
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Célia Fortuna Rodrigues | + 3682 word(s) | 3682 | 2021-09-06 11:11:38 | | | |
| 2 | Vivi Li | Meta information modification | 3682 | 2021-09-08 08:31:17 | | |
Video Upload Options
Patients with severe COVID-19, such as individuals in intensive care units (ICU), are exceptionally susceptible to bacterial and fungal infections. The most prevalent fungal infections are aspergillosis and candidemia. Nonetheless, other fungal species (for instance, Histoplasma spp., Rhizopus spp., Mucor spp., Cryptococcus spp.) have recently been increasingly linked to opportunistic fungal diseases in COVID-19 patients. These fungal co-infections are described with rising incidence, severe illness, and death that is associated with host immune response. Awareness of the high risks of the occurrence of fungal co-infections is crucial to downgrade any arrear in diagnosis and treatment to support the prevention of severe illness and death directly related to these infections.
1. Introduction
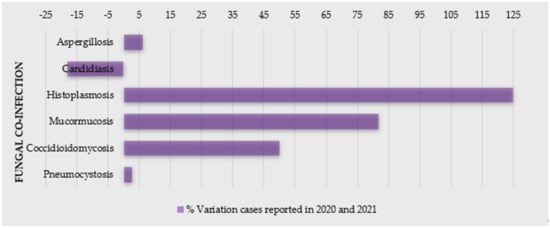
2. Fungal Infections as a Co-Morbidity of COVID-19
2.1. Candidiasis
| Fungal Infection in COVID-19 Infection | Observed Immune Response |
Co-Morbidity/ Disease Models |
Test/Diagnosis Performed | COVID-19 Treatment |
Antifungals Used | Steroids? | Outcome after Treatment | References |
|---|---|---|---|---|---|---|---|---|
| Candidemia Candida duobushaemulonii Candida parapsilosis, Candida lusitaniae |
Elevated pro-inflammatory markers (d-dimer, ferritin, CRP, progressive thrombocytosis) and neutrophilia |
Acute pulmonary embolism with subarachnoid hemorrhage superimposed bacterial pneumonia |
CT scan, Culture, RT-PCR Blood, urine, and DTA |
Meropenem, Levofloxacin Trimethoprim/sulfamethoxazole, Amikacin, tigecycline, colistin |
Intravenous fluconazole |
NR | Dead | [31] |
| Candidemia (Candida glabrata) |
Leucocytes—normal, C-reactive protein and interleukin 6—altered |
Type-2 diabetes ischemic heart disease stadium IV, leg amputation highly suspected bacterial superinfection |
Chest X-ray and CT scan, RT-PCR, serology, MALDI-TOF |
Darunavir/ritonavir, HCQ, piperacillin/tazobactam, teicoplanin, ertapenem, colistin |
Caspofungin | NR | Dead | [32] |
| Candidemia Candida auris (n = 10), Candida albicans (n = 3), Candida tropicalis (n = 1), Candida krusei (P. kudriavzevii) (n = 1) |
NA | Underlying chronic conditions (e.g., hypertension, n = 7; DM, n = 6; and chronic kidney and liver disease, n = 2) | MALDI-TOF and molecular identification—sequencing | NR | Micafungin | NR | Dead (n = 8) | [4] |
| Candidemia Candida auris (n = 3) |
NA | DM, hypertension, chronic renal failure, coronary artery disease, obesity |
Vitek 2 system, MALDI-TOF, sequencing, multiplex PCR |
NR | Anidulafungin | NR | Dead | [33] |
| Candidemia Candida auris (n = 12) |
NA | DM (n = 6), hypertension (n = 6), multiple myeloma (n = 1), stem cell transplantation (n = 1), dyslipidemia (n = 1), end stage renal disease (n = 1), bladder cancer (n = 1), obesity (n = 1), systematic lupus erythematosus (n = 1) |
PCR, MALDI-TOF, Vitek2, whole genome sequencing |
Remdesivir (n = 9), HCQ (n = 1), | Amphotericin B Micafungin, |
n = 10 | Dead (n = 6) Alive (n = 6) |
[34] |
2.2. Aspergillosis
| Fungal Infection in COVID-19 Infection | Observed Immune Response | Co-morbidity/ DiseaseModels |
Test/Diagnosis Performed | COVID-19 Treatment | Antifungals Used | Steroids? | Outcome after Treatment | References |
|---|---|---|---|---|---|---|---|---|
| Aspergillosis Aspergillus spp., CAPA |
Highly permissive inflammatory response | DM, CVD | CT scan, Culture | HCQ | Azoles, liposomal amphotericin B | NR | Alive | [43] |
| Immunocompromised | ARD, HT | CT scan, RT-PCR, Culture, ELISA | NR | Voriconazole | Yes (n = 7) |
Some alive and some dead | [44] | |
| Aspergillosis Aspergillus fumigatus, CAPA |
Immunocompromised | DM, HT | CT scan, Culture | NR | Isavuconazole, voriconazole | No | Alive | [42] |
| HT, coronary heart disease, obesity | CT scan, RT-PCR, Culture, | HCQ, meropenem, azithromycin | Voriconazole | Yes | Dead | [26] | ||
| Low B-cell and T-cell response | Severe dyspnea, hypertension, DM | CT scan, RT-PCR, Serology | RD, multiple antibiotics | Multiple antifungals | No | Alive | [45] | |
| Systemic pro-inflammatory cytokine responses | Asthma, DM, Myeloma | CT scan, RT-PCR, Culture, | NR | Voriconazole, isavuconazole, liposomal amphotericin B, caspofungin, anidulafungin | Yes | Some alive and some dead | [46] | |
| High inflammatory response and immunosuppression | ALL, AML | RT-PCR, CT scan, Culture, Serology | NR | Caspofungin, fluconazole, liposomal amphotericin B, caspofungin, itraconazole | No | Some alive and some dead | [47] | |
| Aspergillosis Aspergillus spp., IA |
Acquired immunodeficiency and immunosuppression | ARD | Antigen, CT scan, Culture, Serology | NR | NR | Yes | Death (quick evolution) |
[48] |
| Strong deregulation of core components of innate immune and inflammatory responses | RHAEM | NA | NA | NA | NA | NR | [49] |
2.3. Histoplasmosis
| Fungal Infection in COVID-19 Infection | Observed Immune Response | Co-morbidity/ Disease Models |
Test/Diagnosis Performed | COVID-19 Treatment | Antifungals Used | Steroids? | Outcome after Treatment | References |
|---|---|---|---|---|---|---|---|---|
| Histoplasmosis Histoplasma capsulatum |
Acquired immunodeficiency | HIV | CT-scan, RT-PCR |
Tenofovir/lamivudine and atazanavir/ritonavir ceftriaxone, azithromycin |
Itraconazole | Yes (dexamethasone) |
Alive | [27][52] |
| HIV | HIV | CT-scan, RT-PCR |
Atazanavir/ritonavir, tenofovir/emtricitabine | Itraconazole, amphotericin B deoxycholate |
No | Alive | [27] | |
| Inflammatory response | NA | CT-scan, RT-PCR |
Levofloxacin | Itraconazole | Yes (methylprednisolone) |
Alive | [53] | |
| NA | NA | CT scan, RT-PCR |
NA | Itraconazole | No | Alive | [54] | |
| Histoplasmosis Histoplasma capsulatum-like intracellular yeasts |
Acquired immunodeficiency | HIV | CT-scan, RT-PCR |
HCQ, lopinavir/ritonavir, tenofovir disoproxil fumarate/emtricitabine plus dolutegravir | Amphotericin B deoxycholate, itraconazole |
No | Lost to follow-up | [55] |
2.4. Mucormycosis
| Co-Morbidity/ DiseaseModels |
Test/Diagnosis Performed | COVID-19 Treatment | Antifungals Used | Steroids? | Outcome after Treatment | References |
|---|---|---|---|---|---|---|
| Obesity HT |
CT-scan, RT-PCR |
None mentioned | Linezolid, meropenem | NA | Died | [67] |
| Asthma HT DM |
CT-scan, RT-PCR |
Remdesivir | Amphotericin B | NA | Died | [68] |
| DM Vascular disease |
CT-scan, RT-PCR |
Tocilizumab, methylprednisolone, dexamethasone | Amphotericin B | Methylprednisolone, dexamethasone | Died | [69] |
| HT | CT-scan, RT-PCR |
Hydrocortisone | Amphotericin B | Hydrocortisone | Died | [70] |
| NA | CT-scan, RT-PCR |
Remdesivir, tocilizumad, dexamethasone | Amphotericin B | Dexamethasone | Died | [71] |
| Asthma HT DM |
CT-scan, RT-PCR |
Remdesivir, dexamethasone | Amphotericin B | Dexamethasone | Died | [72] |
| HT | CT-scan, RT-PCR |
HCQ, lopinavir–ritonavir | Amphotericin B | NA | Died | [73] |
| DM ICM RD |
CT-scan, RT-PCR |
Meropenem | Amphotericin B | Dexamethasone | Alive | [74] |
| DM | CT-scan, RT-PCR |
NA | Amphotericin B | NA | Alive | [75] |
| HT, DM |
CT-scan, RT-PCR |
NA | Liposomal amphotericin B, itraconazole | NA | Alive | [76] |
| NA | RT-PCR CT-scan |
Remdesivir, dexamethasone, metformin, glipizide | Amphotericin B, ceftriaxone | Dexamethasone | Live | [77] |
| DM | CT-scan, RT-PCR |
Meropenem, oseltamivir tocilizumab, sitagliptin/metformin |
Amphotericin B | Methylprednisolone, dexamethasone |
Died | [69] |
| DM | CT-scan, RT-PCR |
Remdesivir, ceftriaxone, azithromycin, dexamethasone | Voriconazole, liposomal amphotericin B | Dexamethasone | Live | [78] |
| DM (1 patient) No co-morbidity (1 patient) |
CT-scan | Remdesivir, convalescent plasma, vancomycin, piperacillin-tazobactam |
Amphotericin B | NA | Live (n = 1) Died n = (1) |
[68] |
| Obesity DM |
CT-scan, RT-PCR |
Amoxicillin-clavulanate, imipenem/linezolid |
Amphotericin B | NA | Died | [79] |
| DM (n = 8) CRF (n = 3) |
CT-scan | Broad-spectrum antibiotics | Liposomal amphotericin B | Dexamethasone | Died (n = 7) Alive (n = 4) |
[80] |
| DM HT (all patients) |
RT-PCR | HCQ, glucocorticoids |
Systemic antifungals | Glucocorticoids | Died (n = 7) Live (n = 8) |
[81] |
| T2DM (4) T2DM with HT (1) HT (1) Kidney Disease (1) |
CT-scan, RT-PCR |
Tocilizumab, prednisolone, piperacillin/tazobac, linezolid |
Voriconazole | Prednisolone | Died (n = 3) Alive (n = 4) |
[82] |
| DM (21-cases) HT (14-cases) Renal failure (1-case) |
CT-scan, RT-PCR |
HCQ, azithromycin | Caspofungin | Combination of steroids | All Live | [76] |
| DM (16) | RT-PCR | Corticosteroids | Liposomal amphotericin B, voriconazole, posaconazole |
On Steroid | Alive (n = 10) Died n = (6) |
[83] |
| HT, UTI |
CT-scan, RT-PCR |
Either dexamethasone or methylprednisolone (7 patients); interferon (2 patient); remdesivir (1 patient); flavipiravir and HCQ (1 patient) |
Amphotericin B, posaconazole | Dexamethasone or Methylprednisolone (n = 7) |
Live | [84] |
| DM | RT-PCR CT-scan |
Remdesivir, levofloxacin, dexamethasone, meropenem, vancomycin, piperacillin/tazobactam | Amphotericin B, posaconazole | Dexamethasone | Live | [85] |
| No co-morbidity | CT-scan, RT-PCR |
HCQ | Amphotericin B | NA | Died | [86] |
| chronic lymphocytic leukemia DM |
RT-PCR | NA | Amphotericin B | NA | Died | [87] |
| DM HT asthma |
RT-PCR | NA | Amphotericin B | No | Died | [88] |
| AML | CT-scan, RT-PCR |
HCQ lopinavir-ritonavir |
Amphotericin B | NA | Died | [73] |
| renal disease | CT-scan, RT-PCR |
Remdesivir, vancomycin, cefepime | Liposomal amphotericin B, posaconazole | Dexamethasone | Died | [72] |
| ICM HF s/p OHT DM HT CKD |
RT-PCR | Remdesivir methylprednisolone |
Fluconazole | Methylprednisolone, dexamethasone |
Died | [89] |
| No history of any co-morbidity | CT-scan, RT-PCR |
Tocilizumab | Liposomal amphotericin B, posaconazole, isavuconazole | Dexamethasone | Live | [90] |
| DM HT |
Piperacillin/tazobactam, HCQ, azithromycinlopin, vir/ritonavir, prednisone Dexamethasone |
Liposomal amphotericin B, isavuconazole, posaconazole | Prednisone, Dexamethasone | Live | [91] | |
| HT | RT-PCR | Remdesivir, dexamethasone | Amphotericin B | Dexamethasone | Died | [92] |
| T2DM (all 6 patients) |
CT-scan, RT-PCR |
Prednisolone, dexamethasone, methylprednisolone | Amphotericin B, posaconazole | Prednisolone, Dexamethasone, methylprednisolone |
All Live |
[93] |
| DM HT |
CT-scan, RT-PCR |
Remdesivir, interferon-alpha | Systemic antifungals | Systemic corticosteroid | Died | [94] |
| T2DM, HT (2) T2DM (3) |
CT-scan, RT-PCR |
Tocilizumab, convalescent plasma, methylprednisolone |
Liposomal amphotericin B, posaconazole |
Methylprednisolone | Died (n = 2) Alive (n = 3) |
[95] |
| T1DM | CT-scan, RT-PCR |
Ceftriaxone, azithromycin, dexamethasone, remdesivir, tocilizumab |
Amphotericin B | Dexamethasone | Live | [71] |
| Obesity hypothyroidism |
CT-scan, RT-PCR |
HCQ, remdesivir, vancomycin, meropenem | Liposomal amphotericin B, posaconazole |
Prednisone | Died | [96] |
| HT Asthma |
RT-PCR | Meropenem, remdesivir, dexamethasone | Liposomal amphotericin B | Dexamethasone, prednisolone | Died | [97] |
2.5. Cryptococcus
| Fungal Infection in COVID-19 Infection | Observed Immune Response | Co-morbidity/ Disease Models |
Test/Diagnosis Performed | COVID-19 Treatment | Antifungals Used | Steroids? | Outcome after Treatment | References |
|---|---|---|---|---|---|---|---|---|
| Cryptococcus neoformans | High inflammatory response and immunosuppression | HAT, HBV | CT-scan, RT-PCR |
meropenem, vancomycin | Fluconazole | Yes (tacrolimus, prednisone) |
Death | [99] |
| Acquired immunodeficiency and immunosuppression | HIV | CT-scan, RT-PCR |
Tenofovir-DF/ Emtricitabine-atazanavir/ritonavir |
Amphotericin B deoxycholate plus fluconazole | No | Death | [100] | |
| High inflammatory response and immunosuppression | Stage IV prostate cancer HT, colon-sigma diverticulosis |
CT-scan | No | Fluconazole Amphotericin B plus flucytosine |
Dexamethasone | Death | [101] | |
| High inflammatory response and immunosuppression | HT, DM | NA but COVID19 positive mentioned |
Tocilizumab and corticosteroids | Anidulafungin, Amphotericin, flucytosine |
Methylprednisolone | Death | [98] | |
| Coccidioidomycosis (Coccidioides immitis, C. posadasii) | Impaired cytokine signaling from CD4+ Th1 and cytotoxic CD8+ T-cells among patients | No associated respiratory symptoms & disease | CT scan, Culture, Serology | NR | Liposomal Amphotericin B | No | Alive | [102] |
| Coccidioidomycosis (Coccidioides immitis) | Depressed cellular immunity | Progressive respiratory symptoms, hypoxemia | CT scan, Culture, | Remdesivir | Fluconazole | No | Alive | [103] |
| Pneumocystis jirovecii | Cytokine release storm | RA | CT scan, Culture, Serology | HCQ, Tocilizumab | Caspofungin, ganciclovir, cefoperazone | Glucocorticoids | NR | [104] |
| Functional immune suppression related to CD4+ lymphocytopenia | HIV, progressive hypoxemia | RT-PCR, Culture, Serology, CT | NR | Trimethoprim- sulfamethoxazole | NR | NR | [105] | |
| Immunocompromised | ARD, DM, HT | RT-PCR, Culture, Serology, | HCQ, Lopinavir-ritonavir | Antifungals and antibacterials | Yes | Some alive and some dead | [106] | |
| Low CD4 count (35.6%) | HIV | CT, RT-PCR, Multiplex PCR | NR | Co-trimoxazole and oral prednisolone | No | Alive | [107] | |
| Anemia, lymphopenia, raised C-reactive protein, immunosuppression | HIV | CT, RT-PCR | NR | Co-trimoxazole, IV pentamidine | No | Death | [108] | |
| Severe depletion of CD4+ cells | HIV | RT-PCR, Culture, CT | Emtricitabine, Ritonavir | Trimethoprim-sulfamethoxazole | No | NR | [109] | |
| Immunocompetent patient | Recovered from COVID-19 | RT-PCR, Culture, CT | Enoxaparin, ceftaroline | Trimethoprim-sulfamethoxazole, methylprednisolone | Yes | Alive | [110] | |
| Immunocompromised patients | HT, hepatic steatosis, massive lung thromboses | RT-PCR, Culture, CT, Histopathology | Remdesivir | Trimethoprim-sulfamethoxazole, prednisone | Yes | Some alive and some dead | [111] | |
| Saccharomyces cerevisiae (boulardii) (n = 2) |
Immunosuppression | HT (first) Diabetes (Second) |
RT-PCR | Oseltamivir HCQ |
Anidulafungin, fluconazole |
No treated with Ultra-Levure [preparation of Saccharomyces cerevisiae (boulardii)] |
Both live | [112] |
| Fusarium proliferatum | immunocompetent diabetic patient | HAT substituted hypothyroidism |
RT-PCR | No | Amphotericin B caspofungin |
No | Live | [113] |
2.6. Other Fungal Infections
References
- Soltani, S.; Zakeri, A.; Zandi, M.; Kesheh, M.M.; Tabibzadeh, A.; Dastranj, M.; Faramarzi, S.; Didehdar, M.; Hafezi, H.; Hosseini, P.; et al. The Role of Bacterial and Fungal Human Respiratory Microbiota in COVID-19 Patients. BioMed Res. Int. 2021, 2021, 6670798.
- Talento, A.F.; Hoenigl, M. Fungal Infections Complicating COVID-19: With the Rain Comes the Spores. J. Fungi 2020, 6, 279.
- Rawson, T.M.; Wilson, R.C.; Holmes, A. Understanding the role of bacterial and fungal infection in COVID-19. Clin. Microbiol. Infect. 2021, 27, 9–11.
- Chowdhary, A.; Tarai, B.; Singh, A.; Sharma, A. Multidrug-resistant Candida auris infections in critically Ill Coronavirus disease patients, India, April–July 2020. Emerg. Infect. Dis. 2020, 26, 2694–2696.
- Chowdhary, A.; Sharma, A. The lurking scourge of multidrug resistant Candida auris in times of COVID-19 pandemic. J. Glob. Antimicrob. Resist. 2020, 22, 175–176.
- Arastehfar, A.; Carvalho, A.; Nguyen, M.H.; Hedayati, M.T.; Netea, M.G.; Perlin, D.S.; Hoenigl, M. COVID-19-associated candidiasis (CAC): An underestimated complication in the absence of immunological predispositions? J. Fungi 2020, 6, 211.
- Kubin, C.J.; McConville, T.H.; Dietz, D.; Zucker, J.; May, M.; Nelson, B.; Istorico, E.; Bartram, L.; Small-Saunders, J.; Sobieszczyk, M.E.; et al. Characterization of Bacterial and Fungal Infections in Hospitalized Patients with Coronavirus Disease 2019 and Factors Associated with Health Care-Associated Infections. Open Forum Infect. Dis. 2021, 8, ofab201.
- Chen, X.; Liao, B.; Cheng, L.; Peng, X.; Xu, X.; Li, Y.; Hu, T.; Li, J.; Zhou, X.; Ren, B. The microbial coinfection in COVID-19. Appl. Microbiol. Biotechnol. 2020, 104, 7777–7785.
- Silva, D.L.; Lima, C.M.; Magalhães, V.C.R.; Baltazar, L.M.; Peres, N.T.A.; Caligiorne, R.B.; Moura, A.S.; Fereguetti, T.; Martins, J.C.; Rabelo, L.F.; et al. Fungal and bacterial coinfections increase mortality of severely ill COVID-19 patients. J. Hosp. Infect. 2021, 113, 145–154.
- Moser, D.; Biere, K.; Han, B.; Hoerl, M.; Schelling, G.; Woehrle, T.; Chouke, A. COVID-19 Impairs Immune Response to Candida albicans. Front. Immunol. 2021, 12, 1–10.
- Mulet Bayona, J.V.; Tormo Palop, N.; Salvador García, C.; Fuster Escrivá, B.; Chanzá Aviñó, M.; Ortega García, P.; Gimeno Cardona, C. Impact of the SARS-CoV-2 Pandemic in Candidaemia, Invasive Aspergillosis and Antifungal Consumption in a Tertiary Hospital. J. Fungi 2021, 7, 440.
- Bhatt, K.; Agolli, A.; Patel, M.H.; Garimella, R.; Devi, M.; Garcia, E.; Amin, H.; Domingue, C.; Del Castillo, R.G.; Sanchez-Gonzalez, M. High mortality co-infections of COVID-19 patients: Mucormycosis and other fungal infections. Discoveries 2021, 9, e126.
- Bienvenu, A.L.; Bleyzac, N.; Richard, J.C.; Leboucher, G. No time for pending confirmation of invasive fungal disease in critically ill COVID-19 patients-think empirical treatment. Crit. Care 2020, 24, 4–5.
- Falcone, M.; Tiseo, G.; Giordano, C.; Leonildi, A.; Menichini, M.; Vecchione, A.; Pistello, M.; Guarracino, F.; Ghiadoni, L.; Forfori, F.; et al. Predictors of hospital-acquired bacterial and fungal superinfections in COVID-19: A prospective observational study. J. Antimicrob. Chemother. 2020, 76, 1078–1084.
- Bardi, T.; Pintado, V.; Gomez-Rojo, M.; Escudero-Sanchez, R.; Azzam Lopez, A.; Diez-Remesal, Y.; Martinez Castro, N.; Ruiz-Garbajosa, P.; Pestaña, D. Nosocomial infections associated to COVID-19 in the intensive care unit: Clinical characteristics and outcome. Eur. J. Clin. Microbiol. Infect. Dis. 2021, 40, 495–502.
- Ansari, S.; Hays, J.P.; Kemp, A.; Okechukwu, R.; Murugaiyan, J.; Ekwanzala, M.D.; Ruiz Alvarez, M.J.; Paul-Satyaseela, M.; Iwu, C.D.; Balleste-Delpierre, C.; et al. The potential impact of the COVID-19 pandemic on global antimicrobial and biocide resistance: An AMR Insights global perspective. JAC-Antimicrobial Resist. 2021, 3, dlab038.
- Černáková, L.; Roudbary, M.; Brás, S.; Tafaj, S.; Rodrigues, C.F. Candida auris: A Quick Review on Identification, Current Treatments, and Challenges. Int. J. Mol. Sci. 2021, 22, 4470.
- Salmanton-Garcia, J.; Sprute, R.; Stemler, J.; Bartoletti, M.; Dupont, D.; Valerio, M.; Garcia-Vidal, C.; Falces-Romero, I.; Machado, M.; de la Villa, S.; et al. COVID-19-Associated Pulmonary Aspergillosis, March–August 2020. Emerg. Infect. Dis. 2021, 27, 1077–1086.
- Danion, F.; Letscher-Bru, V.; Guitard, J.; Sitbon, K.; Dellière, S.; Angoulvant, A.; Desoubeaux, G.; Botterel, F.; Bellanger, A.-P.; Gargala, G.; et al. High mortality of COVID-19 associated mucormycosis in France: A nationwide retrospective study. medRxiv 2021.
- Riad, A.; Gomaa, E.; Hockova, B.; Klugar, M. Oral candidiasis of COVID-19 patients: Case report and review of evidence. J. Cosmet. Dermatol. 2021, 20, 1580–1584.
- Rajendra Santosh, A.B.; Muddana, K.; Bakki, S.R. Fungal Infections of Oral Cavity: Diagnosis, Management, and Association with COVID-19. SN Compr. Clin. Med. 2021, 3, 1373–1384.
- Nargesi, S.; Bongomin, F.; Hedayati, M.T. The impact of COVID-19 pandemic on AIDS-related mycoses and fungal neglected tropical diseases: Why should we worry? PLoS Negl. Trop. Dis. 2021, 15, e0009092.
- Gangneux, J.-P.; Bougnoux, M.-E.; Dannaoui, E.; Cornet, M.; Zahar, J.R. Invasive fungal diseases during COVID-19: We should be prepared. J. Mycol. Med. 2020, 30, 100971.
- Verweij, P.E.; Alanio, A. Fungal infections should be part of the core outcome set for COVID-19. Lancet Infect. Dis. 2021, 21, e145.
- Katz, J. Prevalence of candidiasis and oral candidiasis in COVID-19 patients: A cross-sectional pilot study from the patients’ registry in a large health center. Quintessence Int. 2021, 52, 714–718.
- Prattes, J.; Valentin, T.; Hoenigl, M.; Talakic, E.; Reisinger, A.C.; Eller, P. Invasive pulmonary aspergillosis complicating COVID-19 in the ICU—A case report. Med. Mycol. Case Rep. 2021, 31, 2–5.
- Messina, F.A.; Marin, E.; Caceres, D.H.; Romero, M.; Depardo, R.; Priarone, M.M.; Rey, L.; Vázquez, M.; Verweij, P.E.; Chiller, T.M.; et al. Coronavirus Disease 2019 (COVID-19) in a Patient with Disseminated Histoplasmosis and HIV—A Case Report from Argentina and Literature Review. J. Fungi 2020, 6, 275.
- Seagle, E.E.; Jackson, B.R.; Lockhart, S.R.; Georgacopoulos, O.; Nunnally, N.S.; Roland, J.; Barter, D.M.; Johnston, H.L.; Czaja, C.A.; Kayalioglu, H.; et al. The landscape of candidemia during the COVID-19 pandemic. Clin. Infect. Dis. 2021, ciab562.
- Kayaaslan, B.; Eser, F.; Kaya Kalem, A.; Bilgic, Z.; Asilturk, D.; Hasanoglu, I.; Ayhan, M.; Tezer Tekce, Y.; Erdem, D.; Turan, S.; et al. Characteristics of candidemia in COVID-19 patients; increased incidence, earlier occurrence and higher mortality rates compared to non-COVID-19 patients. Mycoses 2021, 64, 1083–1091.
- Nucci, M.; Barreiros, G.; Guimarães, L.F.; Deriquehem, V.A.S.; Castiñeiras, A.C.; Nouér, S.A. Increased incidence of candidemia in a tertiary care hospital with the COVID-19 pandemic. Mycoses 2021, 64, 152–156.
- Awada, B.; Alam, W.; Chalfoun, M.; Araj, G.; Bizri, A.R. COVID-19 and Candida duobushaemulonii superinfection: A case report. J. Med. Mycol. 2021, 31, 101168.
- Posteraro, B.; Torelli, R.; Vella, A.; Leone, P.M.; De Angelis, G.; De Carolis, E.; Ventura, G.; Sanguinetti, M.; Fantoni, M. Pan-Echinocandin-Resistant Candida glabrata Bloodstream Infection Complicating COVID-19: A Fatal Case Report. J. Fungi 2020, 6, 163.
- De Almeida, J.N.; Brandão, I.B.; Francisco, E.C.; Almeida, S.L.R.; Oliveira Dias, P.; Pereira, F.M.; Santos Ferreira, F.; Andrade, T.S.; Miranda Costa, M.M.; Souza Jordão, R.T.; et al. Axillary Digital Thermometers uplifted a multidrug-susceptible Candida auris outbreak among COVID-19 patients in Brazil. Mycoses 2021, 64, 1062–1072.
- Hanson, B.M.; Dinh, A.Q.; Tran, T.T.; Arenas, S.; Pronty, D.; Gershengorn, H.B.; Ferreira, T.; Arias, C.A.; Shukla, B.S. Candida auris Invasive Infections During a COVID-19 Case Surge. Antimicrob. Agents Chemother. 2021, AAC-01146.
- Steele, E.J.; Gorczynski, R.M.; Lindley, R.A.; Tokoro, G.; Temple, R.; Wickramasinghe, N.C. Origin of new emergent Coronavirus and Candida fungal diseases—Terrestrial or cosmic? Cosm. Genet. Evol. 2020, 106, 75–100.
- Rodrigues, C.; Rodrigues, M.; Silva, S.; Henriques, M. Candida glabrata Biofilms: How Far Have We Come? J. Fungi 2017, 3, 11.
- Chowdhary, A.; Sharma, C.; Meis, J.F. Candida auris: A rapidly emerging cause of hospital-acquired multidrug-resistant fungal infections globally. PLOS Pathog. 2017, 13, e1006290.
- Di Pilato, V.; Codda, G.; Ball, L.; Giacobbe, D.R.; Willison, E.; Mikulska, M.; Magnasco, L.; Crea, F.; Vena, A.; Pelosi, P.; et al. Molecular Epidemiological Investigation of a Nosocomial Cluster of C. auris: Evidence of Recent Emergence in Italy and Ease of Transmission during the COVID-19 Pandemic. J. Fungi 2021, 7, 140.
- Prestel, C.; Anderson, E.; Forsberg, K.; Lyman, M.; de Perio, M.A.; Kuhar, D.; Edwards, K.; Rivera, M.; Shugart, A.; Walters, M.; et al. Candida auris Outbreak in a COVID-19 Specialty Care Unit—Florida, July–August 2020. MMWR. Morb. Mortal. Wkly. Rep. 2021, 70, 56–57.
- Macauley, P.; Epelbaum, O. Epidemiology and Mycology of Candidaemia in non-oncological medical intensive care unit patients in a tertiary center in the United States: Overall analysis and comparison between non-COVID-19 and COVID-19 cases. Mycoses 2021, 64, 634–640.
- Koehler, P.; Bassetti, M.; Chakrabarti, A.; Chen, S.C.; Colombo, A.L.; Hoenigl, M.; Klimko, N.; Lass-Flörl, C.; Oladele, R.O.; Vinh, D.C.; et al. Defining and managing COVID-19-associated pulmonary aspergillosis: The 2020 ECMM/ISHAM consensus criteria for research and clinical guidance. Lancet. Infect. Dis. 2021, 21, e149–e162.
- Nasrullah, A.; Javed, A.; Malik, K. Coronavirus Disease-Associated Pulmonary Aspergillosis: A Devastating Complication of COVID-19. Cureus 2021, 31, e13004.
- Arastehfar, A.; Carvalho, A.; van de Veerdonk, F.L.; Jenks, J.D.; Koehler, P.; Krause, R.; Cornely, O.A.; Perlin, D.S.; Lass-Flörl, C.; Hoenigl, M. COVID-19 Associated Pulmonary Aspergillosis (CAPA)—From Immunology to Treatment. J. Fungi 2020, 6, 91.
- Dupont, D.; Menotti, J.; Turc, J.; Miossec, C.; Wallet, F.; Richard, J.-C.; Argaud, L.; Paulus, S.; Wallon, M.; Ader, F.; et al. Pulmonary aspergillosis in critically ill patients with Coronavirus Disease 2019 (COVID-19). Med. Mycol. 2020, 59, 110–114.
- Wu, S.; Yang, S.; Chen, R.; Chen, H.; Xu, Y.; Lin, B. Dynamic Immune Response Profiles and Recovery of a COVID-19 Patient with Coinfection of Aspergillus fumigatus and Other Baseline Diseases: A Case Report. OMICS A J. Integr. Biol. 2020, 24, 615–618.
- Armstrong-James, D.; Youngs, J.; Bicanic, T.; Abdolrasouli, A.; Denning, D.W.; Johnson, E.; Mehra, V.; Pagliuca, T.; Patel, B.; Rhodes, J.; et al. Confronting and mitigating the risk of COVID-19 associated pulmonary aspergillosis. Eur. Respir. J. 2020, 56, 2002554.
- Brown, L.-A.K.; Ellis, J.; Gorton, R.; De, S.; Stone, N. Surveillance for COVID-19-associated pulmonary aspergillosis. Lancet Microbe 2020, 1, e152.
- Schein, F.; Munoz-Pons, H.; Mahinc, C.; Grange, R.; Cathébras, P.; Flori, P. Fatal aspergillosis complicating severe SARS-CoV-2 infection: A case report. J. Mycol. Med. 2020, 30, 101039.
- De Lamballerie, C.N.; Pizzorno, A.; Fouret, J.; Szpiro, L.; Padey, B.; Dubois, J.; Julien, T.; Traversier, A.; Dulière, V.; Brun, P.; et al. Transcriptional Profiling of Immune and Inflammatory Responses in the Context of SARS-CoV-2 Fungal Superinfection in a Human Airway Epithelial Model. Microorganisms 2020, 8, 1974.
- Wheat, L.J.; Azar, M.M.; Bahr, N.C.; Spec, A.; Relich, R.F.; Hage, C. Histoplasmosis. Infect. Dis. Clin. North Am. 2016, 30, 207–227.
- Azar, M.M.; Hage, C.A. Clinical Perspectives in the Diagnosis and Management of Histoplasmosis. Clin. Chest Med. 2017, 38, 403–415.
- Basso, R.P.; Poester, V.R.; Benelli, J.L.; Stevens, D.A.; Zogbi, H.E.; da Vasconcellos, I.C.S.; Pasqualotto, A.C.; Xavier, M.O. COVID-19 associated histoplasmosis in an AIDS patient. Mycopathologia 2020, 186, 109–112.
- De Macedo, P.M.; Freitas, A.D.; Bártholo, T.P.; Bernardes-Engemann, A.R.; de Abreu Almeida, M.; Almeida-Silva, F.; Zancopé-Oliveira, R.M.; Almeida-Paes, R. Acute Pulmonary Histoplasmosis Following COVID-19: Novel Laboratorial Methods Aiding Diagnosis. J. Fungi 2021, 7, 346.
- Stasiak, C.E.S.; Nigri, D.H.; Cardoso, F.R.; de Almeida Rezende d Mattos, R.S.; Martins, P.A.G.; Carvalho, A.R.S.; de Almeida, S.A.; Rodrigues, R.S.; Rosado-de-Castro, P.H. Case Report: Incidental Finding of COVID-19 Infection after Positron Emission Tomography/CT Imaging in a Patient with a Diagnosis of Histoplasmosis and Recurring Fever. Am. J. Trop. Med. Hyg. 2021, 104, 1651–1654.
- Bertolini, M.; Mutti, M.F.; Barletta, J.A.E.; Falak, A.; Cuatz, D.; Sisto, A.; Ragusa, M.A.; Claros, N.O.F.; Rolón, M.J. COVID-19 associated with AIDS-related disseminated histoplasmosis: A case report. Int. J. STD AIDS 2020, 31, 1222–1224.
- Chakrabarti, A.; Denning, D.W.; Ferguson, B.J.; Ponikau, J.; Buzina, W.; Kita, H.; Marple, B.; Panda, N.; Vlaminck, S.; Kauffmann-Lacroix, C.; et al. Fungal rhinosinusitis. Laryngoscope 2009, 119, 1809–1818.
- Ferguson, B.J. Definitions of fungal rhinosinusitis. Otolaryngol. Clin. North Am. 2000, 33, 227–235.
- Hallur, V.; Prakash, H.; Sable, M.; Preetam, C.; Purushotham, P.; Senapati, R.; Shankarnarayan, S.A.; Bag, N.D.; Rudramurthy, S.M. Cunninghamella arunalokei a New Species of Cunninghamella from India Causing Disease in an Immunocompetent Individual. J. Fungi 2021, 7, 670.
- Scheckenbach, K.; Cornely, O.; Hoffmann, T.K.; Engers, R.; Bier, H.; Chaker, A.; Greve, J.; Schipper, J.; Wagenmann, M. Emerging therapeutic options in fulminant invasive rhinocerebral mucormycosis. Auris Nasus Larynx 2010, 37, 322–328.
- Vairaktaris, E.; Moschos, M.M.; Vassiliou, S.; Baltatzis, S.; Kalimeras, E.; Avgoustidis, D.; Pappas, Z.; Moschos, M.N. Orbital cellulitis, orbital subperiosteal and intraorbital abscess. Report of three cases and review of the literature. J. Cranio-Maxillofac. Surg. 2009, 37, 132–136.
- Mohindra, S.; Mohindra, S.; Gupta, R.; Bakshi, J.; Gupta, S.K. Rhinocerebral mucormycosis: The disease spectrum in 27 patients. Mycoses 2007, 50, 290–296.
- Munir, N.; Jones, N.S. Rhinocerebral mucormycosis with orbital and intracranial extension: A case report and review of optimum management. J. Laryngol. Otol. 2006, 121, 192–195.
- Deshazo, R.D. Fungal Sinusitis. Am. J. Med. Sci. 1998, 316, 39–45.
- Ballester, D.G.; González-García, R.; García, C.M.; Ruiz-Laza, L.; Gil, F.M. Mucormycosis of the head and neck: Report of five cases with different presentations. J. Cranio-Maxillofac. Surg. 2012, 40, 584–591.
- Chen, N.; Zhou, M.; Dong, X.; Qu, J.; Gong, F.; Han, Y.; Qiu, Y.; Wang, J.; Liu, Y.; Wei, Y.; et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A descriptive study. Lancet 2020, 395, 507–513.
- Yang, X.; Yu, Y.; Xu, J.; Shu, H.; Xia, J.; Liu, H.; Wu, Y.; Zhang, L.; Yu, Z.; Fang, M.; et al. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: A single-centered, retrospective, observational study. Lancet Respir. Med. 2020, 8, 475–481.
- Hanley, B.; Naresh, K.N.; Roufosse, C.; Nicholson, A.G.; Weir, J.; Cooke, G.S.; Thursz, M.; Manousou, P.; Corbett, R.; Goldin, R.; et al. Histopathological findings and viral tropism in UK patients with severe fatal COVID-19: A post-mortem study. Lancet Microbe 2020, 1, e245–e253.
- Werthman-Ehrenreich, A. Mucormycosis with orbital compartment syndrome in a patient with COVID-19. Am. J. Emerg. Med. 2021, 42, 264.e5–264.
- Mehta, S.; Pandey, A. Rhino-Orbital Mucormycosis Associated with COVID-19. Cureus 2020, 12, e10726.
- Do Monte Junior, E.S.; dos Santos, M.E.L.; Ribeiro, I.B.; de Oliveira Luz, G.; Baba, E.R.; Hirsch, B.S.; Funari, M.P.; de Moura, E.G.H. Rare and Fatal Gastrointestinal Mucormycosis (Zygomycosis) in a COVID-19 Patient: A Case Report. Clin. Endosc. 2020, 53, 746–749.
- Placik, D.A.; Taylor, W.L.; Wnuk, N.M. Bronchopleural fistula development in the setting of novel therapies for acute respiratory distress syndrome in SARS-CoV-2 pneumonia. Radiol. Case Rep. 2020, 15, 2378–2381.
- Mekonnen, Z.K.; Ashraf, D.C.; Jankowski, T.; Grob, S.R.; Vagefi, M.R.; Kersten, R.C.; Simko, J.P.; Winn, B.J. Acute Invasive Rhino-Orbital Mucormycosis in a Patient with COVID-19-Associated Acute Respiratory Distress Syndrome. Ophthalmic Plast. Reconstr. Surg. 2020, 37, e40–e80.
- Pasero, D.; Sanna, S.; Liperi, C.; Piredda, D.; Pietro Branca, G.; Casadio, L.; Simeo, R.; Buselli, A.; Rizzo, D.; Bussu, F.; et al. A challenging complication following SARS-CoV-2 infection: A case of pulmonary mucormycosis. Infection 2020, 1–6.
- Garg, D.; Muthu, V.; Sehgal, I.S.; Ramachandran, R.; Kaur, H.; Bhalla, A.; Puri, G.D.; Chakrabarti, A.; Agarwal, R. Coronavirus Disease (Covid-19) Associated Mucormycosis (CAM): Case Report and Systematic Review of Literature. Mycopathologia 2021, 186, 289–298.
- Saldanha, M.; Reddy, R.; Vincent, M.J. Title of the Article: Paranasal Mucormycosis in COVID-19 Patient. Indian J. Otolaryngol. Head Neck Surg. 2021, 1–4.
- Krishna, D.S.; Raj, H.; Kurup, P.; Juneja, M. Maxillofacial Infections in Covid-19 Era—Actuality or the Unforeseen: 2 Case Reports. Indian J. Otolaryngol. Head Neck Surg. 2021, 1–4.
- Selarka, L.; Sharma, A.K.; Rathod, G.; Saini, D.; Patel, S.; Sharma, V.K. Mucormycosis—A Dreaded Complication of Covid-19. QJM An Int. J. Med. 2021, hcab166.
- Johnson, A.K.; Ghazarian, Z.; Cendrowski, K.D.; Persichino, J.G. Pulmonary aspergillosis and mucormycosis in a patient with COVID-19. Med. Mycol. Case Rep. 2021, 32, 64–67.
- Waizel-Haiat, S.; Guerrero-Paz, J.A.; Sanchez-Hurtado, L.; Calleja-Alarcon, S.; Romero-Gutierrez, L. A Case of Fatal Rhino-Orbital Mucormycosis Associated with New Onset Diabetic Ketoacidosis and COVID-19. Cureus 2021, 13, e13163.
- Topcu, O.; Ozaslan, M.; Kılıc, İ.H.; Oguzkan, S.B.; Kurt, B.S.; Cay, M.; Tonus, S.S.; Bayram, A. Susceptibility of severe COVID-19 patients to rhino-orbital mucormycosis fungal infection in different clinical manifestations. Jpn. J. Ophthalmol. 2021, 65, 515–525.
- Fouad, Y.A.; Abdelaziz, T.T.; Askoura, A.; Saleh, M.I.; Mahmoud, M.S.; Ashour, D.M.; Ashour, M.M. Spike in Rhino-Orbital-Cerebral Mucormycosis Cases Presenting to a Tertiary Care Center During the COVID-19 Pandemic. Front. Med. 2021, 8, 645270.
- Zurl, C.; Hoenigl, M.; Schulz, E.; Hatzl, S.; Gorkiewicz, G.; Krause, R.; Eller, P.; Prattes, J. Autopsy Proven Pulmonary Mucormycosis Due to Rhizopus microsporus in a Critically Ill COVID-19 Patient with Underlying Hematological Malignancy. J. Fungi 2021, 7, 88.
- Moorthy, A.; Gaikwad, R.; Krishna, S.; Hegde, R.; Tripathi, K.K.; Kale, P.G.; Rao, P.S.; Haldipur, D.; Bonanthaya, K. SARS-CoV-2, Uncontrolled Diabetes and Corticosteroids—An Unholy Trinity in Invasive Fungal Infections of the Maxillofacial Region? A Retrospective, Multi-centric Analysis. J. Maxillofac. Oral Surg. 2021, 20, 418–425.
- Pakdel, F.; Ahmadikia, K.; Salehi, M.; Tabari, A.; Jafari, R.; Mehrparvar, G.; Rezaie, Y.; Rajaeih, S.; Alijani, N.; Barac, A.; et al. Mucormycosis in patients with COVID-19: A cross-sectional descriptive multicenter study from Iran. Mycoses 2021.
- Veisi, A.; Bagheri, A.; Eshaghi, M.; Rikhtehgar, M.H.; Kanavi, M.R.; Farjad, R. Rhino-orbital mucormycosis during steroid therapy in COVID-19 patients: A case report. Eur. J. Ophthalmol. 2021, 112067212110094.
- Alekseyev, K.; Didenko, L.; Chaudhry, B. Rhinocerebral Mucormycosis and COVID-19 Pneumonia. J. Med. Cases 2021, 12, 85–89.
- Ashour, M.M.; Abdelaziz, T.T.; Ashour, D.M.; Askoura, A.; Saleh, M.I.; Mahmoud, M.S. Imaging spectrum of acute invasive fungal rhino-orbital-cerebral sinusitis in COVID-19 patients: A case series and a review of literature. J. Neuroradiol. 2021, in press.
- Revannavar, S.M.; Supriya, S.P.; Samaga, L.; Vineeth, V.K. COVID-19 triggering mucormycosis in a susceptible patient: A new phenomenon in the developing world? BMJ Case Rep. 2021, 14, e241663.
- Maini, A.; Tomar, G.; Khanna, D.; Kini, Y.; Mehta, H.; Bhagyasree, V. Sino-orbital mucormycosis in a COVID-19 patient: A case report. Int. J. Surg. Case Rep. 2021, 82, 105957.
- Buil, J.B.; van Zanten, A.R.H.; Bentvelsen, R.G.; Rijpstra, T.A.; Goorhuis, B.; van der Voort, S.; Wammes, L.J.; Janson, J.A.; Melchers, M.; Heusinkveld, M.; et al. Case series of four secondary mucormycosis infections in COVID-19 patients, the Netherlands, December 2020 to May 2021. Eurosurveillance 2021, 26, 2100510.
- Arana, C.; Ramirez, R.E.C.; Xipell, M.; Casals, J.; Moreno, A.; Herrera, S.; Bodro, M.; Cofan, F.; Diekmann, F.; Esforzado, N. Mucormycosis associated with COVID-19 in two kidney transplant~patients. Transpl. Infect. Dis. 2021, e13652.
- Sharma, S.; Grover, M.; Bhargava, S.; Samdani, S.; Kataria, T. Post coronavirus disease mucormycosis: A deadly addition to the pandemic spectrum. J. Laryngol. Otol. 2021, 135, 442–447.
- Honavar, S.; Sen, M.; Lahane, S.; Lahane, T.; Parekh, R. Mucor in a Viral Land: A Tale of Two Pathogens. Indian J. Ophthalmol. 2021, 69, 244.
- Karimi-Galougahi, M.; Arastou, S.; Haseli, S. Fulminant mucormycosis complicating coronavirus disease 2019 (COVID-19). Int. Forum Allergy Rhinol. 2021, 11, 1029–1030.
- Kanwar, A.; Jordan, A.; Olewiler, S.; Wehberg, K.; Cortes, M.; Jackson, B.R. A Fatal Case of Rhizopus azygosporus Pneumonia Following COVID-19. J. Fungi 2021, 7, 174.
- Khatri, A.; Chang, K.-M.; Berlinrut, I.; Wallach, F. Mucormycosis after Coronavirus disease 2019 infection in a heart transplant recipient—Case report and review of literature. J. Med. Mycol. 2021, 31, 101125.
- Nehara, H.R.; Puri, I.; Singhal, V.; IH, S.; Bishnoi, B.R.; Sirohi, P. Rhinocerebral mucormycosis in COVID-19 patient with diabetes a deadly trio: Case series from the north-western part of India. Indian J. Med. Microbiol. 2021, 39, 180–383.
- Khatib, M.; Ahmed, A.; Shaat, S.; soliman Mohamed, A.; Nashwan, A. Cryptococcemia in a Patient with COVID-19: A Case Report. Clin. Case Rep. 2020, 9, 853–855.
- Passarelli, V.C.; Perosa, A.H.; de Souza Luna, L.K.; Conte, D.D.; Nascimento, O.A.; Ota-Arakaki, J.; Bellei, N. Detected SARS-CoV-2 in Ascitic Fluid Followed by Cryptococcemia: A Case Report. Compr. Clin. Med. 2020, 2, 2414–2418.
- Gonzalez, A.J.C.; Montenegro-Idrogo, J.J.; Vadillo, A.R.V.; Torres, M.S.; Matos, I.V.; Delgado, C.P.R. Hospital-acquired SARS-CoV-2 pneumonia in a person living with HIV. Int. J. 2020, 31, 1320–1322.
- Passerini, M.; Terzi, R.; Piscaglia, M.; Passerini, S.; Piconi, S. Disseminated Cryptococcosis in a Patient with Metastatic Prostate Cancer Who Died in the Coronavirus Disease 2019 (COVID-19) Outbreak. Cureus 2020, 12, e8254.
- Krauth, D.S.; Jamros, C.M.; Rivard, S.C.; Olson, N.H.; Maves, R.C. Accelerated Progression of Disseminated Coccidioidomycosis Following SARS-CoV-2 Infection: A Case Report. Mil. Med. 2021, usab132.
- Chang, C.C.; Senining, R.; Kim, J.; Goyal, R. An Acute Pulmonary Coccidioidomycosis Coinfection in a Patient Presenting with Multifocal Pneumonia with COVID-19. J. Investig. Med. High Impact Case Rep. 2020, 8, 232470962097224.
- Cai, S.; Sun, W.; Li, M.; Dong, L. A complex COVID-19 case with rheumatoid arthritis treated with tocilizumab. Clin. Rheumatol. 2020, 39, 2797–2802.
- Menon, A.A.; Berg, D.D.; Brea, E.J.; Deutsch, A.J.; Kidia, K.K.; Thurber, E.G.; Polsky, S.B.; Yeh, T.; Duskin, J.A.; Holliday, A.M.; et al. A Case of COVID-19 and Pneumocystis jirovecii Coinfection. Am. J. Respir. Crit. Care Med. 2020, 202, 136–138.
- Alanio, A.; Dellière, S.; Voicu, S.; Bretagne, S.; Mégarbane, B. The presence of Pneumocystis jirovecii in critically ill patients with COVID-19. J. Infect. 2021, 82, 84–123.
- Coleman, H.; Snell, L.B.; Simons, R.; Douthwaite, S.T.; Lee, M.J. Coronavirus disease 2019 and Pneumocystis jirovecii pneumonia: A diagnostic dilemma in HIV. AIDS 2020, 34, 1258–1260.
- Kelly, S.; Waters, L.; Cevik, M.; Collins, S.; Lewis, J.; Wu, M.-S.; Blanchard, T.J.; Geretti, A.M. Pneumocystispneumonia, a COVID-19 mimic, reminds us of the importance of HIV testing in COVID-19. Clin. Med. 2020, 20, 590–592.
- Mang, S.; Kaddu-Mulindwa, D.; Metz, C.; Becker, A.; Seiler, F.; Smola, S.; Maßmann, A.; Becker, S.L.; Papan, C.; Bals, R.; et al. Pneumocystis jirovecii Pneumonia and Severe Acute Respiratory Syndrome Coronavirus 2 Coinfection in a Patient with Newly Diagnosed HIV-1 Infection. Clin. Infect. Dis. 2020, 72, 1487–1489.
- Viceconte, G.; Buonomo, A.R.; Lanzardo, A.; Pinchera, B.; Zappulo, E.; Scotto, R.; Moriello, N.S.; Vargas, M.; Iacovazzo, C.; Servillo, G.; et al. Pneumocystis jirovecii pneumonia in an immunocompetent patient recovered from COVID-19. Infect. Dis. 2021, 53, 382–385.
- Jeican, I.I.; Inișca, P.; Gheban, D.; Tuaran, F.; Aluaș, M.; Trombitas, V.; Cristea, V.; Crivii, C.; Junie, L.M.; Albu, S. COVID-19 and Pneumocystis jirovecii Pulmonary Coinfection—The First Case Confirmed through Autopsy. Medicina 2021, 57, 302.
- Ventoulis, I.; Sarmourli, T.; Amoiridou, P.; Mantzana, P.; Exindari, M.; Gioula, G.; Vyzantiadis, T.A. Bloodstream Infection by Saccharomyces cerevisiae in Two COVID-19 Patients after Receiving Supplementation of Saccharomyces in the ICU. J. Fungi 2020, 6, 98.
- Poignon, C.; Blaize, M.; Vezinet, C.; Lampros, A.; Monsel, A.; Fekkar, A. Invasive pulmonary fusariosis in an immunocompetent critically ill patient with severe COVID-19. Clin. Microbiol. Infect. 2020, 26, 1582–1584.





