Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Abeer M Al-Ghananeem | -- | 1537 | 2022-04-15 19:22:08 | | | |
| 2 | Rita Xu | Meta information modification | 1537 | 2022-04-18 05:10:59 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Al-Ghananeem, A.M.; , .; Alrafayah, E.; Abu Laila, S. Pediatric Dosage Forms. Encyclopedia. Available online: https://encyclopedia.pub/entry/21829 (accessed on 04 June 2026).
Al-Ghananeem AM, , Alrafayah E, Abu Laila S. Pediatric Dosage Forms. Encyclopedia. Available at: https://encyclopedia.pub/entry/21829. Accessed June 04, 2026.
Al-Ghananeem, Abeer M, , Enas Alrafayah, Salam Abu Laila. "Pediatric Dosage Forms" Encyclopedia, https://encyclopedia.pub/entry/21829 (accessed June 04, 2026).
Al-Ghananeem, A.M., , ., Alrafayah, E., & Abu Laila, S. (2022, April 15). Pediatric Dosage Forms. In Encyclopedia. https://encyclopedia.pub/entry/21829
Al-Ghananeem, Abeer M, et al. "Pediatric Dosage Forms." Encyclopedia. Web. 15 April, 2022.
Copy Citation
The development of pediatric-specific dose forms is particularly difficult due to a variety of factors relating to pediatric population differences from adult populations. The buccal dosage form is considered a good alternative to oral dosage form if the latter cannot be used in pediatric patients. Both oral and buccal dosage formulations uphold great application qualities for pediatric patients.
pediatrics
dosage form
formulation development
1. Introduction
Pediatric patients have traditionally been treated with off-label adult pharmaceuticals or extemporaneous compounding, which is not optimal for pediatric patients due to a lack of product safety and efficacy. In addition, off-label drug usage becomes much more complicated when it comes to neonates and children under the age of two. This is also applicable to children with rare or chronic disorders or acutely ill children. New drugs are frequently approved for adults without even a minuscule quantity of expertise in pediatric patients. Due to the absence of information, practitioners are commonly obliged to prescribe medications off-label, using poorly defined dosage methods. Half the medicine in the United States alone is not labeled for use among children [1]. Over one-third of pediatric hospitalizations (36.7%) were associated with off-label use of analgesics that have not been labeled for use in children [2].
The Best Pharmaceuticals for Children Act (BPCA) and the Pediatric Research Equity Act (PREA) are aimed to encourage more pediatric medication studies. The major objectives of these regulations include increasing in the number of medications clinically tested for pediatric use as well as ensuring these medications are available to the market with appropriate formulations and doses [3]. In addition to promoting the development of pediatric drugs, there are other peculiarities for pediatric patients that must be considered. As a result, many therapeutic medicines continue to lack pediatric-friendly dosage forms. Although the legislative decisions provided by the BCPA and the PREA benefit the pediatric research of new drugs and their labeling, these mandates can be outweighed by medications previously on the market. Medications made before the application of the legislative regulations provided by the BCPA and PREA are prone to not benefiting from these efforts.
It can be challenging to construct pediatric formulations, especially those suitable for young infants. There is a lack of data on the acceptability of different dosage forms, administration volume, dosage form size and taste, and the safety of formulation excipients in relation to age and development status. Moreover, factors such as dosing, variances in disease processes, study design, and placebo response are all linked to failures in pediatric trials [4]. It is critical to understand the reasons for failed studies and consider new strategies to design better pediatric trials in the future. Wharton et al. reported that pediatric labeling was not established for 78 medications out of 189 products under pediatric exclusivity (1998–2012), which is a failure rate of 42% [5].
The oral route tends to be most favorably used in pediatric formulations. Oral pediatric formulations are oftentimes provided in powder forms for reconstitution. These forms require purified water for reconstitution and sometimes require unique storage conditions in a refrigerated environment; yet these requirements cannot always be met. Liquid and powder forms may be unpalatable and difficult to swallow, which makes them problematic for pediatric patients. Children’s swallowing abilities may vary from adults’; however, it is usually hard for children to swallow solid dosage forms. Children younger than five years old are generally unable to safely swallow solid capsules and tablets larger than 10 mm [6]. It must also be taken into consideration that children may reject medication regardless of tablet size if the flavor is unpleasant. Clarithromycin, for example, is characteristically bitter [7] and has poor palatability when compared to other antibiotics. As a result, medications with similar unpleasantness regarding flavoring may cause conflict with dose scheduling and adherence. In place of the presence of vomiting or nausea via the oral route, despite being less common, the rectal route may be used as an alternative [8]. There is a multitude of rectal dosage forms present within markets, including suppositories, creams, enemas, and ointments; yet, administering them can most often be uncomfortable for children. In case of emergencies or oral route difficulty, the parenteral route may be adopted due to its speed. Despite the advantage of speed, the parenteral route comes with many limitations, such as the need for a trained professional to administer, the invasiveness of the process, the risk of blood-borne infections, and the presence of injury or pain induced by injections [9]. To achieve the rapid onset of action and high bioavailability goals in treatment, clinicians tend to choose the parenteral route. This approach has several drawbacks, including patient acceptability, sterility limits, and the availability of medical experts to administer. Regarding the listed challenges, the buccal route is far more appealing. In addition, the buccal route can be much more suitable in cases such as seizures, where the oral, rectal, or parenteral routes are all limited.
In addition, pediatric patients with cancer suffer from severe breakthrough episodes of pain and are in need of prompt and efficient pain treatment. The oral route, in this situation, is a poor choice, as it may take a prolonged period before eliminating discomfort. However, it could be of benefit for maintenance treatment of pain to have a sustained-release effect of medication over a prolonged period. Buccal medication delivery is an appealing administration route for pediatric pain management since it has a quick onset of action and has no hepatic first-pass metabolism. Although oral and buccal dosage formulations uphold great application qualities for pediatric patients in comparison to other commonly used dosage forms, there are still many challenges related to those dosage forms, which can be summarized into three major areas related to physiological considerations, regulatory expectations, and formulation development consideration (Figure 1).
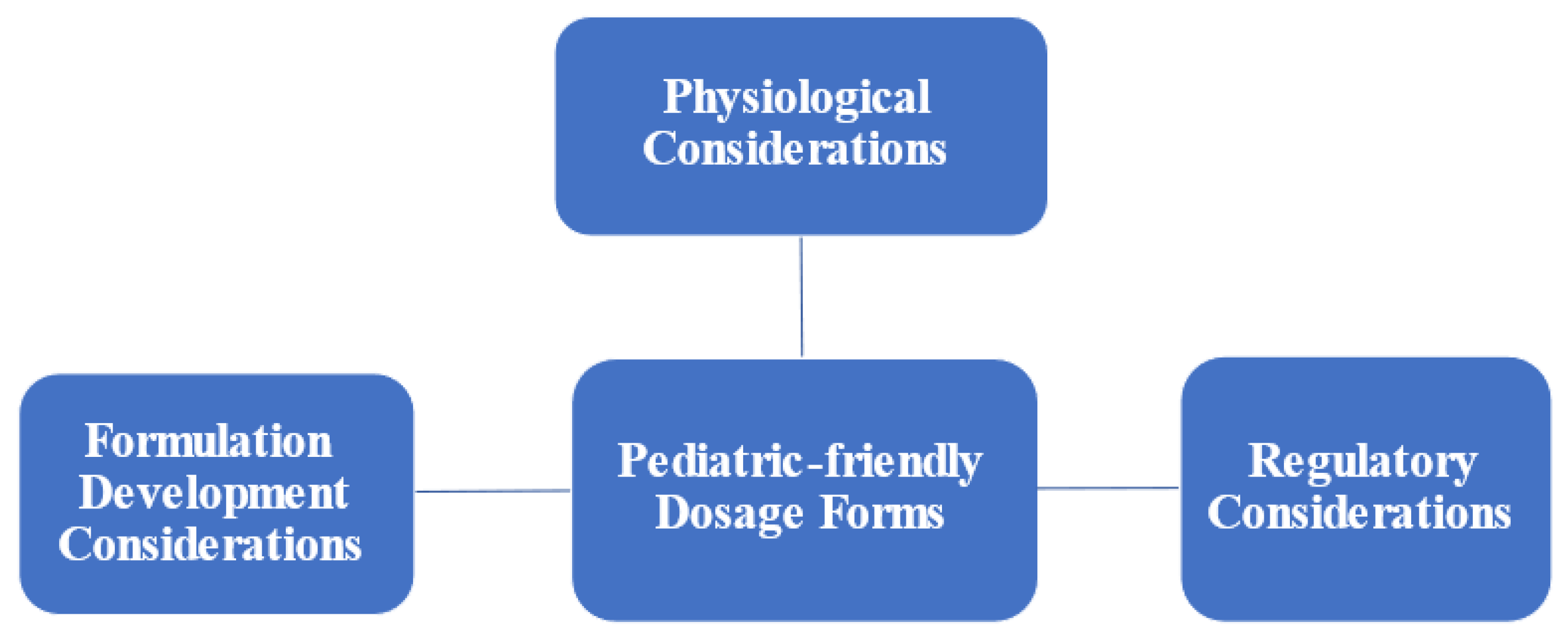
Figure 1. Challenges associated with developing pediatric-friendly dosage forms.
2. Physiological Considerations
Pediatric patients are defined as patients aged from birth to less than 16 or 18 years old (Table 1) [10]. The classification is dependent on the individual’s age. However, categorizing pediatric patients into distinct age groups for drug administration is essentially arbitrary, as it does not consider pharmacokinetic parameters, such as renal or hepatic function, volume of distribution, lipophilicity, relative blood volumes, etc. This is an issue, as certain formulations are age-specific or must be given according to body weight. As a result, the acceptability of different dose forms for different age groups must be carefully considered.
Table 1. Classification of pediatric age categories [10].
| Class | Age Group |
|---|---|
| Neonate | Birth to 27 days |
| Infant and Toddlers | 28 days to 23 months |
| Children | 2 to 11 years |
| Adolescent | 12 to 16–18 years |
The following are some of the clinical and physiological issues to consider while developing buccal pediatric dose forms:
2.1. Heterogeneity among Pediatric Patients
Variability among children (0–17 years) is a significant challenge in developing age-appropriate pediatric-friendly formulations, as this group differs in taste preferences, medicine-related side effects, and patient medical case—all of which can influence doses and dosage forms required [10]. Pediatric patients have different responses to the active ingredients and excipients due to changes in their body physiology.
2.2. Age-Related Compliance
Age-related compliance is an important challenge to consider in formulation design. Compliance is complicated, and sometimes it is caregiver dependent, especially when considering the younger ages and varying disease states. Pediatric patients have different cognitive levels during their growth, which will affect compliance for formulation. There is also a dependency on caregivers to play a role in the administration of the designed formula [11]. Age-appropriate formulations must be utilized to enhance the taste preferences of the children who are accommodated [12].
2.3. Saliva-Flow Rate
For oral and oral transmucosal dosage forms, the presence of saliva is imperative for drug absorption. Saliva provides a relatively aqueous environment to facilitate drug release, dissolution, and absorption. Over the life span of a human, both the saliva-flow rate and composition tend to change [13]. The flow rate tends to increase up until around 5 to 6 years, and then, the saliva flow rate declines, whereas the mean electrolyte content rises [14].
The rate of saliva secretion in the buccal mucosa was found to be significantly lower in children (0.22–0.82 mL/min) than in adults (0.33–1.42 mL/min) [15][16][17].
There is a direct correlation between the degree of hydration via saliva and the objectionable drug swallowing. Premature medication swallowing, on the other hand, may occur in patients with a high saliva-flow rate (the “saliva washout effect”). This action may result in non-uniform medication dispersion in saliva as well as decreased drug absorption by mucosal tissues, resulting in wide-ranging systemic bioavailability [18].
2.4. Gastrointestinal Tract (GIT) pH Values and Drug Absorption
The pH of the GIT varies depending on the location of the tissue and the patient’s age. It has a significant impact on the solubility and diffusion of drug forms, preferring the unionized form. Other factors that impact the pH of the oral mucosa include disease, drug use, nutrition, and saliva-flow rate. In general, as the rate of saliva-flow increases, so does the pH [19][20]. The intra-gastric pH of newborns is higher than 4, and intestinal cytochrome p450 activity increases with age [21]. The mean pH value of the oral mucosa is (6.78 ± 0.04) and (6.64 ± 0.44) in healthy adults and pediatric patients, respectively [19][20].
There is also significant variability in the pharmacology of drug and dosage forms between adult and pediatric populations. This is due to differences in the absorption, allocation, metabolic activity, and excretion (ADME) profile in pediatric populations, particularly within a child’s first few years [22].
References
- Sachs, A.N.; Avant, D.; Lee, C.S.; Rodriguez, W.; Murphy, M.D. Pediatric information in drug product labeling. JAMA 2012, 307, 1914–1915.
- Carmack, M.; Berde, C.; Monuteaux, M.C.; Manzi, S.; Bourgeois, F.T. Off-label use of prescription analgesics among hospitalized children in the United States. Pharmacoepidemiol. Drug Saf. 2020, 29, 474–481.
- Kölch, M.; Schnoor, K.; Fegert, J.M. The EU-regulation on medicinal products for pediatric use. ECAP 2007, 16, 229–235.
- Momper, J.D.; Mulugeta, Y.; Burckart, G.J. Failed pediatric drug development trials. CPT 2015, 98, 245–251.
- Wharton, G.T.; Murphy, M.D.; Avant, D.; Goldsmith, J.V.; Chai, G.; Rodriguez, W.J.; Eisenstein, E.L. Impact of pediatric exclusivity on drug labeling and demonstrations of efficacy. AAP 2014, 134, 512–518.
- Ebiowei SF Orubu & Catherine Tuleu. Medicines for children: Flexible solid oral formulations. Bull. World Health Organ 2017, 95, 238–240.
- Tanigake, A.; Miyanaga, Y.; Nakamura, T.; Tsuji, E.; Matsuyama, K.; Kunitomo, M.; Uchida, T. The bitterness intensity of clarithromycin evaluated by a taste sensor. CPB 2003, 51, 1241–1245.
- De boer, A.; Moolenaar, F.; De leede, L.; Breimer, D. Rectal drug administration. Clin. Pharmacokinet. 1982, 7, 285–311.
- Lam, J.K.; Xu, Y.; Worsley, A.; Wong, I.C. Oral transmucosal drug delivery for pediatric use. Adv. Drug Deliv. Rev. 2014, 73, 50–62.
- Standing, J.F.; Tuleu, C. Paediatric formulations—getting to the heart of the problem. Int. J. Pharm. 2005, 300, 56–66.
- Ivanovska, V.; Rademaker, C.M.; Van dijk, L.; Mantel-Teeuwisse, A.K. Pediatric drug formulations: A review of challenges and progress. AAP 2014, 134, 361–372.
- Davies, E.H.; Tuleu, C. Medicines for children: A matter of taste. J. Pediatr. 2008, 153, 599–604.
- Bradley, R.M. Basic Oral Physiology; Mosby Inc.: Maryland Heights, MO, USA, 1981.
- Gutman, D.; Ben-Aryeh, H. The influence of age on salivary content and rate of flow. IJOS 1974, 3, 314–317.
- Sonesson, M.; Eliasson, L.; Matsson, L. Minor salivary gland secretion in children and adults. Arch. Oral Biol. 2003, 48, 535–539.
- Dezan, C.; Nicolau, J.; Souza, D.; Walter, L. Flow rate, amylase activity, and protein and sialic acid concentrations of saliva from children aged 18, 30 and 42 months attending a baby clinic. Arch. Oral Biol. 2002, 47, 423–427.
- Rotteveel, L.J.; Jongerius, P.H.; Van limbeek, J.; Van den hoogen, F.J. Salivation in healthy schoolchildren. Int. J. Pediatr. Otorhinolaryngol. 2004, 68, 767–774.
- Rathbone, M.J.; Senel, S.; Pather, I. Oral Mucosal Drug Delivery and Therapy; Springer: New York, NY, USA, 2015.
- Aframian, D.; Davidowitz, T.; Benoliel, R. The distribution of oral mucosal pH values in healthy saliva secretors. Oral Dis. 2006, 12, 420–423.
- Hidas, A.; Noy, A.F.; Birman, N.; Shapira, J.; Matot, I.; Steinberg, D.; Moskovitz, M. Oral health status, salivary flow rate and salivary quality in children, adolescents, and young adults with ADHD. Arch. Oral Biol. 2011, 56, 1137–1141.
- Ståhlberg, M.; Hietanen, E.; Mäki, M. Mucosal biotransformation rates in the small intestine of children. Gut 1988, 29, 1058–1063.
- Van den Anker, J.N.; Schwab, M.; Kearns, G. Pediatric Clinical Pharmacology. Handbook of Experimental Pharmacology; Seyberth, H.W., Ed.; Springer: Berlin/Heidelberg, Germany, 2011; pp. 51–75.
More
Information
Subjects:
Pediatrics
Contributors
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
2.4K
Revisions:
2 times
(View History)
Update Date:
18 Apr 2022
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





