
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Harriet Rumgay | + 1929 word(s) | 1929 | 2021-09-13 05:48:20 |
Video Upload Options
Approximately 4% of cases of cancer worldwide are caused by alcohol consumption. Drinking alcohol increases the risk of several cancer types, including cancers of the upper aerodigestive tract, liver, colorectum, and breast.
1. Introduction
Approximately 4% of cancer cases worldwide are caused by alcohol consumption, equating to more than 740,000 cases of cancer globally in 2020 [1]. The impact of alcohol consumption on cancer burden differs by cancer type, and cancers of the oesophagus, liver, and breast represent the most alcohol-attributable cases of cancer globally ( Figure 1 ). Drinking alcohol even at lower levels of intake can increase the risk of cancer and we previously estimated that over 100,000 cases of cancer in 2020 were caused by light and moderate drinking of the equivalent of around one or two alcoholic drinks per day [1]. Despite this, there is low public awareness of the causal link between alcohol and cancer and alcohol use is growing in several regions of the world [2][3].
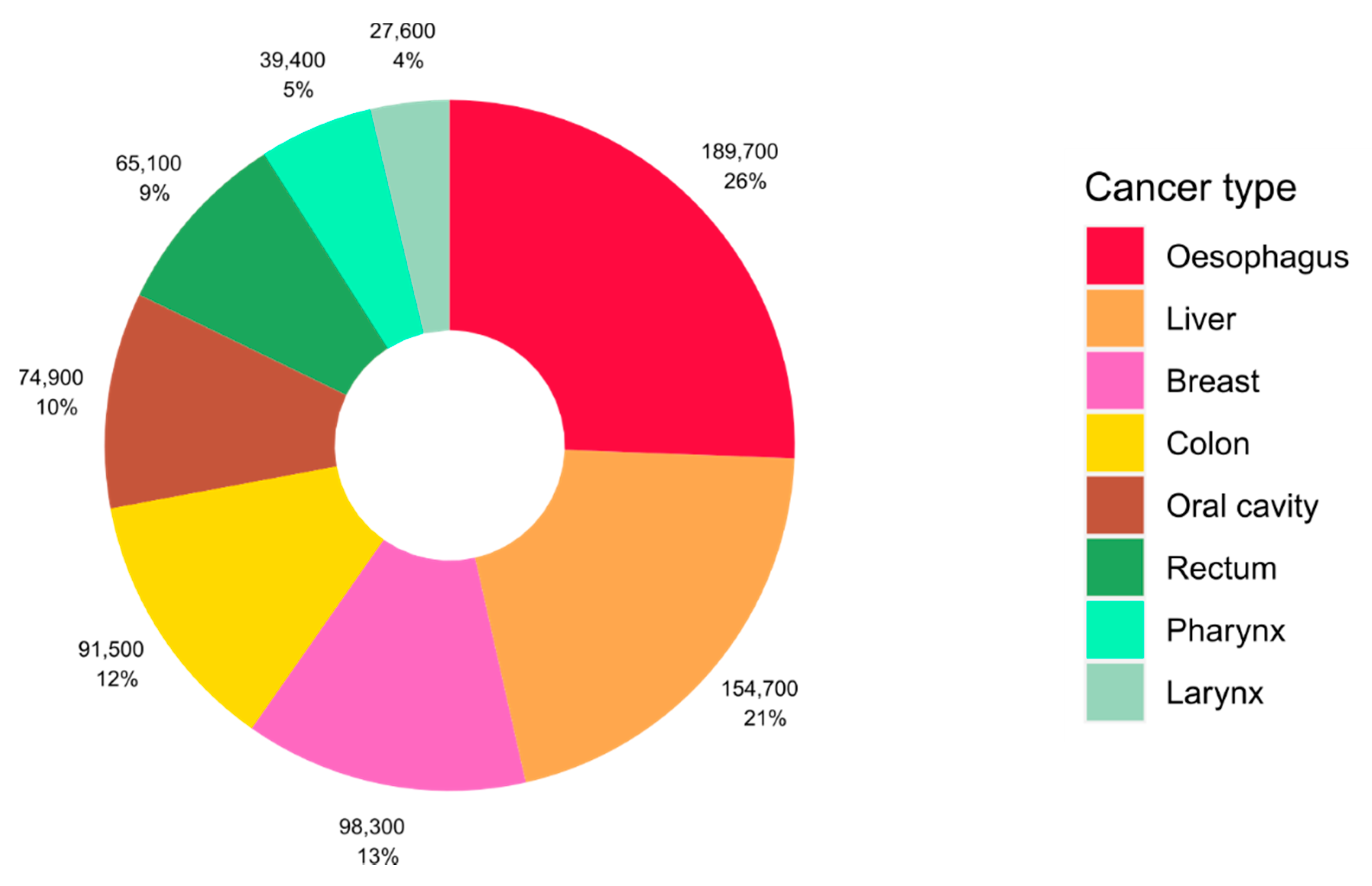
Figure 1. Global number and proportion of cancer cases attributable to alcohol consumption according to cancer type. Source of alcohol-attributable cases: Rumgay and colleagues [1].
More than 30 years ago, in 1988, the International Agency for Research on Cancer (IARC) classified alcoholic beverages as a group 1 carcinogen, the most severe classification [4]. The IARC Monographs program aims to classify cancerous agents according to the strength of the available epidemiological and experimental evidence. Cancers of the oral cavity, pharynx, larynx, oesophagus, and liver were first classified as being causally related to the consumption of alcoholic beverages, and this was expanded to include cancers of the colorectum and female breast in the later monographs on alcoholic beverages in 2010 and 2012, with a positive association observed for cancer of the pancreas [5][6].
The World Cancer Research Fund (WCRF) also conducts classification of physical and dietary components and their potential cancerous effects as part of their Continuous Update Project. The WCRF base their conclusions on the quality of epidemiological evidence and carry out meta-analyses of the association with cancer risk. In the most recent report on Diet, Nutrition, Physical Activity and Cancer, WCRF concluded that there was strong evidence that alcohol consumption increased the risk of cancers of the mouth, pharynx and larynx, oesophagus (squamous cell carcinoma), liver, colorectum, and breast (postmenopausal), with a probable increased risk of stomach cancer and premenopausal breast cancer [7].
2. Alcohol and Cancer Risk
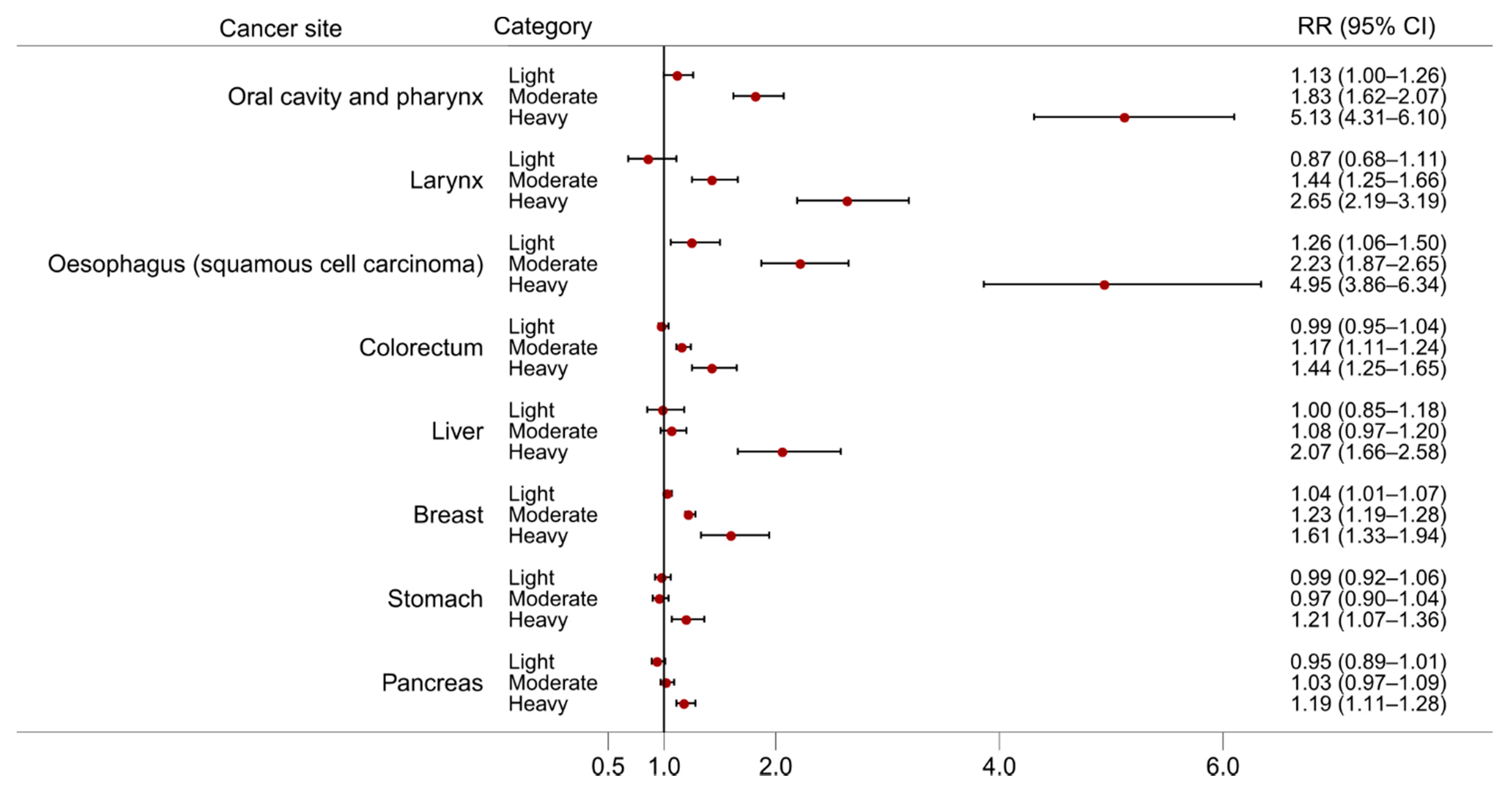
The effects of alcohol consumption on cancer risk have been studied for many decades and an association with alcohol has been observed for multiple cancer sites. Here, we discuss evidence from large meta-analyses of observational studies and emerging evidence from Mendelian randomisation studies. Figure 2 and Figure 3 present the dose-response relationships for the risk of cancer at several sites per 10 g/day increase in alcohol consumption from the meta-analyses carried out in the WCRF Continuous Update Project [7], and the risk of cancer at several sites according to three levels of alcohol intake [light (up to 12.5 g/day), moderate (12.5 to 50 g/day), and heavy (more than 50 g/day)] from a meta-analysis conducted by Bagnardi and colleagues [8], both with respect to the reference category of alcohol non-drinkers.
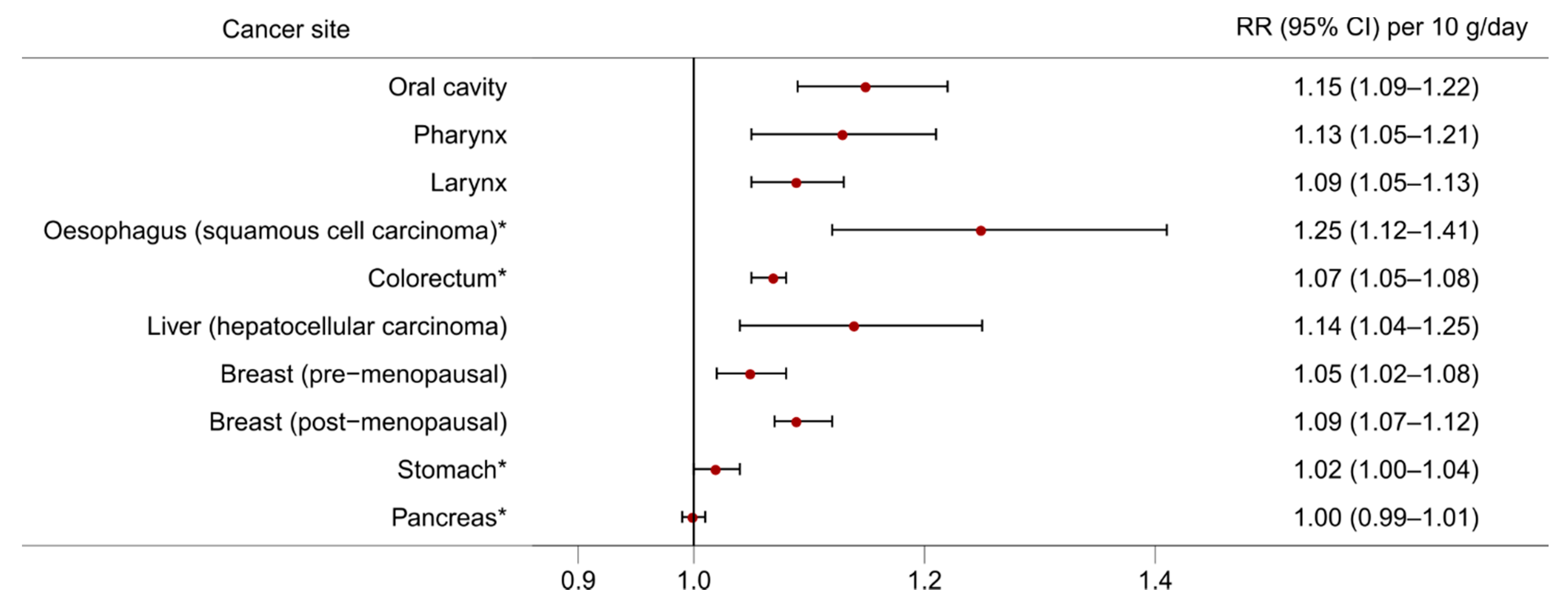
Figure 2. The dose-response relationship for the risk of cancer at different sites per 10 g/day increase in alcohol consumption. Source of relative risk estimates: WCRF Continuous Update Project [7]. RR = Relative risk; CI = Confidence interval. * Non-linear dose-response observed indicating threshold effect.
2.1. Oral Cavity, Pharyngeal, and Laryngeal Cancers
2.2. Oesophageal Cancer
2.3. Colorectal Cancer
2.4. Liver Cancer
2.5. Breast Cancer
2.6. Stomach Cancer
2.7. Pancreatic Cancer
2.8. Other Cancer Types
3. Conclusions
Alcohol and its metabolite acetaldehyde can drive cancer development through several pathways. Many of these pathways are interlinked and show the complexity and breadth of alcohol’s harmful potential. For example, inflammation can result in oxidative stress, but inflammation is a reaction by the immune system which is itself compromised by alcohol use. Furthermore, DNA damage can occur through exposure to acetaldehyde and reactive oxygen species which are both produced through cytochrome P-450 2E1 activity, with acetaldehyde also a product of alcohol dehydrogenase activity.
Alcohol consumption is a well-established risk factor for cancer and has been linked to cancers of the oral cavity and pharynx, oesophagus, liver, colorectum and breast. While studies have provided evidence on alcohol’s carcinogenic potential, further understanding of alcohol’s pathways to cancer development will inform the direction of future research.
References
- Rumgay, H.; Shield, K.; Charvat, H.; Ferrari, P.; Sornpaisarn, B.; Obot, I.; Islami, F.; Lemmens, V.E.P.P.; Rehm, J.; Soerjomataram, I. Global burden of cancer in 2020 attributable to alcohol consumption: A population-based study. Lancet Oncol. 2021, 22, 1071–1080.
- Buykx, P.; Li, J.; Gavens, L.; Hooper, L.; Lovatt, M.; Gomes de Matos, E.; Meier, P.; Holmes, J. Public awareness of the link between alcohol and cancer in England in 2015: A population-based survey. BMC Public Health 2016, 16, 1194.
- Manthey, J.; Shield, K.D.; Rylett, M.; Hasan, O.S.M.; Probst, C.; Rehm, J. Global alcohol exposure between 1990 and 2017 and forecasts until 2030: A modelling study. Lancet 2019, 393, 2493–2502.
- International Agency for Research on Cancer. IARC Monographs on the Evaluation of Carcinogenic Risks to Humans. Volume 44. Alcohol Drinking; 1988; Volume 44, Available online: https://publications.iarc.fr/Book-And-Report-Series/Iarc-Monographs-On-The-Identification-Of-Carcinogenic-Hazards-To-Humans/Alcohol-Drinking-1988 (accessed on 20 June 2021).
- International Agency for Research on Cancer. IARC Monographs on the Evaluation of Carcinogenic Risks to Humans. Volume 96. Alcohol Consumption and Ethyl Carbamate; 2010; Volume 96, Available online: https://publications.iarc.fr/Book-And-Report-Series/Iarc-Monographs-On-The-Identification-Of-Carcinogenic-Hazards-To-Humans/Alcohol-Consumption-And-Ethyl-Carbamate-2010 (accessed on 20 June 2021).
- International Agency for Research on Cancer. IARC Monographs on the Evaluation of Carcinogenic Risks to Humans. Volume 100E. Personal Habits and Indoor Combustions; 2012; Available online: https://publications.iarc.fr/Book-And-Report-Series/Iarc-Monographs-On-The-Identification-Of-Carcinogenic-Hazards-To-Humans/Personal-Habits-And-Indoor-Combustions-2012 (accessed on 20 June 2021).
- World Cancer Research Fund/American Institute for Cancer Research. Diet, Nutrition, Physical Activity and Cancer: A Global Perspective; Continuous Update Project Expert Report; 2018; Available online: https://www.wcrf.org/wp-content/uploads/2021/02/Summary-of-Third-Expert-Report-2018.pdf (accessed on 20 June 2021).
- Bagnardi, V.; Rota, M.; Botteri, E.; Tramacere, I.; Islami, F.; Fedirko, V.; Scotti, L.; Jenab, M.; Turati, F.; Pasquali, E.; et al. Alcohol consumption and site-specific cancer risk: A comprehensive dose–response meta-analysis. Br. J. Cancer 2014, 112, 580.
- Arnold, M.; Ferlay, J.; van Berge Henegouwen, M.I.; Soerjomataram, I. Global burden of oesophageal and gastric cancer by histology and subsite in 2018. Gut 2020, 69, 1564–1571.
- Chang, J.S.; Hsiao, J.-R.; Chen, C.-H. ALDH2 polymorphism and alcohol-related cancers in Asians: A public health perspective. J. Biomed. Sci. 2017, 24, 19.
- Ben, Q.; Wang, L.; Liu, J.; Qian, A.; Wang, Q.; Yuan, Y. Alcohol drinking and the risk of colorectal adenoma: A dose–response meta-analysis. Eur. J. Cancer Prev. 2015, 24, 286–295.
- Ferlay, J.; Ervik, M.; Lam, F.; Colombet, M.; Mery, L.; Piñeros, M.; Znaor, A.; Soerjomataram, I. Global Cancer Observatory: Cancer Today. Available online: https://gco.iarc.fr/today (accessed on 15 December 2020).
- Sun, Q.; Xie, W.; Wang, Y.; Chong, F.; Song, M.; Li, T.; Xu, L.; Song, C. Alcohol Consumption by Beverage Type and Risk of Breast Cancer: A Dose-Response Meta-Analysis of Prospective Cohort Studies. Alcohol Alcohol. 2020, 55, 246–253.





