Your browser does not fully support modern features. Please upgrade for a smoother experience.
Please note this is a comparison between Version 1 by Cristina Maccallini and Version 2 by Rita Xu.
Neurodegenerative diseases are incurable and debilitating conditions that result in progressive degeneration and loss of nerve cells. Oxidative stress has been proposed as one factor that plays a potential role in the pathogenesis of neurodegenerative disorders since neuron cells are particularly vulnerable to oxidative damage. Nuclear factor (erythroid-derived 2)-like 2 (Nrf2) is strictly related to anti-inflammatory and antioxidative cell response; therefore, its activation and the consequent enhancement of the related cellular pathways have been proposed as a potential therapeutic approach.
- electrophilic activators
- multitargeting compounds
- Nrf2 inducers
1. Introduction
Neurodegenerative diseases affect millions of people worldwide and are a leading cause of disability and a major cause of mortality [1]. The treatment of these pathological conditions is only palliative; therefore, there is an urgent need for effective therapeutic agents, as well as a deeper understanding of the molecular changes affecting neuronal cells during the disease progression. Neuroinflammation is a hallmark in the development of neurodegenerative diseases, as well as nitroxidative stress, which is due to the unbalanced production of both reactive oxygen species (ROS) and reactive nitrogen species (RNS) [2][3][2,3]. The key role played by ROS in the onset of age-related neurodegenerative diseases indicates that erythroid-derived 2-like 2 (Nrf2), the master regulator of redox homeostasis [4], may be a promising target for therapeutic interventions. Several Nrf2 activators with different mechanisms and diverse structures have been reported in the literature, but those applied to neurodegenerative diseases are still limited [5]. However, in the very last few years, interesting progress has been made in this field, particularly in enhancing the blood–brain barrier (BBB) permeability of Nrf2 activators, to make them effective drugs, and in designing Nrf2-based multitarget-directed ligands to affect multiple pathways involved in the pathology of neurodegenerative diseases.
2. Implication of Oxidative Stress and Nrf2 Activation in Neurodegenerative Diseases
ROS are a byproduct of several cellular metabolic pathways and enzymatic reactions, and they are classified as radicals, including superoxide anion (O2●−) and hydroxyl (HO●−), as well as nonradical species such as hydrogen peroxide (H2O2) [6]. ROS are reactive molecules with a very short half-life. H2O2, the most stable ROS, has a cellular half-life of 10−3 s, 1000 times higher than other ROS [7][8][7,8]. Although ROS production might be due to environmental factors, it mainly derives from metabolic activities. During mitochondrial respiration, in the electron transport chain (ETC), approximately 1–2% of O2 is not reduced to water, leading to the generation of O2●− and H2O2. Moreover, cytosolic oxidoreductases such as NADPH oxidases (NOX), cytochrome P450 (CYP) oxidases, cyclooxygenases (COX), and monoamine oxidases (MAO) may contribute to ROS production [8]. Physiological ROS levels are maintained by a plethora of exogenous and endogenous antioxidant defenses. Among the exogenous antioxidants, ascorbic acid (vitamin C), α-tocopherol (vitamin E), and carotenoids play a pivotal role. Endogenous antioxidants include enzymatic antioxidants, e.g., superoxide dismutase (SOD), glutathione peroxidase (GPX), and catalase (CAT), as well as nonenzymatic scavengers, e.g., glutathione (GSH) (Figure 1) [9].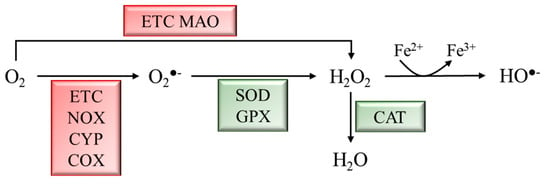
Figure 1. Schematic representation of ROS generation and scavenging. Molecular oxygen (O2) can be partially reduced to superoxide anion (O2●−) by the ETC, NADPH oxidases (NOX), cytochrome P450 (CYP) oxidases, and cyclooxygenases (COX), or to hydrogen peroxide (H2O2) by the ETC and monoamine oxidases (MAO). H2O2 can be converted into hydroxyl radical (HO●−) through the Fenton rection. Enzymatic antioxidants scavenge ROS to produce less reactive molecules. Superoxide dismutase (SOD) and glutathione peroxidase (GPX) convert O2●− to H2O2, which is converted into H2O by catalase (CAT).
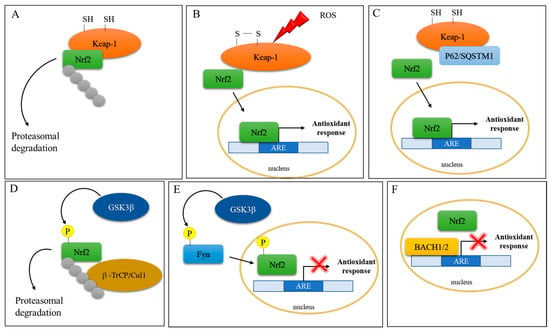
Figure 2. Schematic representation of Nrf2 activation. (A) Under basal conditions, Nrf2 activity is controlled by the cytoplasmic repressor protein Keap1, which sequesters Nrf2 in the cytosol, leading to its ubiquitination and proteasomal degradation. (B) Under oxidative stress conditions, two of the Cys residues in Keap1 become oxidized, impeding the correct orientation of Nrf2 and inhibiting its ubiquitination and degradation. The newly synthesized Nrf2 translocates to the nucleus to induce the expression of antioxidant response genes. (C) P62/sequestosome 1 (p62/SQSTM1) competes with Nrf2 for Keap-1 binding and leads to Nrf2 activation and nuclear translocation. (D) Glycogen synthase kinase-3β (GSK-3β) phosphorylates Nrf2, which is in turn ubiquitinated by β-transducin repeat-containing protein/Cullin-1 E3 ubiquitin ligase (β–TrCP/Cul1). (E) GSK-3β phosphorylates the protein kinase Fyn, which phosphorylates Nrf2, leading to its nuclear export and culminating in inhibition of gene expression (red cross). (F) The BTB and CNC homology transcription factors (BACH1 and BACH2) repress Nrf2 activity (red cross) by competing for ARE binding.
2.1. Nrf2 and Parkinson’s Disease
PD is a progressive neurological movement disorder characterized by tremor, bradykinesia, rigid muscles, and loss of postural balance [28]. The clinical feature of PD is the depletion of dopaminergic (DArgic) neurons in the substantia nigra pars compacta (SNpc), which results in dopamine (DA) deficiency [29]. PD is prevalently an idiopathic disease, with only 10–15% of cases having a family history. However, Lewy bodies found in both sporadic and familial cases of PD contain aggregated forms of α-synuclein (α-syn). The α-syn oligomers are cytotoxic to DArgic neurons [30]. The toxic effects of α-syn oligomers can be ascribed to α-syn enzymatic ferrireductase activity. Aggregation indeed inhibits α-syn enzymatic activity, leading to an accumulation of oxidized Fe, which can participate in the Fenton reaction, culminating in oxidative stress induction [31]. Moreover, mitochondrial α-syn accumulation can suppress mitochondrial respiratory complex I, leading to ROS production and, thus, to oxidative stress [32]. The crucial role of mitochondria-generated ROS in PD pathogenesis was determined from the finding that the 1-methyl-4-phenyl 1,2,3,6-tetrahydropyridine (MPTP) metabolite 1-methyl-4-phenylpyridinium (MPP+) hampers mitochondrial complex I, causing electron leakage and ROS production [33]. PD-like symptoms indeed arose in individuals using illegal drugs contaminated by MPTP, and brain postmortem examinations revealed damage to the DArgic neurons in the SNpc. Other PD genetic risk factors comprise genes involved in the control of mitochondrial redox balance including Parkin, PTEN-induced kinase 1 (PINK1), parkinsonism-associated deglycase (PARK7), and leucine-rich repeat serine/threonine protein kinase 2 (LRRK2) [34]. Parkin, an E3 ubiquitin ligase, and PINK1, a serine/threonine kinase, form a signal transduction pathway exerting a pivotal role in the removal of damaged mitochondria by the mitophagic process [35]; PARK7 encodes for DJ-1, a protein that, by binding the mitochondrial complex I, improves its activity [36]. Mutations in PINK1, DJ-1, and LRRK2 result in mitochondrial dysfunction with impaired bioenergetics and lead to uncontrolled ROS generation [36][37][36,37]. It should be emphasized that DA metabolism itself is a source of oxidative stress. In fact, excess DA can be catabolized by monoamine oxidase (MAO), producing H2O2 or undergoing auto-oxidation to produce highly reactive dopamine quinones (DAQs) and semiquinones [38]. The crucial role played by ROS in PD indicates Nrf2 implication in this disease. In vivo studies showed that both treatment with MPTP and overexpression of α-syn increased DArgic cell death in Nrf2 KO mice [39][40][39,40]. Moreover, the Nrf2-induced cytoprotective gene NQO1 (NADPH-quinone oxidoreductase) is partially sequestered in Lewy bodies, together with p62/SQSTM1, a known activator of Nrf2 [41]. Moreover, Bach1 knockout protects mice against MPTP-induced dopaminergic cell death [42]. Moreover, the brain of LRRK2-transgenic mice and the LRRK2-overexpressing neuronal cell line show reduced expression of Nrf2 and its target genes via GSK3β activation [43]. Studies in Drosophila showed that Nrf2 activation induces mitophagy and counteracts neuronal degeneration in Parkin/Pink1 knockdown flies [44]. In addition to direct neuronal toxicity, α-syn oligomers can activate microglial cells promoting neuroinflammation, which, by further increasing ROS production via NADPH oxydase 2 (NOX2) activation, augments oxidative stress [34][41][34,41]. In this context, DJ-1, by interacting with the p47phox subunit of NOX2, inhibits its action, reducing ROS production [45]. From all the above, PD genetic risk factors are connected to aberrant Nrf2 signaling which might contribute to oxidative stress (Figure 3).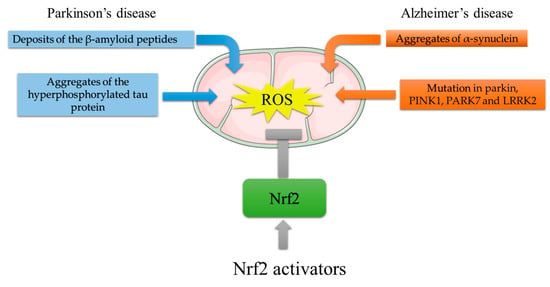
Figure 3. Mitochondrial ROS generation by PD and AD risk factors, and protective effects of Nrf2 activating compounds. ROS generation in AD: deposition of Aβ plaques induces mitochondrial stress; aggregates of the hyperphosphorylated tau protein impair mitochondria distribution and function. ROS generation in PD: aggregated α-syn accumulation suppresses mitochondrial respiratory complex I; mutations in Parkin, PTEN-induced kinase 1 (PINK1), parkinsonism-associated deglycase (PARK7), and leucine-rich repeat serine/threonine protein kinase 2 (LRRK2) result in mitochondrial dysfunction with impaired bioenergetics. The Nrf2-mediated increase in antioxidant response genes can reduce ROS burst. In this light, Nrf2 activators might counteract the ROS-induced damage that leads to neurodegeneration.
