Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Alessia Policlinico Modena University of Modena and Reggio Emilia - Modena Verduri | -- | 1079 | 2024-02-26 16:02:09 | | | |
| 2 | Rita Xu | -188 word(s) | 891 | 2024-02-27 04:29:15 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Verduri, A.; Clini, E.; Carter, B.; Hewitt, J. Symptom Burden in Chronic Obstructive Pulmonary Disease. Encyclopedia. Available online: https://encyclopedia.pub/entry/55478 (accessed on 21 May 2026).
Verduri A, Clini E, Carter B, Hewitt J. Symptom Burden in Chronic Obstructive Pulmonary Disease. Encyclopedia. Available at: https://encyclopedia.pub/entry/55478. Accessed May 21, 2026.
Verduri, Alessia, Enrico Clini, Ben Carter, Jonathan Hewitt. "Symptom Burden in Chronic Obstructive Pulmonary Disease" Encyclopedia, https://encyclopedia.pub/entry/55478 (accessed May 21, 2026).
Verduri, A., Clini, E., Carter, B., & Hewitt, J. (2024, February 26). Symptom Burden in Chronic Obstructive Pulmonary Disease. In Encyclopedia. https://encyclopedia.pub/entry/55478
Verduri, Alessia, et al. "Symptom Burden in Chronic Obstructive Pulmonary Disease." Encyclopedia. Web. 26 February, 2024.
Copy Citation
Chronic obstructive pulmonary disease (COPD), the sixth leading cause of death in the United States in 2022 and the third leading cause of death in England and Wales in 2022, is associated with high symptom burden, particularly dyspnoea. Frailty is a complex clinical syndrome associated with an increased vulnerability to adverse health outcomes.
COPD
frailty
symptoms
dyspnoea
GOLD guidelines
1. Introduction
Chronic obstructive pulmonary disease (COPD) is one of the leading causes of morbidity and remains one of the top three causes of death worldwide [1]. The global prevalence of COPD increases with age, and the burden related to is expected to rise over the next years due to persistent exposure to risk factors and ageing of the world’s population [1][2]. According to the GOLD criteria, roughly 400 million people have been reported to suffer from COPD globally in 2019 [3]. COPD is characterised by chronic respiratory symptoms, including dyspnoea and activity limitation, that have a negative impact on patients’ quality of life and increase the risk of depression and anxiety [1].
Frailty is a complex syndrome described as a state of reduced physiological reserve causing increased vulnerability to adverse events and external stressors. This vulnerability can result in disability, admission to a hospital or a long-term facility, and increased risk of all-cause mortality. There are different validated tools available to measure frailty, ranging from simple assessment of functional status to complex, multi-domain scoring systems that evaluate cognitive, physical, and functional ability [4][5][6][7]. Two main classifications of frailty (the deficit model and the phenotype model) are widely accepted and frequently used in clinical practice [5][8]. The frailty phenotype model proposed by Fried et al. [5] is defined as the presence of three or more of the following domains: exhaustion, weakness, slowness, low activity, and unintentional weight loss. The frailty index (FI) [8] is a quantification of the cumulative burden of health deficits including laboratory findings, physical function disabilities, diseases, symptoms, sensory difficulties, and cognition difficulties.
2. Overview of Symptoms in COPD
Dyspnoea, also known as shortness of breath or breathlessness, is the most typical symptom and debilitating for patients with COPD and is associated with a deterioration in their physical activity [9]. Dyspnoea is defined as “a subjective experience of breathing discomfort that consists of qualitatively distinct sensation that vary in intensity” [10] and results from multiple mechanism, including air trapping, dynamic hyperinflation, and gas exchange abnormalities [11]. Fatigue, described as an individual feeling of tiredness and being drained of energy until exhaustion, is one of the most common symptoms in COPD. It has an impact on activities of daily living and is associated with frustration and problems with concentration [12]. The intensity of fatigue is variable and, similar to dyspnoea, can be increased by intercurrent exacerbation of COPD. Other cardinal symptoms of patients with COPD include chronic cough with sputum production, chest tightness, and wheezing which may be recurrent as well [1].
The prevalence of dyspnoea is high across all stages of airflow obstruction [13]. Dyspnoea intensity has been associated with age ≥70 years, higher severity of airflow obstruction, female gender, obesity, history of moderate-to-severe exacerbations, and comorbidities [14]. Fatigue has been also reported in mild COPD [15].
3. Assessment of Symptoms in COPD
The degree of airflow obstruction can be a poor effective predictor of symptom burden in COPD, especially for dyspnoea and fatigue. Validated questionnaires have been developed to promote a more comprehensive evaluation of breathlessness and other relevant symptoms in these patients. All symptoms in COPD represent an individual experience, difficult to quantify numerically with questionnaires; hence, several scales are available both in research settings and clinical practice [1].
These include the modified Medical Research Council (mMRC) dyspnoea scale (Figure 1), including five statements to measure the degree of disability due to breathlessness in daily activities on a scale from 0 to 4 [16][17], and multidimensional questionnaires such as the COPD Assessment Test (CAT) (Figure 2), which includes eight items describing the clinical manifestations of COPD. Cough, presence of mucus, chest tightness, dyspnoea, limitation in activities of daily living, feeling confident, sleeping, and energy are the components of the test, scoring 0 to 40 [18]. Both are used to describe level of symptoms in the Global Initiative for Chronic Obstructive Lung Disease (GOLD) recommendations that suggest a therapeutic strategy based on the history of exacerbations and burden of symptoms in stable COPD (GOLD 2023) [1].
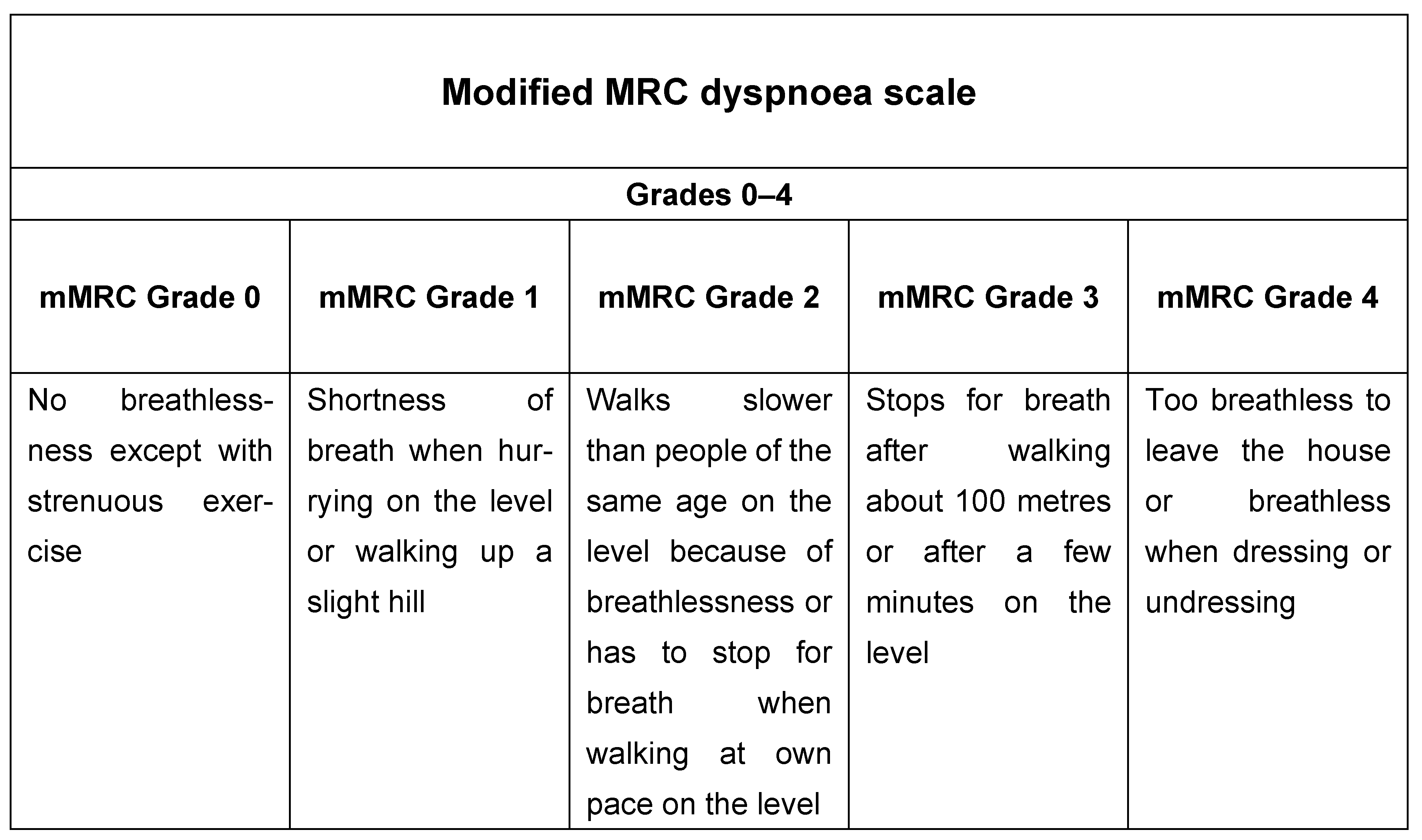
Figure 1. Modified Medical Research Council dyspnoea scale.

Figure 2. COPD Assessment Test.
4. Psychological Burden of Symptoms in COPD Patients
Dyspnoea and fatigue have been associated with anxiety and depression in COPD [19]. These comorbidities may result from the distress related to breathlessness and fatigue that are perceived as negative emotions associated with fear and feeling of sadness by patients [10], resulting in worse patient health and quality of life. Whilst these comorbidities have not been fully studied, the reported prevalences, mainly due to the population assessed in primary or secondary care settings, vary widely with mean range of 35–40% for depression and 28–36% for anxiety [20][21]. Anxiety and fear related to COPD are prevalent complications that widely contribute to disability and difficulties in activities of daily living in this population. Many patients adopt a sedentary lifestyle in anticipation of dyspnoea, and fear of exhaustion can result in experiencing more severe shortness of breath during exercise [22]. It has been noted that patients with COPD and associated depression experience more dyspnoea than their counterparts without depression [23]. The depression symptoms may range from sub-clinical depressive symptoms to clinical depression and, along with anxiety, have an effect on lack of energy, irritability, and feelings of demoralisation [22][24].
References
- Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease. Global Initiative for Chronic Obstructive Lung Disease: 2023 Report. Available online: https://goldcopd.org/ (accessed on 5 October 2023).
- Agusti, A.; Melen, E.; DeMeo, D.L.; Breyer-Kohansal, R.; Faner, R. Pathogenesis of chronic obstructive pulmonary disease: Understanding the contributions of gene-environment interactions across the lifespan. Lancet Respir. Med. 2022, 10, 512–524.
- Adeloye, D.; Song, P.; Zhu, Y.; Campbell, H.; Sheikh, A.; Rudan, I.; NIHR RESPIRE Global Respiratory Health Unit. Global, regional, and national prevalence of, and risk factors for, chronic obstructive pulmonary disease (COPD) in 2019: A systematic review and modelling analysis. Lancet Respir. Med. 2022, 10, 447–458.
- Clegg, A.; Young, J.; Iliffe, S.; Rikkert, M.O.; Rockwood, K. Frailty in elderly people. Lancet 2013, 381, 752–762.
- Fried, L.P.; Tangen, C.M.; Walston, J.; Newman, A.B.; Hirsh, C.; Gottdiener, J.; Seeman, T.; Tracy, R.; Kop, W.J.; Burke, G.; et al. Frailty in older adults: Evidence for a phenotype. J. Gerontol. A Biol. Sci. Med. Sci. 2001, 56, M146–M156.
- Rockwood, K.; Song, X.; MacKnight, C.; Bergman, H.; Hogan, D.B.; McDowell, I.; Mitnitski, A. A global clinical measure of fitness and frailty in elderly people. CMAJ 2005, 173, 489–495.
- Jones, D.M.; Song, X.; Rockwood, K. Operationalizing a frailty index from a standardized comprehensive geriatric assessment. J. Am. Geriatr. Soc. 2004, 52, 1929–1933.
- Mitnitski, A.B.; Mogilner, A.J.; Rockwood, K. Accumulation of deficits as a proxy measure of aging. Sci. World J. 2001, 1, 323–336.
- Anzueto, A.; Miravitlles, M. Pathophysiology of dyspnea in COPD. Postgrad. Med. 2017, 129, 366–374.
- Parshall, M.B.; Schwartzstein, R.M.; Adams, L.; Banzett, R.B.; Manning, H.L.; Bourbeau, J.; Calverley, P.M.; Gift, A.G.; Harver, A.; Laureau, S.C.; et al. An official American Thoracic Society statement: Update on the mechanisms, assessment, and management of dyspnea. Am. J. Respir. Crit. Care Med. 2012, 185, 435–452.
- O’Donnell, D.; Milne, K.M.; James, M.D.; de Torres, J.P.; Neder, J.A. Dyspnea in COPD: New mechanistic insights and management implications. Adv. Ther. 2020, 37, 41–60.
- Spruit, M.A.; Vercoulen, J.H.; Sprangers, M.A.G.; Wouters, E.F.M.; FAntasTIGUE consortium. Fatigue in COPD: An important yet ignored symptom. Lancet Respir. Med. 2017, 5, 542–544.
- Phillips, D.B.; Elbehairy, A.F.; James, M.D.; Vincent, S.G.; Milne, K.M.; de-Torres, J.P.; Neder, J.A.; Kirby, M.; Jensen, D.; Stickland, M.K.; et al. Impaired ventilatory efficiency, dyspnea, and exercise tolerance in Chronic Obstructive Pulmonary Disease: Results from the CanCOLD study. Am. J. Respir. Crit. Care Med. 2022, 205, 1391–1402.
- Hanania, N.A.; O’Donnell, D.E. Activity-related dyspnea in Chronic Obstructive Pulmonary Disease: Physical and psychological consequences, unmet needs, and fiuture directions. Int. J. Chron. Obstruct Pulmon Dis. 2019, 14, 1127–1138.
- Stridsman, C.; Müllerova, H.; Skär, L.; Lindberg, A. Fatigue in COPD and the impact of respiratory symptoms and heart disease—A population-based study. COPD 2013, 10, 125–132.
- American Thoracic Society. Surveillance for respiratory hazards in the occupational setting. Am. Rev. Respir. Dis. 1982, 126, 952–956.
- Bestall, J.C.; Paul, E.A.; Garrod, R.; Garnham, R.; Jones, P.W.; Wedzicha, J.A. Usefulness of the medical research council (MRC) dyspnoea scale as a measure of disability in patients with chronic obstructive pulmonary disease. Thorax 1999, 54, 581–586.
- Jones, P.W.; Harding, G.; Berry, P.; Wiklund, I.; Chen, W.H.; Kline Leidy, N. Development and first validation of the COPD Assessment Test. Eur. Respir. J. 2009, 34, 648–654.
- Hanania, N.A.; Müllerova, H.; Locantore, N.W.; Vestbo, J.; Watkins, M.L.; Wouters, E.F.M.; Rennard, S.I.; Sharafkhaneh, A.; Evaluation of COPD longitudinally to identify predictive surrogate endpoints (ECLIPSE) study investigators. Determinants of depression in the ECLIPSE chronic obstructive pulmonary disease cohort. Am. J. Respir. Crit. Care Med. 2011, 183, 604–611.
- Yohannes, A.M.; Baldwin, R.C.; Connolly, M.J. Mood disorders in elderly patients with Chronic Obstructive Pulmonary Disease. Rev. Clin. Gerontol. 2000, 10, 193–202.
- Pumar, M.I.; Gray, C.R.; Walsh, J.R.; Yang, I.A.; Rolls, T.A.; Ward, D.L. Anxiety and depression—Important psychological comorbidities of COPD. J. Thorac. Dis. 2014, 6, 1615–1631.
- Yohannes, A.M.; Alexolopoulos, G.S. Depression and anxiety in patients with COPD. Eur. Respir. Rev. 2014, 23, 345–349.
- Martinez Rivera, C.; Costan Galicia, J.; Alcázar Navarrete, B.; Garcia-Polo, C.; Ruiz Iturriaga, L.A.; Herrejon, A.; Ros Lucas, J.A.; Garcia-Sidro, P.; Tirado-Conde, G.; Lopez-Campos, J.L.; et al. Factors associated with depression in COPD: A multicenter study. Lung 2016, 194, 335–343.
- Rahi, M.S.; Thilagar, B.; Balaji, S.; Prabhakaran, S.Y.; Mudgal, M.; Rajoo, S.; Yella, P.R.; Satija, P.; Zagorulko, A.; Gunasekaran, K. The impact of anxiety and depression in Chronic Obstructive Pulmonary Disease. Adv. Respir. Med. 2023, 91, 123–134.
More
Information
Subjects:
Health Care Sciences & Services
Contributors
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
692
Revisions:
2 times
(View History)
Update Date:
27 Feb 2024
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





