
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Jerôme Appeldoorn | + 2200 word(s) | 2200 | 2021-08-10 10:42:42 | | | |
| 2 | Enzi Gong | Meta information modification | 2200 | 2021-08-20 02:28:38 | | |
Video Upload Options
Creatine is a natural nitrogenous organic acid that is integral to energy metabolism, and is crucial for proper cell functioning [8,9]. Creatine can be charged to the high-energy product phosphocreatine by creatine kinase and ATP. In the human body, the majority of creatine (>90%) is present in skeletal muscle, cardiac muscle, smooth muscle, the brain, and in the nervous tissue. Furthermore, smaller amounts are present in other tissues and cell types, including the kidney, erythrocytes, and leucocytes.
1. Overview
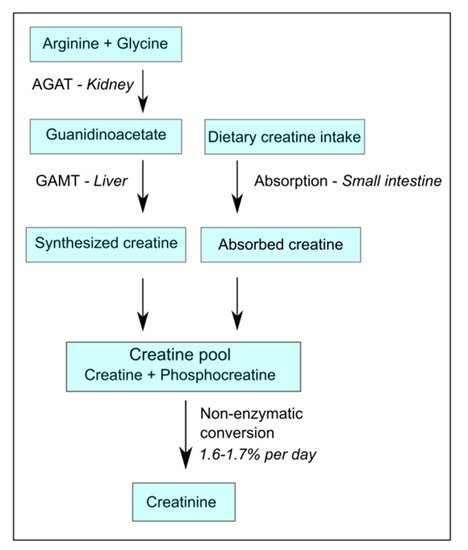
There is great need for the identification of new, potentially modifiable risk factors for the poor health-related quality of life (HRQoL) and of the excess risk of mortality in dialysis-dependent chronic kidney disease patients. Creatine is an essential contributor to cellular energy homeostasis, yet, on a daily basis, 1.6–1.7% of the total creatine pool is non-enzymatically degraded to creatinine and subsequently lost via urinary excretion, thereby necessitating a continuous supply of new creatine in order to remain in steady-state. Because of an insufficient ability to synthesize creatine, unopposed losses to the dialysis fluid, and insufficient intake due to dietary recommendations that are increasingly steered towards more plant-based diets, hemodialysis patients are prone to creatine deficiency, and may benefit from creatine supplementation. To avoid problems with compliance and fluid balance, and, furthermore, to prevent intradialytic losses of creatine to the dialysate, we aim to investigate the potential of intradialytic creatine supplementation in improving outcomes. Given the known physiological effects of creatine, intradialytic creatine supplementation may help to maintain creatine homeostasis among dialysis-dependent chronic kidney disease patients, and consequently improve muscle status, nutritional status, neurocognitive status, HRQoL. Additionally, we describe the rationale and design for a block-randomized, double-blind, placebo-controlled pilot study. The aim of the pilot study is to explore the creatine uptake in the circulation and tissues following different creatine supplementation dosages.
2. End-Stage Kidney Disease
3. Discussion
4. Conclusions
References
- Al Ismaili, F.; Al Salmi, I.; Al Maimani, Y.; Metry, A.M.; Al Marhoobi, H.; Hola, A.; Pisoni, R.L. Epidemiological Transition of End-Stage Kidney Disease in Oman. Kidney Int. Rep. 2017, 2, 27–35.
- Kraus, M.A.; Fluck, R.J.; Weinhandl, E.D.; Kansal, S.; Copland, M.; Komenda, P.; Finkelstein, F.O. Intensive Hemodialysis and Health-Related Quality of Life. Am. J. Kidney Dis. 2016, 68, S33–S42.
- Ma, L.; Zhao, S. Risk factors for mortality in patients undergoing hemodialysis: A systematic review and meta-analysis. Int. J. Cardiol. 2017, 238, 151–158.
- Wallimann, T.; Riek, U.; Möddel, M. Intradialytic creatine supplementation: A scientific rationale for improving the health and quality of life of dialysis patients. Med. Hypotheses 2017, 99, 1–14.
- Levin, A. Identification of patients and risk factors in chronic kidney disease-evaluating risk factors and therapeutic strategies. Nephrol. Dial. Transplant. 2001, 16, 57–60.
- McQuillan, R.; Trpeski, L.; Fenton, S.; Lok, C.E. Modifiable risk factors for early mortality on hemodialysis. Int. J. Nephrol. 2012, 2012, 435736.
- Post, A.; Tsikas, D.; Bakker, S.J.L. Creatine is a conditionally essential nutrient in chronic kidney disease: A hypothesis and narrative literature review. Nutrients 2019, 11, 1044.
- Wyss, M.; Kaddurah-Daouk, R. Creatine and Creatinine Metabolism. Physiol. Rev. 2000, 80, 1107–1213.
- Wallimann, T.; Tokarska-Schlattner, M.; Schlattner, U. The creatine kinase system and pleiotropic effects of creatine. Amino Acids 2011, 40, 1271–1296.
- Clark, J.F. Creatine and Phosphocreatine: A Review of Their Use in Exercise and Sport. J. Athl. Train. 1997, 32, 45.
- Wilson, F.P.; Xie, D.; Anderson, A.H.; Leonard, M.B.; Reese, P.P.; Delafontaine, P.; Horwitz, E.; Kallem, R.; Navaneethan, S.; Ojo, A.; et al. Urinary Creatinine Excretion, Bioelectrical Impedance Analysis, and Clinical Outcomes in Patients with CKD: The CRIC Study. Clin. J. Am. Soc. Nephrol. 2014, 9, 2095–2103.
- Brosnan, J.T.; da Silva, R.P.; Brosnan, M.E. The metabolic burden of creatine synthesis. Amino Acids 2011, 40, 1325–1331.
- Da Silva, R.P.; Clow, K.; Brosnan, J.T.; Brosnan, M.E. Synthesis of guanidinoacetate and creatine from amino acids by rat pancreas. Br. J. Nutr. 2014, 111, 571–577.
- Edison, E.E.; Brosnan, M.E.; Meyer, C.; Brosnan, J.T. Creatine synthesis: Production of guanidinoacetate by the rat and human kidney in vivo. Am. J. Physiol. Ren. Physiol. 2007, 293, 1799–1804.
- Verrey, F.; Singer, D.; Ramadan, T.; Vuille-Dit-Bille, R.N.; Mariotta, L.; Camargo, S.M.R. Kidney amino acid transport. Pflug. Arch. Eur. J. Physiol. 2009, 458, 53–60.
- Weisbord, S.D.; Fried, L.F.; Arnold, R.M.; Rotondi, A.J.; Fine, M.J.; Levenson, D.J.; Switzer, G.E. Development of a symptom assessment instrument for chronic hemodialysis patients: The dialysis symptom index. J. Pain Symptom Manag. 2004, 27, 226–240.
- Hendriks, F.K.; Smeets, J.S.J.; Broers, N.J.H.; van Kranenburg, J.M.X.; van der Sande, F.M.; Kooman, J.P.; Van Loon, L.J.C. End-stage renal disease patients lose a substantial amount of amino acids during hemodialysis. J. Nutr. 2020, 150, 1160–1166.
- Post, A.; Schutten, J.C.; Kremer, D.; van der Veen, Y.; Groothof, D.; Sotomayor, C.G.; Koops, C.A.; de Blaauw, P.; Kema, I.P.; Westerhuis, R.; et al. Creatine homeostasis and protein energy wasting in hemodialysis patients. J. Transl. Med. 2021, 19, 115.
- Joshi, S.; McMacken, M.; Kalantar-Zadeh, K. Plant-Based Diets for Kidney Disease: A Guide for Clinicians. Am. J. Kidney Dis. 2021, 77, 287–296.
- Carrero, J.J.; González-Ortiz, A.; Avesani, C.M.; Bakker, S.J.L.; Bellizzi, V.; Chauveau, P.; Clase, C.M.; Cupisti, A.; Espinosa-Cuevas, A.; Molina, P.; et al. Plant-based diets to manage the risks and complications of chronic kidney disease. Nat. Rev. Nephrol. 2020, 16, 525–542.
- Balestrino, M.; Adriano, E. Beyond sports: Efficacy and safety of creatine supplementation in pathological or paraphysiological conditions of brain and muscle. Med. Res. Rev. 2019, 39, 2427–2459.
- Ostojic, S.M. Dietary creatine intake in U.S. population: NHANES 2017–2018. Nutrition 2021, 87–88, 111207.
- Pastoris, O.; Aquilani, R.; Foppa, P.; Bovio, G.; Segagni, S.; Baiardi, P.; Catapano, M.; Maccario, M.; Salvadeo, A.; Dossena, M. Altered muscle energy metabolism in post-absorptive patients with chronic renal failure. Scand. J. Urol. Nephrol. 1997, 31, 281–287.
- Durozard, D.; Pimmel, P.; Baretto, S.; Caillette, A.; Labeeuw, M.; Baverel, G.; Zech, P. 31P NMR spectroscopy investigation of muscle metabolism in hemodialysis patients. Kidney Int. 1993, 43, 885–892.
- Tagami, T.; Sakuma, H.; Matsumura, K.; Takeda, K.; Mori, S.; Takeuchi, T.; Nakano, T. Evaluation of altered myocardial high energy phosphate metabolism patients on maintenance dialysis using phosphorus-31 magnetic resonance spectroscopy. Investig. Radiol. 1998, 33, 171–176.
- Ogimoto, G.; Sakurada, T.; Imamura, K.; Kuboshima, S.; Maeba, T.; Kimura, K.; Owada, S. Alteration of energy production by the heart in CRF patients undergoing peritoneal dialysis. Mol. Cell. Biochem. 2003, 244, 135–138.
- Devries, M.C.; Phillips, S.M. Creatine supplementation during resistance training in older adults-a meta-analysis. Med. Sci. Sports Exerc. 2014, 46, 1194–1203.
- Chilibeck, P.D.; Kaviani, M.; Candow, D.G.; Zello, G.A. Effect of creatine supplementation during resistance training on lean tissue mass and muscular strength in older adults: A meta-analysis. Open Access J. Sports Med. 2017, 8, 213.
- Kreider, R.B.; Kalman, D.S.; Antonio, J.; Ziegenfuss, T.N.; Wildman, R.; Collins, R.; Candow, D.G.; Kleiner, S.M.; Almada, A.L.; Lopez, H.L. International Society of Sports Nutrition position stand: Safety and efficacy of creatine supplementation in exercise, sport, and medicine. J. Int. Soc. Sports Nutr. 2017, 14, 18.
- Sabatino, A.; Regolisti, G.; Karupaiah, T.; Sahathevan, S.; Sadu Singh, B.K.; Khor, B.H.; Salhab, N.; Karavetian, M.; Cupisti, A.; Fiaccadori, E. Protein-energy wasting and nutritional supplementation in patients with end-stage renal disease on hemodialysis. Clin. Nutr. 2017, 36, 663–671.
- Jadeja, Y.P.; Kher, V. Protein energy wasting in chronic kidney disease: An update with focus on nutritional interventions to improve outcomes. Indian J. Endocrinol. Metab. 2012, 16, 246.
- Farshidfar, F.; Pinder, M.A.; Myrie, S.B. Creatine Supplementation and Skeletal Muscle Metabolism for Building Muscle Mass- Review of the Potential Mechanisms of Action. Curr. Protein Pept. Sci. 2017, 18, 1273–1287.
- Kreider, R.B.; Stout, J.R. Creatine in health and disease. Nutrients 2021, 13, 447.
- Tamopolsky, M.; Zimmer, A.; Paikin, J.; Safdar, A.; Aboud, A.; Pearce, E.; Roy, B.; Doherty, T. Creatine monohydrate and conjugated linoleic acid improve strength and body composition following resistance exercise in older adults. PLoS ONE 2007, 2, e991.
- Dolan, E.; Artioli, G.G.; Pereira, R.M.R.; Gualano, B. Muscular Atrophy and Sarcopenia in the Elderly: Is There a Role for Creatine Supplementation? Biomolecules 2019, 9, 642.
- Zyga, S.; Alikari, V.; Sachlas, A.; Fradelos, E.C.; Stathoulis, J.; Panoutsopoulos, G.; Georgopoulou, M.; Theophilou, P.; Lavdaniti, M. Assessment of Fatigue in End Stage Renal Disease Patients Undergoing Hemodialysis: Prevalence and Associated Factors. Med. Arch. 2015, 69, 376–380.
- Ramkumar, N.; Beddhu, S.; Eggers, P.; Pappas, L.M.; Cheung, A.K. Patient preferences for in-center intense hemodialysis. Hemodial. Int. 2005, 9, 281–295.
- Balestrino, M.; Adriano, E. Creatine as a Candidate to Prevent Statin Myopathy. Biomolecules 2019, 9, 496.
- Angermann, S.; Schier, J.; Baumann, M.; Steubl, D.; Hauser, C.; Lorenz, G.; Günthner, R.; Braunisch, M.C.; Kemmner, S.; Satanovskij, R.; et al. Cognitive Impairment is Associated with Mortality in Hemodialysis Patients. J. Alzheimer’s Dis. 2018, 66, 1529–1537.
- Sehgal, A.R.; Grey, S.F.; DeOreo, P.B.; Whitehouse, P.J. Prevalence, recognition, and implications of mental impairment among hemodialysis patients. Am. J. Kidney Dis. 1997, 30, 41–49.
- Roschel, H.; Gualano, B.; Ostojic, S.M.; Rawson, E.S. Creatine Supplementation and Brain Health. Nutrients 2021, 13, 586.
- Kious, B.M.; Kondo, D.G.; Renshaw, P.F. Creatine for the treatment of depression. Biomolecules 2019, 9, 406.
- Bakian, A.V.; Huber, R.S.; Scholl, L.; Renshaw, P.F.; Kondo, D. Dietary creatine intake and depression risk among U.S. adults. Transl. Psychiatry 2020, 10, 1–11.
- Seliger, S.L.; Weiner, D.E. Cognitive Impairment in Dialysis Patients: Focus on the Blood Vessels? Am. J. Kidney Dis. 2013, 61, 187.
- Bredahl, E.C.; Eckerson, J.M.; Tracy, S.M.; McDonald, T.L.; Drescher, K.M. The Role of Creatine in the Development and Activation of Immune Responses. Nutrients 2021, 13, 751.
- Sestili, P.; Martinelli, C.; Colombo, E.; Barbieri, E.; Potenza, L.; Sartini, S.; Fimognari, C. Creatine as an antioxidant. Amino Acids 2011, 40, 1385–1396.
- Clarke, H.; Kim, D.-H.; Meza, C.A.; Ormsbee, M.J.; Hickner, R.C. The Evolving Applications of Creatine Supplementation: Could Creatine Improve Vascular Health? Nutrients 2020, 12, 2834.
- Lipovac, V.; Gavella, M.; Vuči´c, M.V.; Mrzljak, V.; Roči´c, B.R. Effect of creatine on erythrocyte rheology in vitro. Clin. Hemorheol. Microcirc. 2000, 22, 45–52.
- Tokarska-Schlattner, M.; Epand, R.F.; Meiler, F.; Zandomeneghi, G.; Neumann, D.; Widmer, H.R.; Meier, B.H.; Epand, R.M.; Saks, V.; Wallimann, T.; et al. Phosphocreatine Interacts with Phospholipids, Affects Membrane Properties and Exerts Membrane-Protective Effects. PLoS ONE 2012, 7, e43178.
- Sestili, P.; Ambrogini, P.; Barbieri, E.; Sartini, S.; Fimognari, C.; Calcabrini, C.; Diaz, A.R.; Guescini, M.; Polidori, E.; Luchetti, F.; et al. New insights into the trophic and cytoprotective effects of creatine in in vitro and in vivo models of cell maturation. Amino Acids 2016, 48, 1897–1911.
- Zhou, Y.; Xu, H.; Ding, Y.; Lu, Q.; Zou, M.H.; Song, P. AMPKα1 deletion in fibroblasts promotes tumorigenesis in athymic nude mice by p52-mediated elevation of erythropoietin and CDK2. Oncotarget 2016, 7, 53654–53667.
- Pradeep, S.; Huang, J.; Mora, E.M.; Nick, A.M.; Cho, M.S.; Wu, S.Y.; Noh, K.; Pecot, C.V.; Rupaimoole, R.; Stein, M.A.; et al. Erythropoietin Stimulates Tumor Growth via EphB4. Cancer Cell 2015, 28, 610–622.




