Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Nikolay Zahariev | -- | 7155 | 2023-08-01 09:00:15 | | | |
| 2 | Camila Xu | Meta information modification | 7155 | 2023-08-01 09:12:27 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Zahariev, N.; Katsarov, P.; Lukova, P.; Pilicheva, B. Novel Fucoidan Pharmaceutical Formulations and Their Potential Application. Encyclopedia. Available online: https://encyclopedia.pub/entry/47472 (accessed on 03 June 2026).
Zahariev N, Katsarov P, Lukova P, Pilicheva B. Novel Fucoidan Pharmaceutical Formulations and Their Potential Application. Encyclopedia. Available at: https://encyclopedia.pub/entry/47472. Accessed June 03, 2026.
Zahariev, Nikolay, Plamen Katsarov, Paolina Lukova, Bissera Pilicheva. "Novel Fucoidan Pharmaceutical Formulations and Their Potential Application" Encyclopedia, https://encyclopedia.pub/entry/47472 (accessed June 03, 2026).
Zahariev, N., Katsarov, P., Lukova, P., & Pilicheva, B. (2023, August 01). Novel Fucoidan Pharmaceutical Formulations and Their Potential Application. In Encyclopedia. https://encyclopedia.pub/entry/47472
Zahariev, Nikolay, et al. "Novel Fucoidan Pharmaceutical Formulations and Their Potential Application." Encyclopedia. Web. 01 August, 2023.
Copy Citation
Fucoidan belongs to a family of sulfated, L-fucose-rich polysaccharides found in the cell wall matrix of various species of marine brown algae (Phaeophyta: Laminariaceae, Fucaceae, Chordariaceae and Alariaceae). Fucoidan can also be obtained from sea cucumbers (Holothuroidea: Stichopodidae, Holothuriidae), sea urchin eggs (Echinoidea: Strongylocentrotidae, Arbaciidae) and sea grasses (Cymodoceaceae).
polysaccharides
fucoidan
biological activities
micro- and nanoparticles
1. Introduction
Cancer is one of the major causes of death worldwide. The possible complications during therapy, which can be due to inadequate biodistribution of chemotherapeutics in the organism, should not be underestimated. Current pharmaceutical technology aims at developing drug delivery systems with improved biodistribution of the chemotherapeutics, reduced therapy-related side effects and toxicity and therefore improving the therapeutic efficacy. In recent years the rapid development of micro- and nanotechnologies has led to the formulation of innovative drug systems, which take their place in contemporary oncological therapeutic approaches. Much of the research nowadays is focused on the utilization of natural polymers such as polysaccharides, proteins and lipids as drug carriers for chemotherapeutic agents. Biopolymers are preferred materials for developing drug formulations due to their biocompatibility, biodegradability, low toxicity and low immunogenicity [1]. Natural polymers can be conjugated with specific ligands leading to the formation of pharmaceutical systems with improved functional properties and targeted drug delivery. Some biopolymers possess biological activities and, in addition to being carriers, they can also show a synergistic therapeutic effect with the incorporated active substances [2]. Marine polysaccharides, more specifically, have recently been an object of great scientific interest due to their unique structural and physicochemical properties. Fucoidan is a sulfated polysaccharide which is mainly extracted from brown seaweed. Depending on their origin and type of extraction, fucoidans have different molecular weights and degrees of sulfation, which can affect the biological effects of the polysaccharide and the characteristics of its formulations [1][2][3]. Recently the application of fucoidan in the field of pharmaceutical technology has been widely investigated. This polysaccharide plays an important role as a drug carrier for the formulation of various drug delivery systems, especially as a biopolymer with anticancer activity, used for targeted delivery of chemotherapeutics in oncology [4]. The polymer is characterized with easy structure-forming properties and can be used as a single carrier or in combination with other polymers for the formulation of innovative anticancer strategies with improved therapeutic efficacy, including micro- and nano-sized drug delivery systems.
2. Fucoidan Sources and Chemical Structure
Fucoidan belongs to a family of sulfated, L-fucose-rich polysaccharides found in the cell wall matrix of various species of marine brown algae (Phaeophyta: Laminariaceae, Fucaceae, Chordariaceae and Alariaceae). Fucoidan can also be obtained from sea cucumbers (Holothuroidea: Stichopodidae, Holothuriidae), sea urchin eggs (Echinoidea: Strongylocentrotidae, Arbaciidae) and sea grasses (Cymodoceaceae) [5]. Depending on the extracted species, growth environment and extraction method, fucoidan exhibits different structure and molecular weight (Table 1) [6].
Table 1. Structural characteristics of fucoidan extracted from different types of brown seaweeds.
| Brown Seaweed | Structure | Reference |
|---|---|---|
| Fucus evanescens | Main chain of (1→3)-and (1→4)-α-L-Fucp highly substituted by sulfate groups at O2 and/or O3 positions | [6] |
| Fucus seratus | Main chain of (1→3)-and (1→4)-α-L-Fucp with short branches of α-L-Fucp-(1→4)-α-L-Fucp and α-L-Fucp-(1→3)-α-L-Fucp in O4 of α-(1→3)-L-Fucp and sulfate groups in O2 and/or O4 positions | [7] |
| Chorda filum | Main chain of (1→3)-α-L-Fucp highly ramified at O2 by terminal residues and substituted by sulfate groups at O2 and/or O4 positions. | [7] |
| Fucus distichus | [(1→3)-α-L-Fucp-(2,4-di-SO3-)-(1→4)- α-L-Fucp -(2SO3-)-(1→]n | [8] |
| Undaria pinnatifida | Backbone structure of (1→3):(1→4)-O-glycosidic bonds | [9] |
| Ascophyllum nodosum | [(1→3)-α-L-Fuc-(2SO3-)-(1→4)- α-L-Fuc-(2,3-di-SO3-)-(1→]n | [10] |
| Laminaria saccharina | Main chain of (1→3)-α-L-Fucp branched at O2 and O4 of α-L-Fucp by terminal residues and sulfate groups | [11] |
Over 90% of the total sugar content in fucoidan consists of the deoxyhexose L-fucose [11]. Along with fucose, other monosaccharides can be found in the structure of fucoidan: galactose, glucose, xylose, mannose, rhamnose, arabinose, uronic acid and acetyl groups [12][13]. Although the structure and composition of fucoidans differ depending on the species from which they originate, fucoidans can be categorized into two main types according to their monomeric subunits (Figure 1). Type I fucoidan is composed of α-(1→3)-α-L-fucopyranose backbone linked to sulfate radicals at the C2 and C4 position, while type II fucoidan is composed of α-(1→3)- and α-(1→4)-α-L-fucopyranose backbone, with sulfate radicals attached at C2, C3 and C4 positions [12][13][14].
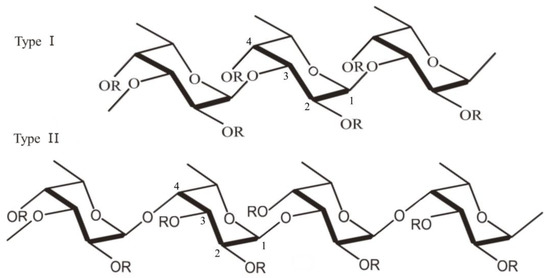
Figure 1. Structure of fucoidan: α-(1→3)-α-L-fucopyranose backbone linked to sulfate radicals at the C2 and C4 position (Type I) and α-(1→3)- and α-(1→4)-α-L-fucopyranose backbone, with sulfate radicals attached at C2, C3 and C4 positions (Type II) (the figure was generated using Microsoft Office Professional 2021 and ChemDraw Pro Software).
It was found that one species of brown algae could produce several types of fucoidan differing in their fucose, aldose, uronic acids, acetyl groups and sulfate content. Zhao et al. for example reported the extraction of four types of fucoidan from Laminaria japonica, which showed different antioxidant activity, depending on sulfate content and monosaccharide composition [15]. The polysaccharide sulfate content and degree of sulfation may vary among species, and it is highly dependent on the season of harvest. A study conducted by Fletcher et al. reported that the sulfate content of fucoidan from Saccharina longicruris increased between March and November, while a decrease was observed between November and June [16].
The molecular weights of fucoidans can range from 10 kDa to 10,000 kDa depending on the fucoidan source and extraction method. According to their molecular weight fucoidans can be categorized as: low molecular weight fucoidans (LMWF)—Mw below 10 kDa, medium molecular weight fucoidans (MMWF)—Mw between 10 and 10,000 kDa and high molecular weight fucoidans (HMWF)—Mw above 10,000 kDa [17][18].
The difference in the chemical content of fucoidans could influence their biological activity. The anticancer effect of fucoidan is strongly dependent on the polymer molecular weight [19]. Some studies report that after oral administration low-molecular-weight fucoidan is more effective compared to the HMW fractions of the polysaccharide. The reduced molecular weight facilitates the polymer intestinal absorption and the consequent expression of its activity against different cancer types, while the HMW fucoidans are effective mainly in the gastrointestinal tract [20]. According to some authors, LMW fucoidan from Cladosiphon navaecaledoniae induces apoptosis in breast cancer cell lines [21]. Other authors stated that treating bladder cancer cell lines with LMW fucoidan from Sargassum hemiphyllum inhibited angiogenesis through downregulation of the HIF-1a/VEGF signaling pathway [22]. Similar results were obtained in a study conducted on mice with induced bladder cancer treated with LMW fucoidan and chemotherapeutic agents (gemcitabine and cisplatin) [23]. According to other authors HMW fucoidan had inhibitory effect over angiogenesis while the LMW polysacharide demonstrated proangiogenic effect [24][25][26]. Furthermore, research conducted on human colon cancer cell line HCT116 using LMW fucoidan showed G1 triggered arrest and apoptosis via the p53-indipendent mechanism [27]. LMW fucoidan was also reported to induce autophagy in human stomach cancer cells (AGS cells) via microtubule-associated protein light chain 3-I transition and accumulation of beclin-1, leading to increased apoptosis [28].
Besides molecular weight, the extraction method is another essential factor which can influence fucoidan bioactivities. Generally, fucoidan is isolated through acidic hydrolysis, however this technique leads to the production of less branched fucoidan chains, which are characterized with lower bioavailability [29]. The sulfate content and the position of the sulfate groups in the polymer chain are also important for fucoidan activities [30]. For example, fucoidan extracted from Sargassum fusiforme with low sulfate content (7.5%), showed lower inhibition of HMEC-1 cells angiogenesis, compared to a polysaccharide with higher sulfate content (20.8%) [31]. The same tendency was reported for fucoidan extracted from Fucus vesiculosus [32]). The highly sulfated fucoidan showed higher antiproliferative effect on breast cancer cells [33].
The route of administration is also a basic factor, influencing fucoidan pharmacokinetics and therapeutic effects. Authors reported limited absorption of the polysaccharide and low plasma concentration after oral administration [34]. HMW fucoidan was reported to remain longer in the blood circulation, compared to LMW polysaccharide, which was quickly eliminated [35]. According to research conducted on rats, intragastric administration of fucoidan from Fucus vesicolosus resulted in maximum plasma concentration within four hours [36]. Tokita et al. studied the polysaccharide pharmacokinetics after a single oral administration of 1 g fucoidan by human volunteers. The results showed a maximum plasma concentration 6 or 9 h after administration [37]. Some studies have reported priority distribution of fucoidan in certain organs such as liver and kidneys [38]. There are also studies demonstrating good skin-penetrating properties of fucoidan after topical application, linear pharmacokinetics (dose applied 50–150 mg/kg) and prolonged half-life after topical delivery resulting in deposition of fucoidan in the skin 60 min after administration [39]. The type of pharmaceutical formulation could also influence the pharmacokinetics of fucoidan. According to Kimura et al., encapsulation of fucoidan in nanoparticles could elevate its cytotoxic activity and this result is related at least partially to increased permeability [40].
3. Fucoidan Biological Activities and Anticancer Mechanisms
Due to its specific structure and composition, fucoidan has attracted the attention of researchers as a promising therapeutic agent and an excipient in various pharmaceutical formulations. Depending on the sulfate content and molecular weight, fucoidans show several biological effects: antioxidant [41][42][43][44], antibacterial [45][46][47][48][49][50], antiviral [51][52][53][54], anticoagulant [55][56], hypolipidemic [57], hypoglycemic [58][59], antitumor [60][61][62][63][64][65][66][67], anti-inflammatory and immunomodulatory activities [68][69][70] (Figure 2, Table 2 and Table 3). Although there are numerous publications and reports on the use of fucoidan as a therapeutic agent and carrier for drug delivery systems, no pharmaceutical dosage form containing fucoidan has been approved and released on the market so far. However, fucoidan is widely used in cosmetics, functional foods and supplements for anti-inflammatory, musculoskeletal, cardiovascular and gastrointestinal disorders.
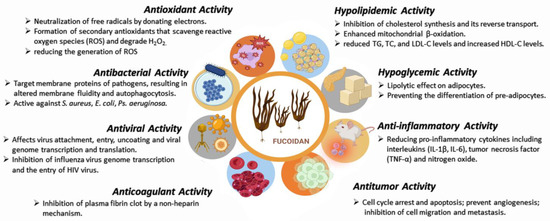
Figure 2. Fucoidan biological activities (created with Microsoft Office Professional 2021).
Table 2. In vitro biological activities of fucoidan.
| Activity | Dose, µg/mL | Source | Cell Lines | Data Obtained | Reference |
|---|---|---|---|---|---|
| Antioxidant | 1 | S. japonica | - | DPPH radical and ABTS+ radical scavenging activity |
[71] |
| Anti- inflammatory |
0.1–100 | S. sagamianum | LPS-induced RAW 264.7 cells |
Inhibition of NO, IL-6, IL-1β, TNF-α, iNOS, COX-2, NF-κB p65 |
[72] |
| Anti- inflammatory |
1–300 | G. pacificum | LPS-induced THP-1 cells |
Protected the THP-1 cells against LPS-stimulated cytotoxicity |
[73] |
| Anti- inflammatory |
3–25 | S. japonica | LPS-induced RAW 264.7 cells |
Decreased production of NO and TNF-α, IL-1β and IL-6. |
[74] |
| Anti- inflammatory |
25–100 | C. minima | LPS-induced RAW 264.7 cells |
Inhibition of NO production and expression of PGE2 |
[75] |
| Antiviral | 10–1000 | L. japonica | Vero E6 cell line from mouse macrophage | Reduced number of infected cells | [76] |
| Antiviral | 50–100 | H. elongata | Vero cell line from African green monkey | Inhibition of Herpes simplex virus type 1 intracellular replication |
[77] |
| Hypoglycemic | 0.5–5 | L. japonica | Cell α-glucosidase | α-glucosidase inhibitory activity | [78] |
| Immuno- modulatory |
5–125 | S. fusiforme | B lymphocytes | Promote LPS-induced spleen lymphocyte proliferation |
[79] |
| Anticancer | 25–100 | S. coreanum | HL-60, CT-26, B-16 and HeLa cell model | Cell apoptosis and activation of caspase-3 and cleavage of poly(ADP-ribose) polymerase | [80] |
| Anticancer | 120 | F. vesiculosus | HeLa G-63, Hep G2 and Chang liver cells model | Inhibition of cell proliferation | [81] |
| Anticancer | 10–500 | U. pinnatifida | Sarcomas and carcinosarcoma cell lines | Induced apoptosis | [82] |
| Anticancer | 0.05–100 | B. fuscopurpurea | Ovarian cancer cells | Inhibition of A2780, COC1, SKOV3, HO-8910 and OVCAR3 ovarian cancer cells proliferation | [83] |
Table 3. In vivo tests, performed with fucoidan from different sources.
| Effect | Dose | Source | Tested Model | Reported Results | Reference |
|---|---|---|---|---|---|
| Anticancer | 5 g/kg p.o. |
C. okamuranus | Mice with induced colon cancer |
Significantly suppressed tumor growth | [84] |
| Anticancer | 5 mg/kg i.p. |
F. vesicolosus | Mice with induced breast cancer |
Inhibition of angiogenesis and induction of apoptosis |
[85] |
| Anticancer | 200 mg/kg i.p. |
- | Mice with induced hepatocellular carcinoma |
Inhibition of cancer cells proliferation |
[86] |
| Anticancer | 0.25 mg/day i.v. |
F. vesicolosus | Mice with induced breast cancer |
Cancer metastasis prevention |
[87] |
| Anticancer | 75 mg/kg p.o. |
S. plagiophyllum | Mice with induced hepatocellular carcinoma |
Inhibition of carcinogen metabolism |
[88] |
| Anticancer | 100 mg/kg p.o. |
C. okamuranus | Mice with induced sarcoma |
Tumor growth reduction by NO produced by macrophages | [89] |
| Immuno- modulatory |
10 mg/kg i.v. |
- | Rabbits with induced bacterial meningitis |
Decreased influx of leukocytes into the cerebrospinal fluid | [90] |
| Immuno- modulatory |
50 mg/kg i.v. |
- | Mice with L-selectin deficient |
Mobilization of hematopoietic progenitor stem cells | [91] |
| Immuno- modulatory |
25 mg/kg i.v. |
F. vesiculosus | Rats with induced myocarditis |
Inhibition of extravasation of macrophages and CD4+ T cells | [92] |
| Immuno- modulatory |
200 mg/kg p.o. |
- | Mice with induced leishmania infection |
Th1 switch in Leishmania infection |
[93] |
| Immuno- modulatory |
20 mg/kg i.p. |
F. vesiculosus | Mice | Increased levels of TNF-α and IL-6 in spleens and blood serum | [94] |
| Immuno- modulatory |
20 mg/kg p.o. |
U. pinnatifida | Mice with induced herpes simplex |
Increased activity of NK cells | [95] |
| Immuno- modulatory |
50 mg/kg i.p. |
M. pyrifera | Mice | Increased maturation and activation of NK cells |
[96] |
| Immuno- modulatory |
500 mg/kg p.o. |
U. pinnatifida | UVB-irradiated mouse skin |
Lowered IFN-γ levels after irradiation; reduced skin edema |
[97] |
| Anti- inflammantory |
25 mg/kg i.v. |
F. vesiculosus | Mice with induced pancreatitis |
Decreased levels of IL-1β, TNF-α and myeloperoxidase | [98] |
| Anti- inflammantory |
10–400 mg/kg p.o./i.p. |
F. vesiculosus | Mice with induced acute colitis |
Decreased levels of IL-1α, IL-1β and IL-10 | [99] |
| Anti- inflammantory |
50–100 mg/kg p.o. |
L. japonica | Mice with induced liver damage |
Reduced levels of TNF-α, IL-1β and IL-6 | [100] |
| Anti- inflammantory |
100 mg/kg p.o. |
L. japonica | Mice with induced diabetes melitus |
Reduced blood glucose level and serum levels of IL-1β, IL-6, TNF-α | [101] |
| Anti- inflammantory |
50–200 mg/kg p.o. |
L. japonica | Mice with induced myocarditis |
Decreased levels of TNF- α and IL-6; increased levels of IL-10 | [102] |
| Anti- inflammantory |
50–200 mg/kg p.o. |
S. muticum | Mice with induced rheumatoid arthritis |
Decreased levels of TNF-α, IFN-γ and IL-6 |
[103] |
| Anti- inflammantory |
- | C. okamuranus | Mice with induced chronic colitis |
Decreased levels of IL-6 and increased levels of IL-10 | [75] |
| Anti- inflammantory |
12.5–50 μg/mL | C. minima | Zebrafish embryos |
Decreased production of NO, ROS, COX-2, iNOS | [104] |
| Anti- inflammantory |
300 mg/mL p.o. |
U. pinnatifida | Mice with induced rheumatoid arthritis |
Reduced cartilage and bone destruction and inflammation | [105] |
| Anti- inflammantory |
2.5–300 mg/kg p.o. |
T. ornata | Rats with induced arthritis |
Decreased levels of TNF-α, IL-6 and PGE2 |
[106] |
| Anti- inflammantory |
50 mg/kg p.o. |
T. ornata | Mice with paw edema |
Reduced the expression of genes of COX-2, IL-1β, the NF-κB signaling pathway | [107] |
As mentioned above, fucoidan is a marine polysaccharide that is characterized by direct and indirect anticancer activity towards cancer cells (Table 4). Furthermore, the polymer possesses high biocompatibility and low toxicity which makes it a suitable adjuvant in cancer treatment [108]. Several mechanisms have been described in the literature regarding the antitumor effect of fucoidan, such as effect on the cell cycle and apoptosis [109], angiogenesis [110], cell migration and metastasis [111] and immunomodulatory anticancer activity [112] (Figure 3).
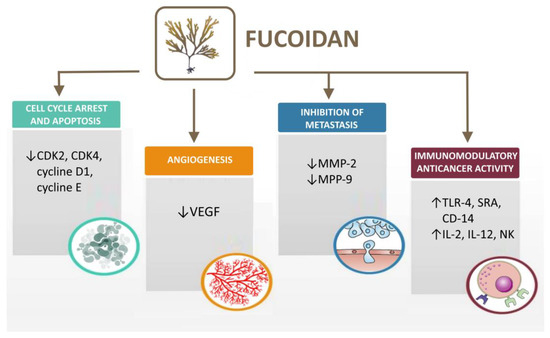
Figure 3. Mechanisms of fucoidan antitumor activity (created with Microsoft Office Professional 2021).
3.1. Cell Cycle Arrest and Apoptosis
There are many studies on the ability of fucoidan to affect cancer cells proliferation by arresting the G1 phase of the cell cycle and reducing CDK2, CDK4 and cyclins D1 and E. Regarding the antitumor activity, one of the most thoroughly studied fucoidans are those isolated from Fucus vesicolosus. There have been several reports on the use of that fucoidan against different types of tumors including lymphoma, gastric, colon, liver and bladder cancers [27][113][114]. Regarding its effect on cell apoptosis, fucoidan induces programmed cell death by both intrinsic and extrinsic pathways [115]. Studies by Zue et al. and Zhang et al. showed that fucoidan promoted apoptosis in hepatocellular carcinoma and MCF-7 breast cancer in dose-dependent manner [86][116]. Furthermore, research by Li et al. revealed that not only did fucoidan not induce apoptosis in healthy cells but it also protected them by preventing programmed cell death [117].
3.2. Fucoidan Effects on Angiogenesis
Most tumors are characterized by uncontrolled and intensive angiogenesis and rapid cell proliferation. There are several reports regarding the capability of fucoidan to prevent angiogenesis. Moreover, fucoidan is reported to possess proangiogenic effect on tumors. Some authors state that the antiangiogenic effect is related to the decrease in the expression of endothelial growth factor (VEGF) [85], but others report that fucoidan increases the expression of VEGF [110]. A literature review published in 2014 summarized that the effect of fucoidan on tumor angiogenesis was dependent on the polysaccharide molecular weight [118]. High molecular weight fucoidans show antiangiogenic effect [119], while low molecular weight fucoidans demonstrate proangiogenic effect on tumors [110]. Furthermore, it has been demonstrated that not only the molecular weight, but also the degree of sulfation, had a significant role for fucoidan angiogenic activity. The more sulfated the fucoidans, the stronger the angiogenic effect [37][120].
3.3. Inhibition of Cell Migration and Metastasis
Most cancer deaths are due to metastases of cancer cells to other organs. The main mechanism of the process involves detachment of cells from the primary tumor, intravasation into blood or lymph vessels, and extravasation in other organs. Crucial to cell detachment is the process of extracellular matrix degradation, which is regulated by metalloproteinases (MPP). Fucoidan has been reported to inhibit MMP-2 and MPP-9 [121][122]. A study conducted by Cho et al. demonstrated that fucoidan inhibited metastasis in A549 human lung cancer cell line in a dose-dependent manner. Treatment of bladder cancer cells (5637) with fucoidan resulted in inhibition of cell migration by reducing MMP-9 expression [122].
3.4. Immunomodulatory Anticancer Activity
Studies on the immunomodulatory anticancer activity of fucoidan suggest that acetylated fucoidan induces macrophage activation through glycoprotein surface membrane receptors, such as Toll-like receptor-4 (TLR-4), scavenger receptor class A (SRA) and cluster of differentiation-14 (CD-14) [123]. Macrophage activation leads to the production of various interleukins such as IL-2 and IL-12, which further activate NK-cell-mediated apoptosis in cancer cells. A study by Zhang et al. showed that the immunomodulatory activity of fucoidan depended on the uronic acid content of the polysaccharide. Fucoidan from Ascophyllum nodosum with higher uronic acid content demonstrated a stronger effect on the immune system, compared to fucoidan extracted from Fucus vesicolosus with lower uronic acid content [123].
Table 4. Anticancer activity of Fucoidan from different sources.
| Fucoidan Source |
Dose µg/mL |
Cancer Type/ Cell Line |
Data Obtained |
Reference |
|---|---|---|---|---|
| Saccharina | 50 | Colon cancer, DLD-1; Brest cancer, T-47D |
Cell proliferation inhibition; Inhibition of EGF receptor binding. |
[124] |
| Sargassum | 200 | Hepatic carcinoma, Huh6, Huh7, SK-Hep1 and HepG2 | Cell proliferation inhibition via TGF-β R1, 2 ↓ Phospho-Smad2/3↓ Smad 4 protein ↓ | [37] |
| Sargassum | 100 | Colon cancer, DLD-1 | Cell proliferation inhibition; Inhibition of the formation of cytotoxic colony. |
[125] |
| F. vesiculosus | 20 | Colon cancer, HT-29 HCT-116 |
Induced apoptosis via caspase-8, 9, 7, 3 activation PARP, Bak, Bid, Fas ↑, survivin, XIAP ↓. | [126] |
| F. vesiculosus | 1000 | Colon cancer, HT-29 | Cell proliferation inhibition and induced cell apoptosis (↓Ras/Raf/ERK proteins). | [127] |
| F. vesiculosus | 300 | Brest cancer, MCF-7 | Induced cell apoptosis via Caspase-8 activation Cytochrome C, Bax ↑ Bcl-2 ↓ Release of APAf-1 ↑. | [32] |
| F. vesiculosus | 90–120 | Brest cancer, MDA-MB-231 | Cell proliferation inhibition via expression of phosphorylated Smad2,3 and Smad4 inhibition. | [128] |
| F. vesiculosus | 50–400 | Lung cancer, Lewis lung carcinoma cells |
Inhibition of metastasis via inhibition of VEGF and MMPs. |
[129] |
| F. vesiculosus | 400 | Lung cancer, A549 | Cell proliferation inhibition and induced cell apoptosis via Caspase-3 ↑ and PARP cleavage. | [130] |
| F. vesiculosus | 1000 | Hepatic carcinoma, Huh-7, SNU-761, SNU-3085 |
Cell proliferation inhibition via Caspase-7, -8, -9 ↑. |
[131] |
| F. vesiculosus | 100–1000 | Hepatic carcinoma, Huh-BAT, Huh-7, SNU-761 |
Induced cell apoptosis via Bax, Bid, Fas ↑ Caspase-7, -8, -9 cleavage Phosphorylatedp42/44↑. | [132] |
| F. vesiculosus | 150 | Leucemia, HL-60 NB4 THP-1 | Induced cell apoptosis via PARP cleavage Caspase-8, 9, 3 ↑ Mcl-1, Bid ↓. |
[133] |
| F. vesiculosus | 50–200 | Leucemia, SUDHL-4, OCI-LY8, NU-DUL-1, TMD8, U293, DB | Induced cell apoptosis via PARP cleavage and cleaved caspase-8,9, 3 ↑. | [134] |
| F. vesiculosus | 12.5–100 | Leucemia, NB4, HL60 |
Cell proliferation inhibition and induced cell apoptosis via Caspase-3, 8, 9, ↑ PARP cleavage and Bax ↑. | [135] |
| F. vesiculosus | 20–100 | Leucemia, U937 | Cell proliferation inhibition and induced cell apoptosis via Caspase-3, 8, 9 ↑, PARP cleavage, Bax↑. | [136] |
| U. pinnatifida | 200–1000 | Colon cancer, WiDr LoVo Brest cancer, MCF-7 |
Cell proliferation inhibition. | [108] |
| U. pinnatifida | 10–200 | Lung cancer, A549 | Cell proliferation inhibition and induced cell apoptosis via Bcl 2, p38, Phospho-PI3K/Akt, procaspase- 3↓ Bax, caspase-9, Phospho-ERK1/2 ↑ PARP cleavage. | [137] |
| U. pinnatifida | 65.2–1000 | Hepatic carcinoma, SMMC-7721 |
Cell proliferation inhibition and induced cell apoptosis via Livin, XIAP mRNA ↓ Caspase-3, -8, -9 ↑ Bax-to-Bcl-2 ratio↑ Cytochrome C ↑. | [138] |
| Cladosiphon | 1000 | Brest cancer, MCF-7 |
Induced cell apoptosis via PARP cleavage Caspase-7,8,9 ↑ Cytochrome C, Bax, Bid↑. |
[139] |
| B. bifurcata | 2–9 | Lung cancer, NSCLC-N6 |
Cell proliferation inhibition via irreversible growth arrest. | [119] |
↑—increased/stimulated levels; ↓—decreased/suppressed levels.
4. Fucoidan-Based Pharmaceutical Formulations
In addition to its biological activity, fucoidan has suitable properties as a drug carrier, which is confirmed by numerous reports in the literature of nano- and microparticles, liposomes, films, hydrogels, etc., based on the polysaccharide (Table 5) [140][141][142][143]. The polymer backbone has anionic properties due to the presence of negatively charged sulfate ester groups. Depending on the specific chemical characteristics and the charge density of fucoidan, the polymer can interact with various biomolecules such as proteins and other polysaccharides [141]. The polysaccharide is soluble in water and acidic solutions, the solubility depending on the molecular weight and the amount of sulfate groups. Highly water-soluble fucoidans form low-viscosity solutions and are therefore generally not used as gelling agents. On the other hand, the viscoelastic properties of fucoidan are highly dependent on the origin of the polysaccharide, its concentration, molecular weight, sulfate content, pH and temperature [5]. The interaction of fucoidan with oppositely charged biopolymers such as chitosan [144], poly(2-hydroxyethyl methacrylate) [145], soybean protein isolate (SPI) [146] and lactoglobulin [147] can lead to the formation of polyelectrolyte complexes with improved characteristics for biomedical application. Polyelectrolyte complexation (complex coacervation) is one of the most widely used methods for obtaining fucoidan micro- and nanoparticles. Other common techniques for formulating particulate drug systems from the polysaccharide are simple coacervation, ionotropic gelation, spray drying, emulsification, etc. (Figure 4) [6]. Fucoidan-based micro- and nanoparticles have been used as drug delivery systems for various anticancer agents such as doxorubicin [148], methotrexate [149], curcumin [150] and cisplatin [151].
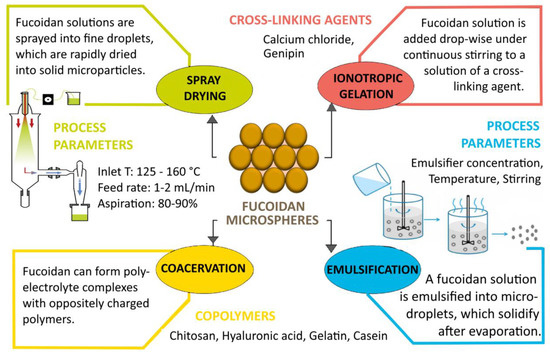
Figure 4. Methods for obtaining fucoidan microparticles (created with Microsoft Office Professional 2021).
4.1. Fucoidan Microparticles
The term microparticles refers to particles ranging in size from 1 µm to 1000 µm. Microparticles can encapsulate hydrophilic and hydrophobic agents and, depending on their structure, can be categorized as microcapsules and microspheres. Microparticles formulated from fucoidan refer to the term fucospheres. Fucospheres can be prepared using a variety of techniques and typically the manufacturing process involves the addition of copolymers or positive charge donors [5]. Such systems can provide increased stability of the drug substance, masking of its organoleptic properties, drug targeting to certain departments of the gastro-intestinal tract, controlled release and increased oral bioavailability [152]. Microspheres based on fucoidan can be used as carriers for nasal application. Combining the advantages of the microcarriers with the mucoadhesive properties of the polymer brings additional benefits such as more effective absorption and increased bioavailability due to the large total surface area of the particles, better contact with the nasal mucosa and specific targeting to the absorption site, including direct nose-to-brain drug delivery [153].
According to a study by Sezer et al., fucospheres can be prepared by crosslinking fucoidan with positively charged chitosan. The authors used bovine serum albumin (BSA) as a model drug and the resulting particles showed smooth spherical morphology and particle size ranging from 0.61 µm to 1.28 µm. Furthermore, the results showed that increasing the fucoidan content led to an increase in the zeta potential and encapsulation efficiency of BSA. The formulated particles demonstrated a sustained release of BSA characterized by a complex triphasic profile [154]. In another study, fucospheres prepared by complexation between fucoidan and chitosan were investigated for potential application in the treatment of skin burns. As previously reported, the size of the prepared microparticles increased with increasing the polymer concentration. The formulated microparticles combined the properties of the two polymers used for their preparation, resulting in a synergic effect between fucoidan and chitosan. The reported increased in vivo skin regeneration induced by the fucospheres was probably because of the effect of fucoidan on the fibroblast migration, the release of growth hormones and cytokines involved in the re-epithelization process [155]. Poly(alkyl cyanoacrylate) (PACA) microcapsules coated with fucoidan, prepared using the emulsion evaporation polymerization method, were reported to have the ability to detect thrombosis, due to the binding of fucoidan to P-selectin. The performed in vivo tests on rats demonstrated that such structures could be valuable targeting carriers for contrast agents, especially for the diagnosis of P-selectin overexpression diseases [156]. Fucospheres have also been formulated as delivery systems for antibiotics and antifungal agents. Sezer et al. used a complexation and precipitation method to prepare ofloxacin-loaded fucoidan microparticles. The formulated fucospheres showed an average particle size of 0.61 to 1.48 µm, a zeta potential of 22.3 mV and drug encapsulation efficiency of 63.9–94.8%. Regarding the drug release profile, ofloxacin-loaded fucoidan microparticles showed a sustained release, consistent with the Higuchi kinetic model [154]. Szekalska et al. used a spray-drying technique to prepare posaconazole-loaded fucoidan/gelatin microspheres for the treatment of fungal infections. The resulting particles had an average size of 12.02 µm to 17.91 µm and an encapsulation efficacy of over 90%. The microspheres were tested in simulated vaginal fluid (SVF) at pH of 4.2 and showed good swelling and mucoadhesive properties, demonstrating sustained release of posoconazole [157].
Since fucoidan can recognize macrophages in the alveoli, fucoidan-based microparticles may be suitable carriers for pulmonary drug delivery [158]. In a study by Cunha et al., fucoidan microparticles were proposed for the treatment of tuberculosis. Isoniazid and rifabutin were used as model drugs. The particles obtained with isoniazid had an average size of 3.78 µm, and those with rifabutin - 1.99 µm. The prepared formulations were considered as a potential pulmonary drug delivery system for the treatment of tuberculosis [159]. Fucoidan microparticles also have great potential to be used as drug delivery systems for cancer treatment. Wang et al. conducted a study on the preparation of doxorubicin loaded poly-L-ornithine/fucoidan-coated calcium carbonate microparticles using layer-by-layer self-assembly fabrication method [93]. First, calcium carbonate particles were prepared and then they were coated with poly-L-ornitine and fucoidan. The resulting blank particles were further loaded with doxorubicin, showing an encapsulation efficiency of over 70%. The in vitro study performed at pH 7.4 showed the microparticles were characterized by a prolonged release of doxorubicin..
4.2. Fucoidan Nanoparticles
Polymeric nanoparticles are usually spherical structures with an average size of 1 to 1000 nm. They can be categorized as nanocapsules and nanospheres depending on their composition and the location of the active pharmaceutical ingredient (API). Nanocapsules can be defined as nanosized vesicles in which the API is encapsulated in a reservoir system surrounded by a polymer membrane, while in nanospheres the drug is homogenously dissolved/dispersed in a polymer matrix. Polymer nanoparticles are multicompartment drug carriers that can provide chemical and enzymatic protection of the API and enable controlled and/or targeted drug release [5]. Due to its biocompatibility, high drug loading, stability and possibility of chemical modifications with organic and inorganic substances, fucoidan has been widely investigated for application as a drug nanocarrier [117]. In the formulation of nanoscale drug delivery systems, fucoidan is usually combined with other polymers such as poly(lactic-co-glycolic acid) (PLGA), chitosan, various proteins or liposome-forming lipids [160][161][162]. In a study by Abdelkader et al., fucoidan-based PEGylated PLGA nanoparticles for the delivery of N-methyl anthranilic acid were formulated using a single emulsion/solvent evaporation method [163]. The optimal formulation showed an average particle size of 365 nm and a zeta potential of −22.30 mV. The polymer nanosystems were characterized by a high encapsulation efficacy of 85.45% and drug loading of 51.36%. The in vitro assay showed initial burst release of 47.91% of the incorporated drug within one hour, followed by cumulative release profile for 4 h. Fucoidan-based nanoparticles containing a hydrophobic anticancer drug were developed by Lai et al. The particles were composed of fucoidan and PLGA and were designed as nanocarriers for docetaxel. The authors found that the incorporation of the drug in the nanoparticles was strongly dependent on the ratio between the two polymers used—fucoidan and poly(lactic-co-glycolic acid). The formulation prepared at a ratio of 10:3 demonstrated the highest encapsulation efficiency of 68.7 ± 4.2% [164].
The study of Huang et al. [165] gave an example of successful fucoidan-chitosan complex formation for the development of nanoparticles as carriers for oral drug delivery. The resulting polyelectrolyte complexes were formulated due to electrostatic interactions between the positively charged amino groups of chitosan and the anionic sulfate groups of fucoidan. The obtained particle models demonstrated an average particle size of 380 nm and an isoelectric point of 5.7. In another study, Huang and Kuo prepared O-carboxymethyl chitosan/fucoidan (O-CMC/F) nanoparticles for curcumin delivery [150]. Fucoidan and O-carboxymethyl chitosan were crosslinked with calcium ions to form nanoparticles with an average size between 100 and 200 nm. After loading with curcumin, the particle size increased to 270 nm. The obtained nanosystems showed high encapsulation efficacy of 92.8% and pH-dependent drug release.
Fucoidan/trimethyl chitosan nanoparticles that enhanced transepithelial penetration of insulin by inhibiting alpha-glucosidase activity were developed by Tsai et al. [166]. The in vitro drug release results showed that insulin release was greater at neutral and intestinal pH compared to gastric fluid, where prolonged release was observed.
Another study conducted by Chen et al. proposed the preparation of self-assembled nanoparticles from arginine-modified chitosan and thiolated fucoidan, which were designed to improve the intestinal epithelial transport of dextran and curcumin [167]. The resulting particles were characterized by pH-dependent drug release and showed improved permeation of the incorporated hydrophobic and hydrophilic drug through the Caco-2 cell monolayer barrier.
To enhance the antiangiogenic effect of fucoidan and to improve its bioavailability, Yu et al. produced oversulfated fucoidan. The modified fucoidan was further used to prepare fucoidan/chitosan nanoparticles by a polyelectrolyte complexation method [168]. The nanoparticles were stable at pH 2.5–6.0, which was probably due to the high positive charge of chitosan forming strong electrostatic interactions, while at pH 6.5 the particles were destabilized and the oversulfated fucoidan was released.
Lin et al. developed amoxicillin-loaded genipin-crosslinked fucoidan/chitosan-N-arginine nanogels for the treatment of Helicobacter pylori infections. Due to the strong anti-inflammatory effect and cell adhesive properties of low molecular weight fucoidans, the polymer was first depolymerized and then crosslinked with genipin to form nanogels [169]. The in vitro drug release results showed that at pH 2, an initial burst release of amoxicillin (52%) was observed, followed by a sustained release due to formation of electrostatic interactions between amoxicillin and low molecular weight fucoidan. At pH 6.5, the nanogels were stable, allowing only a small amount of amoxicillin to be released, while at pH 7.4 the nanogels disassembled and rapidly released the incorporated drug.
Eggshell protein, which has properties enabling it to treat inflammatory bowel disease, undergoes rapid enzymatic degradation when taken orally, severely limiting its bioavailability. A study conducted by Lee et al. demonstrated that fucoidan–chitosan nanoparticles could be used as carriers for that protein. Polymer nanostructures were characterized by a pH-dependent in vitro drug release such that at pH 1.2–2.5 no release was observed, while at pH 7.4 50% of the protein was released in a sustained manner [170].
Fucoidan can also form polyelectrolyte complexes with proteins [146][171]. A study conducted by Fan et al., for example, proposed a formulation of fucoidan/soybean nanoparticles as a delivery system for curcumin [146]. The average size of the obtained particles ranged from 200 to 400 nm and the encapsulation efficiency was up to 97.6%. The in vitro release assay performed in simulated gastric fluid showed that the nano formulations released more than 80% of the incorporated curcumin within 4 h. A storage stability test demonstrated that after one week soybean nanoparticles showed physical instability, while the fucoidan–protein structures remained stable, which confirmed the stabilizing function of fucoidan in the nanoparticle complex.
4.3. Fucoidan Liposomes
Liposomes are other commonly used nanosized drug delivery systems that can offer advantages such as improved solubility, increased drug stability and targeted delivery [172]. A study by Qadir et al. demonstrated that, when encapsulated in liposomes, fucoidan from F. vesiculosus had stronger anticancer activity, reducing interleukin-6 and tumor necrosis factor-α levels, compared to fucoidan nanoparticles [173]. Salviano et al. developed a liposomal drug delivery system composed of fucoidan derivative (cholesteryl-fucoidan) loaded with usnic acid for the treatment of Mycobacterium tuberculosis infection. The formulated systems showed significantly lower IC50 (8.26 ± 1.11 µM) compared to blank liposomes, due to higher uptake and cellular internalization [174]. In another study, Zhang et al. formulated liposomes as delivery systems for bioactive nutraceuticals by coating them with fucoidan. The authors highlighted the stabilizing effect of fucoidan, which can reduce the drug leakage from the liposomes and the initial burst release, thereby improving the stability and bioavailability of liposomes [175].
Table 5. Fucoidan micro and nano-sized formulations and their biomedical applications.
| Active Substance |
Dosage Form |
Therapeutic Application |
Data Obtained |
Reference |
|---|---|---|---|---|
| Fucoidan | Microparticles | Skin burns | Enhanced skin regeneration resulted in an increase in the epithelial thickness in vivo on rabbits. | [155] |
| Perfluorooctyl bromide | Microparticles | Thrombosis | High affinity to P-selectin and ability to detect thrombosis in vivo on rats with induced aortic aneurysm. | [156] |
| Isoniazid, Rifabutin |
Microparticles | Tuberculosis | Effective inhibition of mycobacterial growth. Low toxicity on human alveolar epithelum and monocytic cell line (HTP-1). | [159] |
| Doxorubicin | Microparticles | Breast cancer | Significant antiproliferative activity on MCF-7 breast cancer cell line. Low toxicity on mouse myoblasts (concentration 400 µg/mL). | [162] |
| N-methyl anthranilic acid | Nanoparticles | Inflammation | Significant reduction in carrageenan-induced inflammation in rats by decreasing the cyclooxygenase-2, (TNF)-α E2, NO, IL-1β, IL-6. | [163] |
| Docetaxel | Nanoparticles | Anticancer | High cellular uptake efficiency and subcellular localization. Low cytotoxicity on non-tumor cell lines. | [164] |
| Oversulfated fucoidan |
Nanoparticles | Anticancer | Inhibition of human umbilical vein endothelial cells HUVECs via competitive binding to bFGF receptors (bFGFRs). | [168] |
| Amoxicillin | Nanogels | H. pylori infection | pH-dependent sustained drug release, which can improve the therapy of Helicobacter pylori. |
[169] |
| Piperlongumine | Nanoparticles | Prostate cancer | Higher cytotoxicity in the PC-3 cells than in the non-cancerous hDFB cells; increased the intracellular ROS levels in the PC-3 cells. | [176] |
| Usnic acid | Liposomes | M. tuberculosis | Higher cellular uptake and cellular internalization. | [174] |
5. Fucoidan Nanoparticles for Cancer Therapy
Fucoidan nanoparticles have been extensively studied as drug delivery systems for cancer treatment, due to their multifaceted advantages such as controlled drug release, improved drug permeability and precise targeting to specific cancer cells (Figure 5) [177]. Fucoidan has been outlined as a suitable carrier for various anticancer agents, including doxorubicin (DOX), copper sulfide (CuS), methotrexate (MTX), curcumin (CUR), cisplatin, etc. (Table 6).
Figure 5. Advantages of nanoparticles in cancer treatment (created with Microsoft Office Professional 2021).
Table 6. Fucoidan-based nanoparticulate drug delivery systems for cancer therapy.
| Source, Mw | Copolymer | Drug | Preparation Method |
Administration Route |
Reference |
|---|---|---|---|---|---|
| F. vesiculosus, 200–400 kDa | Gold nanoparticles | Doxorubicin | Electrostatic complexation | Ocular | [148] |
| L. japonica, 80 kDa | Protamine | Doxorubicin | Self-assembly | Intravenous | [178] |
| F. vesiculosus, 200–400 kDa | Polyethyleneimine | Doxorubicin | Coacervation | Intravenous | [179] |
| F. vesiculosus, 200–400 kDa | Polyallylamine HCl | Copper sulfide | Layer-by-layer | Intratumoral | [180] |
| F. vesiculosus, 200–400 kDa | Polyallylamine HCl | Methotrexate | Self-assembly | NA * | [149] |
| F. vesiculosus, 200–400 kDa | Chitosan/Chondroitin | Fucoidan | Coacervation | Oral | [181] |
| F. vesiculosus, 50–190 kDa | Chitosan | Methotrexate | Self-assembly | Topical | [182] |
| F. vesiculosus, 50–190 kDa | Chitosan | Curcumin | Self-assembly | Oral | [183] |
* NA—no available information.
Kim et al. developed fucoidan-coated gold nanoparticles loaded with doxorubicin for photothermal therapy of squamous carcinoma [148]. In vitro cytotoxic assay was conducted on RAW 264.7 macrophage cells and on VX2 squamous cell line. As expected, as the concentration of the nanoparticles increased, cell viability decreased. Furthermore, after laser irradiation of the VX2 cells containing fucoidan-coated gold nanoparticles, maximal cell death was recorded (88%).
Fucoidan nanoparticles have also been used as carriers for cisplatin [151]. The prepared nanoparticles showed a high encapsulation efficacy of 93.3%, an average size of 181.2 nm and a zeta potential of −67.4 mV. An immune protection assay was performed on RAW 264.7 macrophage cells to investigate the cytotoxic effect of encapsulated cisplatin. HCT-8 tumor cells were treated with different concentrations of cisplatin, fucoidan and cisplatin-loaded fucoidan nanoparticles. The formulated nanoparticles caused greater toxicity to the tested cancer cells compared to the free drug.
Using the polyelectrolyte complexation method, Lue et al. developed multi-stimuli-responsive fucoidan/protamine nanoparticles as carriers for doxorubicin [178]. According to TEM and DLS analyses, the average particle size was 180 nm and the zeta potential ranged from −22 mV to −43 mV depending on the fucoidan/protamine ratio. The cytotoxic effect of the nanoparticles was evaluated using MDA-MB-231 cell line. Enzymatic digestion and the acidic intracellular microenvironment of the cancer cell triggered the release of doxorubicin from the nanoparticles, resulting in decreased cell viability. P-selectin expression was determined using a mouse monoclonal antibody (anti-selectin/CD62P) against MDA-MB-231 cells and the result showed that doxorubicin-loaded fucoidan/protamine nanoparticles inhibited platelet activation. The authors suggested that the proposed nanostructures can be used as potential drug delivery systems for intracellular release of anticancer drugs against metastatic breast carcinoma.
In order to develop an immunomodulatory platform for the delivery of doxorubicin, Pawar et al. formulated fucoidan-polyethileneimine nanoparticles using a polyelectrolyte complexation technique [179]. The in vitro release study showed that the drug was released faster at acidic pH 5.5, compared to neutral pH 7.4. In both media the particles demonstrated an initial burst release within the first 24 h, followed by a sustained release. Furthermore, doxorubicin-loaded nanoparticles showed a greater cytotoxic effect on MDA MB-231 and 4T1 cell lines compared to free daunorubicin. The in vivo anticancer assay performed on 4T1 induced tumor in BALB/c mice confirmed the targeted delivery of doxorubicin to the tumor site.
Self-assembled nanoparticles based on a combination of fucoidan with polyallylamine were formulated as drug carriers for methotrexate. The developed polymer nanosystems demonstrated significant inhibition of the proliferation of HeLa and MCF-7 cell lines [149]. In another study, fucoidan was used to functionalize doxorubicin-loaded micelles [184]. The average size of the developed structures was 120 nm and their zeta potential was −20 mV. The biodistribution of the obtained micelles and free doxorubicin was studied in tumor-induced BALB/c mice 1, 8 and 24 days after administration. Fucoidan-functionalized doxorubicin micelles showed high accumulation at the tumor site and limited distribution in the kidneys and liver, making them a promising strategy for the treatment of metastatic cancer.
Kang et al. developed doxorubicin-loaded fucoidan-coated nanoparticles to overcome multidrug resistance in chemotherapy [185]. The obtained particles had an average size of 35 nm and a drug encapsulation efficiency of 35%. The cytotoxicity assay showed that the particles reduced the viability of the human breast cancer cell line (MCF-7ADR), while only mild cytotoxicity was observed in the normal breast cell line (MCFA-10). An in vivo study on BALB/c male mice with induced tumor (transplanted MCF-7ADR cells in the right flank) demonstrated efficient delivery of doxorubicin to the targeted tumor tissues and limited accumulation in the liver.
One of the key factors in cancer growth and metastasis is the P-selectin protein which has a significant role in the activation of platelets associated with cancer cell metastasis. Therefore, targeting and inhibiting the action of P-selectin protein is an essential mechanism for achieving effective cancer therapy. The ability of fucoidan to target P-selectin proteins was among the main reasons for Jafari et al. to use it as a nanocarrier of doxorubicin for the treatment of breast cancer [186]. The formulated polymer particles had an average size of 167.3 nm, a drug loading of 4.81% and a zeta potential of −19.87 mV. By adding polyethylene glycol (PEG), the zeta potential increased to −15.09 mV, indicating that PEG partially shielded the particle surface charge. In vitro drug release was carried out in PBS of pH 7.4 and pH 5.2. No initial burst release was observed in both media in the first hours, probably due to the covalent bonds between doxorubicin and fucoidan. After 72 h, 35% of doxorubicin was released in PBS 7.4, while in PBS 5.2 the release was faster (60%), demonstrating a pH-dependent pattern. The P-selectin expression was studied via P-selectin recombinant rabbit monoclonal antibody using two breast cancer cell lines (MDA-MB-231, MDA-MB-468), compared with normal breast cells (MCF-12A). Western blotting and immunofluorescent imaging revealed that P-selectin was better expressed on MDA-MB-231 cells, compared to the other two cell lines. The developed fucoidan nanoparticles demonstrated high cellular drug uptake and can be used for targeted and sustained release of doxorubicin.
DuRoss et al. investigated the P-selectin targeting properties of temozolomide/talazoparib-loaded fucoidan-coated 1,4-dicarboxybenze metal-organic nanoparticles to achieve enhanced chemotherapeutic effect against colorectal cancer [187]. The obtained particles had a negative zeta potential, a particle size of 30–70 nm and an encapsulation efficiency of 90% for temozolomide and 54% for talazoparib. According to the in vitro test performed in PBS pH 7.4, the formulated nanoparticles released 40% of the incorporated drugs within the first 24 h, followed by sustained release. After 7 days talazoparib was completely released from the particles in contrast to temazolomide (only 60%). In vitro cytotoxicity test was conducted on CT26 cell line, and P-selectin expression was evaluated on bEnd.3 and CT26 cancer cell lines. After treatment of the cells with the developed nanoparticles and subsequent administration of increasing doses of radiation (0, 1, 2, 3, 4, 5 Gy), a significant decrease in cell survival was registered. In vivo biodistribution analysis in tumor-bearing mice showed that the administered nanoparticles had a high accumulation at the tumor site both with or without irradiation, offering improved drug delivery and enhanced radiotherapy.
To achieve improved drug distribution and pharmacokinetics, Chen et al. proposed encapsulation of epigallocatechin-3-gallate (EGCG) and docetaxel (DTX) in D-Alpha-tocopheryl polyethylene glycol 1000 succinate-conjugated fucoidan/hyaluronic acid nanoparticles for the treatment of prostate cancer [188]. The particle size ranged from 189.96 nm to 238.98 nm and the zeta potential from −25.22 mV to −27.42 mV. EGCG:DTX concentration ratio of 2.0:0.2 mg/mL was determined as optimal, resulting in encapsulation efficiency of 43.39% for EGCG and 85.86% for DTX. The formulated nanoparticles were characterized with pH-dependent in vitro drug release. In 24 h at pH 5.5, they released 37.33% EGCG and 43.75% DTX. The obtained particles demonstrated internalization in prostate cancer cells by recognizing CD44 and P-selectin ligand. Furthermore, the in vitro test indicated that the polymer particles inhibited cell growth by inducing G2/M phase arrest of the cells. Additional in vivo studies confirmed that the formulated drug-loaded nanostructures significantly reduced tumor growth and increased M30 protein expression.
Oliveira et al. formulated antibody (ErbB-2) conjugated fucoidan–chitosan nanoparticles loaded with gemcitabine for the treatment of metastatic cancer [189]. The nanoparticle had an average size of 160 nm, a polydispersity index of 0.18 and a positive zeta potential of 21 mV. The targeting capability of the nanoparticles was confirmed by an increased cellular uptake of ErbB-2 positive SKBR3 breast cancer cells. The cytotoxicity assay indicated that the Ab-conjugated nanoparticles exerted increased cytotoxic effect in breast cancer cells (above 80%) compared to free gemcitabine (only 15%) and nanoparticles blended with gemcitabine (20%). The in vivo study on immunocompromised female mice with induced breast cancer demonstrated that the targeting drug delivery system significantly reduced tumor growth and lung metastasis.
Cavalcanti et al. developed fucoidan-coated poly(isobutyl cyanoacrylate) nanoparticles loaded with oncocalyxone A for the treatment of metastatic breast cancer [190]. The produced nanoparticles had an average size of 305 ± 6.49 nm and encapsulation efficiency of 100%. The authors performed a cytotoxicity assay on J774A.1 macrophage cells and MDA-MB-231 breast cancer cell line. The results showed that neither free oncocalyxone A nor oncocalyxone A-loaded nanoparticles had cytotoxic effect on J774A.1 macrophage cell line. The results from the MTT test indicated that the oncocalyxone A-loaded fucoidan nanoparticles exerted higher cytotoxic activity against MDA-MB-231 cells after 72 h of exposure compared to pure oncocalyxone A.
Other anticancer agents—paclitaxel and mitogen-activated protein kinase—were also encapsulated in fucoidan through a nano-precipitation technique [191]. To study the targeting efficacy of the obtained nanoparticles SK-136 murine cell line was used. The results showed that fucoidan-based nanoparticles can specifically target the tumor microenvironment and be localized via MEK inhibitors in both primary and metastatic cancer cells, demonstrating improved anticancer activity.
The provided examples of successful incorporation of anticancer agents into fucoidan nanoparticles convincingly demonstrate the potential of this polysaccharide as a drug carrier. However, most of the reported formulations have been analyzed mainly by in vitro assays and to a lesser extent characterized in vivo. Further research and clinical trials are needed to prove the effectiveness and safety of fucoidan nano- and micro-particles as therapeutic systems and to enable their utilization on the pharmaceutical market as final pharmaceutical products. Although such studies are still scarce in the literature, the positive data from clinical trials on the antitumor effectiveness of fucoidan suggest that fucoidan formulations have great potential as a safe and effective drug-delivering system for application in oncology (Table 7).
Table 7. Clinical trials/Case reports on fucoidan anticancer activity.
| Fucoidan Source |
Cancer Type |
Dose Applied |
Study Type |
Number of Patients |
Clinical Results |
Reference |
|---|---|---|---|---|---|---|
| LMW fucoidan from S. hemiphyllum |
Metastatic colorectal cancer |
4 g/day |
Randomized, double-blind, controlled trial | 54 | Improved disease control |
[192] |
| LMW fucoidan from C. okamuranus |
Advanced metastatic cancer |
400 mL/day |
Open-label clinical study | 20 | Improved therapy |
[67] |
| LMW fucoidan from C. okamuranus |
NK cells from patients in remission | 1.5 g twice a day |
Randomized double-blind placebo-controlled study | 39 | Enhanced NK cell activity |
[193] |
| HMW fucoidan from C. okamuranus |
Colorectal cancer |
150 mL/day |
A randomized trial | 20 | Decreased general fatigue |
[194] |
| Fucoidan (without clarification). |
Rectal cancer |
N/A | A double-blind randomized placebo-controlled study | 100 | N/A | [195] |
| Fucoidan as a dietary supplement |
Squamous cell carcinoma |
4.4 g/day |
A randomized double-blind study | 119 | Study not completed. |
[196] |
| Fucoidan as a dietary supplement |
Hepatocellular carcinoma |
4.4 g/day |
A randomized double-blind study | 100 | Study not completed. |
[197] |
| LMW fucoidan as a dietary supplement |
Lung cancer |
4.4 g twice a day |
A double-blind randomized controlled trial | N/A | Withdrawn. | [198] |
| LMW fucoidan from Undaria pinnatifida |
Brest cancer |
500 mg twice a day |
Open label non-crossover study | 20 | Co-administration with letrozole, tamoxifen. | [199] |
| LMW fucoidan from Nemacystis decipiens |
Prostate, liver, breast, pancreatic cancer | 60–300 mL/day | Case report | 10 | Decreased tumor markers |
[42] |
LMW—low molecular weight; HMW—high molecular weight; N/A—not available information.
References
- Cormode, D.P.; Jarzyna, P.A.; Mulder, W.J.M.; Fayad, Z.A. Modified natural nanoparticles as contrast agents for medical imaging. Adv. Drug Delivery. Rev. 2010, 62, 329–338.
- Fernando, I.P.S.; Kim, D.; Nah, J.W.; Jeon, Y.J. Advances in functionalizing fucoidansand alginates (bio)polymers by structural modifications: A review. Chem. Eng. J. 2019, 355, 33–48.
- Morya, V.; Kim, J.; Kim, E.K. Algal fucoidan: Structural and size-dependent bioactivities and their perspectives. Appl. Microbiol. Biotechnol. 2012, 93, 71–82.
- Wijesinghe, W.A.J.P.; Jeon, Y.J. Biological activities and potential industrial applications of fucose 2rich sulfated polysaccharides and fucoidans isolated from brown seaweeds: A review. Carbohydr. Polym. 2012, 88, 13–20.
- Citkowska, A.; Szekalska, M.; Winnicka, K. Possibilities of Fucoidan Utilization in the Development of Pharmaceutical Dosage Forms. Mar. Drugs 2019, 17, 458.
- Chollet, L.; Saboural, P.; Chauvierre, C.; Villemin, J.N.; Letourneur, D.; Chaubet, F. Fucoidans in Nanomedicine. Mar. Drugs 2016, 14, 145.
- Hentati, F.; Tounsi, L.; Djomdi, D.; Pierre, G.; Delattre, C.; Ursu, A.V.; Fendri, I.; Abdelkafi, S.; Michaud, P. Bioactive Polysaccharides from Seaweeds. Molecules 2020, 25, 3152.
- Bilan, M.I.; Grachev, A.A.; Ustuzhanina, N.E.; Shashkov, A.S.; Nifantiev, N.E.; Usov, A.I. A highly regular fraction of a fucoidan from the brown seaweed Fucus distichus L. Carbohydr. Res. 2004, 339, 511–517.
- Vishchuk, O.S.; Ermakova, S.P.; Zvyagintseva, T.N. Sulfated polysaccharides from brown seaweeds Saccharina japonica and Undaria pinnatifida: Isolation, structural characteristics, and antitumor activity. Carbohydr. Res. 2011, 346, 2769–2776.
- Chevolot, L.; Mulloy, B.; Ratiskol, J.; Foucault, A.; Colliec-Jouault, S. A disaccharide repeat unit is the major structure in fucoidans from two species of brown algae. Carbohydr. Res. 2001, 330, 529–535.
- Zayed, A.; El-Aasr, M.; Ibrahim, A.S.; Ulber, R. Fucoidan Characterization: Determination of Purity and Physicochemical and Chemical Properties. Mar. Drugs 2020, 18, 571.
- Luthuli, S.; Siya, W.; Cheng, Y.; Zheng, X.; Wu, M.; Tong, H. Therapeutic Effects of Fucoidan: A Review on Recent Studies. Mar. Drugs 2019, 17, 487.
- Wang, J.; Zhang, Q.; Zhang, Z.; Li, Z. Antioxidant activity of sulfated polysaccharide fractions extracted from Laminaria japonica. Int. J. Biol. Macromol. 2008, 42, 127–132.
- Yu, J.; Li, Q.; Wu, J.; Yang, X.; Yang, S.; Zhu, W.; Liu, Y. Fucoidan Extracted From Sporophyll of Undaria pinnatifida Grown in Weihai, China—Chemical Composition and Comparison of Antioxidant Activity of Different Molecular Weight Fractions. Front. Nutr. 2021, 8, 636930.
- Zhao, D.; Xu, J.; Xu, X. Bioactivity of fucoidan extracted from Laminaria japonica using a novel procedure with high yield. Food Chem. 2018, 245, 911–918.
- Fletcher, H.R.; Biller, P.; Ross, A.B.; Adams, J. The Seasonal Variation of Fucoidan within Three Species of Brown Macroalgae. Algal Res. 2017, 22, 79–86.
- Senthilkumar, K.; Manivasagan, P.; Venkatesan, J.; Kim, S.K. Brown Seaweed Fucoidan: Biological Activity and Apoptosis, Growth Signaling Mechanism in Cancer. Int. J. Biol. Macromol. 2013, 60, 366–374.
- Anisha, G.S.; Padmakumari, S.; Patel, A.K.; Pandey, A.; Singhania, R.R. Fucoidan from Marine Macroalgae: Biological Actions and Applications in Regenerative Medicine, Drug Delivery Systems and Food Industry. Bioengineering 2022, 9, 472.
- van Weelden, G.; Bobiński, M.; Okła, K.; van Weelden, W.J.; Romano, A.; Pijnenborg, J.M.A. Fucoidan Structure and Activity in Relation to Anti-Cancer Mechanisms. Mar. Drugs 2019, 17, 32.
- Nishimoto, S. Clinical improvement in cancer patients through integrated medicine, mainly using low molecular weight fucoidan supplements. J. Int. Soc. Life Inf. Sci. 2015, 33, 25–47.
- Zhang, Z.Y.; Teruya, K.; Eto, H.; Shirahata, S. Induction of Apoptosis by Low-Molecular-Weight Fucoidan through Calcium- and Caspase-Dependent Mitochondrial Pathways in MDA-MB-231 Breast Cancer Cells. Biosci. Biotechnol. Biochem. 2013, 77, 235–242.
- Chen, M.C.; Hsu, W.L.; Hwang, P.A.; Chou, T.C. Low Molecular Weight Fucoidan Inhibits Tumor Angiogenesis through Downregulation of HIF-1/VEGF Signaling under Hypoxia. Mar. Drugs 2015, 13, 4436–4451.
- Chen, M.C.; Hsu, W.L.; Hwang, P.A.; Chen, Y.L.; Chou, T.C. Combined administration of fucoidan ameliorates tumor and chemotherapy-induced skeletal muscle atrophy in bladder cancer-bearing mice. Oncotarget 2016, 7, 51608–51618.
- Matsubara, K.; Xue, C.; Zhao, X.; Mori, M.; Sugawara, T.; Hirata, T. Effects of middle molecular weight fucoidans on in vitro and ex vivo angiogenesis of endothelial cells. Int. J. Mol. Med. 2005, 15, 695–699.
- Matou, S.; Helley, D.; Chabut, D.; Bros, A.; Fischer, A.M. Effect of fucoidan on fibroblast growth factor-2-induced angiogenesis in vitro. Thromb. Res. 2002, 106, 213–221.
- Chabut, D.; Fischer, A.M.; Hettey, D.; Colliec, S. Low molecular weight fucoidan promotes FGF-2-induced vascular tube formation by human endothelial cells, with decreased PAI-1 release and ICAM-1 downregulation. Thromb. Res. 2004, 113, 93–95.
- Park, H.Y.; Park, S.H.; Jeong, J.W.; Yoon, D.; Han, M.H.; Lee, D.S. Induction of p53-independent apoptosis and G1 cell cycle arrest by fucoidan in HCT116 human colorectal carcinoma cells. Mar. Drugs 2017, 15, 154.
- Park, H.S.; Kim, G.Y.; Nam, T.J.; Kim, N.D.; Choi, Y.H. Antiproliferative activity of fucoidan was associated with the induction of apoptosis and autophagy in AGS human gastric cancer cells. J. Food Sci. 2011, 76, T77–T83.
- Sanjeewa, K.K.A.; Lee, J.S.; Kim, W.S.; Jeon, Y.J. The potential of brown-algae polysaccharides for the development of anticancer agents: An update on anticancer effects reported for fucoidan and laminaran. Carbohydr. Polym. 2017, 177, 451–459.
- Li, B.; Lu, F.; Wei, X.J.; Zhao, R.X. Fucoidan: Structure and bioactivity. Molecules 2008, 13, 1671–1695.
- Li, B.; Zhao, R.X.; Wei, X.J. Anticoagulant activity of fucoidan from Hizikia fusiforme. Agro Food Ind. Hi-Tech 2008, 19, 22–24.
- Koyanagi, S.; Tanigawa, N.; Nakagawa, H.; Soeda, S.; Shimeno, H. Oversulfation of fucoidan enhances its anti-angiogenic and antitumor activities. Biochem. Pharmacol. 2003, 65, 173–179.
- Oliveira, C.; Ferreira, A.S.; Novoa-Carballal, R.; Nunes, C.; Pashkuleva, I.; Neves, N.M.; Coimbra, M.A.; Reis, R.L.; Martins, A.; Silva, T.H. The Key Role of Sulfation and Branching on Fucoidan Antitumor Activity. Macromol. Biosci. 2017, 17, 1600340.
- Irhimeh, M.R.; Fitton, J.H.; Lowenthal, R.M.; Kongtawelert, P. A quantitative method to detect fucoidan in human plasma using a novel antibody. Methods Find. Exp. Clin. Pharmacol. 2005, 27, 705–710.
- Zhang, W.; Sun, D.; Zhao, X.; Jin, W.; Wang, J.; Zhang, Q. Microanalysis and preliminary pharmacokinetic studies of a sulfated polysaccharide from Laminaria japonica. Chin. J. Oceanol. Limnol. 2016, 34, 177–185.
- Pozharitskaya, O.N.; Shikov, A.N.; Faustova, N.M.; Obluchinskaya, E.D.; Kosman, V.M.; Vuorela, H.; Makarov, V.G. Pharmacokinetic and Tissue Distribution of Fucoidan from Fucus vesiculosus after Oral Administration to Rats. Mar. Drugs 2018, 16, 132.
- Tokita, Y.; Nakajima, K.; Mochida, H.; Iha, M.; Nagamine, T. Development of a fucoidan-specific antibody and measurement of fucoidan in serum and urine by sandwich ELISA. Biosci. Biotechnol. Biochem. 2010, 74, 350–357.
- Nagamine, T.; Nakazato, K.; Tomioka, S.; Iha, M.; Nakajima, K. Intestinal Absorption of Fucoidan Extracted from the Brown Seaweed, Cladosiphon okamuranus. Mar. Drugs 2015, 13, 48–64.
- Pozharitskaya, O.N.; Shikov, A.N.; Obluchinskaya, E.D.; Vuorela, H. The Pharmacokinetics of Fucoidan after Topical Application to Rats. Mar. Drugs 2019, 17, 687.
- Kimura, R.; Rokkaku, T.; Takeda, S.; Senba, M.; Mori, N. Cytotoxic Effects of Fucoidan Nanoparticles against Osteosarcoma. Mar. Drugs 2013, 11, 4267–4278.
- Koh, H.; Lu, J.; Zhou, W. Structure characterization and antioxidant activity of fucoidan isolated from Undaria pinnatifida grown in New Zealand. Carbohydr. Polym. 2019, 212, 178–185.
- Silva, M.M.C.L.; dos Santos Lisboa, L.; Paiva, W.S.; Batista, L.A.N.C.; Luchiari, A.C.; Rocha, H.A.O.; Camara, R.B.G. Comparison of in vitro and in vivo antioxidant activities of commercial fucoidans from Macrocystis pyrifera, Undaria pinnatifida, and Fucus vesiculosus. Int. J. Biol. Macromol. 2022, 216, 757–767.
- Lim, S.; Choi, J.; Park, H. Antioxidant activities of fucoidan degraded by gamma irradiation and acidic hydrolysis. Radiat. Phys. Chem. 2015, 109, 23–26.
- Lim, S.J.; Wan Aida, W.M.; Maskat, M.Y.; Mamot, S.; Ropien, J.; Mazita Mohd, D. Isolation and antioxidant capacity of fucoidan from selected Malaysian seaweeds. Food Hydrocoll. 2014, 42, 280–288.
- Kim, K.J.; Yoon, K.Y.; Lee, B.Y. Low molecular weight fucoidan from the sporophyll of Undaria pinnatifida suppresses inflammation by promoting the inhibition of mitogen-activated protein kinases and oxidative stress in RAW264.7 cells. Fitoterapia 2012, 83, 1628–1635.
- Pérez, M.J.; Falqué, E.; Domínguez, H. Antimicrobial Action of Compounds from Marine seaweed. Mar. Drugs 2016, 14, 52.
- Silva, A.; Silva, S.A.; Carpena, M.; Gull, P.; Barroso, M.F.; Prieto, M.A. Macroalgae as a Source of Valuable Antimicrobial Compounds: Extraction and Applications. Antibiotics 2020, 9, 642.
- Liu, M.; Liu, Y.; Cao, M.J.; Liu, G.-M.; Chen, Q.; Sun, L.; Chen, H. Antibacterial activity and mechanisms of depolymerized fucoidans isolated from Laminaria japonica. Carbohydr. Polym. 2017, 172, 294–305.
- Shannon, E.; Abu-Ghannam, N. Antibacterial Derivatives of Marine Algae: An Overview of Pharmacological Mechanisms and Applications. Mar. Drugs 2016, 14, 81.
- Lee, K.Y.; Jeong, M.R.; Choi, S.M.; Na, S.S.; Cha, J.D. Synergistic effect of fucoidan with antibiotics against oral pathogenic bacteria. Arch. Oral Biol. 2013, 58, 482–492.
- Hans, N.; Malik, A.; Naik, S. Antiviral activity of sulfated polysaccharides from marine algae and its application in combating COVID-19: Mini review. Bioresour. Technol. Rep. 2021, 13, 100623.
- Hayashi, K.; Lee, J.-B.; Nakano, T.; Hayashi, T. Anti-influenza A virus characteristics of a fucoidan from sporophyll of Undaria pinnatifida in mice with normal and compromised immunity. Microbes Infect. 2013, 15, 302–309.
- Queiroz, K.C.S.; Medeiros, V.P.; Queiroz, L.S.; Abreu, L.R.D.; Rocha, H.A.O.; Ferreira, C.V.; Jucá, M.B.; Aoyama, H.; Leite, E.L. Inhibition of reverse transcriptase activity of HIV by polysaccharides of brown algae. Biomed. Pharmacother. 2008, 62, 303–307.
- Thuy, T.T.T.; Ly, B.M.; Van, T.T.T.; Quang, N.V.; Tu, H.C.; Zheng, Y.; Seguin-Devaux, C.; Mi, B.; Ai, U. Anti-HIV activity of fucoidans from three brown seaweed species. Carbohydr. Polym. 2015, 115, 122–128.
- Springer, G.F.; Wurzel, H.A.; McNeal, G.M., Jr.; Ansell, N.J.; Doughty, M.F. Isolation of anncoagulant fractions from crude fucoidin. Proc. Sot. Exptl. Biol. Med. 1957, 94, 404–409.
- Grauffel, V.; Kloareg, B.; Mabeau, S.; Durand, P.; Jozefonvicz, J. New natural polysaccharides with potent antithrombic activity: Fucans from brown algae. Biomaterials 1989, 10, 363–368.
- Ren, D.; Wang, Q.; Yang, Y.; Hu, Y.; Song, Y.; He, Y.; Liu, S.; Wu, L. Hypolipidemic effects of fucoidan fractions from Saccharina sculpera (Laminariales, Phaeophyceae). Int. J. Biol. Macromol. 2019, 140, 188–195.
- Oliveira, R.M.; Câmara, R.B.G.; Monte, J.F.S.; Viana, R.L.S.; Melo, K.R.T.; Queiroz, M.F.; Filgueira, L.G.A.; Oyama, L.M.; Rocha, H.A.O. Commercial Fucoidans from Fucus vesiculosus Can Be Grouped into Antiadipogenic and Adipogenic Agents. Mar. Drugs 2018, 16, 193.
- Sim, S.Y.; Shin, Y.E.; Kim, H.K. Fucoidan from Undaria pinnatifida has anti-diabetic effects by stimulation of glucose uptake and reduction of basal lipolysis in 3T3-L1 adipocytes. Nutr. Res. 2019, 65, 54–62.
- Narayani, S.S.; Saravanan, S.; Ravindran, J.; Ramasamy, M.S.; Chitra, J. In vitro anticancer activity of fucoidan extracted from Sargassum cinereum against Caco-2 cells. Int. J. Biol. Macromol. 2019, 138, 618–628.
- Chantree, P.; Na-Bangchang, K.; Martviset, P. Anticancer activity of fucoidan via apoptosis and cell cycle arrest on cholangiocarcinoma cell. Asian Pac. J. Cancer Prev. 2021, 22, 209–217.
- Banafa, A.M.; Roshan, S.; Liu, Y.Y.; Chen, H.J.; Chen, M.J.; Yang, G.X.; He, G.Y. Fucoidan induces G1 phase arrest and apoptosis through caspases-dependent pathway and ROS induction in human breast cancer MCF-7 cells. J. Huazhong Univ. Sci. Technolog. Med. Sci. 2013, 33, 717–724.
- Zhang, Z.; Teruya, K.; Yoshida, T.; Eto, H.; Shirahata, S. Fucoidan extract enhances the anti-cancer activity of chemotherapeutic agents in MDA-MB-231 and MCF-7 breast cancer cells. Mar. Drugs 2013, 11, 81–98.
- Yang, L.; Wang, P.; Wang, H.; Li, Q.; Teng, H.; Liu, Z.; Yang, W.; Hou, L.; Zou, X. Fucoidan derived from Undaria pinnatifida induces apoptosis in human hepatocellular carcinoma SMMC-7721 cells via the ROS-mediated mitochondrial pathway. Mar. Drugs 2013, 11, 1961–1976.
- Chen, S.; Zhao, Y.; Zhang, Y.; Zhang, D. Fucoidan induces cancer cell apoptosis by modulating the endoplasmic reticulum stress cascades. PLoS ONE 2014, 9, e108157.
- Ma, D.; Wei, J.; Chen, S.; Wang, H.; Ning, L.; Luo, S.-H.; Liu, C.-L.; Song, G.; Yao, Q. Fucoidan Inhibits the Progression of Hepatocellular Carcinoma via Causing lncRNA LINC00261 Overexpression. Front. Oncol. 2021, 11, 653902.
- Takahashi, H.; Kawaguchi, M.; Kitamura, K.; Narumiya, S.; Kawamura, M.; Tengan, I.; Nishimoto, S.; Hanamure, Y.; Majima, Y.; Tsubura, S.; et al. An Exploratory Study on the Anti-inflammatory Effects of Fucoidan in Relation to Quality of Life in Advanced Cancer Patients. Integr. Cancer Ther. 2018, 17, 282–291.
- Hwang, P.A.; Phan, N.N.; Lu, W.J.; Ngoc Hieu, B.T.; Lin, Y.C. Low-molecular-weight fucoidan and high-stability fucoxanthin from brown seaweed exert prebiotics and anti-inflammatory activities in Caco-2 cells. J. Food Nutr. Res. 2016, 60, 32033.
- Cui, M.; Li, X.; Geng, L.; Wu, N.; Wang, J.; Deng, Z.; Li, Z.; Zhang, Q. Comparative study of the immunomodulatory effects of different fucoidans from Saccharina japonica mediated by scavenger receptors on RAW264.7 macrophages. Int. J. Biol. Macromol. 2022, 215, 253–261.
- Nakamura, T.; Suzuki, H.; Wada, Y.; Kodama, T.; Doi, T. Fucoidan induces nitric oxide production via p38 mitogen-activated protein kinase and NF-_B-dependent signaling pathways through macrophage scavenger receptors. Biochem. Biophys. Res. Commun. 2006, 343, 286–294.
- Saravana, P.S.; Cho, Y.J.; Park, Y.B.; Woo, H.C.; Chun, B.S. Structural, antioxidant, and emulsifying activities of fucoidan from Saccharina japonica using pressurized liquid extraction. Carbohydr. Polym. 2016, 153, 518–525.
- Kim, M.J.; Kim, K.B.W.R.; Jeong, D.H.; Ahn, D.H. Anti-inflammatory activity of ethanolic extract of Sargassum sagamianum in RAW 264.7 cells. Food Sci. Biotechnol. 2013, 22, 1113–1120.
- Cui, M.; Wu, J.; Wang, S.; Shu, H.; Zhang, M.; Liu, K.; Liu, K. Characterization and anti-inflammatory effects of sulfated polysaccharide from the red seaweed Gelidium pacificum Okamura. Int. J. Biol. Macromol. 2019, 129, 377–385.
- Ni, L.; Wang, L.; Fu, X.; Duan, D.; Jeon, Y.; Xu, J.; Gao, X. In vitro and in vivo anti-inflammatory activities of a fucose-rich fucoidan isolated from Saccharina japonica. Int. J. Biol. Macromol. 2020, 156, 717–729.
- Fernando, I.P.S.; Sanjeewa, K.K.A.; Samarakoon, K.W.; Lee, W.W.; Kim, H.S.; Kang, N.; Ranasinghe, P.; Lee, H.S.; Jeon, Y.J. A fucoidan fraction purified from Chnoospora minima; a potential inhibitor of LPS-induced inflammatory responses. Int. J. Biol. Macromol. 2017, 104, 1185–1193.
- Pavliga, S.N.; Kompanets, G.G.; Tsygankov, V.Y. The experimental research in vitro of carrageenans and fucoidans to decrease activity of Hantavirus. Food Environ. Virol. 2017, 8, 120–124.
- Santoyo, S.; Plaza, M.; Jaime, L.; Ibañez, E.; Reglero, G.; Señorans, J. Pressurized liquids as an alternative Green process to extract antiviral agents from the edible seaweed Himanthalia elongata. J. Appl. Phycol. 2011, 23, 909–917.
- Wan, P.; Yang, X.M.; Cai, B.N.; Chen, H.; Sun, H.L.; Chen, D.K.; Pan, J.Y. Ultrasonic extraction of polysaccharides from Laminaria japonica and their antioxidative and glycosidase inhibitory activities. J. Ocean Univ. China 2015, 14, 651–662.
- Fu, Z.F.; Li, H.H.; Liu, H.B.; Hu, S.M.; Li, Y.J.; Wang, M.X.; Guan, H.S. Bioassay-guided extraction of crude fucose-containing sulphated polysaccharides from Sargassum fusiforme with response surface methodology. J. Ocean Univ. China 2016, 15, 533–540.
- Ko, S.C.; Lee, S.H.; Ahn, G.; Kim, K.N.; Cha, S.H.; Kim, S.K.; Jeon, B.T.; Park, P.J.; Lee, K.W.; Jeon, Y.J. Effect of enzyme-assisted extract of Sargassum coreanum on induction of apoptosis in HL-60 tumor cells. J. Appl. Phycol. 2012, 24, 675–684.
- Zhurishkina, E.V.; Stepanov, S.I.; Shvetsova, S.V.; Kulminskaya, A.A.; Lapina, I.M. A comparison of the effect of fucoidan from alga Fucus vesiculosus and its fractions obtained by anion-exchange chromatography on HeLa G-63, Hep G2, and Chang liver cells. Cell Tissue Biol. 2017, 11, 242–249.
- Bobiński, M.; Okła, K.; Bednarek, W.; Wawruszak, A.; Dmoszyńska-Graniczka, M.; Garcia-Sanz, P.; Wertel, I.; Kotarski, J. The effect of fucoidan, a potential new, natural, anti-neoplastic agent on uterine sarcomas and carcinosarcoma cell lines: ENITEC collaborative study. Arch. Immunol. Ther. Exp. 2019, 67, 125–131.
- Wu, J.; Chen, X.; Qiao, K.; Su, Y.; Liu, Z. Purification, structural elucidation, and in vitro antitumor effects of novel polysaccharides from Bangia fuscopurpurea. Food Sci. Hum. Wellness 2021, 10, 63–71.
- Azuma, K.; Ishihara, T.; Nakamoto, H.; Amaha, T.; Osaki, T.; Tsuka, T.; Imagawa, T.; Minami, S.; Takashima, O.; Ifuku, S.; et al. Effects of oral administration of fucoidan extracted from Cladosiphon okamuranus on tumor growth and survival time in a tumor-bearing mouse model. Mar. Drugs 2012, 10, 2337–2348.
- Xue, M.; Ge, Y.; Zhang, J.; Wang, Q.; Hou, L.; Liu, Y.; Sun, L.; Li, Q. Anticancer properties and mechanisms of fucoidan on mouse breast cancer in vitro and in vivo. PLoS ONE 2012, 7, e43483.
- Zhu, C.; Cao, R.; Zhang, S.X.; Man, Y.N.; Wu, X.Z. Fucoidan inhibits the growth of hepatocellular carcinoma independent of angiogenesis. Evid. Based Complement. Alternat. Med. 2013, 2013, 692549.
- Hsu, H.Y.; Lin, T.Y.; Hwang, P.A.; Tseng, L.M.; Chen, R.H.; Tsao, S.M.; Hsu, J. Fucoidan induces changes in the epithelial to mesenchymal transition and decreases metastasis by enhancing ubiquitin-dependent TGFβ receptor degradation in breast cancer. Carcinogenesis 2013, 34, 874–884.
- Suresh, V.; Anbazhagan, C.; Thangam, R.; Senthilkumar, D.; Senthilkumar, N.; Kannan, S.; Rengasamy, R.; Palani, P. Stabilization of mitochondrial and microsomal function of fucoidan from Sargassum plagiophyllum in diethylnitrosamine induced hepatocarcinogenesis. Carbohydr. Polym. 2013, 92, 1377–1385.
- Takeda, K.; Tomimori, K.; Kimura, R.; Ishikawa, C.; Nowling, T.K.; Mori, N. Anti-tumor activity of fucoidan is mediated by nitric oxide released from macrophages. Int. J. Oncol. 2012, 40, 251–260.
- Granert, C.; Raud, J.; Waage, A.; Lindquist, L. Effects of polysaccharide fucoidin on cerebrospinal fluid interleukin-1 and tumor necrosis factor a in pneumococcal meningitis in the rabbit. Infect. Immun. 1999, 67, 2071–2074.
- Hidalgo, A.; Peired, A.J.; Weiss, L.A.; Katayama, Y.; Frenette, P.S. The integrin αMβ2 anchors hematopoietic progenitors in the bone marrow during enforced mobilization. Blood 2004, 104, 993–1001.
- Tanaka, K.; Ito, M.; Kodama, M.; Tomita, M.; Kimura, S.; Hoyano, M.; Mitsuma, W.; Hirono, S.; Hanawa, H.; Aizawa, Y. Sulfated polysaccharide fucoidan ameliorates experimental autoimmune myocarditis in rats. J. Cardiovasc. Pharmacol. Ther. 2011, 16, 79–86.
- Kar, S.; Sharma, G.; Das, P.K. Fucoidan cures infection with both antimony-susceptible and -resistant strains of Leishmania donovani through Th1 response and macrophage-derived oxidants. Antimicrob. Chemother. 2011, 66, 618–625.
- Jin, J.O.; Zhang, W.; Du, J.Y.; Wong, K.W.; Oda, T.; Yu, Q. Fucoidan can function as an adjuvant in vivo to enhance dendritic cell maturation and function and promote antigen-specific t cell immune responses. PLoS ONE 2014, 9, e99396.
- Hayashi, K.; Nakano, T.; Hashimoto, M.; Kanekiyo, K.; Hayashi, T. Defensive effects of a fucoidan from brown alga Undaria pinnatifida against herpes simplex virus infection. Int. Immunopharmacol. 2008, 8, 109–116.
- Zhang, W.; Oda, T.; Yu, Q.; Jin, J.O. Fucoidan from Macrocystis pyrifera has powerful immune-modulatory effects compared to three other fucoidans. Mar. Drugs 2015, 13, 1084–1104.
- Maruyama, H.; Tamauchi, H.; Kawakami, F.; Yoshinaga, K.; Nakano, T. Suppressive effect of dietary fucoidan on proinflammatory immune response and MMP-1 expression in UVB-irradiated mouse skin. Planta Med. 2015, 81, 1370–1374.
- Carvalho, A.C.; Sousa, R.B.; Franco, A.X.; Costa, J.V.; Neves, L.M.; Ribeiro, R.A.; Sutton, R.; Criddle, D.N.; Soares, P.M.; de Souza, M.H. Protective effects of fucoidan, a p- and l-selectin inhibitor, in murine acute pancreatitis. Pancreas 2014, 43, 82–87.
- Lean, Q.Y.; Eri, R.D.; Fitton, J.H.; Patel, R.P.; Gueven, N. Fucoidan extracts ameliorate acute colitis. PLoS ONE 2015, 10, e0128453.
- AlKahtane, A.A.; Abushouk, A.I.; Mohammed, E.T.; ALNasser, M.; Alarifi, S.; Ali, D.; Alessia, M.S.; Almeer, R.S.; AlBasher, G.; Alkahtani, S. Fucoidan alleviates microcystin-LR-induced hepatic, renal, and cardiac oxidative stress and inflammatory injuries in mice. Environ. Sci. Pollut. Res. 2020, 27, 2935–2944.
- Aleissa, M.S.; Alkahtani, S.; Abd Eldaim, M.A.; Ahmed, A.M.; Bungău, S.G.; Almutairi, B.; Bin-Jumah, M.; AlKahtane, A.A.; Alyousif, M.S.; Abdel-Daim, M.M. Fucoidan ameliorates oxidative stress, inflammation, DNA damage, and hepatorenal injuries in diabetic rats intoxicated with aflatoxin B1. Oxidative Med. Cell. Longev. 2020, 2020, 9316751.
- Jeon, H.; Yoon, W.J.; Ham, Y.M.; Yoon, S.A.; Kang, S.C. Anti-arthritis effect through the anti-inflammatory effect of Sargassum muticum extract in collagen-induced arthritic (CIA) Mice. Molecules 2019, 24, 276.
- Matsumoto, S.; Nagaoka, M.; Hara, T.; Kimura-Takagi, I.; Mistuyama, K.; Ueyama, S. Fucoidan derived from Cladosiphon okamuranus Tokida ameliorates murine chronic colitis through the down-regulation of interleukin 6 production on colonic epithelial cells. Clin. Exp. Immunol. 2004, 136, 432–439.
- Lee, S.H.; Ko, C.I.; Jee, Y.; Jeong, Y.; Kim, M.; Kim, J.S.; Jeon, Y.J. Anti-inflammatory effect of fucoidan extracted from Ecklonia cava in zebrafish model. Carbohydr. Polym. 2013, 92, 84–89.
- Park, S.B.; Chun, K.R.; Kim, J.K.; Suk, K.; Jung, Y.M.; Lee, W.H. The differential effect of high and low molecular weight fucoidans on the severity of collagen-induced arthritis in mice. Phytother. Res. 2010, 24, 1384–1391.
- Ananthi, S.; Gayathri, V.; Malarvizhi, R.; Bhardwaj, M.; Vasanthi, H.R. Anti-arthritic potential of marine macroalgae Turbinaria ornata in complete freund’s adjuvant induced rats. Exp. Toxicol. Pathol. 2017, 69, 672–680.
- Manikandan, R.; Parimalanandhini, D.; Mahalakshmi, K.; Beulaja, M.; Arumugam, M.; Janarthanan, S.; Palanisamy, S.; You, S.; Prabhu, N.M. Studies on isolation, characterization of fucoidan from brown algae Turbinaria decurrens and evaluation of it’s in vivo and in vitro anti-inflammatory activities. Int. J. Biol. Macromol. 2020, 160, 1263–1276.
- Atashrazm, F.; Lowenthal, R.M.; Woods, G.M.; Holloway, A.F.; Dickinson, J.L. Fucoidanand cancer: A multifunctional molecule with anti-tumor potential. Mar. Drugs 2015, 13, 2327–2346.
- Yan, M.D.; Yao, C.J.; Chow, J.M.; Chang, C.L.; Hwang, P.A.; Chuang, S.E.; Peng, J.W.; Lai, G.M. Fucoidan elevates MicroRNA-29b to regulate DNMT3B-MTSS1 Axis and inhibit EMT in human hepatocellular carcinoma cells. Mar. Drugs 2015, 13, 6099.
- Marinval, N.; Saboural, P.; Haddad, O.; Maire, M.; Bassand, K.; Geinguenaud, F.; Djaker, N.; Ben Akrout, K.; Lamy de la Chapelle, M.; Robert, R.; et al. Identification of a pro-angiogenic potential and cellular uptake mechanism of a LMW highly sulfated fraction of Fucoidan from Ascophyllum nodosum. Mar. Drugs 2016, 14, 185.
- Han, Y.S.; Lee, J.H.; Lee, S.H. Fucoidan inhibits themigration and proliferation of HT- 29 human colon cancer cells via the phosphoinositide-3 kinase/Akt/mechanistic target of rapamycin pathways. Mol. Med. Rep. 2015, 12, 3446–3452.
- Xue, M.; Liang, H.; Tang, Q.; Xue, C.; He, X.; Zhang, L.; Zhang, Z.; Liang, Z.; Bian, K.; Zhang, L.; et al. The protective and Immunomodulatory effects of Fucoidan against 7,12-dimethyl benzanthracene-induced experimental mammary carcinogenesis through the PD1/PDL1 signaling pathway in rats. Nutr. Cancer 2017, 69, 1234–1244.
- Yang, G.; Zhang, Q.; Kong, Y.; Xie, B.; Gao, M.; Tao, Y.; Xu, H.; Zhan, F.; Dai, B.; Shi, J.; et al. Antitumor activity of fucoidan against diffuse large B cell lymphoma in vitro and in vivo. Acta Biochim. Biophys. Sin. Shanghai 2015, 47, 9.
- Yoshimoto, M.; Higaki, K.; Nanba, E.; Ikeguchi, M. Anti-proliferation activity of Fucoidan in MKN45 gastric cancer cells and downregulation of phosphorylated ASK1, a cell cycle-regulated kinase. Yonago Acta Med. 2015, 58, 1–7.
- Etman, S.M.; Elnaggar, Y.S.R.; Abdallah, O.Y. Fucoidan, a natural biopolymer in cancer combating: From edible algae to nanocarrier tailoring. Int. J. Biol. Macromol. 2020, 147, 799–808.
- Zhang, Z.; Teruya, K.; Eto, H.; Shirahata, S. Fucoidan extract induces apoptosis inMCF-7 cells via a mechanism involving the ROS-dependent JNK activation and mitochondria-mediated pathways. PLoS ONE 2011, 6, e27441.
- Li, J.; Chen, K.; Li, S.; Liu, T.; Wang, F.; Xia, Y.; Lu, J.; Zhou, Y.; Guo, C. Pretreatment with Fucoidan from Fucus vesiculosus protected against ConA-induced acute liver injury by inhibiting both intrinsic and extrinsic apoptosis. PLoS ONE 2016, 11, e0152570.
- Ustyuzhanina, N.E.; Bilan, M.I.; Ushakova, N.A.; Usov, A.I.; Kiselevskiy, M.V.; Nifantiev, N.E. Fucoidans: Pro- or antiangiogenic agents? Glycobiology 2014, 24, 1265–1274.
- Rui, X.; Pan, H.F.; Shao, S.L.; Xu, X.M. Anti-tumor and anti-angiogenic effects of Fucoidan on prostate cancer: Possible JAK-STAT3 pathway. BMC Complement. Altern. Med. 2017, 17, 378.
- Chen, H.; Cong, Q.; Du, Z.; Liao, W.; Zhang, L.; Yao, Y.; Ding, K. Sulfated fucoidan FP08S2 inhibits lung cancer cell growth in vivo by disrupting angiogenesis via targeting VEGFR2/VEGF and blocking VEGFR2/Erk/VEGF signaling. Cancer Lett. 2016, 382, 44–52.
- Lee, H.; Kim, J.S.; Kim, E. Fucoidan from seaweed Fucus vesiculosus inhibits migration and invasion of human lung Cancer cell via PI3K-Akt-mTOR pathways. PLoS ONE 2012, 7, e50624.
- Cho, T.M.; Kim, W.J.; Moon, S.K. AKT signaling is involved in fucoidan-induced inhibition of growth and migration of human bladder cancer cells. Food Chem. Toxicol. 2014, 64, 344–352.
- Teruya, T.; Tatemoto, H.; Konishi, T.; Tako, M. Structural characteristics and in vitro macrophage activation of acetyl fucoidan from Cladosiphon okamuranus. Glycoconj. J. 2009, 26, 1019–1028.
- Hou, Y.; Wang, J.; Jin, W.; Zhang, H.; Zhang, Q. Degradation of Laminaria japonica fucoidan by hydrogen peroxide and antioxidant activities of the degradation products of different molecular weights. Carbohydr. Polym. 2012, 87, 153–159.
- Imbs, T.I.; Skriptsova, A.V.; Zvyagintseva, T.N. Antioxidant activity of fucose-containing sulfated polysaccharides obtained from Fucus evanescens by different extraction methods. J. Appl. Phycol. 2015, 27, 545–553.
- Park, H.Y.; Kim, G.Y.; Moon, S.K.; Kim, W.J.; Yoo, Y.H.; Choi, Y.H. Fucoidan inhibits the proliferation of human urinary bladder cancer T24 cells by blocking cell cycle progression and inducing apoptosis. Molecules 2014, 19, 5981–5998.
- Kim, E.J.; Park, S.Y.; Lee, J.Y.; Park, J.H. Fucoidan present in brown algae induces apoptosis of human colon cancer cells. BMC Gastroenterol. 2010, 10, 96.
- Hsu, H.Y.; Lin, T.Y.; Hu, C.H.; Shu, D.T.F.; Lu, M.K. Fucoidan upregulates TLR4/CHOP-mediated caspase-3 and PARP activation to enhance cisplatin-induced cytotoxicity in human lung cancer cells. Cancer Lett. 2018, 432, 112–120.
- Teng, H.; Yang, Y.; Wei, H. Fucoidan Suppresses Hypoxia-Induced Lymphangiogenesis and Lymphatic Metastasis in Mouse Hepatocarcinoma. Mar. Drugs 2015, 13, 3514–3530.
- Mabeau, S.; Kloareg, B.; Joseleau, J.P. Fractionation and analysis of fucans from brown algae. Phytochemistry 1990, 29, 2441–2445.
- Alwarsamy, M.; Gooneratne, R.; Ravichandran, R. Effect of fucoidan from Turbinaria conoides on human lung adenocarcinoma epithelial (A549) cells. Carbohydr. Polym. 2016, 152, 207–213.
- Holtkamp, A.D.; Kelly, S.; Ulber, R.; Lang, S. Fucoidans and fucoidanases--focus on techniques for molecular structure elucidation and modification of marine polysaccharides. Appl. Microbiol. Biotechnol. 2009, 82, 1–11.
- Siegel, R.L.; Miller, K.D.; Fedewa, S.A. Colorectal cancer statistics, 2017. CA Cancer J. Clin. 2017, 67, 177–193.
- Thinh, P.D.; Menshova, R.V.; Ermakova, S.P.; Anastyuk, S.D.; Ly, B.M.; Zvyagintseva, T.N. Structural characteristics and anticancer activity of fucoidan from the brown alga Sargassum mcclurei. Mar. Drugs 2013, 11, 1456–1476.
- Back, H.I.; Kim, S.Y.; Park, S.H.; Oh, M.R.; Kim, M.G.; Jeon, J.Y.; Chae, S.W.; Bae, J.S.; Kim, Y.S.; Hwang, Y.J.; et al. Effects of Fucoidan supplementation on Helicobacter pylori in humans. FASEB J. 2010, 24, lb347.
- Vishchuk, O.S.; Ermakova, S.P.; Zvyagintseva, T.N. The fucoidans from brown algae of Far-Eastern seas: Anti-tumor activity and structure-function relationship. Food Chem. 2013, 141, 1211–1217.
- Jin, W.; Cai, X.F.; Na, M.; Lee, J.J.; Bae, K. Triterpenoids and diarylheptanoids from Alnus hirsuta inhibit HIF-1 in AGS cells. Arch. Pharm. Res. 2007, 30, 412–418.
- Ale, M.T.; Mikkelsen, J.D.; Meyer, A.S. Important determinants for fucoidan bioactivity: A critical review of structure-function relations and extraction methods for fucose-containing sulfated polysaccharides from brown seaweeds. Mar. Drugs 2011, 9, 2106–2130.
- Huang, T.H.; Chiu, Y.H.; Chan, Y.L. Prophylactic administration of fucoidan represses cancer metastasis by inhibiting vascular endothelial growth factor (VEGF) and matrix metalloproteinases (MMPs) in Lewis tumor-bearing mice. Mar. Drugs 2015, 13, 1882–1900.
- Iqbal, M.W.; Riaz, T.; Mahmood, S.; Bilal, M.; Manzoor, M.F.; Qamar, S.A.; Qi, X. Fucoidan-based nanomaterial and its multifunctional role for pharmaceutical and biomedical applications. Crit. Rev. Food Sci. Nutr. 2022, 2022, 1–27.
- Cunha, L.; Grenha, A. Sulfated seaweed polysaccharides as multifunctional materials in drug delivery applications. Mar. Drugs 2016, 14, 42.
- Cardoso, M.J.; Costa, R.R.; Mano, J.F. Marine origin polysaccharides in drug delivery systems. Mar. Drugs 2016, 14, 34.
- Sezer, A.D.; Cevher, E. Fucoidan: A versatile biopolymer for biomedical applications. In Active Implants and Scafolds for Tissue Regeneration; Zilberman, M., Ed.; Springer: Berlin/Heidelberg, Germany, 2011; Volume 8, pp. 377–406.
- Huang, Y.C.; Yang, Y.T. Effect of basic fibroblast growth factor released from chitosan–fucoidan nanoparticles on neurite extension. J. Tissue Eng. Regen. Med. 2016, 10, 418–427.
- Lee, H.M.; Kim, J.K.; Cho, T.S. Applications of ophthalmic biomaterials embedded with fucoidan. Ind. Eng. Chem. 2012, 18, 1197–1201.
- Fan, L.; Lu, Y.; Ouyang, X.K.; Ling, J. Development and characterization of soybean protein isolate and fucoidan nanoparticles for curcumin encapsulation. Int. J. Biol. Macromol. 2021, 169, 194–205.
- Park, H.W.; Kim, D.Y.; Shin, W.S. Fucoidan improves the structural integrity and the molecular stability of β-lactoglobulin. Food Sci. Biotechnol. 2018, 27, 1247–1255.
- Kim, H.; Nguyen, V.P.; Manivasagan, P.; Jung, M.J.; Kim, S.W.; Oh, J.; Kang, H.W. Doxorubicin-fucoidan-gold nanoparticles composite for dual-chemo-photothermal treatment on eye tumors. Oncotarget 2017, 8, 113719–113733.
- Wang, P.; Kankala, R.K.; Chen, B.; Long, R.; Cai, D.; Liu, Y.; Wang, S. Poly-allylamine hydrochloride and fucoidan-based self-assembled polyelectrolyte complex nanoparticles for cancer therapeutics. J. Biomed. Mater. Res. A 2019, 107, 339–347.
- Huang, Y.C.; Kuo, T.H. O-carboxylmethyl chitosan/fucoidan nanoparticles increase cellular curcumin uptake. Food Hydrocoll. 2016, 53, 261–269.
- Hwang, P.A.; Lin, X.Z.; Kuo, K.L.; Hsu, F.Y. Fabrication and cytotoxicity of fucoidan-cisplatin nanoparticles for macrophage and tumor cells. Materials 2017, 10, 291.
- Hussain, N.; Jaitley, V.; Florence, A.T. Recent advances in the understanding of uptake of microparticulates across the gastrointestinal lymphatics. Adv. Drug Deliv. Rev. 2001, 50, 107–142.
- Gänger, S.; Schindowski, K. Tailoring Formulations for Intranasal Nose-to-Brain Delivery: A Review on Architecture, Physico-Chemical Characteristics and Mucociliary Clearance of the Nasal Olfactory Mucosa. Pharmaceutics 2018, 10, 116.
- Sezer, A.D.; Akbuǧa, J. The design of biodegradable ofloxacin-based core-shell microspheres: Influence of the formulation parameters on in vitro characterization. Pharm. Dev. Technol. 2012, 17, 118–124.
- Sezer, A.D.; Cevher, E.; Hatipoğlu, F.; Oğurtan, Z.; Baş, A.L.; Akbuğa, J. The use of fucosphere in the treatment of dermal burns in rabbits. Eur. J. Pharm. Biopharm. 2008, 69, 189–198.
- Li, B.; Juenet, M.; Aid-Launais, R.; Maire, M.; Ollivier, V.; Letourneur, D.; Chauvierre, C. Development of polymer microcapsules functionalized with fucoidan to target P-selectin overexpressed in cardiovascular diseases. Adv. Health Mater. 2017, 6, 160.
- Szekalska, M.; Citkowska, A.; Wróblewska, M.; Winnicka, K. The Impact of Gelatin on the Pharmaceutical Characteristics of Fucoidan Microspheres with Posaconazole. Materials 2021, 14, 4087.
- Valente, S.A.; Silva, L.M.; Lopes, G.R.; Sarmento, B.; Coimbra, M.A.; Passos, C.P. Polysaccharide-based formulations as potential carriers for pulmonary delivery—A review of their properties and fates. Carbohydr. Polym. 2022, 277, 118784.
- Cunha, L.; Rodrigues, S.; Rosa da Costa, A.M.; Faleiro, M.L.; Buttini, F.; Grenha, A. Inhalable fucoidan microparticles combining two antitubercular drugs with potential application in pulmonary tuberculosis therapy. Polymers 2018, 10, 636.
- Deepika, M.S.; Thangam, R.; Sheena, T.S.; Sasirekha, R.; Sivasubramanian, S.; Babu, M.D.; Jeganathan, K.; Thirumurugan, R. A novel rutin-fucoidan complex based phytotherapy for cervical cancer through achieving enhanced bioavailability and cancer cell apoptosis. Biomed. Pharmacother 2019, 109, 1181–1195.
- Moustafa, M.A.; El-Refaie, W.M.; Elnaggar, Y.S.; El-Mezayen, N.S.; Awaad, A.K.; Abdallah, O.Y. Fucoidan/hyaluronic acid cross-linked zein nanoparticles loaded with fisetin as a novel targeted nanotherapy for oral cancer. Int. J. Biol. Macromol. 2023, 241, 124528.
- Wang, P.; Kankala, R.K.; Fan, J.; Long, R.; Liu, Y.; Wang, S. Poly-L-ornithine/fucoidan-coated calcium carbonate microparticles by layer-by-layer self-assembly technique for cancer theranostics. J. Mater. Sci. Mater. Med. 2018, 29, 68.
- Abdelkader, D.H.; Elekhnawy, E.; Negm, W.A.; El-Masry, T.A.; Almukainzi, M.; Zayed, A.; Ulber, R. Insight into Fucoidan-Based PEGylated PLGA Nanoparticles Encapsulating Methyl Anthranilic Acid: In Vitro Evaluation and In Vivo Anti-Inflammatory Study. Mar. Drugs 2022, 20, 694.
- Lai, Y.H.; Chiang, C.S.; Hsu, C.H.; Cheng, H.W.; Chen, S.Y. Development and Characterization of a Fucoidan-Based Drug Delivery System by Using Hydrophilic Anticancer Polysaccharides to Simultaneously Deliver Hydrophobic Anticancer Drugs. Biomolecules 2020, 10, 970.
- Huang, Y.C.; Chen, J.K.; Lam, U.I.; Chen, S.Y. Preparing, characterizing, and evaluating chitosan/fucoidan nanoparticles as oral delivery carriers. J. Polym. Res. 2014, 21, 415.
- Tsai, L.C.; Chen, C.H.; Lin, C.W.; Ho, Y.C.; Mi, F.L. Development of mutlifunctional nanoparticles self-assembled from trimethyl chitosan and fucoidan for enhanced oral delivery of insulin. Int. J. Biol. Macromol. 2019, 126, 141–150.
- Chen, C.H.; Lin, Y.S.; Wu, S.J.; Mi, F.L. Mutlifunctional nanoparticles prepared from arginine-modified chitosan and thiolated fucoidan for oral delivery of hydrophobic and hydrophilic drugs. Carbohydr. Polym. 2018, 193, 163–172.
- Yu, S.H.; Tang, D.W.; Hsieh, H.Y.; Wu, W.S.; Lin, B.X.; Chuang, E.Y.; Sung, H.W.; Mi, F.L. Nanoparticle-induced tight-junction opening for the transport of an anti-angiogenic sulfated polysaccharide across Caco-2 cell monolayers. Acta Biomater. 2013, 9, 7449–7459.
- Lin, Y.H.; Lu, K.Y.; Tseng, C.L.; Wu, J.Y.; Chen, C.H.; Mi, F.L. Development of genipin-crosslinked fucoidan/chitosan-N-arginine nanogels for preventing Helicobacter infection. Nanomed 2017, 12, 1491–1510.
- Lee, M.C.; Huang, Y.C. Soluble eggshell membrane protein-loaded chitosan/fucoidan nanoparticles for treatment of defective intestinal epithelial cells. Int. J. Biol. Macromol. 2019, 131, 949–958.
- Liu, Q.; Chen, J.; Qin, Y.; Jiang, B.; Zhang, T. Zein/fucoidan-based composite nanoparticles for the encapsulation of pterostilbene: Preparation, characterization, physicochemical stability, and formation mechanism. Int. J. Biol. Macromol. 2020, 158, 461–470.
- Haggag, Y.; Abu Ras, B.; El-Tanani, Y.; Tambuwala, M.M.; McCarron, P.; Isreb, M.; El-Tanani, M. Co-delivery of a RanGTP inhibitory peptide and doxorubicin using dual-loaded liposomal carriers to combat chemotherapeutic resistance in breast cancer cells. Expert Opin. Drug Deliv. 2020, 17, 1655–1669.
- Qadir, S.A.; Kwon, M.C.; Han, J.G.; Ha, J.H.; Jin, L.; Jeong, H.S.; Kim, J.C.; You, S.G.; Lee, H.Y. Enhancement of immunomodulatory and anticancer activity of fucoidan by nano encapsulation. Food Sci. Biotechnol. 2008, 17, 1254–1260.
- Lima Salviano, T.; dos Santos, M.; Charles, D.; de Siqueira Ferraz Carvalho, R.; Pereira, M.A.; de Arruda, B.; Santos, V.; dos Santos Aguiar, J.; Souto, F.O.; da Silva, C.; et al. Fucoidan-Coated Liposomes: A Target System to Deliver the Antimicrobial Drug Usnic Acid to Macrophages Infected with Mycobacterium tuberculosis. J. Biomed. Nanotechnol. 2021, 17, 1699–1710.
- Zhang, X.; Wei, Z.; Xue, C. Physicochemical properties of fucoidan and its applications as building blocks of nutraceutical delivery systems. Crit. Rev. Food Sci. Nutr. 2021, 62, 8935–8953.
- Choi, D.G.; Venkatesan, J.; Shim, M.S. Selective Anticancer Therapy Using Pro-Oxidant Drug-Loaded Chitosan-Fucoidan Nanoparticles. Int. J. Mol. Sci. 2019, 20, 3220.
- Rioux, L.; Turgeon, S.L.; Beaulieu, M. Rheological characterisation of polysaccharides extracted from brown seaweeds. J. Sci. Food Agric. 2007, 87, 1630–1638.
- Lu, K.Y.; Li, R.; Hsu, C.H.; Lin, C.W.; Chou, S.C.; Tsai, M.L.; Mi, F.L. Development of a new type of multifunctional fucoidan-based nanoparticles for anticancer drug delivery. Carbohydr. Polym. 2017, 165, 410–420.
- Pawar, V.K.; Singh, Y.; Sharma, K.; Shrivastav, A.; Sharma, A.; Singh, A.; Meher, J.G.; Singh, P.; Raval, K.; Kumar, A.; et al. Improved chemotherapy against breast cancer through immunotherapeutic activity of fucoidan decorated electrostatically assembled nanoparticles bearing doxorubicin. Int. J. Biol. Macromol. 2019, 122, 1100–1114.
- Jang, B.; Moorthy, M.S.; Manivasagan, P.; Xu, L.; Song, K.; Lee, K.D.; Kwak, M.; Oh, J.; Jin, J.O. Fucoidan-coated CuS nanoparticles for chemo- and photothermal therapy against cancer. Oncotarget 2018, 9, 12649–12661.
- da Silva, L.C.; Garcia, T.; Mori, M.; Sandri, G.; Bonferoni, M.C.; Finotelli, P.V.; Cinelli, L.P.; Caramella, C.; Cabral, L.M. Preparation and characterization of polysaccharide-based nanoparticles with anticoagulant activity. Int. J. Nanomed. 2012, 7, 2975–2986.
- Barbosa, A.I.; Costa Lima, S.S.; Reis, S. Development of methotrexate loaded fucoidan/chitosan nanoparticles with anti-inflammatory potential and enhanced skin permeation. Int. J. Biol. Macromol. 2019, 124, 1115–1122.
- Huang, Y.C.; Lam, U.I. Chitosan/fucoidan pH sensitive nanoparticles for oral delivery system. J. Chin. Chem. Soc. 2011, 58, 779–785.
- Guo, R.; Deng, M.; He, X.; Li, M.; Li, J.; He, P.; Liu, H.; Li, M.; Zhang, Z.; He, Q. Fucoidan-functionalized activated platelet-hitchhiking micelles simultaneously track tumor cells and remodel the immunosuppressive microenvironment for efficient metastatic cancer treatment. Acta Pharm. Sin. B 2022, 12, 467–482.
- Kang, S.; Kang, K.; Chae, A.; Kim, Y.K.; Jang, H.; Min, D.H. Fucoidan-coated coral-like Pt nanoparticles for computed tomography-guided highly enhanced synergistic anticancer effect against drug-resistant breast cancer cells. Nanoscale 2019, 11, 15173–15183.
- Jafari, M.; Sriram, V.; Xu, Z.; Harris, G.M.; Lee, J.Y. Fucoidan-Doxorubicin Nanoparticles Targeting P-Selectin for Effective Breast Cancer Therapy. Carbohydr. Polym. 2020, 249, 116837.
- DuRoss, A.N.; Landry, M.R.; Thomas, C.R.; Neufeld, M.J.; Sun, C. Fucoidan-coated nanoparticles target radiation-induced P-selectin to enhance chemoradiotherapy in murine colorectal cancer. Cancer Lett. 2021, 500, 208–219.
- Chen, M.L.; Lai, C.J.; Lin, Y.N.; Huang, C.M.; Lin, Y.H. Multifunctional nanoparticles for targeting the tumor microenvironment to improve synergistic drug combinations and cancer treatment effects. J. Mater. Chem. 2020, 8, 10416–10427.
- Oliveira, C.; Gonçalves, C.S.; Martins, E.P.; Neves, N.M.; Reis, R.L.; Costa, B.M.; Silva, T.H.; Martins, A. Fucoidan/chitosan nanoparticles functionalized with anti-ErbB-2 target breast cancer cells and impair tumor growth in vivo. Int. J. Pharm. 2021, 600, 120548.
- Cavalcanti, I.D.L.; Ximenes, R.M.; Pessoa, O.D.L.; Magalhães, N.S.S.; Lira-Nogueira, M.C.B. Fucoidan-coated PIBCA nanoparticles containing oncocalyxone A: Activity against metastatic breast cancer cells. J. Drug Deliv. Sci. Technol. 2021, 65, 102698.
- Shamay, Y.; Elkabets, M.; Li, H.; Shah, J.; Brook, S.; Wang, F.; Adler, K.; Baut, E.; Scaltriti, M.; Jena, P.V. P-selectin is a nanotherapeutic delivery target in the tumor microenvironment. Sci. Transl. Med. 2016, 8, 345.
- Tsai, H.L.; Tai, C.J.; Huang, C.W.; Chang, F.R.; Yuan, J.; Wang, J.Y. Efficacy of low-molecular-weight fucoidan as a supplemental therapy in metastatic colorectal cancer patients: A double-blind randomized controlled trial. Mar. Drugs 2017, 15, 122.
- Tomori, M.; Nagamine, T.; Miyamoto, T.; Iha, M. Effects of Ingesting Fucoidan Derived from Cladosiphon okamuranus Tokida on Human NK Cells: A Randomized, Double-Blind, Parallel-Group, Placebo-Controlled Pilot Study. Mar. Drugs 2021, 19, 340.
- Ikeguchi, M.; Yamamoto, M.; Arai, Y.; Maeta, Y.; Ashida, K.; Katano, K.; Miki, Y.; Kimura, T. Fucoidan reduces the toxicities of chemotherapy for patients with unresectable advanced or recurrent colorectal cancer. Oncol. Lett. 2011, 2, 319–322.
- Tsai, H.; Yeh, Y.; Chen, P.; Chang, Y.; Chen, Y.; Li, C.; Su, W.; Chang, T.; Huang, C.; Wang, J. The auxiliary effects of low-molecular-weight fucoidan on the quality of life for locally advanced rectal cancer patients receiving neoadjuvant concurrent chemoradiotherapy before surgery: A double-blind, randomized, placebo- controlled study. Res. Sq. 2023, 2023, 1–25.
- A Randomized, Double-Blind Study to Evaluate the Clinical Effect and Safety of Fucoidan in Patients with Squamous Cell Carcinomas of the Head and Neck. ClinicalTrials.gov Identifier: NCT04597476, Taiwan; 2020. Available online: https://clinicaltrials.gov/ct2/show/NCT04597476#contacts (accessed on 1 June 2023).
- Study of Oligo-Fucoidan in Advanced Hepatocellular Carcinoma. ClinicalTrials.gov Identifier: NCT04066660, China; 2019. Available online: https://clinicaltrials.gov/ct2/show/NCT04066 (accessed on 1 June 2023).
- To Evaluate the Quality of Life Improvement of Oral Oligo Fucoidan in Subjects Receiving Platinum-Based Chemotherapy with Non-Small Cell Lung Cancer. ClinicalTrials.gov Identifier: NCT03130829, Taiwan; 2019. Available online: https://clinicaltrials.gov/ct2/show/NCT03130829 (accessed on 1 June 2023).
- Tocaciu, S.; Oliver, L.J.; Lowenthal, R.M.; Peterson, G.M.; Patel, R.; Shastri, M.; McGuinness, G.; Olesen, I.; Fitton, J.H. The Effect of Undaria pinnatifida Fucoidan on the Pharmacokinetics of Letrozole and Tamoxifen in Patients with Breast Cancer. Integr. Cancer Ther. 2018, 17, 99–105.
More
Information
Subjects:
Pharmacology & Pharmacy
Contributors
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
1.2K
Revisions:
2 times
(View History)
Update Date:
01 Aug 2023
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





