
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Yohei Tomita | + 622 word(s) | 622 | 2021-10-20 03:59:24 | | | |
| 2 | Deokho Lee | + 58 word(s) | 680 | 2021-10-26 16:41:15 | | | | |
| 3 | Catherine Yang | -84 word(s) | 596 | 2021-10-27 03:34:50 | | | | |
| 4 | Toshihide Kurihara | + 1 word(s) | 597 | 2021-10-27 04:40:16 | | | | |
| 5 | Catherine Yang | -59 word(s) | 538 | 2021-11-01 04:38:02 | | |
Video Upload Options
Diabetic retinopathy (DR) is one of the leading matters of vision-loss globally. Even though there have been extensive efforts to reduce vision loss, the prevalence of DR is still uprising. There are several pharmacological and surgical therapies currently used in clinics, but none of them has not been used as effective therapies at the early stage of DR.
1. Introduction
Diabetic retinopathy (DR) is a severe complication of diabetes mellitus (DM) and the main cause of vision loss [1]. A dramatic socioeconomic cost is needed for DR treatment. Its prevalence has continuously increased globally [2]. The public burden of DR let medical scientists search for better therapeutic approaches, as well as the update of current standards of DR treatment, including laser, anti-vascular endothelial growth factor (VEGF) therapy, steroid, and vitrectomy [3]. Despite the fact that surgical or pharmacological strategy in DR has been advanced, the pathological mechanisms of DR even have yet to be clearly unraveled.
2. Pathophysiology of DR
There have been various insights into the pathophysiology of DR (Figure 1). At first, DR is a microvascular disease, and hyperglycemia is the leading cause of retinal microvascular damage [4]. In this point of view, pathological metabolic pathways such as accumulation of AGEs and induction of PKC, the polyol, and the hexosamine pathways have been suggested in retinal microvascular injury [3].
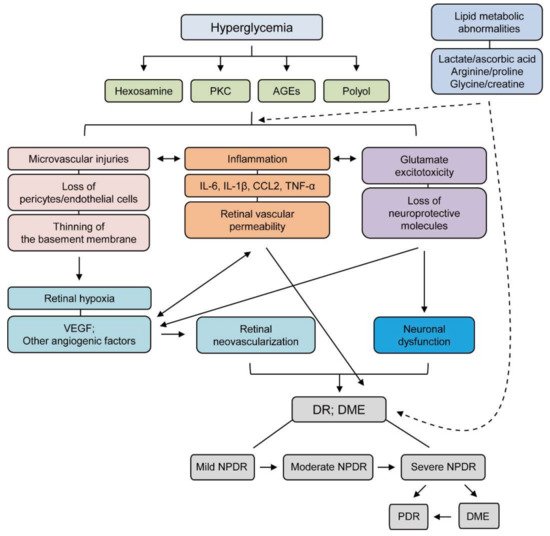
In the early stage of DR, pericyte loss leads to microvasculature destruction [5]. It causes capillary occlusion, finally leading to retinal ischemia. Retinal ischemia induces retinal inflammation as well as retinal degeneration from the early stage to the chronic stage in DR. Retinal inflammation under diabetic conditions is involved in a variety of inflammatory cytokines and chemokines such as (MCP-1/CCL2, TNF-α, IL-1β, IL-6). For retinal degeneration, various pro-apoptotic proteins such as Bax, caspase-3 have been nominated to induce retinal neuronal cell death in DR [6][7]. Taken together, various negative outcomes from microvascular abnormality to retinal cell death, are intermingled to the development and progression of DR. Recently, lipid metabolic dysregulation has been suggested for the development and progression of DR [8][9][10]. Strong correlation of changes in plasma levels of HDL and LDL with the development of severities of DR as well as diabetes has been demonstrated. Dyslipidemia could be promoted under insulin-resistant conditions, which is important for the maintenance of glucose metabolism. Furthermore, increasing evidence showed that lipid-modifying drugs (fenofibrate and/or pemafibrate) could have possible therapeutic effects against DR conditions [3].
3. Current/Future Therapy in DR
At present, the most effective treatment for DR is blood glucose level control. More advanced conditions need laser, anti-VEGF therapy, steroid, and vitrectomy [3]. However, lots of DR patients are still suffering from side effects of those treatments. In this regard, alternative promising treatments are needed in this current situation for DR treatment. As described in Figure 1, lipid and glucose dysregulations as well as retinal cell death, inflammation, and microvascular injury together affect the development and progression of DR. Furthermore, research outcomes from diabetic experimental models showed that peroxisome proliferator-activated receptor alpha (PPARα) activation showed promising therapeutic effects in cellular metabolism and inflammation, which can be used as a future promising treatment for DR.
References
- Bourne, R.R.A.; Flaxman, S.R.; Braithwaite, T.; Cicinelli, M.V.; Das, A.; Jonas, J.B.; Keeffe, J.; Kempen, J.H.; Leasher, J.; Limburg, H.; et al. Magnitude, temporal trends, and projections of the global prevalence of blindness and distance and near vision impairment: A systematic review and meta-analysis. Lancet Glob. Health 2017, 5, e888–e897.
- Leasher, J.L.; Bourne, R.R.; Flaxman, S.R.; Jonas, J.B.; Keeffe, J.; Naidoo, K.; Pesudovs, K.; Price, H.; White, R.A.; Wong, T.Y.; et al. Global Estimates on the Number of People Blind or Visually Impaired by Diabetic Retinopathy: A Meta-analysis from 1990 to 2010. Diabetes Care 2016, 39, 1643–1649.
- Simó, R.; Hernández, C. Neurodegeneration in the diabetic eye: New insights and therapeutic perspectives. Trends Endocrinol. Metab. Tem. 2014, 25, 23–33.
- Lutty, G.A. Effects of diabetes on the eye. Investig. Ophthalmol. Vis. Sci. 2013, 54, ORSF81.
- Bergers, G.; Song, S. The role of pericytes in blood-vessel formation and maintenance. Neuro-Oncology 2005, 7, 452–464.
- Podestà, F.; Romeo, G.; Liu, W.-H.; Krajewski, S.; Reed, J.C.; Gerhardinger, C.; Lorenzi, M. Bax Is Increased in the Retina of Diabetic Subjects and Is Associated with Pericyte Apoptosis in Vivo and in Vitro. Am. J. Pathol. 2000, 156, 1025–1032.
- Kowluru, R.A.; Koppolu, P. Diabetes-induced Activation of Caspase-3 in Retina: Effect of Antioxidant Therapy. Free Radic. Res. 2002, 36, 993–999.
- Barba, I.; Garcia-Ramirez, M.; Hernandez, C.; Alonso, M.A.; Masmiquel, L.; Garcia-Dorado, D.; Simo, R. Metabolic fingerprints of proliferative diabetic retinopathy: An 1H-NMR-based metabonomic approach using vitreous humor. Investig. Ophthalmol. Vis. Sci. 2010, 51, 4416–4421.
- Tomita, Y.; Cagnone, G.; Fu, Z.; Cakir, B.; Kotoda, Y.; Asakage, M.; Wakabayashi, Y.; Hellstrom, A.; Joyal, J.S.; Talukdar, S.; et al. Vitreous metabolomics profiling of proliferative diabetic retinopathy. Diabetologia 2021, 64, 70–82.
- Haines, N.R.; Manoharan, N.; Olson, J.L.; D’Alessandro, A.; Reisz, J.A. Metabolomics Analysis of Human Vitreous in Diabetic Retinopathy and Rhegmatogenous Retinal Detachment. J. Proteome Res. 2018, 17, 2421–2427.





