
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Bibhuti B Das | + 1318 word(s) | 1318 | 2021-08-12 10:09:57 | | | |
| 2 | Catherine Yang | -30 word(s) | 1288 | 2021-08-17 02:45:37 | | |
Video Upload Options
The development of the mRNA vaccine against SARS-CoV-2 is unprecedented in the history of Vaccinology. The prototypes of the mRNA vaccine are BNT162b2 (Pfizer-BioNTech) and mRNA-1273 (Moderna), which gained widespread use to prevent severe SARS-CoV-2 infection. As per CDC guidelines, these vaccines have undergone extensive testing and trials, and myocarditis and pericarditis occurred after the mRNA vaccines were not reported in trials.
1. Introduction
The mRNA vaccines ((BNT162b2, Pfizer-BionTech, Pfizer, Inc.; Philadelphia, PA, USA) and Moderna (mRNA-1273, ModernaTX, Inc.; Cambridge, MA, USA)) demonstrated excellent safety and clinical efficacy profiles in clinical trials in adults in less than one year from the identification of the virus which is unprecedented in the history of vaccinology [1][2]. The mRNA vaccine used in the European Union is Comirnaty, which has the same mRNA, BNT162b2- as the Pfizer-BionTech, and is manufactured according to the same processes and procedures. The only difference is in their label. The mRNA COVID-19 vaccine Moderna is also known as Spikevax, which is used in the European Union. The Food and Drug Administration (FDA) issued emergency use authorization (EUA) on 11 December 2020, for Pfizer-BioNTech COVID-19 vaccine in persons aged > 16 years [3]. The European Medicine Agency (EMA) approved Comirnaty in people from 16 years of age on 21 December 2020. On 10 May 2021, the FDA expanded EUA to use the Pfizer mRNA COVID-19 vaccine for children 12–15 years [4]. The Center for Disease Control and Prevention (CDC) subsequently recommended on 12 May 2021, that persons 12 years and older should get a COVID-19 vaccine.
Post-vaccination myocarditis has been reported as early as 1957 after smallpox vaccination [5]. Analysis of the Vaccine Adverse Event Reporting System (VAERS) data between 2011 and 2015, where a total of 357,188 reports were reviewed and found 199 cases of myocarditis and pericarditis. Only the smallpox vaccine emerged with an expectedly strong correlation with myocarditis and pericarditis [6]. Previous findings should be interpreted with caution regarding limitations affecting the voluntary reporting system and may be underreported. Conversely, in the current era of heightened surveillance by the CDC’s vaccine safety data (VSD) working group and the Vaccine Related Biological Products Advisory Committee (VRBPAC) on immunization practices after COVID-19, and post-marketing surveillance by the vaccine producing companies in the setting of conditional marketing authorization, the reporting of probable myocarditis and pericarditis cases is significantly higher. Since April 2021, increased cases of myocarditis and pericarditis have been reported in the United States after mRNA COVID-19 vaccination, particularly in adolescents and young adults [7][8][9][10][11][12].
The American Academy of Pediatrics (AAP) and the American Heart Association (AHA) have endorsed CDC recommendations and reiterated the potential benefits of COVID-19 vaccination, which outweighs rare myocarditis or pericarditis risks and recommend the vaccination for anyone 12 years of age and older [13][14]. Very little published data on the incidence of mRNA vaccine-associated myocarditis and pericarditis exist except those reported in the media. We performed a systematic search of electronic databases (PubMed, Scopus, medRxiv and bioRxV) with a goal to publish the results in the context of expanding the vaccine target population using the terms “mRNA vaccine complications”, “heart inflammation with COVID-19 vaccine”, “impact of COVID-19 vaccine in children and young adults”, “myocarditis after COVID-19 vaccination” and “pericarditis after COVID-19 vaccination”, and “myopericarditis after COVID-19 vaccination”.
2. Diagnosis and Management
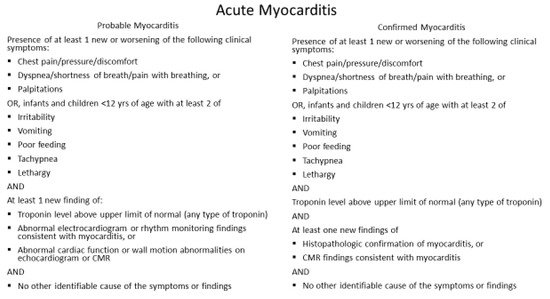

References
- Polack, F.P.; Thomas, S.J.; Kitchin, N.; Absalon, J.; Gurtman, A.; Lockhart, S.; Perez, J.L.; Marc, G.P.; Moreira, E.D.; Zerbini, C.; et al. Safety and Efficacy of the BNT162b2 mRNA COVID-19 Vaccine. N. Engl. J. Med. 2020, 383, 2603–2615.
- Baden, L.R.; El Sahly, H.M.; Essink, B.; Kotloff, K.; Frey, S.; Novak, R.; Diemert, D.; Spector, S.A.; Rouphael, N.; Creech, C.B.; et al. Efficacy and Safety of the mRNA-1273 SARS-CoV-2 Vaccine. N. Engl. J. Med. 2021, 384, 403–416.
- Oliver, S.E.; Gargano, J.W.; Marin, M.; Wallace, M.; Curran, K.G.; Chamberland, M.; McClung, N.; Campos-Outcalt, D.; Morgan, R.; Mbaeyi, S.; et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Pfizer-BioNTech COVID-19 vaccine—United States, December 2020. MMWR Morb. Mortal Wkly Rep. 2020, 69, 1922–1924.
- Wallace, M.; Woodworth, K.R.; Gargano, J.W.; Scobie, H.M.; Blain, A.E.; Moulia, D.; Chamberland, M.; Reisman, N.; Hadler, S.C.; MacNeil, J.R.; et al. The Advisory Committee on Immunization Practices’ Interim Recommendation for using Pfizer-BioNTech COVID-19 Vaccine in Adolescents Aged 12–15 Years—United States, May 2021. MMWR 2021, 70, 749–752.
- Dalgaard, J.B. Fatal myocarditis following smallpox vaccination. Am. Heart J. 1957, 54, 156–157.
- Mei, R.; Raschi, E.; Forcesi, E.; Diemberger, I.; De Ponti, F.; Poluzzi, E. Myocarditis and pericarditis after immunization: Gaining insights through the vaccine adverse event reporting system. Int. J. Cardiol. 2018, 273, 183–186.
- Kime, P. Pentagon Tracking 14 cases of Heart Inflammation in Troops after COVID-19 Shots. Published 26 April 2021. Available online: https://www.military.com/daily-news/2021/04/26/pentagon-tracking-14-cases-of-heart-inflammation-troops-after-covid-19-shots.html (accessed on 16 May 2021).
- Ammirati, E.; Cavalotti, C.; Milazzo, A.; Pedrotti, P.; Soriano, F. Temporal relation between second dose BNT162b2 mRNA COVID-19 vaccine and cardiac involvement in a patient with previous SARS-CoV-2 infection. IJC Heart Vasc. 2021, 34, 100774.
- Marshall, M.; Ferguson, I.D.; Lewis, P.; Jaggi, P.; Gagliardo, C.; Collins, J.S.; Shaughnessya, R.; Carona, R.; Fuss, C.; Corbin, K.J.E.; et al. Symptomatic acute myocarditis in seven adolescents following Pfizer-BioNTech COVID-19 vaccination. Pediatrics 2021.
- Snapiri, O.; Vanziger, C.R.; Chairman, N.; Weissbach, A.; Lowenthal, A.; Ayalon, I.; Adam, D.; Yarden-Bilavsky, H.; Bilavsky, E. Transient cardiac injury in adolescents receiving the BNT162b2 mRNA COVID-19 vaccine. Pediatr. Infect. Dis. J. 2021.
- Rosner, C.M.; Genovese, L.; Tehrani, B.; Atkins, M.; Bakhshi, H.; Chaudhri, S.; Damluji, A.A.; de Lemos, J.A.; Desai, S.S.; Emaminia, A.; et al. Myocarditis temporarily associated with COVID-19 Vaccination. Circulation 2021, in press.
- Larson, K.F.; Ammirati, E.; Adler, E.D.; Cooper, L.T.; Hong, K.N.; Saponara, G.; Couri, D.; Cereda, A.; Procopio, A.; Cavalotti, C.; et al. Myocarditis after BNT1622b2 and mRNA Vaccination. Circulation 2021, in press.
- AAP News. Available online: https://www.aappublications.org/news/2021/06/10/covid-vaccine-myocarditis-rates-061021 (accessed on 18 June 2021).
- AHA Statement on 23 May 2021. Available online: https://newsroom.heart.org/news/covid-19-vaccine-benefits-still-outweigh-risks-despite-possible-rare-heart-complications (accessed on 18 June 2021).
- Tschöpe, C.; Ammirati, E.; Bozkurt, B.; Caforio, A.L.P.; Cooper, L.T.; Felix, S.B.; Hare, J.M.; Heidecker, B.; Heymans, S.; Hübner, N.; et al. Myocarditis and inflammatory cardiomyopathy: Current evidence and future directions. Nat. Rev. Cardiol. 2021, 18, 169–193.
- Das, B.B. Role of endomyocardial biopsy for children presenting with acute systolic heart failure. Pediatr. Cardiol. 2014, 35, 191–196.
- Law, Y.M.; Lal, A.K.; Chen, S.; Cihakova, D.; Cooper, L.T.; Deshpande, S.; Godown, J.; Grosse-Wortmann, L.; Robinson, J.D.; Towbin, J.A. Diagnosis and management of myocarditis in Children. A Scinetific Statement from the American Heart Association. Circulation 2021, 144.
- Radunski, U.K.; Lund, G.K.; Sharing, D.; Bohnen, S.; Stehning, S.; Schnackenburg, B.; Avanesov, M.; Tahir, E.; Adam, G.; Blankenberg, S.; et al. T1, and T2 mapping cardiovascular resonance imaging technique reveal unapparent myocardial injury in patients with myocarditis. Clin. Res. Cardiol. 2017, 106, 10–17.
- Ammirati, E.; Frigerio, M.; Adler, E.D.; Basso, C.; Birnie, D.H.; Brambatti, M.; Friedrich, M.G.; Klingel, K.; Lehtonen, J.; Moslehi, J.J.; et al. Management of Acute Myocarditis and Chronic Inflammatory Cardiomyopathy: An Expert Consensus Document. Circ. Heart Fail. 2020, 13, e007405.
- AAP Recommendations in “COVID-19 Interim Guidance: Return to Sports”. Available online: https://www.aappublications.org/news/2020/12/04/sportsguidance120420 (accessed on 15 June 2021).
- Maron, B.J.; Udelson, J.E.; Bonow, R.O.; Nishimura Raackerman, M.J.; Estes, N.M., III. Eligibility and disqualification recommendations for competitive athletes with cardiovascular abnormalities: A scientific statement from the American Heart Association and American College of Cardiology. Circulation 2015, 132, e273–e280.




