Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Dongdong Qin | -- | 1456 | 2023-11-27 10:42:04 | | | |
| 2 | Fanny Huang | Meta information modification | 1456 | 2023-11-30 03:35:27 | | | | |
| 3 | Fanny Huang | Meta information modification | 1456 | 2023-11-30 03:40:28 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Jiang, C.; Zhou, Y.; Chen, R.; Yang, M.; Zhou, H.; Tang, Z.; Shi, H.; Qin, D. Nanomaterials Applied in the Treatment of Ischemic Stroke. Encyclopedia. Available online: https://encyclopedia.pub/entry/52086 (accessed on 07 February 2026).
Jiang C, Zhou Y, Chen R, Yang M, Zhou H, Tang Z, et al. Nanomaterials Applied in the Treatment of Ischemic Stroke. Encyclopedia. Available at: https://encyclopedia.pub/entry/52086. Accessed February 07, 2026.
Jiang, Chengting, Yang Zhou, Rong Chen, Mengjia Yang, Haimei Zhou, Zhengxiu Tang, Hongling Shi, Dongdong Qin. "Nanomaterials Applied in the Treatment of Ischemic Stroke" Encyclopedia, https://encyclopedia.pub/entry/52086 (accessed February 07, 2026).
Jiang, C., Zhou, Y., Chen, R., Yang, M., Zhou, H., Tang, Z., Shi, H., & Qin, D. (2023, November 27). Nanomaterials Applied in the Treatment of Ischemic Stroke. In Encyclopedia. https://encyclopedia.pub/entry/52086
Jiang, Chengting, et al. "Nanomaterials Applied in the Treatment of Ischemic Stroke." Encyclopedia. Web. 27 November, 2023.
Copy Citation
Ischemic stroke is a leading cause of death and disability in the world. At present, reperfusion therapy and neuroprotective therapy, as guidelines for identifying effective and adjuvant treatment methods, are limited by treatment time windows, drug bioavailability, and side effects. Nanomaterial-based drug delivery systems have the characteristics of extending half-life, increasing bioavailability, targeting drug delivery, controllable drug release, and low toxicity, thus being used in the treatment of ischemic stroke to increase the therapeutic effects of drugs.
ischemic stroke
nanomaterials
nanoparticles
drug delivery
1. Introduction
Ischemic stroke is a leading cause of death and disability in the world [1]. To date, the effective therapy for ischemic stroke is to restore cerebral blood flow via intravenous thrombolysis or mechanical thrombectomy [2]; however, the therapy is limited to narrow time widows [2], and even timely restoration of cerebral blood flow may not prevent long-term neurological deficits, because of secondary neuronal damage caused by reperfusion [3]. These damaging pathological processes (i.e., inflammation, oxidative stress, and excitotoxicity) persist in the brain during the acute stage and even in the sequelae stage [3]. Thus, targeting these pathological processes has great therapeutic prospects for neuroprotection to improve neuronal survival and outcomes after ischemic stroke.
At present, numerous neuroprotective drugs have been developed, but almost all failed in clinical translation [4]. There are some important explanations for this translational failure. On the one hand, it lies in the insufficient concentration of drugs that reach the ischemic area because of the limitations of the blood–brain barrier (BBB) [5]. Although a damaged BBB causes an increase in drug penetration during the acute stage of ischemic stroke, it will be closed again long after ischemic stroke [6]. On the other hand, faced with multiple pathological processes, i.e., inflammation, oxidative stress, and excitotoxicity, a single treatment option cannot salvage the ischemic penumbra. Thus, some researchers have developed drug conjugates with synergistic neuroprotection effects for targeting different pathological processes to reduce the damage of neurons to minimize the ischemic area [7][8]. Another important reason is that it is difficult for drugs to target specific damaged cells. There are many different types of cells, i.e., microglia, astrocytes, and neutrophils, involved in pathological processes, and targeting drug delivery to damaged cells may prevent the side effects of drugs [3]. Therefore, novel technologies that can target drug delivery to an intended area or cells, selectively release drugs, and increase the bioavailability of drugs are promising for the treatment of ischemic stroke.
Nanomaterial-based drug delivery systems have gradually been attracting attention in recent years because of their specific characteristics of targeting drug delivery, controllable drug release, biocompatibility, biodegradability, and low toxicity [9]. Recently, many studies have confirmed that nanomaterials can carry drug targets and cross the BBB, after which they can then conduct secondary targeted drug delivery, and then the drug is released to the damaged tissue and cells in ischemic stroke [10]. Therefore, nanomaterials have great prospects in optimizing the treatment of ischemic stroke. There are several reviews that have reviewed drug delivery systems based on thrombus, the brain–blood barrier (BBB), and ischemic brain parenchyma in ischemic stroke, as well as the different approaches for central nervous system (CNS) drug delivery [11][12][13][14].
2. The Pathogenesis of Ischemic Stroke
Ischemic stroke is a neurological disease characterized by cerebral vascular occlusion. Oxygen depletion, neuroinflammation, and oxidative stress are the main reasons for poor prognoses of ischemic stroke [3][15][16]. Following the interruption of cerebral blood flow, neurons in brain areas dominated by blocked blood vessels will experience hypoxia [15]. Oxygen depletion leads to the irreversible necrosis of neurons, after which a cerebral infarction core is formed [15]. In addition to neuronal necrosis, the BBB is disrupted in ischemic stroke [6]. The BBB is mainly composed of vascular endothelial cells, tight junction proteins (including claudin-5, occludin, and ZO-1), pericytes, and astrocytes [10]. In normal conditions, the BBB could prevent macromolecular substances and peripheral blood cells from entering the brain [10]. Within 120 h of reperfusion after focal cerebral ischemia, BBB permeability is significantly increased, and two peaks appear at 3 h and 72 h [17][18], resulting in leukocytes (i.e., neutrophils and monocytes) in peripheral blood and macromolecular substances entering the ischemic brain, thus further aggravating brain damage [6][19]. The infiltration and accumulation of leukocytes in cerebral ischemic areas depends on the function of adherent proteins expressed on neutrophils, such as integrin αMβ2, CD44, CD11b, macrophage-1 antigen (Mac-1), and lymphocyte function-associated antigen 1 (LFA-1) [20]. During ischemia and reperfusion, intercellular adhesion molecule-1 (ICAM-1), vascular cell adhesion molecule (VCAM)-1, and P-selectin are overexpressed on stressed vascular endothelial cells [6][21]. These molecules can drive leukocytes in peripheral blood to adhere to inflammatory vascular endothelial cells and enter cerebral ischemic areas via membrane-adherent proteins expressed on leukocytes [6][21]. The activation of resident microglia in the brain and the infiltration of leukocytes into the brain result in neuroinflammatory responses that further exacerbate neuronal death [6][22]. In fact, M1-microglia- and leukocyte-mediated neuroinflammatory responses will persist for 1 month after ischemic stroke, which is one of the main reasons for the poor prognoses of ischemic stroke [6][23]. Furthermore, the excessive production of reactive oxygen species (ROS) (i.e., H2O2, O2−, ·OH, and HOCI) after cerebral ischemia onset results in oxidative stress responses, which is also the leading reason for aggravated neuronal death [16][24][25]. Therefore, ensuring the supply of oxygen to the brain and inhibiting neuroinflammatory as well as oxidative stress responses are key to protecting neurons from death and saving ischemic penumbra in ischemic stroke. The abnormally expressed proteins and cells mentioned above may become therapeutic targets for ischemic stroke.
3. Nanomaterials Applied in the Treatment of Ischemic Stroke
Reperfusion through intravenous thrombolysis or mechanical thrombectomy is an effective method for treating ischemic stroke [2][26]; however, there is a strict time window limit [2][26]. Even if patients receive reperfusion treatment in time, it is difficult to avoid reperfusion injury after ischemic stroke [3][27]. Reperfusion injury is mainly caused by infiltrated leukocytes and overproduced oxygen radicals after a sudden increase in oxygen, thus resulting in no reflow of blood after the reperfusion of ischemic stroke, which can even worsen neuronal death [27]. Therefore, numerous neuroprotective drugs have been developed to prevent neuronal damage after reperfusion and extend the therapeutic time window to further improve ischemic stroke prognoses [28]. These neuroprotective drugs, such as those with anti-inflammatory and antioxidant stress effects, have been widely studied in animal and cell experiments, and their therapeutic effects have been confirmed in ischemic stroke models [28]; however, these neuroprotective drugs failed in clinical conversion [29][30]. The main reasons for their failure are attributed to an insufficient concentration of drugs in the ischemic brain and the quick elimination of drugs in peripheral blood. Their low absorption, poor bioavailability, poor targeting, and short half-lives result in insufficient concentrations of drugs in cerebral ischemic areas. In view of these limitations, nanomaterial-based drug delivery systems are widely applied in the treatment of ischemic stroke due to their specific properties of targeted drug delivery, controllable drug release, biocompatibility, biodegradability, and low toxicity [10][11][31]. Furthermore, nanoparticles could integrate multiple therapy approaches for ischemic stroke [7][32][33]; for example, Yuan fabricated a nanoparticle with the dual function of antioxidative and anti-inflammatory activities to target the treatment of ischemic stroke [7]. S. elongatus, a type of cyanobacteria, is encapsulated in nanoparticles and delivered to cerebral ischemic areas to generate oxygen and absorb carbon dioxide, thus rescuing neurons in the ischemic penumbra area [33]. In addition to delivering drugs to cerebral ischemic areas, leukocyte membrane-derived nanovesicles could inhibit the accumulation of neutrophils and monocytes in ischemic brain areas by consuming the binding sites with neutrophils or monocytes [34]. Therefore, it is essential to understand nanocarriers, the targeting mechanisms of nanoparticles, and drug release mechanisms to further improve the use of nanomaterials in the treatment of ischemic stroke. The possible function and mechanism of nanomaterial-based drug delivery systems in ischemic stroke are showed in Figure 1.
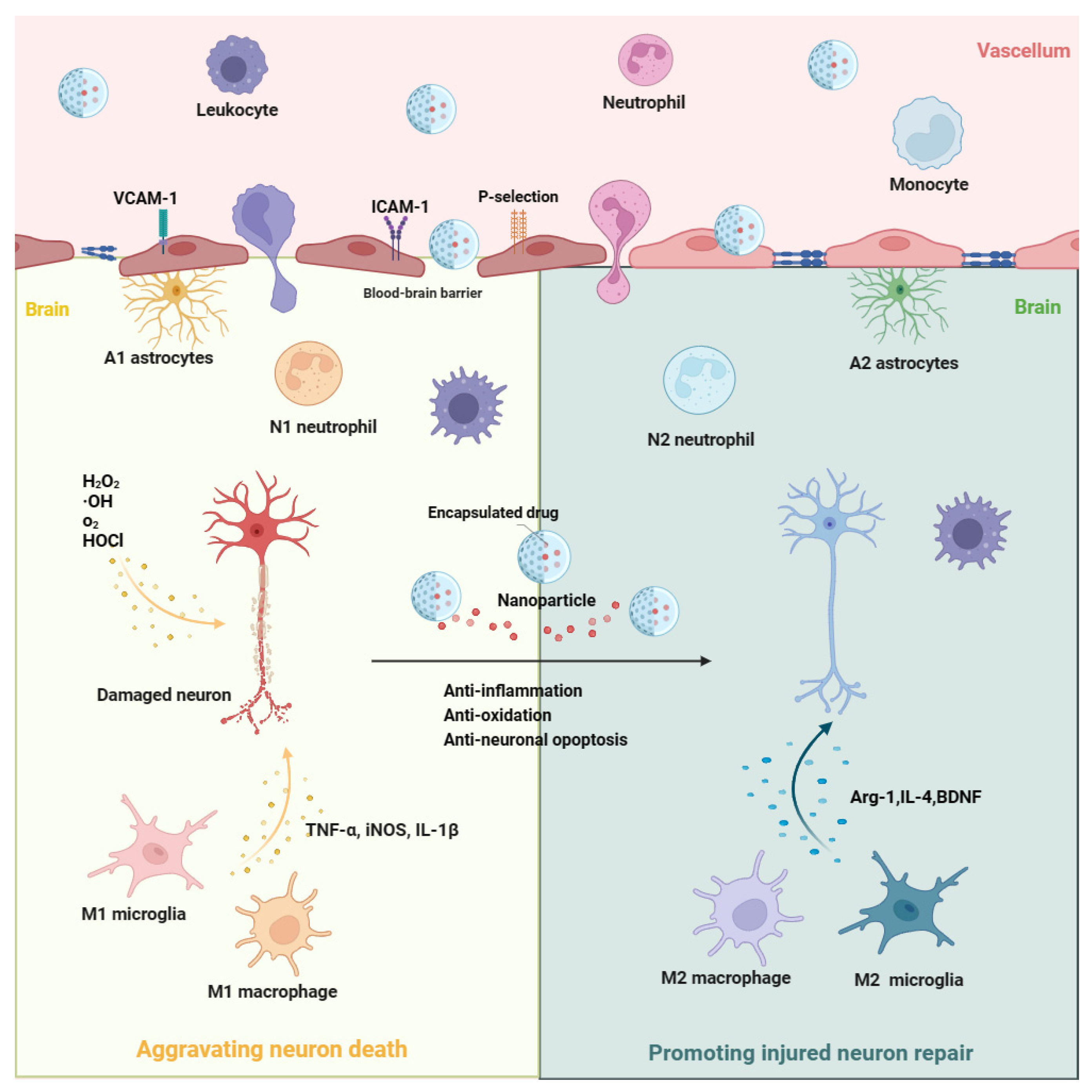
Figure 1. The possible function and mechanism of nanomaterial-based drug delivery systems in ischemic stroke. After ischemic stroke, M1 microglia and A1 astrocyte are rapidly activated in ischemic brain areas. In addition, leukocytes (including neutrophils and monocytes) in peripheral blood are recruited into the ischemic brain area. Among them, M1 microglia, A1 astrocyte, N1 neutrophils, and M1 macrophages would aggravate the neuron death through the overproduction of inflammatory molecules (i.e., TNF-α, iNOS, and IL-1β) and ROS (i.e., H2O2, O2−, ·OH, and HOCI). Based on the nanomaterial-based drug delivery systems, these harmful cell phenotypes may be shifted towards beneficial phenotypes (M2 microglia, A2 astrocyte, N2 neutrophils, and M2 macrophages) to exert the function of anti-inflammation, anti-oxidation, and anti-neuronal apoptosis, thus promoting injured neuron repair in ischemic stroke through the release of drugs or genes that are encapsulated in the nanoparticles. ICAM-1, intercellular adhesion molecule-1; VCAM-1, vascular cell adhesion molecule-1; H2O2, hydrogen peroxide; •OH, hydroxyl radicals; O2, oxygen; HOCl, hypochlorous acid; TNFα, tumor necrosis factor α; iNOS, inducible nitric oxide synthase; IL-1β, interleukin-1β; Arg-1, arginase-1; IL-4, interleukin-4; BDNF, brain-derived neurotrophic factor.
References
- GBD 2019 Stroke Collaborators. Global, regional, and national burden of stroke and its risk factors, 1990–2019: A systematic analysis for the Global Burden of Disease Study 2019. Lancet Neurol. 2021, 20, 795–820.
- Powers, W.J.; Rabinstein, A.A.; Ackerson, T.; Adeoy, O.M.; Bambakidis, N.C.; Becker, K.; Biller, J.; Hoh, B.; Jauch, E.C.; Kidwell, C.S.; et al. Guidelines for the Early Management of Patients with Acute Ischemic Stroke: 2019 Update to the 2018 Guidelines for the Early Management of Acute Ischemic Stroke: A Guideline for Healthcare Professionals from the American Heart Association/American Stroke Association. Stroke 2019, 50, e344–e418.
- Przykaza, L. Understanding the Connection Between Common Stroke Comorbidities, Their Associated Inflammation, and the Course of the Cerebral Ischemia/Reperfusion Cascade. Front. Immunol. 2021, 12, 782569.
- Tao, T.; Liu, M.; Chen, M.; Luo, Y.; Wang, C.; Xu, T.; Jiang, Y.; Guo, Y.; Zhang, J.H. Natural medicine in neuroprotection for ischemic stroke: Challenges and prospective. Pharmacol. Ther. 2020, 216, 107695.
- Kadry, H.; Noorani, B.; Cucullo, L. A blood-brain barrier overview on structure, function, impairment, and biomarkers of integrity. Fluids Barriers CNS 2020, 17, 69.
- Qiu, Y.M.; Zhang, C.L.; Chen, A.Q.; Wang, H.L.; Zhou, Y.F.; Li, Y.N.; Hu, B. Immune Cells in the BBB Disruption After Acute Ischemic Stroke: Targets for Immune Therapy? Front. Immunol. 2021, 12, 678744.
- Yuan, J.; Li, L.; Yang, Q.; Ran, H.; Wang, J.; Hu, K.; Pu, W.; Huang, J.; Wen, L.; Zhou, L.; et al. Targeted Treatment of Ischemic Stroke by Bioactive Nanoparticle-Derived Reactive Oxygen Species Responsive and Inflammation-Resolving Nanotherapies. ACS Nano 2021, 15, 16076–16094.
- Mei, T.; Kim, A.; Vong, L.B.; Marushima, A.; Puentes, S.; Matsumaru, Y.; Matsumnura, A.; Nagasaki, Y. Encapsulation of tissue plasminogen activator in pH-sensitive self-assembled antioxidant nanoparticles for ischemic stroke treatment—Synergistic effect of thrombolysis and antioxidant. Biomaterials 2019, 215, 119209.
- Diez-Pascual, A.M.; Rahdar, A. Functional Nanomaterials in Biomedicine: Current Uses and Potential Applications. ChemMedChem 2022, 17, e202200142.
- Xie, J.; Shen, Z.; Anraku, Y.; Kataoka, K.; Chen, X. Nanomaterial-based blood-brain-barrier (BBB) crossing strategies. Biomaterials 2019, 224, 119491.
- Ma, H.; Jiang, Z.; Xu, J.; Liu, J.; Guo, Z.N. Targeted nano-delivery strategies for facilitating thrombolysis treatment in ischemic stroke. Drug Deliv. 2021, 28, 357–371.
- Zhang, S.; Zhou, Y.; Li, R.; Chen, Z.; Fan, X. Advanced drug delivery system against ischemic stroke. J. Control. Release 2022, 344, 173–201.
- Nozohouri, S.; Sifat, A.E.; Vaidya, B.; Abbruscato, T.J. Novel approaches for the delivery of therapeutics in ischemic stroke. Drug Discov. Today 2020, 25, 535–551.
- He, W.; Zhang, Z.; Sha, X. Nanoparticles-mediated emerging approaches for effective treatment of ischemic stroke. Biomaterials 2021, 277, 121111.
- Liu, S.; Shi, H.; Liu, W.; Furuichi, T.; Timmins, G.S.; Liu, K.J. Interstitial pO2 in ischemic penumbra and core are differentially affected following transient focal cerebral ischemia in rats. J. Cereb. Blood Flow. Metab. 2004, 24, 343–349.
- Zhang, M.; Wang, Z.; Wang, C.; Wu, Y.; Li, Z.; Liu, Z. Visualizing Oxidative Stress Level for Timely Assessment of Ischemic Stroke via a Ratiometric Near-Infrared-II Luminescent Nanoprobe. ACS Nano 2021, 15, 11940–11952.
- Jiao, H.; Wang, Z.; Liu, Y.; Wang, P.; Xue, Y. Specific role of tight junction proteins claudin-5, occludin, and ZO-1 of the blood-brain barrier in a focal cerebral ischemic insult. J. Mol. Neurosci. 2011, 44, 130–139.
- Yang, Y.; Estrada, E.Y.; Thompson, J.F.; Liu, W.; Rosenberg, G.A. Matrix metalloproteinase-mediated disruption of tight junction proteins in cerebral vessels is reversed by synthetic matrix metalloproteinase inhibitor in focal ischemia in rat. J. Cereb. Blood Flow. Metab. 2007, 27, 697–709.
- Kang, L.; Yu, H.; Yang, X.; Zhu, Y.; Bai, X.; Wang, R.; Cao, Y.; Xu, H.; Luo, H.; Lu, L.; et al. Neutrophil extracellular traps released by neutrophils impair revascularization and vascular remodeling after stroke. Nat. Commun. 2020, 11, 2488.
- Jickling, G.C.; Liu, D.Z.; Ander, B.P.; Stamova, B.; Zhan, X.; Sharp, F.R. Targeting neutrophils in ischemic stroke: Translational insights from experimental studies. J. Cereb. Blood Flow. Metab. 2015, 35, 888–901.
- Kolaczkowska, E.; Kubes, P. Neutrophil recruitment and function in health and inflammation. Nat. Rev. Immunol. 2013, 13, 159–175.
- Xiong, X.Y.; Liu, L.; Yang, Q.W. Functions and mechanisms of microglia/macrophages in neuroinflammation and neurogenesis after stroke. Prog. Neurobiol. 2016, 142, 23–44.
- Jiang, C.T.; Wu, W.F.; Deng, Y.H.; Ge, J.W. Modulators of microglia activation and polarization in ischemic stroke (Review). Mol. Med. Rep. 2020, 21, 2006–2018.
- Allen, C.L.; Bayraktutan, U. Oxidative Stress and Its Role in the Pathogenesis of Ischaemic Stroke. Int. J. Stroke 2009, 4, 461–470.
- Liu, Y.; Wang, X.; Li, X.; Qiao, S.; Huang, G.; Hermann, D.M.; Doeppner, T.R.; Zeng, M.; Liu, W.; Xu, G.; et al. A Co-Doped Fe3O4 Nanozyme Shows Enhanced Reactive Oxygen and Nitrogen Species Scavenging Activity and Ameliorates the Deleterious Effects of Ischemic Stroke. ACS Appl. Mater. Interfaces 2021, 13, 46213–46224.
- Kleindorfer, D.O.; Towfighi, A.; Chaturvedi, S.; Cockroft, K.M.; Gutierrez, J.; Lombardi-Hill, D.; Kamel, H.; Kernan, W.N.; Kittner, S.J.; Leira, E.C.; et al. 2021 Guideline for the Prevention of Stroke in Patients with Stroke and Transient Ischemic Attack: A Guideline from the American Heart Association/American Stroke Association. Stroke 2021, 52, e364–e467.
- Jurcau, A.; Ardelean, I.A. Molecular pathophysiological mechanisms of ischemia/reperfusion injuries after recanalization therapy for acute ischemic stroke. J. Integr. Neurosci. 2021, 20, 727–744.
- Paul, S.; Candelario-Jalil, E. Emerging neuroprotective strategies for the treatment of ischemic stroke: An overview of clinical and preclinical studies. Exp. Neurol. 2021, 335, 113518.
- Narayan, S.K.; Cherian, S.G.; Phaniti, P.B.; Chidambaram, S.; Vasanthi, A.H.R.; Arumugam, M. Preclinical animal studies in ischemic stroke: Challenges and some solutions. Anim. Model. Exp. Med. 2021, 4, 104–115.
- Gaire, B.P. Herbal Medicine in Ischemic Stroke: Challenges and Prospective. Chin. J. Integr. Med. 2018, 24, 243–246.
- Villanueva-Flores, F.; Castro-Lugo, A.; Ramírez, O.T.; Palomares, L.A. Understanding cellular interactions with nanomaterials: Towards a rational design of medical nanodevices. Nanotechnology 2020, 31, 132002.
- Li, C.; Zhao, Z.; Luo, Y.; Ning, T.; Liu, P.; Chen, Q.; Chu, Y.; Guo, Q.; Zhang, Y.; Zhou, W.; et al. Macrophage-Disguised Manganese Dioxide Nanoparticles for Neuroprotection by Reducing Oxidative Stress and Modulating Inflammatory Microenvironment in Acute Ischemic Stroke. Adv. Sci. 2021, 8, e2101526.
- Wang, J.; Su, Q.; Lv, Q.; Cai, B.; Xiaohalati, X.; Wang, G.; Wang, Z.; Wang, L. Oxygen-Generating Cyanobacteria Powered by Upconversion-Nanoparticles-Converted Near-Infrared Light for Ischemic Stroke Treatment. Nano Lett. 2021, 21, 4654–4665.
- Wang, Y.; Wang, Y.; Li, S.; Cui, Y.; Liang, X.; Shan, J.; Gu, W.; Qiu, J.; Li, Y.; Wang, G. Functionalized nanoparticles with monocyte membranes and rapamycin achieve synergistic chemoimmunotherapy for reperfusion-induced injury in ischemic stroke. J. Nanobiotechnol. 2021, 19, 331.
More
Information
Subjects:
Neurosciences
Contributors
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
469
Revisions:
3 times
(View History)
Update Date:
30 Nov 2023
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No




