease Prevention. Trends Cardiovasc. Med. 2020, 30, 399–404.
- Battaglia, C.; Mancini, F.; Battaglia, B.; Facchinetti, F.; Artini, P.G.; Venturoli, S. L-Arginine Plus Drospirenone-Ethinyl Estradiol in the Treatment of Patients with PCOS: A Prospective, Placebo Controlled, Randomized, Pilot Study. Gynecol. Endocrinol. 2010, 26, 861–868.
- Orea-Tejeda, A.; Orozco-Gutiérrez, J.J.; Castillo-Martínez, L.; Keirns-Davies, C.; Montano-Hernández, P.; Vázquez-Díaz, O.; Valdespino-Trejo, A.; Infante, O.; Martínez-Memije, R. The Effect of L-Arginine and Citrulline on Endothelial Function in Patients in Heart Failure with Preserved Ejection Fraction. Cardiol. J. 2010, 17, 464–470.
- Hamburg, N.M.; Keyes, M.J.; Larson, M.G.; Vasan, R.S.; Schnabel, R.; Pryde, M.M.; Mitchell, G.F.; Sheffy, J.; Vita, J.A.; Benjamin, E.J. Cross-sectional relations of digital vascular function to cardiovascular risk factors in the Framingham Heart Study. Circulation 2008, 117, 2467–2474.
- Jankowski, J.; Floege, J.; Fliser, D.; Böhm, M.; Marx, N. Cardiovascular Disease in Chronic Kidney Disease: Pathophysiological Insights and Therapeutic Options. Circulation 2021, 143, 1157–1172.
- Annavarajula, S.K.; Dakshinamurty, K.V.; Naidu, M.U.; Reddy, C.P. The Effect of L-Arginine on Arterial Stiffness and Oxidative Stress in Chronic Kidney Disease. Indian J. Nephrol. 2012, 22, 340–346.
- Gaenzer, H.; Sturm, W.; Neumayr, G.; Kirchmair, R.; Ebenbichler, C.; Ritsch, A.; Föger, B.; Weiss, G.; Patsch, J.R. Pronounced postprandial lipemia impairs endothelium-dependent dilation of the brachial artery in men. Cardiovasc. Res. 2001, 52, 509–516.
- Ceriello, A.; Taboga, C.; Tonutti, L.; Quagliaro, L.; Piconi, L.; Bais, B.; Da Ros, R.; Motz, E. Evidence for an Independent and Cumulative Effect of Postprandial Hypertriglyceridemia and Hyperglycemia on Endothelial Dysfunction and Oxidative Stress Generation—Effects of Short- and Long-Term Simvastatin Treatment. Circulation 2002, 106, 1211–1218.
- Fewkes, J.J.; Kellow, N.J.; Cowan, S.F.; Williamson, G.; Dordevic, A.L. A single, high-fat meal adversely affects postprandial endothelial function: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2022, 116, 699–729.
- Deveaux, A.; Pham, I.; West, S.G.; André, E.; Lantoine-Adam, F.; Bunouf, P.; Sadi, S.; Hermier, D.; Mathé, V.; Fouillet, H.; et al. L-Arginine Supplementation Alleviates Postprandial Endothelial Dysfunction When Baseline Fasting Plasma Arginine Concentration is Low: A Randomized Controlled Trial in Healthy Overweight Adults with Cardiometabolic Risk Factors. J. Nutr. 2016, 146, 1330–1340.
- Lin, C.C.; Tsai, W.C.; Chen, J.Y.; Li, Y.H.; Lin, L.J.; Chen, J.H. Supplements of L-arginine attenuate the effects of high-fat meal on endothelial function and oxidative stress. Int. J. Cardiol. 2008, 127, 337–341.
- Romero, M.J.; Platt, D.H.; Caldwell, R.B.; Caldwell, R.W. Therapeutic Use of Citrulline in Cardiovascular Disease. Cardiovasc. Drug Rev. 2006, 24, 275–290.
- Aguayo, E.; Martínez-Sánchez, A.; Fernández-Lobato, B.; Alacid, F. L-Citrulline: A Non-Essential Amino Acid with Important Roles in Human Health. Appl. Sci. 2021, 11, 3293.
- Orozco-Gutiérrez, J.J.; Castillo-Martínez, L.; Orea-Tejeda, A.; Vázquez-Díaz, O.; Valdespino-Trejo, A.; Narváez-David, R.; Keirns-Davis, C.; Carrasco-Ortiz, O.; Navarro-Navarro, A.; Sánchez-Santillán, R. Effect of L-arginine or L-Citrulline Oral Supplementation on Blood Pressure and Right Ventricular Function in Heart Failure Patients with Preserved Ejection Fraction. Cardiol. J. 2010, 17, 612–618.
- Figueroa, A.; Sanchez-Gonzalez, M.A.; Perkins-Veazie, P.M.; Arjmandi, B.H. Effects of Watermelon Supplementation on Aortic Blood Pressure and Wave Reflection in Individuals with Prehypertension: A Pilot Study. Am. J. Hypertens. 2011, 24, 40–44.
- Akashi, K.; Mifune, Y.; Morita, K.; Ishitsuka, S.; Tsujimoto, H.; Ishihara, T. Spatial Accumulation Pattern of Citrulline and Other Nutrients in Immature and Mature Watermelon Fruits. J. Sci. Food Agric. 2017, 97, 479–487.
- Tarazona-Díaz, M.P.; Viegas, J.; Moldao-Martins, M.; Aguayo, E. Bioactive Compounds from Flesh and By-Product of Fresh-Cut Watermelon Cultivars. J. Sci. Food Agric. 2011, 91, 805–812.
- Bailey, S.J.; Blackwell, J.R.; Williams, E.; Vanhatalo, A.; Wylie, L.J.; Winyard, P.G.; Jones, A.M. Two Weeks of Watermelon Juice Supplementation Improves Nitric Oxide Bioavailability but Not Endurance Exercise Performance in Humans. Nitric Oxide-Biol. Chem. 2016, 59, 10–20.
- Figueroa, A.; Wong, A.; Jaime, S.J.; Gonzales, J.U. Influence of L-Citrulline and Watermelon Supplementation on Vascular Function and Exercise Performance. Curr. Opin. Clin. Nutr. Metab. 2017, 20, 92–98.
- Bahri, S.; Zerrouk, N.; Aussel, C.; Moinard, C.; Crenn, P.; Curis, E.; Chaumeil, J.C.; Cynober, L.; Sfar, S. Citrulline: From Metabolism to Therapeutic Use. Nutrition 2013, 29, 479–484.
- Fan, J.; Park, E.; Zhang, L.; Edirisinghe, I.; Burton-Freeman, B.M.; Sandhu, A.K. Pharmacokinetic Parameters of Watermelon (Rind, Flesh and Seeds) Bioactive Components in Human Plasma: A Pilot Study to Investigate the Relationship to Endothelial Function. J. Agric. Food Chem. 2020, 68, 7393–7403.
- Volino-Souza, M.; de Oliveira, G.V.; Conte-Junior, C.A.; Figueroa, A.; Alvares, S.T. Current Evidence of Watermelon (Citrullus lanatus) Ingestion on Vascular Health: A Food Science and Technology Perspective. Nutrients 2022, 14, 2913.
- Vincellette, C.M.; Losso, J.; Early, K.; Spielmann, G.; Irving, B.A.; Allerton, T.D. Supplemental Watermelon Juice Attenuates Acute Hyperglycemia-Induced Macro-and Microvascular Dysfunction in Healthy Adults. J. Nutr. 2021, 151, 3450–3458.
- Ellis, A.C.; Mehta, T.; Nagabooshanam, V.A.; Dudenbostel, T.; Locher, J.L.; Crowe-White, K.M. Daily 100% Watermelon Juice Consumption and Vascular Function among Postmenopausal Women: A Randomized Controlled Trial. Nutr. Metab. Cardiovasc. Dis. NMCD 2021, 31, 2959–2968.
- Figueroa, A.; Wong, A.; Hooshmand, S.; Sanchez-Gonzalez, M.A. Effects Of Watermelon Supplementation on Arterial Stiffness and Wave Reflection Amplitude in Postmenopausal Women. Menopause 2013, 20, 573–577.
- Figueroa, A.; Sanchez-Gonzalez, M.A.; Wong, A.; Arjmandi, B.H. Watermelon Extract Supplementation Reduces Ankle Blood Pressure and Carotid Augmentation Index in Obese Adults with Prehypertension or Hypertension. Am. J. Hypertens. 2012, 25, 640–643.
- Kim, I.Y.; Schutzler, S.E.; Schrader, A.; Spencer, H.J.; Azhar, G.; Deutz, N.E.; Wolfe, R.R. Acute Ingestion of Citrulline Stimulates Nitric Oxide Synthesis but Does Not Increase Blood Flow in Healthy Young and Older Adults with Heart Failure. Am. J. Physiol. Endocrinol. Metab. 2015, 309, E915–E924.
More
Information
Subjects:
Cardiac & Cardiovascular Systems
Contributors
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
1.7K
Entry Collection:
Hypertension and Cardiovascular Diseases
Revisions:
2 times
(View History)
Update Date:
07 Jun 2023
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





