
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Francesco Borgia | + 1914 word(s) | 1914 | 2021-08-26 11:28:57 |
Video Upload Options
Light-based treatments, chiefly photodynamic therapy and phototherapy, are currently applied in skin diseases. The current knowledge about the mechanisms of action of light-based treatments in skin diseases leans to the possible involvement of epigenetic and oxidative stress mechanisms. To better understand and exploit, to the fullest, these relatively safe and reproducible treatments, several studies have focused on miRNAs, small non-encoding RNAs (22–24 nucleotides), after light-based treatments.
1. Introduction
Thanks to the progress of modern research, previously defined medical conditions seem to be more and more well described at a molecular level. One of the missing links of this complex intertwining of external and internal processes is epigenetics, literally “above genetics”, meaning those processes that link genes and their transcriptional products at a very fine level. One of the latest findings in this regard is the topic of this review, microRNAs (miRNAs), small non-encoding RNAs with a sequence capable of binding to mRNA strings. The genes encoding miRNAs, usually scattered sparsely around the genome, or included in introns and untranslated regions (UTRs) of protein genes, are a class of molecules very well integrated in the cellular processes involving multicellular organisms. The first studies regarding miRNAs and human pathology were directed in the oncology field.
Here, research led to an interesting discovery: miRNAs can be tissue-specific and lose that specificity the more the tumor is undifferentiated [1]. Later, other studies extended the field of research regarding the miRNome to other diseases. The skin, one of the main topics of this review, has been thoroughly studied in this sense. The involvement of microRNAs is well established as a mechanism associated with oxidative stress-induced damage, both as a repair mechanism and a proinflammatory one [2], and oxidative stress, particularly in chronic skin diseases treated with light-based therapy, plays a major role in disease activity and therapy response [3][4][5]. The other significant topic of this paper is light-based therapy. More and more different light sources have been used, especially in dermatology, to cure diseases based on the properties of specific wavelengths.
The two main therapies phototherapy (PT) and photodynamic therapy (PDT) use light sources to bring some therapeutic effects into action. Starting with phototherapy, it uses short wavelengths, in the ultraviolet B spectrum (UVB, usually 311 nm), to produce sub-cellular effects such as the maturation and migration of cells, and the lengthening of the turnover process, such as in keratinocytes. When paired with psoralens, the light source produces ultraviolet A rays, in a procedure called PUVA. It has been used effectively in those skin disorders where the immune system or the keratinocytes do not undergo the usual physiological processes (i.e., psoriasis, parapsoriasis, atopic dermatitis). On the other hand, photodynamic therapy acts as an immune booster and inflammatory stimulus. The main protagonists of this process are unstable substances called photosensitizers. The photosensitizers thus far produced have been subdivided by generation time, spanning from the first dyes such as phthalocyanine through the second generation including the omnipresent aminolevulinic acid to the latest third generation which combines heme-like substances with lipid receptors or monoclonal antibodies to carry the photosensitizer on the desired target [6]. Once the light-sensitive substance reaches its goal, a light source in the infrared spectrum (about 630 nm in wavelength in most cases) indirectly produces the formation of reactive oxygen species (ROS), allowing the killing of the infected/rogue cells and the stimulation of a controlled and self-limiting inflammatory process. The latter therapy has been developed, mostly, for those diseases where cell replication is higher and the self-healing mechanisms of the diseased cells are lacking, such as infective diseases and cancers.
Both these topics of interest have proven to be useful tools on several occasions for a better understanding of the base mechanisms that regulate the human organism and have shown to be promising therapies for the present and the future, but many links are still missing and leave us with questions. In fact, light-based therapy seems to be affecting cells not just with the brute force of damaging or ablating tissues but also by having a crucial role on a genetic and epigenetic scale, since both these aspects of the human and non-human physiology have proven to be dynamic rather than a still picture.
2. Involvement of microRNAs as a Response to Phototherapy and Photodynamic Therapy
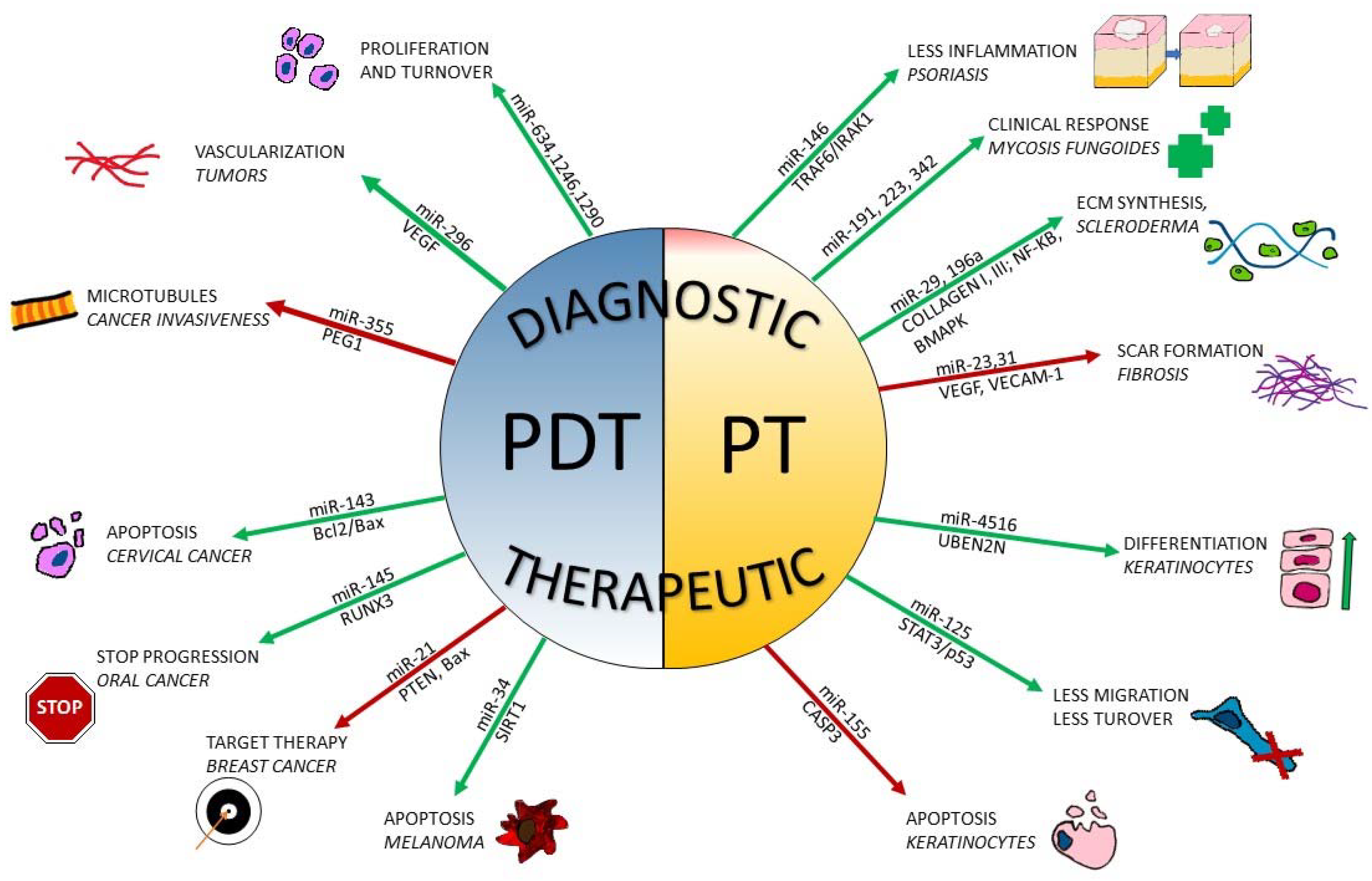
Figure 1. Effects of photodynamic therapy/phototherapy on miRNA expression in skin conditions. Green arrows represent upregulation of circulating/local levels of miRNAs; red arrows represent downregulated levels of miRNAs. On the upper part of the figure, miRNAs are exploited as a diagnostic tool; on the lower part, miRNAs provide therapeutic targets or produce healing effects when down- or upregulated.
3. Conclusions
Since their first applications, light-based therapies have helped several skin conditions, both related and unrelated to malignancy. Being both secure and scarcely invasive, these treatments have proven to have generally scarce side effects, but the current knowledge on their mechanism of action is lacking. To better understand the molecular pathways involved in the healing process, miRNAs have proven to be a helpful tool both as a diagnostic marker and as a possible target therapy. Either by targeting miRNAs or using mimics/inhibitors, the effects of light-based therapy can be enhanced or predict treatment efficacy. Current studies are not enough to focus on just one treatment, but the premiere results are promising. According to the results provided here, certain miRNAs appear to be more frequently associated than others in chronic skin conditions, being either up- or downregulated, and it can be suggested that further clinical trials might focus on targeting or exploiting these molecules.
References
- Esquela-Kerscher, A.; Slack, F.J. Oncomirs–microRNAs with a role in cancer. Nat. Rev. Cancer 2006, 6, 259–269.
- Mannucci, C.; Casciaro, M.; Minciullo, P.L.; Calapai, G.; Navarra, M.; Gangemi, S. Involvement of microRNAs in skin disorders: A literature review. Allergy Asthma Proc. 2017, 38, 9–15.
- Bertino, L.; Guarneri, F.; Cannavò, S.P.; Casciaro, M.; Pioggia, G.; Gangemi, S. Oxidative Stress and Atopic Dermatitis. Antioxidants 2020, 9, 196.
- Cannavò, S.P.; Riso, G.; Casciaro, M.; Di Salvo, E.; Gangemi, S. Oxidative stress involvement in psoriasis: A systematic review. Free. Radic Res. 2019, 53, 829–840.
- Vaccaro, M.; Bagnato, G.; Cristani, M.; Borgia, F.; Spatari, G.; Tigano, V.; Saja, A.; Guarneri, F.; Cannavò, S.P.; Gangemi, S. Oxidation products are increased in patients affected by non-segmental generalized vitiligo. Arch. Dermatol. Res. 2017, 309, 485–490.
- Kwiatkowski, S.; Knap, B.; Przystupski, D.; Saczko, J.; Kędzierska, E.; Knap-Czop, K.; Kotlińska, J.; Michel, O.; Kotowski, K.; Kulbacka, J. Photodynamic therapy–mechanisms, photosensitizers and combinations. Biomed. Pharmacother. 2018, 106, 1098–1107.
- Jiang, L.; Lv, X.; Li, J.; Li, J.; Li, X.; Li, W.; Li, Y. The status of microRNA-21 expression and its clinical significance in human cutaneous malignant melanoma. Acta Histochem. 2012, 114, 582–588.
- Pace, E.; Di Vincenzo, S.; Di Salvo, E.; Genovese, S.; Dino, P.; Sangiorgi, C.; Ferraro, M.; Gangemi, S. MiR-21 upregulation increases IL-8 expression and tumorigenesis program in airway epithelial cells exposed to cigarette smoke. J. Cell Physiol. 2019, 234, 22183–22194.
- Gu, X.; Nylander, E.; Coates, P.J.; Nylander, K. Effect of narrow-band ultraviolet B phototherapy on p63 and microRNA (miR-21 and miR-125b) expression in psoriatic epidermis. Acta Dermatol. Venereol. 2011, 91, 392–397.
- Aguennouz, M.; Guarneri, F.; Oteri, R.; Polito, F.; Giuffrida, R.; Cannavò, S.P. Serum levels of miRNA-21-5p in vitiligo patients and effects of miRNA-21-5p on SOX5, beta-catenin, CDK2 and MITF protein expression in normal human melanocytes. J. Dermatol. Sci. 2021, 101, 22–29.
- Hu, Z.; Fan, H.; Lv, G.; Zhou, Q.; Yang, B.; Zheng, J.; Cao, W. 5-Aminolevulinic acid-mediated sonodynamic therapy induces anti-tumor effects in malignant melanoma via p53-miR-34a-Sirt1 axis. J. Dermatol. Sci. 2015, 79, 155–162.
- Neagu, M.; Constantin, C.; Cretoiu, S.M.; Zurac, S. miRNAs in the Diagnosis and Prognosis of Skin Cancer. Front. Cell Dev. Biol. 2020, 8, 71.
- Eissa, M.G.; Artlett, C.M. The MicroRNA miR-155 Is Essential in Fibrosis. Noncoding RNA 2019, 5, 23.
- Kurowska-Stolarska, M.; Alivernini, S.; Ballantine, L.E.; Asquith, D.L.; Millar, N.L.; Gilchrist, D.S.; Reilly, J.; Ierna, M.; Fraser, A.R.; Stolarski, B.; et al. MicroRNA-155 as a proinflammatory regulator in clinical and experimental arthritis. Proc. Natl. Acad. Sci. USA 2011, 108, 11193–11198.
- Khori, V.; Alizadeh, A.M.; Gheisary, Z.; Farsinejad, S.; Najafi, F.; Khalighfard, S.; Ghafari, F.; Hadji, M.; Khodayari, H. The effects of low-level laser irradiation on breast tumor in mice and the expression of Let-7a, miR-155, miR-21, miR125, and miR376b. Lasers Med. Sci. 2016, 31, 1775–1782.
- Cao, Y.; Li, S.; Chen, C.; Wang, D.; Wu, T.; Dong, H.; Zhang, X. Rattle-type [email protected]2-xS hollow mesoporous nanocrystals with enhanced photothermal efficiency for intracellular oncogenic microRNA detection and chemo-photothermal therapy. Biomaterials 2018, 158, 23–33.
- Moon, S.; Kim, D.K.; Kim, J. Apoptosis-related microRNA-145-5p enhances the effects of pheophorbide a-based photodynamic therapy in oral cancer. Oncotarget 2017, 8, 35184–35192.
- Fang, C.Y.; Chen, P.Y.; Ho, D.C.; Tsai, L.L.; Hsieh, P.L.; Lu, M.Y.; Yu, C.C.; Yu, C.H. miR-145 mediates the anti-cancer stemness effect of photodynamic therapy with 5-aminolevulinic acid (ALA) in oral cancer cells. J. Formos. Med. Assoc. 2018, 117, 738–742.
- Fan, B.; Yang, X.; Li, X.; Lv, S.; Zhang, H.; Sun, J.; Li, L.; Wang, L.; Qu, B.; Peng, X.; et al. Photoacoustic-imaging-guided therapy of functionalized melanin nanoparticles: Combination of photothermal ablation and gene therapy against laryngeal squamous cell carcinoma. Nanoscale 2019, 11, 6285–6296.
- Tian, K.; Liu, W.; Zhang, J.; Fan, X.; Liu, J.; Zhao, N.; Yao, C.; Miao, G. MicroRNA-125b exerts antitumor functions in cutaneous squamous cell carcinoma by targeting the STAT3 pathway. Cell. Mol. Biol. Lett. 2020, 25, 12.
- Ghaderi, R.; Haghighi, F. Immunohistochemistry assessment of p53 protein in Basal cell carcinoma. Iran. J. Allergy Asthma Immunol. 2005, 4, 167–171.





