Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Nevin Varghese | -- | 1928 | 2024-02-21 04:35:44 | | | |
| 2 | Rita Xu | Meta information modification | 1928 | 2024-02-21 08:34:51 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Varghese, N.; Majeed, A.; Nyalakonda, S.; Boortalary, T.; Halegoua-Demarzio, D.; Hann, H. Hepatitis B Virus-Associated Hepatocellular Carcinoma. Encyclopedia. Available online: https://encyclopedia.pub/entry/55259 (accessed on 24 May 2026).
Varghese N, Majeed A, Nyalakonda S, Boortalary T, Halegoua-Demarzio D, Hann H. Hepatitis B Virus-Associated Hepatocellular Carcinoma. Encyclopedia. Available at: https://encyclopedia.pub/entry/55259. Accessed May 24, 2026.
Varghese, Nevin, Amry Majeed, Suraj Nyalakonda, Tina Boortalary, Dina Halegoua-Demarzio, Hie-Won Hann. "Hepatitis B Virus-Associated Hepatocellular Carcinoma" Encyclopedia, https://encyclopedia.pub/entry/55259 (accessed May 24, 2026).
Varghese, N., Majeed, A., Nyalakonda, S., Boortalary, T., Halegoua-Demarzio, D., & Hann, H. (2024, February 21). Hepatitis B Virus-Associated Hepatocellular Carcinoma. In Encyclopedia. https://encyclopedia.pub/entry/55259
Varghese, Nevin, et al. "Hepatitis B Virus-Associated Hepatocellular Carcinoma." Encyclopedia. Web. 21 February, 2024.
Copy Citation
Hepatitis B virus (HBV) affects around 300 million people worldwide and is a significant risk factor for the development of hepatocellular carcinoma (HCC). Nucleos(t)ide analog therapy has aided in decreasing mortality from HBV.
hepatitis B virus
hepatocellular carcinoma
nucleoside analog
1. Introduction
Hepatitis B virus (HBV) is a global public health problem with an estimated 350 million chronic hepatitis B carriers, causing 820,000 deaths in 2019 alone [1][2][3]. HBV is endemic in many parts of the world, including Southeast Asia, China, and Africa [4]. It belongs to a family of DNA viruses called hepadnaviruses, which is composed of at least ten genotypes, A–J [2][5][6]. The virion is an enveloped nucleocapsid that delivers an incomplete circular DNA genome into the host cell, initiating viral replication [7]. HBV is a dynamic, hepatotropic virus and its infection has a wide spectrum of clinical manifestations [7]. Fifteen–forty percent of HBV-infected patients develop cirrhosis, liver failure, or hepatocellular carcinoma (HCC) [1][8]. In fact, HBV is the most common hepatocarcinogen, being accountable for 25% of HCC cases in developed countries and 60% in developing countries [9][10][11][12].
2. HBV Pathophysiology and Hepatocarcinogenesis
HBV is transmitted by percutaneous inoculation or transmission of infectious bodily fluids. In high-prevalence areas, mother-to-child transmission is the predominant mode of transmission, while unprotected sex and injection drug use are the common modes of transmission in low-prevalence areas [13][14]. The incubation period of HBV is between 30 and 180 days. During infection, complete and incomplete viral particles are released into the serum of the host, facilitating viral replication [15].
HBV is a non-cytopathic virus, and the liver damage associated with HBV is caused by the host immune response [16][17]. During acute infection, host immune cells, most prominently CD8 T cells, kill infected cells, inducing hepatic inflammation [4][18]. Around 70% of patients with acute HBV have subclinical or anicteric hepatitis, while 30% have icteric hepatitis [19]. The clearance of HBV is mediated by the adaptive immune system and HBV utilizes multiple strategies to evade this line of defense [19][20][21]. The hypo-responsiveness of HBV-specific T cells may also contribute to persistent HBV infection [21]. While recovery commonly occurs in immunocompetent individuals, a small proportion of those infected can progress to chronic HBV infection, which is defined as the presence of HBsAg for greater than six months [22].
There are four phases of chronic hepatitis B (CHB) infection: immune tolerance, immune clearance, immune control, and immune escape/reactivation [23]. In the immune tolerance phase, ALT levels are still low, viral DNA levels are high (usually at least 2,000,000 IU/mL), and there is minimal or no inflammation on liver biopsy [4][18][23][24][25][26]. This phase may last for a few years to around 30 years [27][28]. In the immune clearance phase, hepatitis B e antigen (HBeAg) is positive, there is intermittent or persistent elevation of ALT levels, elevated HBV DNA levels (at least 2000 IU/mL), and some degree of inflammation or fibrosis on liver biopsy [23][28]. In this phase, HBV-specific CD8 T cells directly attack infected hepatocytes and recruit other immune cells to the liver, which further exacerbate hepatic injury [4][17][18][26][29]. During immune clearance, patients may present with flares, which—while often being asymptomatic—may be characterized by signs of acute hepatitis. During flares, ALT levels may be elevated to greater than five times the upper limit of normal [23][30]. The end of the immune clearance phase and beginning of immune control is marked by seroconversion, which is the loss of HBeAg and development of antibodies to hepatitis B e antigen (HBeAb). Intriguingly, the duration of the immune clearance phase has a critical association with the development of complications; those who seroconvert after the age of 40 have a significantly higher risk of cirrhosis, HCC, and CHB compared to those who seroconverted before the age of 30 [23][31]. In addition, HBeAg positivity is a known risk factor for HCC [26][32]. The immune control phase is characterized by lower levels of HBV DNA (usually <2000 IU/mL) and ALT, although HBsAg remains [4][18][23]. Some patients, even after seroconversion, may continue to have moderate levels of viral replication with associated abnormal ALT, leading to eventual reactivation of the immune active phase; this phenomenon is known as immune escape [23][28][33][34]. Resolution of infection is indicated by disappearance of HBsAg [4][18].
In CHB, there are crucial changes in immune cell activity and function involving both the innate and adaptive immune systems that lead to hepatic inflammation and hepatocyte killing [17]. Chronic infection may progress to liver fibrosis, cirrhosis, and HCC [17][35]. HBV-mediated carcinogenesis is a complex process that involves viral DNA integration into the host genome, ultimately leading to viral manipulation of cell-signaling and proliferation. This leads to a cascade of events which converts normal hepatocytes into malignant cells [36][37][38][39]. Oxidative stress associated with viral hepatitis changes the cellular environment in such a way that promotes carcinogenesis. Overproduction of free radicals and reactive oxidative species leads to the upregulation of inflammatory pathways that result in hepatocyte release of cytokines and chemokines that recruit neutrophils, monocytes, and lymphocytes [18][37][40][41]. As inflammation persists, immune cells, including macrophages and myeloid-derived suppressor cells, become dysfunctional, further amplifying the pro-inflammatory environment. The chronic inflammatory state leads to compensatory hepatocyte proliferation, which leads to accumulation of mutations that promote cell growth and proliferation which predisposes the host to developing HCC (Figure 1) [40][42].
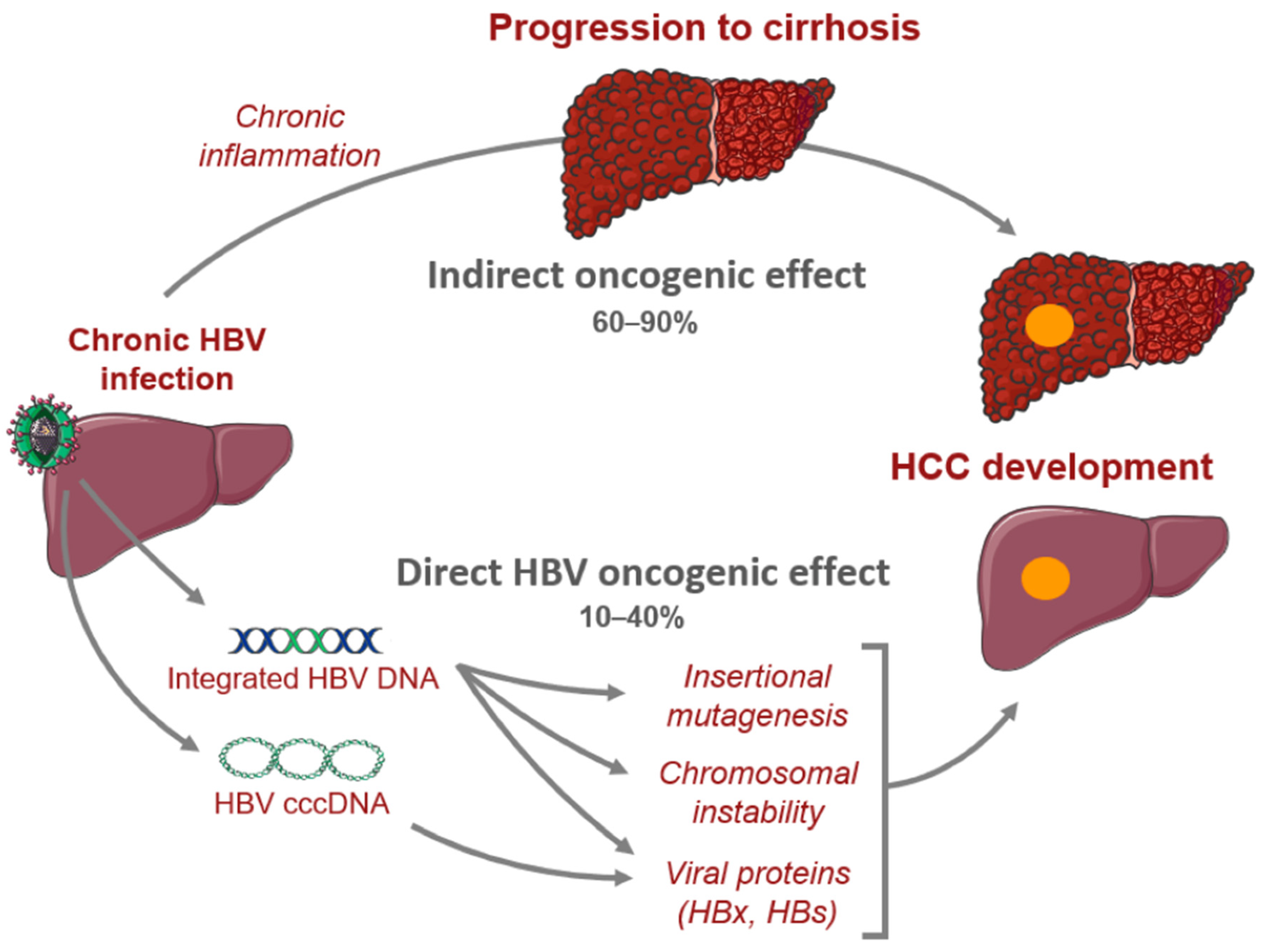
Figure 1. Mechanisms of hepatocarcinogenesis from chronic hepatitis B infection.
Moreover, it was found that the incidence of HCC is fivefold higher among HBV-infected patients with cirrhosis compared to asymptomatic carriers, indicating that cirrhosis may be a pre-malignant condition [38]. Indeed, fibrosis of the liver disrupts the normal architecture which leads to modification of cell–cell interactions and ultimately, loss of regulation over cell proliferation [38].
Furthermore, it is important to note that numerous factors including host characteristics, HBV genotype, viral mutations, viral load, and HBsAg levels all influence the clinical manifestations of HBV infection [6]. Research has shown that there are differences between the various genotypes of HBV in tendency of chronicity, primary mode of transmission, timing of seroconversion, timing of HBsAg clearance, and clinical outcomes [6]. For example, multiple studies have shown that genotype C tends to cause more severe liver disease, including cirrhosis and HCC, compared to other genotypes [6][43][44]. Genotype C also has higher serum HBV levels and was shown to cause DNA mutations more frequently than Genotype B [6][45]. Further research investigating the utility of routine HBV genotyping is needed before implementation into clinical practice.
3. HCC Risk Factors and Surveillance
HCC is one of the major malignant diseases in the world today and ranks fifth in overall frequency. Its incidence is high in Eastern Asia and sub-Saharan Africa and is increasing in many parts of the Western world [46]. Among cancers, the annual mortality from HCC is relatively high because of its rapid progression and poor prognosis. Unfortunately, the diagnosis is typically made later in its course when therapeutic interventions are generally ineffective. Thus, the focus has been on early screening and treatment of known causes, including chronic hepatitis B which is the most frequent underlying cause of HCC. There are several major risk factors for development of HCC in chronic HBV infection. While having a first-degree relative with HCC, metabolic syndrome, type 2 diabetes, and central obesity are all host factors that have been linked to HCC development in HBV-infected patients or carriers, it appears that liver cirrhosis has been consistently identified to be the most significant risk factor for development of HCC during nucleos(t)ide therapy [47][48][49][50][51]. Notably, there is increasing evidence that non-alcoholic fatty liver disease (NAFLD) is becoming one of the largest causes of HCC, particularly in industrialized countries [52]. In these patients, HCC can develop even in the absence of cirrhosis. As there are no specific pharmacological therapies for NAFLD, adoption of healthy lifestyle changes including weight loss and regular aerobic physical activity remain the mainstay treatment. Interestingly, bariatric surgery is known to provide durable weight loss and has been identified to be associated with a decreased risk of HCC. A meta-analysis involving nearly 20 million patients showed that bariatric surgery has a protective effect on risk of HCC occurrence and incidence compared to those subjects who did not undergo the procedure [53]. Studies indicate that the presence of male gender, increasing age, higher HBV DNA level, and core promoter mutations are also independently associated with HCC risk [54][55]. It is postulated that androgens may play a role in the observed difference in incidence of HCC based on gender [56]. Among patients with chronic hepatitis B infection treated with nucleos(t)ide therapy, those with hepatitis D coinfection have been shown to have a nearly sixfold risk of HCC development compared to patients without hepatitis D coinfection [57]. While less investigated, concurrent HCV or HIV infection has also been identified to have an association with increased incidence of HCC [58][59]. The risk factors for hepatocarcinogenesis can be seen in Figure 2.
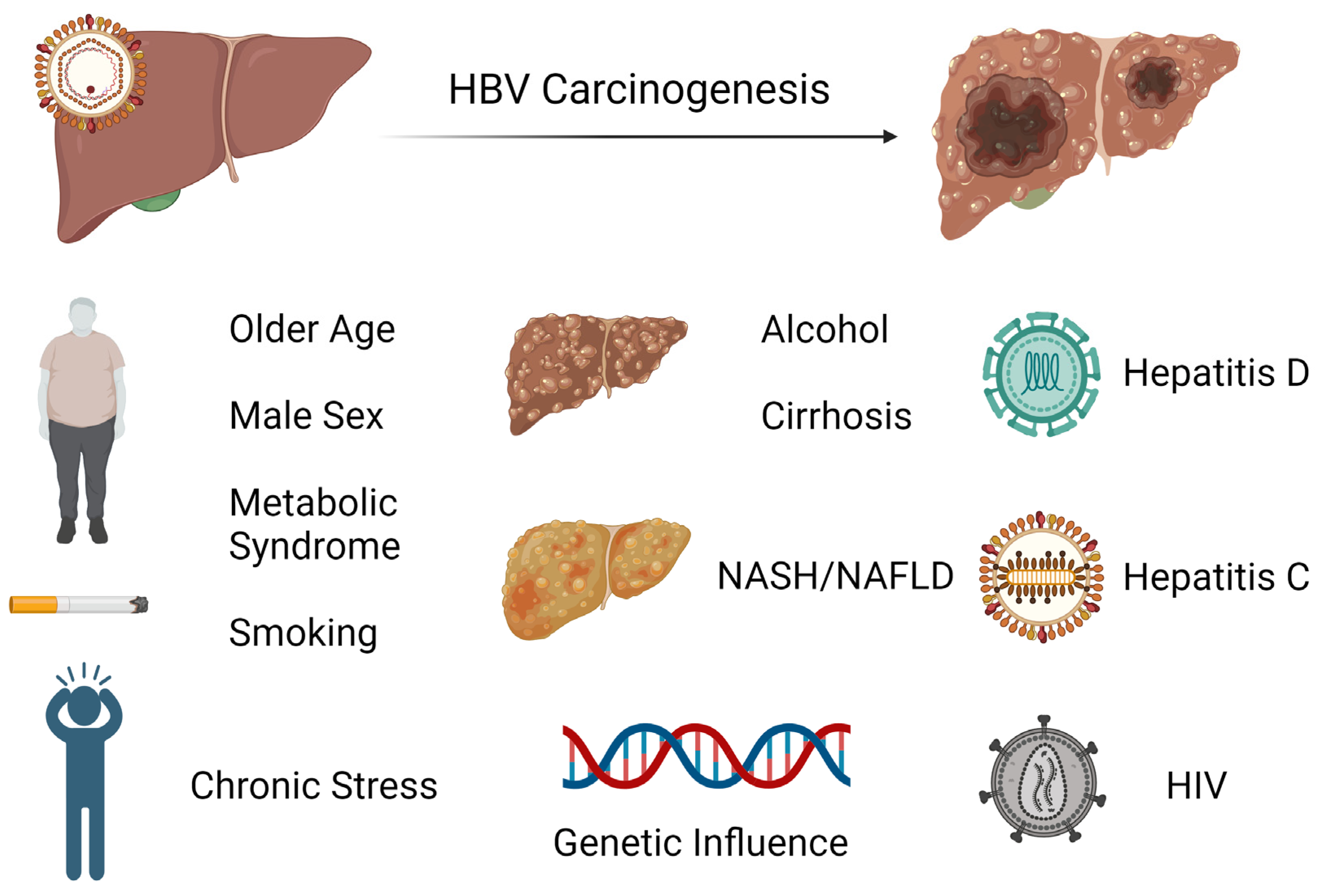
Figure 2. Exogenous and endogenous risk factors for hepatocarcinogenesis from chronic hepatitis B infection.
Surveillance with ultrasound imaging and measurement of alpha-fetoprotein levels has been directed towards these populations to help with early detection of HCC. Guidelines suggest surveillance for HCC in high-risk groups including patients with cirrhosis, noncirrhotic patients with HBV and any of the following characteristics: active hepatitis, family history of HCC, Africans and African Americans, Asian males over 40 years of age, and Asian females over 50 years of age [60][61][62][63]. Other populations that undergo surveillance include patients with chronic hepatitis C virus and advanced liver fibrosis in the absence of cirrhosis, although this is not a consistent recommendation across all societies and the cost effectiveness has not been verified [61].
Currently a knowledge gap remains regarding host factors that contribute to the vagaries of HBV infection outcomes. A group of researchers attempted to explore this by investigating the diverse manifestations of CHB in three families that were observed over decades. Block et al. showed how only one case of HBV-related HCC occurred within every family cluster despite each having the same virus given perinatal transmission from mother to offspring [64]. Furthermore, one of the families had monozygotic twins in which only one sibling developed HBV-related HCC, while the other remained a chronic HBV carrier. The same finding is presenting in a case series by Noverati et al., which presented four family clusters in which patients had very variable courses, some with indolent chronic HBV infection, some requiring treatment, and others who developed HCC or cirrhosis [65]. It is postulated that inheritable immuno-genetic alleles that affect CHB differ from those that influence HBV-related HCC development, which may explain the discrepancy in manifestations in this case series [66]. The study was limited by lack of host and viral genomic analysis, as previous studies have shown certain host polymorphisms and HBV mutations are associated with HBV-related HCC. Nonetheless, this highlights that there are genetic and non-genetic host factors that play a role in development of HCC.
Exogenous, non-genetic factors such as chronic stress have been implicated in the incidence and outcomes of HCC, which may also have contributed to the differing presentations in the case outlined above [18]. One of the first published studies highlighting the significance of stress was by Russ et al., in which the group found in a large UK meta-analysis that those with higher scores on a general health questionnaire measuring psychological distress had a higher mortality from liver disease [67]. Joung et al. outlined how stress can increase inflammatory, oxidative reactions including hypoxia–reoxygenation, overactivation of Kupffer cells, influx of gut-derived lipopolysaccharide and norepinephrine, and overproduction of stress hormones in the sympathetic drive, which cause hepatocellular damage and promote mutagenesis [68]. Studies have shown how the tumor milieu of existing HCC undergoes changes that make it immunosuppressive. Specifically, He et al. discovered how chronic stress transitions cytokines to those that are T helper 2 cell-mediated, a tumor microenvironment that carries a poorer prognosis [69]. Similar studies show how this is exacerbated by the presence of T-regulatory cells that suppress pro-inflammatory cytokines [70][71].
References
- Hou, J.; Liu, Z.; Gu, F. Epidemiology and Prevention of Hepatitis B Virus Infection. Int. J. Med. Sci. 2005, 2, 50–57.
- Bashir Hamidu, R.; Hann, R.R.; Hann, H.-W. Chronicles of HBV and the Road to HBV Cure. Livers 2023, 3, 232–239.
- Hepatitis B. Available online: https://www.who.int/news-room/fact-sheets/detail/hepatitis-b (accessed on 21 December 2023).
- Pithawa, A.K. Sleisenger and Fordtran’s Gastrointestinal and Liver Disease: Pathophysiology, diagnosis, management. Med. J. Armed Forces India 2007, 63, 205.
- Kao, J.H.; Chen, P.J.; Lai, M.Y.; Chen, D.S. Hepatitis B genotypes correlate with clinical outcomes in patients with chronic hepatitis B. Gastroenterology 2000, 118, 554–559.
- Sunbul, M. Hepatitis B virus genotypes: Global distribution and clinical importance. World J. Gastroenterol. 2014, 20, 5427–5434.
- Guidotti, L.G.; Chisari, F.V. Immunobiology and pathogenesis of viral hepatitis. Annu. Rev. Pathol. 2006, 1, 23–61.
- Lok, A.S. Chronic hepatitis B. N. Engl. J. Med. 2002, 346, 1682–1683.
- Parkin, D.M.; Pisani, P.; Ferlay, J. Global cancer statistics. CA Cancer J. Clin. 1999, 49, 33–64.
- Fattovich, G. Natural history and prognosis of hepatitis B. Semin. Liver Dis. 2003, 23, 47–58.
- El-Serag, H.B.; Rudolph, K.L. Hepatocellular carcinoma: Epidemiology and molecular carcinogenesis. Gastroenterology 2007, 132, 2557–2576.
- MacLachlan, J.H.; Cowie, B.C. Hepatitis B virus epidemiology. Cold Spring Harb. Perspect. Med. 2015, 5, a021410.
- Beasley, R.P.; Hwang, L.Y.; Lin, C.C.; Leu, M.L.; Stevens, C.E.; Szmuness, W.; Chen, K.P. Incidence of hepatitis B virus infections in preschool children in Taiwan. J. Infect. Dis. 1982, 146, 198–204.
- Alter, M.J.; Hadler, S.C.; Margolis, H.S.; Alexander, W.J.; Hu, P.Y.; Judson, F.N.; Mares, A.; Miller, J.K.; Moyer, L.A. The changing epidemiology of hepatitis B in the United States. Need for alternative vaccination strategies. JAMA 1990, 263, 1218–1222.
- Chuang, Y.C.; Tsai, K.N.; Ou, J.J. Pathogenicity and virulence of Hepatitis B virus. Virulence 2022, 13, 258–296.
- Ganem, D.; Prince, A.M. Hepatitis B virus infection–Natural history and clinical consequences. N. Engl. J. Med. 2004, 350, 1118–1129.
- Khanam, A.; Chua, J.V.; Kottilil, S. Immunopathology of Chronic Hepatitis B Infection: Role of Innate and Adaptive Immune Response in Disease Progression. Int. J. Mol. Sci. 2021, 22, 5497.
- Noverati, N.; Bashir-Hamidu, R.; Halegoua-DeMarzio, D.; Hann, H.W. Hepatitis B Virus-Associated Hepatocellular Carcinoma and Chronic Stress. Int. J. Mol. Sci. 2022, 23, 3917.
- Liaw, Y.F.; Tsai, S.L.; Sheen, I.S.; Chao, M.; Yeh, C.T.; Hsieh, S.Y.; Chu, C.M. Clinical and virological course of chronic hepatitis B virus infection with hepatitis C and D virus markers. Am. J. Gastroenterol. 1998, 93, 354–359.
- Wieland, S.; Thimme, R.; Purcell, R.H.; Chisari, F.V. Genomic analysis of the host response to hepatitis B virus infection. Proc. Natl. Acad. Sci. USA 2004, 101, 6669–6674.
- Chisari, F.V.; Isogawa, M.; Wieland, S.F. Pathogenesis of hepatitis B virus infection. Pathol. Biol. 2010, 58, 258–266.
- Tripathi, N.; Mousa, O.Y. Hepatitis B. In StatPearls; Statpearls Publishing: Treasure Island, FL, USA, 2023.
- Croagh, C.M.; Lubel, J.S. Natural history of chronic hepatitis B: Phases in a complex relationship. World J. Gastroenterol. 2014, 20, 10395–10404.
- Takashima, H.; Araki, K.; Miyazaki, J.; Yamamura, K.; Kimoto, M. Characterization of T-cell tolerance to hepatitis B virus (HBV) antigen in transgenic mice. Immunology 1992, 75, 398–405.
- Shi, Y.H.; Shi, C.H. Molecular characteristics and stages of chronic hepatitis B virus infection. World J. Gastroenterol. 2009, 15, 3099–3105.
- Wong, G.L. Management of chronic hepatitis B patients in immunetolerant phase: What latest guidelines recommend. Clin. Mol. Hepatol. 2018, 24, 108–113.
- Hui, C.K.; Leung, N.; Yuen, S.T.; Zhang, H.Y.; Leung, K.W.; Lu, L.; Cheung, S.K.; Wong, W.M.; Lau, G.K.; Hong Kong Liver Fibrosis Study, G. Natural history and disease progression in Chinese chronic hepatitis B patients in immune-tolerant phase. Hepatology 2007, 46, 395–401.
- McMahon, B.J. The natural history of chronic hepatitis B virus infection. Hepatology 2009, 49, S45–S55.
- Thimme, R.; Wieland, S.; Steiger, C.; Ghrayeb, J.; Reimann, K.A.; Purcell, R.H.; Chisari, F.V. CD8(+) T cells mediate viral clearance and disease pathogenesis during acute hepatitis B virus infection. J. Virol. 2003, 77, 68–76.
- Jeng, W.J.; Sheen, I.S.; Liaw, Y.F. Hepatitis B virus DNA level predicts hepatic decompensation in patients with acute exacerbation of chronic hepatitis B. Clin. Gastroenterol. Hepatol. 2010, 8, 541–545.
- Chen, Y.C.; Chu, C.M.; Liaw, Y.F. Age-specific prognosis following spontaneous hepatitis B e antigen seroconversion in chronic hepatitis B. Hepatology 2010, 51, 435–444.
- Yang, H.I.; Lu, S.N.; Liaw, Y.F.; You, S.L.; Sun, C.A.; Wang, L.Y.; Hsiao, C.K.; Chen, P.J.; Chen, D.S.; Chen, C.J.; et al. Hepatitis B e antigen and the risk of hepatocellular carcinoma. N. Engl. J. Med. 2002, 347, 168–174.
- Bonino, F.; Rosina, F.; Rizzetto, M.; Rizzi, R.; Chiaberge, E.; Tardanico, R.; Callea, F.; Verme, G. Chronic hepatitis in HBsAg carriers with serum HBV-DNA and anti-HBe. Gastroenterology 1986, 90, 1268–1273.
- Lok, A.S.; Hadziyannis, S.J.; Weller, I.V.; Karvountzis, M.G.; Monjardino, J.; Karayiannis, P.; Montano, L.; Thomas, H.C. Contribution of low level HBV replication to continuing inflammatory activity in patients with anti-HBe positive chronic hepatitis B virus infection. Gut 1984, 25, 1283–1287.
- Bixler, D.; Zhong, Y.; Ly, K.N.; Moorman, A.C.; Spradling, P.R.; Teshale, E.H.; Rupp, L.B.; Gordon, S.C.; Boscarino, J.A.; Schmidt, M.A.; et al. Mortality Among Patients With Chronic Hepatitis B Infection: The Chronic Hepatitis Cohort Study (CHeCS). Clin. Infect. Dis. 2019, 68, 956–963.
- Brechot, C.; Pourcel, C.; Louise, A.; Rain, B.; Tiollais, P. Presence of integrated hepatitis B virus DNA sequences in cellular DNA of human hepatocellular carcinoma. Nature 1980, 286, 533–535.
- Chemin, I.; Zoulim, F. Hepatitis B virus induced hepatocellular carcinoma. Cancer Lett. 2009, 286, 52–59.
- De Mitri, M.S.; Cassini, R.; Bernardi, M. Hepatitis B virus-related hepatocarcinogenesis: Molecular oncogenic potential of clear or occult infections. Eur. J. Cancer 2010, 46, 2178–2186.
- Neuveut, C.; Wei, Y.; Buendia, M.A. Mechanisms of HBV-related hepatocarcinogenesis. J. Hepatol. 2010, 52, 594–604.
- Block, P.D.; Shinn, B.; Kim, J.H.; Hann, H.W. Hepatitis B-related hepatocellular carcinoma and stress: Untangling the host immune response from clinical outcomes. Hepat. Oncol. 2020, 8, HEP35.
- Li, S.; Hong, M.; Tan, H.Y.; Wang, N.; Feng, Y. Insights into the Role and Interdependence of Oxidative Stress and Inflammation in Liver Diseases. Oxidative Med. Cell. Longev. 2016, 2016, 4234061.
- Peneau, C.; Zucman-Rossi, J.; Nault, J.C. Genomics of Viral Hepatitis-Associated Liver Tumors. J. Clin. Med. 2021, 10, 1827.
- Wong, G.L.; Chan, H.L.; Yiu, K.K.; Lai, J.W.; Chan, V.K.; Cheung, K.K.; Wong, E.W.; Wong, V.W. Meta-analysis: The association of hepatitis B virus genotypes and hepatocellular carcinoma. Aliment. Pharmacol. Ther. 2013, 37, 517–526.
- Yang, H.I.; Yeh, S.H.; Chen, P.J.; Iloeje, U.H.; Jen, C.L.; Su, J.; Wang, L.Y.; Lu, S.N.; You, S.L.; Chen, D.S.; et al. Associations between hepatitis B virus genotype and mutants and the risk of hepatocellular carcinoma. J. Natl. Cancer Inst. 2008, 100, 1134–1143.
- Kao, J.H.; Chen, P.J.; Lai, M.Y.; Chen, D.S. Clinical and virological aspects of blood donors infected with hepatitis B virus genotypes B and C. J. Clin. Microbiol. 2002, 40, 22–25.
- Papatheodoridis, G.V.; Lampertico, P.; Manolakopoulos, S.; Lok, A. Incidence of hepatocellular carcinoma in chronic hepatitis B patients receiving nucleos(t)ide therapy: A systematic review. J. Hepatol. 2010, 53, 348–356.
- Chen, C.L.; Yang, H.I.; Yang, W.S.; Liu, C.J.; Chen, P.J.; You, S.L.; Wang, L.Y.; Sun, C.A.; Lu, S.N.; Chen, D.S.; et al. Metabolic factors and risk of hepatocellular carcinoma by chronic hepatitis B/C infection: A follow-up study in Taiwan. Gastroenterology 2008, 135, 111–121.
- Cheuk-Fung Yip, T.; Wai-Sun Wong, V.; Lik-Yuen Chan, H.; Tse, Y.K.; Pik-Shan Kong, A.; Long-Yan Lam, K.; Chung-Yan Lui, G.; Lai-Hung Wong, G. Effects of Diabetes and Glycemic Control on Risk of Hepatocellular Carcinoma After Seroclearance of Hepatitis B Surface Antigen. Clin. Gastroenterol. Hepatol. 2018, 16, 765–773.e762.
- Orito, E.; Hasebe, C.; Kurosaki, M.; Osaki, Y.; Joko, K.; Watanabe, H.; Kimura, H.; Nishijima, N.; Kusakabe, A.; Izumi, N.; et al. Risk of hepatocellular carcinoma in cirrhotic hepatitis B virus patients during nucleoside/nucleotide analog therapy. Hepatol. Res. 2015, 45, 872–879.
- Song, C.; Zhu, J.; Ge, Z.; Yu, C.; Tian, T.; Wang, H.; Han, J.; Shen, H.; Dai, J.; Lu, J.; et al. Spontaneous Seroclearance of Hepatitis B Surface Antigen and Risk of Hepatocellular Carcinoma. Clin. Gastroenterol. Hepatol. 2019, 17, 1204–1206.
- Tan, Y.; Zhang, X.; Zhang, W.; Tang, L.; Yang, H.; Yan, K.; Jiang, L.; Yang, J.; Li, C.; Yang, J.; et al. The Influence of Metabolic Syndrome on the Risk of Hepatocellular Carcinoma in Patients with Chronic Hepatitis B Infection in Mainland China. Cancer Epidemiol. Biomarkers Prev. 2019, 28, 2038–2046.
- Motta, B.M.; Masarone, M.; Torre, P.; Persico, M. From Non-Alcoholic Steatohepatitis (NASH) to Hepatocellular Carcinoma (HCC): Epidemiology, Incidence, Predictions, Risk Factors, and Prevention. Cancers 2023, 15, 5458.
- Ramai, D.; Singh, J.; Lester, J.; Khan, S.R.; Chandan, S.; Tartaglia, N.; Ambrosi, A.; Serviddio, G.; Facciorusso, A. Systematic review with meta-analysis: Bariatric surgery reduces the incidence of hepatocellular carcinoma. Aliment. Pharmacol. Ther. 2021, 53, 977–984.
- Yeung, P.; Wong, D.K.; Lai, C.L.; Fung, J.; Seto, W.K.; Yuen, M.F. Association of hepatitis B virus pre-S deletions with the development of hepatocellular carcinoma in chronic hepatitis B. J. Infect. Dis. 2011, 203, 646–654.
- Yuen, M.F.; Tanaka, Y.; Shinkai, N.; Poon, R.T.; But, D.Y.; Fong, D.Y.; Fung, J.; Wong, D.K.; Yuen, J.C.; Mizokami, M.; et al. Risk for hepatocellular carcinoma with respect to hepatitis B virus genotypes B/C, specific mutations of enhancer II/core promoter/precore regions and HBV DNA levels. Gut 2008, 57, 98–102.
- Keng, V.W.; Largaespada, D.A.; Villanueva, A. Why men are at higher risk for hepatocellular carcinoma? J. Hepatol. 2012, 57, 453–454.
- Jang, T.Y.; Wei, Y.J.; Liu, T.W.; Yeh, M.L.; Liu, S.F.; Hsu, C.T.; Hsu, P.Y.; Lin, Y.H.; Liang, P.C.; Hsieh, M.H.; et al. Role of hepatitis D virus infection in development of hepatocellular carcinoma among chronic hepatitis B patients treated with nucleotide/nucleoside analogues. Sci. Rep. 2021, 11, 8184.
- Hu, J.; Liu, K.; Luo, J. HIV-HBV and HIV-HCV Coinfection and Liver Cancer Development. Cancer Treat. Res. 2019, 177, 231–250.
- Yang, W.T.; Wu, L.W.; Tseng, T.C.; Chen, C.L.; Yang, H.C.; Su, T.H.; Wang, C.C.; Kuo, S.F.; Liu, C.H.; Chen, P.J.; et al. Hepatitis B Surface Antigen Loss and Hepatocellular Carcinoma Development in Patients With Dual Hepatitis B and C Infection. Medicine 2016, 95, e2995.
- Clinical Practice Guidelines for Hepatocellular Carcinoma-The Japan Society of Hepatology 2009 update. Hepatol. Res. 2010, 40 (Suppl. S1), 2–144.
- European Association for the Study of the Liver. EASL Clinical Practice Guidelines: Management of hepatocellular carcinoma. J. Hepatol. 2018, 69, 182–236.
- Kanwal, F.; Singal, A.G. Surveillance for Hepatocellular Carcinoma: Current Best Practice and Future Direction. Gastroenterology 2019, 157, 54–64.
- Marrero, J.A.; Kulik, L.M.; Sirlin, C.B.; Zhu, A.X.; Finn, R.S.; Abecassis, M.M.; Roberts, L.R.; Heimbach, J.K. Diagnosis, Staging, and Management of Hepatocellular Carcinoma: 2018 Practice Guidance by the American Association for the Study of Liver Diseases. Hepatology 2018, 68, 723–750.
- Block, P.; Shinn, B.; Roth, C.; Needleman, L.; Rosato, E.; Hann, H.-W. Vagaries of the Host Response in the Development of Hepatitis B-related Hepatocellular Carcinoma: A Case Series. Curr. Cancer Ther. Rev. 2020, 16, 253–258.
- Noverati, N.; Nguyen, A.; Chalikonda, D.; Halegoua-DeMarzio, D.; Hann, H.W. The Role of Host in the Spectrum of Outcomes in Family Clusters of Hepatitis Infection: From Asymptomatic to Hepatocellular Carcinoma. Case Rep. Gastroenterol. 2023, 17, 104–110.
- Akcay, I.M.; Katrinli, S.; Ozdil, K.; Doganay, G.D.; Doganay, L. Host genetic factors affecting hepatitis B infection outcomes: Insights from genome-wide association studies. World J. Gastroenterol. 2018, 24, 3347–3360.
- Russ, T.C.; Kivimäki, M.; Morling, J.R.; Starr, J.M.; Stamatakis, E.; Batty, G.D. Association between Psychological Distress and Liver Disease Mortality: A Meta-analysis of Individual Study Participants. Gastroenterology 2015, 148, 958–966.e4.
- Joung, J.Y.; Cho, J.H.; Kim, Y.H.; Choi, S.H.; Son, C.G. A literature review for the mechanisms of stress-induced liver injury. Brain Behav. 2019, 9, e01235.
- He, Y.; Gao, H.; Li, X.; Zhao, Y. Psychological stress exerts effects on pathogenesis of hepatitis B via type-1/type-2 cytokines shift toward type-2 cytokine response. PLoS ONE 2014, 9, e105530.
- Granito, A.; Muratori, L.; Lalanne, C.; Quarneti, C.; Ferri, S.; Guidi, M.; Lenzi, M.; Muratori, P. Hepatocellular carcinoma in viral and autoimmune liver diseases: Role of CD4+ CD25+ Foxp3+ regulatory T cells in the immune microenvironment. World J. Gastroenterol. 2021, 27, 2994–3009.
- Han, Y.F.; Zhao, J.; Ma, L.Y.; Yin, J.H.; Chang, W.J.; Zhang, H.W.; Cao, G.W. Factors predicting occurrence and prognosis of hepatitis-B-virus-related hepatocellular carcinoma. World J. Gastroenterol. 2011, 17, 4258–4270.
More
Information
Subjects:
Gastroenterology & Hepatology
Contributors
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
1.0K
Revisions:
2 times
(View History)
Update Date:
21 Feb 2024
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





