
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Prashant Kaushik | -- | 2123 | 2022-04-21 08:40:55 | | | |
| 2 | Vivi Li | Meta information modification | 2123 | 2022-04-22 06:18:04 | | |
Video Upload Options
Datura, a genus of medicinal herb from the Solanaceae family, is credited with toxic as well as medicinal properties. The different plant parts of Datura sp., mainly D. stramonium L., commonly known as Datura or Jimson Weed, exhibit potent analgesic, antiviral, anti-diarrheal, and anti-inflammatory activities, owing to the wide range of bioactive constituents. With these pharmacological activities, D. stramonium is potentially used to treat numerous human diseases, including ulcers, inflammation, wounds, rheumatism, gout, bruises and swellings, sciatica, fever, toothache, asthma, and bronchitis. The primary phytochemicals investigation on plant extract of Datura showed alkaloids, carbohydrates, cardiac glycosides, tannins, flavonoids, amino acids, and phenolic compounds. It also contains toxic tropane alkaloids, including atropine, scopolamine, and hyoscamine. Although some studies on D. stramonium have reported potential pharmacological effects, information about the toxicity remains almost uncertain. Moreover, the frequent abuse of D. stramonium for recreational purposes has led to toxic syndromes. Therefore, it becomes necessary to be aware of the toxic aspects and the potential risks accompanying its use.
1. Introduction
2. Biochemical Composition of Datura
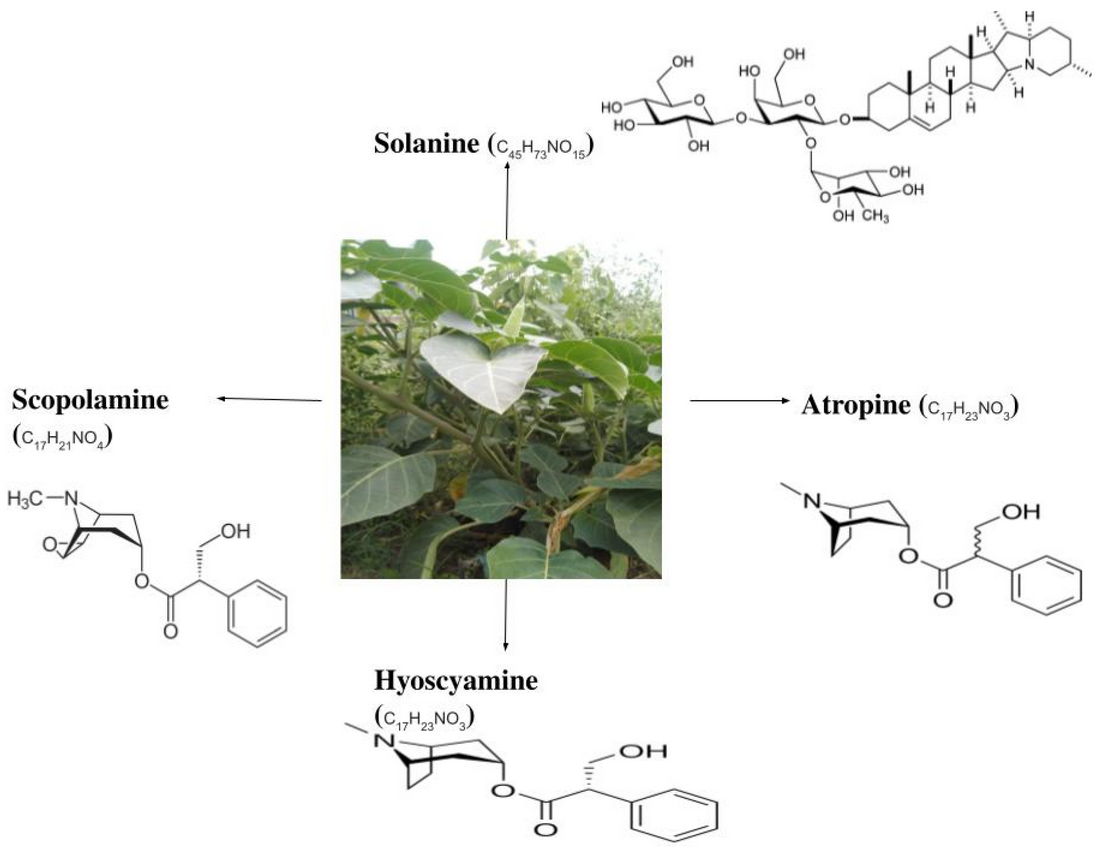
3. Pharmacological Activity of Datura
3.1. Anti-Inflammatory and Analgesic Activities
3.2. Antioxidation Activities
3.3. Antimicrobial Potential of Datura
3.4. Anti-Asthmatic and Bronchodilating Effects
References
- Sayyed, A.; Shah, M. Phytochemistry, Pharmacological and Traditional Uses of Datura stramonium L. Rev. J. Pharm. Phytochem. 2014, 2, 123–125.
- Alabri, T.H.A.; Al Musalami, A.H.S.; Hossain, M.A.; Weli, A.M.; Al-Riyami, Q. Comparative Study of Phytochemical Screening, Antioxidant and Antimicrobial Capacities of Fresh and Dry Leaves Crude Plant Extracts of Datura metel L. J. King Saud Univ. Sci. 2014, 26, 237–243.
- Gaire, B.P.; Subedi, L. A Review on the Pharmacological and Toxicological Aspects of Datura stramonium L. J. Integr. Med. 2013, 11, 73–79.
- Monira, K.M.; Munan, S.M. Review on Datura Metel: A Potential Medicinal Plant. Glob. J. Res. Med. Plants Indig. Med. 2012, 1, 123.
- Nasir, B.; Baig, M.W.; Majid, M.; Ali, S.M.; Khan, M.Z.I.; Kazmi, S.T.B.; Haq, I. Preclinical Anticancer Studies on the Ethyl Acetate Leaf Extracts of Datura Stramonium and Datura Inoxia. BMC Complement. Med. Ther. 2020, 20, 188.
- Shah, V.V.; Shah, N.D.; Patrekar, P.V. Medicinal Plants from Solanaceae Family. Res. J. Pharm. Technol. 2013, 6, 143–151.
- Alam, W.; Khan, H.; Khan, S.A.; Nazir, S.; Akkol, E.K. Datura Metel: A Review on Chemical Constituents, Traditional Uses and Pharmacological Activities. Curr. Pharm. Des. 2020, 27, 2545–2557.
- Al-Snafi, A.E. Medical Importance of Datura fastuosa (Syn: Datura metel) and Datura stramonium—A Review. IOSR J. Pharm. 2017, 7, 43–58.
- Devi, M.R.; Bawari, M.; Paul, S.B.; Sharma, G.D. Neurotoxic and Medicinal Properties of Datura stramonium L.–Review. Assam Univ. J. Sci. Technol. 2011, 7, 139–144.
- Meselhy, K.M. Cytotoxic and Insect-Repellent Activities of Surface Flavonoids from Datura stramonium L. Grown in Egypt. Life Sci. J. 2012, 9, 3154–3158.
- Jakabová, S.; Vincze, L.; Farkas, Á.; Kilár, F.; Boros, B.; Felinger, A. Determination of Tropane Alkaloids Atropine and Scopolamine by Liquid Chromatography–Mass Spectrometry in Plant Organs of Datura Species. J. Chromatogr. A 2012, 1232, 295–301.
- Setshogo, M.P. A Review of Some Medicinal and or Hallucinogenic Solanaceous Plants of Botswana: The Genus Datura L. Int. J. Appl. Res. Nat. Prod. 2015, 1, 15–23.
- Soni, P.; Siddiqui, A.A.; Dwivedi, J.; Soni, V. Pharmacological Properties of Datura stramonium L. as a Potential Medicinal Tree: An Overview. Asian Pac. J. Trop. Biomed. 2012, 2, 1002–1008.
- Kadam, S.D.; Chavhan, S.A.; Shinde, S.A.; Sapkal, P.N. Pharmacognostic Review on Datura. Int. J. Pharm. Chin. Med. 2018, 2, 1–9.
- Naik, V.; Babu, K.S.; Latha, J.; Kolluru, B. A Review on Phytochemical and Pharmacological Activity of Datura stramonium. (Medicinal Plant). Res. J. Pharmacogn. Phytochem. 2018, 10, 77–80.
- Mukhtar, Y.; Tukur, S.; Bashir, R.A. An Overview on Datura stramonium L. (Jimson Weed): A Notable Psychoactive Drug Plant. Am. J. Nat. Sci. 2019, 2, 1–9.
- Das, S.; Kumar, P.; Basu, S.P. Phytoconstituents and Therapeutic Potentials of Datura stramonium Linn. J. Drug Deliv. Ther. 2012, 2, 4–7.
- Boumba, V.; Mitselou, A.; Vujuk, T. Fatal Poisoning from Ingestion of Datura stramonium Seeds. Vet. Hum. Toxicol. 2004, 46, 81–82.
- Bagewadi, Z.K.; Muddapur, U.M.; Madiwal, S.S.; Mulla, S.I.; Khan, A. Biochemical and Enzyme Inhibitory Attributes of Methanolic Leaf Extract of Datura inoxia Mill. Environ. Sustain. 2019, 2, 75–87.
- Fatima, H.; Khan, K.; Zia, M.; Ur-Rehman, T.; Mirza, B.; Haq, I. Extraction Optimization of Medicinally Important Metabolites from Datura innoxia Mill.: An in Vitro Biological and Phytochemical Investigation. BMC Complement. Altern. Med. 2015, 15, 376.
- Nayyar, M.S.; Hanif, M.A.; Mjaeed, M.I.; Ayub, M.A.; Rehman, R. Datura. In Medicinal Plants of South Asia; Elsevier: Amsterdam, The Netherlands, 2020; pp. 207–216.
- Lim, K.M.C.; Dagalea, F.M.S.; Vicencio, M.C.G. Antibacterial Activity of Datura metel Linn. (TALONG-PUNAY) Fruit Extract. J. Pharm. Res. Int. 2020, 32, 96–101.
- Nandakumar, A.; Vaganan, M.M.; Sundararaju, P.; Udayakumar, R. Phytochemical Analysis and Nematicidal Activity of Ethanolic Leaf Extracts of Datura metel, Datura inoxia and Brugmansia suaveolens against Meloidogyne incognita. Asian J. Biol. 2017, 2, 1–11.
- Al-Snafi, A.E. Medicinal Plants Alkaloids, as Promising Therapeutics-A Review (Part 1). IOSR J. Pharm. 2021, 11, 51–67.
- Alinejad, S.; Sarabi, V.; Bakhtvari, A.R.S.; Hashempour, H. Variation in Physiological Traits, Yield and Secondary Metabolites of Jimsonweed (Datura stramonium L.) under Different Irrigation Regimes and Nutrition Systems. Ind. Crop. Prod. 2020, 143, 111916.
- Oseni, O.A.; Olarinoye, C.O.; Amoo, I.A. Studies on Chemical Compositions and Functional Properties of Thorn Apple (Datura stramonium L.) Solanaceae. Afr. J. Food Sci. 2010, 5, 40–44.
- Butnariu, M. An Analysis of Sorghum Halepense’s Behavior in Presence of Tropane Alkaloids from Datura stramonium Extracts. Chem. Cent. J. 2012, 6, 75.
- Maheshwari, N.O.; Khan, A.; Chopade, B.A. Rediscovering the Medicinal Properties of Datura Sp.: A Review. J. Med. Plants Res. 2013, 7, 2885–2897.
- Roy, S.; Samant, L.; Ganjhu, R.; Mukherjee, S.; Chowdhary, A. Assessment of in Vivo Antiviral Potential of Datura metel Linn. Extracts against Rabies Virus. Pharmacogn. Res. 2018, 10, 109.
- Roy, S.; Mukherjee, S.; Pawar, S.; Chowdhary, A. Evaluation of In Vitro Antiviral Activity of Datura metel Linn. against Rabies Virus. Pharmacogn. Res. 2016, 8, 265.
- Hameed Baloch, I.A.; Hanif-ur-Rehman, I.A.B. Review Article on Poisonous Plants of Balochistan. Balochistaniyat 2017, 6, 36–56.
- Agarwal, R.; Gupta, R.; Yadav, R.; Asati, V.; Rathi, J.C. Anti-Inflammatory Activity of Seeds Extract of Datura stramonium against Carrageenan Induced Paw Edema on Albino Wistar Rats. J. Pharm. Biol. Sci. 2019, 7, 41–46.
- Chandan, G.; Kumar, C.; Chibber, P.; Kumar, A.; Singh, G.; Satti, N.K.; Gulilat, H.; Saini, A.K.; Bishayee, A.; Saini, R.V. Evaluation of Analgesic and Anti-Inflammatory Activities and Molecular Docking Analysis of Steroidal Lactones from Datura stramonium L. Phytomedicine 2021, 89, 153621.
- Muthusamy, P.; Nivedhitha, M.; Jayshree, N. Analgesic and Anti-Inflammatory Activities of Datura metel Linn. Root in Experimental Animal Models. Res. J. Pharm. Technol. 2010, 3, 897–899.
- Nivedhitha, S.; Gobinath, M.; Muthusamy, P.; Rao, K.M. Studies on Anti-Inflammatory Activity of Root Extracts of Datura fastuosa (Linn). J. Pharm. Res. 2010, 3, 2686–2688.
- Jaafar, F.R.; Ajeena, S.J.; Mehdy, S.S. Anti-Inflammatory Impacts and Analgesiac Activity of Aqueous Extract Datura innoxia Leaves against Induced Pain and Inflammation in Mice. J. Entomol. Zool. Stud. 2018, 6, 1894–1899.
- Belayneh, Y.M.; Birhanu, Z.; Birru, E.M.; Getenet, G. Evaluation of In Vivo Antidiabetic, Antidyslipidemic, and in Vitro Antioxidant Activities of Hydromethanolic Root Extract of Datura stramonium, L. (Solanaceae). J. Exp. Pharmacol. 2019, 11, 29.
- Iqbal, S.; Sivaraj, C.; Gunasekaran, K. Antioxidant and Anticancer Activities of Methanol Extract of Seeds of Datura stramonium L. Free Radic. Antioxid. 2017, 7, 184–189.
- Al-Snafi, A.E. Medicinal Plants Possessed Antioxidant and Free Radical Scavenging Effects (Part 3)—A Review. IOSR J. Pharm. 2017, 7, 48–62.
- Khan, W.; Subhan, S.; Shams, D.F.; Afridi, S.G.; Ullah, R.; Shahat, A.A.; Alqahtani, A.S. Antioxidant Potential, Phytochemicals Composition, and Metal Contents of Datura Alba. BioMed Res. Int. 2019, 2019, 2403718.
- Gachande, B.D.; Khillare, E.M. In-Vitro Evaluation of Datura Species for Potential Antimicrobial Activity. Biosci. Discov. 2013, 4, 78–81.
- Shagal, M.H.; Modibbo, U.U.; Liman, A.B. Pharmacological Justification for the Ethnomedical Use of Datura stramonium Stem-Bark Extract in Treatment of Diseases Caused by Some Pathogenic Bacteria. Int. Res. Pharm. Pharmacol. 2012, 2, 16–19.
- Girmay, S. Preliminary Phytochemical Screening and In Vitro Antimicrobial Activity of Datura stramonium Leaves Extracts Collected from Eastern Ethiopia. Res. J. Chem. Sci. 2015, 22, 606X.
- Ibrahim, M.; Siddique, S.; Rehman, K.; Husnain, M.; Hussain, A.; Akash, M.S.H.; Azam, F. Comprehensive Analysis of Phytochemical Constituents and Ethnopharmacological Investigation of Genus Datura. Crit. Rev. Eukaryot. Gene Expr. 2018, 28, 223–283.
- Kalim, M.; Hussain, F.; Ali, H.; Ahmad, I.; Iqbal, M.N. Antifungal Activities of Methanolic Extracts of Datura inoxia. PSM Biol. Res. 2016, 1, 70–73.
- Bachheti, R.K.; Rai, I.; Mishra, V.K.; Joshi, A. Antioxidant and Antimicrobial Properties of Seed Oil of Datura metel. J. Environ. Biol. 2018, 39, 182–188.
- Choudhary, M.; Sharma, I.; Agrawal, D.C.; Dhar, M.K.; Kaul, S. Neurotoxic Potential of Alkaloids from Thorn Apple (Datura stramonium L.): A Commonly Used Indian Folk Medicinal Herb. In Medicinal Herbs and Fungi; Springer: Berlin/Heidelberg, Germany, 2021; pp. 391–420.
- Kuraki, T. Bronchodilators for COPD: At What Stage Should Therapeutic Intervention Be Initiated? In Chronic Obstructive Pulmonary Disease; Springer: Berlin/Heidelberg, Germany, 2017; pp. 211–243.
- Yamada, M.; Ichinose, M. The Cholinergic Pathways in Inflammation: A Potential Pharmacotherapeutic Target for COPD. Front. Pharmacol. 2018, 9, 1426.
- Papi, A.; Fabbri, L.M.; Kerstjens, H.A.; Rogliani, P.; Watz, H.; Singh, D. Inhaled Long-Acting Muscarinic Antagonists in Asthma—A Narrative Review. Eur. J. Intern. Med. 2021, 85, 14–22.
- Miraj, S. Datura Stramonium: An Updated Review. Pharm. Chem. 2016, 8, 253–257.





