
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Vera Gramigna | -- | 1972 | 2022-11-08 12:28:24 | | | |
| 2 | Amina Yu | -2 word(s) | 1970 | 2022-11-09 02:22:14 | | |
Video Upload Options
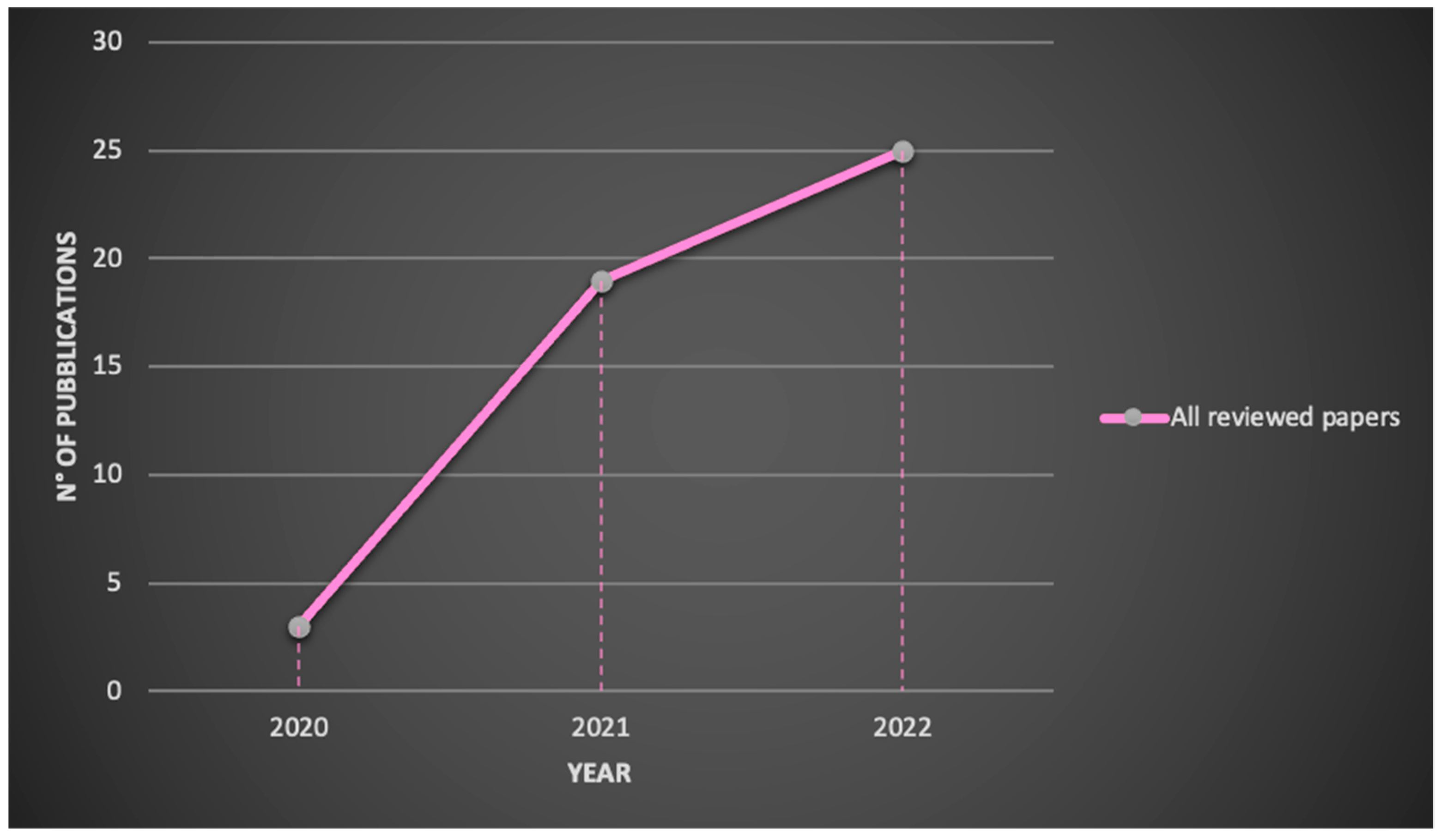
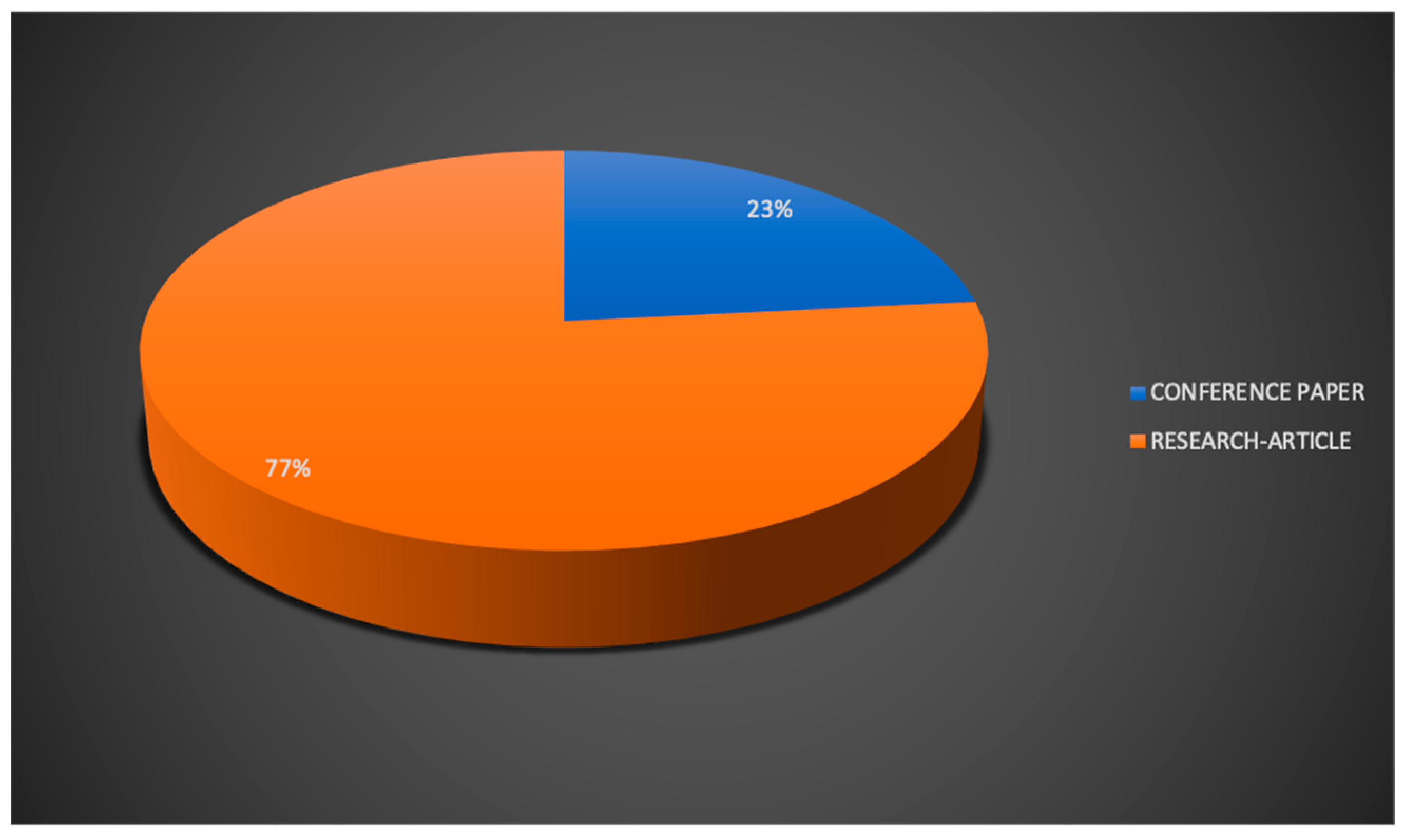
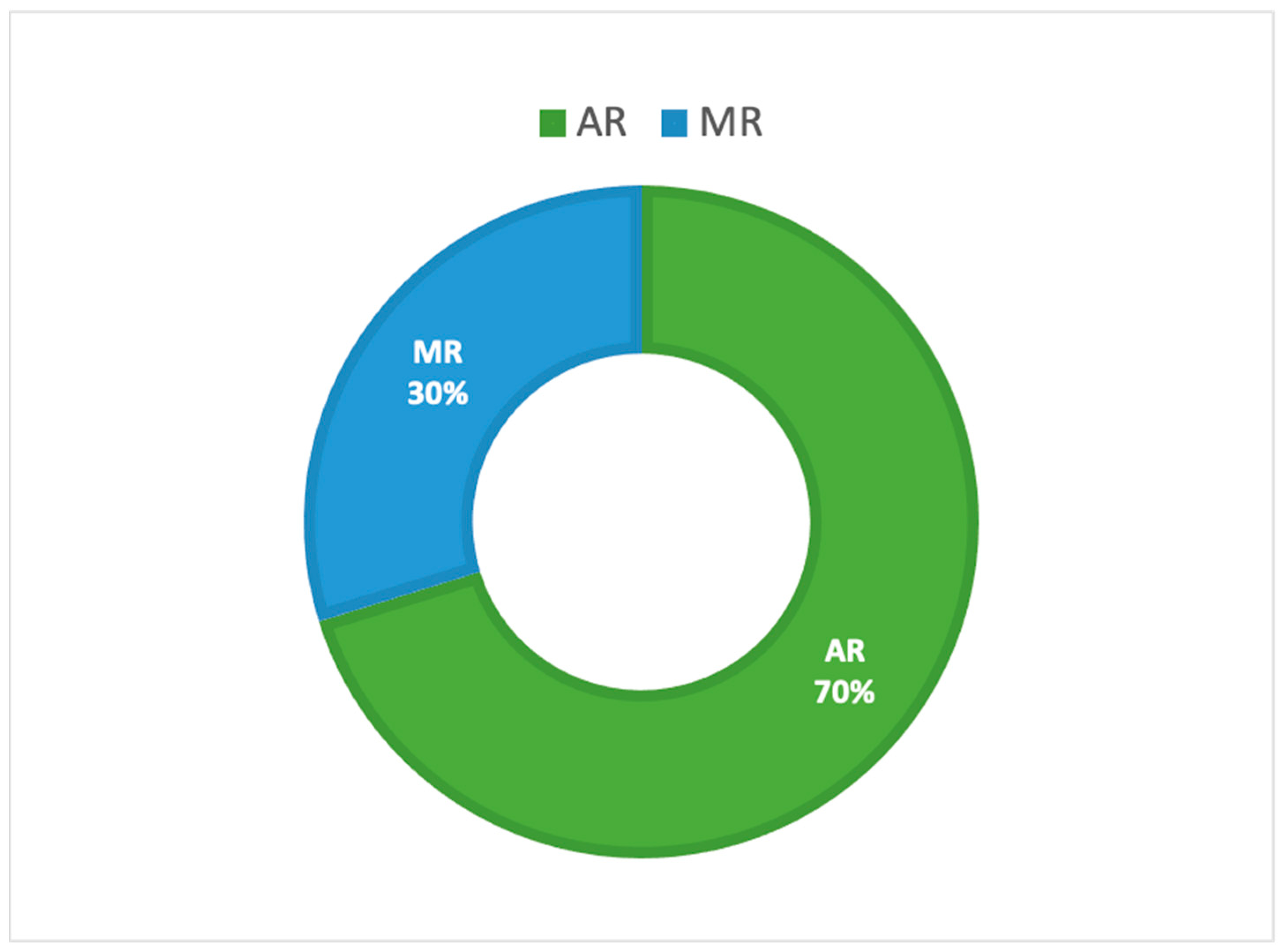
Microsoft® HoloLens was developed and manufactured by Microsoft (MS) and can be presented as a pair of mixed reality smart glasses able to describe an environment in which real and virtual elements appear to coexist. More specifically, the Microsoft® HoloLens is a novel MR-based HMD that makes the user the protagonist of an immersive experience and allows him to interact with the surrounding environment using holograms whilst engaging their senses throughout. It is used in a variety of applications such as medical and surgical aids and systems, medical education and simulation, architecture and several engineering fields (civil, industrial and so on). The use of HoloLens 2 in a medical and healthcare context was analyzed by dividing contributions into the following sub-field applications: surgical navigation, AR-BCI (Brain-Computer Interface) systems integration and human computer interaction (HCI), gait analysis and rehabilitation, medical education and training/virtual teaching/tele-mentoring/tele-consulting and other applications.
1. Surgical Navigation
2. Human Computer Interaction and AR-BCI (Brain-Computer Interface) Systems Integration
3. Gait Analysis and Rehabilitation
4. Medical Education and Training/Virtual Teaching/Tele-Mentoring/Tele-Consulting
5. Other Applications

References
- Wang, L.; Zhao, Z.; Wang, G.; Zhou, J.; Zhu, H.; Guo, H.; Huang, H.; Yu, M.; Zhu, G.; Li, N.; et al. Application of a three-dimensional visualization model in intraoperative guidance of percutaneous nephrolithotomy. Int. J. Urol. 2022, 29, 838–844.
- Liu, X.; Sun, J.; Zheng, M.; Cui, X. Application of Mixed Reality Using Optical See-Through Head-Mounted Displays in Transforaminal Percutaneous Endoscopic Lumbar Discectomy. BioMed Res. Int. 2021, 2021, 9717184.
- Eom, S.; Kim, S.; Rahimpour, S.; Gorlatova, M. AR-Assisted Surgical Guidance System for Ventriculostomy. In Proceedings of the 2022 IEEE Conference on Virtual Reality and 3D User Interfaces Abstracts and Workshops, VRW 2022, Christchurch, New Zealand, 12–16 March 2022; pp. 402–405.
- Kitagawa, M.; Sugimoto, M.; Haruta, H.; Umezawa, A.; Kurokawa, Y. Intraoperative holography navigation using a mixed-reality wearable computer during laparoscopic cholecystectomy. Surgery 2022, 171, 1006–1013.
- Doughty, M.; Ghugre, N.R. Head-Mounted Display-Based Augmented Reality for Image-Guided Media Delivery to the Heart: A Preliminary Investigation of Perceptual Accuracy. J. Imaging 2022, 8, 33.
- Torabinia, M.; Caprio, A.; Fenster, T.B.; Mosadegh, B. Single Evaluation of Use of a Mixed Reality Headset for Intra-Procedural Image-Guidance during a Mock Laparoscopic Myomectomy on an Ex-Vivo Fibroid Model. Appl. Sci. 2022, 12, 563.
- Gsaxner, C.; Pepe, A.; Schmalstieg, D.; Li, J.; Egger, J. Inside-out instrument tracking for surgical navigation in augmented reality. In Proceedings of the ACM Symposium on Virtual Reality Software and Technology, VRST, Osaka, Japan, 8–10 December 2021.
- García-sevilla, M.; Moreta-martinez, R.; García-mato, D.; Pose-diez-de-la-lastra, A.; Pérez-mañanes, R.; Calvo-haro, J.A.; Pascau, J. Augmented reality as a tool to guide psi placement in pelvic tumor resections. Sensors 2021, 21, 7824.
- Amiras, D.; Hurkxkens, T.J.; Figueroa, D.; Pratt, P.J.; Pitrola, B.; Watura, C.; Rostampour, S.; Shimshon, G.J.; Hamady, M. Augmented reality simulator for CT-guided interventions. Eur. Radiol. 2021, 31, 8897–8902.
- Park, B.J.; Hunt, S.J.; Nadolski, G.J.; Gade, T.P. Augmented reality improves procedural efficiency and reduces radiation dose for CT-guided lesion targeting: A phantom study using HoloLens 2. Sci. Rep. 2020, 10, 18620.
- Benmahdjoub, M.; Niessen, W.J.; Wolvius, E.B.; Van Walsum, T. Virtual extensions improve perception-based instrument alignment using optical see-through devices. IEEE Trans. Vis. Comput. Graph. 2021, 27, 4332–4341.
- Benmahdjoub, M.; Niessen, W.J.; Wolvius, E.B.; Walsum, T. Multimodal markers for technology-independent integration of augmented reality devices and surgical navigation systems. Virtual Real 2022.
- Farshad, M.; Spirig, J.M.; Suter, D.; Hoch, A.; Burkhard, M.D.; Liebmann, F.; Farshad-Amacker, N.A.; Fürnstahl, P. Operator independent reliability of direct augmented reality navigated pedicle screw placement and rod bending. N. Am. Spine Soc. J. 2021, 8, 100084.
- Doughty, M.; Singh, K.; Ghugre, N.R. SurgeonAssist-Net: Towards Context-Aware Head-Mounted Display-Based Augmented Reality for Surgical Guidance. In Medical Image Computing and Computer Assisted Intervention; Lecture Notes in Computer Science (including subseries Lecture Notes in Artificial Intelligence and Lecture Notes in Bioinformatics); Springer: Cham, Switzerland, 2021; pp. 667–677.
- Nagayo, Y.; Saito, T.; Oyama, H. Augmented reality self-training system for suturing in open surgery: A randomized controlled trial. Int. J. Surg. 2022, 102, 106650.
- Nagayo, Y.; Saito, T.; Oyama, H. A Novel Suture Training System for Open Surgery Replicating Procedures Performed by Experts Using Augmented Reality. J. Med. Syst. 2021, 45, 60.
- Haxthausen, F.V.; Chen, Y.; Ernst, F. Superimposing holograms on real world objects using HoloLens 2 and its depth camera. Curr. Dir. Biomed. Eng. 2021, 7, 20211126.
- Wierzbicki, R.; Pawłowicz, M.; Job, J.; Balawender, R.; Kostarczyk, W.; Stanuch, M.; Janc, K.; Skalski, A. 3D mixed-reality visualization of medical imaging data as a supporting tool for innovative, minimally invasive surgery for gastrointestinal tumors and systemic treatment as a new path in personalized treatment of advanced cancer diseases. J. Cancer Res. Clin. Oncol. 2022, 148, 237–243.
- Brunzini, A.; Mandolini, M.; Caragiuli, M.; Germani, M.; Mazzoli, A.; Pagnoni, M. HoloLens 2 for Maxillofacial Surgery: A Preliminary Study. In Design Tools and Methods in Industrial Engineering II; Lecture Notes in Mechanical Engineering; Springer: Cham, Switzerland, 2022; pp. 133–140.
- Thabit, A.; Benmahdjoub, M.; van Veelen, M.L.C.; Niessen, W.J.; Wolvius, E.B.; van Walsum, T. Augmented reality navigation for minimally invasive craniosynostosis surgery: A phantom study. Int. J. Comput. Assist. Radiol. Surg. 2022, 17, 1453–1460.
- Cercenelli, L.; Babini, F.; Badiali, G.; Battaglia, S.; Tarsitano, A.; Marchetti, C.; Marcelli, E. Augmented Reality to Assist Skin Paddle Harvesting in Osteomyocutaneous Fibular Flap Reconstructive Surgery: A Pilot Evaluation on a 3D-Printed Leg Phantom. Front. Oncol. 2021, 11, 804748.
- Felix, B.; Kalatar, S.B.; Moatz, B.; Hofstetter, C.; Karsy, M.; Parr, R.; Gibby, W. Augmented Reality Spine Surgery Navigation Increasing Pedicle Screw : Insertion Accuracy for Both Open and Minimally Invasive S Surgeries. Spine 2022, 47, 865–872.
- Tu, P.; Gao, Y.; Lungu, A.J.; Li, D.; Wang, H.; Chen, X. Augmented reality based navigation for distal interlocking of intramedullary nails utilizing Microsoft HoloLens 2. Comput. Biol. Med. 2021, 133, 104402.
- Zhou, Z.; Yang, Z.; Jiang, S.; Zhuo, J.; Zhu, T.; Ma, S. Augmented reality surgical navigation system based on the spatial drift compensation method for glioma resection surgery. Med. Phys. 2022, 49, 3963–3979.
- Ivanov, V.M.; Krivtsov, A.M.; Strelkov, S.V.; Kalakutskiy, N.V.; Yaremenko, A.I.; Petropavlovskaya, M.Y.; Portnova, M.N.; Lukina, O.V.; Litvinov, A.P. Intraoperative use of mixed reality technology in median neck and branchial cyst excision. Future Internet 2021, 13, 214.
- Heinrich, F.; Schwenderling, L.; Joeres, F.; Hansen, C. 2D versus 3D: A Comparison of Needle Navigation Concepts between Augmented Reality Display Devices. In Proceedings of the 2022 IEEE Conference on Virtual Reality and 3D User Interfaces, VR 2022, Christchurch, New Zealand, 12–16 March 2022; pp. 260–269.
- Morita, S.; Suzuki, K.; Yamamoto, T.; Kunihara, M.; Hashimoto, H.; Ito, K.; Fujii, S.; Ohya, J.; Masamune, K.; Sakai, S. Mixed Reality Needle Guidance Application on Smartglasses Without Pre-procedural CT Image Import with Manually Matching Coordinate Systems. CardioVascular Interv. Radiol. 2022, 45, 349–356.
- Mitani, S.; Sato, E.; Kawaguchi, N.; Sawada, S.; Sakamoto, K.; Kitani, T.; Sanada, T.; Yamada, H.; Hato, N. Case-specific three-dimensional hologram with a mixed reality technique for tumor resection in otolaryngology. Laryngoscope Investig. Otolaryngol. 2021, 6, 432–437.
- Vávra, P.; Roman, J.; Zonča, P.; Ihnát, P.; Němec, M.; Kumar, J.; Habib, N.; El-Gendi, A. Recent Development of Augmented Reality in Surgery: A Review. J. Healthc. Eng. 2017, 2017, 4574172.
- Zabcikova, M.; Koudelkova, Z.; Jasek, R.; Lorenzo Navarro, J.J. Recent advances and current trends in brain-computer interface research and their applications. Int. J. Dev. Neurosci. 2022, 82, 107–123.
- van Dokkum, L.E.H.; Ward, T.; Laffont, I. Brain computer interfaces for neurorehabilitation-its current status as a rehabilitation strategy post-stroke. Ann. Phys. Rehabil. Med. 2015, 58, 3–8.
- Palumbo, A.; Gramigna, V.; Calabrese, B.; Ielpo, N. Motor-imagery EEG-based BCIs in wheelchair movement and control: A systematic literature review. Sensors 2021, 21, 6285.
- Kos’Myna, N.; Tarpin-Bernard, F. Evaluation and comparison of a multimodal combination of BCI paradigms and eye tracking with affordable consumer-grade hardware in a gaming context. IEEE Trans. Comput. Intell. AI Games 2013, 5, 150–154.
- Amores, J.; Richer, R.; Zhao, N.; Maes, P.; Eskofier, B.M. Promoting relaxation using virtual reality, olfactory interfaces and wearable EEG. In Proceedings of the 2018 IEEE 15th International Conference on Wearable and Implantable Body Sensor Networks, BSN 2018, Las Vegas, NV, USA, 4–7 March 2018; pp. 98–101.
- Semertzidis, N.; Scary, M.; Andres, J.; Dwivedi, B.; Kulwe, Y.C.; Zambetta, F.; Mueller, F.F. Neo-Noumena: Augmenting Emotion Communication. In Proceedings of the Conference on Human Factors in Computing Systems, Honolulu, HI, USA, 25–30 April 2020.
- Kohli, V.; Tripathi, U.; Chamola, V.; Rout, B.K.; Kanhere, S.S. A review on Virtual Reality and Augmented Reality use-cases of Brain Computer Interface based applications for smart cities. Microprocess. Microsyst. 2022, 88, 104392.
- Kosmyna, N.; Hu, C.Y.; Wang, Y.; Wu, Q.; Scheirer, C.; Maes, P. A Pilot Study using Covert Visuospatial Attention as an EEG-based Brain Computer Interface to Enhance AR Interaction. In Proceedings of the International Symposium on Wearable Computers, ISWC, Cancun, Mexico, 12–16 September 2020; pp. 43–47.
- Kosmyna, N.; Wu, Q.; Hu, C.Y.; Wang, Y.; Scheirer, C.; Maes, P. Assessing Internal and External Attention in AR using Brain Computer Interfaces: A Pilot Study. In Proceedings of the 2021 IEEE 17th International Conference on Wearable and Implantable Body Sensor Networks, BSN 2021, Athens, Greece, 27–30 July 2021.
- Wolf, J.; Lohmeyer, Q.; Holz, C.; Meboldt, M. Gaze comes in Handy: Predicting and preventing erroneous hand actions in ar-supported manual tasks. In Proceedings of the 2021 IEEE International Symposium on Mixed and Augmented Reality, ISMAR 2021, Bari, Italy, 4–8 October 2021; pp. 166–175.
- Wolf, E.; Fiedler, M.L.; Dollinger, N.; Wienrich, C.; Latoschik, M.E. Exploring Presence, Avatar Embodiment, and Body Perception with a Holographic Augmented Reality Mirror. In Proceedings of the 2022 IEEE Conference on Virtual Reality and 3D User Interfaces, VR 2022, Christchurch, New Zealand, 12–16 March 2022; pp. 350–359.
- Koop, M.M.; Rosenfeldt, A.B.; Owen, K.; Penko, A.L.; Streicher, M.C.; Albright, A.; Alberts, J.L. The Microsoft HoloLens 2 Provides Accurate Measures of Gait, Turning, and Functional Mobility in Healthy Adults. Sensors 2022, 22, 2009.
- Held, J.P.O.; Yu, K.; Pyles, C.; Bork, F.; Heining, S.M.; Navab, N.; Luft, A.R. Augmented reality-based rehabilitation of gait impairments: Case report. JMIR mHealth uHealth 2020, 8, e17804.
- Wolf, J.; Wolfer, V.; Halbe, M.; Maisano, F.; Lohmeyer, Q.; Meboldt, M. Comparing the effectiveness of augmented reality-based and conventional instructions during single ECMO cannulation training. Int. J. Comput. Assist. Radiol. Surg. 2021, 16, 1171–1180.
- Mill, T.; Parikh, S.; Allen, A.; Dart, G.; Lee, D.; Richardson, C.; Howell, K.; Lewington, A. Live streaming ward rounds using wearable technology to teach medical students: A pilot study. BMJ Simul. Technol. Enhanc. Learn. 2021, 7, 494–500.
- Levy, J.B.; Kong, E.; Johnson, N.; Khetarpal, A.; Tomlinson, J.; Martin, G.F.; Tanna, A. The mixed reality medical ward round with the MS HoloLens 2: Innovation in reducing COVID-19 transmission and PPE usage. Future Healthc. J. 2021, 8, e127–e130.
- Sivananthan, A.; Gueroult, A.; Zijlstra, G.; Martin, G.; Baheerathan, A.; Pratt, P.; Darzi, A.; Patel, N.; Kinross, J. Using Mixed Reality Headsets to Deliver Remote Bedside Teaching during the COVID-19 Pandemic: Feasibility Trial of HoloLens 2. JMIR Form. Res. 2022, 6, e35674.
- Rafi, D.; Stackhouse, A.A.; Walls, R.; Dani, M.; Cowell, A.; Hughes, E.; Sam, A.H. A new reality: Bedside geriatric teaching in an age of remote learning. Future Healthc. J. 2021, 8, e714–e716.
- Dolega-Dolegowski, D.; Proniewska, K.; Dolega-Dolegowska, M.; Pregowska, A.; Hajto-Bryk, J.; Trojak, M.; Chmiel, J.; Walecki, P.; Fudalej, P.S. Application of holography and augmented reality based technology to visualize the internal structure of the dental root—A proof of concept. Head Face Med. 2022, 18, 12.
- Bui, D.T.; Barnett, T.; Hoang, H.; Chinthammit, W. Usability of augmented reality technology in tele-mentorship for managing clinical scenarios-A study protocol. PLoS ONE 2022, 17, e0266255.
- Bala, L.; Kinross, J.; Martin, G.; Koizia, L.J.; Kooner, A.S.; Shimshon, G.J.; Hurkxkens, T.J.; Pratt, P.J.; Sam, A.H. A remote access mixed reality teaching ward round. Clin. Teach. 2021, 18, 386–390.
- Mentis, H.M.; Avellino, I.; Seo, J. AR HMD for Remote Instruction in Healthcare. In Proceedings of the 2022 IEEE Conference on Virtual Reality and 3D User Interfaces Abstracts and Workshops, VRW 2022, Christchurch, New Zealand, 12–16 March 2022; pp. 437–440.
- Onishi, R.; Morisaki, T.; Suzuki, S.; Mizutani, S.; Kamigaki, T.; Fujiwara, M.; Makino, Y.; Shinoda, H. GazeBreath: Input Method Using Gaze Pointing and Breath Selection. In Proceedings of the Augmented Humans 2022, Kashiwa, Chiba, Japan, 13–15 March 2022; pp. 1–9.
- Johnson, P.B.; Jackson, A.; Saki, M.; Feldman, E.; Bradley, J. Patient posture correction and alignment using mixed reality visualization and the HoloLens 2. Med. Phys. 2022, 49, 15–22.
- Kurazume, R.; Hiramatsu, T.; Kamei, M.; Inoue, D.; Kawamura, A.; Miyauchi, S.; An, Q. Development of AR training systems for Humanitude dementia care. Adv. Robot. 2022, 36, 344–358.
- Matyash, I.; Kutzner, R.; Neumuth, T.; Rockstroh, M. Accuracy measurement of HoloLens2 IMUs in medical environments. Curr. Dir. Biomed. Eng. 2021, 7, 633–636.





