
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Elena Jane Mason | + 1520 word(s) | 1520 | 2021-02-19 10:47:39 | | | |
| 2 | Vicky Zhou | Meta information modification | 1520 | 2021-02-22 03:58:47 | | |
Video Upload Options
Breast-conserving surgery’s main goal is to fully remove the tumor with clear margins, while avoiding resection of healthy breast tissue in order to achieve better cosmetic results.
1. Introduction
Breast cancer (BC) is the most commonly diagnosed cancer and the leading cause of cancer-related death among women [1]. A successful BC treatment is based on a multidisciplinary use of surgery, chemotherapy and radiation therapy, with surgery as the central component of treatment for early-stage breast cancer [2][3]. Breast-conserving surgery (BCS) followed by adjuvant radiotherapy, known as breast conservation therapy (BCT), has become the alternative treatment to mastectomy for early stage breast cancer because of equivalent survival and lower morbidity [4][5][6].
Local recurrence after BCS is strongly correlated to the surgical margin status, as demonstrated by a large number of follow-up studies [7][8][9][10][11]. The main goal of BCS is to fully remove the tumor with clear margins, while avoiding resection of healthy breast tissue in order to achieve better cosmetic results. Image-guided preoperative localization is mandatory for guiding surgery of non-palpable lesions or surgically relevant extension of palpable lesions to improve both oncological and cosmetic outcomes [12][13]. Over the last decade, methods for preoperative localization of breast lesions for BCS have evolved rapidly due to innovative techniques and discovery of novel agents. However, cooperation and communication between breast surgeons and radiologists still play a crucial role.
Different image guided localization techniques are variably used in different institutions depending on personal choices, skills and available technologies. As a general rule, the method chosen should be the most precise to localize the lesion or marker left after biopsy, thus improving free margin rates and decreasing operative time, and possibly cause little to no discomfort to the patient. Preoperative breast lesions localization techniques currently available are wire localization, carbon marking, radio-guided occult lesion localization (ROLL), radioactive seed localization (RSL), magnetic seed localization and non-radioactive radar localization, intraoperative ultrasound and preoperative skin tattoo localization (Table 1). In this article, we provide an overview of current literature of all commercially available techniques. The aim of this review is to educate practicing radiologists and breast surgeons so they can knowingly select new techniques to improve patient care.
Table 1. Comparison of different localization techniques. Abbreviations: ROLL = radio-guided occult lesion localization; RSL = radioactive seed localization; Magseed = magnetic seed localization; IOUS = intraoperative ultrasound; Skin tattoo = preoperative localization with skin tattoo; OR = operating room; US = ultrasound; MRI = magnetic resonance imaging. * Success is defined as removal of target lesion. ** Authors’ experience.
| Technique | Materials/Procedures | Advantages | Disadvantages | Success * Rate | Clear Margins Rate |
|---|---|---|---|---|---|
| Wire localization | Wire Preloaded needle introducer |
Simple Cost-effective Different kinds of image-guidance |
Wire migration Scheduling difficulties Limits surgical decisions |
97.5% [14] | 70.8–87.4% [15] |
| Carbon marking | Diluted charcoal powder | Simple Different kinds of image-guidance Cost-effective Cannot dislodge Scheduling flexibility |
Carbon can distort or obscure lesion Unfit for large breasts Unfit for multifocal or extensive lesions |
99% [16] | 61–85% [17][18] |
| ROLL | Nuclear radiotracer Technetium 99 Gamma ray probe |
Different kinds of image-guidance Does not limit surgeon |
Scheduling difficulties Radiation Cost |
95–99% [19] | 92% [20][21] |
| RSL | Iodine 125 seed Preloaded needle introducer Gamma probe set for I-125 |
Scheduling flexibility Does not limit surgeon Different kinds of image-guidance |
Radiation Not repositionable after deployment |
100% [22][23] | 73.5–96.7% [22][23] |
| Magseed | Paramagnetic seed Preloaded needle introducer |
Scheduling flexibility No radiation Does not limit surgeon |
Cost Not repositionable after deployment Non magnetizable surgical equipment MRI artifacts |
99.86% [24][25][26][27] | 88.75% [24] |
| Radiofrequency identification tags | Radiofrequency reflector Needle introducer Detector |
Scheduling flexibility No radiation Does not limit surgeon |
Cost Depth limit Not repositionable after deployment Interference with halogen lights in the OR |
97–100% [28][29] | 85–100% [28][29][30] |
| IOUS | Portable or OR-stationed US machine and sterile transducer cover | Scheduling flexibility No radiation Does not limit surgeon Non-invasive |
Unemployable in US-invisible lesions Surgeon learning curve Interference with air during dissection |
100% [31][32][33][34][35] | 81–97% [32][34] |
| Skin tattoo | Dermographic marker Lead markers |
Simple and safe Cost-effective Non-invasive Different kinds of image-guidance Does not limit surgeon |
Scheduling difficulties Inability to depict marker |
99.5% ** | 95.9% ** |
2. Preoperative Localization with a Skin Tattoo
Preoperative localization with a skin tattoo is a simple and safe technique amply utilized in our centre, as it is easily performed, extremely well tolerated by patients and effective in terms of successful excision and clear margin rates. This method can be carried out by acquiring either sonographic or mammographic images, depending on the type of lesion, but ultrasounds are employed whenever possible because the procedure is easier. In this case, patients lie in the supine position with their arms extended to mimic the position held during surgery. The tumor is located, and its distance from the skin surface is measured taking care not to apply pressure with the probe, so as to report accurately the depth of the tumor in relation to the skin surface [36]. The distance between the lesion, the nipple and the pectoralis major muscle is also measured, as is the distance between separate lesions in case of multifocal or multicentric disease [37][38]. Radiologists with experience in this technique visualize the tumors at their largest diameter to achieve the optimal correspondence between the lesion and the skin markers. The tumor’s projection on the skin surface is pinpointed with a dermographic skin marker and the drawing is covered to avoid accidental erasure (Figure 1). The whole procedure, performed by an experienced radiologist, takes 5–10 min and provides minimum patient discomfort. Limitations include poor results in case of sonographically invisible lesions, microcalcifications or biopsy markers, but are easily overcome by implementing this technique with a mammographic approach. Stereotactic-guided skin marking is also a non-invasive technique, albeit it provides a little more discomfort to the patient due to breast compression. Mammograms are acquired in double projection and measurements are performed on the images to determine the distance between the lesion and the nipple, the skin surface and the fascia.
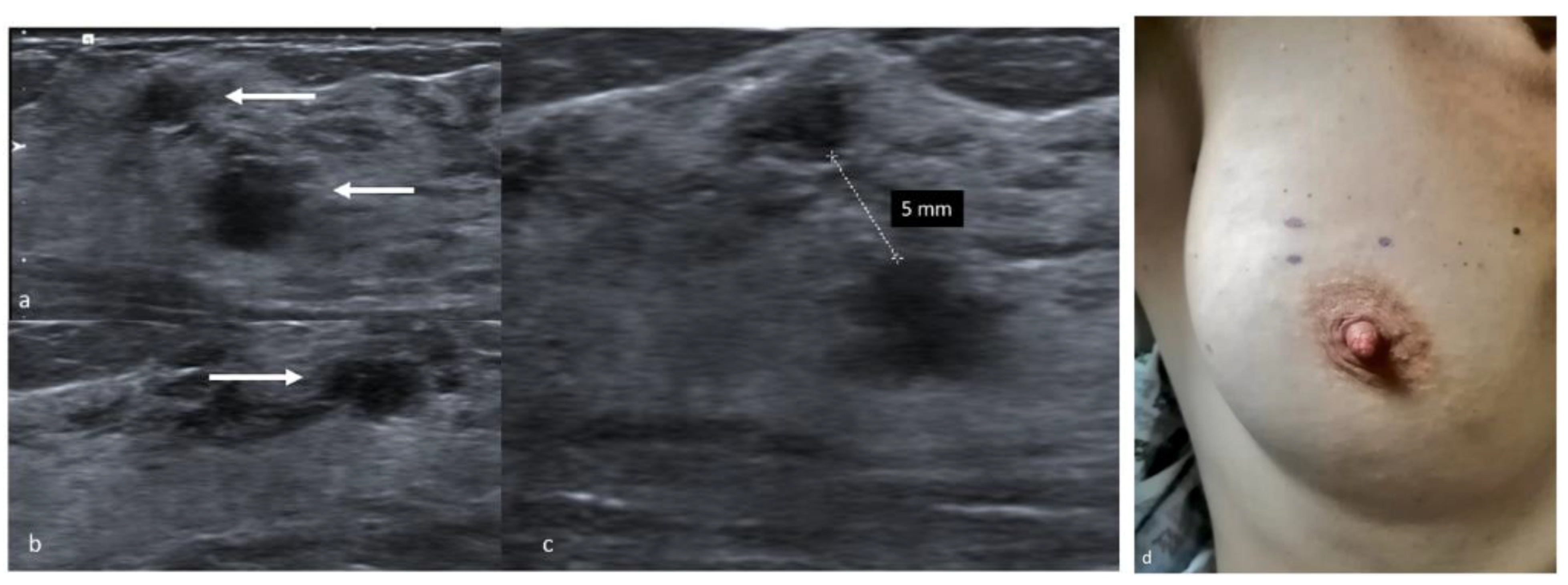
The radiologist then estimates the projection of the tumor on the skin surface and positions a lead marker in the corresponding spot. In case of bigger lesions, such as extensive microcalcifications, or multifocal disease, multiple lead markers can be employed to determine lesion margins. A second stereotactic pair of images is acquired to confirm the correct localization, and in case of inaccurate positioning, the lead markers can be repositioned more accurately and confirmed by a further mammogram [39] (Figure 2). At the end of the procedure the lead markers are removed, and the skin tattoo is drawn in their place. In the operating room, the mark is exposed and retraced with a specific marker resistant to antiseptic solutions, and painting and draping procedures are carried out carefully without wiping out the ink. Our centre strongly advocates pursuit of the maximum aesthetic result achievable with oncological safety, and because this localization technique employs only a temporary skin tattoo, the surgeon is granted total liberty in choice of incision and oncoplastic technique. The skin flap is dissected in the direction of the tattoo, then the incision is deepened and a lumpectomy is carried out taking into account tumor depth measured during the preoperative localization. In some cases, a non-palpable lesion becomes palpable after dissection of the skin flap, allowing the surgeon to easily complete the excision, however in most cases the excision has to be conducted by reassessing the original position of the skin mark from time to time. Once the excision is completed, metallic clips are placed on the orienting sutures in different numbers, so as to recognize margins in the specimen X-ray. The sample is then placed into a transparent plastic bag and sent to the Radiology Department, and mammograms are acquired in double projection. The tumor is usually visible as a radiopaque nodule, and its position inside the lumpectomy specimen is described as either well centered or close to one or more surgical margins, and reported to the operating surgeon. In dense, glandular specimens the nodule can be difficult to distinguish from the surrounding mammary parenchyma: in these cases, the exam can be completed with a specimen ultrasound [40] (Figure 3). If close margins are detected in either technique the surgeon can acquire further cavity shave margins on the affected border.
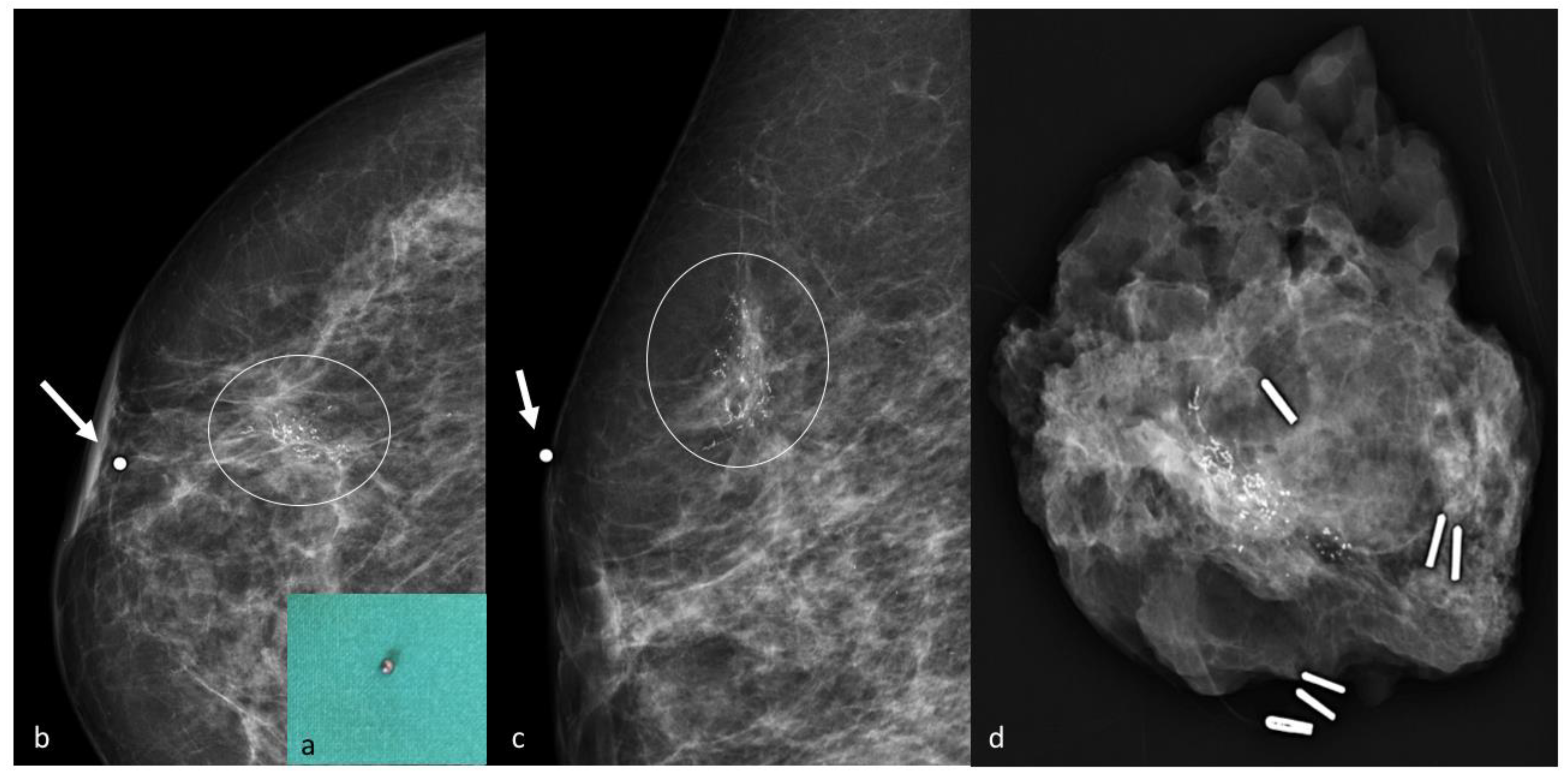
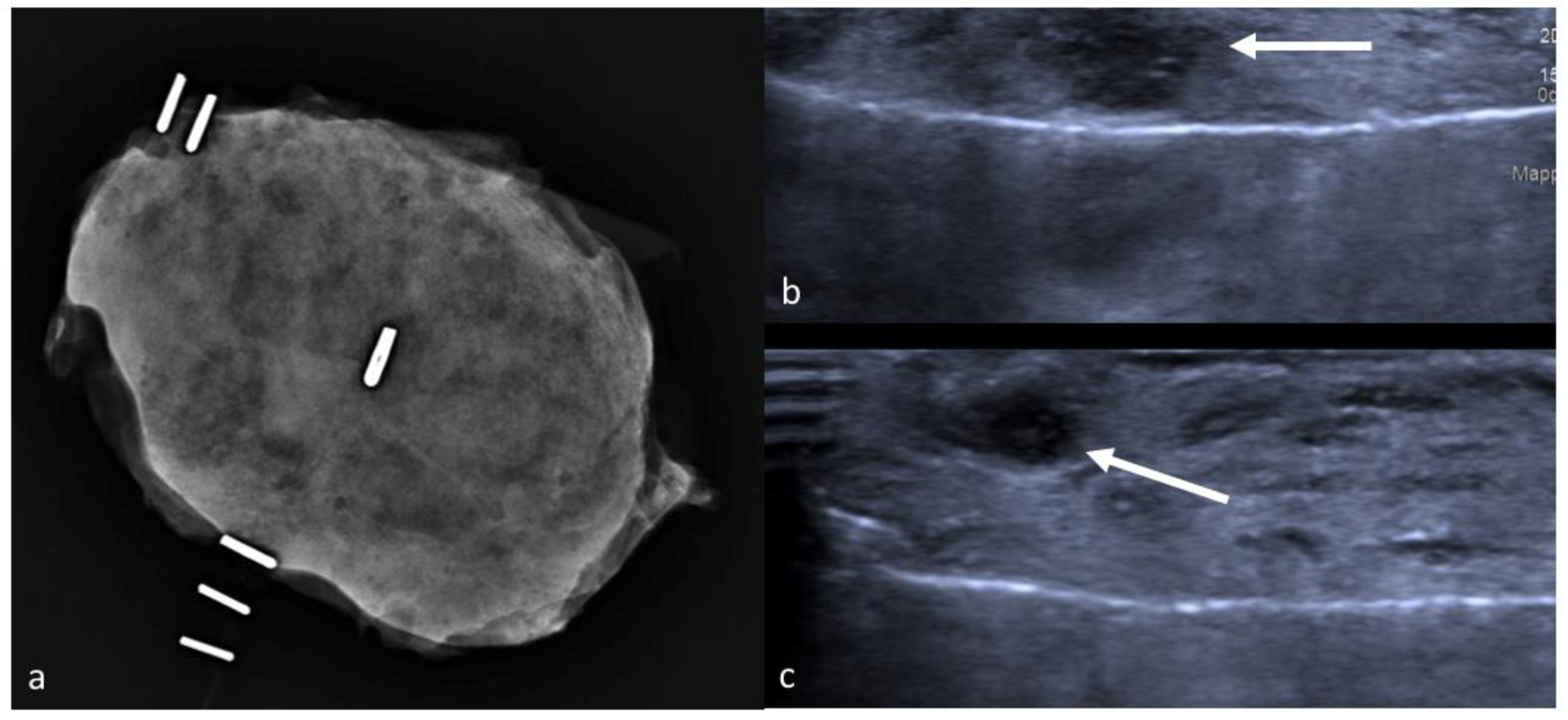
This technique is quick, easily performed by breast radiologists and extremely cost-effective. It does not require equipment that is not normally present in any breast surgery department, and is therefore feasible even with scarce resources. Limitations include accurate scheduling to time the procedure before surgery thus avoiding accidental mark erasure, and a certain degree of experience by the surgeon in reassessing the tumor’s position based on the skin mark during dissection. Reports on this technique are widely deficient in the literature, however a preliminary analysis of the data from our high-volume centre examining the outcome of 199 lumpectomies performed for non-palpable breast tumors between August and December 2019 identified a global success rate of 99.5% (198/199) and a clear margins rate of 95.9% (192/199). As these rates did not differ significantly from other localization techniques, this method appears safe and especially ideal in the case of limited resources or spending reviews.
References
- Sharma, R. Breast cancer incidence, mortality and mortality-to-incidence ratio (MIR) are associated with human development, 1990–2016: Evidence from Global Burden of Disease Study 2016. Breast Cancer 2019, 26, 428–445.
- Moo, T.-A.; Sanford, R.; Dang, C.; Morrow, M. Overview of breast cancer therapy. PET Clin. 2018, 13, 339–354.
- Franceschini, G.; Terribile, D.; Fabbri, C.; Magno, S.; D’Alba, P.; Chiesa, F.; Di Leone, A.; Masetti, R. Management of locally advanced breast cancer. Mini-review. Minerva Chir. 2007, 62, 249–255. Available online: http://europepmc.org/abstract/MED/17641585 (accessed on 8 November 2020).
- Fisher, B.; Anderson, S.; Bryant, J.; Margolese, R.G.; Deutsch, M.; Fisher, E.R.; Jeong, J.-H.; Wolmark, N. Twenty-year follow-up of a randomized trial comparing total mastectomy, lumpectomy, and lumpectomy plus irradiation for the treatment of invasive breast cancer. N. Engl. J. Med. 2002, 347, 1233–1241.
- Veronesi, U.; Cascinelli, N.; Mariani, L.; Greco, M.; Saccozzi, R.; Luini, A.; Aguilar, M.; Marubini, E. Twenty-year follow-up of a randomized study comparing breast-conserving surgery with radical mastectomy for early breast cancer. N. Engl. J. Med. 2002, 347, 1227–1232.
- Sanchez, A.M.; Franceschini, G.; D’Archi, S.; De Lauretis, F.; Scardina, L.; Di Giorgio, D.; Accetta, C.; Masetti, R. Results obtained with level II oncoplastic surgery spanning 20 years of breast cancer treatment: Do we really need further demonstration of reliability? Breast J. 2020, 26, 125–132.
- Peterson, M.E.; Schultz, D.J.; Reynolds, C.; Solin, L.J. Outcomes in breast cancer patients relative to margin status after treatment with breast-conserving surgery and radiation therapy: The University of Pennsylvania experience. Int. J. Radiat. Oncol. Biol. Phys. 1999, 43, 1029–1035.
- Singletary, S.E. Surgical margins in patients with early-stage breast cancer treated with breast conservation therapy. Am. J. Surg. 2002, 184, 383–393.
- Corsi, F.; Sorrentino, L.; Bossi, D.; Sartani, A.; Foschi, D. preoperative localization and surgical margins in conservative breast surgery. Int. J. Surg. Oncol. 2013, 2013, 793819.
- Park, C.C.; Mitsumori, M.; Nixon, A.; Recht, A.; Connolly, J.; Gelman, R.; Silver, B.; Hetelekidis, S.; Abner, A.; Harris, J.R.; et al. Outcome at 8 years after breast-conserving surgery and radiation therapy for invasive breast cancer: Influence of margin status and systemic therapy on local recurrence. J. Clin. Oncol. 2000, 18, 1668–1675.
- Franceschini, G.; Sanchez, A.M.; Di Leone, A.; Magno, S.; Moschella, F.; Accetta, C.; Natale, M.; Di Giorgio, D.; Scaldaferri, A.; D’Archi, S.; et al. Update on the surgical management of breast cancer. Ann. Ital. Chir. 2015, 86, 89–99.
- Hayes, M.K. Update on preoperative breast localization. Radiol. Clin. N. Am. 2017, 55, 591–603.
- Jeffries, D.O.; Dossett, L.A.; Jorns, J.M. Localization for breast surgery: The next generation. Arch. Pathol. Lab. Med. 2017, 141, 1324–1329.
- Jackman, R.J.; Marzoni, F.A. Needle-localized breast biopsy: Why do we fail? Radiology 1997, 204, 677–684.
- Bick, U.; Trimboli, R.M.; Athanasiou, A.; Balleyguier, C.; Baltzer, P.A.T.; Bernathova, M.; Borbély, K.; Brkljacic, B.; Carbonaro, L.A.; Clauser, P.; et al. Image-guided breast biopsy and localisation: Recommendations for information to women and referring physicians by the European Society of Breast Imaging. Insights Imaging 2020, 11, 1–18.
- Riedl, C.C.; Pfarl, G.; Helbich, T.H.; Memarsadeghi, M.; Wagner, T.; Rudas, M.; Fuchsjäger, M. Comparison of wire versus carbon localization of non-palpable breast lesions. RöFo 2002, 174, 1126–1131.
- Rose, A.; Collins, J.; Neerhut, P.; Bishop, C.; Mann, G.B. Carbon localisation of impalpable breast lesions. Breast 2003, 12, 264–269.
- Tran, Q.; Mizumoto, R.; Tran, M.; Reintals, M.; Gounder, V. Carbon-track localisation as an adjunct to wire-guided excision of impalpable breast lesions: A retrospective cohort study. Int. J. Surg. Open 2019, 21, 7–11.
- Öcal, K.; Dag, A.; Turkmenoglu, M.O.; Günay, E.C.; Yûcel, E.; Duce, M.N. Radioguided occult lesion localization versus wire-guided localization for non-palpable breast lesions: Randomized controlled trial. Clinics 2011, 66, 1003–1007.
- De Cicco, C.; Pizzamiglio, M.; Trifirò, G.; Luini, A.; Ferrari, M.; Prisco, G.; Galimberti, V.; Cassano, E.; Viale, G.; Intra, M.; et al. Radioguided occult lesion localisation (ROLL) and surgical biopsy in breast cancer. Technical aspects. Q. J. Nucl. Med. 2002, 46, 145–151.
- Luini, A.; Zurrida, S.; Paganelli, G.; Galimberti, V.; Sacchini, V.; Monti, S.; Veronesi, P.; Viale, G. Comparison of radioguided excision with wire localization of occult breast lesions. BJS 1999, 86, 522–525.
- Gray, R.J.; Salud, C.; Nguyen, K.; Dauway, E.; Friedland, J.; Berman, C.; Peltz, E.; Whitehead, G.; Cox, C.E. Randomized prospective evaluation of a novel technique for biopsy or lumpectomy of nonpalpable breast lesions: Radioactive seed versus wire localization. Ann. Surg. Oncol. 2001, 8, 711–715.
- Rao, R.; Moldrem, A.; Sarode, V.; White, J.; Amen, M.; Rao, M.; Andrews, V.; Euhus, D.; Radford, L.; Ulissey, M. Experience with seed localization for nonpalpable breast lesions in a public health care system. Ann. Surg. Oncol. 2010, 17, 3241–3246.
- Gera, R.; Tayeh, S.; Al-Reefy, S.; Mokbel, K. Evolving role of magseed in wireless localization of breast lesions: Systematic review and pooled analysis of 1,559 procedures. Anticancer. Res. 2020, 40, 1809–1815.
- Endomag. Available online: https://www.endomag.com/ (accessed on 11 November 2020).
- Zacharioudakis, K.; Down, S.; Bholah, Z.; Lee, S.; Khan, T.; Howe, M.; Maxwell, A.; Harvey, J. Is the future magnetic? Magseed localisation of non palpable breast cancer—A multicentre comparative cohort study. Breast 2019, 44, S112.
- Thekkinkattil, D.; Kaushik, M.; Hoosein, M.; Al-Attar, M.; Pilgrim, S.; Gvaramadze, A.; Hyklova, L.; Jibril, A. A prospective, single-arm, multicentre clinical evaluation of a new localisation technique using non-radioactive Magseeds for surgery of clinically occult breast lesions. Clin. Radiol. 2019, 74, 974.e7–974.e11.
- Mango, V.L.; Wynn, R.T.; Feldman, S.; Friedlander, L.; Desperito, E.; Patel, S.N.; Gomberawalla, A.; Ha, R. Beyond wires and seeds: Reflector-guided breast lesion localization and excision. Radiology 2017, 284, 365–371.
- Mango, V.; Ha, R.; Gomberawalla, A.; Wynn, R.; Feldman, S. Evaluation of the SAVI SCOUT surgical guidance system for localization and excision of nonpalpable breast lesions: A feasibility study. Am. J. Roentgenol. 2016, 207, W69–W72.
- Cox, C.E.; Garcia-Henriquez, N.; Glancy, M.J.; Whitworth, P.; Cox, J.M.; Themar-Geck, M.; Prati, R.; Jung, M.; Russell, S.; Appleton, K.; et al. Pilot study of a new nonradioactive surgical guidance technology for locating nonpalpable breast lesions. Ann. Surg. Oncol. 2016, 23, 1824–1830.
- Jadeja, P.H.; Mango, V.; Patel, S.; Friedlander, L.; Desperito, E.; Ayala-Bustamante, E.; Wynn, R.; Chen-Seetoo, M.; Taback, B.; Feldman, S.; et al. Utilization of multiple SAVI SCOUT surgical guidance system reflectors in the same breast: A single-institution feasibility study. Breast J. 2018, 24, 531–534.
- Colakovic, N.; Zdravkovic, D.; Skuric, Z.; Mrda, D.; Gacic, J.; Ivanovic, N. Intraoperative ultrasound in breast cancer surgery—from localization of non-palpable tumors to objectively measurable excision. World J. Surg. Oncol. 2018, 16, 1–7.
- Haid, A.; Knauer, M.; Dunzinger, S.; Jasarevic, Z.; Köberle-Wührer, R.; Schuster, A.; Toeppker, M.; Haid, B.; Wenzl, E.; Offner, F. Intra-operative sonography: A valuable aid during breast-conserving surgery for occult breast cancer. Ann. Surg. Oncol. 2007, 14, 3090–3101.
- Fortunato, L.; Penteriani, R.; Farina, M.; Vitelli, C.E.; Piro, F. Intraoperative ultrasound is an effective and preferable technique to localize non-palpable breast tumors. Eur. J. Surg. Oncol. (EJSO) 2008, 34, 1289–1292.
- Ramos, M.; Díaz, J.C.; Ramos, T.; Ruano, R.; Aparicio, M.; Sancho, M.; González-Orús, J.M. Ultrasound-Guided Excision Combined with Intraoperative Assessment of Gross Macroscopic Margins Decreases the Rate of Reoperations for Non-Palpable Invasive Breast Cancer. Breast 2012, 22, 520–524. Available online: https://www.unboundmedicine.com/medline/citation/23110817/Ultrasound_guided_excision_combined_with_intraoperative_assessment_of_gross_macroscopic_margins_decreases_the_rate_of_reoperations_for_non_palpable_invasive_breast_cancer_ (accessed on 30 October 2020).
- Carlino, G.; Rinaldi, P.; Giuliani, M.; Rella, R.; Bufi, E.; Padovano, F.; Ciardi, C.; Romani, M.; Belli, P.; Manfredi, R. Ultrasound-guided preoperative localization of breast lesions: A good choice. J. Ultrasound 2019, 22, 85–94.
- Volders, J.H.; Haloua, M.H.; Krekel, N.M.A.; Meijer, S.; Van Den Tol, P.M. Current status of ultrasound-guided surgery in the treatment of breast cancer. World J. Clin. Oncol. 2016, 7, 44–53.
- Franceschini, G.; Visconti, G.; Sanchez, A.M.; Di Leone, A.; Salgarello, M.; Masetti, R. Oxidized regenerated cellulose in breast surgery: Experimental model. J. Surg. Res. 2015, 198, 237–244.
- Madeley, C.; Kessell, M.; Madeley, C.; Taylor, D.B. A comparison of stereotactic and tomosynthesis-guided localisation of impalpable breast lesions. J. Med. Radiat. Sci. 2019, 66, 170–176.
- Fusco, R.; Petrillo, A.; Catalano, O.; Sansone, M.; Granata, V.; Filice, S.; D’Aiuto, M.; Pankhurst, Q.; Douek, M. Procedures for location of non-palpable breast lesions: A systematic review for the radiologist. Breast Cancer 2012, 21, 522–531.





