Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | saber saedmocheshi | -- | 2164 | 2022-08-29 15:33:40 | | | |
| 2 | Beatrix Zheng | + 3 word(s) | 2167 | 2022-08-30 08:08:57 | | | | |
| 3 | Beatrix Zheng | -28 word(s) | 2139 | 2022-08-30 08:09:23 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Nobari, H.; Saedmocheshi, S.; Murawska-Ciałowicz, E.; Clemente, F.M.; Suzuki, K.; Silva, A.F. Athletes during an Ramadan Fasting Period. Encyclopedia. Available online: https://encyclopedia.pub/entry/26625 (accessed on 24 May 2026).
Nobari H, Saedmocheshi S, Murawska-Ciałowicz E, Clemente FM, Suzuki K, Silva AF. Athletes during an Ramadan Fasting Period. Encyclopedia. Available at: https://encyclopedia.pub/entry/26625. Accessed May 24, 2026.
Nobari, Hadi, Saber Saedmocheshi, Eugenia Murawska-Ciałowicz, Filipe Manuel Clemente, Katsuhiko Suzuki, Ana Filipa Silva. "Athletes during an Ramadan Fasting Period" Encyclopedia, https://encyclopedia.pub/entry/26625 (accessed May 24, 2026).
Nobari, H., Saedmocheshi, S., Murawska-Ciałowicz, E., Clemente, F.M., Suzuki, K., & Silva, A.F. (2022, August 29). Athletes during an Ramadan Fasting Period. In Encyclopedia. https://encyclopedia.pub/entry/26625
Nobari, Hadi, et al. "Athletes during an Ramadan Fasting Period." Encyclopedia. Web. 29 August, 2022.
Copy Citation
The Ramadan fasting period (RFP) means abstaining from consuming food and/or beverages during certain hours of the day—from sunrise to sunset. Engaging in exercise and sports during the RFP leads to the lipolysis of adipose tissue and an increase in the breakdown of peripheral fat, leading to an increase in fat consumption. The effects of the RFP on functional, hematological, and metabolic parameters needs further study as existing studies have reported contradictory results. The differences in the results of various studies are due to the geographical characteristics of Muslim athletes, their specific diets, and their genetics, which explain these variations.
diet
intermittent fasting
calorie restriction
dehydration
exercise
balanced hormones
health promotion
hypoglycemia
1. Nutritional Considerations for Athletes during an RFP
Macronutrients are very important for athletes. During an Ramadan fasting period (RFP) and energy restriction, athletes lose weight due to reduced food intake. Therefore, a proper diet plan during this period can help an athlete achieve a good balance between energy intake and consumption [1][2]. However, athletes should not focus on micronutrients, but rather they should include macronutrients in their diets [3].
1.1. Protein
Consuming protein is one weight management strategy that increases the feeling of satiety as well as heat production [4][5]. People with high-protein diets do not have a big problem because they are used to consuming less energy [6][7]. Therefore, planning a high-protein diet can be a solution for athletes during RFPs. High-protein diets increase satiety, increase thermal energy, and reduce fat consumption [8]. Using protein supplements, along with resistance training and other supplements, such as creatine and beta-hydroxy-beta-methylbutyric acid (HMB), helps maintain energy [9][10].
1.2. Lipids
Adequate lipids in the diet are very important due to the structural and storage properties of this nutrient [11]. Therefore, engaging in resistance training during energy restriction can induce the consumption of carbohydrates and lipids, and it can eliminate the consequences of an RFP. The dietary recommendation for RFPs is to consume a low-fat meal with a high carbohydrate level [12][13][14]. It has been suggested that fasting increases the number of beta-adrenoceptors in adipose tissue in rats [15], but a decrease in beta-adrenoceptors has been observed in human adipose tissues [15]. Fasting conditions lead to an increase in the basal lipolysis of adipose tissue, but the lipolytic response (even of antihypertensives) to catecholamines decreases [16]. Fasting increases the levels of catabolic hormones, such as GH [17] and glucagon [16], as well as catecholamines, which leads to increased lipolysis [18].
1.3. Hydration Strategies
Maintaining a water–salt balance during an RFP is important for athletes, but it is challenging when they must continue their training and competition programs [19][20][21]. A lack of water can create three conditions for Muslim athletes:
- ⮚
-
The RFP prevents athletes from being hydrated during a race, and they become dehydrated.
- ⮚
-
The lack of water causes a drop in performance.
- ⮚
-
The lack of water disrupts the balance of water and electrolytes [21].
Many factors affect exercise performance during RFP conditions [21]. The duration of exercise is an important factor as short-term activities are less affected by RFP conditions. As the duration of food and water deprivation increases during Ramadan, so does the condition of hypohydration [22][23]. It has been observed that the deprivation of fluids reduces one’s level of consciousness and results in mental fatigue, ultimately causing functional impairment [24][25]. However, ambient temperatures and humidity can affect the hydration of the athlete [26][27]. Many criteria can be used to diagnose dehydration, such as the frequency, volume, and color of the urine [28]. Using the following solutions can prevent dehydration in the body during an RFP:
-
Reduce the time in situations where there is a possibility of dehydration, such as exposure to sunlight.
-
Be sure to check the hydration status of the body.
-
Before an RFP begins, fluids should be selected according to the conditions and contain minerals and energy that reduce water loss.
-
The consumption of fluids when a person is not participating in an RFP should be regular, such as during the night.
-
As much as possible, one should train and compete for 2 to 3 h after sunset [29].
2. Response of Hematocrit to an RFP in Athletes
During 1 of the 12 months of the Islamic calendar (“Ramadan”), mature and healthy Muslims abstain from drinking and eating from sunrise to sunset [29]. An RFP during the holy month of Ramadan can cause many changes in the psychological and physiological characteristics of a person [30][31]. Physiological changes that have been observed include dehydration [30], metabolic responses [30][31], sleep and wakefulness changes, hormone secretion, and the function of various organs of the body [31]. Athletes must manage these changes by developing a proper training plan [32]. By considering one’s water supply and nutrition during Ramadan, the stability of the athlete’s blood counts can be maintained [33].
2.1. Erythrocyte States
Studies have shown conflicting results regarding Ramadan’s effect on the body’s iron status. Boehlell et al. [34] observed a significant increase in hematocrit (Hct) and hemoglobin (Hb) concentrations in rugby players at the end of Ramadan compared to a control. However, Hosseini and Hejazi [35] observed a decrease in Hct, Hb, and red blood cells (RBC) in young football players following an RFP. Additionally, Hosseini et al. [36] failed to observe significant changes after a Ramadan RFP in Hct and Hb but saw a decrease in RBC [36]. When considering different times of the day, Maughan et al. [37] reported small changes (less than 2%) in the Hct levels of football players during Ramadan.
2.2. Platelet Count
When examining the effect of an RFP on blood platelet count in three sports, an increase in the number of cells was seen in wrestlers [35], but this increase was not observed in football players [38] or weightlifters [39].
3. Immunosuppression and Related Cells during an RFP
Malnutrition is a dangerous factor affecting the homeostasis of the body and the maintenance of the physiological balance of living organisms. Usually, all living organisms have a way to control their energy reserves. When energy availability is high, the body stores the excess energy in fat tissue, and when the energy availability is low, the fat tissue is used. Malnutrition and overnutrition can cause cytokine and hormone responses to these conditions. One of the first reports regarding this included tumor necrosis factor-alpha (TNF-α). Overfeeding was found to increase levels of TNF-α, whereas undernutrition caused a decrease in TNF-α levels [40]. TNF-α is a known pro-inflammatory cytokine essential for the acute phase response. Studies have shown that reducing energy intake can suppress the immune system and increase the incidence of infectious diseases [41]. Figure 1 shows the impact of energy deprivation and malnutrition on the immune system.
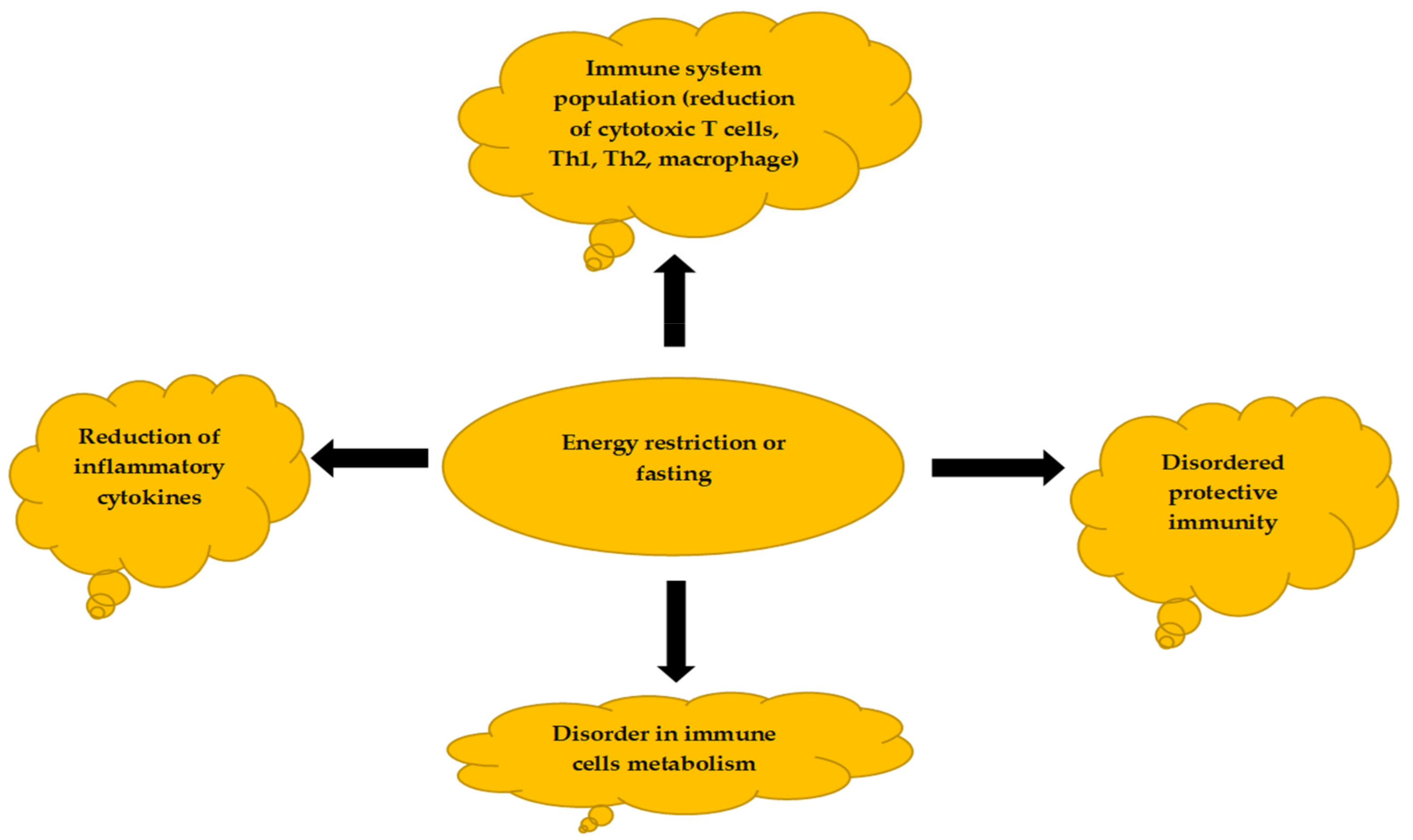
Figure 1. Changes in energy availability can drastically impact immune cell functions.
4. Response of the Immune System to an RFP in Athletes
An RFP significantly reduces inflammation and reduces the incidence of cancer in animal models [42]. In a human study (with 21 males and 29 females), changes in circulating pro-inflammatory cytokines, such as interleukin 1β (IL-1β), interleukin 6 (IL-6), and tumor necrosis factor (TNF), were evaluated [43]. TNF-α and immune cells (total leukocytes, monocytes, granulocytes, and lymphocytes) were observed during 3 periods: 1 week before Ramadan, 3 weeks after Ramadan, and 1 month after Ramadan. It was observed that the pro-inflammatory cytokines IL-1β, IL-6, and TNF-α decreased significantly during Ramadan [44]. In addition, a significant decrease in immune cells was observed during Ramadan, but they returned to baseline [45]. The effect of Ramadan on oxidative stress and cell damage in healthy individuals was evaluated in 14 healthy volunteers. Researchers observed no significant changes in oxidative stress by measuring malondialdehyde (MDA), glutathione [46], glutathione peroxidase [46][47], and catalase levels after Ramadan [48]. An RFP decreased IL-12 levels during weeks 1 and 4 of Ramadan as compared to week 3. Changes in IL-12 levels can be a result of changes in diet and sleep patterns [49]. It has been observed that an RFP can increase macrophage levels and decrease bacterial levels in the body. In addition, this research showed that an RFP can increase interferon-gamma (IFN-γ), which activates antimicrobial mechanisms in the body [50]. The chart in Figure 2 clearly shows the impact of Ramadan on the immune system.
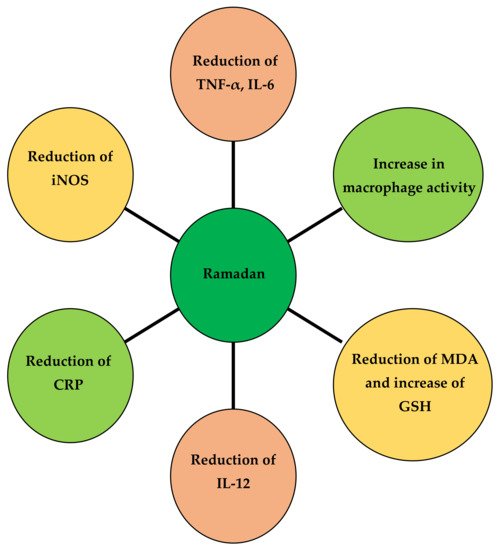
Figure 2. The beneficial effects of energy constraints on the immune system.
5. Changing the Performance and Record of Athletes during Ramadan
Many studies have examined the effects of energy restriction and RFPs on physical activity [51], but most of these studies included beginner athletes [52]. Few studies have examined the effect of RFPs and energy constraints on the performance of professional athletes [53][54][55]. The positive effects of physical exercise and an RFP on the body and overall health have been proven. Both are positive ways to increase the lipolysis of adipose tissue and muscle and reduce body fat [56]. This is also very important for Muslim athletes, as they take care of their bodies and try to maintain and improve their athletic performances [56]. It is important for Muslim athletes to be in an RFP state and exercise as it is important for them to perform their religious duties and maintain and strengthen their performance and training record [56]. When examining the effect of energy restriction and short-term RFPs on exercise performance, it was observed that physical function decreased, and this decrease was evident during an RFP. This result has been observed during moderate-term RFPs (24 to 55 h), and its main causes have been associated with dehydration; prolonged, tedious exercise; and/or very high levels of exercise. Contrary to these findings, researchers did not observe a significant reduction in athletic performance during short RFPs (11 to 24 h) [57][58]. For example, studies by Fashi et al. [55] and Stannard et al. [59] found that even a short fast can have a positive effect on a muscle’s physiological adaptation to endurance exercises. Of course, this research was performed on beginners and non-professionals. The changes observed in endurance performance during Ramadan are not limited to the training protocol, and the physiological adjustments resulting from an RFP can lead to a slowing of the metabolism during these conditions [60]. In the first week of an RFP, serum sodium, chloride, and protein levels usually increase (during the dehydrated period), a process that results in a loss of 1.13 kg of body weight, which is mostly due to dehydration. Following an increase in these factors, the release of catecholamines is suppressed, causing less venous blood to return to the heart, ultimately leading to a decrease in sympathetic function. An RFP also reduced functional capacity and maximal oxygen consumption. These changes returned to their original state when the fasting was over [60][61].
5.1. Endurance Training
Aragon-Vargas [62] reviewed the effects of an RFP lasting from 24 h to 4 days on endurance exercise and concluded that it had a negative effect on endurance. Most studies on RFPs have looked at the short-term effects, with few studies evaluating the long-term effects of RFPs. According to the literature, it takes 10 days to adjust to an RFP. In addition, most studies have examined the effect of an RFP on animal models [63][64]. Studies on animal models are difficult to correlate to humans. Zerguini et al. [65] observed a decrease in physical performance in Algerian players during Ramadan.
5.2. Resistance Training
The reduced energy-intake during an RFP can lead to a decrease in lean mass and strength, which could reduce one’s production of force and power [66]. Real-Hohn et al. [67] evaluated a fasting period (20:4) for 4 days a week and did not observe a significant effect on muscle production and muscle cross-section. Several other studies have not observed a significant effect of RFPs on energy production or power. Trabelsi et al. [68] examined the effect of an RFP on bodybuilders and did not observe a significant difference in body mass or body composition.
5.3. Sprint Performance
Various studies have shown a decrease in anaerobic capacity during Ramadan. Salama et al. [69] showed that an RFP reduced aerobic performances in the 100- and 800-m races. However, many studies [22][70] observed only a slight decrease in the mean sprint performances, but these findings were not statistically significant. Additionally, by keeping the training load constant during Ramadan, sprint speeds were significantly faster [71].
5.4. Power-Output Measure
Studies have shown that an RFP had no significant effect on a participant’s performance on Wingate anaerobic tests (peak power and average power) [72][73] but they showed a significant reduction in anaerobic capacity compared to the non-RFP hours of 17:00 and 21:00 [73].
5.5. Blood Lactate Concentration
RFPs did not have a significant effect on lactate accumulation and the time required to reach maximum blood lactate levels [55][74]. Furthermore, researchers did not observe a significant effect on blood lactate concentrations due to a 20-min run during Ramadan [75]. Additionally, another study examining the 30-s vertical jump test in judo did not observe significant changes [52].
Conflicting results have been observed in many studies. There are several reasons for such differences, including the length of fasting and the physical characteristics of the study participants. According to various studies, athletes should be advised to remain moderately active during Ramadan to ensure adequate performance and energy storage. It is recommended that more studies be performed on fasting status and athletic performance. These studies should evaluate the different mechanisms the body uses to respond to fasting conditions during Ramadan and compare them to the results of Ramadan fasting on the physiologic variables of athletes.
References
- Helms, E.R.; Zinn, C.; Rowlands, D.S.; Brown, S.R. A systematic review of dietary protein during caloric restriction in resistance trained lean athletes: A case for higher intakes. Int. J. Sport Nutr. Exerc. Metab. 2014, 24, 127–138.
- Campbell, B.I.; Aguilar, D.; Colenso-Semple, L.M.; Hartke, K.; Fleming, A.R.; Fox, C.D.; Longstrom, J.M.; Rogers, G.E.; Mathas, D.B.; Wong, V. Intermittent energy restriction attenuates the loss of fat free mass in resistance trained individuals. A randomized controlled trial. J. Funct. Morphol. Kinesiol. 2020, 5, 19.
- Phillips, S.M. A brief review of higher dietary protein diets in weight loss: A focus on athletes. Sports Med. 2014, 44, 149–153.
- Westerterp-Plantenga, M.S. Challenging energy balance-during sensitivity to food reward and modulatory factors implying a risk for overweight-during body weight management including dietary restraint and medium-high protein diets. Physiol. Behav. 2020, 221, 112879.
- Santos-Hernández, M.; Miralles, B.; Amigo, L.; Recio, I. Intestinal signaling of proteins and digestion-derived products relevant to satiety. J. Agric. Food Chem. 2018, 66, 10123–10131.
- Mariotti, F.; Gardner, C.D. Dietary protein and amino acids in vegetarian diets—A review. Nutrients 2019, 11, 2661.
- Pesta, D.H.; Samuel, V.T. A high-protein diet for reducing body fat: Mechanisms and possible caveats. Nutr. Metab. 2014, 11, 53.
- Patterson, R.E.; Sears, D.D. Metabolic effects of intermittent fasting. Annu. Rev. Nutr. 2017, 37, 371–393.
- Burke, L.M.; King, C. Ramadan fasting and the goals of sports nutrition around exercise. J. Sports Sci. 2012, 30, S21–S31.
- Zuo, L.; He, F.; Tinsley, G.M.; Pannell, B.K.; Ward, E.; Arciero, P.J. Comparison of high-protein, intermittent fasting low-calorie diet and heart healthy diet for vascular health of the obese. Front. Physiol. 2016, 7, 350.
- Hager, A.-S.; Wolter, A.; Jacob, F.; Zannini, E.; Arendt, E.K. Nutritional properties and ultra-structure of commercial gluten free flours from different botanical sources compared to wheat flours. J. Cereal Sci. 2012, 56, 239–247.
- Paoli, A.; Tinsley, G.; Bianco, A.; Moro, T. The influence of meal frequency and timing on health in humans: The role of fasting. Nutrients 2019, 11, 719.
- Marques-Lopes, I.; Forga, L.; Martınez, J.A. Thermogenesis induced by a high-carbohydrate meal in fasted lean and overweight young men: Insulin, body fat, and sympathetic nervous system involvement. Nutrition 2003, 19, 25–29.
- Rodríguez-Villar, C.; Manzanares, J.M.; Casals, E.; Pérez-Heras, A.; Zambón, D.; Gomis, R.; Ros, E. High-monounsaturated fat, olive oil-rich diet has effects similar to a high-carbohydrate diet on fasting and postprandial state and metabolic profiles of patients with type 2 diabetes. Metab. Clin. Exp. 2000, 49, 1511–1517.
- Jensen, M.D.; Haymond, M.W.; Gerich, J.E.; Cryer, P.E.; Miles, J.M. Lipolysis during fasting. Decreased suppression by insulin and increased stimulation by epinephrine. J. Clin. Investig. 1987, 79, 207–213.
- Klein, S.; Holland, O.B.; Wolfe, R.R. Importance of blood glucose concentration in regulating lipolysis during fasting in humans. Am. J. Physiol. Endocrinol. Metab. 1990, 258, E32–E39.
- Coppack, S.W.; Jensen, M.D.; Miles, J.M. In Vivo regulation of lipolysis in humans. J. Lipid Res. 1994, 35, 177–193.
- Bai, J.; Farias-Pereira, R.; Zhang, Y.; Jang, M.; Park, Y.; Kim, K.H. C. elegans ACAT regulates lipolysis and its related lifespan in fasting through modulation of the genes in lipolysis and insulin/IGF-1 signaling. BioFactors 2020, 46, 754–765.
- Gao, J.; Shakhmatova, E.; Iu, V.N. Responses of the rat kidney to the water load test and vasopressin administered during normal feeding and fasting. Ross. Fiziol. Zhurnal Im. IM Sechenova 2004, 90, 202–211.
- Finnell, J.S.; Saul, B.C.; Goldhamer, A.C.; Myers, T.R. Is fasting safe? A chart review of adverse events during medically supervised, water-only fasting. BMC Complement. Altern. Med. 2018, 18, 67.
- Trabelsi, K.; Rebai, H.; El-Abed, K.; Stannard, S.R.; Khannous, H.; Masmoudi, L.; Sahnoun, Z.; Hakim, A.; Fellman, N.; Tabka, Z. Effect of ramadan fasting on body water status markers after a rugby sevens match. Asian J. Sports Med. 2011, 2, 186–194.
- Chaouachi, A.; Leiper, J.B.; Chtourou, H.; Aziz, A.R.; Chamari, K. The effects of Ramadan intermittent fasting on athletic performance: Recommendations for the maintenance of physical fitness. J. Sports Sci. 2012, 30, S53–S73.
- Aziz, A.R.; Wahid, M.F.; Png, W.; Jesuvadian, C.V. Effects of Ramadan fasting on 60 min of endurance running performance in moderately trained men. Br. J. Sports Med. 2010, 44, 516–521.
- Solianik, R.; Sujeta, A. Two-day fasting evokes stress, but does not affect mood, brain activity, cognitive, psychomotor, and motor performance in overweight women. Behav. Brain Res. 2018, 338, 166–172.
- Solianik, R.; Žlibinaitė, L.; Drozdova-Statkevičienė, M.; Sujeta, A. Forty-eight-hour fasting declines mental flexibility but improves balance in overweight and obese older women. Physiol. Behav. 2020, 223, 112995.
- Gigou, P.-Y.; Dion, T.; Asselin, A.; Berrigan, F.; Goulet, E.D. Pre-exercise hyperhydration-induced bodyweight gain does not alter prolonged treadmill running time-trial performance in warm ambient conditions. Nutrients 2012, 4, 949–966.
- Zorbas, Y.; Ichinose, M.; Sakagamis, M. Fluid electrolyte changes in physically healthy subjects during prolonged restriction of motor activity and daily hyperhydration. Mater. Med. Polona. Pol. J. Med. Pharm. 1993, 25, 97–107.
- Bak, A.; Tsiami, A.; Greene, C. Methods of assessment of hydration status and their usefulness in detecting dehydration in the elderly. Curr. Res. Nutr. Food Sci. 2017, 5, 43–54.
- Trabelsi, K.; Stannard, S.R.; Chtourou, H.; Moalla, W.; Ghozzi, H.; Jamoussi, K.; Hakim, A. Monitoring athletes’ hydration status and sleep patterns during Ramadan observance: Methodological and practical considerations. Biol. Rhythm Res. 2018, 49, 337–365.
- Ramadan, J.; Telahoun, G.; Al-Zaid, N.S.; Barac-Nieto, M. Responses to exercise, fluid, and energy balances during Ramadan in sedentary and active males. Nutrition 1999, 15, 735–739.
- Roky, R.; Chapotot, F.; Hakkou, F.; Benchekroun, M.T.; Buguet, A. Sleep during Ramadan intermittent fasting. J. Sleep Res. 2001, 10, 319–327.
- Bouhlel, E.; Shephard, R.J. Optimizing Physical Performance during Fasting and Dietary Restriction: Implications for Athletes and Sports Medicine; CRC Press: Boca Raton, FL, USA, 2015.
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Ann. Intern. Med. 2009, 151, 264–269.
- Bouhlel, E.; Salhi, Z.; Bouhlel, H.; Mdella, S.; Amamou, A.; Zaouali, M.; Mercier, J.; Bigard, X.; Tabka, Z.; Zbidi, A. Effect of Ramadan fasting on fuel oxidation during exercise in trained male rugby players. Diabetes Metab. 2006, 32, 617–624.
- Attarzadeh Hosseini, S.R.; Hejazi, K. The Effects of Ramadan Fasting and Physical Activity on Blood Hematological-Biochemical Parameters. Iran. J. Basic Med. Sci. 2013, 16, 845–849.
- Hosseini, S.; Motahari Rad, M.; Hejazi, K. The effects of Ramadan fasting and physical activity on body composition and hematological biochemical parameters. J. Fasting Health 2014, 2, 96–103.
- Maughan, R.J.; Leiper, J.B.; Bartagi, Z.; Zrifi, R.; Zerguini, Y.; Dvorak, J. Effect of Ramadan fasting on some biochemical and haematological parameters in Tunisian youth soccer players undertaking their usual training and competition schedule. J. Sports Sci. 2008, 26, S39–S46.
- DeLang, M.D.; Salamh, P.A.; Chtourou, H.; Saad, H.B.; Chamari, K. The Effects of Ramadan Intermittent Fasting on Football Players and Implications for Domestic Football Leagues Over the Next Decade: A Systematic Review. Sports Med. 2021, 52, 585–600.
- Tayebi, S.M.; Hanachi, P.; Niaki, A.G.; Ali, P.N.; Ghaziani, F.G.-A. Ramadan fasting and weight-lifting training on vascular volumes and hematological profiles in young male weight-lifters. Glob. J. Health Sci. 2010, 2, 160.
- Alwarawrah, Y.; Kiernan, K.; MacIver, N.J. Changes in nutritional status impact immune cell metabolism and function. Front. Immunol. 2018, 9, 1055.
- Fock, R.A.; Vinolo, M.A.R.; Rocha, V.d.M.S.; de Sá Rocha, L.C.; Borelli, P. Protein-energy malnutrition decreases the expression of TLR-4/MD-2 and CD14 receptors in peritoneal macrophages and reduces the synthesis of TNF-α in response to lipopolysaccharide (LPS) in mice. Cytokine 2007, 40, 105–114.
- Wang, X.; Yang, Q.; Liao, Q.; Li, M.; Zhang, P.; Santos, H.O.; Kord-Varkaneh, H.; Abshirini, M. Effects of intermittent fasting diets on plasma concentrations of inflammatory biomarkers: A systematic review and meta-analysis of randomized controlled trials. Nutrition 2020, 79, 110974.
- Nobari, H.; Cholewa, J.M.; Pérez-Gómez, J.; Castillo-Rodríguez, A. Effects of 14-weeks betaine supplementation on pro-inflammatory cytokines and hematology status in professional youth soccer players during a competition season: A double blind, randomized, placebo-controlled trial. J. Int. Soc. Sports Nutr. 2021, 18, 42.
- Adawi, M.; Watad, A.; Brown, S.; Aazza, K.; Aazza, H.; Zouhir, M.; Sharif, K.; Ghanayem, K.; Farah, R.; Mahagna, H. Ramadan fasting exerts immunomodulatory effects: Insights from a systematic review. Front. Immunol. 2017, 8, 1144.
- Chaouachi, A.; Coutts, A.J.; Wong, D.P.; Roky, R.; Mbazaa, A.; Amri, M.; Chamari, K. Haematological, inflammatory, and immunological responses in elite judo athletes maintaining high training loads during Ramadan. Appl. Physiol. Nutr. Metab. 2009, 34, 907–915.
- Ho, R.C.; Hirshman, M.F.; Li, Y.; Cai, D.; Farmer, J.R.; Aschenbach, W.G.; Witczak, C.A.; Shoelson, S.E.; Goodyear, L.J. Regulation of IκB kinase and NF-κB in contracting adult rat skeletal muscle. Am. J. Physiol. Cell Physiol. 2005, 289, C794–C801.
- Nobari, H.; Nejad, H.A.; Kargarfard, M.; Mohseni, S.; Suzuki, K.; Carmelo Adsuar, J.; Pérez-Gómez, J. The Effect of Acute Intense Exercise on Activity of Antioxidant Enzymes in Smokers and Non-Smokers. Biomolecules 2021, 11, 171.
- Mo’ez, A.-I.E.; Salem, M.L.; Jahrami, H.A.; Madkour, M.I.; BaHammam, A.S. Ramadan intermittent fasting and immunity: An important topic in the era of COVID-19. Ann. Thorac. Med. 2020, 15, 125–133.
- Moghadam, M.T.; Taati, B.; Paydar Ardakani, S.M.; Suzuki, K. Ramadan fasting during the COVID-19 pandemic; observance of health, nutrition and exercise criteria for improving the immune system. Front. Nutr. 2021, 7, 570235.
- Rhodes, C.H. A Single Bout of 36 Hours of Fasting in Humans Induces Potent Immunomodulatory Effects on Macrophage and Upregulates the Circulation of Multiple Metabolites That Mimic These Immunomodulatory Effects In Vitro and Extend Lifespan in C. elegans; University of California: Davis, CA, USA, 2020.
- Rynders, C.A.; Thomas, E.A.; Zaman, A.; Pan, Z.; Catenacci, V.A.; Melanson, E.L. Effectiveness of intermittent fasting and time-restricted feeding compared to continuous energy restriction for weight loss. Nutrients 2019, 11, 2442.
- Chaouachi, A.; Coutts, A.J.; Chamari, K.; Wong, d.P.; Chaouachi, M.; Chtara, M.; Roky, R.; Amri, M. Effect of Ramadan intermittent fasting on aerobic and anaerobic performance and perception of fatigue in male elite judo athletes. J. Strength Cond. Res. 2009, 23, 2702–2709.
- Abaidia, A.-E.; Daab, W.; Bouzid, M.A. Effects of Ramadan fasting on physical performance: A systematic review with meta-analysis. Sports Med. 2020, 50, 1009–1026.
- Bouzid, M.A.; Abaïdia, A.-E.; Bouchiba, M.; Ghattassi, K.; Daab, W.; Engel, F.A.; Chtourou, H. Effects of Ramadan fasting on recovery following a simulated soccer match in professional soccer players: A pilot study. Front. Physiol. 2019, 10, 1480.
- Fashi, M.; Ahmadizad, S.; Nobari, H.; Pérez-Gómez, J.; Oliveira, R.; Carlos-Vivas, J.; Ardigò, L.P. Effect of acute ramadan fasting on muscle function and buffering system of male athletes. Healthcare 2021, 9, 397.
- Zouhal, H.; Saeidi, A.; Salhi, A.; Li, H.; Essop, M.F.; Laher, I.; Rhibi, F.; Amani-Shalamzari, S.; Abderrahman, A.B. Exercise training and fasting: Current insights. Open Access J. Sports Med. 2020, 11, 1–28.
- Small, S.D.; Margolis, L.M. Impact of Dietary Carbohydrate Restriction versus Energy Restriction on Exogenous Carbohydrate Oxidation during Aerobic Exercise. Adv. Nutr. 2021, 13, 559–567.
- Levy, E.; Chu, T. Intermittent fasting and its effects on athletic performance: A review. Curr. Sports Med. Rep. 2019, 18, 266–269.
- Stannard, S.R.; Buckley, A.J.; Edge, J.A.; Thompson, M.W. Adaptations to skeletal muscle with endurance exercise training in the acutely fed versus overnight-fasted state. J. Sci. Med. Sport 2010, 13, 465–469.
- Weinsier, R.L. Fasting—A review with emphasis on the electrolytes. Am. J. Med. 1971, 50, 233–240.
- Darzabi, T.; Hejazi, K. The Effects of Ramadan Fasting on Electrolytes Index, Serum Osmolarity and Body Composition in Fasting and Non-Fasting Students: A Quasi-Experimental Study. Jundishapur J. Chronic Dis. Care 2020, 9, e100079.
- Aragón-Vargas, L.F. Effects of fasting on endurance exercise. Sports Med. 1993, 16, 255–265.
- Muñoz-Hernández, L.; Márquez-López, Z.; Mehta, R.; Aguilar-Salinas, C.A. Intermittent fasting as part of the management for T2DM: From animal models to human clinical studies. Curr. Diabetes Rep. 2020, 20, 13.
- Lv, M.; Zhu, X.; Wang, H.; Wang, F.; Guan, W. Roles of caloric restriction, ketogenic diet and intermittent fasting during initiation, progression and metastasis of cancer in animal models: A systematic review and meta-analysis. PLoS ONE 2014, 9, e115147.
- Zerguini, Y.; Kirkendall, D.; Junge, A.; Dvorak, J. Impact of Ramadan on physical performance in professional soccer players. Br. J. Sports Med. 2007, 41, 398–400.
- Liu, Y.; Cotillard, A.; Vatier, C.; Bastard, J.-P.; Fellahi, S.; Stevant, M.; Allatif, O.; Langlois, C.; Bieuvelet, S.; Brochot, A. A dietary supplement containing cinnamon, chromium and carnosine decreases fasting plasma glucose and increases lean mass in overweight or obese pre-diabetic subjects: A randomized, placebo-controlled trial. PLoS ONE 2015, 10, e0138646.
- Real-Hohn, A.; Navegantes, C.; Ramos, K.; Ramos-Filho, D.; Cahuê, F.; Galina, A.; Salerno, V.P. The synergism of high-intensity intermittent exercise and every-other-day intermittent fasting regimen on energy metabolism adaptations includes hexokinase activity and mitochondrial efficiency. PLoS ONE 2018, 13, e0202784.
- Trabelsi, K.; Stannard, S.R.; Ghlissi, Z.; Maughan, R.J.; Kallel, C.; Jamoussi, K.; Zeghal, K.M.; Hakim, A. Effect of fed-versus fasted state resistance training during Ramadan on body composition and selected metabolic parameters in bodybuilders. J. Int. Soc. Sports Nutr. 2013, 10, 23.
- Salama, B.; Hsairi, M.; Belaid, J.; Achour, N.; Achour, A.; Nacef, T. Food intake and energy expenditure in high school athletes before, during and after the month of Ramadan: Effect of fasting on performance. La Tunis. Méd. 1993, 71, 85–89.
- Mhenni, T.; Souissi, A.; Tayech, A.; Yousfi, N.; Mejri, M.A.; Chamari, K.; Souissi, N.; Khlifa, R.; Haddad, M. The effect of Ramadan fasting on the morning–evening difference in team-handball-related short-term maximal physical performances in elite female team-handball players. Chronobiol. Int. 2021, 38, 1488–1499.
- Killen, S.S.; Marras, S.; McKenzie, D.J. Fast growers sprint slower: Effects of food deprivation and re-feeding on sprint swimming performance in individual juvenile European sea bass. J. Exp. Biol. 2014, 217, 859–865.
- Chtourou, H.; Hammouda, O.; Souissi, H.; Chamari, K.; Chaouachi, A.; Souissi, N. The effect of Ramadan fasting on physical performances, mood state and perceived exertion in young footballers. Asian J. Sports Med. 2011, 2, 177–185.
- Chtourou, H.; Hammouda, O.; Chaouachi, A.; Chamari, K.; Souissi, N. The effect of time-of-day and Ramadan fasting on anaerobic performances. Int. J. Sports Med. 2012, 33, 142–147.
- Champagne, C.D.; Crocker, D.E.; Fowler, M.A.; Houser, D.S. Fasting physiology of the pinnipeds: The challenges of fasting while maintaining high energy expenditure and nutrient delivery for lactation. In Comparative Physiology of Fasting, Starvation, and Food Limitation; Springer: Berlin/Heidelberg, Germany, 2012; pp. 309–336.
- Güvenç, A. Effects of Ramadan fasting on body composition, aerobic performance and lactate, heart rate and perceptual responses in young soccer players. J. Hum. Kinet. 2011, 29, 79–91.
More
Information
Contributors
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
1.0K
Revisions:
3 times
(View History)
Update Date:
30 Aug 2022
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





