
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Laura Sabatino | -- | 3442 | 2023-06-13 17:29:38 | | | |
| 2 | Lindsay Dong | Meta information modification | 3442 | 2023-06-15 03:30:31 | | |
Video Upload Options
Beyond its key role in calcium homeostasis, vitamin D has been found to significantly affect the cardiovascular (CV) system. In fact, low vitamin D levels have been associated with increased CV risk, as well as increased CV morbidity and mortality. The majority of effects of this molecule are related directly or indirectly to its antioxidative and anti-inflammatory properties. Generally, vitamin D insufficiency is considered for 25-hydroxyvitamin D (25(OH)D) levels between 21–29 ng/mL (corresponding to 52.5–72.5 nmol/L), deficiency as 25(OH)D levels less than 20 ng/mL (<50 nmol/L), and extreme deficiency as 25(OH)D less than 10 ng/mL (<25 nmol/L). However, the definition of an optimal vitamin D status, as defined by 25(OH)D, remains controversial for many extra-bone conditions, including CV disease.
1. Introduction
2. Vitamin D Metabolism
UVB sun rays are the main source of vitamin D, whereas less than 10% derives from dietary intake (e.g., salmon, mackerel and herring, mushrooms, eggs, and fish liver oil), but may be also added to other foods or available as a dietary supplement. Skin exposure to solar UV irradiation induces photolysis of a derivative of cholesterol (7-dehydrocholesterol) into pre-vitamin D3, then isomerized to vitamin D3 (cholecalciferol) [1]. As a liposoluble/hydrophobic molecule, vitamin D3 requires the binding with a transporter protein (vitamin D-binding protein, VDBP) to circulate in the blood. Then, it is hydroxylated in the liver to form 25(OH)D, the major circulating metabolite [1]. In the kidney, hydroxylation catalyzed by the 1alfa-hydroxylase enzyme produces the active hormone, 1,25-dihydroxy vitamin D (1,25(OH)2D), while 24-hydroxylase (CYP24) promotes the production of inactive forms [1]. When released by its binding with DBP to the tissues, 1,25(OH)2D mediates a number of actions through its intracellular vitamin D receptor (VDR). The main objectives are control of calcium and phosphorus homeostasis (kidney and intestine as principal target tissues) and bone health and turnover. Although 1,25(OH)2D represents the active form, there is general agreement on the measure of 25(OH)D as the best index of vitamin D status [2]. Notably, 25(OH)D has a higher concentration in the bloodstream with respect to the active form 1,25(OH)2D and shows a longer circulating half-life if compared to 1,25(OH)2D (3 weeks vs. 4 h, respectively), thus providing more representative information about the vitamin D status. Moreover, 1,25(OH)2D values are regulated through PTH (upregulation) and higher serum calcium and phosphate levels (downregulation). Therefore, because vitamin D deficiency may induce secondary hyperparathyroidism, 1,25(OH)2D may result in reduced, normal or even elevated despite evidence of vitamin deficiency.
3. Methodological Determinants
3.1. Preanalytical Issues
3.2. Analytical Issues
4. Environmental Determinants, Lifestyle Habits, and Skin Pigmentation Affecting 25(OH)D Status
| Environmental Determinants | Anthropometric Determinants | Life-Style Determinants |
|---|---|---|
sunlight exposure: intensity and duration season latitude length of day presence of clouds air pollution/ozone |
aging race/phototype gender body mass index/obesity genetic asset: presence of specific polymorphisms hepatic/renal dysfunction pregnancy |
dietary intake supplementation/fortified foods sunscreen/clothes time spent outdoor/outdoor sports |
5. Anthropometric Characteristics
6. Vitamin D and Genetic Determinants
7. Vitamin D Mechanisms Related to Its Antioxidant/Antiinflammatory Action and Vascular Health
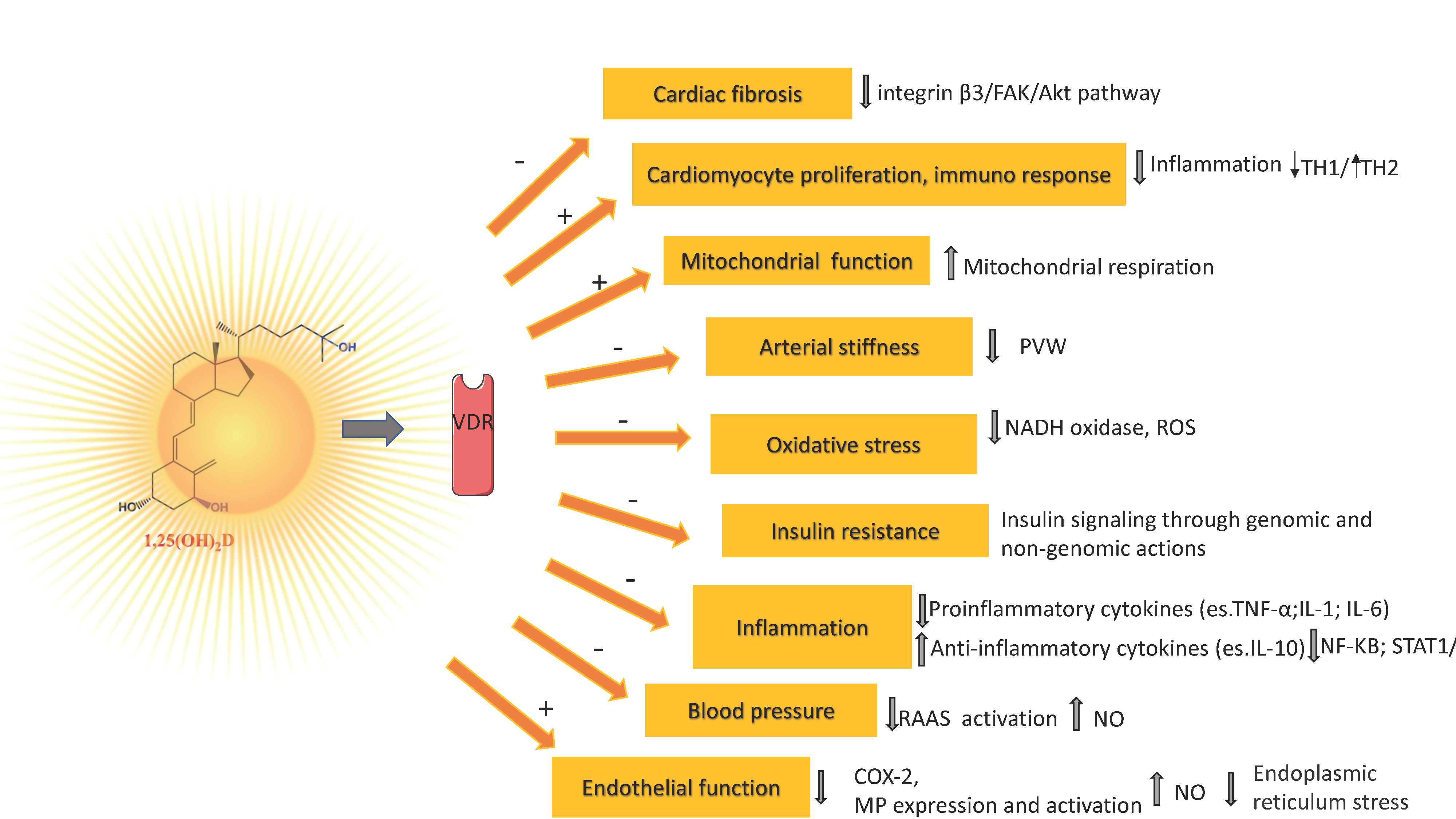
8. Observational Studies
9. Randomized Controlled Trials
References
- Silva, I.C.J.; Lazaretti-Castro, M. Vitamin D Metabolism and Extraskeletal Outcomes: An Update. Arch. Endocrinol. Metab. 2022, 66, 748–755.
- Holick, M.F.; Binkley, N.C.; Bischoff-Ferrari, H.A.; Gordon, C.M.; Hanley, D.A.; Heaney, R.P.; Murad, M.H.; Weaver, C.M. Evaluation, Treatment, and Prevention of Vitamin D Deficiency: An Endocrine Society Clinical Practice Guideline. J. Clin. Endocrinol. Metab. 2011, 96, 1911–1930.
- Graham, L. IOM Releases Report on Dietary Reference Intakes for Calcium and Vitamin D. Am. Fam. Physician 2011, 83, 1352.
- Holick, M.F. The Vitamin D Deficiency Pandemic: Approaches for Diagnosis, Treatment and Prevention. Rev. Endocr. Metab. Disord. 2017, 18, 153–165.
- Liu, Z.; Huang, S.; Yuan, X.; Wang, Y.; Liu, Y.; Zhou, J. The Role of Vitamin D Deficiency in the Development of Paediatric Diseases. Ann. Med. 2023, 55, 127–135.
- Bianchi, S.; Maffei, S.; Prontera, C.; Battaglia, D.; Vassalle, C. Preanalytical, Analytical (DiaSorin LIAISON) and Clinical Variables Potentially Affecting the 25-OH Vitamin D Estimation. Clin. Biochem. 2012, 45, 1652–1657.
- Harvey, S.M.; Murphy, V.E.; Gibson, P.G.; Clarke, M.; Jensen, M.E. The Impact of Sample Type on Vitamin d Quantification and Clinical Classification during Pregnancy. Nutrients 2020, 12, 3872.
- Yu, C.L.; Falk, R.T.; Kimlin, M.G.; Rajaraman, P.; Sigurdson, A.J.; Horst, R.L.; Cosentino, L.M.; Linet, M.S.; Freedman, D.M. The Impact of Delayed Blood Centrifuging, Choice of Collection Tube, and Type of Assay on 25-Hydroxyvitamin D Concentrations. Cancer Causes Control 2010, 21, 643–648.
- Wielders, J.P.M.; Wijnberg, F.A. Preanalytical Stability of 25(OH)-Vitamin D3 in Human Blood or Serum at Room Temperature: Solid as a Rock. Clin. Chem. 2009, 55, 1584–1585.
- Battault, S.; Whiting, S.J.; Peltier, S.L.; Sadrin, S.; Gerber, G.; Maixent, J.M. Vitamin D Metabolism, Functions and Needs: From Science to Health Claims. Eur. J. Nutr. 2013, 52, 429–441.
- Borai, A.; Khalil, H.; Alghamdi, B.; Alhamdi, R.; Ali, N.; Bahijri, S.; Ferns, G. The Pre-Analytical Stability of 25-Hydroxyvitamin D: Storage and Mixing Effects. J. Clin. Lab. Anal. 2020, 34, e23037.
- Colak, A.; Toprak, B.; Dogan, N.; Ustuner, F. Effect of Sample Type, Centrifugation and Storage Conditions on Vitamin D Concentration. Biochem. Med. 2013, 23, 321–325.
- Zelzer, S.; Meinitzer, A.; Enko, D.; Simstich, S.; Le Goff, C.; Cavalier, E.; Herrmann, M.; Goessler, W. Simultaneous Determination of 24,25- and 25,26-Dihydroxyvitamin D3 in Serum Samples with Liquid-Chromatography Mass Spectrometry–A Useful Tool for the Assessment of Vitamin D Metabolism. J. Chromatogr. B Anal. Technol. Biomed. Life Sci. 2020, 1158, 122394.
- Cavalier, E. Long-Term Stability of 25-Hydroxyvitamin D: Importance of the Analytical Method and of the Patient Matrix. Clin. Chem. Lab. Med. 2021, 59, E389–E391.
- Carter, G.D. 25-Hydroxyvitamin D Assays: The Quest for Accuracy. Clin. Chem. 2009, 55, 1300–1302.
- Fraser, W.D.; Milan, A.M. Vitamin D Assays: Past and Present Debates, Difficulties, and Developments. Calcif. Tissue Int. 2013, 92, 118–127.
- Tsiaras, W.G.; Weinstock, M.A. Factors Influencing Vitamin d Status. Acta Derm. Venereol. 2011, 91, 115–124.
- Kimlin, M.G. Geographic Location and Vitamin D Synthesis. Mol. Asp. Med. 2008, 29, 453–461.
- Engelsen, O. The Relationship between Ultraviolet Radiation Exposure and Vitamin D Status. Nutrients 2010, 2, 482–495.
- Spiro, A.; Buttriss, J.L. Vitamin D: An Overview of Vitamin D Status and Intake in Europe. Nutr. Bull. 2014, 39, 322–350.
- Aldrees, T.; Alohali, S.; Albosaily, A.; Almatrafi, S.; Aldhahri, S. Seasonal Variations in Serum Levels of Vitamin D and Other Biochemical Markers among KSA Patients Prior to Thyroid Surgery. J. Taibah Univ. Med. Sci. 2020, 15, 522–528.
- Karagüzel, G.; Dilber, B.; Çan, G.; Ökten, A.; Deǧer, O.; Holick, M.F. Seasonal Vitamin D Status of Healthy Schoolchildren and Predictors of Low Vitamin D Status. J. Pediatr. Gastroenterol. Nutr. 2014, 58, 654–660.
- Bjarnadottir, A.; Kristjansdottir, A.G.; Hrafnkelsson, H.; Johannsson, E.; Magnusson, K.T.; Thorsdottir, I. Insufficient Autumn Vitamin D Intake and Low Vitamin D Status in 7-Year-Old Icelandic Children. Public Health Nutr. 2015, 18, 208–217.
- Petersen, R.A.; Damsgaard, C.T.; Dalskov, S.M.; Sorensen, L.B.; Hjorth, M.F.; Ritz, C.; Kjolbæk, L.; Andersen, R.; Tetens, I.; Krarup, H.; et al. Vitamin D Status and Its Determinants during Autumn in Children at Northern Latitudes: A Cross-Sectional Analysis from the Optimal Well-Being, Development and Health for Danish Children through a Healthy New Nordic Diet (OPUS) School Meal Study. Br. J. Nutr. 2016, 115, 239–250.
- Hansen, L.; Tjønneland, A.; Køster, B.; Brot, C.; Andersen, R.; Cohen, A.S.; Frederiksen, K.; Olsen, A. Vitamin D Status and Seasonal Variation among Danish Children and Adults: A Descriptive Study. Nutrients 2018, 10, 1801.
- Pierrot-Deseilligny, C.; Souberbielle, J.C. Is Hypovitaminosis D One of the Environmental Risk Factors for Multiple Sclerosis? Brain 2010, 133, 1869–1888.
- Bhattoa, H.P.; Nagy, E.; More, C.; Kappelmayer, J.; Balogh, A.; Kalina, E.; Antal-Szalmas, P. Prevalence and Seasonal Variation of Hypovitaminosis D and Its Relationship to Bone Metabolism in Healthy Hungarian Men over 50 Years of Age: The HunMen Study. Osteoporos. Int. 2013, 24, 179–186.
- Cashman, K.D.; Dowling, K.G.; Škrabáková, Z.; Gonzalez-Gross, M.; Valtueña, J.; De Henauw, S.; Moreno, L.; Damsgaard, C.T.; Michaelsen, K.F.; Mølgaard, C.; et al. Vitamin D Deficiency in Europe: Pandemic? Am. J. Clin. Nutr. 2016, 103, 1033–1044.
- Ghareghani, M.; Reiter, R.J.; Zibara, K.; Farhadi, N. Latitude, Vitamin D, Melatonin, and Gut Microbiota Act in Concert to Initiate Multiple Sclerosis: A New Mechanistic Pathway. Front. Immunol. 2018, 9, 2484.
- Datta, P.; Philipsen, P.A.; Olsen, P.; Petersen, B.; Johansen, P.; Morling, N.; Wulf, H.C. Major Inter-Personal Variation in the Increase and Maximal Level of 25-Hydroxy Vitamin D Induced by UVB. Photochem. Photobiol. Sci. 2016, 15, 536–545.
- Vassalle, C.; Pérez-López, F. The Importance of Some Analytical Aspects and Confounding Factors in Relation to Clinical Interpretation of Results. In Vitamin D: Daily Requirements, Dietary Sources and Symptoms of Deficiency; Nova Publisher: New York, NY, USA, 2013; ISBN 978-1-62808-816-8.
- Meehan, M.; Penckofer, S. The Role of Vitamin D in the Aging Adult. J. Aging Gerontol. 2014, 2, 60–71.
- Kim, C.S.; Kim, S.W. Vitamin D and Chronic Kidney Disease. Korean J. Intern. Med. 2014, 29, 416–427.
- Jean, G.; Souberbielle, J.C.; Chazot, C. Vitamin D in Chronic Kidney Disease and Dialysis Patients. Nutrients 2017, 9, 328.
- Muscogiuri, G.; Barrea, L.; Di Somma, C.; Laudisio, D.; Salzano, C.; Pugliese, G.; de Alteriis, G.; Colao, A.; Savastano, S. Sex Differences of Vitamin D Status across BMI Classes: An Observational Prospective Cohort Study. Nutrients 2019, 11, 3034.
- Heaney, R.P.; Recker, R.R.; Grote, J.; Horst, R.L.; Armas, L.A.G. Vitamin D3 Is More Potent than Vitamin D2in Humans. J. Clin. Endocrinol. Metab. 2011, 96, 447–452.
- Nimitphong, H.; Park, E.; Lee, M.J. Vitamin D Regulation of Adipogenesis and Adipose Tissue Functions. Nutr. Res. Pract. 2020, 14, 553–567.
- Pereira-Santos, M.; Costa, P.R.F.; Assis, A.M.O.; Santos, C.A.S.T.; Santos, D.B. Obesity and Vitamin D Deficiency: A Systematic Review and Meta-Analysis. Obes. Rev. 2015, 16, 341–349.
- Wang, X.; Chang, X.; Zhu, Y.; Wang, H.; Sun, K. Metabolically Obese Individuals of Normal Weight Have a High Risk of 25-Hydroxyvitamin D Deficiency. Am. J. Med. Sci. 2016, 352, 360–367.
- Fiamenghi, V.I.; de Mello, E.D. Vitamin D Deficiency in Children and Adolescents with Obesity: A Meta-Analysis. J. Pediatr. 2021, 97, 273–279.
- Abbas, M.A. Physiological Functions of Vitamin D in Adipose Tissue. J. Steroid Biochem. Mol. Biol. 2017, 165, 369–381.
- Verweij, K.J.; Mosing, M.A.; Zietsch, B.P.; Medlan, M. Estimating Heritability from Twin Studies. Stat. Hum. Genet. Methods Protoc. Methods Mol. Biol. 2012, 850, 151–170.
- Karohl, C.; Su, S.; Kumari, M.; Tangpricha, V.; Veledar, E.; Vaccarino, V.; Raggi, P. Heritability and Seasonal Variability of Vitamin D Concentrations in Male Twins. Am. J. Clin. Nutr. 2010, 92, 1393–1398.
- Orton, S.M.; Morris, A.P.; Herrera, B.M.; Ramagopalan, S.V.; Lincoln, M.R.; Chao, M.J.; Vieth, R.; Sadovnick, A.D.; Ebers, G.C. Evidence for Genetic Regulation of Vitamin D Status in Twins with Multiple Sclerosis. Am. J. Clin. Nutr. 2008, 88, 441–447.
- Yu, H.J.; Kwon, M.J.; Woo, H.Y.; Park, H. Analysis of 25-Hydroxyvitamin D Status According to Age, Gender, and Seasonal Variation. J. Clin. Lab. Anal. 2016, 30, 905–911.
- Dastani, Z.; Li, R.; Richards, B. Genetic Regulation of Vitamin D Levels. Calcif. Tissue Int. 2013, 92, 106–117.
- Lander, E.; Kruglyak, L. Genetic Dissection of Complex Traits: Guidelines for Interpreting and Reporting Linkage Results. Nat. Genet. 1995, 11, 241–247.
- Shinkyo, R.; Sakaki, T.; Kamakura, M.; Ohta, M.; Inouye, K. Metabolism of Vitamin D by Human Microsomal CYP2R1. Biochem. Biophys. Res. Commun. 2004, 324, 451–457.
- McGrath, J.J.; Saha, S.; Burne, T.H.J.; Eyles, D.W. A Systematic Review of the Association between Common Single Nucleotide Polymorphisms and 25-Hydroxyvitamin D Concentrations. J. Steroid Biochem. Mol. Biol. 2010, 121, 471–477.
- Sakaki, T.; Kagawa, N.; Yamamoto, K.; Inouye, K. Metabolism of Vitamin D3 by Cytochromes P450. Front. Biosci. 2005, 10, 119–134.
- Benjamin, E.J.; Dupuis, J.; Larson, M.G.; Lunetta, K.L.; Booth, S.L.; Govindaraju, D.R.; Kathiresan, S.; Keaney, J.F.; Keyes, M.J.; Lin, J.P.; et al. Genome-Wide Association with Select Biomarker Traits in the Framingham Heart Study. BMC Med. Genet. 2007, 8, S11.
- Jiang, X.; Kiel, D.P.; Kraft, P. The Genetics of Vitamin D. Bone 2019, 126, 59–77.
- Wang, T.T.; Tavera-Mendoza, L.E.; Laperriere, D.; Libby, E.; MacLeod, N.B.; Nagai, Y.; Bourdeau, V.; Konstorum, A.; Lallemant, B.; Zhang, R.; et al. Large-Scale in Silico and Microarray-Based Identification of Direct 1,25-Dihydroxyvitamin D3 Target Genes. Mol. Endocrinol. 2005, 19, 2685–2695.
- Bouillon, R.; Marcocci, C.; Carmeliet, G.; Bikle, D.; White, J.H.; Dawson-Hughes, B.; Lips, P.; Munns, C.F.; Lazaretti-Castro, M.; Giustina, A.; et al. Skeletal and Extraskeletal Actions of Vitamin D: Current Evidence and Outstanding Questions. Endocr. Rev. 2019, 40, 1109–1151.
- Marino, R.; Misra, M. Extra-Skeletal Effects of Vitamin D. Nutrients 2019, 11, 1460.
- Goncalves-Mendes, N.; Talvas, J.; Dualé, C.; Guttmann, A.; Corbin, V.; Marceau, G.; Sapin, V.; Brachet, P.; Evrard, B.; Laurichesse, H.; et al. Impact of Vitamin D Supplementation on Influenza Vaccine Response and Immune Functions in Deficient Elderly Persons: A Randomized Placebo-Controlled Trial. Front. Immunol. 2019, 10, 65.
- Zmijewski, M.A. Vitamin D and Human Health. Int. J. Mol. Sci. 2019, 20, 145.
- Modarresi-Ghazani, F.; Hejazi, M.E.; Gharekhani, A.; Entezari-Maleki, T. Role of Vitamin D in Cardiovascular Disease. Arch. Iran. Med. 2016, 19, 359–362.
- Kim, D.H.; Meza, C.A.; Clarke, H.; Kim, J.S.; Hickner, R.C. Vitamin D and Endothelial Function. Nutrients 2020, 12, 575.
- Molinari, C.; Uberti, F.; Grossini, E.; Vacca, G.; Carda, S.; Invernizzi, M.; Cisari, C. 1α,25-Dihydroxycholecalciferol Induces Nitric Oxide Production in Cultured Endothelial Cells. Cell. Physiol. Biochem. 2011, 27, 661–668.
- Andrukhova, O.; Slavic, S.; Zeitz, U.; Riesen, S.C.; Heppelmann, M.S.; Ambrisko, T.D.; Markovic, M.; Kuebler, W.M.; Erben, R.G. Vitamin D Is a Regulator of Endothelial Nitric Oxide Synthase and Arterial Stiffness in Mice. Mol. Endocrinol. 2014, 28, 53–64.
- Jain, S.K.; Micinski, D.; Huning, L.; Kahlon, G.; Bass, P.F.; Levine, S.N. Vitamin D and L-Cysteine Levels Correlate Positively with GSH and Negatively with Insulin Resistance Levels in the Blood of Type 2 Diabetic Patients. Eur. J. Clin. Nutr. 2014, 68, 1148–1153.
- Nakai, K.; Fujii, H.; Kono, K.; Goto, S.; Kitazawa, R.; Kitazawa, S.; Hirata, M.; Shinohara, M.; Fukagawa, M.; Nishi, S. Vitamin D Activates the Nrf2-Keap1 Antioxidant Pathway and Ameliorates Nephropathy in Diabetic Rats. Am. J. Hypertens. 2014, 27, 586–595.
- Bhat, M.; Ismail, A. Vitamin D Treatment Protects against and Reverses Oxidative Stress Induced Muscle Proteolysis. J. Steroid Biochem. Mol. Biol. 2015, 152, 171–179.
- Calton, E.K.; Keane, K.N.; Newsholme, P.; Soares, M.J. The Impact of Vitamin D Levels on Inflammatory Status: A Systematic Review of Immune Cell Studies. PLoS ONE 2015, 10, e0141770.
- Li, Y.C. Molecular Mechanism of Vitamin D in the Cardiovascular System. J. Investig. Med. 2011, 59, 868–871.
- Turin, A.; Bax, J.J.; Doukas, D.; Joyce, C.; Lopez, J.J.; Mathew, V.; Pontone, G.; Shah, F.; Singh, S.; Wilber, D.J.; et al. Interactions Among Vitamin D, Atrial Fibrillation, and the Renin-Angiotensin-Aldosterone System. Am. J. Cardiol. 2018, 122, 780–784.
- Li, Y.C.; Kong, J.; Wei, M.; Chen, Z.-F.; Liu, S.Q.; Cao, L.-P. 1,25-Dihydroxyvitamin D3 Is a Negative Endocrine Regulator of the Renin-Angiotensin System. J. Clin. Investig. 2002, 110, 229–238.
- Yuan, W.; Pan, W.; Kong, J.; Zheng, W.; Szeto, F.L.; Wong, K.E.; Cohen, R.; Klopot, A.; Zhang, Z.; Yan, C.L. 1,25-Dihydroxyvitamin D3 Suppresses Renin Gene Transcription by Blocking the Activity of the Cyclic AMP Response Element in the Renin Gene Promoter. J. Biol. Chem. 2007, 282, 29821–29830.
- Zhou, C.; Lu, F.; Cao, K.; Xu, D.; Goltzman, D.; Miao, D. Calcium-Independent and 1,25(OH)2D3-Dependent Regulation of the Renin-Angiotensin System in 1α-Hydroxylase Knockout Mice. Kidney Int. 2008, 74, 170–179.
- Zhang, W.; Chen, L.; Zhang, L.; Xiao, M.; Ding, J.; Goltzman, D.; Miao, D. Administration of Exogenous 1,25(OH)2D3 Normalizes Overactivation of the Central Renin-Angiotensin System in 1α(OH)Ase Knockout Mice. Neurosci. Lett. 2015, 588, 184–189.
- Tomaschitz, A.; Pilz, S.; Ritz, E.; Grammer, T.; Drechsler, C.; Boehm, B.O.; März, W. Independent Association between 1,25-Dihydroxyvitamin D, 25-Hydroxyvitamin D and the Renin-Angiotensin System. The Ludwigshafen Risk and Cardiovascular Health (LURIC) Study. Clin. Chim. Acta 2010, 411, 1354–1360.
- Bernini, G.; Carrara, D.; Bacca, A.; Carli, V.; Virdis, A.; Rugani, I.; Duranti, E.; Ghiadoni, L.; Bernini, M.; Taddei, S. Effect of Acute and Chronic Vitamin D Administration on Systemic Renin Angiotensin Systemin Essential Hypertensives and Controls. J. Endocrinol. Investig. 2013, 36, 216–220.
- McMullan, C.J.; Borgi, L.; Curhan, G.C.; Fisher, N.; Forman, J.P. The Effect of Vitamin D on Renin-Angiotensin System Activation and Blood Pressure: A Randomized Control Trial. J. Hypertens. 2016, 35, 822–829.
- Kunutsor, S.K.; Apekey, T.A.; Steur, M. Vitamin D and Risk of Future Hypertension: Meta-Analysis of 283,537 Participants. Eur. J. Epidemiol. 2013, 28, 205–221.
- Zhang, D.; Cheng, C.; Wang, Y.; Sun, H.; Yu, S.; Xue, Y.; Liu, Y.; Li, W.; Li, X. Effect of Vitamin D on Blood Pressure and Hypertension in the General Population: An Update Meta-Analysis of Cohort Studies and Randomized Controlled Trials. Prev. Chronic Dis. 2020, 17, E03.
- Kunutsor, S.K.; Burgess, S.; Munroe, P.B.; Khan, H. Vitamin D and High Blood Pressure: Causal Association or Epiphenomenon? Eur. J. Epidemiol. 2014, 29, 1–14.
- Shu, L.; Huang, K. Effect of Vitamin D Supplementation on Blood Pressure Parameters in Patients with Vitamin D Deficiency: A Systematic Review and Meta-Analysis. J. Am. Soc. Hypertens. 2018, 12, 488–496.
- Elliott, P.; McKenna, W. Hypertrophic Cardiomyopathy: A 50th Anniversary. Heart 2008, 94, 1247–1248.
- Rodríguez, A.J.; Scott, D.; Srikanth, V.; Ebeling, P. Effect of Vitamin D Supplementation on Measures of Arterial Stiffness: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Clin. Endocrinol. 2016, 84, 645–657.
- Codoñer-Franch, P.; Tavárez-Alonso, S.; Simó-Jordá, R.; Laporta-Martín, P.; Carratalá-Calvo, A.; Alonso-Iglesias, E. Vitamin D Status Is Linked to Biomarkers of Oxidative Stress, Inflammation, and Endothelial Activation in Obese Children. J. Pediatr. 2012, 161, 848–854.
- Gradinaru, D.; Borsa, C.; Ionescu, C.; Margina, D.; Prada, G.I.; Jansen, E. Vitamin D Status and Oxidative Stress Markers in the Elderly with Impaired Fasting Glucose and Type 2 Diabetes Mellitus. Aging Clin. Exp. Res. 2012, 24, 595–602.
- Asghari, S.; Hamedi-Shahraki, S.; Amirkhizi, F. Vitamin D Status and Systemic Redox Biomarkers in Adults with Obesity. Clin. Nutr. ESPEN 2021, 45, 292–298.
- Cӑtoi, A.F.; Iancu, M.; Pârvu, A.E.; Cecan, A.D.; Bidian, C.; Chera, E.I.; Pop, I.D.; Macri, A.M. Relationship between 25 Hydroxyvitamin d, Overweight/Obesity Status, pro-Inflammatory and Oxidative Stress Markers in Patients with Type 2 Diabetes: A Simplified Empirical Path Model. Nutrients 2021, 13, 2889.
- Dhas, Y.; Banerjee, J.; Damle, G.; Mishra, N. Serum 25(OH)D Concentration and Its Association with Inflammation and Oxidative Stress in the Middle-Aged Indian Healthy and Diabetic Subjects. Steroids 2020, 154, 951–957.
- Jaksic, M.; Martinovic, M.; Gligorovic-Barhanovic, N.; Vujacic, A.; Djurovic, D.; Nedovic-Vukovic, M. Association between Inflammation, Oxidative Stress, Vitamin D, Copper and Zinc with Pre-Obesity and Obesity in School Children from the City of Podgorica, Montenegro. J. Pediatr. Endocrinol. Metab. 2019, 32, 951–957.
- Verdoia, M.; Nardin, M.; Gioscia, R.; Afifeh, A.M.S.; Viglione, F.; Negro, F.; Marcolongo, M.; Luca, G. De Association between Vitamin D Deficiency and Serum Homocysteine Levels and Its Relationship with Coronary Artery Disease. J. Thromb. Thrombolysis 2021, 52, 523–531.
- Danikiewicz, A.; Hudzik, B.; Nowak, J.; Kowalska, J.; Zieleń-Zynek, I.; Szkodzinski, J.; Tun, H.N.; Zubelewicz-Szkodzinska, B. Serum Gamma Glutamyltransferase Is Associated with 25-Hydroxyvitamin d Status in Elderly Patients with Stable Coronary Artery Disease. Int. J. Environ. Res. Public Health 2020, 17, 8980.
- Machulsky, N.F.; Barchuk, M.; Gagliardi, J.; González, D.; Lombardo, M.; Escudero, A.G.; Gigena, G.; Blanco, F.; Schreier, L.; Fabre, B.; et al. Vitamin D Is Related to Markers of Vulnerable Plaque in Acute Myocardial Infarction. Curr. Vasc. Pharmacol. 2017, 15, 355–360.
- Tomson, J.; Emberson, J.; Hill, M.; Gordon, A.; Armitage, J.; Shipley, M.; Collins, R.; Clarke, R. Vitamin D and Risk of Death from Vascular and Non-Vascular Causes in the Whitehall Study and Meta-Analyses of 12 000 Deaths. Eur. Heart J. 2013, 34, 1365–1374.
- Gaksch, M.; Jorde, R.; Grimnes, G.; Joakimsen, R.; Schirmer, H.; Wilsgaard, T.; Mathiesen, E.B.; Njølstad, I.; Løchen, M.L.; Maürz, W.; et al. Vitamin D and Mortality: Individual Participant Data Meta-Analysis of Standardized 25-Hydroxyvitamin D in 26916 Individuals from a European Consortium. PLoS ONE 2017, 12, e0170791.
- Yang, J.; Ou-Yang, J.; Huang, J.; Wilhelm, M. Low Serum Vitamin D Levels Increase the Mortality of Cardiovascular Disease in Older Adults: A Dose-Response Meta-Analysis of Prospective Studies. Medicine 2019, 98, 810–819.
- Zhang, R.; Li, B.; Gao, X.; Tian, R.; Pan, Y.; Jiang, Y.; Gu, H.; Wang, Y.; Wang, Y.; Liu, G. Serum 25-HydroxyVitamin D and the Risk of Cardiovascular Disease: Dose-Response Meta-Analysis of Prospective Studies1-3. Am. J. Clin. Nutr. 2017, 105, 810–819.
- Elamin, M.B.; Elnour, N.O.A.; Elamin, K.B.; Fatourechi, M.M.; Alkatib, A.A.; Almandoz, J.P.; Liu, H.; Lane, M.A.; Mullan, R.J.; Hazem, A.; et al. Vitamin D and Cardiovascular Outcomes: A Systematic Review and Meta-Analysis. J. Clin. Endocrinol. Metab. 2011, 96, 1931–1942.
- Kalvandi, F.; Azarbayjani, M.A.; Azizbeigi, R.; Azizbeigi, K. Elastic Resistance Training Is More Effective than Vitamin D3 Supplementation in Reducing Oxidative Stress and Strengthen Antioxidant Enzymes in Healthy Men. Eur. J. Clin. Nutr. 2022, 76, 610–615.
- Asemi, Z.; Samimi, M.; Tabassi, Z.; Shakeri, H.; Esmaillzadeh, A. Vitamin D Supplementation Affects Serum High-Sensitivity C-Reactive Protein, Insulin Resistance, and Biomarkers of Oxidative Stress in Pregnant Women. J. Nutr. 2013, 143, 1432–1438.
- Timar, A.; Saberi-Karimian, M.; Ghazizadeh, H.; Parizadeh, S.M.R.; Sabbaghzadeh, R.; Emadzadeh, M.; Eshaghi, F.; Tavallaie, S.; Ferns, G.A.; Ghayour-Mobarhan, M. Evaluation of the Serum Prooxidant-Antioxidant Balance before and after Vitamin D Supplementation in Adolescent Iranian Girls. Adv. Med. Sci. 2019, 64, 174–180.
- de Medeiros Cavalcante, I.G.; Silva, A.S.; Costa, M.J.C.; Persuhn, D.C.; Issa, C.T.M.I.; de Luna Freire, T.L.; da Conceição Rodrigues Gonçalves, M. Effect of Vitamin D3 Supplementation and Influence of BsmI Polymorphism of the VDR Gene of the Inflammatory Profile and Oxidative Stress in Elderly Women with Vitamin D Insufficiency Vitamin D3 Megadose Reduces Inflammatory Markers. Exp. Gerontol. 2015, 66, 10–16.
- Scholten, S.; Sergeev, I.; Birger, C.; Song, Q. Effects of Vitamin D and Quercetin, Alone and in Combination, on Cardiorespiratory Fitness and Muscle Function in Physically Active Male Adults. Open Access J. Sport. Med. 2015, 6, 229–239.
- Nikooyeh, B.; Neyestani, T.R.; Tayebinejad, N.; Alavi-Majd, H.; Shariatzadeh, N.; Kalayi, A.; Zahedirad, M.; Heravifard, S.; Salekzamani, S. Daily Intake of Vitamin D- or Calcium-Vitamin D-Fortified Persian Yogurt Drink (Doogh) Attenuates Diabetes-Induced Oxidative Stress: Evidence for Antioxidative Properties of Vitamin D. J. Hum. Nutr. Diet. 2014, 27, 276–823.
- Tamadon, M.R.; Soleimani, A.; Keneshlou, F.; Mojarrad, M.Z.; Bahmani, F.; Naseri, A.; Kashani, H.H.; Hosseini, E.S.; Asemi, Z. Clinical Trial on the Effects of Vitamin D Supplementation on Metabolic Profiles in Diabetic Hemodialysis. Horm. Metab. Res. 2018, 50, 50–55.
- Johny, E.; Jala, A.; Nath, B.; Alam, M.J.; Kuladhipati, I.; Das, R.; Borkar, R.M.; Adela, R. Vitamin D Supplementation Modulates Platelet-Mediated Inflammation in Subjects With Type 2 Diabetes: A Randomized, Double-Blind, Placebo-Controlled Trial. Front. Immunol. 2022, 13, 869591.
- Pasupuleti, P.; Suchitra, M.M.; Bitla, A.R.; Sachan, A. Attenuation of Oxidative Stress, Interleukin-6, High-Sensitivity C-Reactive Protein, Plasminogen Activator Inhibitor-1, and Fibrinogen with Oral Vitamin D Supplementation in Patients with T2DM Having Vitamin D Deficiency. J. Lab. Physicians 2022, 14, 190–196.
- Thethi, T.K.; Bajwa, M.A.; Ghanim, H.; Jo, C.; Weir, M.; Goldfine, A.B.; Umpierrez, G.; Desouza, C.; Dandona, P.; Fang-Hollingsworth, Y.; et al. Effect of Paricalcitol on Endothelial Function and Inflammation in Type 2 Diabetes and Chronic Kidney Disease. J. Diabetes Complicat. 2015, 29, 433–437.
- Yiu, Y.F.; Yiu, K.H.; Siu, C.W.; Chan, Y.H.; Li, S.W.; Wong, L.Y.; Lee, S.W.L.; Tam, S.; Wong, E.W.K.; Lau, C.P.; et al. Randomized Controlled Trial of Vitamin D Supplement on Endothelial Function in Patients with Type 2 Diabetes. Atherosclerosis 2013, 227, 140–146.
- Renke, G.; Starling-Soares, B.; Baesso, T.; Petronio, R.; Aguiar, D.; Paes, R. Effects of Vitamin D on Cardiovascular Risk and Oxidative Stress. Nutrients 2023, 15, 769.
- Pei, Y.Y.; Zhang, Y.; Peng, X.C.; Liu, Z.R.; Xu, P.; Fang, F. Association of Vitamin D Supplementation with Cardiovascular Events: A Systematic Review and Meta-Analysis. Nutrients 2022, 14, 3158.





