Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Fumihiko Urabe | + 923 word(s) | 923 | 2021-08-23 10:58:17 | | | |
| 2 | Rita Xu | -24 word(s) | 899 | 2021-08-24 05:29:02 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Urabe, F. ABO Blood Type. Encyclopedia. Available online: https://encyclopedia.pub/entry/13481 (accessed on 13 March 2026).
Urabe F. ABO Blood Type. Encyclopedia. Available at: https://encyclopedia.pub/entry/13481. Accessed March 13, 2026.
Urabe, Fumihiko. "ABO Blood Type" Encyclopedia, https://encyclopedia.pub/entry/13481 (accessed March 13, 2026).
Urabe, F. (2021, August 23). ABO Blood Type. In Encyclopedia. https://encyclopedia.pub/entry/13481
Urabe, Fumihiko. "ABO Blood Type." Encyclopedia. Web. 23 August, 2021.
Copy Citation
Venous thromboembolism, which includes both deep venous thrombosis and pulmonary embolism, is a major cause of morbidity and mortality among patients with cancer. The impact of ABO blood type in the development of venous thromboembolism in cancer patients remains controversial. To develop a sense of current opinion in this area, we conducted a systematic review and meta-analysis. Blood type is routinely determined preoperatively by objective and standardized methods, and our results suggest that these blood type results are useful for risk stratification and potentially for encouraging appropriate strategies for implementation of prophylactic treatment strategy in venous thromboembolism management.
ABO blood type
venous thromboembolism
meta-analysis
1. Introduction
Venous thromboembolism, which includes both deep venous thrombosis and pulmonary embolism, is a major cause of morbidity and mortality among patients with cancer [1][2]. In particular, venous thromboembolism is a serious and frequent complication of pelvic surgery for malignancy and is the most common cause of mortality in patients who die within 30 days after surgery [3][4].
Although our references reported several types of genetic predisposition to venous thromboembolism, such as single-nucleotide polymorphisms (SNPs), most of those variations were encountered so rarely that their clinical importance remains controversial [5]. It is thus important to characterize predisposing factors for venous thromboembolism, so that risk can be stratified accurately and prophylactic treatment strategies can be implemented effectively.
Previous hematologic studies have reported that ABO blood type is a significant genetic risk factor for venous thromboembolism [6][7]. Specifically, among the four blood groups (A, B, AB, and O), the risk of venous thromboembolism has been found to be significantly higher for non-O blood types than for type O [6][7]. However, no systematic assessment has been conducted of the relationship between blood type and venous thromboembolism risk in patients with cancer.
2. Study Selection
We found a total of 598 studies for an initial assessment. From these, we removed 40 duplicates and excluded non-relevant studies, review articles, meeting abstracts, case reports, replies, editorials or commentaries, and studies in languages other than English. This left 40 studies for review, from which we identified nine studies for systematic review [8][9][10][11][12][13][14][15][16] and five studies [9][10][12][13][14] for qualitative meta-analysis (Figure 1).
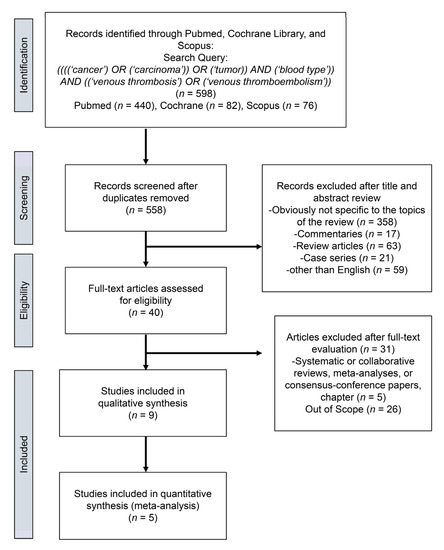
Figure 1. Preferred Reporting Items from the Systematic Review and Meta-Analysis (PRISMA) flow chart showing the process of article selection.
3. Characteristics of the Included Studies
Table 1 lists the general characteristics of the eligible studies. All studies had a retrospective design and were published between 2004 and 2020. Patients were enrolled from Europe in 1 study, from North America in 7 studies, and from Asia in 1 study. Overall, 1118 of 25,884 patients developed venous thromboembolism. The treatment details were reported for seven studies in 24,996 patients: 24,473 of those patients (97.9%) underwent a surgical procedure (biopsy or surgical resection). The rate of development of venous thromboembolism in patients whose blood type was O and non-O was 9.2% and 13.6%, respectively. All of the eligible studies were retrospective, so pharmacologic prophylaxis was not standardized. In addition, the timing of diagnostic evaluation of patients for venous thromboembolism was based on symptom presentation and/or clinical evaluation, and most of the studies did not follow a precise protocol. Multivariate logistic regression analyses were not performed in three studies [8][11][15], and although Wang et al. evaluated the association of venous thromboembolism with ABO blood type, they reported a higher risk of each non-O blood type (A/B/AB) compared to O blood type (OR (95% CI); A: 2.072 (1.204–3.566), B: 1.944 (1.020–3.873), AB: 2.706 (1.432–5.114)). These four studies were excluded from our meta-analysis.
Table 1. Characteristics of all articles included in the study.
| VTE | |||||||
|---|---|---|---|---|---|---|---|
| First Author of Study and [Ref.] | Country | Recruitment Period | Study Design | Total | Yes | No | NOS |
| Streiff et al. [8] | USA | 1991–2001 | Cohort, retrospective | 130 | 28 | 102 | 6 |
| Tollefson et al. [9] | USA | 1987–2010 | Cohort, retrospective | 18472 | 271 | 18201 | 7 |
| Wang J et al. [10] | USA | 1980–2005 | Cohort, retrospective | 2076 | 216 | 2060 | 7 |
| Mizrahi et al. [11] | Canada | 1995–2013 | Cohort, retrospective | 523 | 56 | 467 | 6 |
| Li et al. [12] | USA | NR | Cohort, retrospective | 670 | 236 | 434 | 6 |
| Spavor et al. [13] | Canada | NR | Cohort, retrospective | 218 | 63 | 155 | 6 |
| Bhanvadia et al. [14] | USA | 2003–2015 | Cohort, retrospective | 1341 | 90 | 1251 | 7 |
| Heenkenda et al. [15] | Sweden | NR | Cohort, retrospective | 139 | 47 | 92 | 6 |
| Wang G et al. [16] | China | 2018–2019 | Cohort, retrospective | 2315 | 131 | 2174 | 7 |
NOS, Newcastle-Ottawa Scale; VTE, venous thromboembolism; NR, not reported.
4. Meta-Analysis
The association of ABO blood type with development of venous thromboembolism in patients with cancers.
The impact of ABO blood type on the development of venous thromboembolism was investigated in five studies, in a total of 22,777 patients with cancer. The Cochrane Q test (chi-square 1.86, p = 0.761) and the I2 test (I2 = 0.0%) showed no heterogeneity, so we used a fixed-effect model. The forest plots indicated a significant association between non-O blood type and the development of venous thromboembolism (pooled OR: 1.74, 95% CI, 1.44–2.10, z = 5.70, Figure 2A). The funnel plots showed no studies exceeding the pseudo 95% CI (Figure 2B).
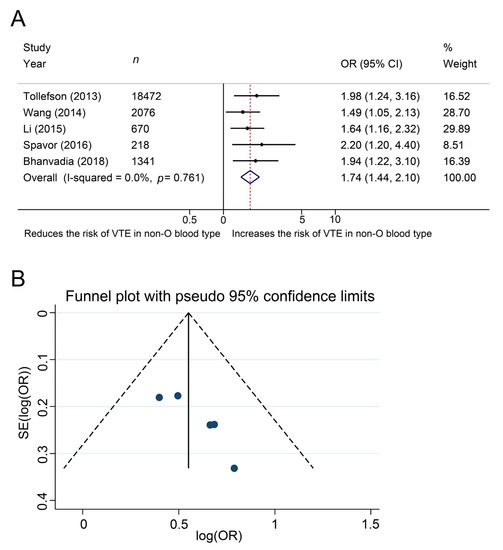
Figure 2. Forest (A) and funnel (B) plot showing the association of ABO blood type with the development of venous thromboembolism among patients with cancer.
5. Additional Analysis
The association of ABO blood type with the development of venous thromboembolism in patients after pelvic surgery for malignancy.
The effects of ABO blood type on the development of venous thromboembolism was investigated in three studies, in a total of 21,889 patients with cancer after pelvic surgery. The Cochrane Q test (chi-square 1.24, p = 0.537) and the I2 test (I2 = 0.0%) showed no heterogeneity, so we used a fixed-effect model. The forest plots demonstrated that non-O blood type was significantly associated with the development of venous thromboembolism (pooled OR: 1.73, 95% CI, 1.36–2.20, z = 4.43, Figure 3A). The funnel plots did not demonstrate any study over the pseudo 95% CI (Figure 3B).
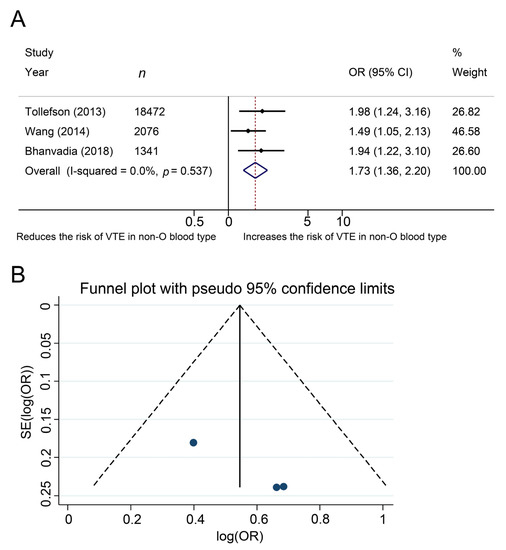
Figure 3. Forest (A) and funnel (B) plot showing the association of ABO blood type with the development of venous thromboembolism among patients who underwent pelvic surgery for urological cancer.
References
- Park, B.; Messina, L.; Dargon, P.; Huang, W.; Ciocca, R.; Anderson, F.A. Recent trends in clinical outcomes and resource utilization for pulmonary embolism in the United States: Findings from the nationwide inpatient sample. Chest 2009, 136, 983–990.
- Nakchbandi, I.A.; Löhr, J.-M. Coagulation, anticoagulation and pancreatic carcinoma. Nat. Clin. Pract. Gastroenterol. Hepatol. 2008, 5, 445–455.
- Agnelli, G.; Bolis, G.; Capussotti, L.; Scarpa, R.M.; Tonelli, F.; Bonizzoni, E.; Moia, M.; Rossi, R.; Sonaglia, F.; Valarani, B.; et al. A clinical outcome-based prospective study on venous thromboembolism in cancer surgery: The @RISTOS project. Ann. Surg. 2006, 243, 89–95.
- Van Hemelrijck, M.; Garmo, H.; Holmberg, L.; Bill-Axelson, A.; Carlsson, S. Thromboembolic events following surgery for prostate cancer. Eur. Urol. 2013, 63, 354–363.
- Heit, J.A.; Cunningham, J.M.; Petterson, T.M.; Armasu, S.M.; Rider, D.N.; De Andrade, M. Genetic variation within the anticoagulant, procoagulant, fibrinolytic and innate immunity pathways as risk factors for venous thromboembolism. J. Thromb. Haemost. 2011, 9, 1133–1142.
- Dentali, F.; Sironi, A.P.; Ageno, W.; Turato, S.; Bonfanti, C.; Frattini, F.; Crestani, S.; Franchini, M. Non-O blood type is the commonest genetic risk factor for VTE: Results from a meta-analysis of the literature. Semin. Thromb. Hemost. 2012, 38, 535–548.
- Kabrhel, C.; Varraso, R.; Kraft, P.; Rimm, E.B.; Goldhaber, S.Z.; Camargo, C.; Fuchs, C.S.; Wolpin, B.M. Prospective study of ABO blood type and the risk of pulmonary embolism in two large cohort studies. Thromb. Haemost. 2010, 104, 962–971.
- Streiff, M.B.; Segal, J.; Grossman, S.A.; Kickler, T.S.; Weir, E.G. ABO blood group is a potent risk factor for venous thromboembolism in patients with malignant gliomas. Cancer 2004, 100, 1717–1723.
- Tollefson, M.K.; Karnes, R.J.; Rangel, L.; Carlson, R.; Boorjian, S.A. Blood type, lymphadenectomy and blood transfusion predict venous thromboembolic events following radical prostatectomy with pelvic lymphadenectomy. J. Urol. 2014, 191, 646–651.
- Wang, J.K.; Boorjian, S.A.; Frank, I.; Tarrell, R.F.; Thapa, P.; Jacob, E.K.; Tauscher, C.D.; Tollefson, M.K. Non-O blood type is associated with an increased risk of venous thromboembolism after radical cystectomy. Urology 2014, 83, 140–145.
- Mizrahi, T.; Leclerc, J.-M.; David, M.; Ducruet, T.; Robitaille, N. ABO group as a thrombotic risk factor in children with acute lymphoblastic leukemia: A retrospective study of 523 pediatric patients. Blood 2013, 122, 2370.
- Li, D.; Pise, M.N.; Overman, M.J.; Liu, C.; Tang, H.; Vadhan-Raj, S.; Abbruzzese, J.L. ABO non-O type as a risk factor for thrombosis in patients with pancreatic cancer. Cancer Med. 2015, 4, 1651–1658.
- Spavor, M.; Halton, J.; Dietrich, K.; Israels, S.; Shereck, E.; Yong, J.; Yasui, Y.; Mitchell, L.G. Age at cancer diagnosis, non-O blood group and asparaginase therapy are independently associated with deep venous thrombosis in pediatric oncology patients: A risk model. Thromb. Res. 2016, 144, 27–31.
- Bhanvadia, S.; Kazerouni, K.; Bazargani, S.T.; Miranda, G.; Cai, J.; Daneshmand, S.; Djaladat, H. Validating the role of ABO blood type in risk of perioperative venous thromboembolism after radical cystectomy. World J. Urol. 2018, 37, 173–179.
- Heenkenda, M.K.; Malmström, A.; Lysiak, M.; Mudaisi, M.; Bratthäll, C.; Milos, P. Assessment of genetic and non-genetic risk factors for venous thromboembolism in glioblastoma—The predictive significance of B blood group. Thromb. Res. 2019, 183, 136–142.
- Wang, G.; Wang, H.; Shen, Y.; Dong, J.; Wang, X.; Wang, X.; Zheng, Y.; Guo, S. Association between ABO blood group and venous thrombosis related to the peripherally inserted central catheters in cancer patients. J. Vasc. Access 2020, 2020.
More
Information
Subjects:
Urology & Nephrology
Contributor
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
956
Revisions:
2 times
(View History)
Update Date:
24 Aug 2021
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





