Treatment of ovarian cancer is challenging due to late stage diagnosis, acquired drug resistance mechanisms, and systemic toxicity of chemotherapeutic agents. Combination chemotherapy has the potential to enhance treatment efficacy by activation of multiple downstream pathways to overcome drug resistance and reducing required dosages. Sequence of delivery and the dosing schedule can further enhance treatment efficacy. Formulation of drug combinations into nanoparticles can further enhance treatment efficacy. Due to their versatility, polymer-based nanoparticles are an especially promising tool for clinical translation of combination therapies with tunable dosing schedules.
1. Introduction
Ovarian cancer is primarily diagnosed in advanced stages (stage III and later) when the 5-year survival rate is only 30% [
1,
2,
3,
4,
5]. The standard of care includes surgery to remove the majority of the tumor followed by chemotherapy [
6,
7,
8]. At advanced stages, surgery alone is ineffective at completely removing the cancer as microscopic tumor tissue and macroscopic peritoneal implants form [
9]. For these patients, platinum-based chemotherapy, such as cisplatin, following surgery was the standard of care for over 40 years. Platinum agents induced cytotoxicity by disrupting deoxyribonucleic acid (DNA) synthesis and normal cellular function. In the 1990’s the United States Food and Drug Administration approved paclitaxel (Taxol), an extract from the bark of the Yew tree for cancer treatment [
6].
However, treating ovarian cancer remains challenging with the currently available chemotherapeutic agents [
4,
5]. Combination and sequential treatment schedules of drug combinations is a common practice for managing recurrent ovarian cancer [
4,
5,
10,
11]. For example, one of the common sequences is first-line carboplatin and paclitaxel therapy followed by a re-treatment of both drugs at first relapse. While this treatment has been found to prolong survival and improve quality of life for patients, it is associated with severe systemic toxicity and only a small population of patients exhibit long-term remission [
9].
Due to various factors such as the type of ovarian cancer, genetic mutations, and development of resistance mechanisms, selection of appropriate drug combinations as well as treatment schedules is challenging. Both clinical and pre-clinical studies have investigated sequence schedules of drug combinations to overcome these limitations. The goal is to leverage the downstream effects of the drugs to induce synergistic interactions [
10,
12,
13]. Clinically, sequences of drug combinations are treated on the order of days to weeks [
14]. In contrast, preclinical studies performed in in vitro and in vivo animal studies of sequential drug treatments are often conducted on the order of hours i.e., the same timescale as many drug-activated pathways [
15,
16,
17]. Therefore, direct comparisons between clinical and pre-clinical results are challenging due to a difference in time schedules. Furthermore, while delivering therapeutic dosages on the same time scale as cellular activity can enhance therapeutic efficacy, clinical translation of the protocols is difficult. Two major challenges for clinical translation are patient compliance and increased cytotoxicity. Thus, treating patients with recurrent ovarian cancer and acquired drug resistance mechanisms remains a significant challenge [
4,
5,
9].
Nanoparticle delivery of drug combinations can overcome many of these limitations. Encapsulating drugs into nanocarriers allows for control over the pharmacokinetic properties by controlling drug release as well as increasing circulation half-life and lowering interaction with healthy tissue. Nanoparticle carriers can be designed to accumulate in tumor tissue by utilizing the enhanced permeability and retention (EPR) effect. Additionally, several nanoparticle formulations loaded with chemotherapeutic drugs have been approved by the United States Food and Drug Administration for treating ovarian cancer [
4,
5,
18]. Specifically, polymer nanoparticles offer control over parameters including size and material selection i.e., drug combinations. Therefore, polymer nanoparticles are an especially attractive approach for improving delivery of chemotherapeutic agents [
18,
19]. With appropriate selection of the polymer, nanocarriers can facilitate high loading of hydrophobic drugs and tunable release of the payload. The chemical-physical properties can also be potentially tuned to ensure stability during storage and administration [
20]. Furthermore, use of biodegradable polymers is promising to avoid accumulation of the nanocarriers. Biodegradable polyesters such as poly (lactic acid) (PLA), poly (lactic acid-co-glycolic acid) (PLGA) and poly (ε-caprolactone) are especially promising due to their well-established use [
20]. PLGA is a particularly promising system to tune the degradation rate of the system [
18,
21]. A formulation of paclitaxel using PLA has entered Phase II clinical trials [
20,
22].
2. Nanoparticle Formulation of Drug Combinations
Overall, platinum and taxane based drug combinations have been well studied for treating ovarian cancer. Dosing schedules can be used to improve treatment efficacy. However, it is challenging to translate pre-clinical studies on sequential drug dosing (hours to days) to clinical (days to weeks) studies due to timescale disparity. Furthermore, there are many limitations of free drug formulations. For example, free drug formulation is limited by high systemic toxicity and poorly water-solubility [
29,
32]. Thus, achieving a safe and efficacious drug dose is a significant challenge [
7].
Formulation of these drugs combinations into nanoparticles for ovarian cancer treatment can address many of these challenges [
29,
32]. Incorporation of the drugs into nanoparticles can improve the solubility and reduce toxicity [
18,
69]. Controlled drug release from nanoparticles could facilitate sequential drug delivery to facilitate improved control of the pharmacokinetics [
30,
31,
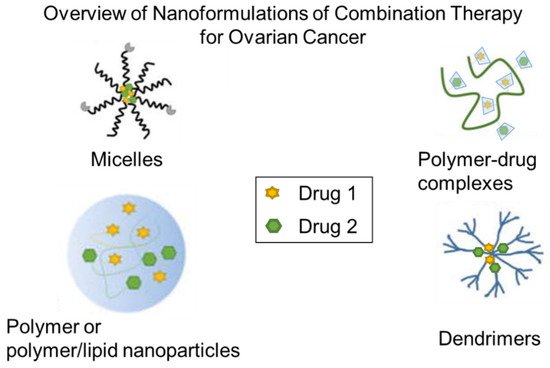
70]. Thus, we review polymer-based nanoparticles (micelles, dendrimers, and solid lipid polymer-based platforms ()) for simultaneous and sequential delivery of platinum- or taxane-based combinations applied to ovarian cancer with an emphasis on quantitative evaluation of nanoparticle formulation on drug synergy.
Figure 1. Schematic overview of the polymer-based nanocarriers used for combination therapy in ovarian cancer included in this review.
2.1. Polymer Nanoparticles and Micelles
Micelles and amphiphilic (hydrophobic core/hydrophilic shell) polymer nanoparticles are advantageous for chemotherapeutic treatment because they can facilitate high drug loading, as well as controlled and stimuli-responsive drug release [
30,
69]. The formulation of polymeric micelles leverages the self-assembly of the amphiphilic polymer. Some of these self-assembly methods include ultrasonication, thin-film dispersion, and nanoprecipitation, where amphiphilic polymers form core-shell structures. Drugs are loaded into micelles either by encapsulation into the core or conjugation to the polymers. The selection of the polymer and ratio of the polymer to core materials affect the surface chemistry, degradation rate, as well as particle size and shape (important for the EPR effect i.e., selective accumulation at the tumor site) [
18,
71]. Thorough reviews of micellar nanoparticles for chemotherapeutic treatment of cancer can be found elsewhere [
70,
72]. In this review, we will focus on nanoparticles encapsulating platinum or taxane agents in combination with small molecules drugs for the treatment of ovarian cancer.
2.2. Platinum Based Combinations
Polymer nanoparticles encapsulating platinum-drug combinations have been investigated for ovarian cancer treatment (summarized in ). This class of drug is commonly combined with paclitaxel for synergistic drug interactions. For example, carboplatin and paclitaxel were co-encapsulated into folic acid targeted PEGylated nanoparticles by click chemistry and sonication. Specifically, azide functionalized p-phosphonated calix[4]arene was used as a surfactant to stabilize paclitaxel and carboplatin nanoparticles formed by sonication. Folic acid-PEG-alkyne was conjugated to the azide functionalized p-phosphonated calix[4]arene nanoparticles using azide-alkyne click chemistry. The resulting particles had a hydrodynamic diameter of 160–185 nm by dynamic light scattering with a polydispersity index between 0.24 and 0.27. The drug ratio was fixed at 1:0.2 paclitaxel: carboplatin. Encapsulating the drugs into nanoparticles increased their potency in SKOV-3 and HO-8910 ovarian cancer cell lines as indicated by the~2-fold decrease in IC50 concentration compared to the free drug in the same ratio. Conjugating the nanoparticle to the folic acid-PEG further increased the potency in vitro. An increase in cell apoptosis by flow cytometry was also observed upon encapsulation. Encapsulation increased the cell mortality rate of SKOV-3 by 2.5-fold; conjugation further increased the cell mortality rate by 3-fold in vitro. The nanoparticle efficacy was also studied in vivo using ovarian cancer xenografts. Briefly, 5–6-week-old BALB/c mic were injected with SKOV-3 tumor cells. When the tumors reached a volume of 200 mm
3, they were treated via an intratumor injection once every other day. The efficacy of the nanoparticle formulations was compared to the free drugs in solution. The conjugated nanoparticles significantly reduced the tumor volume after 18 days compared to the free drug and the nanoparticles without folic acid-PEG [
73].
Co-loaded cisplatin, paclitaxel micelles have also been formulated into injectable hydrogels for ovarian cancer treatment for sustained, localized drug release. Shen et al. covalently linked to diblock copolymers of poly(ethylene glycol) and poly(lactide/glycolide) (mPEG-b-PLGA) copolymers to Pt(IV) prodrug. The prodrug was an amphiphilic stabilizer for the micelle; cisplatin was released upon intracellular reduction. It self-assembled into micelles, encapsulating paclitaxel. Its concentrated solution shows a reversible sol-gel transition as the temperature increases. The formulations were prepared by dissolving the paclitaxel and prodrug stabilizer in acetone, removing the solvent, freeze drying, and redissolving the mixture in water. The in vitro cytotoxicity was evaluated using SKOV-3 cells. The co-loaded formulation was significantly more potent than prodrug stabilizer as indicated by the over 3600-fold decrease in IC50 value. The drug combination was synergistic; the combination index was approximately 0.9 [
74].
Alternative stabilizers such as peptide-based materials have also been considered. For example, cisplatin and paclitaxel were coloaded into polypeptide-based polymeric micelles. Specifically, triblock copolymers of PEG, glutamic acid, and phenylalanine were self-assembled into micelles with a hydrophobic phenylalanine core, intermediate glutamic acid shell, and PEG corona. The intermediate glutamic acid shell was crosslinked with carbodiimide chemistry. Paclitaxel and cis-dichlorodiamminoplatinum (II) were coloaded into the crosslinked micelles; paclitaxel was loaded into the hydrophobic core whereas the cisplatin coordinated with the carboxylic acids of the intermediate glutamic acid shell. Folic acid was conjugated to the drug loaded nanoparticles using PEG spacers (Fmoc-NH-PEG-NH
2, molecular weight 7500 g/mol) via carbodiimide chemistry. The resulting crosslinked micelles were about 90 nm in diameter by dynamic light scattering. The efficacy of the nanoparticles was evaluated in vitro using A2780 ovarian cancer cells. Interestingly, conjugation of folic acid increased the potency of dual drug loaded nanoparticle as indicated by the 2-fold decrease in IC50 after 24 h. The in vivo efficacy was studied using peritoneal carcinomatosis generated by intraperitoneal injection of A2780/Luc cells treated every 4 days via tail vein injections. CA-125 a protein elevated in advanced ovarian cancer and was used as an indicator of tumor progression. Formulating the cisplatin into nanoparticles with paclitaxel reduced CA-125 levels compared to free cisplatin. Conjugating the nanoparticles to folic acid further reduced CA 125-levels. Conjugation to folic acid also significantly increased cisplatin accumulation in tumor tissue compared to formulations without folic acid. Finally, the co-loaded particles demonstrated improved tumor inhibition and survival compared to single drug formulations and the same drug ratio confirming the advantage of delivering the drug combination in a single carrier [
75].
Table 1. Polymer nanocarriers coencapsulating platinum-based agents with other anticancer drugs.
|
Nanoparticle
|
Drugs
|
In Vitro
|
Key Results In Vitro
|
In Vivo
|
Key Results In Vivo
|
Source
|
|
Folic acid (FA)-PEGylated calix[4]arene nanoparticle
|
carboplatin/paclitaxel
|
SKOV-3, HO-8910
|
Encapsulation increased the cell mortality rate of SKOV-3 by 2.5-fold; conjugation further increased the cell mortality rate by 3-fold in vitro
|
SKOV-3 xenograft (armpit) treated once every other day via intratumor injection
|
Reduced tumor volume compared to the free drug
|
[73]
|
|
Folic acid (FA)-PEGylated-polypeptide-nanogels
|
cisplatin/paclitaxel
|
A2780/Luc
|
2-fold decrease in IC50 after 24 h using FA
|
A2780/Luc xenograft (IP) treated once every 4 days via tail vein injection
|
Increased cisplatin accumulation in tumor tissue; improved tumor inhibition and survival compared to single drug formulations
|
[75]
|
|
Poly(2-oxazoline) micelles
|
cisplatin/paclitaxel
|
A2780 and A2780cis (platinum resistant)
|
40:3 ratios of PTX to C6CP resulted in combination indexes less than 0.2 in A2780CisR cells; CI highly dependent on the drug ratio
|
A2780/Luc xenograft (right flank) treated once every 4 days via tail vein injection
|
reduced tumor growth, increased survival compared to single drug loaded micelles
|
[76]
|
|
PEG-poly-(L-lysine)
|
Cisplatin/doxorubicin
|
A2780/A2780DDP (platinum resistant)
|
2.5-to 3.3-fold decrease in IC50 of cisplatin, CI 0.21–55
|
-
|
-
|
[77]
|
|
PLGA-PEG
|
cisplatin/paclitaxel
|
SKOV-3
|
The co-loaded formulation was significantly more potent than prodrug stabilizer (3600-fold decrease in IC50)
|
-
|
-
|
[74]
|
|
PLGA-PEG NPs
|
cisplatin/wortmannin (DNA repair inhibitor)
|
A2780 and A2780cis (platinum resistant)
|
synergistically enhanced efficacy of A2780cis (CI ~ 0.04) with a 21-fold decrease in IC50, but were additive in A2780 cells (CI ~ 0.9–1.2)
|
A2780 and A2780cis xenograft (right flank) treated once by trail vein injection
|
reduced tumor growth rates compared to the free drugs; Increased cisplatin localization in the tumor
|
[78]
|
|
Hyaluronic acid micelles
|
cisplatin/EGCG
|
SKOV-3
|
Slight decrease in cell viability compared to single drug loaded NPs. Intracellular uptake was possible facilitating Pt accumulation.
|
SKOV-3-Luc xenograft (IP) treated once a week for 3 weeks by IP injection
|
increased the Pt accumulation in the tumor and reduced tumor volume as well as increased survival rate compared to free cisplatin
|
[79]
|
|
PCL-based triblock co-polymer micelle carriers
|
oxoplatin/curcumin
|
A2780
|
strong synergistic interaction (CI ~ 0.3)
|
-
|
-
|
[80]
|
|
poly(norbornene)-co-poly(ethylene glycol)
|
Cisplatin/doxorubicin camptothecin
|
OVCAR-3
|
The triple drug co-loaded formulation was more potent than the single drug (cisplatin) or two drug loaded combination as indicated by the decrease in IC50 (up to 11-fold)
|
-
|
-
|
[81]
|
2.3. Taxane Based Combinations
Polymer nanoparticle formulations of taxane-based drug combinations have also been considered (and summarized in ). For example, Boztas et al. utilized poly (β-cyclodextrin triazine) (PCDT) to formulate combinations of paclitaxel and curcumin. Curcumin, a low-molecular weight polyphenol extracted from turmeric, has had synergistic effects when combined with paclitaxel using polymer and polymer nanoparticle platforms. Curcumin can inhibit the proliferation and survival or tumor cells as well as improve the drug resistance of tumor cells. Therapeutic applications of curcumin in the preclinical and clinical stages have been limited due to its low water solubility, low dissolution rate, and poor viability. Thus, formulation using polymers has been considered [
82,
83,
84]. PCDT was synthesized through a one-step condensation polymerization of β-cyclodextrin triazine. The resulting polymer had a molecular weight of 25.7 kg/mol by GPC. Curcumin was incorporated by forming an inclusion complex with the PCDT in a mixture of acetone and water and freeze-drying. Then, the paclitaxel was complexed in a mixture of ethanol and water followed by freeze drying. The potency of the drug formulations were evaluated in vitro using various cancer cell lines including ovarian cancer cell lines A2780 and SKOV-3. The drugs were significantly more potent when complexed with the polymer. For example, there was a 15-fold decease in IC50 concentration in A2780 cells when compared to the free drug combination. There was also a five-fold decrease in IC50 concentration in SKOV-3 cells compared to the free drug combination. Interestingly, the drugs acted synergistically in the polymer complex. The combination index was 0.69 and 0.65 for A2780 and SKOV-3 cells, respectively. The combination index was lower than the free drug combinations in both cell lines (0.82 and 1.0 for A2780 and SKOV-3 cell lines, respectively). Quantitative apoptotic activity analysis by flow cytometry indicated that the polymer/drug combination increases apoptosis in A2780 and SKOV-3 cells compared to the free drug combination. The increase in drug efficacy suggest that the polymer platform improves drug solubility and bioavailability of the drugs [
85].
Table 2. Polymer nanocarrier formulations of paclitaxel-based drug combinations.
|
Nanoparticle
|
Drugs
|
In Vitro
|
Key Results In Vitro
|
In Vivo
|
Key Results In Vivo
|
Source
|
|
Cyclodextrin nanocarries
|
paclitaxel/curcumin
|
A2780, SKOV-3
|
Syngeistic (CI ~ 0.65) when compared to free drugs (CI ~ 1)
|
-
|
-
|
[85]
|
|
PEI-g-stearic acid micelles coated with hyaluronic acid
|
paclitaxel/curcumin
|
SKOV-3 and SKOV-3-TR30 (multi-drug resistant)
|
17.3-fold lower IC50 in SKOV-3 cells and 115-fold lower in SKOV-3-TR30 cells compared to free paclitaxel
|
every other day for 5 times via tail vein injection
|
Reduces tumor volume compared to free drug (t-test, 5%) and PTX only nanoparticles (t-test 10%)
|
[86]
|
|
PEO-PCL nanoparticles
|
paclitaxel/tamoxifen
|
SKOV-3, SKOV-3TR
|
10-fold decrease in IC50 of paclitaxel (SKOV-3), CI ~ 0.4 and (CI ~ 0.7) in SKOV-3TR
|
SKOV-3, SKOV-3TR xenograft (flank) treated at day 1 and day 24 through tail vein injection
|
suppressed tumor growth, lowering systemic toxicity, tamoxifen enhanced cytotoxicity of paclitaxel
|
[87]
|
|
mPEG-PCL polymer micelles
|
paclitaxel/tacrolimus (FK506)
|
A2780/T (PTX resistant)
|
5.3-fold decrease in IC50 compared to PTX only micelles;
|
-
|
-
|
[88]
|
|
Chitosan/alginate nanocapsules
|
paclitaxel/lapatnib
|
OVCAR-3
|
Increased cytotoxicity compared to PTX
|
-
|
-
|
[89]
|
|
PS-PEG nanoparticles
|
paclitaxel/lapatinib
|
OVCA-432
|
1500-fold decrease in IC compared to free drug; co-loaded formulation 4.4 fold decrease in IC50 concentration compared to PTX only formulation; CI 0.23; co-loaded formulation more potent than two single drug loaded nanoparticle (CI 0.40)
|
-
|
-
|
[90]
|
|
EGFR-peptide-PCL nanoparticles
|
paclitaxel/lonidamine
|
SKOV-3, SKOV-3TR, OVCAR-5 (MDR)
|
2-fold decrease in IC50 of paclitaxel in OVCAR-5 cells under hypoxic conditions (no change in IC50 under noroxative conditions or other cell types)
|
-
|
-
|
[91]
|
|
PEG-b-PCL micelles
|
paclitaxel/cyclopamine/gossypol
|
SKOV-3, ES-2
|
2D model: no increased potency compared to paclitaxel micelles; 3D model: disaggregation of the spheroid
|
ES-2, SKOV-3 xenografts via IP injection once a week for 3 weeks via IP injection
|
significantly reduced tumor volume and extended survival time compared to free paclitaxel
|
[92]
|
Additional polymer-based nanoparticle formulations combining curcumin and paclitaxel have also been reported. Specifically, the drug combination was incorporated into polyethylenimine-g-stearic acid micelles coated with hyaluronic acid. The drug-loaded micelles were prepared by probe ultrasonication. Briefly, the drugs dissolved in ethanol were added to the micelles dispersed in water and sonicated, stirred, dialyzed, and centrifuged to remove unincorporated drugs, filtered (0.45 μm), and lyophilized. The drug loaded particles had a diameter of approximately 190 nm with a polydispersity index of 0.252 measured by dynamic light scattering. The potency of the nanoparticles was assessed in vitro using SKOV-3 and SKOV3-TR30 cells. Formulating paclitaxel into nanoparticles significantly increased its potency. There was a 12-fold decrease in IC50 for paclitaxel in SKOV-3 cells compared to the free drug. Interestingly, there was a larger effect of SKOV3-TR30 cells; a 72-fold decrease in IC50 for paclitaxel was observed compared to the free drug. Formulating curcumin with the polymer micelles also enhanced its potency. There was a 3.7-to 5.5-fold decrease curcumin IC50 upon formulation compared to the free drug for SKOV-3 and SKOV3-TR30 cells, respectively. Co-encapsulation of the drugs further increased paclitaxel potency. The IC50 was 17.3-fold lower in SKOV-3 cells and 115-fold lower in SKOV-3-TR30 cells compared to free paclitaxel. Notably, the co-loaded formulation was more potent than treating with free paclitaxel combined with curcumin nanoparticles. The formulation of the combination was also beneficial compared to the paclitaxel only nanoparticles; there was a ~1.5-fold decrease in IC50 of paclitaxel when formulating the combination compared to paclitaxel only. The in vivo efficacy was evaluated using a SKOV-3 xenograft model injected subcutaneously in the right side. Treatments were administered via tail vein injection every other day for 5 cycles. The co-loaded formulation reduced tumor volume in vivo compared to the free drugs. These results demonstrate paclitaxel and curcumin can be incorporated into polymer micelles with promising effects in vitro and in vivo [
86].
2.4. Other Drug Combinations
While paclitaxel and platinum chemotherapeutic agents are the most prevalent in both free drug and nanoparticle formulations, nanoparticle formulations of other drug combinations have been investigated in ovarian cancer in vitro and in vivo and are summarized in . For example, Li et al. incorporated in docetaxel and gemcitabine on folate-targeted nanoparticles to treat ovarian cancer. Specifically, docetaxel and gemcitabine were co-loaded in nanoparticles stabilized by folic acid-conjugated to PEG-b-PLGA using the nanoprecipitation method. The drugs and modified polymer were dissolved in chloroform and then the chloroform was evaporated to form a film. The film was redispersed in PBS and homogenized for 10 cycles and 25,000 psi. The resulting dispersions were centrifuged to recover the free drug. Upon redispersion, spherical, drug-loaded nanoparticle formed by self-assembly. The resulting nanoparticle size was ~120 nm by TEM. The particle dispersions appeared to be stable over 3 months; no particle aggregation or change in particle size was observed. The cytotoxic effect of the nanoparticles was evaluated in vitro using SKOV-3 cells. Formulating the drug combination into nanoparticles increased the potency by over 3.5-fold as indicated by the decrease in IC50 value. The efficacy of the nanoparticles was studied in vivo using a xenograft model. The mice were treated via tail vein injection every 2 days for 3 weeks. At the end of treatment, the nanoparticles had significantly reduced tumor volume compared to the free drugs. Overall, the results showed the nanoparticles significantly reduced tumor volume, rate of tumor growth, and reduced off-target toxicity compared to free drug combination [
93].
Table 3. Formulations of other drug combinations using polymer micelles/nanoparticles.
|
Nanoparticle
|
Drugs
|
In Vitro
|
Key Results In Vitro
|
In Vivo
|
Key Results In Vivo |
Source |
|
Folate-PEG-PLGAnanoparticles
|
docetaxel/gemcitabine
|
SKOV-3
|
3.59-fold drop in the IC50 and improve cytotoxicity in SKOV-3 cells as compared to free drug combination
|
SKOV-3 xenograft treated every 2 days for 3 weeks via tail vein injections
|
Reduced tumor volume and rate of tumor growth compared to free drug combination with no organ toxicity |
[93] |
|
mPEG-PLA polymer micelles
|
doxorubicin/gemcitabine
|
SKOV-3
|
drug internalization via endocytosis
|
-
|
- |
[94] |
|
mPEG-PLA nanoparticles
|
doxorubicin/verapamil
|
A2780, SKOV-3, A2780/DOX, and SKOV-3/DOXR
|
micelles increased drug accumulation and enhanced apoptosis
|
A2780/DOXR and SKOV-3/DOXR xenograft treated every 3 days for 2 weeks via tail vein injection
|
inhibited tumor growth and increased survival time compared to free doxobucin with reduced side effects |
[95] |
|
mPEG-b-poly[N-2-hydroxyethyl)-aspartamide]/phenylboronic acid
|
Doxorubicin/irinotecan
|
SKOV-3
|
Micelles increase IC50 compared to free drug; co-loaded micelles synergistic compared to single drug loaded (CI 0.3)
|
-
|
- |
[96] |
|
Pluronic® F-127 micelles
|
resveratrol co-loaded with quercetin or curcumin in NPs with free adriamycrin
|
ES2-Luc, A2780, and A2780ADR, ES2-Luc
|
Up to 10 –fold reduction in IC50 and synergistic (CI < 0.5) in A2780 and A2780ADR cells
|
ES2-Luc and A2780ADR xenografts treated with weekly injections for 4 weeks via tail vein injection
|
Significant tumor reduction and cardioprotective effect compared to ADR alone |
[97] |
|
mPEG-b-PLA micelles
|
Chetomin/Everolimus
|
ES-2, OVCAR-3, TOV-21G
|
Combination index for co-loaded micelle was <1 compared to single drug loaded micelles
|
ES-2 treated with weekly injections for 3 weeks via tail vein injection
|
Significant tumor reduction compared to empty micelles and saline control |
[98] |
|
Amphiphilic drug-drug conjugate nanopartpices
|
floxuridine-chlorambucil
|
OVCAR-3
|
Combination index was nanodrugs~0.3 compared to~0.7 for the free drug
|
-
|
- |
[99] |
2.5. Lipid Nanoparticles
Microemulsions and lipid based nanoparticles are a well-established platform for cancer treatment with improved safety compared to the free drug [
18]. When used in combination with carboplatin and bevacizumab, PEGylated-liposomal doxorubicin has recently been proposed as the new standard clinical treatment for platinum-eligible recurrent ovarian cancer [
100]. Adding polymers to the liposome formulations has also been used to enhance the structural stability and tune the drug release mechanism of drug combinations. For example, poly-L-lysine, a polycation, and hyaluronic acid, a polyanion were sequentially deposited on liposomes containing cisplatin (in the core) and either olaparib or talazoparib, poly(ADP-ribose (PARP) inhibitors (in the lipid bilayer). The resulting hybrid polymer-lipid nanoparticles were 90 ± 12 nm by dynamic light scattering. Due to the drug distribution in the nanoparticle structure, sequential release of the PARP inhibitors followed by release of the cisplatin was achieved. Examining the drug potency in vitro, formulating the drugs enhanced potency compared each of the free drug in both OVCAR-8 and COV-362 cells as indicated by the decrease in IC50 value (B). The in vivo efficacy of the nanoparticle formulations was examined using mice with OVCAR-8 xenografts intraperitoneally injected and treated by tail vein injection every week. The nanoparticle formulation of the drug combination was a more effective treatment than the free drug combination at reducing tumor burden and metastasis as well as increasing survival [
101].
Solid lipid nanoparticles are also a promising platform to achieve controlled drug release because the drug mobility in a solid lipid is expected to be significantly lower than a lipid in the liquid phase. Solid lipid particles can be prepared by freeze spray drying and used for retarded release after peroral administration. Aqueous dispersions of submicron particles are typically produced via high pressure homogenization of lipid, water, and an emulsifier (which has been found to be more effective than high shear mixing or ultrasound). Dilution of microemulsions has also been used to achieve dispersions of solid lipid nanoparticles with average particle size below 500 nm. Typically, the dispersions are stabilized with emulsifiers such as triglycerides, fatty acids, or steroids. Amphiphilic block copolymers such as Poloxamers (Pluronics, triblock copolymers of polyethylene glycol-b-polyoxypropylene-b-polyethylene glycol) have also been used as stabilizers. Lipid nanoparticles can encapsulate hydrophobic drugs in the core by dispersing the drug in the lipid prior to homogenization. Alternatively, drugs can be conjugated to the lipid. Detailed reviews on the formulation of solid lipid nanoparticles can be found elsewhere [
102,
103]. Lipid based nanoparticles can be combined with polymers to achieve controlled release drug (small molecule) cocktails. In this review, we highlight examples of lipid polymer hybrid nanoparticles used to deliver combinations of chemotherapeutics to treat ovarian cancer. Details of lipid-polymer nanocarrier studies are found in .
Table 4. Lipid-polymer nanocarriers for co-delivery of anticancer drugs.
|
Nanoparticle
|
Drugs
|
In Vitro
|
Key Results In Vitro
|
In Vivo
|
Key Results In Vivo
|
Source
|
|
Polyelectrolyte coated liposome
|
Cisplatin/olaparib or talazoparib
|
OVCAR-8 and COV362
|
enhanced potency (reduced IC50) compared to free drugs
|
OVCAR-8 xenografts treated by tail vein injection once a week
|
Reduced tumor burden and metastasis as well as increasing survival
|
[101]
|
|
PEGylated lipid nanoemulsion
|
paclitaxel/curcumin
|
SKOV-3, SKOV-3TR (drug resistant)
|
enhanced cytotoxicity and increased apoptosis, slightly synergistic (CI = 0.93) in SKOV-3 and additive in SKOV-3TR compared to free drugs
|
-
|
-
|
[104]
|
|
PEG stabilized microemulsion
|
brucea oil/tripterine
|
SKOV-3
|
CI = 0.90 at an 20:1 w:w ratio of brucea oil to tripterine
|
-
|
-
|
[105]
|
|
iRGD peptide Lipid-polymer hybrid nanoparticles
|
paclitaxel/tetrandrine
|
A2780/PTX cells (paclitaxel resistant)
|
CI 0.49–0.64 depending on drug ratios; increased intracellular paclitaxel accumulation apoptosis when co-loaded
|
-
|
-
|
[106]
|
|
Lipid-templated polymer-caged nanobins
|
cisplatin/doxorubicin
|
OVCAR-3
|
enhanced cytotoxicity compared to both free drug and single-drug nanobins; CI between 0.27 and 0.67 depending on drug ratio compared
|
-
|
-
|
[107]
|
|
DSPE-PEG micelles
|
paclitaxel/tanespimycin (17-AAG)
|
-
|
-
|
SKOV-3 xenograft (flank) with sequential delivery of paclitaxel (free or NPs) once a week and followed by 17-AAG (free or NPs) 3 days later for 3 weeks, administed through tail vein injection
|
increased tumor accumulation by 2-fold,~2-fold reduction in tumor mass after 43 days significant tumor growth arrest compared to free drug combinations
|
[112]
|
|
Core-shell DOPA, DSPE-PEG, and cholesterol nanoparticles
|
carboplatin/gemcitabine
|
SKOV-3, A2780/CDPP (platinum resistant cells)
|
CI~0.5 comparable to free drugs
|
SKOV-3, A2780/CDDP (platinum-resistant) xenografts (right flank) injected by IP once every 3 days for a total of 3 injections
|
reduced tumor weight by 12-fold compared to free drug combination
|
[113]
|
|
mPEG-DPPE/calcium phosphate nanoparticle
|
triptolide/curcumin
|
SKOV-3
|
Higher apoptosis rate compared to free drugs
|
SKOV-3 xenografts (upper left axillary fossa) treated twice a week for 24 days via tail vein injection
|
Reduced tumor volume compared to free drugs
|
[114]
|
2.6. Dendrimers
As an alternative to assembled polymer micelles and nanoparticles, another versatile polymer nanoparticle platform for drug delivery has been dendrimers. Dendrimers are hyperbranched, three-dimensional polymers. Starting from a core, they contain layers of branched repeating units and end groups on the outer layer of repeat units. Dendrimers are produced using iterative reactions. Each repeated reaction results in an additional layer of branches, i.e., a generation. The properties and resulting structure of the dendrimer can be tuned. For example, the polymer composition and number of branches will affect the size, hydrophobicity, surface charge. For drug delivery applications, therapeutic moieties can be covalently conjugated to polymer branches or entrapped in the dendrimer core by electrostatic or hydrophobic interaction. More detailed reviews of dendrimer synthesis and formulation can be found elsewhere [
115,
116,
117,
118]. In this review, we highlight examples of dendrimers used to deliver combinations of chemotherapeutics to treat ovarian cancer. Details of these dendrimer studies are found in .
Table 5. Dendrimer based nanocarriers for co-delivery of anticancer drugs.
|
Nanoparticle
|
Drugs
|
In Vitro
|
Key Results In Vitro
|
In Vivo
|
Key Results In Vivo
|
Source
|
|
PEG 3-generation telodendrimer micelles
|
cisplatin/paclitaxel
|
SKOV-3, ES-2
|
Antagonistic at 1:1 ratio; synergistic at 2:1 ratio of cisplatin to paclitaxel (CI = 0.21 for SKOV-3)
|
SKOV-3 xenograft (flank) treated 3 times at 4-day intervals via tail vein injection
|
highest accumulation in the tumor tissue, decreased tumor volume, increased survival time, and reduced renal toxicity compared to free cisplatin, cisplatin loaded telodendrimers, or paclitaxel loaded dendrimers
|
[119]
|
|
PLA/PLGA/PEG dendrimers
|
cisplatin prodrug/aspirin prodrug
|
A2780/CP70 (cisplatin resistant)
|
~4-fold decreased IC50 in nanoparticle formulation
|
-
|
-
|
[121]
|
|
PEG dendrimers
|
Oxaliplatin/curcumin dendrimers
|
SKOV-3/OVCAR-3
|
CI 0.855 in SKOV-3/CI 0.708 in OVCAR-3 after 48 h of treatment (IC50)
|
-
|
-
|
[122]
|
|
3-generation PEG-PAMAM dendrimers
|
paclitaxel/borneol
|
A2780/PTX (paclitaxel resistant)
|
3-fold lower IC50 value compared to the free drug combination
|
A2780/PTX xenograft (back) once every two days for 7 tail vein injections
|
decrease in tumor volume, compared with the free drug combination
|
[123]
|
|
Linear-dendritic telodendrimers
|
doxorubicin/bortezomib
|
SKOV-3
|
Synergistic effects observed at bortezomib: doxorubicin ratios between 1:1 and 1:10; antagonistic at lower ratios
|
SKOV-3 xenograft (flank) treated every 4 days for a total of 3 tail vein injections
|
decreased toxicity delayed tumor growth compared to free drugs
|
[124]
|
This entry is adapted from the peer-reviewed paper 10.3390/nano11041048