
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Mara Lúcia Gonçalves Diogo | + 1215 word(s) | 1215 | 2021-10-27 06:02:56 | | | |
| 2 | Jason Zhu | -1 word(s) | 1214 | 2021-11-01 03:09:49 | | | | |
| 3 | Peter Tang | Meta information modification | 1214 | 2021-11-11 02:19:09 | | |
Video Upload Options
Acne is a dermatosis that affects almost 90% of the adolescent population worldwide and its treatment is performed with retinoids, antimicrobials, acids, and topical or systemic antibiotics. Side effects such as skin irritation in addition to microbial resistance to antibiotics are the main side effects found. Phototherapy with blue light is being used as an alternative treatment.
1. Introduction
The Simple Grading of Acne [1], published by the Global Alliance to Improve Outcomes in Acne (2003), classifies lesions as Grade I, or non-inflammatory, in which they have only closed and open comedones; Grade II, which, in addition to many comedones, there are also papules and pustules, causing inflammatory lesions; Grade III, which presents a mixture of papules, pustules, comedones, nodules and cysts; Grade IV, which in addition to all previous factors, also presents fistulas and abscesses, affecting its severity with lesions that evolve to scar processes.
The IGA (Investigator Global Assessment) scale, recommended by the FDA (Federal Drug Administration), 2005 [1], follows the diagnostic criteria: Grade 0—Clean skin, without inflammatory and non-inflammatory lesions; Grade 1—Almost clean skin, with few non-inflammatory lesions and no more than one inflammatory lesion; Grade 2—Mild severity, higher than grade 1, with some non-inflammatory lesions and few inflammatory lesions (papules and pustules without nodular lesions); Grade 3—Moderate severity, many non-inflammatory lesions, some inflammatory lesions and no more than a small nodular lesion; Grade 4—Severe, higher than grade 3, many non-inflammatory and inflammatory lesions, some nodular lesions. The FDA does not recommend the use of Grade 5, as other authors indicate in the literature [2].
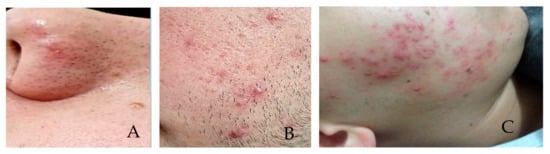
Grade I, comedones, without inflammatory lesions ( Figure 1 A); Grade II, comedones, papules, and pustules with varying intensity and few to numerous inflammatory lesions with some erythema ( Figure 1 B); Grade III, comedones, papules, and pustules with an intense inflammatory reaction that leads to the formation of nodules, which may contain pus (cysts) ( Figure 1 C); Grade IV, comedones, papules, pustules and fistulas, larger cysts forming large lesions [3].
Domestic therapy with blue light was evaluated using a device with a wavelength of 414 nm and after 3 weeks there was a significant decrease in the inflammatory lesion and erythema [4]. The skin presented a smoother texture and increased tone [5]. Some authors state that inflammatory lesions respond better to blue light phototherapy than non-inflammatory lesions [6].
2. Method of Research
The bibliographic search followed the development of the SR protocol (Systematic Review) of the literature and will follow the Preferred Reporting items for Systematic Reviews and MetaAnalyses (PRISMA) guidelines ( Figure 2 ) which provides a checklist for transparency in the selection process of articles.
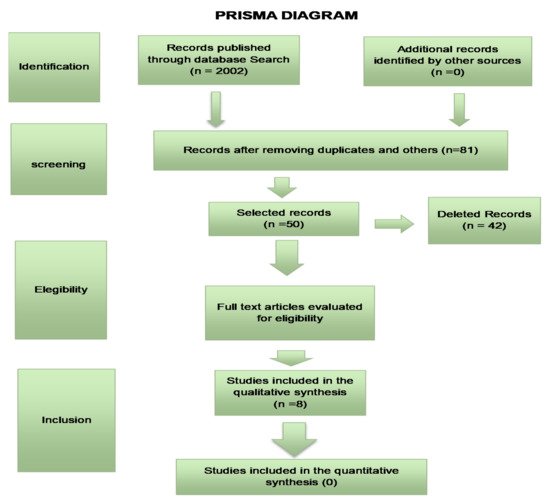
The research question (Patient, Intervention, Comparison and Outcomes/Outcome (PICO), in the Table 1 , was as follows: What is the clinical evidence for the action of blue light in improving acne concerning conventional treatments?
| Patient | With Inflammatory Acne |
|---|---|
| Intervention | Photobiomodulation with blue light |
| Comparison | Medicines/other therapies |
| Outcomes | Reduction of lesions |
The searches were carried out at PubMed (8–10 April 2021), Cochrane (13–15 April 2021), and Scopus (19–21 April 2021) databases, and the following terms and combinations were used: (Acne) and (photobiomodulation) or (LLLT) Low Level Light Therapy or (Phototherapy) or (LED) Light Emitting Diode and (blue light). After the search, the titles and abstracts of the articles were independently selected by two reviewers, and in the case of disagreement, a third evaluator determined the inclusion or not.
3. Current Studies
Cheema et al. [7], compared 124 patients with mild to moderate acne in a controlled and randomized study, divided into 2 groups, one treated with blue light, wavelength between 407 and 420 nm, and the size of the spot opening of the device of 55 mm, and the other with BPO at 4%. The evaluation was made by counting lesions and the evaluation of the severity of acne determined by the number of lesions: Acne was classified as mild acne: less than 20 comedones, less than 15 inflammatory lesions, or total count of lesions less than 30; Moderate acne: between 20 and 100 comedones, 15 to 50 inflammatory lesions or total count of lesions from 30 to 125. Patients in the blue group received treatment for 15 min in each session, twice a week, for 6 weeks, and patients in the BPO group used the product every night for 6 weeks. There was a greater reduction in lesions in the blue light group compared to the BPO treated group (76% × 60%). Another finding in this study was the reduced adverse effects in the blue light group when compared to BPO.
In the complete face study, with open evaluation, 13 patients were treated with light for 15 min, twice a week, for 4 weeks. There was a reduction of 81% of inflammatory lesions. In the split-face, double-blind, self-controlled study, one side of the face was chosen to be treated for 15 min, twice a week, for 4 weeks. 23 patients were treated and evaluated by a blind doctor. There was a 20% reduction in inflammatory lesions and an average of 60% reduction of lesions. The untreated side had an average reduction of 30% in inflammatory lesions.
Kwon et al. [8], conducted a study with 24 patients evaluating inflammatory acne, through injury count and sebum measurement, comparing blue light (450 nm) associated with 1450 nm laser diode and blue light alone on hemifaces during 3 sessions with an interval of 4 weeks. The blue light was applied for 3 min with an irradiance of 3.5 to 7 mW/cm 2 and a dose of 0.6 to 1.2 J/cm 2. There was an improvement of 62.3% and 35.2% for the combination of blue light and diode laser and blue light, respectively, in the inflammatory lesions of acne. However, the improvement of seborrhea was verified with the combined laser diode lights (1450 nm) associated with blue light.
In the study by Papageorgiou et al. [9], a comparison was made of the blue light (415 nm), blue and red combined, white light, and benzoyl peroxide in cream, with 107 patients divided into these 4 groups. The device was applied for 15 min daily for 12 weeks at a distance of 25 cm, with a dose of 320 J/cm 2 and 4.23 mW/cm 2 of irradiance. Although the results favored the combined group of blue and red light with a small advantage, there was an improvement in inflammatory lesions with the blue light of 63% and in the commedones of 45%.
4. Discussion on Blue Light
To answer the question “What is the clinical evidence for the action of blue light in improving acne condition when compared to conventional treatments?” from the PICO research conducted in the systematic review, researchers found a number of scientific articles that proved the efficacy of treatments with LED and blue light devices in the effective improvement of acne and with minor or non-existent adverse effects compared to conventional treatments such as BPO.
In the study by Papargeorgiou et al. [9], the red light associated with blue light had a better result in the improvement of acne lesions at first (76%), which did not occur at the end of treatment. Even so, blue light alone was also quite effective at the end of treatment, with an average improvement of 54% in acne lesions (45% in comedones and 63% in inflammatory lesions).
This result corroborates most studies that assess the effect of blue light on acne treatment and demonstrate that irradiation of Cutibacterium acnes colonies with visible blue light led to photoexcitation of bacterial porphyrins, singlet oxygen production and eventually bacterial destruction, indicating that acne can be successfully treated with blue visible light phototherapy.
References
- Thiboutot, D.; Gollnick, H.; Bettoli, V.; Dréno, B.; Kang, S.; Leyden, J.J.; Shalita, A.R.; Lozada, V.T.; Berson, D.; Finlay, A.Y.; et al. New insights into the management of acne: An update from the Global Alliance to Improve Outcomes in Acne Group. J. Am. Acad. Dermatol. 2009, 60, S1–S50.
- Doshi, A.; Zaheer, A.; Stiller, M.J. A comparison of current acne grading systems and proposal of a novel system. Int. J. Dermatol. 1997, 36, 416–418.
- Fox, L.; Csongradi, C.; Aucamp, M.; Du Plessis, J.; Gerber, M. Treatment Modalities for Acne. Molecules 2016, 21, 1063.
- De Arruda, L.H.F.; Kodani, V.; Filho, A.B.; Mazzaro, C.B. Estudo clínico, prospectivo, aberto, randomizado e comparativo para avaliar a segurança e a eficácia da luz azul versus peróxido de benzoíla 5% no tratamento da acne inflamatória graus II e III. An. Bras. Dermatol. 2009, 84, 463–468.
- Gold, M.H.; Sensing, W.; Biron, J.A. Clinical efficacy of home-use blue-light therapy for mild-to moderate acne. J. Cosmet. Laser Ther. 2011, 13, 308–314.
- Kwon, H.; Lee, J.; Yoon, J.; Park, S.; Ryu, H.; Park, B.; Kim, Y.; Suh, D. The clinical and histological effect of home-use, combination blue-red LED phototherapy for mild-to-moderate acne vulgaris in Korean patients: A double-blind, randomized controlled trial. Br. J. Dermatol. 2012, 168, 1088–1094.
- Cheema, A.N.; Ameen, U.; Javaid, R.; Bokhari, M.A. Efficacy and safety of blue light versus 4% topical benzoyl peroxide in mild to moderate acne. J. Pak. Assoc. Dermatol. 2018, 28, 79–84.
- Kwon, H.H.; Choi, S.C.; Jung, J.Y.; Bae, Y.; Park, G.-H. A Novel Combined Light-Based Treatment of Acne Vulgaris with 1450-nm Diode Laser and 450-nm Blue Light. Dermatol. Surg. 2019, 45, 1147–1154.
- Papageorgiou, P.; Katsambas, A.; Chu, A. Phototherapy with blue (415 nm) and red (660 nm) light in the treatment of acne vulgaris. Br. J. Dermatol. 2000, 142, 973–978.





