The human brain is the most complex organ, controlling all the amazing things we do by regulating several molecular pathways. It comprises billions of cells, called neurons, which control the proper functioning of our body. Neurons stimulate and transmit signals that enable us to talk, move, think, and accomplish everything we do. The brain cells are closely interconnected with each other. Therefore, the slightest miscommunications within cells in a particular area can lead to a disruption in other activities controlled by brain, causing major brain disorders. Neurodegenerative diseases can also be characterized by progressive loss in the functioning of the brain due to an accumulation of toxic proteins that exhibit clinical syndromes
[1][2]. Therefore, brain disorders should not be taken lightly, as they can result in widespread problems
[3], ultimately leading to neuronal death and shrinkage. The word “neurodegenerative” is formed of two parts—“neuro,” which means brain, and “degenerative,” which means dying or breaking down. Inadequate communication among brain cells lead to devastating effects, influencing several activities of an individual such as movement, memory, speech intelligence, and many more
[4][5]. Neurodegenerative diseases are highly complex, and their etiology is sometimes very hard to predict.
Different areas of the brain encounter different types of neurodegenerative diseases, and they are described in Table 1. Examples of neurodegenerative diseases include Parkinson’s disease, Huntington disease, Alzheimer’s disease, amyotrophic lateral sclerosis, and many more.
The symptoms of neurodegenerative diseases are mainly encountered in older groups of people
[6]. This group of people is highly vulnerable to memory loss, which results in a poor quality of life and loss of personality
[7][8][9]. With the increasing population worldwide, the incidence of neurological diseases is also increasing. According to published data, it has been determined that new cases of Parkinson’s disease and Alzheimer’s disease have increased abruptly over the span of the last 30 years. Around the globe, more than 10 million people are suffering from Parkinson’s disease and more than 5.4 million people are living with Alzheimer’s disease, indicating that neurodegenerative diseases are the leading cause of death worldwide and are highly prevalent in populations of people 60 years of age
[10]. The massive increase in neurodegenerative diseases can be contributing to an increase in the prevalence of amyotrophic lateral sclerosis (ALS) disease. In addition, it has been determined that a large population of the elderly age group is estimated to be suffering from Huntington disease.
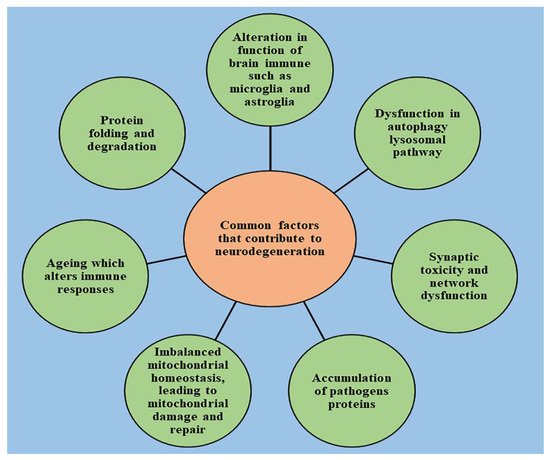
The current review explains the most common pathways that are responsible for the initiation and progression of commonly occurring neurodegenerative disorders.
2. Role of Cell Death in the Onset of Neurodegeneration
Neurological disorders are mainly characterized by increased degradation in the functioning of neurons due to the destruction of synapses and axons, eventually leading to nerve cell death. An understanding of the mechanism that leads to the homeostasis of cellular elements and neurodegradation is highly important for developing novel therapeutic treatments for the diseases
[15][16][17][18][19]. The healthy cells in the human body transform to preserve the normal homeostasis of tissues; however, post-mitotic neurons harbor very little capacity to regenerate and their survival is essential to ensure the proper functioning of the nervous system
[20]. The death of neurons promotes the development of nervous system; however, if occurring in excess, it leads to declined functioning of nervous system and causes the progression of neurodegenerative diseases, which can be indicated by a range of acute insults, from stroke and traumatic brain injury (TBI) to enduring critical conditions such as Parkinson’s disease
[21], Alzheimer’s disease
[22], and amyotrophic lateral sclerosis
[23].
Several studies have been conducted to understand the neuropathology behind the chronic conditions of these diseases, and stereotypical patterns of neurodegeneration have been identified in different regions of the central nervous system, which correspond to the disease severity clinically
[24]. Several other pathological pathways, such as impairment in axonal transport and synaptic function, oxidative stress, dysfunction of lysosomes and mitochondria
[25][26], activation of microglial cells and protein aggregation, also contribute to neuronal damage
[27]. Other factors such as genetics, age, and environmental factors influence the disruption of neuronal homeostasis and aggravate the existing neurodegeneration by activating the signaling of different molecules, ultimately causing cell death and declined functioning of the nervous system
[28].
With the advancement of technology in recent years, the understanding of pathology and genetic changes invoked in neurodegenerative diseases has significantly improved but is still unsatisfying. Due to complex biology, the connection between the origin and execution of the death of neurons is still lucid
[2]. The pathway involved in cell death and the mechanism responsible for its activation is still under question, and unraveling it is important to drive the development of new target-oriented therapeutic medications. There are several pathways that regulate the cell death of neurons, which are explained below.
3. Oxidative Stress and Its Role in Neurodegeneration
The most vital entity for all living organisms is oxygen. Oxygen plays an important role in the physiological functioning of the body, as it is involved in several processes, such as tissue formation, and is a basic element for the growth of every cell. It is highly crucial in inducing gene transcription and signal transduction
[29]. However, in excess it may produce detrimental outcomes. The conditions of stress occur mainly due to an imbalance between concentrations of reactive oxygen species (hydroxyl free radical, oxygen) and antioxidants
[30]. The imbalance arises mainly due to two factors, which include the excessive synthesis of reactive oxygen species or a disturbance in the antioxidant system of the body
[31]. Mitochondria supplies adenosine triphosphate (ATP) to the cells by breaking down glucose molecules, a process called oxidative phosphorylation, and by the synthesis of several other essential biological molecules. The proteins and enzymes required in oxidative phosphorylation are mainly programmed by the DNA of the mitochondria. Apart from the production of ATP via electron transport chain and oxidative phosphorylation, mitochondria are also involved in producing molecules that have a tendency to overcome oxidative stress via apoptotic mechanisms and other functions in cells
[32].
The enrichment of mitochondria with enzymes involved in redox reaction and dysfunction of mitochondria is the principal cause of oxidative stress and excessive production of reactive oxygen species in the cellular environment. A phospholipid called cardiolipin is found in the membrane of mitochondria and is specifically involved with proteins in the electron transport chain. Any abnormality in the oxidative phosphorylation process causes the dysfunction of mitochondria cells and the generation of reactive oxygen species (ROS) made up of univalent oxygen molecules. The most important molecule in reactive oxygen species is nitric oxide, which regulates the production and relaxation of the muscle cells of vasculature, leukocyte adhesion, platelet aggregation, angiogenesis, thrombosis, hemodynamics, vascular tone, and many more
[33].
The major sources of free radicals include redox metabolism in mitochondria, the metabolism of phospholipids, and several other proteolytic pathways. For normal physiological functioning of the body, the concentration of reactive oxygen species must be low. High concentrations and excessive exposure to ROS leads to the destruction of macromolecules such as DNA, proteins, and lipids, which ultimately cause necrosis and apoptotic cell death
[34].
Oxidative stress is also the key element that regulates aging and several other neurological conditions. The chemical integrity of the brain controls the higher functioning of the central nervous system. The human brain is most susceptible to oxidative stress, as it devours a huge proportion of oxygen and is highly rich in lipids
[35]. Higher oxygen consumption produces an abundant number of ROS. The membrane of the neurons is made up of polyunsaturated fatty acids, which are also prone to reactive oxygen species
[36].
Several neurodegenerative diseases such as Alzheimer’s disease, amyotrophic lateral sclerosis, Huntington disease, and Parkinson’s disease are a result of alterations in biochemical and biomolecular components mainly due to oxidative stress. Hydrogen peroxide, a highly reactive hydroxyl radical and super oxide anion, are some of the negative oxygen species that are involved in neurodegeneration. Therefore, a dire need arises to understand the principal role of oxidative stress in the etiology of neurodegeneration. Apart from reactive oxygen species, reactive nitrogen species such as nitric oxide also possesses destructive effects on neurons
[37]. It is important to understand the pathophysiology involved in cell death via ROS and initiate treatment by targeting the specific pathways involved to combat these diseases.
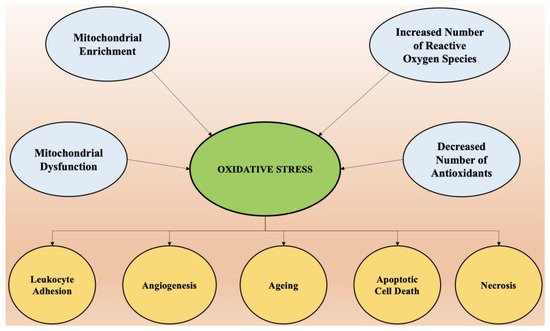
Oxidative stress is the predominant factor responsible for the pathogenesis of numerous chronic diseases such as diabetes, rheumatoid arthritis, obesity, etc., and almost all neurological disorders. Scavenging of free radicals by antioxidants can prevent aging and oxidative stress-mediated pathological conditions. The factors that cause oxidative stress and the physiological changes that come as a result of increased reactive oxygen species are presented in Figure 2.
Figure 2. The factors that cause oxidative stress and the physiological changes that come as a result of increased reactive oxygen species.
An insufficiency in the antioxidant-medicated defense system leads to increased concentrations of oxidative species, which is highly problematic, as neuron cells are made up of polyunsaturated lipids, which are extremely susceptible to oxidation and create deleterious effects on biomolecules
[38]. Changes in proteins, lipids, enzymes, DNA, ribonucleic acid (RNA), and other biomolecules under stress conditions can be used as biomarkers due to their highly sensitive nature and thus can be helpful in the determination of oxidative stress
[39]. Reactive oxygen species such as OH, ONOO, etc. can be generated by altering the functioning of proteins and lipids.
The heterocyclic bases of DNA and RNA, mainly guanine, is extremely prone to oxidative damage and can be attacked by reactive oxygen species, which leads to the formation of 8-hydroxy-2-deoxyguanosine and 8-hydroxyguanine. These modified bases, when increased to a certain extent in the brain, produce significant damage and are the principle cause of Parkinson’s disease
[40]. The carbonylation and nitration of proteins is also predominantly witnessed in brains of Alzheimer’s patients.
Lipids form the plasma membrane of the neuron cells and act as a barrier between extracellular and intracellular spaces, and hence play a major role in the functioning of neuron cells
[41]. However, these lipids are easily attacked by free radicals and go through lipid peroxidation, which decreases the fluidity of the membrane and causes leakage, which encourages the entry of substances that are usually not allowed to pass intracellularly but now cross these barriers through specific channels, thereby mutilating enzymes, membrane proteins, and receptors
[42].
A significant role of pro-oxidants in neurodegenerative disorders has also been established, apart from the endogenous and exogenous sources of oxidative stress. Rich sources of polyphenols such as vegetables and fruits play an important part in generating defense antioxidant mechanisms. Awareness to increase such ingredients in the diet on a routine basis can be highly beneficial. However, the occurrence of neurodegenerative diseases and other chronic health problems is not solely dependent upon antioxidants, and there may be several other factors that induce oxidative stress and have been identified as pro-oxidants
[43]. Pro-oxidants are any xenobiotic or endobiotic species that increases the production of reactive oxygen species or reactive nitrogen species by inhibiting the antioxidant system and triggering oxidative stress in tissues and cells. Exogeneous prooxidants include dietary supplements, pathogens, and toxicant drugs, whereas endogenous prooxidants include environmental pollution, metabolites of drugs, anxiety, climate change, and many more.
Heavy metals also play an important role in oxidative stress and have harmful effects on the reproductive system, respiratory system, central nervous system, cardiovascular system, and vital organs of the body
[44]. These metal ions accumulate in the environment of the human body and combine with other xenobiotics and exert deteriorating effects on the immune system and hematology. Exposure to heavy metal ions such as lead and mercury and a deficiency in necessary metal ions like zinc and selenium lead to an increase in oxidative stress and produce deleterious effects by generating abnormality in the redox functioning of the cell
[45].
The role of mercury in biological processes is minimal but its presence and accumulation in the body can produce harmful effects. Oxidative stress, which is mediated by the presence of mercury, can lead to the damage of biomolecular membranes, which further initiates the synthesis of hydrogen peroxide
[46]. The neurotoxic effects of mercury have been discovered, and it has been determined that excessive mercury causes tremors and memory issues in the brain, accompanied by altered hearing and vision. Another heavy metal, lead, is also toxic to humans because of its nature to induce oxidative stress
[47]. The damage produced by lead significantly depends upon the dose, route and duration of exposure, health status, and age of the individual. Lead has a high affinity for the -SH group, which is mainly present in amino acids and other metal cofactors that cause a significant reduction in the enzymes responsible for antioxidant activity, thereby elevating oxidative stress and causing failure of vital organs.
Another heavy metal, arsenic, is also prone to binding with the -SH group of glutathione, leading to the production of hydrogen peroxide. Arsenic is also responsible for the inhibition of glucose absorption in cells and the oxidation of fatty acids
[48].
Recently, the role of ferroptosis has also emerged as being involved in inducing oxidative stress, which causes neuron cell damage and cell apoptosis
[49][50]. The process of ferroptosis is mainly dependent upon the production of soluble and lipid reactive oxygen species by enzymatic reactions that mediate the transitioning of iron metal. Ferroptosis-mediated oxidative stress and mitochondrial dysfunction causes the death of neurons as well as cell apoptosis and targeting them can be an efficient strategy to prevent neurodegenerative diseases
[51].
4. Role of Neuroinflammation in the Onset of Neurodegeneration
Recent studies have demonstrated a bridge between chronic inflammation and neurodegeneration. Apoptosis or programmed cell death and necrosis lead to neuronal cell death in the brain
[52]. An increased burden of neurodegenerative conditions on the health care system and a lack of effective treatments available pose an urgent need to identify new drug targets. The most common feature that has been found in several neurodegenerative diseases such as Parkinson’s disease and Alzheimer’s disease is chronic neuroinflammation. Glial cells have been identified as the mediators of neurodegeneration and are responsible for the onset and progression of these diseases.
Neuronal health is mainly monitored by the nervous system’s immune cells, called microglia
[53]. These cells are activated upon any injury to neurons or infections, which further produces proinflammatory factors (M1 phenotype) or anti-inflammatory factors (M2 phenotype). For a healthy functioning of the human brain, it is necessary to have the correct balance between anti-inflammatory mediators, which allow for the repair and healing of tissues, and proinflammatory mediators, which clear the cellular debris and misfolded protein aggregation is maintained
[54]. The activation of microglia cells in Alzheimer’s and Parkinson’s disease is mainly tilted towards the M1 phenotype, which leads to an exaggeration of inflammation and accelerates the progression of the disease
[55]. The new therapies for the management of neurodegeneration include induction of the M2 phenotype and deactivation of the M1 phenotype in the brain.
Astrocytes are another type of glial cells that are present in the brain and regulate the maintenance and maturation of neuronal cells. They are highly sensitive and respond to injury very quickly, as do microglia cells
[56]. Depending upon their activation, they can be neuroprotective by stimulating repair and reducing inflammation or be neurotoxic by promoting inflammation and contributing to the death of neuronal cells. Activated astrocytes also act as a proinflammatory factor in Parkinson’s disease and Alzheimer’s disease
[57]. Their role has been implicated in the breakdown of the blood–brain barrier, thereby encouraging the infiltration of immune cells into the brain, which increases neuronal death by excessive stimulation and impairment of the uptake of neurotransmitter glutamate. Another type of glial cell, called oligodendrocytes, also poses a significant role in neurodegeneration
[58]. Oligodendrocytes form a sheath of myelin around the nerve fibers, which permits the efficient and rapid transmission of electrical impulses across neurons and thus induces signal transmission. Damage in these cells has been attributed to the progression of multiple sclerosis and other neurodegenerative diseases in which the immune system attacks oligodendrocytes and damages the myelin sheath, thereby reducing levels of myelin proteins in brain tissue
[59].
5. Conclusions
The number of patients suffering from neurological disorders is increasing at an alarming rate. Several pathologies have been identified that cause the onset of neurological diseases; however, there is still a significant gap in the understanding and targeting of them for the development of medications for prevention and cure. With advancing technologies, the understanding of molecular mechanisms in populations exposed to vulnerable neurodegenerative diseases is also improving, which will lead to deeper insights into the functional interplay between several factors such as oxidative stress, neuronal cell death, and neuroinflammation in the occurrence of neurological diseases, which has been described in the article. Eventually, studying pathological mechanisms can lead to the targeted derived production of therapies that will improve global health and invoke management of neurological disorders, thereby improving the quality of life of individuals.