Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Marcel F. Kunrath | + 4048 word(s) | 4048 | 2021-06-04 13:06:44 | | | |
| 2 | Ron Wang | Meta information modification | 4048 | 2021-06-08 05:01:59 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Kunrath, M. Zirconia Implant-Prosthetic Components' Tissue Response. Encyclopedia. Available online: https://encyclopedia.pub/entry/10586 (accessed on 09 May 2026).
Kunrath M. Zirconia Implant-Prosthetic Components' Tissue Response. Encyclopedia. Available at: https://encyclopedia.pub/entry/10586. Accessed May 09, 2026.
Kunrath, Marcel. "Zirconia Implant-Prosthetic Components' Tissue Response" Encyclopedia, https://encyclopedia.pub/entry/10586 (accessed May 09, 2026).
Kunrath, M. (2021, June 07). Zirconia Implant-Prosthetic Components' Tissue Response. In Encyclopedia. https://encyclopedia.pub/entry/10586
Kunrath, Marcel. "Zirconia Implant-Prosthetic Components' Tissue Response." Encyclopedia. Web. 07 June, 2021.
Copy Citation
Dental components manufactured with zirconia (ZrO2) represent a significant percentage of the implant-prosthetic market in dentistry. However, during the last few years, we have observed robust clinical and pre-clinical scientific investigations on zirconia both as a prosthetic and an implantable material. Dental devices manufactured from ZrO2 are structurally and chemically stable with biocompatibility levels allowing for safe and long-term function in the oral environment.
mucointegration
osseointegration
zirconia
biocompatibility
cell response
1. Introduction
The requirements for biomaterials are for them to be biocompatible coupled with high durability while exposed to the harshness of the oral environment. Additionally, they should not affect or interfere with the recipient’s physiology and general health. Prosthetic components and implants made from zirconia (ZrO2) reveal excellent biological and mechanical properties and superior aesthetic advantages when compared to other biomaterials available on the market [1][2][3]. With the ever increasing body of research conducted around zirconia, clinical use of zirconia implants is on the rise due to their biological, aesthetic and physical properties. [4]. Moreover, it presents itself as an excellent material in the manufacture of customized implants, prosthetic components and various other dental prostheses by means of 3D printing technology [5][6][7].
The challenge with products manufactured with ZrO2 is their hardness and the complexity in the treatment of their surfaces [1][8]. However, current advanced manufacturing protocols have been able to develop nanoscale textures on this material by applying techniques such as anodizing, high-intensity lasers, acid etching and surface coatings [8][9][10][11][12]. Gnilitskyi and collaborators reported the use of high-speed femtosecond laser on ZrO2 surfaces for surface nanotexturization, which has been proven to be of significant importance in terms of cell adhesion and osseointegration in an animal model [9]. Thus, the nano-interaction between ZrO2-based surfaces and cells reveals a new and promising path in research which needs more scientific investigation.
Studies on the biological interaction of ZrO2 have become increasingly relevant and are following a path similar to other well proven materials such as titanium and its alloys [13][14]. Rottmar et al. demonstrated that zirconia surfaces had the best performance with regards to fibrinogen adsorption and thrombogenicity [15]. Furthermore, reports prove zirconia to have an advantage in terms of biological properties with soft peri-implant tissues thereby modulating fibers and cell attachment and behavior with greater effectiveness and biocompatibility [16][17]. Along with the properties mentioned above, zirconia has a low surface energy [18][19], therefore it retains very low amounts of plaque and consequently has less bacterial colonization on its surface. In a study, Kunrath et al. showed by comparing surfaces with different morphologies which were exposed to the bacterium Staphylococcus epidermidis that there was less bacterial adhesion on ZrO2 surfaces [18]. Moreover, Roehling et al., revealed a significant reduction in the formation of oral biofilm on zirconia surfaces after 72 hours [19].
2. Zirconia Applications and Variations
With the aim of offering an alternative to metal-based dental prostheses, structural ceramics have been improved and are now widely used in dentistry. Among all dental ceramics, zirconia has emerged as a versatile and promising material due to its biological, mechanical and optical properties which have contributed to its rapid and widespread adoption in dentistry. Zirconia has been a material of choice which, when used with CAD/CAM technology, has allowed the fabrication of various prosthetic components and customized implants for a broad range of treatment options. Zirconia-based ceramics are routinely used for structural applications in engineering such as in the manufacturing of cutting tools, gas sensors, refractories and structural opacifiers [20]. The ceramic composites that are currently in use in medical and dental devices originated from structural materials used in the aerospace and military industry. In order to meet structural demands, zirconia is doped with stabilizers to achieve high strength and fracture toughness [21]. These materials have been modified to suit the additional requirements of biocompatibility [22].
3. Surface Modifications Aiming at Improved Biological Responses
3.1. Sand Blasting
Sandblasting, which is also known as airborne particle abrasion, produces a surface topography that has micro-roughness. Various parameters affect the roughness that is created on the implant surface, this includes the size, shape and kinetic energy of the particles used in the sandblasting process [23]. During the process of sandblasting, compressed air pressure creates an impulse which ejects the particles toward the surface of the implant. Thus, the kinetic energy which is obtained by the particles depends on their density, volume and velocity. The main advantage of the process of sandblasting is that a homogenous and gentle anisotropic abrasion can be obtained on hard materials like ceramic, glass and silicon. Alumina particles are the generally preferred sandblasting materials because of their low cost, hardness and needle-like shape. The major disadvantage of using the sandblasting technique is that it may slightly change the surface chemistry because of inevitable alumina contamination and in the case of ceramics induce micro-cracks within the implant or the prosthetic part prior to any functional stresses [24]. Many studies have proven that although the sandblasted zirconia surfaces show slight enhancement in cell attachment, their metabolic activity is still inferior to that of etched zirconia surfaces [23][25].
3.2. Acid Etching
The process of acid etching is performed with either hydrofluoric acid, nitric acid or sulfuric acid. Acid etching treatment can also be used to overcome alumina contamination as it has been proven to remove the alumina residues (Table 1). Heat treatment follows thereafter, which helps smoothen the sharp edges made as a result of the etching process [26]. Advantages of acid etching include the homogenous roughening of the material, regardless of its size and shape [27]. This method presents no risk of delamination and does not exert stress on the material [28]. However, it might cause undesirable chemical changes which can be a disadvantage of the process [29]. The topography formed after acid etching depends on prior treatment, composition of acid mixture, temperature and the length of exposure to the etchant. Acid etching is generally used to generate a micro scale surface texture which has the ability to achieve interlocking between the implant and the bone [27]. Recent studies show that combining the sandblasting and acid etching techniques enhances the degree of micro-roughness of zirconia as well. Such a combination has been proposed and is currently used in some commercially available zirconia implants; the purpose is to optimize micro-roughness, which would also provide a more receptive surface for osteoblast cell attachment and proliferation [26][30].
Table 1. Summary of the current chemical and physical treatments for zirconia implant surface.
| Zirconia Implants Surface Treatments | ||||
|---|---|---|---|---|
| Treatment | Procedure | Disadvantages | Characteristics | References |
| Sandblasting | High pressure alumina (Al2O3) release | Surface micro-cracks, Structural stress, contaminations | Low cost, hardness and needle-like shape | [23][25] |
| Acid etching | Combinations of: (1) ≃48% hydrofluoric acid (HF) (2) ≃70% nitric acid (HNO3) (3) ≃98% Sulfuric acid (H2SO4) |
Undesired chemical changes | Remove the alumina contamination. Micro scale surface texture for bone to implant contact interface | [27][28][29] |
| Selective infiltration technique | Coating and glass heating procedure | Extended only to the surface grains | Nano-porous surface | [31][32] |
| Polishing | Silicon carbide polishing paper with diamond or silica suspension | Smoother surface compared to acid etching and sandblasting | Average surface roughness between 8 and 200 nm. No surface chemistry modifications. | [32][33][34] |
| Laser treatment | (1) CO2 laser (2) ER:YAG (3) Cr:YSGG |
Disrupts chemical structure | No surface contamination. Improve material wettability |
[35][36][37] |
| Ultraviolet light treatment (UVC) | UVC photons | No effects on surface roughness and surface chemistry | Effect of superhydrophilicity | [38][39][40][41][42][43][44] |
| Coating | Obtained by electrophoretic deposition (EPD) and plasma-spraying: (1) Reinforced hydroxyapatite (HA) (2) Calcium Phosphate (Ca(PO)4) (3) Bioglaze (RKKP) |
Coating-implant bond strength and modification of chemical structure | Low cost and a high deposition rate. Good biocompatibility, corrosion resistance, and bioactivity | [45][46][47][48][49][50][51][52] |
| Biofunctionalization | (1) Immobilized arginine—glycine—aspartate (RGD) | Structural chemical changes | Improved biochemical properties and biological responses | [39][40][41][42][43][44][45][46][47][48][49][50][51][52][53][54][55] |
| Self-assembly | Self-assembled monolayers of active organic compound and terminal functionalization | Van der Waals layer interactions | Surface vapor deposition of active organic compound and molecule adhesion | [56][57][58][59][60] |
3.3. Selective Infiltration Technique
This technique involves coating the surface of the material with a specific infiltration glass and then heating it at a temperature higher than its glass transition temperature. This is followed by the infiltration of molten glass that occurs between the material grains (Table 1). This technique can be used for selective roughening because only the surface grains joined with the infiltration glass are involved in the process, thereby allowing control over the area requiring treatment. Traces of infiltration agent left behind, can further be removed by immersion in a solution of 5% hydrofluoric acid and rinsing with water [31]. This selective infiltration etching technique is often used to create a nano-porous surface on zirconia implants [32]. The major advantage of this technique is that the actual surface chemistry of material remains unchanged, and the nanoscale roughness of the surface can be enhanced without losing any material or changing the microscopic surface roughness.
3.4. Polishing
Polishing gives a comparatively smoother surface than acid etching and sandblasting (Table 1). It is known that the epithelial cells are more likely to adhere to rough surfaces (acid etching and sandblasting) as compared to smoother polished surfaces, whereas fibroblasts adhere well onto both roughened and smooth surfaces [33]. Polishing of a zirconia surface is performed by using a silicon carbide polishing paper and a diamond or silica suspension using a polishing machine [34]. Mechanical surface treatment that includes polishing, allows a change in the surface topography without modifying the actual surface chemistry or structural integrity. The average surface roughness of a polished zirconia biomaterial is between 8 and 200 nm [32][34]. Polishing also serves to clean the implant surface to a certain extent, along with giving it a smooth texture.
3.5. Laser Treatment
In contrast with sandblasting and acid etching techniques, laser treatment exerts zero risk of surface contamination as there is no direct contact between the laser and the biomaterial [35]. The laser surface treatments also tend to improve the material wettability by altering the surface properties, which further plays a major role in cell adhesion. The test for wettability is conducted by putting one drop of the liquid on a flat solid surface of the material and the contact angle is further used to represent the final shape of that drop (Table 1). The higher the contact angle, the lower the wettability of the material. The wettability of material also affects the protein adsorption and cellular adhesion [36]. Protein adsorption depends completely on the nature of the protein-bearing aqueous solution, and the cells are believed to behave differently in response to different organization of the adsorbed protein layers. It is therefore important that the implant surface wettability be elevated, thereby allowing optimal protein adsorption. However, the use of lasers on zirconia ceramic has been reported to disrupt its chemical structure with the potential of inducing pre-function cracks and partial transformation to the monoclinic phase as a result [36][37].
3.6. Ultraviolet Light Treatment
Various studies have shown that bone implant contact of the implants treated with ultraviolet (UV) light was deeply enhanced because of the effect of superhydrophilicity (Table 1). A material is described to be superhydrophilic when the contact angle of the water droplet is less than 5° [38][39]. Hydrophilicity is one of the key factors involved in the initial interaction with proteins and cells that is beneficial for the early phases of wound healing and osseointegration [40]. When the hydrophilic oxide surface binds to water, hydroxyl (OH−) and oxygen (O2−) groups are formed on the outermost layer. The formation of hydroxylated oxide surface improves the surface reactivity with the surrounding ions, amino acids and proteins in the tissue fluid. When compared to hydrophobic surfaces, osteoblasts cultured on hydrophilic surfaces have shown to exhibit higher levels of differentiation markers, including alkaline phosphatase and osteocalcin [41][42]. The effect of hydrophilic surfaces on osseointegration can be observed with improvements in the bone implant contact and bone anchorage that occurs in the early stages of bone healing. Other studies have shown that the atomic percentage of hydrocarbon will change after UV treatment [43][44].
3.7. Coating
Coating of yttrium stabilized zirconia (YSZ) with reinforced hydroxyapatite (HA) has shown positive results in the enhancement of adhesive strength and coating stability [42]. Because of their versatility, calcium phosphate (Ca(PO)4)(CP)-based coatings are generally fabricated using plasma-spraying techniques. Despite its numerous drawbacks, this technique is said to provide low cost and a high deposition rate [45][46] (Table 1). For depositing CP-based coatings, new techniques are constantly being developed to address the issues associated with plasma spraying. In an in vitro study, Pardun et al. synthesized a YSZ/HA coating by wet powder spraying (WPS) using a double action airbrush spray. Although WPS shows versatility in coating curved surfaces with different thickness, the long-term stability of these coatings has not been confirmed [47][48].
Because of its simplicity and highly versatile nature, electrophoretic deposition (EPD) has been proposed as an alternative to traditional techniques. An approach that combines both plasma electrolytic oxidation and electrophoretic deposition has been made to fabricate and coat zirconia or hydroxyapatite film on zirconium [49][50][51]. Good biocompatibility, corrosion resistance and bioactivity obtained through this process broadens the potential applications of EPD. Apart from HA, silica is also commonly used as a coating material for zirconia. The use of RKKP has also shown a positive cell response and osseointegration. Coating with RKKP was fabricated using either an enameling and firing technique or thermal treatment. AP40, another silica bioactive glass, was also determined to be comparable in terms of reactivity with RKKP [48]. Frandsen et al. sputter coated a commercial zirconia implant with a film of titanium and conducted anodization to produce a coating of TiO2 nanotubes on the surface. Along with the enhanced osteoblast behavior, superhydrophilicity was also observed on the treated implant [52].
3.8. Biofunctionalization
Biomimetic surface modification, also called biofunctionalization, involves immobilization of biomolecules on the surface to change their biochemical properties and biological responses [39]. Biofunctionalization also allows anchorage of organic components such as proteins, enzymes and peptides on the implant surface thereby determining the type of tissue that develops at the implant-bone interface (Table 1). Arginine-glycine-aspartate (RGD) is commonly used as an adhesive peptide [53]. Many other adhesive proteins are found to possess RGD as their cell recognition site, including fibronectin, fibrinogen and collagen. These RGD sequences are identified using at least one of the integrins [54]. Adhesion proteins and integrins form a pair to provide cell anchorage, differentiation and growth signal. The RGD peptide has shown to be successfully immobilized with physical-chemical modifications (surface polarization) or applying functionalized coatings on Y-TZP and thereby enhancing the biocompatibility of the material as well as cell attachment to its surface [53][55]. The existence of biomolecules at the surface of biomaterials simulates the native cellular micro-environment in control of cell behavior. For instance, Arg-Gly-Asp (RGD), a cell-binding order, which originated from the extracellular matrix (ECM) protein like the fibronectin, has been extensively used because it encourages cell adhesion by enabling integrin receptors. RGD-containing peptides improve the connection of numerous cell types on different types of biomaterials [53][55].
3.9. Self-Assembly
An autonomous process by which the components are organized into patterns or structures without any external intervention is called self-assembly [56] (Table 1). Self-assembled monolayers (SAMs) (Figure 2) are formed by the process of solution deposition, i.e., the immersion of a particular substrate into the solution of an active surfactant in a particular solvent which may either be organic or aqueous, or the solid surface vapor deposition of an active organic compound or by aerosol spraying. The driving force for self-assembly is generally the specific interaction between the head group of the surfactant and substrate surface. Most of the surfactants consist of three distinctive parts, namely, the surface active head group which binds strongly to the surface, the terminal group which is located at the monolayer surface shows the interfacial properties of the assembly and the alkane chain which serves as a linker between the head and the terminal groups and facilitates the packing of the molecules in the monolayer with the Van der Waals interactions between adjacent methylene groups that orient and stabilize the monolayer [57]. Therefore, by carefully composing the mixture of substrate, SAM solution, and subsequent terminal functionalization, a multitude of subsequent molecule adhesions is feasible [58][59][60][61]. In this typical procedure, clean or freshly prepared substrate is absorbed in a diluted 1/10 ml solution of surfactant compound(s) in highly pure solvent for 12–48 h at room temperature. After this, the slides are vacated, cleaned with solvent and dried under a flow of nitrogen [57][59]. Nanoscale modifications of dental implants have been an active scientific research area, where new techniques such as SAMs are offering approaches to standardize tissue response and microbiota micro environment in accordance with the conditions of bio-activity, anti-adhesion, anti-bacterial or combined effects (Table 1).
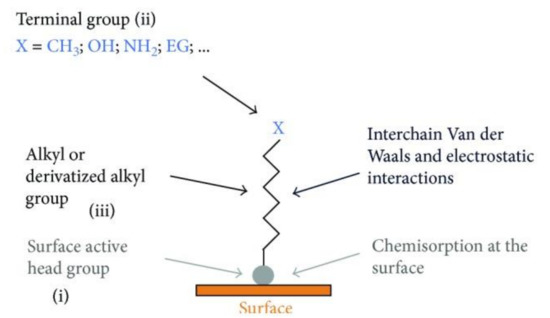
Figure 2. Scheme demonstrating the process of SAMs formation. Detailed chemical parts of the surface functionalization (i, ii and iii). Reprinted with permission under Creative Commons Attribution 4.0 International License, reference [57].
4. Biological Responses
The biological responses performed after the placement of a biomaterial in the oral environment are very important for tissues where there is a need for healing [3][12][13]. Surface modifications, functionalization of ZrO2, as well as innovations in the base-material can induce individualized cellular responses promoting a better performance of the device once it is implanted [9][12][17][62]. As a result, intraosseous implants, components for implants and oral prostheses made from ZrO2 have attracted the attention of researchers and clinicians due to their biocompatibility properties (Table 2). Materials made from ZrO2 have consistently shown better biological reactions in periodontal and epithelial tissues where most of the cells are fibroblasts, red-blood cells, platelets, defense and epithelial cells [63][64][65][66][67][68][69][70][71][72][73][74][75][76][77][78][79][80][81][82][83][84][85][86][87][88][89][90][91][92]. In addition, these cells are crucial for the short and long-term success of biomaterials placed in the oral environment although their original task is to protect against contamination from the external environment. Active in vitro/in vivo research is being developed to discover the main ways to modify ZrO2 for better modulation of cells found in soft tissues (Figure 3 and Figure 4).

Figure 3. Different ZrO2-surfaces morphologies modified by varied surface treatments (a–f). Microscopies using electron microscopy (SEM) and confocal microscopy showing the different responses of osteoprogenitor cells regarding morphology and nuclei position on four different ZrO2-modified surfaces. The cells presented an elongated morphology in some surfaces (g,h) and a flattened morphology in other topographies (i,j). Showing, as reported in the study, that surface morphology characteristics in zirconia are more important for cell evolution and consequent proliferation than properties such as roughness and wettability. Reprinted and adapted with permission under Creative Commons Attribution 4.0 International License, reference [76].
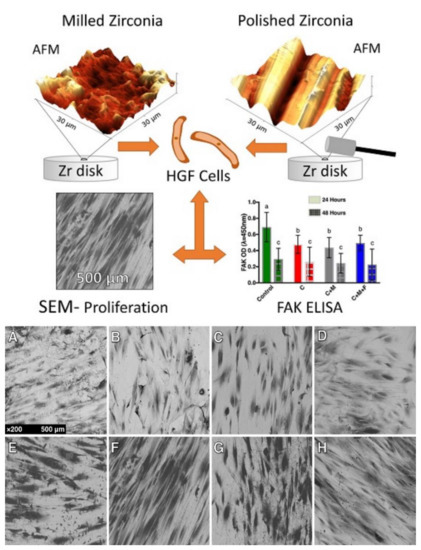
Figure 4. SEM micrographs demonstrating the different behavior and alignment of human gingival fibroblasts on different ZrO2-modified surfaces developed for implant abutments submitted to three different polishing protocols under a 24-h culture (A–D) and 48-h culture (E–H). The more polished surfaces showed greater cell counts (B–D, F–H) revealing an influence of polishing in the proliferation of this cell at 24 h and 48 h. Letters (a,b,c) represent statistical significance between the groups. Reprinted with permission under Creative Commons Attribution 4.0 International License, reference [80].
Table 2. Summary of the current cellular and tissular interactions of the ZrO2 derivates.
| ZrO2-Derivates Interactions | ||||
|---|---|---|---|---|
| Cellular and Tissular Response | Tissue | Cells | Effects | References |
| Connective tissue cells | Fibroblasts Macrophages |
-Increased cells migration and proliferation. -Fibronectin and vitronectin release. -Collagen and extracellular matrix proteins release. -Better cellular activity with hydrophilic surfaces. |
[77][78][79][80][81][82][83][84] | |
| Blood cells | Erythrocytes Platelets |
-Fibrinogen cascade activation. -Plasma proteins activation. |
[63][64][65][66] | |
| Defense cells | Neutrophils, Leukocytes | -Histamine release. -Mast cell degranulation. |
[63][64][65][66][67][68][69][70][71][72][73][74][75][76][77][78][79][80][81][82][83][84][85][86][87][88][89][90][91][92][93] | |
| Epithelium tissue | Epithelial cells | -Increased differentiation and proliferation. -Faster healing process and protective scarring. |
[85][86][87][88][89] | |
| Osteoprogenitors | Osteoblasts | -Increased migration and proliferation. -Increased activity of osteopontin, osteocalcin, BMP-2 genes.-Osteoprogenitors sells adherence and proliferation. |
[69][70][71][72][73][74][75][76] | |
| Oral biofilms cells | Bacteria cells | -Lower bacterial adhesion and proliferation. -Reduced bacteria activity. |
[94][95][96][97][98][99][100][101][102] | |
5. Clinical Benefits
5.1. Osseointegration of Zirconia Implants
Osseointegration is one of the most important criteria for the success of an implant treatment. Bone apposition that takes place on different types of implant surfaces depends on the surface properties of the implant [103][104]. Authors suggested [105] that zirconia coating on the surface of titanium implants favors bone apposition more than titanium uncoated implants. The coating provides a favorable interaction between the bone-implant region promoting the development of more mature bone apposition [105].
Regarding post-loading osseointegration evaluation, Akagawa et al. [106], found that there is no significant difference in clinical features between the loaded and unloaded zirconia implants. However, the bone-implant contact for the unloaded group was 81.9% whereas it was 69.8% for the loaded group (Table 3). Another study that examined the role of osseointegration under various loading conditions around one-stage threaded zirconia implants, showed no difference in bone-implant contact ratio among the single freestanding, connected freestanding and mixed implant-tooth prosthetics using partially stabilized zirconia implants [107]. These findings were in agreement with a report that compared the bone-implant contact (BIC) (after 4 weeks of healing) of submerged zirconia implants, non-submerged zirconia implants and submerged titanium as the control [108] (Table 3). The results demonstrated the best performance with regards to bone-volume density in submerged zirconia implants (80%), followed by submerged titanium (74%) and non-submerged zirconia (63%) [108]. Moreover, no statistical difference was found between the BIC of all three types of implants when zirconia implants were compared to titanium and alumina [109]. Based on some studies, it was also suggested that the zirconia implants might withstand occlusal loads over a longer period of time [110].
Table 3. Summary of the hard tissues’ response of the ZrO2-based materials.
| Bone Tissue Response to ZrO2 | |||
|---|---|---|---|
| Effect | Author | Effectiveness | Reference |
| Implant Loading | Akagawa et al. Stadlinger et al. |
No bone-implant contact (BIC) with significant difference between the loaded and unloaded zirconia implants (BIC loaded: 81.9%; BIC unloaded: 69.8%). No BIC significant difference submerged zirconia and the non-submerged zirconia implants. |
[106][108] |
| Chemical Property | Gahlert et al. Noumbissi et al. Sollazzo et al. |
No difference of bone formation pattern in direct contact with zirconia and surface-modified titanium implant surfaces. Zirconia oxide high resistance to corrosion and ions release. Higher BIC percentage of zirconia implant compared to titanium implant. |
[105][111][112] |
| Surface Treatments | Sennerby et al. | Sandblasted zirconia implants can achieve a higher stability in bone than machined zirconia implants. | [113] |
| Biocompatibility | Liagre et al. Hisbergues et al. Helmer et al. |
No pseudo-teratogen effect. No evidence of high cytotoxicity or inflammation. No evidence of local bone reaction associated to the alumina treatment. |
[114][115][116] |
5.2. Clinical Stability of Zirconia Implants
There are generally two types of modalities to assess osseointegration of dental implants. There are destructive methods such as the pull-push technique and reverse torque and on the other hand there are non-destructive modalities such as resonance frequency analysis (RFA) and the Periotest. It should be noted that none of those techniques and modalities measure osseointegration per se, they rather assess implant stability. The Periotest assesses stability by measuring the amount of micromovement of the implant and the RFA measures the frequency returning from an implant. In both cases, values are given to the measurements and correspond to a certain level of implant stability. Torque removal forces are used as a biomechanical measure for anchorage or osseointegration in which the greater forces required to remove implants may be portrayed as an increase in the strength of osseointegration [117] (Table 3).
5.3. Clinical Cytotoxicity and Soft Tissue Response to Zirconia Implants
To test the biocompatibility of zirconia, various in vitro tests were conducted on osteoblasts, fibroblasts, lymphocytes, monocytes and macrophages where it was observed that zirconia had no cytotoxic effect on the bone forming cells and rather made them capable of elaborating the extracellular matrix by synthesizing various essential and structural proteins [66]. Zirconia is biocompatible as it does not induce any pseudo-teratogen effect [114] (Table 3). Laser-modified zirconia has shown a better adhesion to the bone forming cells due to their high wettability. Furthermore, it does not activate the pathologic inflammatory pathways as reported by Liagre et al. [114]. When tested with fibroblasts, wear products of zirconia friction showed cytotoxic only with a high percentage of particles release [118]. However, it has also been noted that further studies are required to provide any evidence. Both the powder and particle forms of zirconia when tested in vitro on different cell lines (human and murine) like lymphocytes, monocytes or macrophages, did not induce elevated cytotoxicity or inflammation compared to titanium [115] (Table 3).
During in vivo biocompatibility tests of zirconia, it was found that when it was implanted in the soft tissue, a thin layer of fibrous tissue encapsulated it, like what is seen with alumina. Furthermore, no cytotoxicity was observed in the soft tissue in relation to wear products of zirconia [119][120]. According to the findings of a study where pellets of stabilized zirconia with 6% Y2O3 were inserted into the femurs of monkeys, zirconia was found to be biocompatible to hard tissue when tested in vivo. As compared to alumina, no difference in bone reaction was seen in case of zirconia [116]. In a study by Kohal et al., it was found that cell proliferation around zirconia was comparable to that of titanium, but the surface modification of zirconia did not show any improvement in osseointegration [26].
References
- Zhang, Y.; Lawn, B.R. Evaluating dental zirconia. Dent. Mater. 2019, 35, 15–23.
- Chen, Y.-W.; Moussi, J.; Drury, J.L.; Wataha, J.C. Zirconia in biomedical applications. Expert Rev. Med. Devices 2016, 13, 945–963.
- Bosshardt, D.D.; Chappuis, V.; Buser, D. Osseointegration of titanium, titanium alloy and zirconia dental implants: Current knowledge and open questions. Periodontol. 2000 2017, 73, 22–40.
- Lorusso, F.; Noumbissi, S.; Francesco, I.; Rapone, B.; Khater, A.G.A.; Scarano, A. Scientific trends in clinical research on zirconia dental implants: A bibliometric review. Materials 2020, 13, 5534.
- Scarano, A.; Stoppaccioli, M.; Casolino, T. Zirconia crowns cemented on titanium bars using CAD/CAM: A five-year follow-up prospective clinical study of 9 patients. BMC Oral Health 2019, 19, 286.
- Kunrath, M.F. Customized dental implants: Manufacturing processes, topography, osseointegration and future perspectives of 3D fabricated implants. Bioprinting 2020, e00107.
- Wang, W.; Yu, H.; Liu, Y.; Jiang, X.; Gao, B. Trueness analysis of zirconia crowns fabricated with 3-dimensional printing. J. Prosthet. Dent. 2019, 121, 285–291.
- Gupta, S.; Noumbissi, S.; Kunrath, M.F. Nano modified zirconia dental implants: Advances and the frontiers for rapid osseointegration. Med. Devices Sens. 2020, 3, e10076.
- Gnilitskyi, I.; Pogorielov, M.; Viter, R.; Ferraria, A.M.; Carapeto, A.P.; Oleshko, O.; Orazi, L.; Mishchenko, O. Cell and tissue response to nanotextured Ti6Al4V and Zr implants using high-speed femtosecond laser-induced periodic surface structures. Nanomed. Nanotechnol. Biol. Med. 2019, 21, 102036.
- De la Hoz, M.F.T.; Katunar, M.R.; González, A.; Sanchez, A.G.; Díaz, A.O.; Ceré, S. Effect of anodized zirconium implants on early osseointegration process in adult rats: A histological and histomorphometric study. Prog. Biomater. 2019, 8, 249–260.
- Pobloth, A.-M.; Mersiowsky, M.J.; Kliemt, L.; Schell, H.; Dienelt, A.; Pfitzner, B.M.; Burgkart, R.; Detsch, R.; Wulsten, D.; Boccaccini, A.R. Bioactive coating of zirconia toughened alumina ceramic implants improves cancellous osseointegration. Sci. Rep. 2019, 9, 1–16.
- Kunrath, M.F.; Diz, F.M.; Magini, R.; Galárraga-Vinueza, M.E. Nanointeraction: The profound influence of nanostructured and nano-drug delivery biomedical implant surfaces on cell behavior. Adv. Colloid Interface Sci. 2020, 102265.
- Altmann, B.; Rabel, K.; Kohal, R.J.; Proksch, S.; Tomakidi, P.; Adolfsson, E.; Bernsmann, F.; Palmero, P.; Fürderer, T.; Steinberg, T. Cellular transcriptional response to zirconia-based implant materials. Dent. Mater. 2017, 33, 241–255.
- Hanawa, T. Zirconia versus titanium in dentistry: A review. Dent. Mater. J. 2020, 39, 24–36.
- Rottmar, M.; Müller, E.; Guimond-Lischer, S.; Stephan, M.; Berner, S.; Maniura-Weber, K. Assessing the osteogenic potential of zirconia and titanium surfaces with an advanced in vitro model. Dent. Mater. 2019, 35, 74–86.
- Iinuma, Y.; Hirota, M.; Hayakawa, T.; Ohkubo, C. Surrounding tissue response to surface-treated zirconia implants. Materials 2020, 13, 30.
- Da Cruz, M.B.; Marques, J.F.; Fernandes, B.F.; Costa, M.; Miranda, G.; da Mata, A.D.S.P.; Carames, J.M.M.; Silva, F.S. Gingival fibroblasts behavior on bioactive zirconia and titanium dental implant surfaces produced by a functionally graded technique. J. Appl. Oral Sci. 2020, 28.
- Kunrath, M.F.; Monteiro, M.S.; Gupta, S.; Hubler, R.; de Oliveira, S.D. Influence of titanium and zirconia modified surfaces for rapid healing on adhesion and biofilm formation of staphylococcus epidermidis. Arch. Oral Biol. 2020, 117, 104824.
- Roehling, S.; Astasov-Frauenhoffer, M.; Hauser-Gerspach, I.; Braissant, O.; Woelfler, H.; Waltimo, T.; Kniha, H.; Gahlert, M. In vitro biofilm formation on titanium and zirconia implant surfaces. J. Periodontol. 2017, 88, 298–307.
- Rashad, M.M.; Baioumy, H.M. Effect of thermal treatment on the crystal structure and morphology of zirconia nanopowders produced by three different routes. J. Mater. Process. Technol. 2008, 195, 178–185.
- Kelly, J.R.; Denry, I. stabilized zirconia as a structural ceramic: An overview. Dent. Mater. 2008, 24, 289–298.
- Vagkopoulou, T.; Koutayas, S.O.; Koidis, P.; Strub, J.R. Zirconia in dentistry: Part 1. Discovering the nature of an upcoming bioceramic. Eur. J. Esthet. Dent. 2009, 4.
- Hempel, U.; Hefti, T.; Kalbacova, M.; Wolf-Brandstetter, C.; Dieter, P.; Schlottig, F. Response of osteoblast-like SAOS-2 Cells to zirconia ceramics with different surface topographies. Clin. Oral Implants Res. 2010, 21, 174–181.
- Strickstrock, M.; Rothe, H.; Grohmann, S.; Hildebrand, G.; Zylla, I.M.; Liefeith, K. Influence of surface roughness of dental zirconia implants on their mechanical stability, cell behavior and osseointegration. BioNanoMaterials 2017, 18.
- Roehling, S.K.; Meng, B.; Cochran, D.L. Sandblasted and acid-etched implant surfaces with or without high surface free energy: Experimental and clinical background. In Implant Surfaces and Their Biological and Clinical Impact; Springer: Berlin/Heidelberg, Germany, 2015; pp. 93–136.
- Kohal, R.J.; Bächle, M.; Att, W.; Chaar, S.; Altmann, B.; Renz, A.; Butz, F. Osteoblast and bone tissue response to surface modified zirconia and titanium implant materials. Dent. Mater. Off. Publ. Acad. Dent. Mater. 2013, 29, 763–776.
- Iwaya, Y.; Machigashira, M.; Kanbara, K.; Miyamoto, M.; Noguchi, K.; Izumi, Y.; Ban, S. Surface properties and biocompatibility of acid-etched titanium. Dent. Mater. J. 2008, 27, 415–421.
- Chrcanovic, B.R.; Freire-Maia, B.; Gomez, R.S. Small central odontogenic fibroma mimicking hyperplastic dental follicle and dentigerous cyst. J. Maxillofac. Oral Surg. 2014, 13, 332–336.
- Hoshing, U.A.; Patil, S.; Medha, A.; Bandekar, S.D. Comparison of shear bond strength of composite resin to enamel surface with laser etching versus acid etching: An in vitro evaluation. J. Conserv. Dent. JCD 2014, 17, 320–324.
- Langhoff, J.D.; Voelter, K.; Scharnweber, D.; Schnabelrauch, M.; Schlottig, F.; Hefti, T.; Kalchofner, K.; Nuss, K.; von Rechenberg, B. Comparison of chemically and pharmaceutically modified titanium and zirconia implant surfaces in dentistry: A study in sheep. Int. J. Oral Maxillofac. Surg. 2008, 37, 1125–1132.
- Aboushelib, M.N.; Kleverlaan, C.J.; Feilzer, A.J. Selective infiltration-etching technique for a strong and durable bond of resin cements to zirconia-based materials. J. Prosthet. Dent. 2007, 98, 379–388.
- Aboushelib, M.N.; Osman, E.; Jansen, I.; Everts, V.; Feilzer, A.J. Influence of a nanoporous zirconia implant surface of on cell viability of human osteoblasts. J. Prosthodont. Off. J. Am. Coll. Prosthodont. 2013, 22, 190–195.
- Klinge, B.; Meyle, J. Working group 2 soft-tissue integration of implants. consensus report of working group 2. Clin. Oral Implant. Res. 2006, 17, 93–96.
- Kimura, Y.; Matsuzaka, K.; Yoshinari, M.; Inoue, T. Initial attachment of human oral keratinocytes cultured on zirconia or titanium. Dent. Mater. J. 2012, 31, 346–353.
- Yasuno, K.; Kakura, K.; Taniguchi, Y.; Yamaguchi, Y.; Kido, H. Zirconia implants with laser surface treatment peri implant bone response and enhancement of osseointegration. J. Hard Tissue Biol. 2014, 23, 93–100.
- Hao, L.; Lawrence, J. Effects of CO2 laser irradiation on the wettability and human sin fibroblast cell response of magnesia partially stabilized zirconia. Mater. Sci. Eng. C Mater. Biol. Appl. 2003, 23, 627–639.
- Hao, L.; Ma, D.R.; Lawrence, J.; Zhu, X. Enhancing osteoblast functions on a magnesia partially stabilized zirconia bioceramic by means of laser irradiation. Mater. Sci. Eng. C Mater. Biol. Appl. 2005, 25, 496–502.
- Ogawa, T. Ultraviolet photofunctionalization of titanium implants. Int. J. Oral Maxillofac. Implant. 2014, 29, e95-102.
- Hsu, S.K.; Hsu, H.C.; Ho, W.F.; Yao, C.H.; Chang, P.L.; Wu, S.C. Biomolecular modification of zirconia surfaces for enhanced biocompatibility. Thin Solid Films 2014, 572, 91–98.
- Sawase, T.; Jimbo, R.; Baba, K.; Shibata, Y.; Ikeda, T.; Atsuta, M. Photo-induced hydrophilicity enhances initial cell behavior and early bone apposition. Clin. Oral Implant. Res. 2008, 19, 491–496.
- Tengvall, P.; Lundström, I. Physico-chemical considerations of titanium as a biomaterial. Clin. Mater. 1992, 9, 115–134.
- Zhao, G.; Schwartz, Z.; Wieland, M.; Rupp, F.; Geis-Gerstorfer, J.; Cochran, D.L.; Boyan, B.D. High surface energy enhances cell response to titanium substrate microstructure. J. Biomed. Mater. Res. A 2005, 74, 49–58.
- Sartoretto, S.C.; Alves, A.T.N.N.; Resende, R.F.B.; Calasans-Maia, J.; Granjeiro, J.M.; Calasans-Maia, M.D. early osseointegration driven by the surface chemistry and wettability of dental implants. J. Appl. Oral Sci. 2015, 23, 279–287.
- Tuna, T.; Wein, M.; Swain, M.; Fischer, J.; Att, W. Influence of ultraviolet photofunctionalization on the surface characteristics of zirconia-based dental implant materials. Dent. Mater. Off. Publ. Acad. Dent. Mater. 2015, 31, e14–e24.
- Herman, H. Plasma spray deposition processes. MRS Bull. 1988, 13, 60–67.
- Yang, Y.; Kim, K.-H.; Ong, J.L. A Review on Calcium Phosphate Coatings Produced Using a Sputtering Process--an Alternative to Plasma Spraying. Biomaterials 2005, 26, 327–337.
- Pardun, K.; Treccani, L.; Volkmann, E.; Streckbein, P.; Heiss, C.; Li Destri, G.; Marletta, G.; Rezwan, K. Mixed zirconia calcium phosphate coatings for dental implants: Tailoring coating stability and bioactivity potential. Mater. Sci. Eng. C Mater. Biol. Appl. 2015, 48, 337–346.
- Zhang, B.; Kwok, C.T.; Cheng, F.T.; Man, H.C. Fabrication of nano-structured HA/CNT coatings on Ti6Al4V by electrophoretic deposition for biomedical applications. J. Nanosci. Nanotechnol. 2011, 11, 10740–10745.
- Sandhyarani, M.; Rameshbabu, N.; Venkateswarlu, K.; Rama Krishna, L. Fabrication, Characterization and in-vitro evaluation of nano structured zirconia/hydroxyapatite composite film on zirconium. Surf. Coat. Technol. 2014, 238, 58–67.
- Stanic, V.; Aldini, N.N.; Fini, M.; Giavaresi, G.; Giardino, R.; Krajewski, A.; Ravaglioli, A.; Mazzocchi, M.; Dubini, B.; Bossi, M.G.P.; et al. Osteointegration of bioactive glass-coated zirconia in healthy bone: An in vivo evaluation. Biomaterials 2002, 23, 3833–3841.
- Bosetti, M.; Vernè, E.; Ferraris, M.; Ravaglioli, A.; Cannas, M. In vitro characterisation of zirconia coated by bioactive glass. Biomaterials 2001, 22, 987–994.
- Frandsen, C.J.; Noh, K.; Brammer, K.S.; Johnston, G.; Jin, S. Hybrid micro/nano-topography of a TiO2 nanotube-coated commercial zirconia femoral knee implant promotes bone cell adhesion in vitro. Mater. Sci. Eng. C Mater. Biol. Appl. 2013, 33, 2752–2756.
- Morra, M. Biochemical modification of titanium surfaces: Peptides and ECM proteins. Eur. Cells Mater. 2006, 12, 1–15.
- Schwarz, F.; Herten, M.; Sager, M.; Wieland, M.; Dard, M.; Becker, J. Histological and immunohistochemical analysis of initial and early osseous integration at chemically modified and conventional SLA titanium implants: Preliminary results of a pilot study in dogs. Clin. Oral Implants Res. 2007, 18, 481–488.
- Ruoslahti, E.; Pierschbacher, M.D. New perspectives in cell adhesion: RGD and integrins. Science 1987, 238, 491–497.
- Whitesides, G.M.; Grzybowski, B. Self-assembly at all scales. Science 2002, 295, 2418–2421.
- Freitas, S.C.; Correa-Uribe, A.; Martins, M.C.L.; Pelaez-Vargas, A. Self-assembled monolayers for dental implants. Int. J. Dent. 2018, 2018, 4395460.
- Love, J.C.; Estroff, L.A.; Kriebel, J.K.; Nuzzo, R.G.; Whitesides, G.M. Self-assembled monolayers of thiolates on metals as a form of nanotechnology. Chem. Rev. 2005, 105, 1103–1169.
- Ulman, A. Formation and structure of self-assembled monolayers. Chem. Rev. 1996, 96, 1533–1554.
- Mastrangelo, F.; Quaresima, R.; Canullo, L.; Scarano, A.; Muzio, L.L.; Piattelli, A. Effects of Novel laser dental implant microtopography on human osteoblast proliferation and bone deposition. Int. J. Oral Maxillofac. Implant. 2020, 35, 320–329.
- Aita, H.; Hori, N.; Takeuchi, M.; Suzuki, T.; Yamada, M.; Anpo, M.; Ogawa, T. The effect of ultraviolet functionalization of titanium on integration with bone. Biomaterials 2009, 30, 1015–1025.
- Shahramian, K.; Abdulmajeed, A.; Kangasniemi, I.; Söderling, E.; Närhi, T. TiO2 coating and UV photofunctionalization enhance blood coagulation on zirconia surfaces. BioMed Res. Int. 2019, 2019, 8078230.
- Traini, T.; Caputi, S.; Gherlone, E.; Degidi, M.; Piattelli, A. Fibrin clot extension on zirconia surface for dental implants: A quantitative in vitro study. Clin. Implant Dent. Relat. Res. 2014, 16, 718–727.
- Mödinger, Y.; Teixeira, G.Q.; Neidlinger-Wilke, C.; Ignatius, A. Role of the complement system in the response to orthopedic biomaterials. Int. J. Mol. Sci. 2018, 19, 3367.
- Campelo, C.S.; Chevallier, P.; Vaz, J.M.; Vieira, R.S.; Mantovani, D. Sulfonated chitosan and dopamine based coatings for metallic implants in contact with blood. Mater. Sci. Eng. C Mater. Biol. Appl. 2017, 72, 682–691.
- Rahmati, M.; Mozafari, M. A critical review on the cellular and molecular interactions at the interface of zirconia-based biomaterials. Ceram. Int. 2018, 44, 16137–16149.
- Bharate, V.; Kumar, Y.; Koli, D.; Pruthi, G.; Jain, V. Effect of different abutment materials (zirconia or titanium) on the crestal bone height in 1 year. J. Oral Biol. Craniofacial Res. 2020, 10, 372–374.
- Kolaczkowska, E.; Kubes, P. Neutrophil recruitment and function in health and inflammation. Nat. Rev. Immunol. 2013, 13, 159–175.
- Najeeb, S.; Zafar, M.S.; Khurshid, Z.; Zohaib, S.; Almas, K. The role of nutrition in periodontal health: An update. Nutrients 2016, 8.
- Munro, T.; Miller, C.M.; Antunes, E.; Sharma, D. Interactions of osteoprogenitor cells with a novel zirconia implant surface. J. Funct. Biomater. 2020, 11, 50.
- Da Costa Fernandes, C.J.; Ferreira, M.R.; Bezerra, F.J.B.; Zambuzzi, W.F. Zirconia stimulates ECM-remodeling as a prerequisite to pre-osteoblast adhesion/proliferation by possible interference with cellular anchorage. J. Mater. Sci. Mater. Med. 2018, 29, 41.
- Katunar, M.R.; Gomez Sanchez, A.; Santos Coquillat, A.; Civantos, A.; Martinez Campos, E.; Ballarre, J.; Vico, T.; Baca, M.; Ramos, V.; Cere, S. In vitro and in vivo characterization of anodised zirconium as a potential material for biomedical applications. Mater. Sci. Eng. C Mater. Biol. Appl. 2017, 75, 957–968.
- Mostafa, D.; Aboushelib, M. Bioactive-hybrid-zirconia implant surface for enhancing osseointegration: An in vivo study. Int. J. Implant Dent. 2018, 4, 20.
- Rezaei, N.M.; Hasegawa, M.; Ishijima, M.; Nakhaei, K.; Okubo, T.; Taniyama, T.; Ghassemi, A.; Tahsili, T.; Park, W.; Hirota, M.; et al. Biological and osseointegration capabilities of hierarchically (Meso-/Micro-/Nano-Scale) roughened zirconia. Int. J. Nanomed. 2018, 13, 3381–3395.
- Roehling, S.; Gahlert, M.; Janner, S.; Meng, B.; Woelfler, H.; Cochran, D.L. Ligature-Induced peri-implant bone loss around loaded zirconia and titanium implants. Int. J. Oral Maxillofac. Implants 2019, 34, 357–365.
- Rabel, K.; Kohal, R.-J.; Steinberg, T.; Tomakidi, P.; Rolauffs, B.; Adolfsson, E.; Palmero, P.; Fürderer, T.; Altmann, B. Controlling osteoblast morphology and proliferation via surface micro-topographies of implant biomaterials. Sci. Rep. 2020, 10, 12810.
- Atsuta, I.; Ayukawa, Y.; Kondo, R.; Oshiro, W.; Matsuura, Y.; Furuhashi, A.; Tsukiyama, Y.; Koyano, K. Soft tissue sealing around dental implants based on histological interpretation. J. Prosthodont. Res. 2016, 60, 3–11.
- Yang, Y.; Zheng, M.; Liao, Y.; Zhou, J.; Li, H.; Tan, J. Different behavior of human gingival fibroblasts on surface modified zirconia: A comparison between ultraviolet (UV) light and plasma. Dent. Mater. J. 2019, 38, 756–763.
- Wang, Y.; Zhang, Y.; Sculean, A.; Bosshardt, D.D.; Miron, R.J. Macrophage behavior and interplay with gingival fibroblasts cultured on six commercially available titanium, zirconium, and titanium-zirconium dental implants. Clin. Oral Investig. 2019, 23, 3219–3227.
- Fischer, N.G.; Wong, J.; Baruth, A.; Cerutis, D.R. Effect of clinically relevant CAD/CAM zirconia polishing on gingival fibroblast proliferation and focal adhesions. Materials 2017, 10, 1358.
- Rohr, N.; Zeller, B.; Matthisson, L.; Fischer, J. Surface structuring of zirconia to increase fibroblast viability. Dent. Mater. Off. Publ. Acad. Dent. Mater. 2020, 36, 779–786.
- Nishihara, H.; Haro Adanez, M.; Att, W. Current status of zirconia implants in dentistry: Preclinical tests. J. Prosthodont. Res. 2019, 63, 1–14.
- Naveau, A.; Rignon-Bret, C.; Wulfman, C. Zirconia abutments in the anterior region: A systematic review of mechanical and esthetic outcomes. J. Prosthet. Dent. 2019, 121, 775–781.
- Igarashi, K.; Nakahara, K.; Kobayashi, E.; Watanabe, F.; Haga-Tsujimura, M. Hard and soft tissue responses to implant made of three different materials with microgrooved collar in a dog model. Dent. Mater. J. 2018, 37, 964–972.
- Rigolin, M.S.M.; Basso, F.G.; Hebling, J.; de Costa, C.A.S.; de Assis Mollo Junior, F.; Dorigatti de Avila, E. Effect of different implant abutment surfaces on OBA-09 epithelial cell adhesion. Microsc. Res. Tech. 2017, 80, 1304–1309.
- Okabe, E.; Ishihara, Y.; Kikuchi, T.; Izawa, A.; Kobayashi, S.; Goto, H.; Kamiya, Y.; Sasaki, K.; Ban, S.; Noguchi, T.; et al. Adhesion properties of human oral epithelial-derived cells to zirconia. Clin. Implant Dent. Relat. Res. 2016, 18, 906–916.
- Nothdurft, F.P.; Fontana, D.; Ruppenthal, S.; May, A.; Aktas, C.; Mehraein, Y.; Lipp, P.; Kaestner, L. Differential behavior of fibroblasts and epithelial cells on structured implant abutment materials: A comparison of materials and surface topographies. Clin. Implant Dent. Relat. Res. 2015, 17, 1237–1249.
- Atsuta, I.; Ayukawa, Y.; Furuhashi, A.; Narimatsu, I.; Kondo, R.; Oshiro, W.; Koyano, K. Epithelial sealing effectiveness against titanium or zirconia implants surface. J. Biomed. Mater. Res. A 2019, 107, 1379–1385.
- Madeira, S.; Barbosa, A.; Moura, C.G.; Buciumeanu, M.; Silva, F.S.; Carvalho, O. Aunps and Agμps-functionalized zirconia surfaces by hybrid laser technology for dental implants. Ceram. Int. 2020, 46, 7109–7121.
- Riivari, S.; Shahramian, K.; Kangasniemi, I.; Willberg, J.; Närhi, T.O. TiO2-modified zirconia surface improves epithelial cell attachment. Int. J. Oral Maxillofac. Implants 2019, 34, 313–319.
- Lee, D.-J.; Ryu, J.-S.; Shimono, M.; Lee, K.-W.; Lee, J.-M.; Jung, H.-S. differential healing patterns of mucosal seal on zirconia and titanium implant. Front. Physiol. 2019, 10, 796.
- Shahramian, K.; Gasik, M.; Kangasniemi, I.; Walboomers, X.F.; Willberg, J.; Abdulmajeed, A.; Närhi, T. Zirconia implants with improved attachment to the gingival tissue. J. Periodontol. 2020, 91, 1213–1224.
- Tetè, S.; Zizzari, V.L.; Borelli, B.; De Colli, M.; Zara, S.; Sorrentino, R.; Scarano, A.; Gherlone, E.; Cataldi, A.; Zarone, F. Proliferation and adhesion capability of human gingival fibroblasts onto zirconia, lithium disilicate and feldspathic veneering ceramic in vitro. Dent. Mater. J. 2014, 33, 7–15.
- Singh, B.N.; Veeresh, V.; Mallick, S.P.; Jain, Y.; Sinha, S.; Rastogi, A.; Srivastava, P. Design and evaluation of chitosan/chondroitin sulfate/nano-bioglass based composite scaffold for bone tissue engineering. Int. J. Biol. Macromol. 2019, 133, 817–830.
- Kunrath, M.F.; Dos Santos, R.P.; de Oliveira, S.D.; Hubler, R.; Sesterheim, P.; Teixeira, E.R. Osteoblastic cell behavior and early bacterial adhesion on macro-, micro-, and nanostructured titanium surfaces for biomedical implant applications. Int. J. Oral Maxillofac. Implants 2020, 35, 773–781.
- Degidi, M.; Artese, L.; Scarano, A.; Perrotti, V.; Gehrke, P.; Piattelli, A. Inflammatory infiltrate, microvessel density, nitric oxide synthase expression, vascular endothelial growth factor expression, and proliferative activity in peri-implant soft tissues around titanium and zirconium oxide healing caps. J. Periodontol. 2006, 77, 73–80.
- Scarano, A.; Piattelli, M.; Caputi, S.; Favero, G.A.; Piattelli, A. Bacterial adhesion on commercially pure titanium and zirconium oxide disks: An in vivo human study. J. Periodontol. 2004, 75, 292–296.
- Do Nascimento, C.; Pita, M.S.; Fernandes, F.H.N.C.; Pedrazzi, V.; de Albuquerque, R.F., Jr.; Ribeiro, R.F. Bacterial adhesion on the titanium and zirconia abutment surfaces. Clin. Oral Implants Res. 2014, 25, 337–343.
- Moritz, J.; Abram, A.; Čekada, M.; Gabor, U.; Garvas, M.; Zdovc, I.; Kocjan, A. Nanoroughening of sandblasted 3Y-TZP surface by alumina coating deposition for improved osseointegration and bacteria reduction. J. Eur. Ceram. Soc. 2019, 39, 4347–4357.
- Pérez-Tanoira, R.; Horwat, D.; Kinnari, T.J.; Pérez-Jorge, C.; Gómez-Barrena, E.; Migot, S.; Esteban, J. Bacterial adhesion on biomedical surfaces covered by yttria stabilized zirconia. J. Mater. Sci. Mater. Med. 2016, 27, 6.
- Han, A.; Tsoi, J.K.H.; Lung, C.Y.K.; Matinlinna, J.P. An introduction of biological performance of zirconia with different surface characteristics: A review. Dent. Mater. J. 2020, 39, 523–530.
- Han, A.; Tsoi, J.K.; Rodrigues, F.P.; Leprince, J.G.; Palin, W.M. Bacterial adhesion mechanisms on dental implant surfaces and the influencing factors. Int. J. Adhes. Adhes. 2016, 69, 58–71.
- Zechner, W.; Tangl, S.; Fürst, G.; Tepper, G.; Thams, U.; Mailath, G.; Watzek, G. Osseous healing characteristics of three different implant types. Clin. Oral Implants Res. 2003, 14, 150–157.
- Albrektsson, T.; Wennerberg, A. Oral implant surfaces: Part 2—Review focusing on clinical knowledge of different surfaces. Int. J. Prosthodont. 2004, 17, 544–564.
- Sollazzo, V.; Pezzetti, F.; Scarano, A.; Piattelli, A.; Bignozzi, C.A.; Massari, L.; Brunelli, G.; Carinci, F. Zirconium oxide coating improves implant osseointegration in vivo. Dent. Mater. Off. Publ. Acad. Dent. Mater. 2008, 24, 357–361.
- Akagawa, Y.; Ichikawa, Y.; Nikai, H.; Tsuru, H. Interface histology of unloaded and early loaded partially stabilized zirconia endosseous implant in initial bone healing. J. Prosthet. Dent. 1993, 69, 599–604.
- Akagawa, Y.; Hosokawa, R.; Sato, Y.; Kamayama, K. Comparison between freestanding and tooth-connected partially stabilized zirconia implants after two years’ function in monkeys: A clinical and histologic study. J. Prosthet. Dent. 1998, 80, 551–558.
- Stadlinger, B.; Hennig, M.; Eckelt, U.; Kuhlisch, E.; Mai, R. Comparison of zirconia and titanium implants after a short healing period. a pilot study in minipigs. Int. J. Oral Maxillofac. Surg. 2010, 39, 585–592.
- Dubruille, J.H.; Viguier, E.; Le Naour, G.; Dubruille, M.T.; Auriol, M.; Le Charpentier, Y. Evaluation of combinations of titanium, zirconia, and alumina implants with 2 bone fillers in the dog. Int. J. Oral Maxillofac. Implants 1999, 14, 271–277.
- Kohal, R.-J.; Papavasiliou, G.; Kamposiora, P.; Tripodakis, A.; Strub, J.R. Three-dimensional computerized stress analysis of commercially pure titanium and yttrium-partially stabilized zirconia implants. Int. J. Prosthodont. 2002, 15, 189–194.
- Gahlert, M.; Röhling, S.; Wieland, M.; Sprecher, C.M.; Kniha, H.; Milz, S. Osseointegration of zirconia and titanium dental implants: A histological and histomorphometrical study in the maxilla of pigs. Clin. Oral Implants Res. 2009, 20, 1247–1253.
- Noumbissi, S.; Scarano, A.; Gupta, S. A Literature review study on atomic ions dissolution of titanium and its alloys in implant dentistry. Materials 2019, 12, 368.
- Sennerby, L.; Dasmah, A.; Larsson, B.; Iverhed, M. Bone tissue responses to surface-modified zirconia implants: A histomorphometric and removal torque study in the rabbit. Clin. Implant Dent. Relat. Res. 2005, 7, S13–S20.
- Liagre, B.; Moalic, S.; Vergne, P.; Charissoux, J.L.; Bernache-Assollant, D.; Beneytout, J.L. Effects of alumina and zirconium dioxide particles on arachidonic acid metabolism and proinflammatory interleukin production in osteoarthritis and rheumatoid synovial cells. J. Bone Jt. Surg. Br. 2002, 84, 920–930.
- Hisbergues, M.; Vendeville, S.; Vendeville, P. Zirconia: Established facts and perspectives for a biomaterial in dental implantology. J. Biomed. Mater. Res. B Appl. Biomater. 2009, 88, 519–529.
- Helmer, J.C.; Driskell, T.D. Research on Bioceramics: Symposium on Use of Ceramics as Surgical Implants; Clemson University: Clemson, SC, USA, 1969.
- Klokkevold, P.R.; Nishimura, R.D.; Adachi, M.; Caputo, A. Osseointegration enhanced by chemical etching of the titanium surface. a torque removal study in the rabbit. Clin. Oral Implants Res. 1997, 8, 442–447.
- Ito, A.; Tateishi, T.; Niwa, S.; Tange, S. In-vitro evaluation of the cytocompatibility of wear particles generated by UHMWPE/zirconia friction. Clin. Mater. 1993, 12, 203–209.
- Christel, P.; Meunier, A.; Heller, M.; Torre, J.P.; Peille, C.N. Mechanical properties and short-term in-vivo evaluation of yttrium-oxide-partially-stabilized zirconia. J. Biomed. Mater. Res. 1989, 23, 45–61.
- Ichikawa, Y.; Akagawa, Y.; Nikai, H.; Tsuru, H. Tissue compatibility and stability of a new zirconia ceramic in vivo. J. Prosthet. Dent. 1992, 68, 322–326.
More
Information
Subjects:
Materials Science, Biomaterials
Contributor
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
1.5K
Revisions:
2 times
(View History)
Update Date:
08 Jun 2021
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





