Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Alexandru Achim | -- | 1604 | 2022-08-22 09:56:43 | | | |
| 2 | Jessie Wu | Meta information modification | 1604 | 2022-08-23 05:04:59 | | | | |
| 3 | Jessie Wu | Meta information modification | 1604 | 2022-08-23 07:51:15 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Achim, A.; Stanek, A.; Homorodean, C.; Spinu, M.; Onea, H.L.; Lazăr, L.; Marc, M.; Ruzsa, Z.; Olinic, D.M. Management of Peripheral Artery Disease in Diabetes. Encyclopedia. Available online: https://encyclopedia.pub/entry/26348 (accessed on 10 May 2026).
Achim A, Stanek A, Homorodean C, Spinu M, Onea HL, Lazăr L, et al. Management of Peripheral Artery Disease in Diabetes. Encyclopedia. Available at: https://encyclopedia.pub/entry/26348. Accessed May 10, 2026.
Achim, Alexandru, Agata Stanek, Călin Homorodean, Mihail Spinu, Horea Laurenţiu Onea, Leontin Lazăr, Mădălin Marc, Zoltán Ruzsa, Dan Mircea Olinic. "Management of Peripheral Artery Disease in Diabetes" Encyclopedia, https://encyclopedia.pub/entry/26348 (accessed May 10, 2026).
Achim, A., Stanek, A., Homorodean, C., Spinu, M., Onea, H.L., Lazăr, L., Marc, M., Ruzsa, Z., & Olinic, D.M. (2022, August 22). Management of Peripheral Artery Disease in Diabetes. In Encyclopedia. https://encyclopedia.pub/entry/26348
Achim, Alexandru, et al. "Management of Peripheral Artery Disease in Diabetes." Encyclopedia. Web. 22 August, 2022.
Copy Citation
Peripheral artery disease (PAD) increases the risk of diabetes, while diabetes increases the risk of PAD, and certain symptoms in each disease increase the risk of contracting the other. The phenotypic manifestations of atherosclerosis vary in each individual and throughout the body; it is not fully understood why plaque formation has such a heterogeneous distribution, although different arterial systems are correlated. Moreover, risk factors (such as diabetes mellitus, hypertension, smoking, etc.) undoubtedly aggravate atherogenesis and cardiovascular mortality through a dual risk: firstly, the intrinsic risk of the underlying disease; secondly, it increases the risk of atherosclerosis in various target organs.
guidelines
PAD
antiplatelet therapy
1. Introduction
The phenotypic manifestations of atherosclerosis vary in each individual and throughout the body; it is not fully understood why plaque formation has such a heterogeneous distribution, although different arterial systems are correlated [1][2][3]. Moreover, risk factors (such as diabetes mellitus, hypertension, smoking, etc.) undoubtedly aggravate atherogenesis and cardiovascular mortality through a dual risk: firstly, the intrinsic risk of the underlying disease; secondly, it increases the risk of atherosclerosis in various target organs. In other words, the co-prevalence of two atherogenic conditions is not simply an association due to shared risk factors; one may in fact play a fundamental role in the pathophysiology of the other and vice versa. Researchers know that there is a bidirectional relationship between the risk of cardiovascular disease and systemic diseases, such as diabetes mellitus or primary hypertension. Thus, the complex relationship between atherogenesis and risk factors intersects at several levels, and perhaps the severity of the patient’s clinical manifestations best demonstrates this harmful interplay [4][5].
An evocative example would be peripheral artery disease (PAD), which is a direct macrovascular disorder of diabetes mellitus (DM). PAD raises the risk of DM, and DM raises the risk of PAD. Each 1% increase in hemoglobin A1c (HbA1c) is associated with a nearly 30% increase in the risk of developing PAD during the follow-up period. PAD also manifests earlier in diabetics and progresses more rapidly to critical limb ischemia. In addition, a diabetic patient with PAD has a 14.2% increased risk of major cardiovascular events when HbA1c increases by 1% [6][7]. This deleterious interaction is self-evident, although the relationship between diabetes and vasculopathy has not been fully elucidated, despite considerable research efforts in molecular, animal, and translational models. Currently, the consequences of peripheral ischemia are thought to result from the interaction between hemodynamic, neurohumoral, and metabolic factors, leading to endothelial dysfunction. However, numerous fundamental questions remain unanswered. For instance, the phenomenon of the regression of microvascular disease following strict glycemic control is not observed in the larger vessels [5]. This situation highlights the need for an aggressive multidisciplinary approach to limb salvage in the diabetic population.
2. Management: Differences between Guidelines
The treatment of PAD in patients with DM has two main goals: to improve peripheral blood flow in symptomatic patients and to treat vascular risk factors and concomitant disorders, with an emphasis on coronary and cerebrovascular vascular diseases. Exercise training, such as structured walking, should be prescribed, while weight control must be advocated for overweight diabetics. A step-by-step schematic approach is shown in Figure 1.
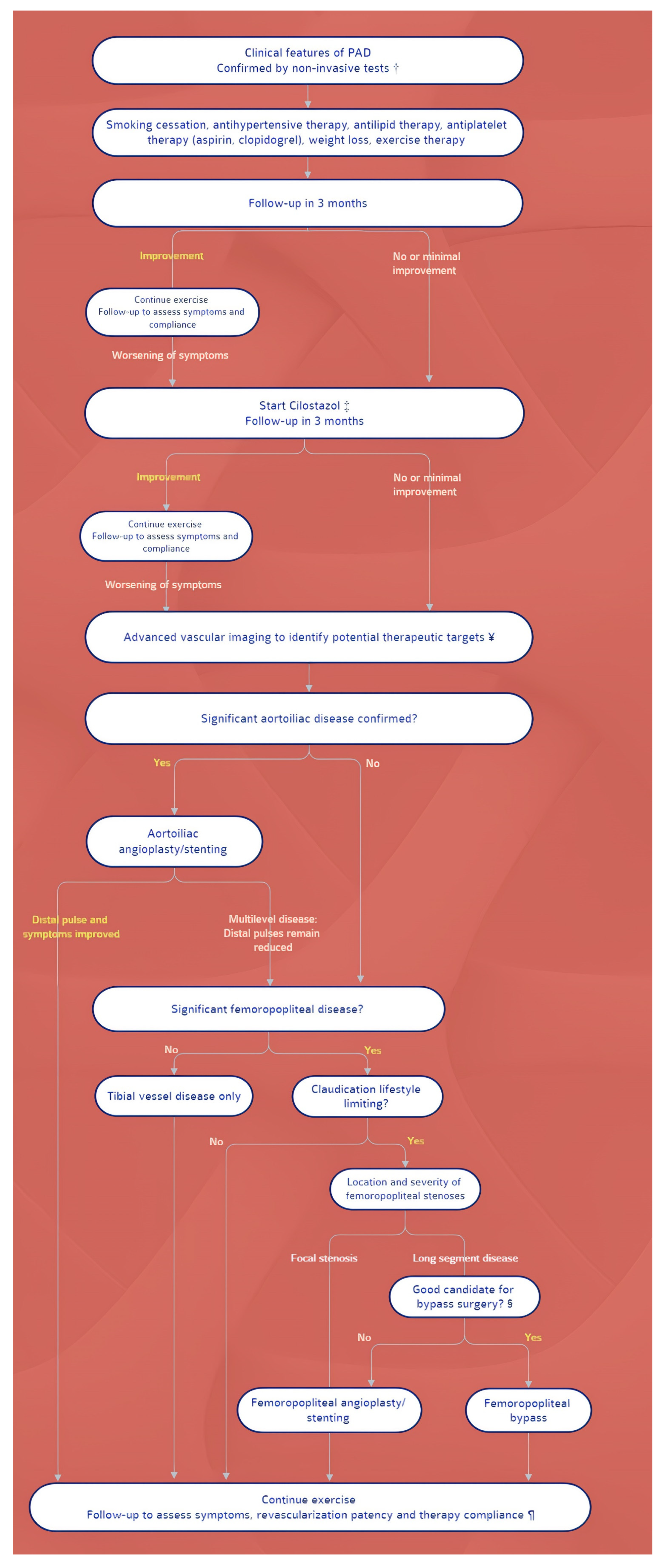
Figure 1. Algorithm for the management of PAD. Symbols: † Noninvasive studies include ankle-brachial pressure index, pulse volume recordings, partitioned pressures, and exercise testing. ‡ Cilostazol is recommended for patients with moderate-to-severe claudication. For patients with contraindications or for patients who do not tolerate cilostazol, pentoxifylline is an alternative. These can be prescribed simultaneously with the launching of an exercise program. ¥ CT or MR angiography. For patients with inflow occlusive disease (weak femoral pulse), conventional catheter-based arteriography may be performed initially, in expectation of possible intervention. § Optimal candidates for peripheral bypass surgery have favorable anatomy for bypass (target vessel, good runoff, and, ideally, vein conduit), are medically fit, and have an anticipated life expectancy that will allow the patient to benefit from the procedure. ¶ Following revascularization, antiplatelet therapy depends upon the nature of revascularization (i.e., the type of stent, type of bypass conduit); if initiated, cilostazol may be stopped.
The American College of Cardiology/American Heart Association (ACC/AHA) 2016 guidelines [8] and the European Society of Cardiology/European Society for Vascular Surgery (ESC/ESVS) 2017 guidelines [9] strongly recommend smoking cessation, glycemic control, blood pressure control, and statin therapy. The European guidelines also recommend therapeutic targets: low-density lipoprotein (LDL) levels of less than 70 mg/dL or a >50% reduction from baseline value, with blood pressure < 140/90 mmHg. Both guidelines also suggest the use of inhibitors of the renin-angiotensin system to decrease ischemic events [8][9]. Metformin is the oral antidiabetic drug of choice in concomitant DM and PAD. An SGLT-2 inhibitor or GLP-1 agonist may also be used. More prudent SGLT-2 inhibitors are empagliflozin and dapagliflozin, as canagliflozin may increase the risk of amputation and should, therefore, be avoided. The use of basal insulin analogs is considered safe [10].
Both U.S. and European guidelines promote single antiplatelet therapy, either aspirin or clopidogrel, in symptomatic individuals. The U.S. guidelines recommend aspirin or clopidogrel to reduce coronary events [8], whereas the European guidelines do not support antiplatelet agents in asymptomatic cases unless other indications, such as coronary artery disease, are present [9]. Clopidogrel may be preferred to aspirin, according to the European guidelines, whereas the American guidelines refrain from making this statement. Dual antiplatelet therapy (DAPT) with aspirin and clopidogrel is only recommended for 1 month after percutaneous and surgical revascularization, according to the ESC guidelines (Class I) [9]. At the same time, the ACC guidelines give a Class-IIb recommendation for long-term dual antiplatelet inhibition [8]. The ACC guidelines also give anticoagulant therapy a Level-III harm recommendation and state that pentoxifylline is not effective for the treatment of claudication (also in Class III) [11]. Of note, the American guidelines promote the use of cilostazol (Class I, level of evidence A), whereas the European guidelines do not mention this drug. There is a strong emphasis on home-based training, either supervised or unsupervised (a Class-I recommendation in both guidelines).
Both guidelines have opted for a Class IIa-level recommendation for revascularization in patients with intermittent severe claudication. These procedures are recommended only when guideline-directed therapy and structured exercise programs fail. Although exercise therapy is crucial, its use is limited in frail patients or patients with ulcers or gangrene. The association between PAD and frailty syndrome in patients living with DM has recently been described [12]. Regarding endovascular approaches, both groups agree that revascularization should be performed in patients with hemodynamically significant upper inflow (aortoiliac) disease and lifestyle-limiting pain. For femoropopliteal disease (outflow vessels), the ACC guidelines advocate an endovascular approach, whereas the European guidelines favor such an approach only for femoropopliteal occlusions that are greater than 25 cm in length. However, both the ACC and ESC consent to surgical bypass for patients who are considered suitable for surgery. In Europe, the emphasis is on revascularization and contemporary therapies, whereas the American experts underline post-procedural surveillance and wound care [8][9]. The importance of surgical advice and consultation is, therefore, self-evident; an ideal multidisciplinary team for a diabetic patient with PAD would include an angiologist, a cardiologist, an interventionist, a vascular surgeon, a radiologist, and a diabetologist. The upcoming guidelines should emphasize this holistic approach, while the inclusion of a noninvasive protocol for assessment before and after revascularization would leverage the contribution of vascular imaging.
In cases of critical limb ischemia, both advisory bodies advocate revascularization. They also agree that endovascular and surgical revascularization procedures achieve similar outcomes. Controlling glycemia is a critical factor in reducing limb loss, foot wounds, and infection [8][9]. The relevance of DM is that both guidelines mention this practice and put forward the idea of educating these patients on self-foot examination and healthy foot behaviors.
Regarding acute limb ischemia (ALI), both guidelines support rapid emergency assessment and the initiation of heparin. If the limb is salvageable, the two groups again diverge: the American guidelines favor catheter-based thrombolysis (Class I) over percutaneous mechanical thrombectomy (Class IIa), surgical thromboembolectomy (Class IIa), and ultrasound-accelerated catheter-based thrombolysis (IIb) based on small studies, whereas the European guidelines do not recognize the superiority of thrombolysis over open surgical procedures [8][9]. Systemic thrombolysis has no role in ALI [13]. Catheter-based thrombolysis has a satisfactory clinical outcome, with a rate of 75–92% of complete or partial thrombus resolution, but patients with symptoms of longer duration (> 14 days) have better outcomes after surgery [13]. If blood flow is successfully restored after 24 h of continuous thrombolysis, angiography should be performed to identify preexisting arterial lesions that can be managed by endovascular (e.g., stenting) or surgical techniques (e.g., bypass).
Finally, it should be noted that at the time of publication of these guidelines, the results of the COMPASS [14] and VOYAGER PAD [15] trials were not published. Both studies have shown benefits in terms of cardiovascular events, including adverse limb events, compared with patients taking aspirin alone. The results of these studies, together with the introduction of SGLT2 inhibitors on a large scale, will bring new horizons and perhaps a dedicated section in future guidelines that will address the needs of this high-risk category of patients. Hypoglycemic drugs remain paramount but not sufficient; for example, a recent study showed that the drugs commonly used for the treatment of diabetes were inefficient at preventing the thickening of the basement membrane that is induced by the diabetogenic medium. Contrastingly, DAPT, a γ-secretase inhibitor that blocks the NOTCH pathway, stopped the thickening of the basement membrane in the organoids in vitro and in the diabetic mouse [16]. The mechanisms underlying diabetic vasculopathy are still not fully understood, which limits therapeutic drug development. As a matter of course, all cardiovascular disease risk factors associated with DM should be addressed: hypertension (BP < 130/80 mmHg), hyperlipidemia (LDL < 55 mg/dL), weight loss, physical activity, nutritional intake, smoking cessation, etc.
References
- Wong, N.D.; Gransar Shaw, L.; Polk, D.; Moon, J.H.; Miranda-Peats, R.; Hayes, S.W.; Thomson, L.E.; Rozanski, A.; Friedman, J.D.; Berman, D.S. Thoracic aortic calcium versus coronary artery calcium for the prediction of coronary heart disease and cardiovascular disease events. JACC Cardiovasc. Imaging 2009, 2, 319–326.
- Achim, A.; Kákonyi, K.; Nagy, F.; Jambrik, Z.; Varga, A.; Nemes, A.; Chan, J.S.K.; Toth, G.G.; Ruzsa, Z. Radial Artery Calcification in Predicting Coronary Calcification and Atherosclerosis Burden. Cardiol. Res. Pract. 2022, 2022, 5108389.
- Homorodean, C.; Leucuta, D.C.; Ober, M.; Homorodean, R.; Spinu, M.; Olinic, M.; Tataru, D.; Olinic, D.M. Intravascular ultrasound insights into the unstable features of the coronary atherosclerotic plaques: A systematic review and meta-analysis. Eur. J. Clin. Investig. 2022, 52, e13671.
- Achim, A.; Marc, M.; Ruzsa, Z. Surgical Turned-Downed CHIP Cases-Can PCI Save the Day? Front. Cardiovasc. Med. 2022, 9, 872398.
- The Diabetes Control and Complications Trial (DCCT) Research Group. Effect of intensive diabetes management on macrovascular events and risk factors in the Diabetes Control and Complications Trial. Am. J. Cardiol. 1995, 75, 894–903.
- Jones, W.S.; Baumgartner, I.; Hiatt, W.R.; Heizer, G.; Conte, M.S.; White, C.J.; Berger, J.S.; Held, P.; Katona, B.G.; International Steering Committee and Investigators of the EUCLID Trial; et al. Ticagrelor Compared with Clopidogrel in Patients with Prior Lower Extremity Revascularization for Peripheral Artery Disease. Circulation 2017, 135, 241–250.
- Low Wang, C.C.; Blomster, J.I.; Heizer, G.; Berger, J.S.; Baumgartner, I.; Fowkes, F.G.R.; Held, P.; Katona, B.G.; Norgren, L.; EUCLID Trial Executive Committee and Investigators; et al. Cardiovascular and Limb Outcomes in Patients with Diabetes and Peripheral Artery Disease: The EUCLID Trial. J. Am. Coll. Cardiol. 2018, 72, 3274–3284.
- Gerhard-Herman, M.D.; Gornik, H.L.; Barrett, C.; Barshes, N.R.; Corriere, M.A.; Drachman, D.E.; Fleisher, L.A.; Fowkes, F.G.R.; Hamburg, N.M.; Kinlay, S.; et al. 2016 AHA/ACC Guideline on the Management of Patients with Lower Extremity Peripheral Artery Disease: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation 2017, 135, e686–e725.
- Aboyans, V.; Ricco, J.B.; Bartelink, M.E.L.; Björck, M.; Brodmann, M.; Cohnert, T.; Collet, J.-P.; Czerny, M.; De Carlo, M.; ESC Scientific Document Group; et al. 2017 ESC Guidelines on the Diagnosis and Treatment of Peripheral Arterial Diseases, in collaboration with the European Society for Vascular Surgery (ESVS): Document covering atherosclerotic disease of extracranial carotid and vertebral, mesenteric, renal, upper and lower extremity arteriesEndorsed by: The European Stroke Organization (ESO)The Task Force for the Diagnosis and Treatment of Peripheral Arterial Diseases of the European Society of Cardiology (ESC) and of the European Society for Vascular Surgery (ESVS). Eur. Heart J. 2018, 39, 763–816.
- Balletshofer, B.; Ito, W.; Lawall, H.; Malyar, N.; Oberländer, Y.; Reimer, P.; Rittig, K.; Zähringer, M. Position Paper on the Diagnosis and Treatment of Peripheral Arterial Disease (PAD) in People with Diabetes Mellitus. Exp. Clin. Endocrinol. Diabetes 2019, 127 (Suppl. 1), S105–S113.
- Törngren, K.; Eriksson, S.; Arvidsson, J.; Falkenberg, M.; Johnsson, Å.A.; Sjöberg, C.; Lagerstrand, K.; Nordanstig, J. A Reperfusion BOLD-MRI Tissue Perfusion Protocol Reliably Differentiate Patients with Peripheral Arterial Occlusive Disease from Healthy Controls. J. Clin. Med. 2021, 10, 3643.
- Jakubiak, G.K.; Pawlas, N.; Cieślar, G.; Stanek, A. Chronic Lower Extremity Ischemia and Its Association with the Frailty Syndrome in Patients with Diabetes. Int. J. Environ. Res. Public Health 2020, 17, 9339.
- Olinic, D.M.; Stanek, A.; Tătaru, D.A.; Homorodean, C.; Olinic, M. Acute Limb Ischemia: An Update on Diagnosis and Management. J. Clin. Med. 2019, 8, 1215.
- Eikelboom, J.W.; Connolly, S.J.; Bosch, J.; Dagenais, G.R.; Hart, R.G.; Shestakovska, O.; Diaz, R.; Alings, M.; Lonn, E.M.; COMPASS Investigators; et al. Rivaroxaban with or without Aspirin in Stable Cardiovascular Disease. N. Engl. J. Med. 2017, 377, 1319–1330.
- Bonaca, M.P.; Bauersachs, R.M.; Anand, S.S.; Debus, E.S.; Nehler, M.R.; Patel, M.R.; Fanelli, F.; Capell, W.H.; Diao, L.; Jaeger, N.; et al. Rivaroxaban in Peripheral Artery Disease after Revascularization. N. Engl. J. Med. 2020, 382, 1994–2004.
- Wimmer, R.A.; Leopoldi, A.; Aichinger, M.; Wick, N.; Hantusch, B.; Novatchkova, M.; Taubenschmid, J.; Hämmerle, M.; Esk, C.; Bagley, J.A.; et al. Human blood vessel organoids as a model of diabetic vasculopathy. Nature 2019, 565, 505–510.
More
Information
Subjects:
Peripheral Vascular Disease
Contributors
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
706
Revisions:
3 times
(View History)
Update Date:
23 Aug 2022
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





