
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Martyna Krzykawska-Serda | + 6857 word(s) | 6857 | 2021-08-03 05:25:41 | | | |
| 2 | Vivi Li | Meta information modification | 6857 | 2021-10-08 05:42:52 | | |
Video Upload Options
Cancer is one of the leading causes of death in humans. Despite the progress in cancer treatment, and an increase in the effectiveness of diagnostic methods, cancer is still highly lethal and very difficult to treat in many cases. Combination therapy, in the context of cancer treatment, seems to be a promising option that may allow minimizing treatment side effects and may have a significant impact on the cure. It may also increase the effectiveness of anti-cancer therapies. Moreover, combination treatment can significantly increase delivery of drugs to cancerous tissues. Photodynamic therapy and hyperthermia seem to be ideal examples that prove the effectiveness of combination therapy. These two kinds of therapy can kill cancer cells through different mechanisms and activate various signaling pathways. Both PDT and hyperthermia play significant roles in the perfusion of a tumor and the network of blood vessels wrapped around it.
1. Introduction: Aims of Anti-Cancer Combination Therapy
1.1. Combination Treatment–Definition, Pros, and Cons
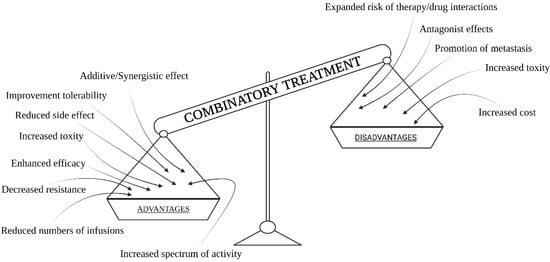
1.2. Action Strategies and the Greatest Successes in the Fight against Cancer
2. General Information about Photodynamic Therapy and Hyperthermia
2.1. PDT
2.2. Hyperthermia
| Temperature Range (°C) | Selected Area in the Human Body |
|---|---|
| 36.32–37.76 | rectal |
| 35.76–37.52 | tympanic |
| 35.61–37.61 | urine |
| 35.73–37.41 | oral |
| 35.01–36.93 | axillary |
3. Proposed Combinations That Are Currently Used in Multimodal Cancer Treatment
3.1. Radiotherapy
3.2. Chemotherapy
3.3. Surgical Intervention
References
- Bray, F.; Me, J.F.; Soerjomataram, I.; Siegel, R.L.; Torre, L.A.; Jemal, A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA A Cancer J. Clin. 2018, 68, 394–424.
- Siegel, R.L.; Miller, K.D.; Jemal, A. Cancer statistics, 2020. CA Cancer J. Clin. 2020, 70, 7–30.
- Nicholas, C.; Lesinski, G.B. Immunomodulatory cytokines as therapeutic agents for melanoma. Immunomodulatory 2013, 3, 673–690.
- Mokhtari, R.B.; Homayouni, T.S.; Baluch, N.; Morgatskaya, E.; Kumar, S.; Das, B.; Yeger, H. Combination therapy in combating cancer. Oncotarget 2017, 8, 38022–38043.
- Wang, T.; Narayanaswamy, R.; Ren, H.; Torchilin, V.P. Combination therapy targeting both cancer stem-like cells and bulk tumor cells for improved efficacy of breast cancer treatment. Cancer Biol. Ther. 2016, 17, 698–707.
- Yuan, S.; Wang, F.; Chen, G.; Zhang, H.; Feng, L.; Wang, L.; Colman, H.; Keating, M.J.; Li, X.; Xu, R.-H.; et al. Effective Elimination of Cancer Stem Cells By a Novel Drug Combination Strategy. STEM CELLS 2012, 31, 23–34.
- Delbaldo, C.; Michiels, S.; Syz, N.; Soria, J.-C.; Le Chevalier, T.; Pignon, J.-P. Benefits of Adding a Drug to a Single-Agent or a 2-Agent Chemotherapy Regimen in Advanced Non–Small-Cell Lung Cancer. JAMA 2004, 292, 470–484.
- García-Román, J.; Zentella-Dehesa, A. Vascular permeability changes involved in tumor metastasis. Cancer Lett. 2013, 335, 259–269.
- Chen, J.; Weihs, D.; Vermolen, F.J. Computational modeling of therapy on pancreatic cancer in its early stages. Biomech. Model. Mechanobiol. 2019, 19, 427–444.
- Srivani, G.; Behera, S.K.; Dariya, B.; Chalikonda, G.; Alam, A.; Nagaraju, G.P. HIF-1α and RKIP: A computational approach for pancreatic cancer therapy. Mol. Cell. Biochem. 2020, 472, 95–103.
- Lala, M.; Li, T.R.; de Alwis, D.P.; Sinha, V.; Mayawala, K.; Yamamoto, N.; Siu, L.L.; Chartash, E.; Aboshady, H.; Jain, L. A six-weekly dosing schedule for pembrolizumab in patients with cancer based on evaluation using modelling and simulation. Eur. J. Cancer 2020, 131, 68–75.
- Yang, Y.-C.; Chiang, C.-S. Challenges of Using High-Dose Fractionation Radiotherapy in Combination Therapy. Front. Oncol. 2016, 6, 165.
- Zheng, X.; Chen, Y.; Zheng, D.; Xiao, Y.; Chen, J.; Pan, J.; Chen, W. Diffusion kurtosis imaging and tumour microstructure for monitoring response to radiotherapy in human nasopharyngeal carcinoma xenografts. Jpn. J. Clin. Oncol. 2020, 50, 548–555.
- Bhuyan, B.K. Kineticsof Cell Kill by Hyperthermia. Cancer Res. 1979, 39, 2277–2284.
- Overgaard, J.; Overgaard, J. The current and potential role of hyperthermia in radiotherapy. Int. J. Radiat. Oncol. 1989, 16, 535–549.
- Cheng, Y.; Weng, S.; Yu, L.; Zhu, N.; Yang, M.; Yuan, Y. The Role of Hyperthermia in the Multidisciplinary Treatment of Malignant Tumors. Integr. Cancer Ther. 2019, 18.
- Pritchard, J.R.; Lauffenburger, D.A.; Hemann, M.T. Understanding resistance to combination chemotherapy. Drug Resist. Updat. 2012, 15, 249–257.
- Jones, E.L.; Prosnitz, L.R.; Dewhirst, M.W.; Marcom, P.K.; Hardenbergh, P.H.; Marks, L.B.; Brizel, D.; Vujaskovic, Z. Thermochemoradiotherapy Improves Oxygenation in Locally Advanced Breast Cancer. Clin. Cancer Res. 2004, 10, 4287–4293.
- Behrouzkia, Z.; Joveini, Z.; Keshavarzi, B.; Eyvazzadeh, N.; Aghdam, R.Z. Hyperthermia: How Can It Be Used? Oman Med. J. 2016, 31, 89–97.
- Dasari, S.; Tchounwou, P.B. Cisplatin in cancer therapy: Molecular mechanisms of action. Eur. J. Pharmacol. 2014, 740, 364–378.
- Krzykawska-Serda, M.; Dąbrowski, J.M.; Arnaut, L.G.; Szczygieł, M.; Urbanska, K.; Stochel, G.; Elas, M. The role of strong hypoxia in tumors after treatment in the outcome of bacteriochlorin-based photodynamic therapy. Free. Radic. Biol. Med. 2014, 73, 239–251.
- Arnaut, L.G.; Pereira, M.M.; Dabrowski, J.; Silva, E.F.F.; Schaberle, F.; Abreu, A.R.; Rocha, L.B.; Barsan, M.M.; Urbanska, K.; Stochel, G.; et al. Photodynamic Therapy Efficacy Enhanced by Dynamics: The Role of Charge Transfer and Photostability in the Selection of Photosensitizers. Chem. A Eur. J. 2014, 20, 5346–5357.
- Dave, D.; Desai, U.; Despande, N. Photodynamic Therapy: A View through Light. J. Orofac. Res. 2012, 2, 82–86.
- Oniszczuk, A.; Wojtunik-Kulesza, K.A.; Oniszczuk, T.; Kasprzak, K. The potential of photodynamic therapy (PDT)—Experimental investigations and clinical use. Biomed. Pharmacother. 2016, 83, 912–929.
- Allison, R.R.; Downie, G.H.; Cuenca, R.; Hu, X.; Childs, C.J.; Sibata, C.H.; Allison, R.R.; Downie, G.H.; Cuenca, R.; Hu, X.; et al. Photosensitizers in clinical PDT. Photodiagnosis Photodyn. Ther. 2004, 1, 27–42.
- Kataoka, H.; Nishie, H.; Hayashi, N.; Tanaka, M.; Nomoto, A.; Yano, S.; Joh, T. New photodynamic therapy with next-generation photosensitizers. Ann. Transl. Med. 2017, 5, 183.
- Abrahamse, H.; Hamblin, M.R. New photossensitizersfot photodynamic therapy. Biochem. J. 2017, 473, 347–364.
- Rivera, J.A.R.; Medina, M.L.V.M.; Zegarra, M.L.; Rodriguez, R. Efficacy, Safety and Quality of Life After TOOKAD® Soluble VTP for Localized Prostate Cancer (PCM304). Steba Biotech S.A.; 2013. Available online: https://clinicaltrials.gov/ct2/show/NCT01875393 (accessed on 26 April 2021).
- Emberton, M. Efficacy and Safety Study of TOOKAD® Soluble for Localised Prostate Cancer Compared to Active Surveillance. (PCM301). Steba Biotech S.A.; 2019. Available online: https://clinicaltrials.gov/ct2/show/NCT01310894 (accessed on 26 April 2021).
- Trachtenberg, J. Study of WST09 in Prostate Cancer after Radiation: Repeat Procedure. STEBA France; 2010. Available online: https://clinicaltrials.gov/ct2/show/NCT00305929 (accessed on 26 April 2021).
- Trachtenberg, J. Phase II/III Study of WST09 in Prostate Cancer after Radiation Therapy. STEBA France; 2010. Available online: https://clinicaltrials.gov/ct2/show/NCT00312442 (accessed on 26 April 2021).
- Almeida, L. Photodynamic Therapy with LUZ11 in Advanced Head and Neck Cancer. Luzitin SA; 2016. Available online: https://clinicaltrials.gov/ct2/show/NCT02070432 (accessed on 26 April 2021).
- Daniell, M.D.; Hill, J.S. A History of Photodynamic Therapy. ANZ J. Surg. 1991, 61, 340–348.
- Ackroyd, R.; Kelty, C.; Brown, N.; Reed, M. The History of Photodetection and Photodynamic Therapy. Photochemistry Photobiol. 2001, 74, 656–669.
- Brancaleon, L.; Moseley, H.; Brancaleon, L.; Moseley, H. Laser and Non-laser Light Sources for Photodynamic Therapy. Lasers Med. Sci. 2002, 17, 173–186.
- Zhang, C.; Chen, W.; Zhang, T.; Jiang, X.; Hu, Y. Hybrid nanoparticle composites applied to photodynamic therapy: Strategies and applications. J. Mater. Chem. B 2020, 8, 4726–4737.
- Fukumura, D.; Jain, R.K. Tumor microenvironment abnormalities: Causes, consequences, and strategies to normalize. J. Cell. Biochem. 2006, 101, 937–949.
- Joyce, J.A. Therapeutic targeting of the tumor microenvironment. Cancer Cell 2005, 7, 513–520.
- Bristow, R.G.; Hill, R.P.; Bristow, R.G.; Hill, R.P. Hypoxia, DNA repair and genetic instability. Nat. Rev. Cancer 2008, 8, 180–192.
- Semenza, G.L. The hypoxic tumor microenvironment: A driving force for breast cancer progression. Biochim. et Biophys. Acta (BBA) Bioenerg. 2016, 1863, 382–391.
- Vaupel, P.; Mayer, A. Hypoxia in cancer: Significance and impact on clinical outcome. Cancer Metastasis Rev. 2007, 26, 225–239.
- Protsiv, M.; Ley, C.; Lankester, J.; Hastie, T.; Parsonnet, J. Decreasing human body temperature in the United States since the Industrial Revolution. eLife 2020, 9.
- Geneva, I.; Cuzzo, B.; Fazili, T.; Javaid, W. Normal Body Temperature: A Systematic Review. Open Forum Infect. Dis. 2019, 6, ofz032.
- Liu, Z. Clinical effects of high frequency hyperthermia-assisted irinotecan chemotherapy on patients with middle and advanced colorectal cancer and its safety assessment. Oncol. Lett. 2018, 17, 215–220.
- Tempel, N.V.D.; Horsman, M.; Kanaar, R. Improving efficacy of hyperthermia in oncology by exploiting biological mechanisms. Int. J. Hyperth. 2016, 32, 446–454.
- Hildebrandt, B.; Wust, P.; Ahlers, O.; Dieing, A.; Sreenivasa, G.; Kerner, T.; Felix, R.; Riess, H. The cellular and molecular basis of hyperthermia. Crit Rev. Oncol Hematol. 2002, 116, 69–75.
- Guillemin, P.; Gui, L.; Lorton, O.; Zilli, T.; Crowe, L.A.; Desgranges, S.; Montet, X.; Terraz, S.; Miralbell, R.; Salomir, R.; et al. Mild hyperthermia by MR-guided focused ultrasound in an ex vivo model of osteolytic bone tumour: Optimization of the spatio-temporal control of the delivered temperature. J. Transl. Med. 2019, 17, 1–19.
- Piotr, G.A.S. Essential Facts on the History of Hyperthermia and their Connections with Electromedicine. arXiv 2017, 12, 37–40.
- Szasz, A.; Iluri, N.; Szasz, O. Local Hyperthermia in Oncology—To Choose or not to Choose? In Hyperthermia; IntechOpen: London, UK, 2013.
- Seynhaeve, A.; Amin, M.; Haemmerich, D.; van Rhoon, G.; Hagen, T.T. Hyperthermia and smart drug delivery systems for solid tumor therapy. Adv. Drug Deliv. Rev. 2020, 163–164, 125–144.
- MacEwan, S.R.; Callahan, D.J.; Chilkoti, A. Stimulus-responsive macromolecules and nanoparticles for cancer drug delivery. Nanomedicine 2010, 5, 793–806.
- Matteucci, M.L.; Anyarambhatla, G.; Rosner, G.; Azuma, C.; Fisher, P.E.; Dewhirst, M.W.; Needham, D.; Thrall, D.E. Hyperthermia increases accumulation of technetium-99m-labeled liposomes in feline sarcomas. Clin. Cancer Res. 2000, 6, 3748–3755.
- Rao, W.; Deng, Z.-S.; Liu, J. A Review of Hyperthermia Combined with Radiotherapy/Chemotherapy on Malignant Tumors. Crit. Rev. Biomed. Eng. 2010, 38, 101–116.
- Oei, A.L.; Vriend, L.E.M.; Crezee, J.; Franken, N.A.P.; Krawczyk, P.M. Effects of hyperthermia on DNA repair pathways: One treatment to inhibit them all. Radiat. Oncol. 2015, 10, 1–13.
- Ahmed, K.; Zaidi, S.F. Treating cancer with heat: Hyperthermia as promising strategy to enhance apoptosis. J. Pak. Med. Assoc. 2013, 63, 504–508.
- Lapin, N.A.; Krzykawska-Serda, M.; Dilliard, S.; Mackeyev, Y.; Serda, M.; Wilson, L.J.; Curley, S.A.; Corr, S.J. The effects of non-invasive radiofrequency electric field hyperthermia on biotransport and biodistribution of fluorescent fullerene derivative in a murine orthotopic model of breast adenocarcinoma. J. Control. Release 2017, 260, 92–99.
- Huang, S.H.; Yang, K.J.; Wu, J.C.; Chang, K.J.; Wang, S.M. Effects of hyperthermia on the cytoskeleton and focal adhesion proteins in a human thyroid carcinoma cell line. J. Cell. Biochem. 1999, 75, 327–337.
- Eppink, B.; Krawczyk, P.M.; Stap, J.; Kanaar, R. Hyperthermia-induced DNA repair deficiency suggests novel therapeutic anti-cancer strategies. Int. J. Hyperth. 2012, 28, 509–517.
- Bouwman, P.; Jonkers, J. The effects of deregulated DNA damage signalling on cancer chemotherapy response and resistance. Nat. Rev. Cancer 2012, 12, 587–598.
- Frey, B.; Weiss, E.-M.; Rubner, Y.; Wunderlich, R.; Ott, O.J.; Sauer, R.; Fietkau, R.; Gaipl, U.S. Old and new facts about hyperthermia-induced modulations of the immune system. Int. J. Hyperth. 2012, 28, 528–542.
- Alanazi, F.K.; Radwan, A.A.; Alsarra, I. Biopharmaceutical applications of nanogold. Saudi Pharm. J. 2010, 18, 179–193.
- Hu, Q.; Sun, W.; Wang, C.; Gu, Z. Recent advances of cocktail chemotherapy by combination drug delivery systems. Adv. Drug Deliv. Rev. 2016, 98, 19–34.
- Baskar, R.; Lee, K.A.; Yeo, R.; Yeoh, K.-W. Cancer and Radiation Therapy: Current Advances and Future Directions. Int. J. Med. Sci. 2012, 9, 193–199.
- Jackson, S.P.; Bartek, J. The DNA-damage response in human biology and disease. Nat. Cell Biol. 2009, 461, 1071–1078.
- Herskind, C.; Ma, L.; Liu, Q.; Zhang, B.; Schneider, F.; Veldwijk, M.R.; Wenz, F. Biology of high single doses of IORT: RBE, 5 R’s, and other biological aspects. Radiat. Oncol. 2017, 12, 24.
- Hall, N.; Rouge, B. The physics of proton therapy. Phys. Med. Biol. 2015, 60.
- Strojan, P. Role of radiotherapy in melanoma management. Radiol. Oncol. 2010, 44, 1–12.
- Dewey, W.C. Arrhenius relationships from the molecule and cell to the clinic. Int. J. Hyperth. 2009, 25, 3–20.
- Arruebo, M.; Vilaboa, N.; Sáez-Gutierrez, B.; Lambea, J.; Tres, A.; Valladares, M.; González-Fernández, A. Assessment of the Evolution of Cancer Treatment Therapies. Cancers 2011, 3, 3279–3330.
- Morgan, N.Y.; Kramer-Marek, G.; Smith, P.D.; Camphausen, K.; Capala, J. Nanoscintillator Conjugates as Photodynamic Therapy-Based Radiosensitizers: Calculation of Required Physical Parameters. Radiat. Res. 2009, 171, 236–244.
- Schaffer, M.; Ertl-Wagner, B.; Kulka, U.; Jori, G.; Duhmke, E.; Hofstetter, A.; Schaffer, P.M. The Application of Photofrin II® as a Sensitizing Agent for Ionizing Radiation-A New Approach in Tumor Therapy? Curr. Med. Chem. 2005, 12, 1209–1215.
- Luksiene, Z.; Kalvelyte, A.; Supino, R. On the combination of photodynamic therapy with ionizing radiation. J. Photochem. Photobiol. B Biol. 1999, 52, 35–42.
- De Almeida, D.R.Q.; Terra, L.F.; Labriola, L. Photodynamic therapy in cancer treatment—An update review. J. Cancer Metastasis Treat. 2019, 2019.
- Schirrmacher, V. From chemotherapy to biological therapy: A review of novel concepts to reduce the side effects of systemic cancer treatment (Review). Int. J. Oncol. 2018, 54, 407–419.
- Phung, D.C.; Nguyen, H.T.; Tran, T.T.P.; Jin, S.G.; Yong, C.S.; Truong, D.H.; Tran, T.H.; Kim, J.O. Combined hyperthermia and chemotherapy as a synergistic anticancer treatment. J. Pharm. Investig. 2019, 49, 519–526.
- Cheng, L.; Wang, C.; Feng, L.; Yang, K.; Liu, Z. Functional Nanomaterials for Phototherapies of Cancer. Chem. Rev. 2014, 114, 10869–10939.
- Song, C.W. Effect of local hyperthermia on blood flow and microenvironment: A review. Cancer Res. 1984, 44, 4721s–4730s.
- Issels, R.D. Hyperthermia adds to chemotherapy. Eur. J. Cancer 2008, 44, 2546–2554.
- Bettaieb, A.; Averill-Bates, D.A. Thermotolerance induced at a fever temperature of 40 °C protects cells against hyperthermia-induced apoptosis mediated by death receptor signalling. Biochem. Cell Biol. 2008, 86, 521–538.
- Pawlik, T.M.; Scoggins, C.R.; Zorzi, D.; Abdalla, E.K.; Andres, A.; Eng, C.; Curley, S.A.; Loyer, E.M.; Muratore, A.; Mentha, G.; et al. Effect of Surgical Margin Status on Survival and Site of Recurrence After Hepatic Resection for Colorectal Metastases. Ann. Surg. 2005, 241, 715–724.
- Hemming, A.W.; Reed, A.; Langham, M.; Fujita, S.; Howard, R.J. Combined Resection of the Liver and Inferior Vena Cava for Hepatic Malignancy. Ann. Surg. 2004, 239, 712–721.
- Ware, M.; Nguyen, L.P.; Law, J.J.; Krzykawska-Serda, M.; Taylor, K.M.; Cao, H.S.T.; Anderson, A.O.; Pulikkathara, M.; Newton, J.M.; Ho, J.C.; et al. A new mild hyperthermia device to treat vascular involvement in cancer surgery. Sci. Rep. 2017, 7, 1–14.
- Dixon, K.; Gibbins, S.; Moghissi, K. A Surgical View of Photodynamic Therapy in Oncology: A Review. Surg. J. 2015, 1, e1–e15.
- Moghissi, K.; Stringer, M.; Dixon, K. Fluorescence photodiagnosis in clinical practice. Photodiagnosis Photodyn. Ther. 2008, 5, 235–237.
- Eljamel, M.S. Fluorescence image-guided surgery of brain tumors: Explained step-by-step. Photodiagnosis Photodyn. Ther. 2008, 5, 260–263.





