
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Christina Tang | + 4687 word(s) | 4687 | 2021-05-21 11:47:20 | | | |
| 2 | Peter Tang | Meta information modification | 4687 | 2021-05-25 05:05:15 | | |
Video Upload Options
Treatment of ovarian cancer is challenging due to late stage diagnosis, acquired drug resistance mechanisms, and systemic toxicity of chemotherapeutic agents. Combination chemotherapy has the potential to enhance treatment efficacy by activation of multiple downstream pathways to overcome drug resistance and reducing required dosages. Sequence of delivery and the dosing schedule can further enhance treatment efficacy. Formulation of drug combinations into nanoparticles can further enhance treatment efficacy. Due to their versatility, polymer-based nanoparticles are an especially promising tool for clinical translation of combination therapies with tunable dosing schedules.
1. Introduction
2. Nanoparticle Formulation of Drug Combinations
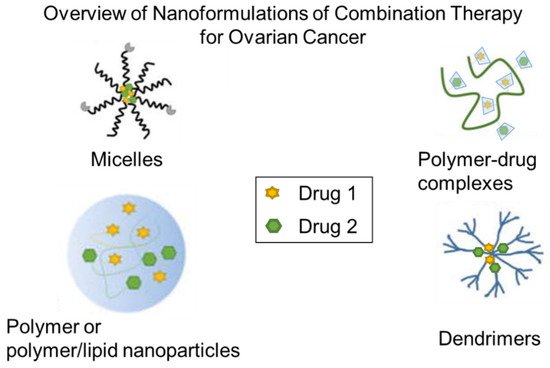
2.1. Polymer Nanoparticles and Micelles
2.2. Platinum Based Combinations
|
Nanoparticle |
Drugs |
In Vitro |
Key Results In Vitro |
In Vivo |
Key Results In Vivo |
Source |
|---|---|---|---|---|---|---|
|
Folic acid (FA)-PEGylated calix[4]arene nanoparticle |
carboplatin/paclitaxel |
SKOV-3, HO-8910 |
Encapsulation increased the cell mortality rate of SKOV-3 by 2.5-fold; conjugation further increased the cell mortality rate by 3-fold in vitro |
SKOV-3 xenograft (armpit) treated once every other day via intratumor injection |
Reduced tumor volume compared to the free drug |
[31] |
|
Folic acid (FA)-PEGylated-polypeptide-nanogels |
cisplatin/paclitaxel |
A2780/Luc |
2-fold decrease in IC50 after 24 h using FA |
A2780/Luc xenograft (IP) treated once every 4 days via tail vein injection |
Increased cisplatin accumulation in tumor tissue; improved tumor inhibition and survival compared to single drug formulations |
[33] |
|
Poly(2-oxazoline) micelles |
cisplatin/paclitaxel |
A2780 and A2780cis (platinum resistant) |
40:3 ratios of PTX to C6CP resulted in combination indexes less than 0.2 in A2780CisR cells; CI highly dependent on the drug ratio |
A2780/Luc xenograft (right flank) treated once every 4 days via tail vein injection |
reduced tumor growth, increased survival compared to single drug loaded micelles |
[34] |
|
PEG-poly-(L-lysine) |
Cisplatin/doxorubicin |
A2780/A2780DDP (platinum resistant) |
2.5-to 3.3-fold decrease in IC50 of cisplatin, CI 0.21–55 |
- |
- |
[35] |
|
PLGA-PEG |
cisplatin/paclitaxel |
SKOV-3 |
The co-loaded formulation was significantly more potent than prodrug stabilizer (3600-fold decrease in IC50) |
- |
- |
[32] |
|
PLGA-PEG NPs |
cisplatin/wortmannin (DNA repair inhibitor) |
A2780 and A2780cis (platinum resistant) |
synergistically enhanced efficacy of A2780cis (CI ~ 0.04) with a 21-fold decrease in IC50, but were additive in A2780 cells (CI ~ 0.9–1.2) |
A2780 and A2780cis xenograft (right flank) treated once by trail vein injection |
reduced tumor growth rates compared to the free drugs; Increased cisplatin localization in the tumor |
[36] |
|
Hyaluronic acid micelles |
cisplatin/EGCG |
SKOV-3 |
Slight decrease in cell viability compared to single drug loaded NPs. Intracellular uptake was possible facilitating Pt accumulation. |
SKOV-3-Luc xenograft (IP) treated once a week for 3 weeks by IP injection |
increased the Pt accumulation in the tumor and reduced tumor volume as well as increased survival rate compared to free cisplatin |
[37] |
|
PCL-based triblock co-polymer micelle carriers |
oxoplatin/curcumin |
A2780 |
strong synergistic interaction (CI ~ 0.3) |
- |
- |
[38] |
|
poly(norbornene)-co-poly(ethylene glycol) |
Cisplatin/doxorubicin camptothecin |
OVCAR-3 |
The triple drug co-loaded formulation was more potent than the single drug (cisplatin) or two drug loaded combination as indicated by the decrease in IC50 (up to 11-fold) |
- |
- |
[39] |
2.3. Taxane Based Combinations
|
Nanoparticle |
Drugs |
In Vitro |
Key Results In Vitro |
In Vivo |
Key Results In Vivo |
Source |
|---|---|---|---|---|---|---|
|
Cyclodextrin nanocarries |
paclitaxel/curcumin |
A2780, SKOV-3 |
Syngeistic (CI ~ 0.65) when compared to free drugs (CI ~ 1) |
- |
- |
[43] |
|
PEI-g-stearic acid micelles coated with hyaluronic acid |
paclitaxel/curcumin |
SKOV-3 and SKOV-3-TR30 (multi-drug resistant) |
17.3-fold lower IC50 in SKOV-3 cells and 115-fold lower in SKOV-3-TR30 cells compared to free paclitaxel |
every other day for 5 times via tail vein injection |
Reduces tumor volume compared to free drug (t-test, 5%) and PTX only nanoparticles (t-test 10%) |
[44] |
|
PEO-PCL nanoparticles |
paclitaxel/tamoxifen |
SKOV-3, SKOV-3TR |
10-fold decrease in IC50 of paclitaxel (SKOV-3), CI ~ 0.4 and (CI ~ 0.7) in SKOV-3TR |
SKOV-3, SKOV-3TR xenograft (flank) treated at day 1 and day 24 through tail vein injection |
suppressed tumor growth, lowering systemic toxicity, tamoxifen enhanced cytotoxicity of paclitaxel |
[45] |
|
mPEG-PCL polymer micelles |
paclitaxel/tacrolimus (FK506) |
A2780/T (PTX resistant) |
5.3-fold decrease in IC50 compared to PTX only micelles; |
- |
- |
[46] |
|
Chitosan/alginate nanocapsules |
paclitaxel/lapatnib |
OVCAR-3 |
Increased cytotoxicity compared to PTX |
- |
- |
[47] |
|
PS-PEG nanoparticles |
paclitaxel/lapatinib |
OVCA-432 |
1500-fold decrease in IC compared to free drug; co-loaded formulation 4.4 fold decrease in IC50 concentration compared to PTX only formulation; CI 0.23; co-loaded formulation more potent than two single drug loaded nanoparticle (CI 0.40) |
- |
- |
[48] |
|
EGFR-peptide-PCL nanoparticles |
paclitaxel/lonidamine |
SKOV-3, SKOV-3TR, OVCAR-5 (MDR) |
2-fold decrease in IC50 of paclitaxel in OVCAR-5 cells under hypoxic conditions (no change in IC50 under noroxative conditions or other cell types) |
- |
- |
[49] |
|
PEG-b-PCL micelles |
paclitaxel/cyclopamine/gossypol |
SKOV-3, ES-2 |
2D model: no increased potency compared to paclitaxel micelles; 3D model: disaggregation of the spheroid |
ES-2, SKOV-3 xenografts via IP injection once a week for 3 weeks via IP injection |
significantly reduced tumor volume and extended survival time compared to free paclitaxel |
[50] |
2.4. Other Drug Combinations
|
Nanoparticle |
Drugs |
In Vitro |
Key Results In Vitro |
In Vivo |
Key Results In Vivo | Source |
|---|---|---|---|---|---|---|
|
Folate-PEG-PLGAnanoparticles |
docetaxel/gemcitabine |
SKOV-3 |
3.59-fold drop in the IC50 and improve cytotoxicity in SKOV-3 cells as compared to free drug combination |
SKOV-3 xenograft treated every 2 days for 3 weeks via tail vein injections |
Reduced tumor volume and rate of tumor growth compared to free drug combination with no organ toxicity | [51] |
|
mPEG-PLA polymer micelles |
doxorubicin/gemcitabine |
SKOV-3 |
drug internalization via endocytosis |
- |
- | [52] |
|
mPEG-PLA nanoparticles |
doxorubicin/verapamil |
A2780, SKOV-3, A2780/DOX, and SKOV-3/DOXR |
micelles increased drug accumulation and enhanced apoptosis |
A2780/DOXR and SKOV-3/DOXR xenograft treated every 3 days for 2 weeks via tail vein injection |
inhibited tumor growth and increased survival time compared to free doxobucin with reduced side effects | [53] |
|
mPEG-b-poly[N-2-hydroxyethyl)-aspartamide]/phenylboronic acid |
Doxorubicin/irinotecan |
SKOV-3 |
Micelles increase IC50 compared to free drug; co-loaded micelles synergistic compared to single drug loaded (CI 0.3) |
- |
- | [54] |
|
Pluronic® F-127 micelles |
resveratrol co-loaded with quercetin or curcumin in NPs with free adriamycrin |
ES2-Luc, A2780, and A2780ADR, ES2-Luc |
Up to 10 –fold reduction in IC50 and synergistic (CI < 0.5) in A2780 and A2780ADR cells |
ES2-Luc and A2780ADR xenografts treated with weekly injections for 4 weeks via tail vein injection |
Significant tumor reduction and cardioprotective effect compared to ADR alone | [55] |
|
mPEG-b-PLA micelles |
Chetomin/Everolimus |
ES-2, OVCAR-3, TOV-21G |
Combination index for co-loaded micelle was <1 compared to single drug loaded micelles |
ES-2 treated with weekly injections for 3 weeks via tail vein injection |
Significant tumor reduction compared to empty micelles and saline control | [56] |
|
Amphiphilic drug-drug conjugate nanopartpices |
floxuridine-chlorambucil |
OVCAR-3 |
Combination index was nanodrugs~0.3 compared to~0.7 for the free drug |
- |
- | [57] |
2.5. Lipid Nanoparticles
|
Nanoparticle |
Drugs |
In Vitro |
Key Results In Vitro |
In Vivo |
Key Results In Vivo |
Source |
|---|---|---|---|---|---|---|
|
Polyelectrolyte coated liposome |
Cisplatin/olaparib or talazoparib |
OVCAR-8 and COV362 |
enhanced potency (reduced IC50) compared to free drugs |
OVCAR-8 xenografts treated by tail vein injection once a week |
Reduced tumor burden and metastasis as well as increasing survival |
[59] |
|
PEGylated lipid nanoemulsion |
paclitaxel/curcumin |
SKOV-3, SKOV-3TR (drug resistant) |
enhanced cytotoxicity and increased apoptosis, slightly synergistic (CI = 0.93) in SKOV-3 and additive in SKOV-3TR compared to free drugs |
- |
- |
[62] |
|
PEG stabilized microemulsion |
brucea oil/tripterine |
SKOV-3 |
CI = 0.90 at an 20:1 w:w ratio of brucea oil to tripterine |
- |
- |
[63] |
|
iRGD peptide Lipid-polymer hybrid nanoparticles |
paclitaxel/tetrandrine |
A2780/PTX cells (paclitaxel resistant) |
CI 0.49–0.64 depending on drug ratios; increased intracellular paclitaxel accumulation apoptosis when co-loaded |
- |
- |
[64] |
|
Lipid-templated polymer-caged nanobins |
cisplatin/doxorubicin |
OVCAR-3 |
enhanced cytotoxicity compared to both free drug and single-drug nanobins; CI between 0.27 and 0.67 depending on drug ratio compared |
- |
- |
[65] |
|
DSPE-PEG micelles |
paclitaxel/tanespimycin (17-AAG) |
- |
- |
SKOV-3 xenograft (flank) with sequential delivery of paclitaxel (free or NPs) once a week and followed by 17-AAG (free or NPs) 3 days later for 3 weeks, administed through tail vein injection |
increased tumor accumulation by 2-fold,~2-fold reduction in tumor mass after 43 days significant tumor growth arrest compared to free drug combinations |
[66] |
|
Core-shell DOPA, DSPE-PEG, and cholesterol nanoparticles |
carboplatin/gemcitabine |
SKOV-3, A2780/CDPP (platinum resistant cells) |
CI~0.5 comparable to free drugs |
SKOV-3, A2780/CDDP (platinum-resistant) xenografts (right flank) injected by IP once every 3 days for a total of 3 injections |
reduced tumor weight by 12-fold compared to free drug combination |
[67] |
|
mPEG-DPPE/calcium phosphate nanoparticle |
triptolide/curcumin |
SKOV-3 |
Higher apoptosis rate compared to free drugs |
SKOV-3 xenografts (upper left axillary fossa) treated twice a week for 24 days via tail vein injection |
Reduced tumor volume compared to free drugs |
[68] |
2.6. Dendrimers
|
Nanoparticle |
Drugs |
In Vitro |
Key Results In Vitro |
In Vivo |
Key Results In Vivo |
Source |
|---|---|---|---|---|---|---|
|
PEG 3-generation telodendrimer micelles |
cisplatin/paclitaxel |
SKOV-3, ES-2 |
Antagonistic at 1:1 ratio; synergistic at 2:1 ratio of cisplatin to paclitaxel (CI = 0.21 for SKOV-3) |
SKOV-3 xenograft (flank) treated 3 times at 4-day intervals via tail vein injection |
highest accumulation in the tumor tissue, decreased tumor volume, increased survival time, and reduced renal toxicity compared to free cisplatin, cisplatin loaded telodendrimers, or paclitaxel loaded dendrimers |
[73] |
|
PLA/PLGA/PEG dendrimers |
cisplatin prodrug/aspirin prodrug |
A2780/CP70 (cisplatin resistant) |
~4-fold decreased IC50 in nanoparticle formulation |
- |
- |
[74] |
|
PEG dendrimers |
Oxaliplatin/curcumin dendrimers |
SKOV-3/OVCAR-3 |
CI 0.855 in SKOV-3/CI 0.708 in OVCAR-3 after 48 h of treatment (IC50) |
- |
- |
[75] |
|
3-generation PEG-PAMAM dendrimers |
paclitaxel/borneol |
A2780/PTX (paclitaxel resistant) |
3-fold lower IC50 value compared to the free drug combination |
A2780/PTX xenograft (back) once every two days for 7 tail vein injections |
decrease in tumor volume, compared with the free drug combination |
[76] |
|
Linear-dendritic telodendrimers |
doxorubicin/bortezomib |
SKOV-3 |
Synergistic effects observed at bortezomib: doxorubicin ratios between 1:1 and 1:10; antagonistic at lower ratios |
SKOV-3 xenograft (flank) treated every 4 days for a total of 3 tail vein injections |
decreased toxicity delayed tumor growth compared to free drugs |
[77] |
References
- Reid, B.M.; Permuth, J.B.; Sellers, T.A. Epidemiology of Ovarian Cancer: A Review. Cancer Biol. Med. 2017, 14, 9–32.
- Deb, B.; Uddin, A.; Chakraborty, S. MiRNAs and Ovarian Cancer: An Overview. J. Cell. Physiol. 2018, 233, 3846–3854.
- Morice, P.; Gouy, S.; Leary, A. Mucinous Ovarian Carcinoma. N. Engl. J. Med. 2019, 380, 1256–1266.
- Miller, E.M.; Samec, T.M.; Alexander-Bryant, A.A. Nanoparticle Delivery Systems to Combat Drug Resistance in Ovarian Cancer. Nanomed. Nanotechnol. Biol. Med. 2021, 31, 102309.
- Barani, M.; Bilal, M.; Sabir, F.; Rahdar, A.; Kyzas, G.Z. Nanotechnology in Ovarian Cancer: Diagnosis and Treatment. Life Sci. 2021, 266, 118914.
- Jayson, G.C.; Kohn, E.C.; Kitchener, H.C.; Ledermann, J.A. Ovarian Cancer. Lancet 2014, 384, 1376–1388.
- Kim, S.; Han, Y.; Kim, S.I.; Kim, H.-S.; Kim, S.J.; Song, Y.S. Tumor Evolution and Chemoresistance in Ovarian Cancer. NPJ Precis. Oncol. 2018, 2, 1–9.
- Ghoneum, A.; Afify, H.; Salih, Z.; Kelly, M.; Said, N. Role of Tumor Microenvironment in Ovarian Cancer Pathobiology. Oncotarget 2018, 9, 22832–22849.
- Azaïs, H.; Estevez, J.P.; Foucher, P.; Kerbage, Y.; Mordon, S.; Collinet, P. Dealing with Microscopic Peritoneal Metastases of Epithelial Ovarian Cancer. A Surgical Challenge. Surg. Oncol. 2017, 26, 46–52.
- Mancini, R.; Modlin, J. Chemotherapy Administration Sequence: A Review of the Literature and Creation of a Sequencing Chart. J. Hematol. Oncol. Pharm. 2011, 1, 17–25.
- Paliwal, R.; Paliwal, S.R.; Kenwat, R. Nanomedicine-Based Multidrug Resistance Reversal Strategies in Cancer Therapy; Academic Press: Cambridge, MA, USA, 2021.
- Brotto, L.; Brundage, M.; Hoskins, P.; Vergote, I.; Cervantes, A.; Casado, H.A.; Poveda, A.; Eisenhauer, E.; Tu, D. Randomized Study of Sequential Cisplatin-Topotecan/Carboplatin-Paclitaxel versus Carboplatin-Paclitaxel: Effects on Quality of Life. Support. Care Cancer 2016, 24, 1241–1249.
- Waltmire, C.N.; Alberts, D.S.; Dorr, R.T. Sequence-Dependent Cytotoxicity of Combination Chemotherapy Using Paclitaxel, Carboplatin and Bleomycin in Human Lung and Ovarian Cancer. Anticancer. Drugs 2001, 12, 595–602.
- Orr, B.; Edwards, R.P. Diagnosis and Treatment of Ovarian Cancer. Hematol. Oncol. Clin. N. Am. 2018, 32, 943–964.
- Rowinsky, E.K.; Citardi, M.J.; Noe, D.A.; Donehower, R.C. Sequence-Dependent Cytotoxic Effects Due to Combinations of Cisplatin and the Antimicrotubule Agents Taxol and Vincristine. J. Cancer Res. Clin. Oncol. 1993, 119, 727–733.
- Huynh, N.; Wang, S.; King-Jones, K. Spatial and Temporal Control of Gene Manipulation in Drosophila via Drug-Activated Cas9 Nucleases. Insect Biochem. Mol. Biol. 2020, 120, 103336.
- Freimund, A.E.; Beach, J.A.; Christie, E.L.; Bowtell, D.D.L. Mechanisms of Drug Resistance in High-Grade Serous Ovarian Cancer. Hematol. Oncol. Clin. N. Am. 2018, 32, 983–996.
- Tang, C.; Levit, S.; Zeevi, M.; Vasey, C.; Fromen, C. Polymer Colloids Enable Medical Applications. In Polymer Colloids: Formation, Characterization and Applications; Royal Society of Chemistry: London, UK, 2020; pp. 358–398.
- Correa, S.; Boehnke, N.; Barberio, A.E.; Deiss-Yehiely, E.; Shi, A.; Oberlton, B.; Smith, S.G.; Zervantonakis, I.; Dreaden, E.C.; Hammond, P.T. Tuning Nanoparticle Interactions with Ovarian Cancer through Layer-by-Layer Modification of Surface Chemistry. ACS Nano 2020, 14, 2224–2237.
- Ferrari, R.; Sponchioni, M.; Morbidelli, M.; Moscatelli, D. Polymer Nanoparticles for the Intravenous Delivery of Anticancer Drugs: The Checkpoints on the Road from the Synthesis to Clinical Translation. Nanoscale 2018, 10, 22701–22719.
- Ghitman, J.; Biru, E.I.; Stan, R.; Iovu, H. Review of Hybrid PLGA Nanoparticles: Future of Smart Drug Delivery and Theranostics Medicine. Mater. Des. 2020, 193, 108805.
- Prajapati, S.K.; Jain, A.; Jain, A.; Jain, S. Biodegradable Polymers and Constructs: A Novel Approach in Drug Delivery. Eur. Polym. J. 2019, 120, 109191.
- Rajora, A.K.; Ravishankar, D.; Zhang, H.; Rosenholm, J.M. Recent Advances and Impact of Chemotherapeutic and Antiangiogenic Nanoformulations for Combination Cancer Therapy. Pharmaceutics 2020, 12, 592.
- Li, Y.; Gao, Y.; Zhang, X.; Guo, H.; Gao, H. Nanoparticles in Precision Medicine for Ovarian Cancer: From Chemotherapy to Immunotherapy. Int. J. Pharm. 2020, 591, 119986.
- Gurunathan, S.; Kang, M.H.; Qasim, M.; Kim, J.H. Nanoparticle-Mediated Combination Therapy: Two-in-One Approach for Cancer. Int. J. Mol. Sci. 2018, 19, 3264.
- Yoon, M.S.; Lee, Y.J.; Shin, H.J.; Park, C.W.; Han, S.B.; Jung, J.K.; Kim, J.S.; Shin, D.H. Recent Advances and Challenges in Controlling the Spatiotemporal Release of Combinatorial Anticancer Drugs from Nanoparticles. Pharmaceutics 2020, 12, 1156.
- Shim, G.; Kim, M.G.; Kim, D.; Park, J.Y.; Oh, Y.K. Nanoformulation-Based Sequential Combination Cancer Therapy. Adv. Drug Deliv. Rev. 2017, 115, 57–81.
- Taghipour-Sabzevar, V.; Sharifi, T.; Moghaddam, M.M. Polymeric Nanoparticles as Carrier for Targeted and Controlled Delivery of Anticancer Agents. Ther. Deliv. 2019, 10, 527–550.
- Pan, J.; Rostamizadeh, K.; Filipczak, N.; Torchilin, V.P. Polymeric Co-Delivery Systems in Cancer Treatment: An Overview on Component Drugs’ Dosage Ratio Effect. Molecules 2019, 24, 1035.
- Sur, S.; Rathore, A.; Dave, V.; Reddy, K.R.; Chouhan, R.S.; Sadhu, V. Recent Developments in Functionalized Polymer Nanoparticles for Efficient Drug Delivery System. Nano-Struct. Nano-Objects 2019, 20, 100397.
- Mo, J.; Wang, L.; Huang, X.; Lu, B.; Zou, C.; Wei, L.; Chu, J.; Eggers, P.K.; Chen, S.; Raston, C.L.; et al. Multifunctional Nanoparticles for Co-Delivery of Paclitaxel and Carboplatin against Ovarian Cancer by Inactivating the JMJD3-HER2 Axis. Nanoscale 2017, 9, 13142–13152.
- Shen, W.; Chen, X.; Luan, J.; Wang, D.; Yu, L.; Ding, J. Sustained Codelivery of Cisplatin and Paclitaxel via an Injectable Prodrug Hydrogel for Ovarian Cancer Treatment. ACS Appl. Mater. Interfaces 2017, 9, 40031–40046.
- Desale, S.S.; Soni, K.S.; Romanova, S.; Cohen, S.M.; Bronich, T.K. Targeted Delivery of Platinum-Taxane Combination Therapy in Ovarian Cancer. J. Control. Release 2015, 220, 651–659.
- Wan, X.; Beaudoin, J.J.; Vinod, N.; Min, Y.; Makita, N.; Bludau, H.; Jordan, R.; Wang, A.; Sokolsky, M.; Kabanov, A.V. Co-Delivery of Paclitaxel and Cisplatin in Poly(2-Oxazoline) Polymeric Micelles: Implications for Drug Loading, Release, Pharmacokinetics and Outcome of Ovarian and Breast Cancer Treatments. Biomaterials 2019, 192, 1–14.
- Zhang, G.; Zhu, Y.; Wang, Y.; Wei, D.; Wu, Y.; Zheng, L.; Bai, H.; Xiao, H.; Zhang, Z. PH/Redox Sensitive Nanoparticles with Platinum(Iv) Prodrugs and Doxorubicin Enhance Chemotherapy in Ovarian Cancer. RSC Adv. 2019, 9, 20513–20517.
- Zhang, M.; Hagan, C.T.; Min, Y.; Foley, H.; Tian, X.; Yang, F.; Mi, Y.; Au, K.M.; Medik, Y.; Roche, K.; et al. Nanoparticle Co-Delivery of Wortmannin and Cisplatin Synergistically Enhances Chemoradiotherapy and Reverses Platinum Resistance in Ovarian Cancer Models. Biomaterials 2018, 169, 1–10.
- Bae, K.H.; Tan, S.; Yamashita, A.; Ang, W.X.; Gao, S.J.; Wang, S.; Chung, J.E.; Kurisawa, M. Hyaluronic Acid-Green Tea Catechin Micellar Nanocomplexes: Fail-Safe Cisplatin Nanomedicine for the Treatment of Ovarian Cancer without off-Target Toxicity. Biomaterials 2017, 148, 41–53.
- Scarano, W.; De Souza, P.; Stenzel, M.H. Dual-Drug Delivery of Curcumin and Platinum Drugs in Polymeric Micelles Enhances the Synergistic Effects: A Double Act for the Treatment of Multidrug-Resistant Cancer. Biomater. Sci. 2015, 3, 163–174.
- Liao, L.; Liu, J.; Dreaden, E.C.; Morton, S.W.; Shopsowitz, K.E.; Hammond, P.T.; Johnson, J.A. A Convergent Synthetic Platform for Single-Nanoparticle Combination Cancer Therapy: Ratiometric Loading and Controlled Release of Cisplatin, Doxorubicin, and Camptothecin. J. Am. Chem. Soc. 2014, 136, 5896–5899.
- Alven, S.; Aderibigbe, B.A. Efficacy of Polymer-Based Nanocarriers for Co-Delivery of Curcumin and Selected Anticancer Drugs. Nanomaterials 2020, 10, 1556.
- Gera, M.; Sharma, N.; Ghosh, M.; Huynh, D.L.; Lee, S.J.; Min, T.; Kwon, T.; Jeong, D.K. Nanoformulations of Curcumin: An Emerging Paradigm for Improved Remedial Application. Oncotarget 2017, 8, 66680–66698.
- Pourhanifeh, M.H.; Darvish, M.; Tabatabaeian, J.; Fard, M.R.; Mottaghi, R.; Azadchehr, M.J.; Jahanshahi, M.; Sahebkar, A.; Mirzaei, H. Therapeutic Role of Curcumin and Its Novel Formulations in Gynecological Cancers. J. Ovarian Res. 2020, 13, 1–16.
- Boztas, A.O.; Karakuzu, O.; Galante, G.; Ugur, Z.; Kocabas, F.; Altuntas, C.Z.; Yazaydin, A.O. Synergistic Interaction of Paclitaxel and Curcumin with Cyclodextrin Polymer Complexation in Human Cancer Cells. Mol. Pharm. 2013, 10, 2676–2683.
- Zhao, M.D.; Li, J.Q.; Chen, F.Y.; Dong, W.; Wen, L.J.; Fei, W.D.; Zhang, X.; Yang, P.L.; Zhang, X.M.; Zheng, C.H. Co-Delivery of Curcumin and Paclitaxel by “Core-Shell” Targeting Amphiphilic Copolymer to Reverse Resistance in the Treatment of Ovarian Cancer. Int. J. Nanomed. 2019, 14, 9453–9467.
- Devalapally, H.; Duan, Z.; Seiden, M.V.; Amiji, M.M. Modulation of Drug Resistance in Ovarian Adenocarcinoma by Enhancing Intracellular Ceramide Using Tamoxifen-Loaded Biodegradable Polymeric Nanoparticles. Clin. Cancer Res. 2008, 14, 3193–3203.
- Wang, N.; He, T.; Shen, Y.; Song, L.; Li, L.; Yang, X.; Li, X.; Pang, M.; Su, W.; Liu, X.; et al. Paclitaxel and Tacrolimus Coencapsulated Polymeric Micelles That Enhance the Therapeutic Effect of Drug-Resistant Ovarian Cancer. ACS Appl. Mater. Interfaces 2016, 8, 4368–4377.
- Vergara, D.; Bellomo, C.; Zhang, X.; Vergaro, V.; Tinelli, A.; Lorusso, V.; Rinaldi, R.; Lvov, Y.M.; Leporatti, S.; Maffia, M. Lapatinib/Paclitaxel Polyelectrolyte Nanocapsules for Overcoming Multidrug Resistance in Ovarian Cancer. Nanomed. Nanotechnol. Biol. Med. 2012, 8, 891–899.
- Levit, S.L.; Yang, H.; Tang, C. Rapid Self-Assembly of Polymer Nanoparticles for Synergistic Codelivery of Paclitaxel and Lapatinib via Flash Nanoprecipitation. Nanomaterials 2020, 10, 561.
- Milane, L.; Duan, Z.; Amiji, M. Development of EGFR-Targeted Polymer Blend Nanocarriers for Combination Paclitaxel/Lonidamine Delivery to Treat Multi-Drug Resistance in Human Breast and Ovarian Tumor Cells. Mol. Pharm. 2011, 8, 185–203.
- Cho, H.; Lai, T.C.; Kwon, G.S. Poly(Ethylene Glycol)-Block-Poly(ε-Caprolactone) Micelles for Combination Drug Delivery: Evaluation of Paclitaxel, Cyclopamine and Gossypol in Intraperitoneal Xenograft Models of Ovarian Cancer. J. Control. Release 2013, 166, 1–9.
- Li, S.; Li, X.; Ding, J.; Han, L.; Guo, X. Anti-Tumor Efficacy of Folate Modified PLGA-Based Nanoparticles for the Co-Delivery of Drugs in Ovarian Cancer. Drug Des. Devel. Ther. 2019, 13, 1271–1280.
- Liu, D.; Chen, Y.; Feng, X.; Deng, M.; Xie, G.; Wang, J.; Zhang, L.; Liu, Q.; Yuan, P. Micellar Nanoparticles Loaded with Gemcitabine and Doxorubicin Showed Synergistic Effect. Colloids Surfaces B Biointerfaces 2014, 113, 158–168.
- Zheng, W.; Li, M.; Lin, Y.; Zhan, X. Encapsulation of Verapamil and Doxorubicin by MPEG-PLA to Reverse Drug Resistance in Ovarian Cancer. Biomed. Pharmacother. 2018, 108, 565–573.
- Wu, Y.; Lv, S.; Li, Y.; He, H.; Ji, Y.; Zheng, M.; Liu, Y.; Yin, L. Co-Delivery of Dual Chemo-Drugs with Precisely Controlled, High Drug Loading Polymeric Micelles for Synergistic Anti-Cancer Therapy. Biomater. Sci. 2020, 8, 949–959.
- Al Fatease, A.; Shah, V.; Nguyen, D.X.; Cote, B.; LeBlanc, N.; Rao, D.A.; Alani, A.W.G. Chemosensitization and Mitigation of Adriamycin-Induced Cardiotoxicity Using Combinational Polymeric Micelles for Co-Delivery of Quercetin/Resveratrol and Resveratrol/Curcumin in Ovarian Cancer. Nanomed. Nanotechnol. Biol. Med. 2019, 19, 39–48.
- Doddapaneni, B.S.; AL-Fatease, A.M.; Rao, D.A.; Alani, A.W.G. Dual-Drug Loaded Micelle for Combinatorial Therapy Targeting HIF and MTOR Signaling Pathways for Ovarian Cancer Treatment. J. Control. Release 2019, 307, 272–281.
- Huang, P.; Wang, G.; Wang, Z.; Zhang, C.; Wang, F.; Cui, X.; Guo, S.; Huang, W.; Zhang, R.; Yan, D. Floxuridine-Chlorambucil Conjugate Nanodrugs for Ovarian Cancer Combination Chemotherapy. Colloids Surfaces B Biointerfaces 2020, 194, 111164.
- Pfisterer, J.; Shannon, C.M.; Baumann, K.; Rau, J.; Harter, P.; Joly, F.; Sehouli, J.; Canzler, U.; Schmalfeldt, B.; Dean, A.P.; et al. Bevacizumab and Platinum-Based Combinations for Recurrent Ovarian Cancer: A Randomised, Open-Label, Phase 3 Trial. Lancet Oncol. 2020, 21, 699–709.
- Mensah, L.B.; Morton, S.W.; Li, J.; Xiao, H.; Quadir, M.A.; Elias, K.M.; Penn, E.; Richson, A.K.; Ghoroghchian, P.P.; Liu, J.; et al. Layer-by-layer Nanoparticles for Novel Delivery of Cisplatin and PARP Inhibitors for Platinum-based Drug Resistance Therapy in Ovarian Cancer. Bioeng. Transl. Med. 2019, 4, 1–18.
- Bhise, K.; Kashaw, S.K.; Sau, S.; Iyer, A.K. Nanostructured Lipid Carriers Employing Polyphenols as Promising Anticancer Agents: Quality by Design (QbD) Approach. Int. J. Pharm. 2017, 526, 506–515.
- Bayón-Cordero, L.; Alkorta, I.; Arana, L. Application of Solid Lipid Nanoparticles to Improve the Efficiency of Anticancer Drugs. Nanomaterials 2019, 9, 474.
- Ganta, S.; Amiji, M. Coadministration of Paclitaxel and Curcumin in Nanoemulsion Formulations to Overcome Multidrug Resistance in Tumor Cells. Mol. Pharm. 2009, 6, 928–939.
- Zhao, H.; Chen, M.; Zhao, Z.; Zhu, L.; Yuan, S. A Multicomponent-Based Microemulsion for Boosting Ovarian Cancer Therapy through Dual Modification with Transferrin and SA-R6H4. Drug Deliv. Transl. Res. 2020.
- Zhang, J.; Wang, L.; Fai Chan, H.; Xie, W.; Chen, S.; He, C.; Wang, Y.; Chen, M. Co-Delivery of Paclitaxel and Tetrandrine via IRGD Peptide Conjugated Lipid-Polymer Hybrid Nanoparticles Overcome Multidrug Resistance in Cancer Cells. Sci. Rep. 2017, 7, 1–14.
- Lee, S.M.; O’Halloran, T.V.; Nguyen, S.T. Polymer-Caged Nanobins for Synergistic Cisplatin-Doxorubicin Combination Chemotherapy. J. Am. Chem. Soc. 2010, 132, 17130–17138.
- Katragadda, U.; Fan, W.; Wang, Y.; Teng, Q.; Tan, C. Combined Delivery of Paclitaxel and Tanespimycin via Micellar Nanocarriers: Pharmacokinetics, Efficacy and Metabolomic Analysis. PLoS ONE 2013, 8.
- Poon, C.; Duan, X.; Chan, C.; Han, W.; Lin, W. Nanoscale Coordination Polymers Codeliver Carboplatin and Gemcitabine for Highly Effective Treatment of Platinum-Resistant Ovarian Cancer. Mol. Pharm. 2016, 13, 3665–3675.
- Liu, L.; Xiong, X.; Shen, M.; Ru, D.; Gao, P.; Zhang, X.; Huang, C.; Sun, Y.; Li, H.; Duang, Y. Co-Delivery of Triptolide and Curcumin for Ovarian Caner Targeting Therapy via MPEG-DPPE/CaP Nanoparticle. J. Biomed. Nanotechnol. 2018, 14, 1761–1772.
- Sherje, A.P.; Jadhav, M.; Dravyakar, B.R.; Kadam, D. Dendrimers: A Versatile Nanocarrier for Drug Delivery and Targeting. Int. J. Pharm. 2018, 548, 707–720.
- Kesavan, A.; Pakala, S.B.; Rayala, S.K.; Venkatraman, G. Effective Strategies and Applications of Dendrimers in the Treatment of Ovarian Cancer. Curr. Pharm. Des. 2017, 23, 3099–3104.
- Sharma, A.K.; Gothwal, A.; Kesharwani, P.; Alsaab, H.; Iyer, A.K.; Gupta, U. Dendrimer Nanoarchitectures for Cancer Diagnosis and Anticancer Drug Delivery. Drug Discov. Today 2017, 22, 314–326.
- Dias, A.P.; da Silva Santos, S.; da Silva, J.V.; Parise-Filho, R.; Igne Ferreira, E.; El Seoud, O.; Giarolla, J. Dendrimers in the Context of Nanomedicine. Int. J. Pharm. 2020, 573, 118814.
- Cai, L.; Xu, G.; Shi, C.; Guo, D.; Wang, X.; Luo, J. Telodendrimer Nanocarrier for Co-Delivery of Paclitaxel and Cisplatin: A Synergistic Combination Nanotherapy for Ovarian Cancer Treatment. Biomaterials 2015, 37, 456–468.
- Pathak, R.K.; Dhar, S. A Nanoparticle Cocktail: Temporal Release of Predefined Drug Combinations. J. Am. Chem. Soc. 2015, 137, 8324–8327.
- Seyed Hosseini, E.; Alizadeh Zarei, M.; Babashah, S.; Nakhaei Sistani, R.; Sadeghizadeh, M.; Haddad Kashani, H.; Amini Mahabadi, J.; Izadpanah, F.; Atlasi, M.A.; Nikzad, H. Studies on Combination of Oxaliplatin and Dendrosomal Nanocurcumin on Proliferation, Apoptosis Induction, and Long Non-Coding RNA Expression in Ovarian Cancer Cells. Cell Biol. Toxicol. 2019, 35, 247–266.
- Zou, L.; Wang, D.; Hu, Y.; Fu, C.; Li, W.; Dai, L.; Yang, L.; Zhang, L. Drug Resistance Reversal in Ovarian Cancer Cells of Paclitaxel and Borneol Combination Therapy Mediated by PEG-PAMAM Nanoparticles. Oncotarget 2017, 8, 60453–60468.
- Wang, L.; Shi, C.; Wright, F.A.; Guo, D.; Wang, X.; Wang, D.; Wojcikiewicz, R.J.H.; Luo, J. Multifunctional Telodendrimer Nanocarriers Restore Synergy of Bortezomib and Doxorubicin in Ovarian Cancer Treatment. Cancer Res. 2017, 77, 3293–3305.




