
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Pierantonia Zedde | + 1336 word(s) | 1336 | 2021-11-01 07:45:30 | | | |
| 2 | Amina Yu | Meta information modification | 1336 | 2021-11-16 04:37:42 | | |
Video Upload Options
The vulvar area is a common site of contact dermatitis due to the thin skin, easily traversable by irritant and allergic substances. The nonkeratinized vulvar vestibule is likely to be more permeable than the keratinized portions of the vulva and thus more susceptible to exogenous topical agents. The vulva is an area of occlusion due to both its intrinsic anatomical structure and the frequent use of occlusive napkins or underwear, which increase penetration or absorption of both irritants and allergens. Furthermore, women at different ages, due to urine and feces as children and to vaginal mucosal atrophy and the increase in the vulvar pH in menopause, may have an altered barrier function and, in incontinent elderly subjects, the use of diapers may contribute to increased susceptibility to irritants and allergens.
1. Irritant Contact Dermatitis
| Vulvar Irritants | |
|---|---|
| Strong Irritants | Weak Irritants |
| Imiquimod | Friction/rubbing |
| Trichloroacetic acid | Urine/feces/vaginal secretions/sweat/semen/saliva |
| Podophyllin | Sanitary napkins |
| 5-fluorouracil | Soaps/detergents |
| Antiseptic or scented wipes | |
| Sodium hypochlorite | Deodorants |
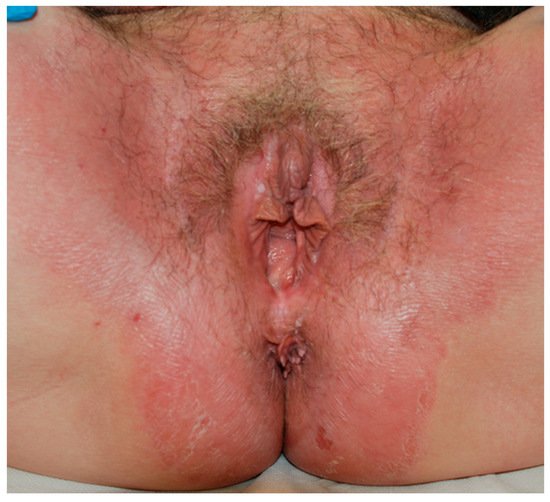
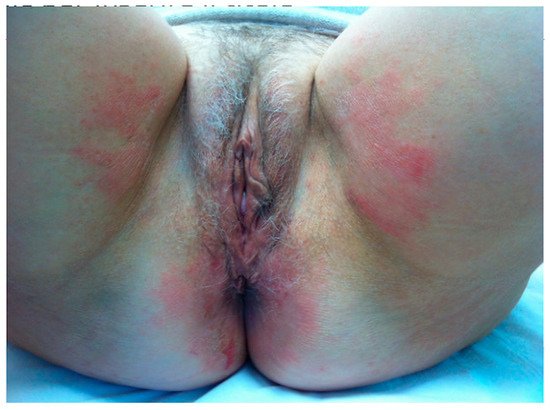
2. Allergic Contact Dermatitis

| Authors | Pathologies | N° Patients | % Positiveness |
% Relevant p.t. |
Allergens | |
|---|---|---|---|---|---|---|
| Doherty et al. | 1990 | Vulvar itching | 50 | 78 | - | nickel, fragrances, neomycin, local anesthetics |
| Marren et al. | 1992 | Vulvar dermatoses | 135 | 47 | 29 | nickel, fragrances, preservatives, ethylenediamine, topical medicaments |
| Brenan et al. | 1996 | Chronic vulvar symptoms | 700 | 42 | - | nickel, fragrances, ethylenediamine |
| Goldsmith et al. | 1997 | Anogenital dermatoses | 201 | 39 | 28 | antibiotics, local anesthetics, fragrances, corticosteroids |
| Lewis et al. | 1997 | Vulvar symptoms | 121 | 58.7 | 49 | local anesthetics, fragrances, neomycin |
| Lucke et al. | 1998 | Vulvar dermatoses | 55 | 65 | - | nickel, fragrances, medicaments, dyes |
| Bauer et al. | 2000 | Anogenital symptoms | 351 | 47 | 34.8 | nickel, fragrances, local anesthetics |
| Crone et al. | 2000 | Vulvar dermatoses | 38 | 47 | 28 | fragrances, preservatives, medicaments |
| Virgili et al. | 2003 | Vulvar lichen simplex chronicus | 61 | 47.5 | 26 | nickel, preservatives, fragrances, medicaments |
| Nardelli et al. | 2004 | Vulvar symptoms | 92 | 38 | 16 | medicaments |
| Utas et al. | 2008 | Vulvar itching | 50 | 52 | 16 | preservatives, fragrances, medicaments |
| Haverhoek et al. | 2008 | Vulvar pruritus | 43 | 81.4 | 44 | preservatives, fragrances, medicaments |
| Warshsoaw et al. | 2008 | Anogenital dermatoses | 570 | 44.1 | 27 | medicaments, corticosteroids |
| Vermaat et al. | 2008 | Anogenital dermatoses | 53 | 66 | 20 | fragrances, spices |
| O’Gorman et al. | 2013 | Vulvar itching | 90 | 69 | 39 | preservatives, fragrances, medicaments |
| Al-Niaimi at al. | 2014 | Vulvar symptoms | 282 | 54 | 49 | nickel, fragrances, neomycin |
| Trivedi et al. | 2018 | Vulvar itching | - | 64 | 54 | preservatives, fragrances |
References
- Bains, S.N.; Nash, P. Irritant Contact Dermatitis. Clin. Rev. Allergy Immunol. 2019, 56, 99–109.
- Nosbaum, A.; Vocanson, M.; Rozieres, A.; Hennino, A.; Nicolas, J.F. Allergic and irritant contact dermatitis. Eur. J. Dermatol. EJD 2009, 19, 325–332.
- Farage, M.A. Vulvar susceptibility to contact irritants and allergens: A review. Arch. Gynecol. Obstet. 2005, 272, 167–172.
- Davis, M.D.P. Unusual patterns in contact dermatitis: Medicaments. Dermatol. Clin. 2009, 27, 289–297.
- Marren, P.; Wojnarowska, F.; Powell, S. Allergic contact dermatitis and vulvar dermatoses. Br. J. Dermatol. 1992, 126, 52–56.
- Brenan, J.A.; Dennerstein, G.J.; Sfameni, S.F.; Drinkwater, P.; Marin, G.; Scurry, J.P. Evaluation of patch testing in patients with chronic vulvar symptoms. Australas. J. Dermatol. 1996, 37, 40–43.
- Goldsmith, P.C.; Rycroft, R.J.G.; White, I.R.; Ridley, C.M.; Neill, S.M.; McFadden, J.P. Contact sensitivity in women with anogenital dermatoses. Contact Dermat. 1997, 36, 174–175.
- Lewis, F.M.; Harrington, C.I.; Gawkrodger, D.J. Contact sensitivity in pruritus vulvae: A common and manageable problem. Contact Dermat. 1994, 31, 264–265.
- Lucke, T.W.; Fleming, C.J.; McHenry, P.; Lever, R. Patch testing in vulval dermatoses: How relevant is nickel? Contact Dermat. 1998, 38, 111–112.
- Bauer, A.; Geier, J.; Elsner, P. Allergic contact dermatitis in patients with anogenital complaints. J. Reprod. Med. 2000, 45, 649–654.
- Crone, A.M.; Stewart, E.; Wojnarowska, F.; Powell, S.M. Aetiological factors in vulvar dermatitis. J. Eur. Acad. Dermatol. Venereol. JEADV 2000, 14, 181–186.
- Utaş, S.; Ferahbaş, A.; Yildiz, S. Patients with vulval pruritus: Patch test results. Contact Dermat. 2008, 58, 296–298.
- Vermaat, H.; Van Meurs, T.; Rustemeyer, T.; Bruynzeel, D.P.; Kirtschig, G. Vulval allergic contact dermatitis due to peppermint oil in herbal tea. Contact Dermat. 2008, 58, 364–365.
- O’Gorman, S.M.; Torgerson, R.R. Allergic contact dermatitis of the vulva. Dermat. Contact Atopic Occup. Drug 2013, 24, 64–72.
- Al-Niaimi, F.; Felton, S.; Williams, J. Patch testing for vulval symptoms: Our experience with 282 patients. Clin. Exp. Dermatol. 2014, 39, 439–442.
- Trivedi, M.K.; Woodruff, C.M.; Kornik, R.; Botto, N. Patch Testing in Vulvar Allergic Contact Dermatitis. Dermat. Contact Atopic Occup. Drug 2018, 29, 95–96.
- Nardelli, A.; Degreef, H.; Goossens, A. Contact allergic reactions of the vulva: A 14-year review. Dermat. Contact Atopic Occup. Drug 2004, 15, 131–136.
- Warshaw, E.M.; Furda, L.M.; Maibach, H.I.; Rietschel, R.L.; Fowler, J.F., Jr.; Belsito, D.V.; Zug, K.A.; DeLeo, V.A.; Marks, J.G., Jr.; Toby Mathias, C.G.; et al. Anogenital dermatitis in patients referred for patch testing: Retrospective analysis of cross-sectional data from the North American Contact Dermatitis Group, 1994–2004. Arch. Dermatol. 2008, 144, 749–755.
- Haverhoek, E.; Reid, C.; Gordon, L.; Marshman, G.; Wood, J.; Selva-Nayagam, P. Prospective study of patch testing in patients with vulval pruritus. Australas. J. Dermatol. 2008, 49, 80–85.
- Virgili, A.; Bacilieri, S.; Corazza, M. Evaluation of contact sensitization in vulvar lichen simplex chronicus. A proposal for a battery of selected allergens. J. Reprod. Med. 2003, 48, 33–36.




