Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Waheb A. Jabbar | -- | 2534 | 2022-11-14 09:08:48 | | | |
| 2 | Conner Chen | + 12 word(s) | 2546 | 2022-11-15 08:49:56 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Abdulmalek, S.; Nasir, A.; Jabbar, W.A.; Almuhaya, M.A.M.; Bairagi, A.K.; Khan, M.A.; Kee, S. Internet of Wearable Things. Encyclopedia. Available online: https://encyclopedia.pub/entry/34446 (accessed on 22 May 2026).
Abdulmalek S, Nasir A, Jabbar WA, Almuhaya MAM, Bairagi AK, Khan MA, et al. Internet of Wearable Things. Encyclopedia. Available at: https://encyclopedia.pub/entry/34446. Accessed May 22, 2026.
Abdulmalek, Suliman, Abdul Nasir, Waheb A. Jabbar, Mukarram A. M. Almuhaya, Anupam Kumar Bairagi, Md. Al-Masrur Khan, Seong-Hoon Kee. "Internet of Wearable Things" Encyclopedia, https://encyclopedia.pub/entry/34446 (accessed May 22, 2026).
Abdulmalek, S., Nasir, A., Jabbar, W.A., Almuhaya, M.A.M., Bairagi, A.K., Khan, M.A., & Kee, S. (2022, November 14). Internet of Wearable Things. In Encyclopedia. https://encyclopedia.pub/entry/34446
Abdulmalek, Suliman, et al. "Internet of Wearable Things." Encyclopedia. Web. 14 November, 2022.
Copy Citation
The Internet of Wearable Things (IoWT) aims to improve people’s quality of daily life. It involves sensors fitted into wearable devices, monitoring the individual’s activity, health factors, and other things.
IoT
IoWT
healthcare
1. Internet of Wearable Things
The Internet of Wearable Things (IoWT) aims to improve people’s quality of daily life. It involves sensors fitted into wearable devices, monitoring the individual’s activity, health factors, and other things. The data collected from the IoWT can be fed into medical infrastructure, giving clinicians remote access to their patients’ data as they go about their daily lives. Building on the internet of things (IoT) architecture, a novel integrative framework for IoWT is currently being developed. The IoWT is a revolutionary technology that has the potential to change the healthcare industry by creating an ecosystem for automated telehealth treatments [1].
As shown in Figure 1, the architecture of the IoWT and its connections consists of three elements: the WBAN, the gateway connected to the Internet, and the cloud. The WBAN is a front-end component of IoWT that wraps around the body to collect health-related data unnoticed. The WBAN collects data from sensors in direct contact with the body or from sensors in the environment that can collect indirect data about a person’s behavior. The WBAN can either analyze the data or transmit them for remote analysis. In addition, mobile computing devices such as smartphones, tablets, and laptops must be connected to the Internet to send data to powerful computing resources [2].
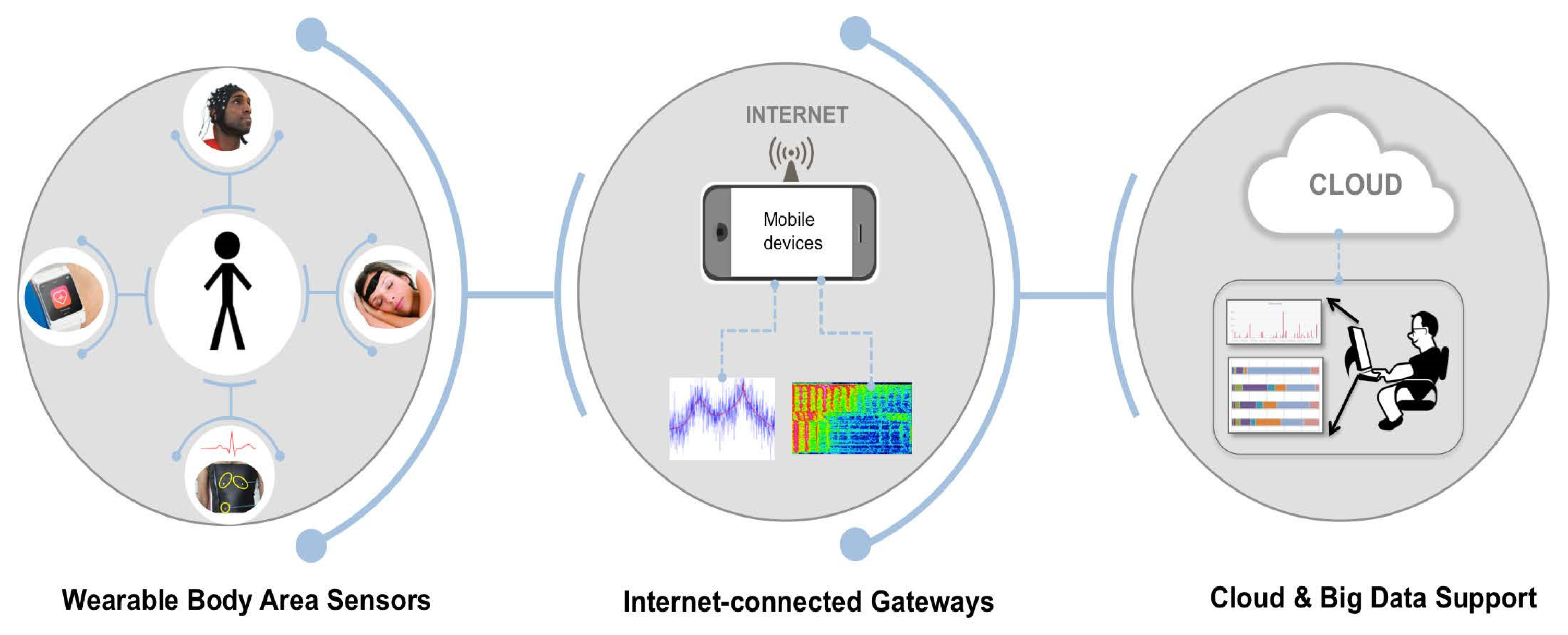
Figure 1. Architectural elements of IoWT [2].
2. Wireless Network Technologies for IoT Healthcare
Healthcare systems can be monitored remotely using various wireless network technologies. The existence and operation of IoT emerging technologies, such as RFID, wireless network technologies (BLE, Wi-Fi, Zigbee), and low-power wireless area network (LPWAN) technologies (such as LoRa and SigFox) are engaging in terms of the IoT’s long-term development and deployment. They enhance device connectivity to the Internet, and the efficiency of IoT application operation [3].
BLE, LoRa, and Zigbee are wireless sensor network technologies; meanwhile, to identify and trace products, RFID is used. BLE can transfer data between different mobile devices [4]. Communication methods can be long in their range (LoRa, SigFox, and Wi-Fi) or short-range (Bluetooth, RFID, and Zigbee) [5]. Due to new communication protocols being created exclusively for IoT devices, such as LoraWAN, NB-IoT, and Sigfox, it is anticipated that the popularity of these applications will increase, enabling a far-reaching remote monitoring system [6][7].
An essential component of the IoT is the WSN. The IoT, which has already been established, can connect things to the Internet, allowing humans to interact with computers and for computers to interact with other computers. Thus, the combination of the IoT and WSN facilitates machine-to-machine communication. Figure 2 illustrates the architecture of IoT with the WSN. It shows sensor nodes communicating with a gateway in a separate network. Many devices are linked to the gateway via Wi-Fi or the Internet, ensuring interoperability [8].

Figure 2. Relationship of WSN to IoT [8].
The researchers in [5] counted the existing wireless applications in connected healthcare facilities to study operational wireless methods for transmitting data across short distances. The system design and implementation of family mobile medical care are presented in this study. The Android mobile client, data transmission, and a system server are part of the system. Wireless data transfer is potentially possible, at least in theory. An example of the mobile healthcare system’s success is shown here. In the first place, family members’ sign characteristics might be collected via sensors on medical equipment. electrocardiograph (ECG), blood pressure (BP), blood-oxygen saturation (SpO2), respiration, and sleep are parameters of interest. The mobile terminal uploads data to a back-end Web server with a wireless network, Bluetooth, and Wi-Fi. Data storage, computation, and analysis are all handled by the MySQL database server [5]. A family member’s smartphone or tablet may be used to show data icons or text, making it easy for them to monitor their loved one’s health at any time and location. Family members may prevent significant health issues through early intervention, encouragement, and healthcare maintenance.
3. Wearable Sensors in Healthcare-Monitoring Systems
In real-time, the healthcare sector may use wearable devices to monitor and save patients’ activity and physiological functions. Such devices have one or more sensor nodes, but each sensor node typically has a radio transceiver, a low-speed processing unit, and small memory. The sensors can measure various physiological parameters and activity, including SpO2, BP and temperature, electrodermal activity (EDA), electrocardiograph (ECG), electromyography, heart rate (HR), and RR [9][10].
Bluetooth, infrared, near-field communication (NFC), RFID, Wi-Fi, and Zigbee wireless transceiver technologies can support wearable devices communicating with smartphones and other devices. The technology promotes care by facilitating remote diagnosis and monitoring [6]. An important issue of discussion in this period revolves around the IoT in healthcare. One of the essential parts of healthcare is identifying and treating illness. In order to achieve this, the body sensor network will be valuable. Additionally, the data may be accessible from any location in the world [11].
A wearable sensor gadget created by Vedaei can monitor and analyze the actions of patients. An IoT technology that measures social distance might help prevent a COVID-19 sufferer from becoming sick. Three layers of IoT sensors, machine learning algorithms, and smartphone apps are used to monitor BP, SpO2, cough rate, and temperature daily. The frameworks outlined by the authors helped the users keep a safe distance between themselves and the transmission of the virus and update their information often. A distance-monitoring system based on Radio Frequency (RF) was also presented in the research, which may be used in both indoor and outdoor contexts. In order to compare the findings under environmental restrictions, the authors looked at two alternative situations. Those who wrote the article claim to have helped expose COVID-19 [12].
Another study [13] demonstrated an IoT-connected wearable sensor network system for industrial outdoor workplace health and safety applications. Wearable sensors worn by the worker collect physiological and environmental data, which are transferred to the system operator and employees for monitoring and analysis. Data harvested from multiple workers wearing wearable sensors can be transferred through a LoRa network to a gateway. The LoRa network combines a Bluetooth-based medical signal-detecting network with a heterogeneous IoT platform. The authors describe the sensor node hardware and design, the gateway, and the cloud application. A heterogeneous wearable IoT device sensor network system for health and safety usage is shown in Figure 3.

Figure 3. Healthcare-monitoring system using wearable sensor [13].
3.1. Use Cases of Health-Monitoring Sensors
Medical science research is currently dominated by medical healthcare, which mostly relies on how it integrates with the IoT. This integration is receiving a lot of attention due to its crucial role in utilizing technological paradigms to save human lives. These integrated systems contain three crucial phases, namely, the modules for data collection, data processing, and data evaluation. Healthcare monitoring plays a significant role in the data collection module due to its active involvement in gathering data from various sources and specimens. Most healthcare-monitoring systems use sensors to obtain the necessary input data. The more concise and timely the data, the more accurate the results.
Sensors are employed for more than just data collection; they can also be used for various ongoing and post-monitoring tasks in IoT-based healthcare systems. Blood pressure, body temperature, pulse oximetry, and blood glucose are a few examples of heterogeneous wearable sensing devices developed to collect patients’ biomedical data [14] in the era of fast-growing IoT. The proper quality and development of these IoT-based healthcare-monitoring systems are directly related to reliable data from sensors or sensor networks, which necessitates using advanced signal-processing techniques, sensor data fusion, and data analytics. In medical science, sensors that measure heart rate, body temperature, and other things are used to find and diagnose diseases at the earliest stage.
It has been observed that health-monitoring sensors are utilized in various use cases of medical science for healthcare purposes, such as the monitoring of hemoglobin concentration, molecular diagnostics, clinical diagnosis of albumin-related diseases, heart-rate detection, blood-oxygen-saturation detection, respiratory-rate detection, anemia detection, Alzheimer’s disease, and many more.
There are many applications for wearable sensors. IoT-assisted wearables are widely used these days. The friendliness of such devices has created a boom in their application in all fields. With the healthcare field being no exception, the IoT’s exploits in healthcare are enormous. Various technologies are linked to existing technology that helps generate data for monitoring and analysis.
There is a lot of use cases for IoT-based sensors in real-time environments, which are mentioned below:
Use Cases/Applications
1. Heart-rate detection/Cardiac monitoring systems/Stroke
The first application of health-monitoring sensors was through IoT-based healthcare-monitoring systems; these can gather and measure the necessary data, transmit these data through various stages reliably to the gateway and the cloud server, and perform some edge tasks to provide low-latency decision-making for cardiac-related diseases and prediction. Some of the pieces utilize sensors to determine heart rate [15]. Several projects involve using WSN technology to continuously monitor heart patients who need a real-time monitoring system [16]. This WSN has several medical-grade sensors and devices that can track blood pressure, body temperature, heart rate, and pulse. A critical patient’s real-time ECG is also preserved so that the patient is continuously watched [16][17][18][19][20].
- 2.
-
Body-temperature measuring
During the pandemic, IoT-based smart health-monitoring devices with sensors for COVID-19 patients based on body temperature, pulse, and SpO2 were beneficial. Through a mobile application, these systems can measure a human’s body temperature, oxygen saturation, and pulse rate [21].
- 3.
-
Activity recognition
One of the many uses for medical wearables now being used is activity recognition. Almost all fitness trackers perform this kind of recognition. Fitness trackers are now the most popular wearables for tracking a person’s activity. A lot of guesswork is being carried out in the background, but most of them include a highly sensitive 3D accelerometer that allows the sensor to determine the acceleration [15].
- 4.
-
Blood-glucose monitoring and hemoglobin concentration
Heart-rate sensors, blood-glucose monitors, endoscopic capsules, and other devices make up the Internet of Medical Things (IoMT), which together, create the IoMT diabetic-based WBSN monitoring system [22][23].
5. Respiration-rate detection and monitoring
Some writers employed sophisticated sensors that keep track of breathing patterns. A bio-impedance sensor can be useful [15][24][25].
- 6.
-
Sleep monitoring
This sleep-tracking app assists the user in adjusting their sleep patterns and maintaining a healthy life cycle. For this, various sensors are utilized. Wearables often track heart rate, pulse rate, SpO2 levels, and breathing patterns, and by taking these measurements into account, they may make an educated decision regarding the quality of sleep [26].
- 7.
-
Alzheimer’s disease monitoring and Anemia detection
Monitoring for Alzheimer’s disease has several issues and needs to be handled carefully. When a patient is alone, diagnosing them with Alzheimer’s is impossible [27][28][29][30].
- 8.
-
Molecular diagnostics and Clinical diagnosis
Due to quick and affordable healthcare applications with reduced risk of infection, recent developments in biosensors for patient-friendly diagnosis and implantable devices for patient-friendly therapy have attracted a lot of attention. The rapid development of point-of-care (POC) sensor platforms and implantable devices with specialized functionality has been made possible by incorporating recently created materials into medical equipment [31][32]. A lot of work has been conducted on the clinical diagnosis of albumin-related diseases [33][34].
- 9.
-
Blood-oxygen-saturation detection
Along with precise, ongoing monitoring of intravascular oxygen levels, it is crucial to monitor patients’ cardiovascular health following cardiothoracic surgery [35]. There are new types of data, such as oxygen saturation, which are continuously collected using oxygen-saturation (SpO2) sensors and represent the percentage of oxygen-saturated hemoglobin compared to the total amount of hemoglobin in the blood; these are becoming available for market wearables. Other behavioral and physiological biometric types are already available in many market wearables [36][37][38].
Thus, it has been shown that health-monitoring sensors are used in various applications and can be used in the future for various diseases, particularly those that focus more on sample or data collection, monitoring, or evaluation. It can be asserted that whenever a sensor is employed, there is a possibility to collect the necessary data and deliver the desired outcomes, depending on precision and accuracy. Additionally, incorporating the cloud, geographic information systems, and mobile devices has improved the process of sensor-based data gathering and monitoring while allowing for flexible remote sharing and communication.
Numerous case studies and applications are possible for health-monitoring sensors. They can be used to measure hemoglobin concentration; for molecular diagnostics; to provide clinical diagnoses of disorders associated with albumin; to measure heart rate, blood-oxygen saturation, respiration rate, and anemia; to diagnose Alzheimer’s; and for many other things.
3.2. Classification of Health-Monitoring Sensors
With advancements in wireless communications, medical sensor technology, and data-collection methods, it is now possible to remotely monitor a person’s health by putting wearable technology on them and analyzing the data collected. These sensors and wearable devices can be integrated into various accessories such as clothing, wristbands, glasses, socks, hats, and shoes, as well as other devices such as smartphones, headphones, and wristwatches.
Pawan Singh [39] classified medical sensors into two categories: contact sensors (i.e., on-body or wearables) and non-contact sensors (i.e., peripherals). Contact sensors are further classified into two sub-categories: monitoring and therapeutic. Again, non-contact sensors are further classified into three sub-categories. All the sub-categories are further classified based on their use. Figure 4 illustrates the classification of health-monitoring sensors with examples of their use.

Figure 4. Classification of health-monitoring sensors [39].
Primarily, health-monitoring sensors can be divided into contact (i.e., on-body) and non-contact (i.e., peripheral) sensors. Contact sensors are attached to the body to monitor physiological behaviors, chemical-level identification, and optical measurement-related monitoring. Contact sensors are also used in therapy-related monitoring such as medication, stimulation, and emergencies. Non-contact sensors are used for monitoring fitness- and wellness-related factors, behavior, and rehabilitation. An example of each type of monitoring is shown in Figure 4.
The following are some of the medical applications that could benefit from the use of medical sensors and wearable devices [40]:
- Monitoring vital signs in hospitals.
- Aging in place and in motion.
- Assistance with motor and sensory impairments.
- Large-scale medical and behavioral research in the field.
Based on the applications in which they are most frequently used, the health-monitoring sensors could be divided into different groups for performance-wise evaluations. These sensors can be divided into many categories, which are covered in the subsections. Figure 5 is a collection of several wearable sensors applied in various research projects and employed in IoT systems in healthcare.
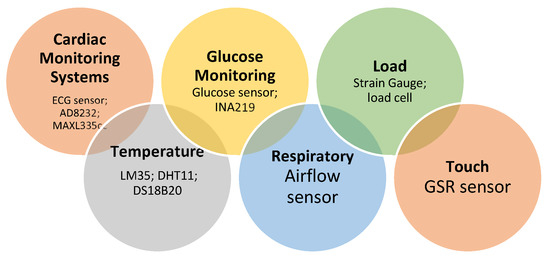
3.3. Performance Evaluation of IoT Sensors
Any healthcare-monitoring system’s sensors serve as its brain and heart. Thus, they must be reliable. Almost all types of sensors used should be small, quiet, accurate, have short data-transmission delays, use little power, and perform well overall. Wearable sensors must be both precise and compact, which presents a challenge. However, in case of wearable sensors, the more value is given to outputs, and they need to be reasonably accurate, too, so that the doctor can use these values to make decisions. Medical-grade sensors are large and difficult to transport and require specialized equipment and trained personnel [15].
Additionally, various IoT sensor-based applications constantly require authentication, security, and privacy. Numerous protocols are readily available on the market to assist with security and help offer some solutions over an extended period. Nevertheless, these integrated and crucial data-based apps’ security measures are constantly vulnerable to intrusion.
References
- Seneviratne, S.; Hu, Y.; Nguyen, T.; Lan, G.; Khalifa, S.; Thilakarathna, K.; Hassan, M.; Seneviratne, A. A survey of wearable devices and challenges. IEEE Commun. Surv. Tutor. 2017, 19, 2573–2620.
- Hiremath, S.; Yang, G.; Mankodiya, K. Wearable Internet of Things: Concept, architectural components and promises for person-centered healthcare. In Proceedings of the 2014 4th International Conference on Wireless Mobile Communication and Healthcare—Transforming Healthcare Through Innovations in Mobile and Wireless Technologies (MOBIHEALTH), Athens, Greece, 3–5 November 2014; pp. 304–307.
- Misran, N.; Islam, M.S.; Beng, G.K.; Amin, N.; Islam, M.T. IoT Based Health Monitoring System with LoRa Communication Technology. In Proceedings of the 2019 International Conference on Electrical Engineering and Informatics (ICEEI), Bandung, Indonesia, 9–10 July 2019; pp. 514–517.
- Dias, R.M.; Marques, G.; Bhoi, A.K. Internet of Things for Enhanced Food Safety and Quality Assurance: A Literature Review. Adv. Electron. Commun. Comput. 2021, 709, 653–663.
- Sahu, M.L.; Atulkar, M.; Ahirwal, M.K.; Ahamad, A. Vital Sign Monitoring System for Healthcare Through IoT Based Personal Service Application. Wirel. Pers. Commun. 2021, 122, 129–156.
- Philip, N.Y.; Rodrigues, J.J.P.C.; Wang, H.; Fong, S.J.; Chen, J. Internet of Things for In-Home Health Monitoring Systems: Current Advances, Challenges and Future Directions. IEEE J. Sel. Areas Commun. 2021, 39, 300–310.
- Almuhaya, M.A.; Jabbar, W.A.; Sulaiman, N.; Abdulmalek, S. A survey on Lorawan technology: Recent trends, opportunities, simulation tools and future directions. Electronics 2022, 11, 164.
- Desai, M.R.; Toravi, S. A Smart Sensor Interface for Smart Homes and Heart Beat Monitoring using WSN in IoT Environment. In Proceedings of the 2017 International Conference on Current Trends in Computer, Electrical, Electronics and Communication (CTCEEC), Mysore, India, 8–9 September 2017; pp. 74–77.
- Alekya, R.; Boddeti, N.D.; Monica, K.S.; Prabha, R.; Venkatesh, V. IoT based smart healthcare monitoring systems: A literature review. Eur. J. Mol. Clin. Med. 2021, 7, 2020.
- Malapane, T.J. A Cyber-Physical System for Smart Healthcare; University of Johannesburg: Johannesburg, South Africa, 2020.
- Jain, U.; Gumber, A.; Ajitha, D.; Rajini, G.; Subramanian, B. A Review on a Secure IoT-Based Healthcare System. In Proceedings of the Advances in Automation, Signal Processing, Instrumentation, and Control: Select Proceedings of i-CASIC, India, 27–28 February 2020; pp. 3005–3016.
- Vedaei, S.S.; Fotovvat, A.; Mohebbian, M.R.; Rahman, G.M.E.; Wahid, K.A.; Babyn, P.; Marateb, H.R.; Mansourian, M.; Sami, R. COVID-SAFE: An IoT-Based System for Automated Health Monitoring and Surveillance in Post-Pandemic Life. IEEE Access 2020, 8, 188538–188551.
- Wu, F.; Wu, T.; Yuce, M.R. Design and Implementation of a Wearable Sensor Network System for IoT-Connected Safety and Health Applications. In Proceedings of the 2019 IEEE 5th World Forum on Internet of Things (WF-IoT), Limerick, Ireland, 15–18 April 2019; pp. 87–90.
- Wan, J.; AAH Al-awlaqi, M.; Li, M.; O’Grady, M.; Gu, X.; Wang, J.; Cao, N. Wearable IoT enabled real-time health monitoring system. EURASIP J. Wirel. Commun. Netw. 2018, 2018, 298.
- Mamdiwar, S.D.; Shakruwala, Z.; Chadha, U.; Srinivasan, K.; Chang, C.-Y. Recent advances on IoT-assisted wearable sensor systems for healthcare monitoring. Biosensors 2021, 11, 372.
- Pal, A.; Visvanathan, A.; Choudhury, A.D.; Sinha, A. Improved heart rate detection using smart phone. In Proceedings of the 29th Annual ACM Symposium on Applied Computing, Gyeongju, Korea, 24–28 March 2014; pp. 8–13.
- Gogate, U.; Bakal, J. Healthcare monitoring system based on wireless sensor network for cardiac patients. Biomed. Pharmacol. J. 2018, 11, 1681.
- Arun, U.; Natarajan, S.; Rajanna, R.R. A novel IoT cloud-based real-time cardiac monitoring approach using NI myRIO-1900 for telemedicine applications. In Proceedings of the 2018 3rd International Conference on Circuits, Control, Communication and Computing (I4C), Bangalore, India, 3–5 October 2018; pp. 1–4.
- Pal, A.; Sinha, A.; Dutta Choudhury, A.; Chattopadyay, T.; Visvanathan, A. A robust heart rate detection using smart-phone video. In Proceedings of the 3rd ACM MobiHoc Workshop on Pervasive Wireless Healthcare, Bangalore, India, 29 July 2013; pp. 43–48.
- Gaoan, G.; Zhenmin, Z. Heart rate measurement via smart phone acceleration sensor. In Proceedings of the 2014 International Conference on Smart Computing, Hong Kong, China, 3–5 November 2014; pp. 295–300.
- Saha, R.; Biswas, S.; Sarmah, S.; Karmakar, S.; Das, P. A Working Prototype Using DS18B20 Temperature Sensor and Arduino for Health Monitoring. SN Comput. Sci. 2021, 2, 1–21.
- Adeniyi, E.A.; Ogundokun, R.O.; Awotunde, J.B. IoMT-based wearable body sensors network healthcare monitoring system. In IoT in Healthcare and Ambient Assisted Living; Springer: Berlin/Heidelberg, Germany, 2021; pp. 103–121.
- Fan, Z.; Zhou, Y.; Zhai, H.; Wang, Q.; He, H. A Smartphone-Based Biosensor for Non-Invasive Monitoring of Total Hemoglobin Concentration in Humans with High Accuracy. Biosensors 2022, 12, 781.
- Charlton, P.H.; Birrenkott, D.A.; Bonnici, T.; Pimentel, M.A.; Johnson, A.E.; Alastruey, J.; Tarassenko, L.; Watkinson, P.J.; Beale, R.; Clifton, D.A. Breathing rate estimation from the electrocardiogram and photoplethysmogram: A review. IEEE Rev. Biomed. Eng. 2017, 11, 2–20.
- Karlen, W.; Garde, A.; Myers, D.; Scheffer, C.; Ansermino, J.M.; Dumont, G.A. Estimation of respiratory rate from photoplethysmographic imaging videos compared to pulse oximetry. IEEE J. Biomed. Health Inform. 2015, 19, 1331–1338.
- Haghi, M.; Neubert, S.; Geissler, A.; Fleischer, H.; Stoll, N.; Stoll, R.; Thurow, K. A flexible and pervasive IoT-based healthcare platform for physiological and environmental parameters monitoring. IEEE Internet Things J. 2020, 7, 5628–5647.
- Pirani, E.Z.; Bulakiwala, F.; Kagalwala, M.; Kalolwala, M.; Raina, S. Android based assistive toolkit for alzheimer. Procedia Comput. Sci. 2016, 79, 143–151.
- Batsis, J.A.; Boateng, G.G.; Seo, L.M.; Petersen, C.L.; Fortuna, K.L.; Wechsler, E.V.; Peterson, R.J.; Cook, S.B.; Pidgeon, D.; Dokko, R.S. Development and usability assessment of a connected resistance exercise band application for strength-monitoring. World Acad. Sci. Eng. Technol. 2019, 13, 340.
- Wang, R.; Aung, M.S.; Abdullah, S.; Brian, R.; Campbell, A.T.; Choudhury, T.; Hauser, M.; Kane, J.; Merrill, M.; Scherer, E.A. CrossCheck: Toward passive sensing and detection of mental health changes in people with schizophrenia. In Proceedings of the 2016 ACM International Joint Conference on Pervasive and Ubiquitous Computing, Heidelberg, Germany, 12–16 September 2016; pp. 886–897.
- Ghatpande, N.S.; Apte, P.P.; Joshi, B.N.; Naik, S.S.; Bodas, D.; Sande, V.; Uttarwar, P.; Kulkarni, P.P. Development of a novel smartphone-based application for accurate and sensitive on-field hemoglobin measurement. RSC Adv. 2016, 6, 104067–104072.
- Li, P.; Lee, G.-H.; Kim, S.Y.; Kwon, S.Y.; Kim, H.-R.; Park, S. From diagnosis to treatment: Recent advances in patient-friendly biosensors and implantable devices. ACS Nano 2021, 15, 1960–2004.
- Song, J.; Pandian, V.; Mauk, M.G.; Bau, H.H.; Cherry, S.; Tisi, L.C.; Liu, C. Smartphone-based mobile detection platform for molecular diagnostics and spatiotemporal disease mapping. Anal. Chem. 2018, 90, 4823–4831.
- Hussain, S.; Chen, X.; Wang, C.; Hao, Y.; Tian, X.; He, Y.; Li, J.; Shahid, M.; Iyer, P.K.; Gao, R. Aggregation and Binding-Directed FRET Modulation of Conjugated Polymer Materials for Selective and Point-of-Care Monitoring of Serum Albumins. Anal. Chem. 2022, 94, 10685–10694.
- Muthuraj, B.; Hussain, S.; Iyer, P.K. A rapid and sensitive detection of ferritin at a nanomolar level and disruption of amyloid β fibrils using fluorescent conjugated polymer. Polym. Chem. 2013, 4, 5096–5107.
- Lu, W.; Bai, W.; Zhang, H.; Xu, C.; Chiarelli, A.M.; Vázquez-Guardado, A.; Xie, Z.; Shen, H.; Nandoliya, K.; Zhao, H. Wireless, implantable catheter-type oximeter designed for cardiac oxygen saturation. Sci. Adv. 2021, 7, eabe0579.
- Muratyan, A.; Cheung, W.; Dibbo, S.V.; Vhaduri, S. Opportunistic multi-modal user authentication for health-tracking IoT wearables. In Proceedings of the The Fifth International Conference on Safety and Security with IoT, Da Nang, Vietnam, 25 April 2021; pp. 1–18.
- Fang, D.; Hu, J.; Wei, X.; Shao, H.; Luo, Y. A smart phone healthcare monitoring system for oxygen saturation and heart rate. In Proceedings of the 2014 International Conference on Cyber-Enabled Distributed Computing and Knowledge Discovery, Shanghai, China, 13–15 October 2014; pp. 245–247.
- Nemcova, A.; Jordanova, I.; Varecka, M.; Smisek, R.; Marsanova, L.; Smital, L.; Vitek, M. Monitoring of heart rate, blood oxygen saturation, and blood pressure using a smartphone. Biomed. Signal Process. Control 2020, 59, 101928.
- Singh, P. Internet of things based health monitoring system: Opportunities and challenges. Int. J. Adv. Res. Comput. Sci. 2018, 9, 224–228.
- Ko, J.; Lu, C.; Srivastava, M.B.; Stankovic, J.A.; Terzis, A.; Welsh, M. Wireless sensor networks for healthcare. Proc. IEEE 2010, 98, 1947–1960.
- Rashmi, I.; Sahana, M.; Sangeetha, R.; Shruthi, K. IOT based Patient Health Monitoring System to Remote Doctors using Embedded Technology. Int. J. Eng. Res. Technol. 2020, 8, 230–233.
- Prakash, B.; Nagesh, M.; Mukunda, D.; Gowda, C. Arm Based Health Care Monitoring Services Using Wireless Network. Int. Res. J. Mod. Eng. Technol. Sci. 2020, 2. Available online: https://www.researchgate.net/profile/Mukunda-D-S/publication/341607121_ARM_BASED_HEALTH_CARE_MONITORING_SERVICES_USING_WIRELESS_NETWORK/links/5eca2d6792851c11a884f973/ARM-BASED-HEALTH-CARE-MONITORING-SERVICES-USING-WIRELESS-NETWORK.pdf (accessed on 5 October 2022).
- Misbahuddin, S.; Al-Ahdal, A.R.; Malik, M.A. Low-Cost MPI Cluster Based Distributed in-Ward Patients Monitoring System. In Proceedings of the 2018 IEEE/ACS 15th International Conference on Computer Systems and Applications (AICCSA), Aqaba, Jordan, 28 October–1 November 2018; pp. 1–6.
- Patil, H.; Manohare, S.; Magdum, S.; Gore, M.S. Smart Healthcare Monitoring and Patient Report Generation System Using IOT. Int. J. Res. Appl. Sci. Eng. Technol. 2020, 8. Available online: https://www.academia.edu/43408033/Smart_Healthcare_Monitoring_and_Patient_Report_Generation_System_using_IOT (accessed on 5 October 2022).
- Mhatre, P.; Shaikh, A.; Khanvilkar, S. Non Invasive E-Health Care Monitoring System Using IOT. Int. J. Innov. Res. Technol. 2020, 6, 307–311.
- Zaman, F.; Lee, S.; Rahim, M.K.; Khan, S. Smart Antennas and Intelligent Sensors Based Systems: Enabling Technologies and Applications; Hindawi: London, UK, 2019; Volume 2019.
More
Information
Subjects:
Engineering, Biomedical
Contributors
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
2.6K
Revisions:
2 times
(View History)
Update Date:
15 Nov 2022
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





