
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Saman Maleki Vareki | + 3397 word(s) | 3397 | 2020-11-24 15:35:10 | | | |
| 2 | Nicole Yin | -1298 word(s) | 2099 | 2020-11-26 05:19:04 | | |
Video Upload Options
The majority of pancreatic cancer patients have a poor prognosis, where the five-year survival rate is 9% in the United States, with an increasing incidence rate of 1.03% per year. Pancreatic ductal adenocarcinoma (PDAC) is an aggressive form of pancreatic cancer that makes up 90% of all diagnosed cases of pancreatic cancer. Other types of pancreatic cancer, such as neuroendocrine tumors, which secrete insulin, or acinar carcinomas, which release digestive enzymes, are less common. PDAC develops from neoplasms of the cells lining the pancreatic ducts and usually presents without symptoms until advanced stages of the disease. Here we discuss strategies for immunomodulation of pancreatic cancer.
1. Introduction
The majority of pancreatic cancer patients have a poor prognosis, where the five-year survival rate is 9% in the United States, with an increasing incidence rate of 1.03% per year[1][2]. Pancreatic ductal adenocarcinoma (PDAC) is an aggressive form of pancreatic cancer that makes up 90% of all diagnosed cases of pancreatic cancer[3]. Other types of pancreatic cancer, such as neuroendocrine tumors, which secrete insulin, or acinar carcinomas, which release digestive enzymes, are less common. PDAC develops from neoplasms of the cells lining the pancreatic ducts and usually presents without symptoms until advanced stages of the disease[4].
At this time, there are limited treatment options for patients with advanced and incurable PDAC, all of which are chemotherapy based. The FOLFIRINOX regimen (a combination of oxaliplatin, irinotecan, leucovorin, and fluorouracil) is often used as the first line of treatment for patients who are likely to be able to tolerate the relatively high toxicity[5][6]. The median overall survival for this regimen is 11.1 months[6]. Patients with comorbidities are often treated with gemcitabine alone or in combination with albumin-bound (nab)-paclitaxel with a median overall survival of only approximately 6.8 and 8.5 months, respectively[5][6][7]. Surgical resection remains the only potentially curative option, with a median overall survival of 54.4 months when combined with adjuvant FOLFIRINOX[8]. However, only about 20% of patients are considered resectable at the time of diagnosis[9].
Immunotherapy with immune checkpoint blockade (ICB) has been a breakthrough in treating some of the most treatment-refractory cancers, including advanced melanoma and metastatic non-small-cell lung carcinoma[10][11]. However, ICBs did not show efficacy in PDAC, and tumors showed primary resistance to monotherapy with ipilimumab (an anticytotoxic T lymphocyte antigen 4) or atezolizumab (anti-programmed cell death receptor ligand 1)[10][12]. Currently, the only approved immunotherapy for pancreatic cancer is pembrolizumab (anti-PD1), recommended for use in patients with mismatch repair deficiencies (dMMR) or microsatellite instability (MSI)-high tumors as a second line of treatment[13][14]. MSI-high tumors often have a higher tumor mutation burden and a more T-cell-inflamed microenvironment that is not typically seen in the immune-hostile PDAC tumor microenvironment. Modifying the tumor microenvironment to create a more T-cell-inflamed microenvironment might improve PDAC response to immunotherapy, either alone or in combination with other therapies.
2. Adjuvant and Neoadjuvant Therapies
Surgical resection is the best curative option for PDAC patients, although ultimately, 80% of those who undergo surgery recur, either due to micrometastases or microscopic residual disease in the tumor bed[1][15]. The current standard of care for upfront resectable PDAC is surgery followed by adjuvant combination chemotherapy[16]. The administration of gemcitabine and capecitabine after surgery resulted in median overall survival of 28.0 months, a modest increase compared to gemcitabine monotherapy with a median overall survival of 25.5 months[17]. The majority of patients in this trial had lymph node involvement. The efficacy of immunotherapy has also been tested in both neoadjuvant and adjuvant settings in other tumor types. Neoadjuvant immunotherapy has shown great promise primarily by reinvigorating exhausted T-cells before surgery. Tumor-specific CD8+ T-cells can be primed by antigens derived from the primary tumor and can continue to exert their cytotoxic effects on micrometastases once the primary tumor is removed[18]. While univariate analysis showed that neoadjuvant immunotherapy resulted in better overall survival than adjuvant immunotherapy in pancreatic cancer patients, multivariate analysis showed that those treatment strategies were not significantly different[19].
Interestingly, adjuvant immunotherapy combined with chemotherapy was more effective than chemotherapy alone[20]. The combination may be effective, as chemotherapy can ablate tumors and release tumor antigens in the process. These antigens can then prime T-cells. Furthermore, treatment strategies reducing desmoplasia allows T-cells to infiltrate the tumor microenvironment more effectively[21]. Administration of nab-paclitaxel was found to reduce the density of the desmoplastic stroma in preclinical models and facilitated the delivery of gemcitabine to the tumor[22].
The combination of radiation and chemotherapy was also effective in stimulating an anti-tumor immune response. Neoadjuvant chemoradiation given as 30 Gy of radiation combined with gemcitabine and a fluoropyrimidine derivative was found to increase the infiltration of both CD4+ and CD8+ T-cells. As expected, increased CD8+ T-cell infiltration of the tumors was associated with prolonged overall survival and lower recurrence rates in patients with resectable pancreatic cancer[23]. Another study assessing the effect of neoadjuvant chemoradiation showed no difference in the recruitment of CD4+ or CD8+ T-cells; however, a decrease in FOXP3+ Tregs was observed[24]. More studies are required to determine if T-cells’ recruitment can be further improved by optimizing the timing of treatment and surgery.
3. Combination Strategies
PDAC is a complex disease with several cellular components that can either hinder or promote anti-tumor immunity. Therefore, successful therapeutic strategies may combine several existing therapies. For example, a combination of different ICBs to chemotherapy has shown success in lung cancer. Chemotherapy can induce apoptosis of tumor cells, and in the process, release tumor antigens that can activate anti-tumor immunity. A randomized phase II trial (NCT0287931) compared the use of gemcitabine and nab-paclitaxel against gemcitabine and nab-paclitaxel combined with durvalumab (anti-PDL1) and tremelimumab (anti-CTLA-4). Of the 11 patients that received gemcitabine, nab-paclitaxel, durvalumab, and tremelimumab, 8 achieved a partial response, showing the potential of combination therapy[25]. A CD40 agonist is being combined with gemcitabine, nab-paclitaxel, and nivolumab (anti-PD1) in a phase 1b clinical trial (NCT02482168) in patients with metastatic PDAC. Of 24 patients, 14 had a partial response[26]. Currently, this trial has progressed to a phase II study (NCT03214250).
4. T-Cell Activation Strategies for PDAC Treatment
With the modest progress made with chemotherapy, radiation, and ICBs, novel treatment strategies for pancreatic cancer are actively being explored. Considering that CD8+ T-cells play a large role in the long-term survival of PDAC patients, approaches often involve activation of the anti-tumor immune response.
4.1. Chimeric Antigen Receptor (CAR) T-Cells
CAR T-cell therapy is an adoptive cell therapy, where autologous T-cells are isolated and genetically engineered to express receptors that bind to tumor antigens. These modified T-cells are then reinfused into the patient. When CAR T-cells recognize target antigens, they become activated and exert cytotoxic effects on the tumor cell (Figure 1a). Currently, CAR T-cell therapy has only been approved by the FDA for hematologic malignancies[27]. The safety of a mesothelin-specific CAR T-cell therapy was tested in six patients with chemotherapy-refractory metastatic PDAC. These patients did not experience a cytokine storm or dose-limiting toxicities. However, only two patients achieved stable disease with overall survival of 3.8 and 5.4 months[28]. Preclinical studies are also testing the efficacy of switchable CAR T-cells against human epithelial growth factor receptor 2 (HER2) antigen. Switchable CAR T-cells are composed of two parts. For the first part, the autologous T-cells are engineered with the signaling portion of the T-cell receptor and the second part consists of a “switch” protein that binds to both the signaling portion of the autologous T-cells and the tumor antigen. This allows the fine-tuning of the T-cell response by administering variable concentrations of the switch protein. The switch CAR T-cell against HER2 antigen led to the complete remission of xenograft models derived from patients with stage IV PDAC[29].
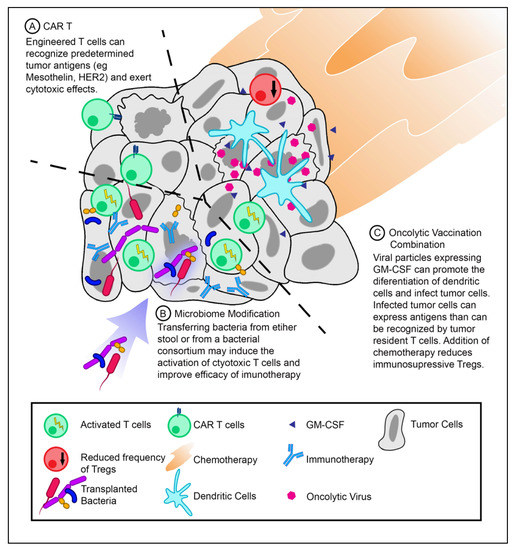
Figure 1. T-cell activation strategies for pancreatic ductal adenocarcinoma (PDAC) treatment. (A) Infusion of chimeric antigen receptor T-cells (CAR T-cells) against PDAC tumor antigens. CAR T-cells can recognize antigens specific for their CARs and exert cytotoxic effects. (B) Modifying the tumor microbiome may introduce novel antigens that can activate T-cells and improve the efficacy of immunotherapeutics. (C) Therapeutic vaccination with oncolytic viruses expressing granulocyte–macrophage colony-stimulating factor (GM-CSF) in combination with chemotherapy (low-dose cyclophosphamide) can increase the frequency of dendritic cells while decreasing the frequency of Tregs.
Unfortunately, engineered T-cells become progressively dysfunctional within the tumor and require repeated reinfusions to achieve a therapeutic benefit in experimental models[30]. One study attempted to mitigate this process by modulating TAM function. The administration of agonistic anti-CD40 along with CAR T-cells resulted in increased proliferation and cytotoxic abilities of CAR T-cells[31]. Notably, while the depletion of TAMs resulted in increased proliferation of endogenous T-cells, there was no marked increase in CAR T-cell infiltration of the tumor[31]. The efficacy of CAR T-cell function can also be improved by coexpressing an engineered immunomodulatory fusion protein. A fusion protein consisting of the inhibitory Fas receptor ectodomain and a stimulatory 4-1BB endodomain could convert inhibitory signals into activating ones. The use of CAR T-cells expressing the Fas-4-1BB fusion protein was found to significantly improve survival in an aggressive mouse model of pancreatic cancer[32]. This suggests that several methods can be developed to improve the efficacy of current CAR T-cell technology to treat pancreatic cancers.
4.2. Microbiome Modification
As mentioned previously, the tumor microbiome can predict the overall survival of PDAC patients. This suggests that modification of the microbiome can potentially increase the response to therapeutics. The microbiome can be altered either by antibiotics, FMT, or defined bacterial consortia (Figure 1b).
4.2.1. Antibiotics
Recently, the use of antibiotics has been shown to abrogate the effects of anti-PD1 immunotherapy in both melanoma and renal cell carcinoma[33]. However, the opposite was found to be true by Pushalkar et al.[34] in regard to PDAC. An increase in bacteria was found in the cancerous pancreas of mice compared to healthy pancreas. Decreasing bacterial abundance using broad-spectrum antibiotics was successful in slowing tumor growth in KC mice (spontaneous pancreatic neoplasia model). This growth was further attenuated by combining broad-spectrum antibiotics with anti-PD1. The use of antibiotics was found to increase the intratumoral CD8/CD4 T-cell ratio, which may explain the reduction in tumor growth (Figure 2a)[34]. Antibiotic treatment strategies could be employed in neoadjuvant settings to abrogate harmful bacteria before surgery. More studies are required to validate this strategy.
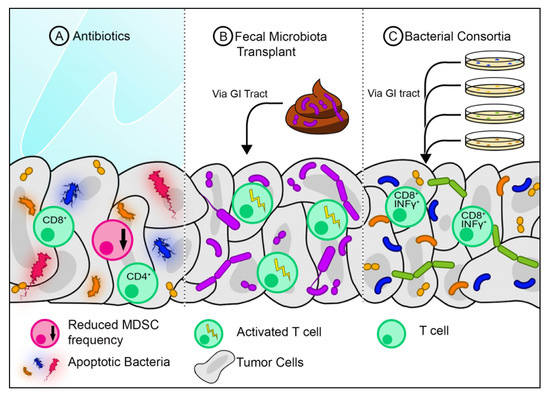
Figure 2. Strategies for modifying the tumor microbiome. (A) Antibiotics eliminate certain bacteria and may reduce frequencies of myeloid-derived suppressor cells (MDSC) while also increasing the frequency of CD4+ and CD8+ T-cells. (B) Fecal microbiota transplants from healthy individuals can introduce new bacteria into the gut, where in addition to re-establishing gut microbiome diversity, some of the newly introduced bacteria may translocate to the tumor. These bacteria may activate certain T-cell populations. (C) A Consortium of bacteria of known species grown in vitro can be introduced to the gut where it can translocate to the tumor. Certain combinations of bacterial species can activate anti-tumor CD8+ T-cells.
4.2.2. Fecal Microbiota Transplantation
FMT is commonly used to treat dysbiosis of the gut with a high success rate, such as with refractory Clostridium difficile infections. Presumably, FMT can be used to treat other conditions with microbial dysbiosis, including PDAC[35][36]. Akkermansia muciniphila, a commensal bacterium commonly found in healthy stool, was found to induce increased infiltration of CD4+ T-cells in RET melanomas when combined with the anti-PD1 antibody[33]. This suggests that certain bacteria found in healthy stool samples may boost immunity by activating certain populations of T-cells. Modifying the gut microbiome via FMT may also be an attractive strategy in the neoadjuvant setting for PDAC (Figure 2b).
4.2.3. Bacterial Consortia
The gut is colonized by various bacterial populations, some of which have a capacity to induce T-cell activation (Figure 2c). A consortium of 11 bacteria was found to increase the frequency of INFγ+-producing CD8+ T-cells in the intestines of germ-free mice. This consortium consisted of seven Bacteroidales and four non-Bacteroidales species, all of which needed to be administered in combination to achieve maximal T-cell activation. When administered with an anti-PD1 or anti-CTLA 4, the mix of 11 bacteria slowed tumor growth in mice[37]. This suggests that a mix of bacteria may be taken as a probiotic to improve the efficacy of immunotherapy. Whether this would benefit PDAC patients still needs to be explored.
4.3. Oncolytic Vaccine Combinations
Oncologic vaccines work to expose the host immune system to tumor-specific antigens. To date, vaccines on their own have shown no clinical benefits in pancreatic cancer[38]. However, there are some promising results indicative of inducing an anti-tumor immune response when vaccines are combined with chemotherapy. An irradiated, granulocyte-macrophage colony-stimulating factor (GM-CSF), secreting, allogeneic PDAC vaccine (GVAX) was given as a single agent or in combination with low-dose cyclophosphamide to patients with resectable PDAC. After two weeks of vaccine administration, tertiary lymphoid organs were found inside tumor biopsies. This indicates that lymphocytes are actively infiltrating the tumor microenvironment and facilitating an adaptive response[39].
References
- Siegel, R.L.; Miller, K.D.; Jemal, A. Cancer statistics, 2019. CA. Cancer J. Clin. 2019, 69, 7–34.
- Saad, A.M.; Turk, T.; Al-Husseini, M.J.; Abdel-Rahman, O. Trends in pancreatic adenocarcinoma incidence and mortality in the United States in the last four decades; A SEER-based study. BMC Cancer 2018, 18, 1–11.
- Michael Orth; Philipp Metzger; S. Gerum; Julia Mayerle; Günter Schneider; Claus Belka; Maximilian Schnurr; Kirsten Lauber; Pancreatic ductal adenocarcinoma: biological hallmarks, current status, and future perspectives of combined modality treatment approaches. Radiation Oncology 2019, 14, 1-20, 10.1186/s13014-019-1345-6.
- Jorg Kleeff; Murray Korc; Minoti Apte; Carlo La Vecchia; Colin D. Johnson; Andrew V. Biankin; Rachel E. Neale; Margaret Tempero; David A. Tuveson; Ralph H. Hruban; et al.John P. Neoptolemos Pancreatic cancer. Nature Reviews Disease Primers 2016, 2, 16022-16022, 10.1038/nrdp.2016.22.
- Muñoz Martín, A.J.; Adeva, J.; Martínez-Galán, J.; Reina, J.J.; Hidalgo, M. Pancreatic ductal adenocarcinoma: Metastatic disease. Clin. Transl. Oncol. 2017, 19, 1423–1429.
- Vaccaro, V.; Sperduti, I.; Milella, M. FOLFIRINOX versus gemcitabine for metastatic pancreatic cancer. N. Engl. J. Med. 2011, 365, 768–769.
- Daniel D. Von Hoff; Thomas Ervin; Francis P. Arena; E. Gabriela Chiorean; Jeffrey Infante; Malcolm Moore; Thomas Seay; Sergei A. Tjulandin; Wen Wee Ma; Mansoor N. Saleh; et al.Marion HarrisMichele ReniScot DowdenDaniel LaheruNathan BaharyRamesh K. RamanathanJosep TaberneroManuel HidalgoDavid GoldsteinEric Van CutsemXinyu WeiJose IglesiasMarkus F. Renschler Increased Survival in Pancreatic Cancer with nab-Paclitaxel plus Gemcitabine. New England Journal of Medicine 2013, 369, 1691-1703, 10.1056/nejmoa1304369.
- Thierry Conroy; Pascal Hammel; Mohamed Hebbar; Meher Ben Abdelghani; Alice C. Wei; Jean-Luc Raoul; Laurence Choné; Eric Francois; Pascal Artru; James J. Biagi; et al.Thierry LeComteEric AssenatRoger FarouxMarc YchouJulien VoletAlain SauvanetGilles BreysacherFrédéric Di FioreChristine CrippsPetr KavanPatrick TexereauKarine Bouhier-LeporrierFaiza Khemissa-AkouzJean-Louis LegouxBéata JuzynaSophie GourgouChristopher J. O’CallaghanClaire Jouffroy-ZellerPatrick RatDavid MalkaFlorence CastanJean-Baptiste Bachet FOLFIRINOX or Gemcitabine as Adjuvant Therapy for Pancreatic Cancer. New England Journal of Medicine 2018, 379, 2395-2406, 10.1056/nejmoa1809775.
- Jin He; Nita Ahuja; Martin A. Makary; John L. Cameron; Frederic E. Eckhauser; Michael A. Choti; Ralph H. Hruban; Timothy M. Pawlik; Christopher L. Wolfgang; 2564 resected periampullary adenocarcinomas at a single institution: trends over three decades. HPB 2014, 16, 83-90, 10.1111/hpb.12078.
- Brahmer, J.R.; Tykodi, S.S.; Chow, L.Q.M.; Hwu, W.J.; Topalian, S.L.; Hwu, P.; Drake, C.G.; Camacho, L.H.; Kauh, J.; Odunsi, K.; et al. Safety and activity of anti-PD-L1 antibody in patients with advanced cancer. N. Engl. J. Med. 2012, 366, 2455–2465.
- Topalian, S.L.; Hodi, F.S.; Brahmer, J.R.; Gettinger, S.N.; Smith, D.C.; McDermott, D.F.; Powderly, J.D.; Carvajal, R.D.; Sosman, J.A.; Atkins, M.B.; et al. Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N. Engl. J. Med. 2012, 366, 2443–2454.
- Richard E. Royal; Catherine Levy; Keli Turner; Aarti Mathur; Marybeth Hughes; Udai S. Kammula; Richard M. Sherry; Suzanne L. Topalian; James C. Yang; Israel Lowy; et al.Steven A. Rosenberg Phase 2 Trial of Single Agent Ipilimumab (Anti-CTLA-4) for Locally Advanced or Metastatic Pancreatic Adenocarcinoma. Journal of Immunotherapy 2010, 33, 828-833, 10.1097/cji.0b013e3181eec14c.
- Sohal, D.P.S.; Kennedy, E.B.; Khorana, A.; Copur, M.S.; Crane, C.H.; Garrido-Laguna, I.; Krishnamurthi, S.; Moravek, C.; O’Reilly, E.M.; Philip, P.A.; et al. Metastatic pancreatic cancer: ASCO clinical practice guideline update. J. Clin. Oncol. 2018, 36, 2545–2556.
- Marabelle, A.; Le, D.T.; Ascierto, P.A.; Di Giacomo, A.M.; de Jesus-Acosta, A.; Delord, J.P.; Geva, R.; Gottfried, M.; Penel, N.; Hansen, A.R.; et al. Efficacy of pembrolizumab in patients with noncolorectal high microsatellite instability/ mismatch repair–deficient cancer: Results from the phase II KEYNOTE-158 study. J. Clin. Oncol. 2020, 38, 1–10.
- Donghui Li; Keping Xie; Robert Wolff; James L. Abbruzzese; Pancreatic cancer. The Lancet 2004, 363, 1049-1057, 10.1016/s0140-6736(04)15841-8.
- Thomas Seufferlein; Thomas J. Ettrich; Treatment of pancreatic cancer-neoadjuvant treatment in resectable pancreatic cancer (PDAC).. Translational Gastroenterology and Hepatology 2019, 4, 21-21, 10.21037/tgh.2019.03.05.
- John P Neoptolemos; Daniel H Palmer; Paula Ghaneh; Eftychia E Psarelli; Juan W Valle; Christopher M Halloran; Olusola Faluyi; Derek A O'reilly; David Cunningham; Jonathan Wadsley; et al.Suzanne DarbyTim MeyerRoopinder GillmoreAlan AnthoneyPehr LindBengt GlimeliusStephen FalkJakob R IzbickiGary William MiddletonSebastian CumminsPaul J RossHarpreet WasanAlec McDonaldTom CrosbyYuk Ting MaKinnari PatelDavid SherriffRubin SoomalDavid BorgSharmila SothiPascal HammelThilo HackertRichard JacksonMarkus W Büchler Comparison of adjuvant gemcitabine and capecitabine with gemcitabine monotherapy in patients with resected pancreatic cancer (ESPAC-4): a multicentre, open-label, randomised, phase 3 trial. The Lancet 2017, 389, 1011-1024, 10.1016/s0140-6736(16)32409-6.
- Jake S. O'donnell; Esmée P. Hoefsmit; Mark J. Smyth; Christian U. Blank; Michele Wl Teng; The Promise of Neoadjuvant Immunotherapy and Surgery for Cancer Treatment. Clinical Cancer Research 2019, 25, 5743-5751, 10.1158/1078-0432.ccr-18-2641.
- Saber Amin; Michael Baine; Jane Meza; Chi Lin; The impact of neoadjuvant and adjuvant immunotherapy on the survival of pancreatic cancer patients: a retrospective analysis. BMC Cancer 2020, 20, 1-10, 10.1186/s12885-020-07016-8.
- Thuy B. Tran; Vijay K. Maker; Ajay V. Maker; Impact of Immunotherapy after Resection of Pancreatic Cancer. Journal of the American College of Surgeons 2019, 229, 19-27.e1, 10.1016/j.jamcollsurg.2019.01.016.
- Abasi Ene–Obong; Andrew J. Clear; Jennifer Watt; Jun Wang; Rewas Fatah; John C. Riches; John F. Marshall; Joanne Chin–Aleong; Claude Chelala; John G. Gribben; et al.Alan G. RamsayHemant M. Kocher Activated Pancreatic Stellate Cells Sequester CD8+ T Cells to Reduce Their Infiltration of the Juxtatumoral Compartment of Pancreatic Ductal Adenocarcinoma. Gastroenterology 2013, 145, 1121-1132, 10.1053/j.gastro.2013.07.025.
- Daniel D. Von Hoff; Ramesh K. Ramanathan; Mitesh J. Borad; Daniel A. Laheru; Lon S. Smith; Tina E. Wood; Ronald L. Korn; Neil Desai; Vuong Trieu; Jose L. Iglesias; et al.Hui ZhangPatrick Soon-ShiongTao ShiN.V. RajeshKumarAnirban MaitraManuel Hidalgo Gemcitabine Plusnab-Paclitaxel Is an Active Regimen in Patients With Advanced Pancreatic Cancer: A Phase I/II Trial. Journal of Clinical Oncology 2011, 29, 4548-4554, 10.1200/jco.2011.36.5742.
- Yuki Homma; Koichi Taniguchi; Takashi Murakami; Kazuya Nakagawa; Masatoshi Nakazawa; Ryusei Matsuyama; Ryutaro Mori; Kazuhisa Takeda; Michio Ueda; Yasushi Ichikawa; et al.Kuniya TanakaItaru Endo Immunological Impact of Neoadjuvant Chemoradiotherapy in Patients with Borderline Resectable Pancreatic Ductal Adenocarcinoma. Annals of Surgical Oncology 2013, 21, 670-676, 10.1245/s10434-013-3390-y.
- Takahiro Tsuchikawa; Satoshi Hirano; Eiichi Tanaka; Joe Matsumoto; Kentaro Kato; Toru Nakamura; Yuma Ebihara; Toshiaki Shichinohe; Novel aspects of preoperative chemoradiation therapy improving anti-tumor immunity in pancreatic cancer. Cancer Science 2013, 104, 531-535, 10.1111/cas.12119.
- Daniel John Renouf; Neesha C. Dhani; Petr Kavan; Derek J. Jonker; Alice Chia-Chi Wei; Tina Hsu; Patricia A. Tang; Barbara Graham; Lisa Gallinaro; Tasnia Hasan; et al.Weiwei LiKate HartDongsheng TuChristopher J. O'callaghan The Canadian Cancer Trials Group PA.7 trial: Results from the safety run in of a randomized phase II study of gemcitabine (GEM) and nab-paclitaxel (Nab-P) versus GEM, nab-P, durvalumab (D), and tremelimumab (T) as first-line therapy in metastatic pancreatic ductal adenocarcinoma (mPDAC).. Journal of Clinical Oncology 2018, 36, 349-349, 10.1200/jco.2018.36.4_suppl.349.
- Mark H. O'hara; Eileen M. O'reilly; Mick Rosemarie; Gauri Varadhachary; Zev A. Wainberg; Andrew Ko; George A. Fisher; Osama Rahma; Jaclyn P. Lyman; Christopher R. Cabanski; et al.Erica L. CarpenterTravis HollmannPier Federico GherardiniLacey KitchCheryl SelinskyTheresa LavalleeOvid C. TrifanUte DuganVanessa M. Hubbard-LuceyRobert H. Vonderheide Abstract CT004: A Phase Ib study of CD40 agonistic monoclonal antibody APX005M together with gemcitabine (Gem) and nab-paclitaxel (NP) with or without nivolumab (Nivo) in untreated metastatic ductal pancreatic adenocarcinoma (PDAC) patients. Clinical Trials 2019, 79, CT004-CT004, 10.1158/1538-7445.sabcs18-ct004.
- Varada Date; Sujit Nair; Emerging vistas in CAR T-cell therapy: challenges and opportunities in solid tumors. Expert Opinion on Biological Therapy 2020, null, 1-16, 10.1080/14712598.2020.1819978.
- Gregory L. Beatty; Mark H. O’Hara; Simon F. Lacey; Drew A. Torigian; Farzana Nazimuddin; Fang Chen; Irina M. Kulikovskaya; Michael C. Soulen; Maureen McGarvey; Anne Marie Nelson; et al.Whitney L. GladneyBruce L. LevineJ. Joseph MelenhorstGabriela PlesaCarl H. June Activity of Mesothelin-Specific Chimeric Antigen Receptor T Cells Against Pancreatic Carcinoma Metastases in a Phase 1 Trial. Gastroenterology 2018, 155, 29-32, 10.1053/j.gastro.2018.03.029.
- Deepak Raj; Ming-Hsin Yang; David Rodgers; Eric N Hampton; Julfa Begum; Arif Mustafa; Daniela Lorizio; Irene Garces; David Propper; James G Kench; et al.H M KocherTravis S. YoungAlexandra AicherChristopher Heeschen Switchable CAR-T cells mediate remission in metastatic pancreatic ductal adenocarcinoma. Gut 2018, 68, 1052-1064, 10.1136/gutjnl-2018-316595.
- Ingunn M. Stromnes; Thomas M. Schmitt; Ayaka Hulbert; J. Scott Brockenbrough; Hieu N. Nguyen; Carlos Cuevas; Ashley M. Dotson; Xiaoxia Tan; Jennifer L. Hotes; Philip D. Greenberg; et al.Sunil R. Hingorani T Cells Engineered against a Native Antigen Can Surmount Immunologic and Physical Barriers to Treat Pancreatic Ductal Adenocarcinoma. Cancer Cell 2015, 28, 638-652, 10.1016/j.ccell.2015.09.022.
- Ingunn M. Stromnes; Adam L. Burrack; Ayaka Hulbert; Patrick Bonson; Cheryl Black; J. Scott Brockenbrough; Jackson F. Raynor; Ellen J. Spartz; Robert H. Pierce; Philip D. Greenberg; et al.Sunil R. Hingorani Differential Effects of Depleting versus Programming Tumor-Associated Macrophages on Engineered T Cells in Pancreatic Ductal Adenocarcinoma. Cancer Immunology Research 2019, 7, 977-989, 10.1158/2326-6066.cir-18-0448.
- Shannon K. Oda; Kristin G. Anderson; Pranali Ravikumar; Patrick Bonson; Nicolas M. Garcia; Cody M. Jenkins; Summer Zhuang; Andrew W. Daman; Edison Y. Chiu; Breanna M. Bates; et al.Philip D. Greenberg A Fas-4-1BB fusion protein converts a death to a pro-survival signal and enhances T cell therapy. Journal of Experimental Medicine 2020, 217, e20191166, 10.1084/jem.20191166.
- Bertrand Routy; Emmanuelle Le Chatelier; Lisa DeRosa; Connie P. M. Duong; Maryam Tidjani Alou; Romain Daillère; Aurélie Fluckiger; Meriem Messaoudene; Conrad Rauber; Maria P. Roberti; et al.Marine FidelleCaroline FlamentVichnou Poirier-ColamePaule OpolonChristophe KleinKristina IribarrenLaura MondragónNicolas JacquelotMinard-Colin VéroniqueGladys FerrereCéline ClémensonLaura MezquitaJordi Remon MasipCharles NaltetSolenn BrosseauCoureche KaderbhaiCorentin RichardHira RizviFlorence LevenezNathalie GalleronBenoit QuinquisNicolas PonsBernhard RyffelVéronique Minard-ColinPatrick GoninJean-Charles SoriaEric DeutschYohann LoriotFrançois GhiringhelliGérard ZalcmanFrançois GoldwasserBernard EscudierMatthew D. HellmannAlexander EggermontDidier RaoultLaurence AlbigesGuido KroemerLaurence Zitvogel Gut microbiome influences efficacy of PD-1–based immunotherapy against epithelial tumors. Science 2017, 359, 91-97, 10.1126/science.aan3706.
- Smruti Pushalkar; Mautin Hundeyin; Donnele Daley; Constantinos P. Zambirinis; Emma Kurz; Ankita Mishra; Navyatha Mohan; Berk Aykut; Mykhaylo Usyk; Luisana E. Torres; et al.Gregor WerbaKevin ZhangYuqi GuoQianhao LiNeha AkkadSarah LallBenjamin WadowskiJohana GutierrezJuan Andres Kochen RossiJeremy W. HerzogBrian DiskinAlejandro Torres-HernandezJosh LeinwandWei WangPardeep S. TaunkShivraj SavadkarMalvin JanalAnjana SaxenaXin LiDeirdre CohenR. Balfour SartorDeepak SaxenaGeorge Miller The Pancreatic Cancer Microbiome Promotes Oncogenesis by Induction of Innate and Adaptive Immune Suppression. Cancer Discovery 2018, 8, 403-416, 10.1158/2159-8290.cd-17-1134.
- Erick Riquelme; Yu Zhang; Liangliang Zhang; Maria Montiel; Michelle Zoltan; Wenli Dong; Pompeyo Quesada; Ismet Sahin; Vidhi Chandra; Anthony San Lucas; et al.Paul ScheetHanwen XuSamir M. HanashLei FengJared K. BurksKim-Anh DoChristine B. PetersonDeborah NejmanChing-Wei D. TzengMichael P. KimCynthia L. SearsNadim AjamiJoseph PetrosinoLaura D. WoodAnirban MaitraRavid StraussmanMatthew KatzJames Robert WhiteRobert JenqJennifer WargoFlorencia McAllister Tumor Microbiome Diversity and Composition Influence Pancreatic Cancer Outcomes. Cell 2019, 178, 795-806.e12, 10.1016/j.cell.2019.07.008.
- Ryan M Chanyi; Laura Craven; Brandon Harvey; Gregor Reid; Michael J Silverman; Jeremy P. Burton; Faecal microbiota transplantation: Where did it start? What have studies taught us? Where is it going?. SAGE Open Medicine 2017, 5, 205031211770871, 10.1177/2050312117708712.
- Takeshi Tanoue; Satoru Morita; Damian R. Plichta; Ashwin N. Skelly; Wataru Suda; Yuki Sugiura; Seiko Narushima; Hera Vlamakis; Iori Motoo; Kayoko Sugita; et al.Atsushi ShiotaKozue TakeshitaKeiko Yasuma-MitobeDieter RiethmacherTsuneyasu KaishoJason M. NormanDaniel MucidaMakoto SuematsuTomonori YaguchiVanni BucciTakashi InoueYutaka KawakamiBernat OlleBruce RobertsMasahira HattoriRamnik J. XavierKoji AtarashiKenya Honda A defined commensal consortium elicits CD8 T cells and anti-cancer immunity. Nature 2019, 565, 600-605, 10.1038/s41586-019-0878-z.
- Gregory L. Beatty; Shabnam Eghbali; Rebecca Kim; Deploying Immunotherapy in Pancreatic Cancer: Defining Mechanisms of Response and Resistance. American Society of Clinical Oncology Educational Book 2017, 37, 267-278, 10.1200/edbk_175232.
- Eric R. Lutz; Annie A. Wu; Elaine Bigelow; Rajni Sharma; Guanglan Mo; Kevin Soares; Sara Solt; Alvin Dorman; Anthony Wamwea; Allison Yager; et al.Daniel LaheruChristopher L. WolfgangJiang WangRalph H. HrubanRobert A. AndersElizabeth M. JaffeeLei Zheng Immunotherapy Converts Nonimmunogenic Pancreatic Tumors into Immunogenic Foci of Immune Regulation. Cancer Immunology Research 2014, 2, 616-631, 10.1158/2326-6066.cir-14-0027.





