Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Dalibor Mijaljica | -- | 2103 | 2022-04-20 23:29:26 | | | |
| 2 | Peter Tang | Meta information modification | 2103 | 2022-04-21 04:12:48 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Mijaljica, D.; Spada, F.; Harrison, I. Soaps and Syndets in Skin Cleansing. Encyclopedia. Available online: https://encyclopedia.pub/entry/22051 (accessed on 08 June 2026).
Mijaljica D, Spada F, Harrison I. Soaps and Syndets in Skin Cleansing. Encyclopedia. Available at: https://encyclopedia.pub/entry/22051. Accessed June 08, 2026.
Mijaljica, Dalibor, Fabrizio Spada, Ian Harrison. "Soaps and Syndets in Skin Cleansing" Encyclopedia, https://encyclopedia.pub/entry/22051 (accessed June 08, 2026).
Mijaljica, D., Spada, F., & Harrison, I. (2022, April 20). Soaps and Syndets in Skin Cleansing. In Encyclopedia. https://encyclopedia.pub/entry/22051
Mijaljica, Dalibor, et al. "Soaps and Syndets in Skin Cleansing." Encyclopedia. Web. 20 April, 2022.
Copy Citation
Skin cleansers generally come in one of two types: soap-based and synthetic detergents, or syndets. While the latter can effectively maintain the native skin structure, function and integrity, the former tends to negatively affect the skin by causing barrier disruption, lipid dissolution and pH alteration. Despite this, soap is still often preferred, possibly due to the negative connotations around anything that is not perceived as ‘natural’.
capacity
charge
ingredient
mildness
pH
cleanser
skin
soap
surfactant
syndet
1. Introduction
The stratum corneum (SC) is the uppermost layer of the skin’s epidermis, and is a biochemically complex but highly organised interface with the external environment. The SC is usually described as a ‘bricks and mortar’ structure in which the protein enriched, flattened corneocytes (dead keratinocytes lacking vital cellular organelles) are the ‘bricks’, and the lipid-rich matrix in which they are embedded is the ‘mortar’ [1]. This lipid matrix predominantly contains ceramides (40–50%), cholesterol (25%) and free fatty acids (10–15%) [2][3][4][5]. These three major classes of lipids within the SC are biophysically and biochemically distinct from other conventional eukaryotic membrane constituents (e.g., glycerolipids, sphingolipids, sterols) that are involved in the structural and functional landscape of the cell membrane’s lipid bilayers [6]. SC lipid precursors are generated during keratinocyte differentiation, and are afterwards intracellularly packaged into lamellar bodies in a highly ordered manner and subsequently enzymatically converted and eventually secreted into the extracellular domain of the SC [2][3][7]. The SC lipids spontaneously and in an orderly manner form multiple bilayers, which interact with corneocyte envelope-bound lipids [4][8]. In deeper layers of the SC, lipids are predominantly ordered into a densely packed orthorhombic crystalline configuration, which acts as a restrictive barrier to liquid transport. Closer to the SC surface, the lipids form a dispersed hexagonal lattice configuration that permits more liquid to pass through more freely [9][10].
The highly ordered SC lipid configuration is characterised by its unique properties, composition, and the specialised compartmentalisation within the lamellar lipid membrane, which maintains SC water content, regulates water flux, and modifies the rate and magnitude of transepidermal water loss (TEWL). Such mechanisms are highly dynamic and function continuously to maintain homeostasis of the SC, the epidermis and the skin in its entirety [2]. As such, the SC is a robust factory that is in operation at all times, ensuring the maintenance of the skin’s adaptive and protective barrier [2][11]. Exogenous stressors can impede the skin’s protective properties, so reducing exposure to, and minimising practices such as skin cleansing with, harsh cleansers (e.g., alkaline soaps) that can cause perturbation and damage to the SC proteins, lipids and natural moisturising factor (NMF) components (e.g., free amino acids, sugars) is critical to decreasing the stress load on the skin’s structural and functional integrity [2].
It is generally recognised [7][9][12][13][14] that all types of skin, from healthy to diseased, infant to aged, need to be kept clean in order to preserve their barrier properties. The main objective of skin cleansing is to remove impurities from the skin’s surface [15][16] and to control its odour, without removing protective SC surface proteins and lipids, affecting skin microbiota [17] or altering pH [13][18]. This can be a substantial challenge, as the skin’s composition and barrier integrity are intricate, inconsistent, and dynamic, as described above [13][18].
As most of the impurities and contaminants that are found on the skin’s surface are not water-soluble, cleansing the skin with water alone is inadequate; hence, there is a need for surfactant-containing products [15]. Unlike water, surfactant-containing products are capable of breaking down and emulsifying most of those skin impurities and contaminants into finer particles and enabling their subsequent detachment and removal from the surface of the skin [3][7]. This makes surfactants a key component of skin maintenance. However, not all surfactants are created equal, with some, namely soap-based surfactants, creating more problems than they address [3][9][10][13][16][17][19][20][21][22][23][24][25][26][27][28][29][30][31].
2. Soaps vs. Syndets: Similarities and Differences
A diverse range of skin cleansers exist today, but they all generally fall into two types: soap-based and syndets. Both soap- and syndet-based cleansers contain at least one (often more than one) surfactant, a class of organic compounds that are amphiphilic/amphipathic, that is, they contain both nonpolar or hydrophobic (water-hating and lipid-loving) moieties, also known as ‘tails’, and polar or hydrophilic (water-loving) moieties, also known as ‘heads’. Therefore, they are soluble in both water and organic solvents [21]. Due to surfactants’ unique chemistry and characteristics, hydrophobic compounds present in excess sebum and other undesired substances (e.g., dirt, oils) on the skin’s surface are washed away with greater ease than could be achieved with water alone [7][9][12][13].
While soaps and syndets are similar in that they cleanse dirt and impurities from the surface of the skin, their distinct chemical properties and physiological effects can be markedly different [3][9][10][13][16][17][19][20][21][22][23][24][25][26][27][28][29][30][31] (Figure 1).
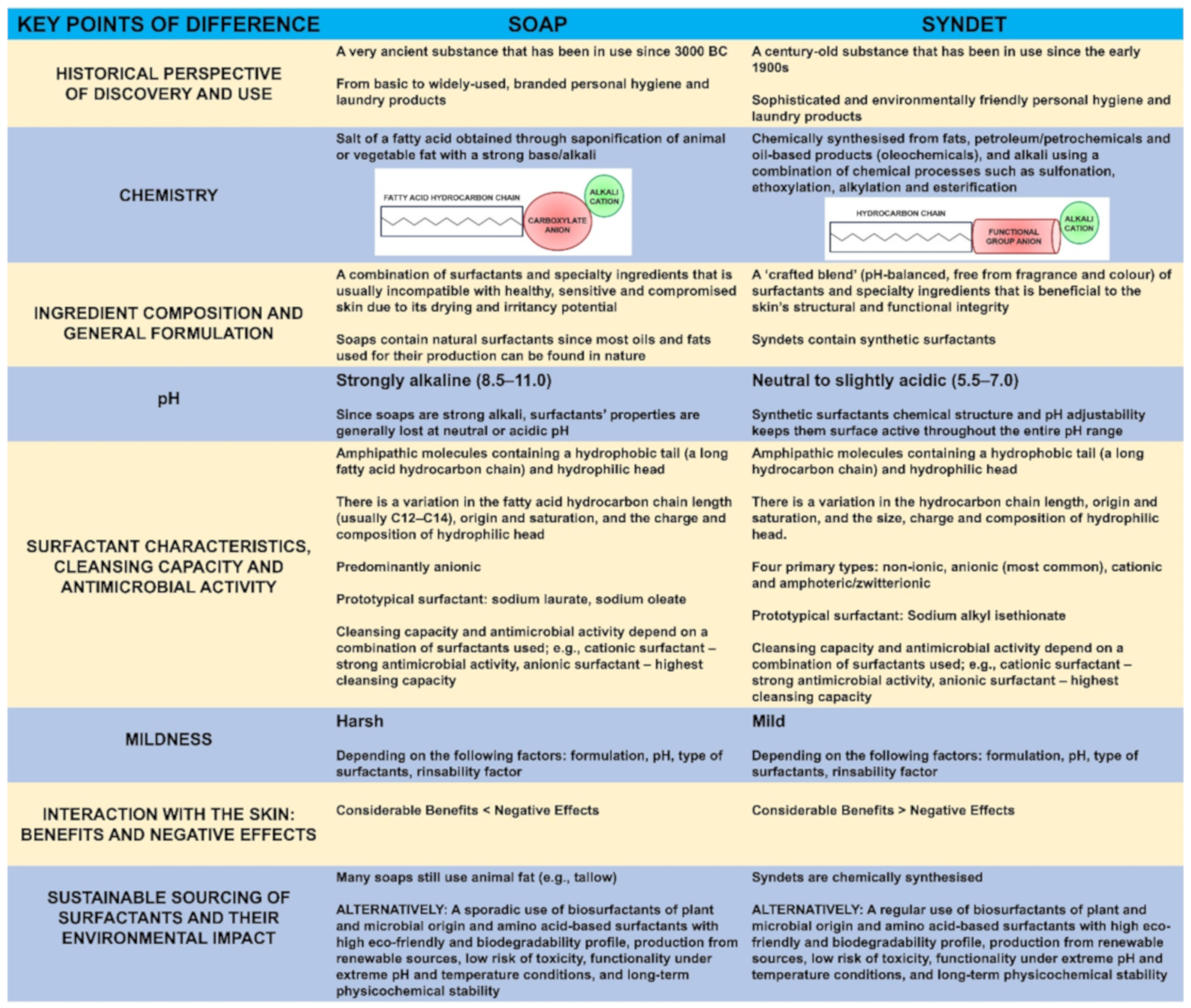
2.1. Soaps vs. Syndets: Key Points of Difference
The key points of difference between soaps and syndets (Figure 1) include the following: their historical perspective of discovery and use [19][29]; chemistry [9][16][24][29]; ingredient composition and general formulation [3][17][25]; pH [22][24][25]; surfactant characteristics [13][21][32], cleansing capacity [13][16][21][27][32][33] and antimicrobial activity [23][28]; mildness [13][16][21][27]; sustainable sourcing of surfactants and their environmental impact [26][30][34][35][36]; and interaction with the skin [3], associated benefits and negative effects [3][9][10][20][25].
3. Effects of Mild Syndets and Harsh Soaps on the Skin
Selecting an optimal and suitable cleanser is key to maintaining the skin acid mantle, its barrier function and integrity, and preserving the skin’s overall health at the same time. The exact needs of the skin differ with age and skin condition (Figure 2). Therefore, it is essential to understand these needs and differences in order to identify the most suitable cleanser for every situation. For instance, thinner skin can be more prone to TEWL, so soaps may increase this negative effect by exacerbating TEWL, whereas syndets may limit further TEWL and improve hydration. It seems that the interaction of mild syndets with the skin can be beneficial for almost every situation and will tip the balance as the positives outweigh the negatives, whereas the interaction of harsh soaps with the skin can have a much greater potential to cause a range of negative effects such as impaired barrier function, dryness and irritancy, and will tip the balance towards the negative effects (Figure 2). Therefore, fine-tuning of the complex characteristics of cleansers is absolutely necessary in order to produce cleansing formulations with optimal benefits and minimal adverse effects [7][9][12][13].
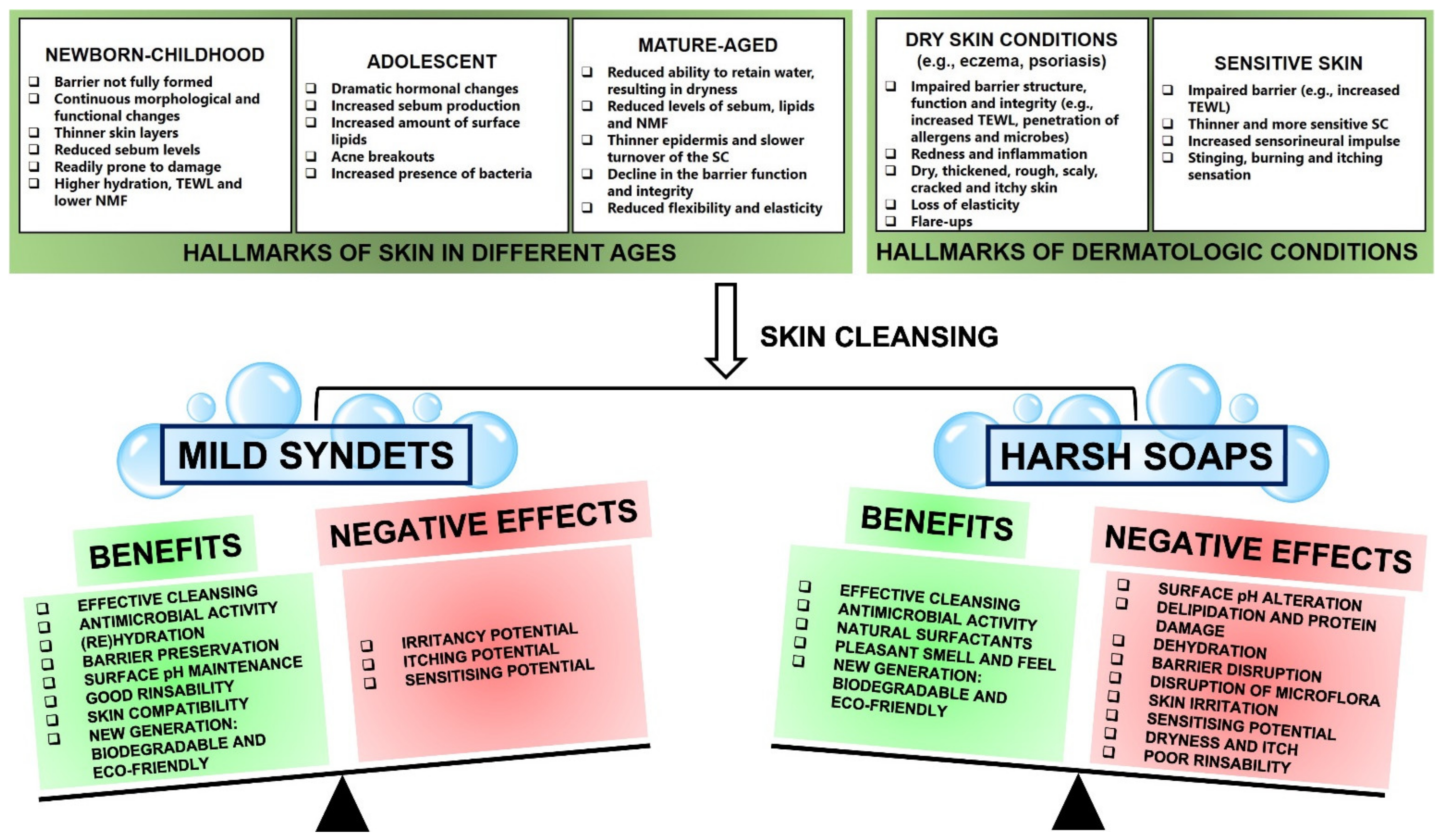
3.1. Mild Syndets: Considerable Benefits and Minimal Negative Effects
Children in general, especially newborns and infants, have a unique skin structure and physiology. While newborn skin is still not fully formed, it is sufficiently mature to cope with the usual demands of life. The skin continuously undergoes a period of rapid anatomical and physiological transformation, particularly in relation to SC hydration, TEWL, sebum and NMF production, development of the skin barrier (in terms of structural and functional integrity), the transition to a more acidic skin surface and skin maturation [13][38][39]. This process of maturation and morphological and functional changes continues for several years, indicating that newborn-childhood skin is particularly vulnerable to sensitisation, inflammation, irritation and unfavourable changes in skin barrier function [13][39] (Figure 2). Therefore, it is an imperative to use a suitable cleanser with mild properties for a child’s skin [39].
At puberty, the levels of circulating growth and reproduction hormones increase dramatically, causing various changes in the skin, including a high prevalence of acne [13]. A defining characteristic of acne is abnormal sebum production, making the skin oily, an issue that can be compounded by the drying nature of acne medication, such as benzoyl peroxide. Thus, effective cleansers, especially facial cleansers for acne management, must satisfy two opposing needs: (1) removal of sebum and (2) maintaining skin moisture [13]. A mild, fragrance-free and irritant-free cleanser with good rinsability is the recommended cleanser for acne management [7][13]. The cleansing regimen should suit the needs of the individual patient [7][14] (Figure 2).
At the other end of the spectrum, aged skin is characterised by changes such as impaired barrier function, thinner epidermis, reduced skin elasticity and decreased sweat and sebum production. Such changes ultimately result in a reduced ability of the skin to retain water, eventually leading to dry and fragile skin [13][40]. When it comes to cleansing aged skin, the recommendations remain the same as that for young skin: avoid alkaline cleansers and use products that are mild in nature, and able to maintain or even replenish the skin’s moisture [40] (Figure 2).
In individuals with dry skin conditions, including eczema, the use of traditional soap with its characteristic high pH can aggravate the skin, leading to loss of intracellular lipids, leaving the skin with a red, rough and scaly appearance [13][41]. This damage can potentially expose dermal nerve endings (a hallmark of sensitive skin), resulting in itching, burning, and pain [42]. Skin barrier impairment can also contribute to the penetration of allergens and an increased colonisation of bacteria such as S. aureus. Again, when it comes to cleansing, the recommendations remain similar: use mildly acidified syndets for cleansing, with an adjusted pH value in order to reduce the participation of infectious organisms, irritants, or allergens as well as to minimise irritation and itching potential [7][13][14][41] (Figure 2).
Unfortunately, even syndets with favourable mildness can potentially remove skin’s essential constituents, compromise the integrity and functionality of the SC, and can inevitably result in some weakening of the skin barrier, sensitisation and irritation (Figure 2). Thus, skin cleansing activity should be conducted with care because the careless use of skin cleansers in general, and especially the use of harsh alkaline soaps, will undoubtedly cause adverse skin reactions [43]. A best-suited and mild-in-nature cleanser such as a syndet should effortlessly and simultaneously maintain a fine balance between skin cleansing on the one hand and the preservation of the skin’s homeostatic properties on the other, with minimal to no irritation, disruption of, or damage to the skin’s physiological parameters, including hydration, acid mantle, and thus, overall barrier function [3][7].
3.2. Harsh Soaps: Extensive Short-Term and Long-Term Negative Effects and Some Benefits
Harsh soaps have the potential and aggressiveness to initiate changes to SC proteins, lipids and pH, disrupt resident microflora, and progressively increase damage over time, which in turn can cause a fundamental destruction of the barrier integrity that underpins skin health (Figure 2). Overall, the use of harsh soaps can cause cumulative skin effects including dryness, roughness, scaling, after-wash tightness, irritation and itching [7][14][17][20][37] (Figure 3).
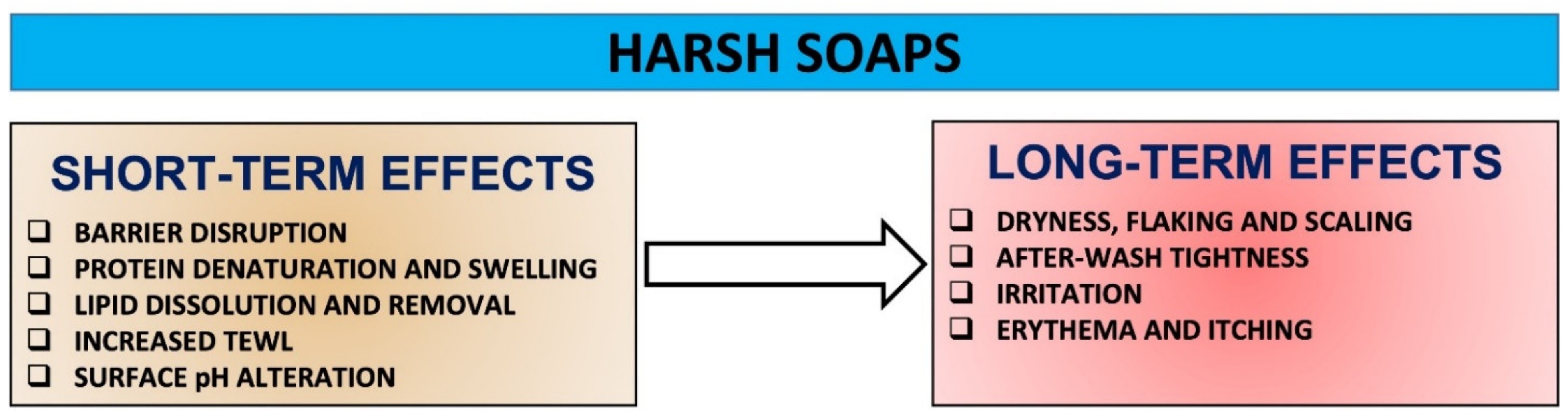
Most of the water absorbed by the SC during cleansing is present within the corneocytes. This results in a significant protein denaturation and swelling, and ultimate keratinocyte damage. Harsh soaps increase the swelling further, and the extent of surfactant-induced swelling is dependent upon the surfactant’s nature and its irritation potential. In addition, harsh soaps binding to proteins may also reduce the water-holding capacity of proteins. For example, the extent of swelling in the presence of sodium laurate-containing soap is significantly higher than that in the presence of a sodium cocoyl isethionate-containing syndet [20]. Furthermore, harsh soaps have been shown to remove NMF components and cause damage to the corneocyte envelope [20]. Therefore, the higher loss of water-soluble proteins after a single wash with soap vs. syndet is consistent with the greater damage potential of soap, depending on its structural and charge-density differences, direct effects of pH on the SC, and/or indirect effects of pH on the solution chemistry of charged head groups [7][14][20]. As water evaporates at a rapid rate from the upper layers of the skin, a differential stress is created in the SC, and this is thought to be the origin of the after-wash tightness [20].
Harsh soaps have an ability to disrupt and potentially damage bilayer lipids by extracting endogenous cholesterol, fatty acids and ceramides or intercalating into the lipid bilayer. Lipid barrier dissolution has numerous clinical consequences for the skin, including dryness, increased TEWL, fissuring, flaking, erythema and itch [14]. For example, insertion of anionic surfactants into the lipid bilayer can induce charge disruption in the bilayer and abruptly disturb membrane packing and organisation, permeability and overall structural and functional integrity. Even a subtle or partial removal of such lipids can make the lipid bilayer unstable [14][20]. It was shown that a harsh soap removes more cholesterol than a syndet [20]. While the exact reasons for this difference are not clear at present, it is likely that the alkaline pH of soap allows ionisation of the bilayer fatty acids, allowing easier cholesterol extraction from the SC. Furthermore, it is possible that the increased swelling of soap-damaged SC allows deeper layers of the SC to be readily exposed to the soap [20].
References
- Évora, A.S.; Adams, M.J.; Johnson, S.A.; Zhang, Z. Corneocytes: Relationship between Structural and Biomechanical Properties. Ski. Pharmacol. Physiol. 2021, 34, 146–161.
- Del Rosso, J.Q.; Levin, J. The clinical relevance of maintaining the functional integrity of the stratum corneum in both healthy and disease-affected skin. J. Clin. Aesthetic Dermatol. 2011, 4, 22–42.
- Mukherjee, S.; Chandrashekar, B.; Gaikwad, R. Cleansers: To use or not to use. Indian J. Paediatr. Dermatol. 2015, 16, 193–197.
- Das, C.; Olmsted, P.D. The physics of stratum corneum lipid membranes. Philos. Trans. R. Soc. London. Ser. A Math. Phys. Eng. Sci. 2016, 374, 20150126.
- Lefèvre-Utile, A.; Braun, C.; Haftek, M.; Aubin, F. Five Functional Aspects of the Epidermal Barrier. Int. J. Mol. Sci. 2021, 22, 11676.
- Dingjan, T.; Futerman, A.H. The fine-tuning of cell membrane lipid bilayers accentuates their compositional complexity. BioEssays 2021, 43, 2100021.
- Mukhopadhyay,, P. Cleansers and their role in various dermatological disorders. Indian J. Dermatol. 2011, 56, 2–6.
- Mundstock, A.; Abdayem, R.; Pirot, F.; Haftek, M. Alteration of the Structure of Human Stratum Corneum Facilitates Transdermal Delivery. Open Dermatol. J. 2014, 8, 72–79.
- Ananthapadmanabhan, K.P.; Moore, D.; Subramanyan, K.; Misra, M.; Meyer, F. Cleansing without compromise: The impact of cleansers on the skin barrier and the technology of mild cleansing. Dermatol. Ther. 2004, 17, 16–25.
- Ananthapadmanabhan, K.; Mukherjee, S.; Chandar, P. Stratum corneum fatty acids: Their critical role in preserving barrier integrity during cleansing. Int. J. Cosmet. Sci. 2013, 35, 337–345.
- Wilson, M. The importance of skin cleansing for people with incontinence. Nurs. Resid. Care 2017, 19, 321–326.
- Draelos, Z.; Hornby, S.; Walters, R.; Appa, Y. Hydrophobically modified polymers can minimize skin irritation potential caused by surfactant-based cleansers. J. Cosmet. Dermatol. 2013, 12, 314–321.
- Reis, C.M.S.; Reis-Filho, E. Cleansers; Clinical Approaches and Procedures in Cosmetic Dermatology; Springer: Berlin/Heidelberg, Germany, 2016; pp. 1–10. Available online: https://link.springer.com/referenceworkentry/10.1007/978-3-319-20250-1_14-1 (accessed on 11 January 2022).
- Navare, B.; Thakur, S.; Nakle, S. A review on surfactants: Role in skin, irritation, SC damage, and effect of mild cleansing over damaged skin. Int. J. Adv. Res. Ideas Innov. Technol. 2019, 5, 1077–1081.
- Greive, K. Cleansers and moisturisers: The basics. Wound Pract. Res. J. Aust. Wound Manag. Assoc. 2015, 23, 76–81.
- Li, Z. Modern Mild Skin Cleansing. J. Cosmet. Dermatol. Sci. Appl. 2020, 10, 85–98.
- Walters, R.M.; Mao, G.; Gunn, E.T.; Hornby, S. Cleansing Formulations That Respect Skin Barrier Integrity. Dermatol. Res. Pr. 2012, 2012, 495917.
- Wong, R.; Geyer, S.; Weninger, W.; Guimberteau, J.-C.; Wong, J.K. The dynamic anatomy and patterning of skin. Exp. Dermatol. 2016, 25, 92–98.
- Routh, H.B.; Bhowmik, K.R.; Parish, L.C.; Witkowski, J.A. Soaps: From the phoenicians to the 20th century—A historical review. Clin. Dermatol. 1996, 14, 3–6.
- Flynn, T.C.; Petros, J.; Clark, R.E.; Viehman, G.E. Dry skin and moisturizers. Clin. Dermatol. 2001, 19, 387–392.
- Corazza, M.; Lauriola, M.M.; Zappaterra, M.; Bianchi, A.; Virgili, A. Surfactants, skin cleansing protagonists. J. Eur. Acad. Dermatol. Venereol. 2010, 24, 1–6.
- Correa, M.C.M.; Nebus, J. Management of Patients with Atopic Dermatitis: The Role of Emollient Therapy. Dermatol. Res. Pract. 2012, 2012, 836931.
- Duncan, C.N.; Riley, T.V.; Carson, K.C.; Budgeon, C.A.; Siffleet, J. The effect of an acidic cleanser versus soap on the skin pH and micro-flora of adult patients: A non-randomised two group crossover study in an intensive care unit. Intensiv. Crit. Care Nurs. 2013, 29, 291–296.
- Friedman, M. Chemistry, Formulation, and Performance of Syndet and Combo Bars. In Soap Manufacturing Technology, 2nd ed.; Spitz, L., Ed.; Elsevier: Cambridge, MA, USA; AOCS Press: Urbana, IL, USA, 2016; pp. 73–106. Available online: https://www.sciencedirect.com/science/article/pii/B9781630670658500049 (accessed on 11 January 2022).
- Draelos, Z.D. The science behind skin care: Cleansers. J. Cosmet. Dermatol. 2018, 17, 8–14.
- Kogawa, A.C.; Cernic, B.G.; Couto, L.G.D.D.; Salgado, H.R.N. Synthetic detergents: 100 years of history. Saudi Pharm. J. 2017, 25, 934–938.
- Cornwell, P.A. A review of shampoo surfactant technology: Consumer benefits, raw materials and recent developments. Int. J. Cosmet. Sci. 2018, 40, 16–30.
- Falk, N.A. Surfactants as Antimicrobials: A Brief Overview of Microbial Interfacial Chemistry and Surfactant Antimicrobial Activity. J. Surfactants Deterg. 2019, 22, 1119–1127.
- Coiffard, L.; Couteau, C. Soap and syndets: Differences and analogies, sources of great confusion. Eur Rev. Med. Pharm. Sci 2020, 24, 11432–11439.
- Chirani, M.R.; Kowsari, E.; Teymourian, T.; Ramakrishna, S. Environmental impact of increased soap consumption during COVID-19 pandemic: Biodegradable soap production and sustainable packaging. Sci. Total Environ. 2021, 796, 149013.
- Oyekunle, J.A.; Ore, O.T.; Ogunjumelo, O.H.; Akanni, M.S. Comparative chemical analysis of Indigenous Nigerian soaps with conventional ones. Heliyon 2021, 7, e06689.
- Belhaj, A.F.; Elraies, K.A.; Mahmood, S.M.; Zulkifli, N.N.; Akbari, S.; Hussien, O.S. The effect of surfactant concentration, salinity, temperature, and pH on surfactant adsorption for chemical enhanced oil recovery: A review. J. Pet. Explor. Prod. Technol. 2019, 10, 125–137.
- Nazdrajic, S.; Bratovcic, A. The role of surfactants in liquid soaps and its antimicrobial properties. Int. J. Adv. Res. 2019, 7, 501–507.
- Tripathy, D.B.; Mishra, A.; Clark, J.; Farmer, T. Synthesis, chemistry, physicochemical properties and industrial applications of amino acid surfactants: A review. Comptes Rendus. Chim. 2018, 21, 112–130.
- Bjerk, T.R.; Severino, P.; Jain, S.; Marques, C.; Silva, A.M.; Pashirova, T.; Souto, E.B. Biosurfactants: Properties and Applications in Drug Delivery, Biotechnology and Ecotoxicology. Bioeng. 2021, 8, 115.
- Farias, C.B.B.; Almeida, F.C.; Silva, I.A.; Souza, T.C.; Meira, H.M.; Silva, R.D.C.F.S.D.; Luna, J.M.; Santos, V.A.; Converti, A.; Banat, I.M.; et al. Production of green surfactants: Market prospects. Electron. J. Biotechnol. 2021, 51, 28–39.
- Lambers, H.; Piessens, S.; Bloem, A.; Pronk, H.; Finkel, P. Natural skin surface pH is on average below 5, which is beneficial for its resident flora. Int. J. Cosmet. Sci. 2006, 28, 359–370.
- Stamatas, G.N.; Walters, R.M.; Martin, K.M. Formulating for unique needs of baby skin. Personal Care 2011, 31–36.
- Hugill, K. Neonatal skin cleansing revisited: Whether or not to use skin cleansing products. Br. J. Midwifery 2014, 22, 694–698.
- Farage, M.A.; Miller, K.W.; Elsner, P.; Maibach, H.I. Structural Characteristics of the Aging Skin: A Review. Cutan. Ocul. Toxicol. 2007, 26, 343–357.
- Solodkin, G.; Chaudhar, U.; Subramanyan, K.; Johnson, A.W.; Yan, X.; Gottlieb, A. Benefits of mild cleansing: Synthetic sur-factant based (syndet) bars for patients with atopic dermatitis. Cutis 2006, 77, 317–324.
- Duarte, I.; Silveira, J.E.P.S.; Hafner, M.D.F.S.; Toyota, R.; Pedroso, D.M.M. Sensitive skin: Review of an ascending concept. An. Bras. Dermatol. 2017, 92, 521–525.
- Surber, C.; Dragicevic, N.; Kottner, J. Skin Care Products for Healthy and Diseased Skin. Metab. Disord. Nutr. Correl. Ski. 2018, 54, 183–200.
More
Information
Subjects:
Dermatology
Contributors
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
7.0K
Revisions:
2 times
(View History)
Update Date:
21 Apr 2022
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





