Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Alessandra Bearz | -- | 1963 | 2022-06-24 23:13:52 | | | |
| 2 | Conner Chen | -7 word(s) | 1956 | 2022-06-27 04:42:22 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Bearz, A.; Carlo, E.D.; Bertoli, E.; Conte, A.D.; Stanzione, B.; Berto, E.; Revelant, A.; Spina, M. Egfr Mutations in Lung Cancer. Encyclopedia. Available online: https://encyclopedia.pub/entry/24465 (accessed on 21 May 2026).
Bearz A, Carlo ED, Bertoli E, Conte AD, Stanzione B, Berto E, et al. Egfr Mutations in Lung Cancer. Encyclopedia. Available at: https://encyclopedia.pub/entry/24465. Accessed May 21, 2026.
Bearz, Alessandra, Elisa De Carlo, Elisa Bertoli, Alessandro Del Conte, Brigida Stanzione, Eleonora Berto, Alberto Revelant, Michele Spina. "Egfr Mutations in Lung Cancer" Encyclopedia, https://encyclopedia.pub/entry/24465 (accessed May 21, 2026).
Bearz, A., Carlo, E.D., Bertoli, E., Conte, A.D., Stanzione, B., Berto, E., Revelant, A., & Spina, M. (2022, June 24). Egfr Mutations in Lung Cancer. In Encyclopedia. https://encyclopedia.pub/entry/24465
Bearz, Alessandra, et al. "Egfr Mutations in Lung Cancer." Encyclopedia. Web. 24 June, 2022.
Copy Citation
Epidermal growth factor receptor (EGFR) is a transmembrane protein with cytoplasmic kinase activity that transduces important growth factor signals from the extracellular milieu to cells. Given that more than 60% of non-small cell lung cancers (NSCLC) express EGFR, EGFR has emerged as an important therapeutic target for the treatment of these tumors.
NSCLC
oncogenic biomarkers
brain metastases
1. Introduction
Lung cancer is one of the most commonly diagnosed cancers (11.6% of all new tumors) [1]. Despite a decline in the death rate in recent years, lung cancer is still the leading cause of cancer deaths [2]. Non-small-cell lung cancer (NSCLC) accounts for 85% of lung cancers, with 60–70% of patients presenting at either stage III B or stage IV of the disease [3].
Brain metastases (BMs) are a common complication in a wide range of cancers, but they are particularly common among NSCLC patients. Indeed, the incidence rate of BMs at diagnosis is 10–20% and up to 40% during the course of the disease [4][5][6].
In recent times, the lifetime incidence of the central nervous system (CNS) metastases in NSCLC has increased as a result of both improved neuro-imaging techniques by the use of magnetic resonance imaging and furthermore of an increase in patient survival because of better systemic control of extracranial disease.
In patients with metastatic lung cancer, BMs are associated with inferior health-related quality of life (QoL) and poor prognosis (life expectancy ranging between 3 and 13 months) [7].
Historically, CNS has been considered a pharmacological sanctuary because of the physical and chemical characteristics of the blood–brain barrier (BBB), a diffusion barrier essential for CNS function. The continuous tight junctions that join the endothelial cells in the brain capillaries limit the influx of circulating factors from blood to brain [8].
Local treatments have traditionally been the cornerstone of BMs management. Surgical resection (SR), stereotactic radiosurgery (SRS), and whole-brain radiation therapy (WBRT) have been the primary treatment modalities.
Brain irradiation can significantly impair BBB integrity.
WBRT is associated with a significant rate of neurological toxicities, and acute, early-delayed, and late effects. Unlike acute neurological symptoms, which are usually reversible, long-term effects appear several months or years later and are generally irreversible [9][10][11]. Partial brain RT may also have late effects on cognitive function, although the risk is lower than with WBRT. Figure 1
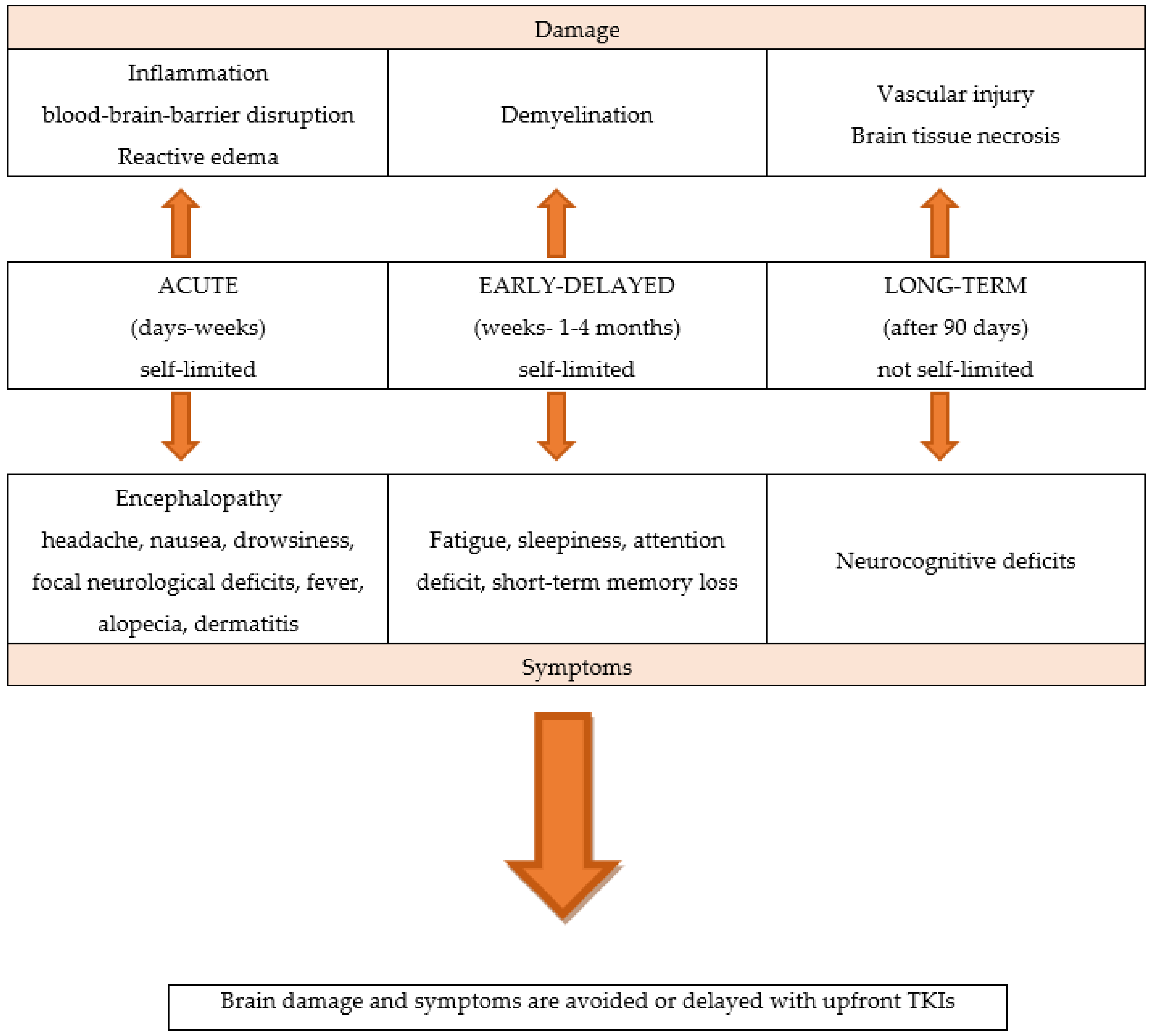
Figure 1. The neurological toxicities of brain radiotherapy.
The selection of local treatment is based on the number of BMs, the size or location of BMs, the symptoms of encephalic disease, and the status of extracranial metastases.
For patients with symptomatic or a limited number of BMs, who have a controlled primary disease or are suitable for radical treatment, local therapy with a neurosurgical resection or with SRS is recommended. Instead, WBRT is considered for pluri-metastatic CNS disease [12].
SR is often the standard of care (SoC) for solitary or symptomatic brain metastasis, and it can provide immediate and effective relief from symptomatic mass effects [13][14]. The combination of the neurosurgical resection of solitary brain metastasis and postoperative RT favored the combination treatment. A phase III randomized control trial compared post-operative SRS to the surgical cavity with WBRT in patients who underwent resection of a single brain metastasis and demonstrated a lower probability of deterioration in cognitive function and no difference in overall survival (OS) [15]; thus, adjuvant SRS to the surgical resection bed should be considered the preferred local therapy.
A systematic review did not show a significant outcome difference between SR and SRS in patients with single brain metastasis [16].
SRS alone has become the SoC for patients with a good performance status, who cannot undergo resection and/or have a limited number of BMs (1–4 BMs) [17].
SRS allows many precisely focused radiation beams, improving healthy tissue preservation and less cognitive decline.
In past decades, WBRT was the most widely used local treatment for the management of patients with multiple BMs. The radiation schedules include a classical dose of 30 gray (Gy) in 10 fractions or a short course of 20 Gy in 5 fractions, showing similar efficacy [18].
In the last few years, the role of WBRT is declining because of the potential cognitive deficits and the limited clinical benefit compared with best supportive care [19][20].
Therefore, because of its high risk of cognitive function deterioration and unproven survival benefit, the WBRT could be an upfront treatment option for patients with symptomatic BMs; alternatively, a wait-and-see approach could be adopted.
Cytotoxic chemotherapy (CT) plays a limited role in controlling BMs because of the drugs’ inability to cross the BBB and penetrate the CNS [21].
Platinum-based regimens have been the most commonly used therapy for metastatic NSCLC. These CT regimens demonstrated low systemic response rate (RR) in a few brain RT-naïve patients [22].
Thus, upfront CT could represent the better option then WBRT in NSCLC patients with multiple asymptomatic BMs, who are not eligible for SRS. Therefore, WBRT could be reserved for symptomatic patients with good performance status or for intracranial non-responders.
In recent years, both single-agent immune checkpoint inhibitors (ICIs) and a combination of CT plus ICIs have shown better efficacy than platinum-based regimens in NSCLC patients, who do not harbor a driver oncogene alteration in randomized phase III clinical trials. A future critical challenge is knowing how to identify NSCLC patients with CNS disease who benefit from ICIs and the potential of combining radiation with ICIs.
Recently, routine molecular testing has become the SoC for determining the optimal treatment of newly diagnosed advanced or metastatic NSCLC patients. In particular, a range of predictive and prognostic biomarkers have been identified in adenocarcinoma: epidermal growth factor receptor (EGFR) mutations, anaplastic lymphoma kinase (ALK) rearrangements, c-ros oncogene 1 (ROS1) rearrangements, v-Raf murine sarcoma viral oncogene homolog B1 (BRAF) mutations, Kirsten rat sarcoma viral oncogene homologue (KRAS) mutations, neurotrophic receptor tyrosine kinase (NTRK) 1/2/3 rearrangements, rearranged during transfection (RET) rearrangements, N-methyl-N′-nitroso-guanidine human osteosarcoma transforming gene (MET) exon14 skipping mutations, and activating human epidermal growth factor receptor 2 (HER2) mutations [23][24][25]. Figure 2
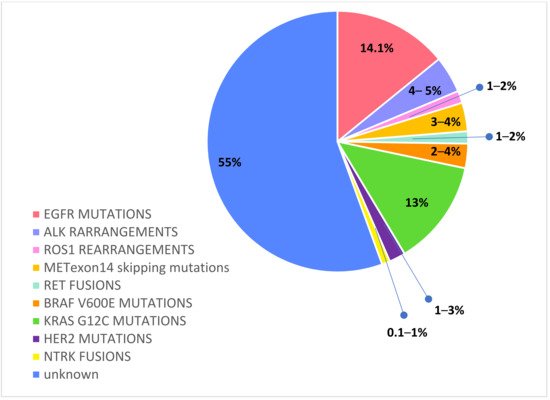
Figure 2. Druggable molecular alterations with tailored treatments in oncogene-addicted NSCLC.
According to previous reports, driver oncogenic alterations, such as EGFR, ALK, ROS1, RET, NTRK, and HER2, have a higher frequency in never smokers, younger age, females, and Asian NSCLC patients, with a tendency to early metastasis and to brain dissemination [26].
The sequencing of the human genome has permitted one to characterize different molecular subgroups of lung cancer patients, who are grouped under the definition of oncogene-addicted NSCLC.
The identification of an ever-increasing number of potentially druggable molecular alterations has led to the development of tailored treatments, which are tyrosine kinase inhibitors (TKIs), with remarkable results in terms of intracranial disease control and OS. Multiple randomized phase III studies demonstrated the superiority of first-line targeted therapies over platinum-based CT for oncogene-addicted NSCLC patients.
Compared to non-oncogenic-driven NSCLC, the prognosis of mutated patients has continuously improved. NSCLC patients with oncogenic-driven mutations are more likely to develop BMs because of the better control of extracranial disease and prolonged survival.
Given the significant CNS activity of novel targeted agents, there is growing evidence that upfront treatment with tailored systemic therapies can sufficiently control BMs.
There are several reasons why local brain irradiation can be deferred in favor of first-line next-generation TKIs:
- The newer generation targeted systemic therapies have demonstrated far greater CNS penetration than CT or older targeted agents; the newer molecular targeted agents are liposoluble compounds with low molecular weight and can cross the BBB; furthermore, they have the ability to penetrate cerebrospinal fluid (CSF).
- Oncogene-addicted NSCLC patients are living several years rather than only a few months, allowing for more time for BMs to develop, as well as for adverse effects from prior RT to manifest.
- These factors lead to a treatment strategy shift, privileging brain penetrant TKIs systemic therapies over local treatments, maintaining patient QoL by minimizing the RT-related consequences.
In the era of targeted therapies, the management of BMs is a challenging issue. It remains unclear whether it is reasonable enough to defer RT until the intracranial progression is noted in patients on TKIs; therefore, the question of how and when to perform brain RT remains open.
Studies on the clinical efficacy of RT combined with TKIs for patients with CNS metastases are very limited and largely retrospective; most adopt only WBRT, and many prospective trials recruit relatively small numbers of patients without considering oncogenic mutational status [27][28][29]. Furthermore, data for patients with molecular driver alterations other than those EGFR are even more scarce, and the efficacy of combined RT with these agents is only anecdotal [30].
Perspective trials appropriately designed to assess the optimal timing of brain RT are necessary.
2. Egfr Mutations
Activated EGFR mutations, predominantly exon 19 deletions and exon 21 L858R mutations, occur in approximately 14.1% of Caucasian NSCLC [31].
Among EGFR mutated NSCLC patients, BMs have an increased frequency, considering baseline incidence ranging from 23% to 32% [32][33][34][35] and a further risk of intracranial progression of about 15–20% during first-generation TKIs treatment [36][37].
These data reflect a pharmacokinetic failure of the first- and second- generation EGFR TKIs to penetrate the brain. Though erlotinib, gefitinib, and afatinib have intracranial activity, these agents have a limited BBB penetration, and they are detected in CFS only at a low concentration, in the 1 to 5 percent range of what is observed in the serum [38][39][40][41].
By contrast, third-generation irreversible TKI osimertinib achieves a greater intracerebral concentration and has shown high intracranial response rates, even against leptomeningeal carcinomatosis [42][43][44].
Osimertinib was first approved in the second-line setting in patients that developed a T790M mutation after failure of a first-generation TKI.
Pooled data from two phase II trials—AURA extension and AURA2—in 50 T790M-positive advanced NSCLC patients with BMs progressed to prior EGFR TKI have demonstrated the significant intracranial activity of osimertinib; CNS objective response rate (ORR) and disease control rate (DCR) were 54% and 92%, respectively, and CNS response was observed regardless of prior brain irradiation [45].
In the randomized phase III AURA 3 trial osimertinib demonstrated significantly greater progression-free survival (PFS) than platinum-based doublet-CT in patients with EGFR T790M advanced NSCLC and progression on prior EGFR-TKI treatment. Among 116 patients with BMs (measurable or not), PFS was longer with osimertinib compared to CT (11.7 vs. 5.6 months, HR 0.32; and 95% CI: 0.15–0.69) and cumulative incidence of CNS progression at 6 months was lower with osimertinib compared to CT (11.5% vs. 28.2%) [46].
Subsequently, osimertinib was approved in the first-line setting on the basis of the randomized phase III FLAURA trial, which evaluated the efficacy of upfront osimertinib versus a SoC EGFR TKI (erlotinib or gefitinib) in treatment-naïve EGFR mutant (exon 19 del or L858R) advanced NSCLC patients [47].
The CNS activity of osimertinib was confirmed in a subset analysis of the randomized phase III FLAURA trial, which evaluated the efficacy of upfront osimertinib versus a SoC EGFR TKI (erlotinib or gefitinib) in treatment-naïve EGFR mutant (exon 19 del or L858R) advanced NSCLC patients. In the preplanned, exploratory analysis (CNS analysis set, N = 128), osimertinib reported that improved CNS RR (66% vs. 43%) and median CNS PFS among patients with measurable and/or non-measurable CNS lesions was longer (not reached vs. 13.9 months, HR 0.48, 95% CI: 0.26–0.86, and p = 0.04). Furthermore, osimertinib reduced the risk of CNS progression in the overall study population (6% vs. 15%), regardless of the presence or absence of known or treated CNS metastases at baseline. Among patients with BMs evaluable for response (N = 41), osimertinib improved the CNS RR (91% vs. 68%) [48].
Data from this analysis show that osimertinib reveal encouraging activity against CNS involvement, with a greater intracranial response and clinical benefit both in preventing or delaying BMs.
Randomized trials comparing upfront osimertinib with brain irradiation are lacking. Although retrospective data indicate that the deferral of RT may be associated with worse outcomes compared with early RT [49][50][51][52][53], those studies were all conducted with earlier-generation EGFR TKIs, which have less intracranial activity than osimertinib.
In sum, the available data suggest that osimertinib demonstrates the greatest CNS activity and prevention of CNS progression, making it the preferred initial treatment option for EGFR-mutated NSCLC with BMs, deferring brain RT and its neurocognitive defects in case of intracranial progression.
References
- Bray, F.; Ferlay, J.; Soerjomataram, I.; Siegel, R.L.; Torre, L.A.; Jemal, A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 2018, 68, 394–424.
- Siegel, R.L.; Miller, K.D.; Jemal, A. Cancer statistics. CA Cancer J. Clin. 2020, 70, 7–30.
- Molina, J.R.; Yang, P.; Cassivi, S.D.; Schild, S.E.; Adjei, A.A. Non-small cell lung cancer: Epidemiology, risk factors, treatment, and survivorship. Mayo Clin. Proc. 2008, 83, 584–594.
- Waqar, S.N.; Samson, P.P.; Robinson, C.G.; Bradley, J.; Devarakonda, S.; Du, L.; Govindan, R.; Gao, F.; Puri, V.; Morgensztern, D. Non-small-cell Lung Cancer with Brain Metastasis at Presentation. Clin. Lung Cancer 2018, 19, e373–e379.
- Nishino, M.; Soejima, K.; Mitsudomi, T. Brain metastases in oncogene-driven non-small cell lung cancer. Transl. Lung Cancer Res. 2019, 8 (Suppl. 3), S298–S307.
- Moro-Sibilot, D.; Smit, E.; de Castro Carpeño, J.; Lesniewski-Kmak, K.; Aerts, J.; Villatoro, R.; Kraaij, K.; Nacerddine, K.; Dyachkova, Y.; Smith, K.T.; et al. Non-small cell lung cancer patients with brain metastases treated with first-line platinum-doublet chemotherapy: Analysis from the European FRAME study. Lung Cancer 2015, 90, 427–432.
- Sperduto, P.W.; Mesko, S.; Jing, L.; Cagney, D.; Aizer, A.; Lin, N.U.; Nesbit, E.; Kruser, T.J.; Chan, J.; Braunstein, S.; et al. Survival in Patients with Brain Metastases: Summary Report on the Updated Diagnosis-Specific Graded Prognostic Assessment and Definition of the Eligibility Quotient. J. Clin. Oncol. 2020, 38, 3773–3784.
- Kadry, H.; Noorani, B.; Cucullo, L.A. Blood–brain barrier overview on structure, function, impairment, and biomarkers of integrity. BMC 2020, 17, 69.
- Morganti, J.M.; Jopson, T.D.; Liu, S.; Gupta, N.; Rosi, S. Cranial irradiation alters the brain’s microenvironment and permits CCR2+ macrophage infiltration. PLoS ONE 2014, 9, e93650.
- Yoshida, Y.; Sejimo, Y.; Kurachi, M.; Ishizaki, Y.; Nakano, T.; Takahashi, A. X-ray irradiation induces disruption of the blood-brain barrier with localized changes in claudin-5 and activation of microglia in the mouse brain. Neurochem. Int. 2018, 119, 199–206.
- Nordal, R.A.; Wong, C.S. Molecular targets in radiation-induced blood-brain barrier disruption. Int. J. Radiat. Oncol. Biol. Phys. 2005, 62, 279–287.
- Perlow, H.K.; Dibs, K.; Liu, K.; Jiang, W.; Rajappa, P.; Blakaj, D.M.; Palmer, J.; Raval, R.R. Whole-Brain Radiation Therapy Versus Stereotactic Radiosurgery for Cerebral Metastases. Neurosurg. Clin. N. Am. 2020, 31, 565–573.
- Patchell, R.A.; Tibbs, P.A.; Walsh, J.W.; Dempsey, R.J.; Maruyama, Y.; Kryscio, R.J.; Markesbery, W.R.; Macdonald, J.S.; Young, B. A randomized trial of surgery in the treatment of single metastases to the brain. N. Engl. J. Med. 1990, 322, 494–500.
- Vecht, C.J.; Haaxma-Reiche, H.; Noordijk, E.M.; Padberg, G.W.; Voormolen, J.H.; Hoekstra, F.H.; Tans, J.T.; Lambooij, N.; Metsaars, J.A.; Wattendorff, A.R.; et al. Treatment of single brain metastasis: Radiotherapy alone or combined with neurosurgery? Ann. Neurol. 1993, 33, 583–590.
- Brown, P.D.; Ballman, K.V.; Cerhan, J.H.; Anderson, S.K.; Carrero, X.W.; Whitton, A.C.; Greenspoon, J.; Parney, I.F.; Laack, N.N.I.; Ashman, J.B.; et al. Postoperative stereotactic radiosurgery compared with whole brain radiotherapy for resected metastatic brain disease (NCCTG N107C/CEC·3): A multicentre, randomised, controlled, phase 3 trial. Lancet Oncol. 2017, 18, 1049–1060.
- Qin, H.; Wang, C.; Jiang, Y.; Zhang, X.; Zhang, Y.; Ruan, Z. Patients with single brain metastasis from non-small cell lung cancer equally benefit from stereotactic radiosurgery and surgery: A systematic review. Med. Sci. Monit. 2015, 21, 144–152.
- Aoyama, H.; Shirato, H.; Tago, M.; Nakagawa, K.; Toyoda, T.; Hatano, K.; Kenjyo, M.; Oya, N.; Hirota, S.; Shioura, H.; et al. Stereotactic radiosurgery plus whole-brain radiation therapy vs. stereotactic radiosurgery alone for treatment of brain metastases: A randomized controlled trial. JAMA 2006, 295, 2483–2491.
- Rades, D.; Schild, S.E.; Lohynska, R.; Veninga, T.; Stalpers, L.J.; Dunst, J. Two radiation regimens and prognostic factors for brain metastases in nonsmall cell lung cancer patients. Cancer 2007, 110, 1077–1082.
- Mulvenna, P.; Nankivell, M.; Barton, R.; Faivre-Finn, C.; Wilson, P.; McColl, E.; Moore, B.; Brisbane, I.; Ardron, D.; Holt, T.; et al. Dexamethasone and supportive care with or without whole brain radiotherapy in treating patients with non-small cell lung cancer with brain metastases unsuitable for resection or stereotactic radiotherapy (QUARTZ): Results from a phase 3, non-inferiority, randomised trial. Lancet 2016, 388, 2004–2014.
- Li, J.; Bentzen, S.M.; Li, J.; Renschler, M.; Mehta, M.P. Relationship between neurocognitive function and quality of life after whole-brain radiotherapy in patients with brain metastasis. Int. J. Radiat. Oncol. Biol. Phys. 2008, 71, 64–70.
- van den Bent, M.J. The role of chemotherapy in brain metastases. Eur. J. Cancer 2003, 39, 2114–2120.
- Cortes, J.; Rodriguez, J.; Aramendia, J.M.; Salgado, E.; Gurpide, A.; Garcia-Foncillas, J.; Aristu, J.J.; Claver, A.; Bosch, A.; Lopez-Picazo, J.M.; et al. Front-line paclitaxel/cisplatin-based chemotherapy in brain metastases from non-small-cell lung cancer. Oncology 2003, 64, 28–35.
- Tsao, A.S.; Scagliotti, G.V.; Bunn, P.A., Jr.; Carbone, D.P.; Warren, G.W.; Bai, C.; de Koning, H.J.; Yousaf-Khan, A.U.; McWilliams, A.; Tsao, M.S.; et al. Scientific Advances in Lung Cancer 2015. J. Thorac. Oncol. 2016, 1, 613–638.
- Ettinger, D.S.; Wood, D.E.; Aisner, D.L.; Akerley, W.; Bauman, J.R.; Bharat, A.; Bruno, D.S.; Chang, J.Y.; Chirieac, L.R.; D’Amico, T.A.; et al. National comprehensive cancer network. NCCN clinical Practice guidelines in oncology 2021. J. Natl. Compr. Cancer Netw. 2021, 19, 254–266.
- Jordan, E.J.; Kim, H.R.; Arcila, M.E.; Barron, D.; Chakravarty, D.; Gao, J.; Chang, M.T.; Ni, A.; Kundra, R.; Jonsson, P.; et al. Prospective Comprehensive Molecular Characterization of Lung Adenocarcinomas for Efficient Patient Matching to Approved and Emerging Therapies. Cancer Discov. 2017, 7, 596–609.
- Chevallier, M.; Borgeaud, M.; Addeo, A.; Friedlaender, A. Oncogenic driver mutations in non-small cell lung cancer: Past, present and future. World J. Clin. Oncol. 2021, 12, 217–237.
- Pesce, G.A.; Klingbiel, D.; Ribi, K.; Zouhair, A.; von Moos, R.; Schlaeppi, M.; Caspar, C.B.; Fischer, N.; Anchisi, S.; Peters, S.; et al. Outcome, quality of life and cognitive function of patients with brain metastases from non-small cell lung cancer treated with whole brain radiotherapy combined with gefitinib or temozolomide. A randomised phase II trial of the Swiss Group for Clinical Cancer Research (SAKK 70/03). Eur. J. Cancer. 2012, 48, 377–384.
- Ma, S.; Xu, Y.; Deng, Q.; Yu, X. Treatment of brain metastasis from non-small cell lung cancer with whole brain radiotherapy and Gefitinib in a Chinese population. Lung Cancer. 2009, 5, 198–203.
- Doherty, M.K.; Korpanty, G.J.; Tomasini, P.; Alizadeh, M.; Jao, K.; Labbé, C.; Mascaux, C.M.; Martin, P.; Kamel-Reid, S.; Tsao, M.S.; et al. Treatment options for patients with brain metastases from EGFR/ALK-driven lung cancer. Radiother. Oncol. 2017, 123, 195–202.
- Zhang, I.; Zaorsky, N.G.; Palmer, J.D.; Mehra, R.; Lu, B. Targeting brain metastases in ALK-rearranged non-small-cell lung cancer. Lancet Oncol. 2015, 16, e510–e521.
- Zhang, Y.L.; Yuan, J.Q.; Wang, K.F.; Fu, X.H.; Han, X.R.; Threapleton, D.; Yang, Z.Y.; Mao, C.; Tang, J.L. The prevalence of EGFR mutation in patients with non-small cell lung cancer: A systematic review and meta-analysis. Oncotarget 2016, 7, 78985–78993.
- Iuchi, T.; Shingyoji, M.; Itakura, M.; Yokoi, S.; Moriya, Y.; Tamura, H.; Yoshida, Y.; Ashinuma, H.; Kawasaki, K.; Hasegawa, Y.; et al. Frequency of brain metastases in non-small-cell lung cancer, and their association with epidermal growth factor receptor mutations. Int. J. Clin. Oncol. 2015, 20, 674–679.
- Rangachari, D.; Yamaguchi, N.; VanderLaan, P.A.; Folch, E.; Mahadevan, A.; Floyd, S.R.; Uhlmann, E.J.; Wong, E.T.; Dahlberg, S.E.; Huberman, M.S.; et al. Brain metastases in patients with EGFR-mutated or ALK-rearranged non-small-cell lung cancers. Lung Cancer 2015, 88, 108–111.
- Hendriks, L.; Smit, E.F.; Vosse, B.A.; Mellema, W.W.; Heideman, D.A.; Bootsma, G.P.; Westenend, M.; Pitz, C.; de Vries, G.J.; Houben, R.; et al. EGFR mutated non-small cell lung cancer patients: More prone to development of bone and brain metastases? Lung Cancer 2014, 84, 86–91.
- Remon, J.; Besse, B. Brain Metastases in Oncogene-Addicted Non-Small Cell Lung Cancer Patients: Incidence and Treatment. Front. Oncol. 2018, 8, 88.
- Heon, S.; Yeap, B.Y.; Britt, G.J.; Costa, D.B.; Rabin, M.S.; Jackman, D.M.; Johnson, B.E. Development of central nervous system metastases in patients with advanced non-small cell lung cancer and somatic EGFR mutations treated with gefitinib or erlotinib. Clin. Cancer Res. 2010, 16, 5873–5882.
- Patel, S.H.; Rimner, A.; Foster, A.; Zhang, Z.; Woo, K.M.; Yu, H.A.; Riely, G.J.; Wu, A.J. Patterns of initial and intracranial failure in metastatic EGFR-mutant non-small cell lung cancer treated with erlotinib. Lung Cancer 2017, 108, 109–114.
- Chiu, C.H.; Tsai, C.M.; Chen, Y.M.; Chiang, S.C.; Liou, J.L.; Perng, R.P. Gefitinib is active in patients with brain metastases from non-small cell lung cancer and response is related to skin toxicity. Lung Cancer 2005, 47, 129–138.
- Wei, Y.F.; Lim, C.K.; Tsai, M.S.; Huang, M.S.; Chen, K.Y. Intracranial Responses to Afatinib at Different Doses in Patients With EGFR-mutated Non-small- cell Lung Carcinoma and Brain Metastases. Clin. Lung Cancer 2019, 20, e274–e283.
- Zee, Y.K.; Chin, T.M.; Wong, A.S.C. Fatal cystic change of brain metastasis after response to gefitinib in non-small-cell lung cancer. J. Clin. Oncol. 2009, 27, e145–6.
- Togashi, Y.; Masago, K.; Fukudo, M.; Terada, T.; Fujita, S.; Irisa, K.; Sakamori, Y.; Kim, Y.H.; Mio, T.; Inui, K.I.; et al. Cerebrospinal fluid concentration of erlotinib and its active metabolite OSI-420 in patients with central nervous system metastases of non-small cell lung cancer. J. Thorac. Oncol. 2010, 5, 950–955.
- Colclough, N.; Chen, K.; Johnström, P.; Strittmatter, N.; Yan, Y.; Wrigley, G.L.; Schou, M.; Goodwin, R.; Varnäs, K.; Adua, S.J.; et al. Preclinical Comparison of the Blood-brain barrier Permeability of Osimertinib with Other EGFR TKIs. Clin. Cancer Res. 2021, 27, 189–201.
- Ballard, P.; Yates, J.W.T.; Yang, Z.; Kim, D.W.; Yang, J.C.H.; Cantarini, M.; Pickup, K.; Jordan, A.; Hickey, M.; Grist, M. Preclinical Comparison of Osimertinib with Other EGFR-TKIs in EGFR-Mutant NSCLC Brain Metastases Models, and Early Evidence of Clinical Brain Metastases Activity. Clin. Cancer Res. 2016, 22, 5130–5140.
- Yang, J.C.H.; Kim, S.W.; Kim, D.W.; Lee, J.S.; Cho, B.C.; Ahn, J.S.; Lee, D.H.; Kim, T.M.; Goldman, J.W.; Natale, R.B.; et al. Osimertinib in Patients with Epidermal Growth Factor Receptor Mutation-Positive Non-Small-Cell Lung Cancer and Leptomeningeal Metastases: The BLOOM Study. J. Clin. Oncol. 2020, 38, 538–547.
- Goss, G.; Tsai, C.M.; Shepherd, F.A.; Ahn, M.J.; Bazhenova, L.; Crinò, L.; de Marinis, F.; Felip, E.; Morabito, A.; Hodge, R.; et al. CNS response to osimertinib in patients with T790M-positive advanced NSCLC: Pooled data from two phase II trials. Ann. Oncol. 2018, 29, 687–693.
- Mok, T.; Ahn, M.J.; Han, J.Y.; Kang, J.H.; Katakami, N.; Kim, H.; Hodge, R.; Ghiorghiu, D.C.; Cantarini, M.; Wu, Y.L.; et al. CNS response to osimertinib in patients (pts) with T790M-positive advanced NSCLC: Data from a randomized phase III trial (AURA3). J. Clin. Oncol, 2017; 35.
- Soria, J.C.; Ohe, Y.; Vansteenkiste, J.; Reungwetwattana, T.; Chewaskulyong, B.; Lee, K.H.; Dechaphunkul, A.; Imamura, F.; Nogami, N.; Kurata, T.; et al. Osimertinib in untreated EGFR-mutated advanced non-small-cell lung cancer. N. Engl. J. Med. 2018, 378, 113–125.
- Reungwetwattana, T.; Nakagawa, K.; Cho, B.C.; Cobo, M.; Cho, E.K.; Bertolini, A.; Bohnet, S.; Zhou, C.; Lee, K.H.; Nogami, N.; et al. CNS Response to Osimertinib Versus Standard Epidermal Growth Factor Receptor Tyrosine Kinase Inhibitors in Patients With Untreated EGFR-Mutated Advanced Non-Small-Cell Lung Cancer. J. Clin. Oncol. 2018, 36, 3290–3297.
- Iuchi, T.; Shingyoji, M.; Sakaida, S.; Hatano, K.; Nagano, O.; Itakura, M.; Kageyama, H.; Yokoi, S.; Hasegawa, Y.; Kawasaki, K.; et al. Phase II trial of gefitinib alone without radiation therapy for Japanese patients with brain metastases from EGFR-mutant lung adenocarcinoma. Lung Cancer 2013, 82, 282–287.
- Grommes, C.; Oxnard, G.N.; Kris, M.G.; Miller, V.A.; Pao, W.; Holodny, A.I.; Clarke, J.L.; Lassman, A.B. “Pulsatile” high-dose weekly erlotinib for CNS metastases from EGFR mutant non-small cell lung cancer. Neuro Oncol. 2011, 13, 1364–1369.
- Gerber, N.K.; Yamada, Y.; Rimner, A.; Shi, W.; Riely, G.J.; Beal, K.; Yu, H.A.; Chan, T.A.; Zhang, Z.; Wu, A.J. Erlotinib versus radiation therapy for brain metastases in patients with EGFR-mutant lung adenocarcinoma. Int. J. Radiat. Oncol. Biol. Phys. 2014, 89, 322–329.
- Magnuson, W.J.; Lester-Coll, N.H.; Wu, A.J.; Yang, T.J.; Lockney, N.A.; Gerber, N.K.; Beal, K.; Amini, A.; Patil, T.; Kavanagh, B.D.; et al. Management of Brain Metastases in Tyrosine Kinase Inhibitor-Naïve Epidermal Growth Factor Receptor-Mutant Non-Small-Cell Lung Cancer: A Retrospective Multi-Institutional Analysis. J. Clin. Oncol. 2017, 35, 1070–1077.
- Welsh, J.W.; Komaki, R.; Amini, A.; Munsell, M.F.; Unger, W.; Allen, P.K.; Chang, J.Y.; Wefel, J.S.; McGovern, S.L.; Garland, L.L.; et al. Phase II trial of erlotinib plus concurrent whole-brain radiation therapy for patients with brain metastases from non-small-cell lung cancer. J. Clin. Oncol. 2013, 31, 895–902.
More
Information
Subjects:
Oncology
Contributors
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
760
Revisions:
2 times
(View History)
Update Date:
27 Jun 2022
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





