Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Andrea López Botella | + 3425 word(s) | 3425 | 2021-09-24 07:41:25 | | | |
| 2 | Lindsay Dong | Meta information modification | 3425 | 2021-10-26 05:27:01 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Botella, A. Heavy Metals on Male Fertility. Encyclopedia. Available online: https://encyclopedia.pub/entry/15350 (accessed on 28 May 2026).
Botella A. Heavy Metals on Male Fertility. Encyclopedia. Available at: https://encyclopedia.pub/entry/15350. Accessed May 28, 2026.
Botella, Andrea. "Heavy Metals on Male Fertility" Encyclopedia, https://encyclopedia.pub/entry/15350 (accessed May 28, 2026).
Botella, A. (2021, October 25). Heavy Metals on Male Fertility. In Encyclopedia. https://encyclopedia.pub/entry/15350
Botella, Andrea. "Heavy Metals on Male Fertility." Encyclopedia. Web. 25 October, 2021.
Copy Citation
Heavy metals are endocrine disruptors which interfere with processes mediated by endogenous hormones of the organism, negatively affecting endocrine functions. Some studies have correlated heavy metal exposure with male infertility. However, the number of studies conducted on humans are limited.
endocrine disrupting compounds
environmental exposure
heavy metals
human sperm
male fertility
occupational exposure
1. Introduction
The definition of infertility was established by the American Society for Reproductive Medicine and it is defined as the failure to get pregnant after one year or more of regular sexual intercourse without the use of contraceptives. It can be due to an impairment of the capacity of reproduction, individually or with the partner. Globally, 15% of worldwide couples suffer infertility, which is equivalent to 48.5 million couples. Specifically, male partners are responsible for 20–30% of the overall infertility cases [1]. Further to that, those values change depending on the geographical region. The increased prevalence of infertility could be due to social factors, changes in seminal quality due to lifestyle habits (alcohol and tobacco consumption) and changes in sexual behavior [2]. The decline of male fertility is a worldwide matter of concern since available studies suggest a lower semen quality over the years. Worldwide data revealed a decrease in sperm concentration (−0.64 million/mL per year) from 1973 to 2011 [3]. Recent retrospective evidence and basic studies have shown relationships between the decrease in sperm quality and a poor diet, increased obesity rates and exposure to environmental toxins [4].
To address male infertility, a compilation of the patient’s sexual history, a complete physical examination, a serological test and a semen analysis are needed [5]. To evaluate male fertility and its management, the basic semen analysis has been considered fundamental. However, despite sperm analysis being routinely used, it cannot help to discriminate between infertile and fertile men. Thus, it is only useful to classify men as subfertile [6]. Due to the intra-individual variability, the World Health Organization [7] recommendation is the performance of two or three seminograms to obtain detailed information on the patient’s seminal parameters. Furthermore, the etiological factors affecting male infertility are varied, including environmental [8] and genetic factors, endocrine and immunological disorders, and obstructive lesions and infections in the male reproductive tract [9].
Conventional semen parameters are not useful, since 30–40% of the cases suffer unexplained or idiopathic male infertility [10]. Therefore, the routine sperm analysis assessment itself is not sufficient to test the fertilizing ability of spermatozoa. As a consequence, the development of new functional tests providing newer biomarkers of the sperm fertilizing capacity are needed [11]. Indeed, the physiology and functionality assessment of sperm should include studies on molecular biomarkers, such as the acrosome reaction, reactive oxygen species (ROS), DNA damage and chromatin structure [12]. DNA fragmentation plays an important role in subfertile patients [13]. This fact is a major matter of concern as DNA integrity is important for a proper embryo development [14] and it could be implicated in in vitro fertilization processes, as in the intracytoplasmic sperm injection, for instance [13]. The main culprits for DNA damage are an abortive apoptosis, problems during the protamine substitution in the spermatogenesis process and ROS production [13]. In this context, oxidative stress is considered an important cause of male infertility. Approximately 40% of patients show evidence of redox attack, thus exhibiting high levels of lipid peroxidation and oxidative DNA damage. In addition, it has been observed that a certain region in chromosome 15 may be especially vulnerable to oxidative attack and its genetic location is associated with male infertility [15].
Up-to-date literature links environmental contaminants and human reproductive health worries [16]. Male reproductive function is vulnerable to different environmental and occupational factors, of which only a few have been well identified. Different compounds are considered to be the main culprits for male fertility reduction, such as pesticides, dioxins, solvents and heavy metals. [17]. At this point, it is important to emphasize that environmental quality has recently decreased mainly due to anthropic activities that increase the level of environmental pollutants. Some of these pollutants can act as certain endogenous hormones and are therefore a cause for concern. They are the so-called endocrine disrupting compounds (EDCs) and are considered exogenous substances that are involved in the processes regulated by endogenous hormones of the organism, thus disrupting endocrine functions [18]. This group includes different substances, such as dioxins, bisphenol A and heavy metals. Although there is no authoritative definition for the term heavy metals [19], this group of elements has been considered as “naturally occurring metals having atomic number (Z) greater than 20 and an elemental density greater than 5 g cm−3” [20]. Therefore, a total of 51 different elements can be included in the category of “heavy metals”. In most cases, contaminated food is the main source of exposure to these species [21].
Since the human body has no biochemical pathways to detoxify them, heavy metal exposition leads to an accumulation in the body. For that, in the last century, the risks to health and development derived from the exposure to heavy metals have become a matter of interest. In particular, the aforementioned chemical species can affect male fertility by lowering the seminal quality, thereby causing infertility [22]. For example, copper (Cu) and chromium (Cr) were found in the semen samples of a father and his son from the “Land of Fires”, in Italy. This region is a highly environmentally polluted area, exposed to diverse chemicals and heavy metals [23]. Not only that, but the results obtained from this research showed alterations in the content of sperm nuclear basic proteins (SNBP) and a low DNA binding affinity. In addition, the son’s proteins showed unstable DNA binding, thus able to produce DNA damage [23]. Such evidence highlights the transgenerational inherited consequences of environmental-pollution exposition on molecular alterations in the sperm cell. Furthermore, men from highly contaminated regions showed higher zinc (Zn), Cr and Cu and lower iron (Fe) concentrations in semen, lower sperm motility and higher DNA damage than those that had not been exposed to environmental pollutants [24].
2. Heavy Metals on Human Male Fertility
2.1. Heavy Metals Effects in the Reproductive Processes
Heavy metal exposure has been identified as an influential factor on male sperm production and fertility [25][26][27]. However, the mechanisms that alter the reproductive processes are complex. The toxicant effects can be directly produced by the action on the reproductive organs, or, indirectly, by impairing the hormonal regulation [28]. Moreover, different biological matrices are used to evaluate male reproductive risks. The biological matrices usually analyzed are blood, serum, semen, seminal plasma, urine, or hair. Heavy metals are found at higher concentrations in blood or urine [17].
There is some controversy about the impact of heavy metal exposure on biological matrices. Thus, semen had been considered a less informative marker of occupational exposure. Furthermore, it is recognized that the heavy metals determination in spermatozoa cells is not a more enlightening marker of the occupational (or non-occupational) exposure than the biological and traditional monitoring by urine and blood. In contrast, for some specific research and clinical purposes, the study of spermatic cells and semen could be appropriate [17]. Following this idea, a recent study from the EcoFoodFertility initiative concluded that semen could be considered an early biomarker of environmental exposure to Zn, Cr and Cu, since higher concentrations of these elements had been demonstrated in men residing in areas with high environmental impact [24]. In particular, the sperm DNA fragmentation assessment has been recently proposed as a marker of air pollution [29]. Regarding environmental pollution, a retrospective observational study in China carried out during the COVID-19 outbreak showed higher susceptibility to poorer sperm motility [30]. Due to that, air pollution and COVID-19 may be currently considered hazardous to male fertility. Interestingly, according to a recent study performed in China, a higher percentage of apoptotic cells in the testis was present in COVID-19-infected patients and a decreased sperm concentration (39.1% of COVID-19 patients) was found in semen [31]. Those findings highlight that, in air polluted countries such as China, COVID-19 may exacerbate the effects of environmental contaminants, leading to impaired male fertility.
Most EDCs have intrinsic estrogenic or androgenic activity, being the gonads the targets of most of these compounds [32]. Different endpoints are used to study the masculine reproductive function, and the seminal quality and the endocrine and cellular secretion function have been the most frequently used [33]. Among others, Cd, arsenic (As) and Pb were recently identified as major toxicants affecting the reproduction function. The toxicity mechanisms include oxidative stress, inflammation, apoptosis and endocrine disruption [34]. Cd effects have been widely studied. Different toxicity mechanisms are linked to Cd exposition, including inflammation, cytotoxicity, oxidative stress, apoptosis and disruption of signaling pathways, which regulate the reproductive functions [35].
Almost all the masculine reproductive tract units are targets of EDCs. Testes are the direct target of a lot of toxicants, such as Cd [36]. Elements such as Cd, mercury (Hg) and Pb produce a dysfunction in Sertoli cells (SCs) [33]. Toxicants affecting Leydig cells can cause anomalies in the testosterone secretion, which results in an impaired SCs function and in a defective spermatogenesis. Moreover, the Leydig cells and SCs affectation can lead to the seminiferous epithelium reduction [37]. In addition, the affectation of the spermatogenesis process can occur through the alteration of the adhesion between germ cells or SCs [33]. Most of the studies where the role of the SCs is assessed have been carried out in vitro. Note that comparisons between the results found in vitro and in vivo studies are difficult [38]. Besides, a brief exposure of the testes to Cd could alter the molecular defense system. Cd reaches its molecular targets (FAK and cadherins), impairing the cell adhesion function and interrupting the spermatogenesis process [32].
There is evidence that certain toxicants interact with the secretion of hypothalamic releasing factors, luteinizing hormone (LH) and follicle-stimulating hormone (FSH), all of which play a major role in sperm quality [28]. Besides, the endocrine-hormone levels could inform about the functionality of the testicular cells, although it is not a well considered biomarker [33]. The hypothalamic–pituitary–testis (HPT) axis is also an EDC target [35][39], which results in the alteration of the physiological function of the testis [40]. During the steroidogenesis process, heavy metals disrupt the androgen production. This could be mediated by receptors or by direct effects on gene transcription.
Furthermore, EDCs induce oxidative stress, which plays an important role in male infertility [22]. In physiological conditions, ROS are molecules that affect normal sperm functionality, whereas seminal plasma contains antioxidant molecules and biomolecules that help to maintain the balance [41]. However, exposure to heavy metals increases the production of ROS and decreases the antioxidant defenses. This fact induces alterations in SCs, such as DNA damage, lipid peroxidation and, ultimately, apoptosis [33]. Patients with an elevated ROS production in semen may benefit from an antioxidant therapy. Antioxidant supplements can be separated in two categories, synthetic or natural. Synthetic antioxidants are chemically synthesized and isolated compounds, while natural antioxidants are spontaneously present in foods. The consumption of natural antioxidants seems to increase the total antioxidant capacity [42]. In agreement with this, a diet rich in carotenoids, for instance, could improve the sperm motility and morphology [43]. In addition, lower rates of aneuploid sperm were correlated with dietary folate intake [44]. Hence, dietary supplementation with antioxidants may be interesting to ameliorate seminal quality, thus improving male reproductive health.
2.2. Sources of Heavy Metals Exposure
Localized exposure to heavy metals, e.g., due to one’s occupation, or to one’s lifestyle habits, is the most common type of exposure. Generally, the human population is exposed to heavy metals voluntarily. The voluntary way of exposure to these toxicants can be by oral supplementation. On the contrary, involuntary exposure can be through the intake of contaminated water or food. Nowadays, the environment is a matter of concern because heavy metals are widely distributed [45].
Food Exposure
Although diet, which includes daily intakes of antioxidants, may be useful to improve the ROS production in semen, it is also a common way to consume heavy metals.
The intake of contaminated food is a usual source of exposure to heavy metals, as described above. Contamination can happen during the handling of food and its processing. Contaminated soils may also contribute to the pollution of food of both vegetable and animal origin [22]. Drinking water contaminated with As has arisen as an important health problem in Asia, India and China, among other countries [46]. Focusing on food, fruits may contain Cu, Pb and Zn at high concentrations [47]. Moreover, strawberries, dates, spinach and cucumber contain Cd, in addition to the above-mentioned elements [48]. In milk, meat and meat-derived products, elements such as As, Cd and Pb were detected [49]. In seafood, inorganic As was found in algae [50]. Additionally, in cereals such as Indian rice, As, Pb, Cd and Hg were found, although the values did not exceed the maximum residue limits [51].
Environmental Exposure
Environmental exposure includes the exposure to environmental pollutants, including tobacco smoke. They have the potential to alter the male reproductive system, thus worsening the capacity of conceiving a healthful offspring [52]. The environmental pollutants also have transgenerational genetic effects, which may affect future generations. This problem is currently an important matter of concern [26]. Studies with environmentally realistic exposure levels to heavy metals and their impact on male reproductive outcomes are scarce, while those with high occupational-exposure levels had been widely documented. However, low-exposure effects have been evidenced, being stronger for elements such as Cd, Pb and Hg [53].
A meta-analysis found that the environment pollution reduced sperm motility. There is some concern about the decline of male fertility in metropolitan areas [54] and, especially, in countries with a higher risk of exposure, such as Nigeria [55]. The sperm concentration in the African population has decreased significantly by 73% during the last 50 years [56]. This problem is caused by multiple exposures to environmental toxins, including Cd and Pb. Future studies should analyze the relationship among the nature of the duration, the intensity of the exposure and the degree of infertility, as the effect on male fertility depends on those parameters [54]. Although the influencing factors are multiple, exposure to pesticides and heavy metals is the main culprit [56].
Heavy metals such as Pb or As are present in tobacco smoke, as well as Cu, Cd [57], Cr and nickel (Ni) [58][59]. As mentioned above, some studies suggest a relationship between tobacco smoke and adverse reproductive outcomes [52]. Hg is another highly toxic environmental pollutant. Recent research found that it may cause impairments in the reproductive function, leading to deformations in the seminiferous tubules and in Leydig cells and giving rise to a final testicular deterioration [60].
Environmental toxicants lead to ROS formation. This stress is associated with several deleterious effects, such as testicular apoptosis, erroneous protamination, abnormal sperm functionality and viability, and oxidative DNA damage, causing male infertility [15][61]. This pro-oxidative microenvironment is produced, among others, by certain heavy metals (Cd, Pb, Cr, manganese (Mn), Hg, Zn and Cu). Cd is a widely studied heavy metal, which increases the activity of ROSs and induces changes in the enzymatic activity systems and inflammatory reactions [62]. As mentioned above, Cr and Cu are two heavy metals responsible for an altered content of SNBP in men environmentally exposed to pollutants. In addition, they are correlated with spermatic DNA damage due to an unstable DNA binding [23]. Further to this, an altered protamines/histones ratio was found in 84% of men residing in air polluted areas and, thus, exposed to these elements. Moreover, a different DNA binding pattern was found in men with a normal protamines/histone ratio. Unexpectedly, in those samples, SNBP were involved in the oxidative damage present in the spermatic DNA [63]. Some studies performed on animal models, such as Mytilus galloprovincialis L., yielded similar conclusions as those drawn for humans. For instance, in the presence of Cd, protamine-like proteins (PL) as PL-II suffered complete conformational changes, promoting a different DNA-binding mode. This resulted in affecting the sperm chromatin organization, which is crucial for a successful fertilization [64].
Nevertheless, further studies focusing on the molecular mechanisms are needed. In addition, the epigenetic modifications implicated in smoking cigarettes needs to be known, since tobacco smoke is a widely present environmental contaminant. More importantly, as these modifications are heritable, it would be interesting to study the transgenerational effects of tobacco smoke through the paternal line [65][66].
Occupational Exposure
Hazardous occupations in reproductive terms are evaluated based on years of service and agents of exposure. Normally, exposure data and other cause–effect parameters are insufficient to indicate which chemical factor is responsible for reproductive dysfunctions [28]. Workers exposed to heavy metals present a high risk of suffering a reproductive dysfunction [67]. Pb was one of the most studied elements which had a negative relationship with male fertility. Others, such as Cd and Cr, also have negative effects on fertility [68]. It must be borne in mind that the effects overlap due to multiple exposures. Observed adverse effects include reduced fertility, poor seminal quality, enhanced risk of lower birth weight, miscarriages and permanent sterility [67].
Some reports have suggested a decline in sperm concentration and an increase in reproductive disorders over the past 50 years. Occupational exposure to heavy metals such as inorganic Pb and Hg occurs in professions related to metal smelting or welding, or boron mining [69]. Specifically, welding is considered as one of the main occupational agents that negatively affects male fertility [70]. Welding is an occupation that endangers workers, because of the exposure to fumes and dust that contain, among others, metals. In this area, the exposure level in the western world has declined, but some specific workers still work in such industries, so fertility remains threatened [70]. It can be concluded that occupational exposure to metals is associated with an impaired male reproductive function. The evidence of this effect is stronger for some metals, such as Pb, Mn and Hg, than for others, such as Cd, Cr and Ni [10].
3. Conclusions
The masculine reproductive function is vulnerable to several environmental and occupational hazards. Those compounds have not been totally identified, but substances as dioxins, polychlorinated biphenyls, phthalates, polycyclic aromatic hydrocarbons, pesticides, alkylphenols, bisphenol A and heavy metals (Hg, Cd, Pb, As, Pb, etc.) are some of them [21]. Exposure to heavy metals, which can happen through occupational or environmental exposure, is, nowadays, a threat to reproductive health (Figure 1).
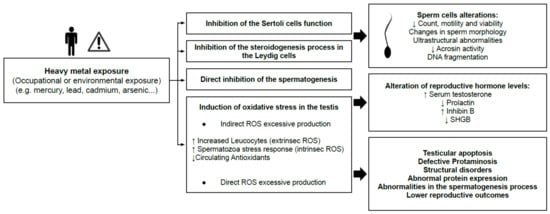
Figure 1. Summary of the effects of heavy metal exposure on men’s reproductive health. ROS, reactive oxygen species; SHBG, Sex Hormone Binding Globulin.
Those chemicals can mimic hormonal functions, so they are also known as endocrine disrupting compounds (EDCs). Man exposed to heavy metals have lower seminal quality, which is related to infertility or to a subfertility status. The negative effects are produced through the inhibition of the normal function of Sertoli and Leydig cells, the disruption of spermatogenesis and by the induction of oxidative stress in testes (indirect and direct reactive oxygen species production). Abnormal parameters of sperm count, motility, viability, morphology and DNA fragmentation, together with alterations in hormones levels, can also be found in men exposed to EDCs. Along with the design of appropriate therapeutic strategies to prevent located exposures to heavy metals, defects and deficiencies need to be considered. This is very relevant to overcome male factor fertility problems. To combat this, it is necessary to develop adequate tools (sensitive, non-invasive, fast and reliable) for heavy metal assessment in order to clear the diagnosis and improve seminal parameters.
Human studies are scarce and there is a lack of homogeneity in the methodology. In addition, the nature of the biological matrix (urine, blood, blood plasma, seminal plasma, semen, etc.) shows different results, making it difficult to choose one as the best option due to the different information that they provide. However, it should be noticed that the sperm content could be an accurate indicator of the impact of certain toxic substances on the reproduction potential.
Nevertheless, despite the discrepancies among the different methodologies observed in the studies, they generally emphasize the existence of a significant correlation between exposure to heavy metals and lower seminal quality, related to a lower fertility rate. Further to this, we found evidence suggesting that scientific research has proved that Pb and Cd are the analytes that most negatively affect seminal quality. Both have been correlated by different researchers with lower sperm concentrations, an abnormal spermatic morphology and lower sperm viability.
Further investigation is needed to completely understand on a molecular and cellular basis, how environmental and occupational exposure to heavy metals is related to infertility and, ultimately, its impact on reproductive outcomes. Due to the available facts, a greater collaboration between clinicians, epidemiologists and scientists is needed to identify the environmental chemicals, as well as the molecular and cellular processes, responsible for reproductive problems. If the aforementioned information is verified, it would be highly useful to introduce a heavy metal assessment in the biological analysis of samples of patients attending an assisted-reproduction center, allowing a personal diagnosis and prognosis and preventing men infertility. This would improve the success of the assisted reproductive techniques.
References
- Agarwal, A.; Mulgund, A.; Hamada, A.; Chyatte, M.R. A unique view on male infertility around the globe. Reprod. Biol. Endocrinol. 2015, 13, 1–9.
- Brugo-Olmedo, S.; Chillik, C.; Kopelman, S. Definición y causas de la infertilidad. Rev. Colomb. Obstet. Ginecol. 2003, 54, 227–248.
- Levine, H.; Jørgensen, N.; Martino-Andrade, A.; Mendiola, J.; Weksler-Derri, D.; Mindlis, I.; Pinotti, R.; Swan, S.H. Temporal trends in sperm count: A systematic review and meta-regression analysis. Hum. Reprod. Update 2017, 23, 646–659.
- Mann, U.; Shiff, B.; Patel, P. Reasons for worldwide decline in male fertility. Curr. Opin. Urol. 2020, 30, 296–301.
- Lindgren, M. Male Infertility. J. Physician Assis. 2018, 3, 139–147.
- Guzick, D.S.; Overstreet, J.W.; Factor-Litvak, P.; Brazil, C.K.; Nakajima, S.T.; Coutifaris, C.; Carson, S.A.; Cisneros, P.; Steinkampf, M.P.; Hill, J.A.; et al. Sperm Morphology, Motility, and Concentration in Fertile and Infertile Men. N. Engl. J. Med. 2001, 345, 1388–1393.
- World Health Organization. WHO Laboratory Manual for the Examination and Processing of Human Semen; World Health Organization: Geneva, Switzerland, 2010.
- Kenkel, S.; Rolf, C.; Nieschlag, E. Occupational risks for male fertility: An analysis of patients attending a tertiary referral centre. Int. J. Androl. 2001, 24, 318–326.
- Wald, M. Male infertility: Causes and cures. Sex. Reprod. Menopause 2005, 3, 83–87.
- Bracke, A.; Peeters, K.; Punjabi, U.; Hoogewijs, D.; Dewilde, S. A search for molecular mechanisms underlying male idiopathic infertility. Reprod. Biomed. Online 2018, 36, 327–339.
- Wang, C.; Swerdloff, R.S. Limitations of semen analysis as a test of male fertility and anticipated needs from newer tests. Fertil. Steril. 2014, 102, 1502–1507.
- Khatun, A.; Rahman, S.; Pang, M.-G. Clinical assessment of the male fertility. Obstet. Gynecol. Sci. 2018, 61, 179–191.
- Muratori, M.; Marchiani, S.; Maggi, M.; Forti, G.; Baldi, E. Origin and biological significance of DNA fragmentation in human spermatozoa. Front. Biosci. 2006, 11, 1491–1499.
- Uppangalaa, S.; Pudakalakattib, S.; D’souzaa, F.; Salian, S.R.; Kalthur, G.; Kumar, P.; Atreya, H.; Adiga, S.K. Influence of sperm DNA damage on human preimplantation embryo metabolism. Reprod. Biol. 2016, 16, 234–241.
- Aitken, R.J.; Baker, M.A. The Role of Genetics and Oxidative Stress in the Etiology of Male Infertility—A Unifying Hypothesis? Front. Endocrinol. 2020, 11, 581838.
- Ma, Y.; He, X.; Qi, K.; Wang, T.; Qi, Y.; Cui, L.; Wang, F.; Song, M. Effects of environmental contaminants on fertility and reproductive health. J. Environ. Sci. 2019, 77, 210–217.
- Figa-Talamanca, I.; Traina, M.E.; Urbani, E. Occupational exposures to metals, solvents and pesticides: Recent evidence on male reproductive effects and biological markers. Occup. Med. 2001, 51, 174–188.
- Kopp, R.; Martínez, I.O.; Legradi, J.; Legler, J. Exposure to endocrine disrupting chemicals perturbs lipid metabolism and circadian rhythms. J. Environ. Sci. 2017, 62, 133–137.
- Duffus, J.H. “Heavy metals” a meaningless term? (IUPAC Technical Report). Pure Appl. Chem. 2002, 74, 793–807.
- Ali, H.; Khan, E. What are heavy metals? Long-standing controversy over the scientific use of the term ‘heavy metals’—Proposal of a comprehensive definition. Toxicol. Environ. Chem. 2018, 100, 6–19.
- Balabanic, D.; Klemencic, A.K. Diet containing endocrine-disruptors and reproductive health. Handbook of Diet and Nutrition in the Menstrual Cycle. J. Reprod. Fertil. 2014, 2014, 359–372.
- Balabanič, D.; Rupnik, M.S.; Klemenčič, A.K. Negative impact of endocrine-disrupting compounds on human reproductive health. Reprod. Fertil. Dev. 2011, 23, 403–416.
- Lettieri, G.; Marra, F.; Moriello, C.; Prisco, M.; Notari, T.; Trifuoggi, M.; Giarra, A.; Bosco, L.; Montano, L.; Piscopo, M. Molecular Alterations in Spermatozoa of a Family Case Living in the Land of Fires. A First Look at Possible Transgenerational Effects of Pollutants. Int. J. Mol. Sci. 2020, 21, 6710.
- Bergamo, P.; Volpe, M.G.; Lorenzetti, S.; Mantovani, A.; Notari, T.; Cocca, E.; Cerullo, S.; Di Stasio, M.; Cerino, P.; Montano, L. Human semen as an early, sensitive biomarker of highly polluted living environment in healthy men: A pilot biomonitoring study on trace elements in blood and semen and their relationship with sperm quality and RedOx status. Reprod. Toxicol. 2016, 66, 1–9.
- Droller, M. Environment and the genitourinary tract. Otolaryngol. Neck Surg. 1996, 114, 248–252.
- Jenardhanan, P.; Panneerselvam, M.; Mathur, P.P. Effect of environmental contaminants on spermatogenesis. Semin. Cell Dev. Biol. 2016, 59, 126–140.
- Ilieva, I.; Sainova, I.; Yosifcheva, K. Toxic Effects of Heavy Metals (Lead and Cadmium) on Sperm Quality and Male Fertility. Acta Morphol. Anthropol. 2020, 27, 63–75.
- Kumar, S. Occupational Exposure Associated with Reproductive Dysfunction. J. Occup. Health 2004, 46, 1–19.
- Bosco, L.; Notari, T.; Ruvolo, G.; Roccheri, M.C.; Martino, C.; Chiappetta, R.; Carone, D.; Bosco, G.L.; Carrillo, L.; Raimondo, S.; et al. Sperm DNA fragmentation: An early and reliable marker of air pollution. Environ. Toxicol. Pharmacol. 2018, 58, 243–249.
- Yang, T.; Deng, L.; Sun, B.; Zhang, S.; Xian, Y.; Xiao, X.; Zhan, Y.; Xu, K.; Buonocore, J.J.; Tang, Y.; et al. Semen quality and windows of susceptibility: A case study during COVID-19 outbreak in China. Environ. Res. 2021, 197, 111085.
- Li, H.; Xiao, X.; Zhang, J.; Zafar, M.I.; Wu, C.; Long, Y.; Lu, W.; Pan, F.; Meng, T.; Zhao, K.; et al. Impaired spermatogenesis in COVID-19 patients. EClinicalMedicine 2020, 28, 100604.
- Wan, H.T.; Mruk, D.D.; Wong, C.K.C.; Cheng, C.Y. Targeting testis-specific proteins to inhibit spermatogenesis: Lesson from endocrine disrupting chemicals. Expert Opin. Ther. Targets 2013, 17, 839–855.
- Reis, M.M.S.; Moreira, A.C.; Sousa, M.; Mathur, P.; Oliveira, P.F.; Alves, M.G. Sertoli cell as a model in male reproductive toxicology: Advantages and disadvantages. J. Appl. Toxicol. 2015, 35, 870–883.
- Lovaković, B.T. Cadmium, arsenic, and lead: Elements affecting male reproductive health. Curr. Opin. Toxicol. 2020, 19, 7–14.
- De Angelis, C.; Galdiero, M.; Pivonello, C.; Salzano, C.; Gianfrilli, D.; Piscitelli, P.; Lenzi, A.; Colao, A.; Pivonello, R. The environment and male reproduction: The effect of cadmium exposure on reproductive function and its implication in fertility. Reprod. Toxicol. 2017, 73, 105–127.
- Pavlova, E.; Atanassova, N. Impact of Cadmium on Male Fertility. Acta Morphol. Anthropol. 2018, 25, 108–116.
- Manfo, F.P.T.; Nantia, E.A.; Mathur, P.P. Effect of Environmental Contaminants on Mammalian Testis. Curr. Mol. Pharmacol. 2015, 7, 119–135.
- Ramos-Treviño, J.; Bassol-Mayagoitia, S.; Hernández-Ibarra, J.A.; Ruiz-Flores, P.; Nava-Hernández, M.P. Toxic effect of cadmium, lead, and arsenic on the sertoli cell: Mechanisms of damage involved. DNA Cell Biol. 2018, 37, 600–608.
- Plunk, E.C.; Richards, S.M. Endocrine-Disrupting Air Pollutants and Their Effects on the Hypothalamus-Pituitary-Gonadal Axis. Int. J. Mol. Sci. 2020, 21, 9191.
- Vigeh, M.; Smith, D.; Hsu, P.-C. How does lead induce male infertility? Iran. J. Reprod. Med. 2011, 9, 1–8.
- Sheweita, S.; Tilmisany, A.; Al-Sawaf, H. Mechanisms of Male Infertility: Role of Antioxidants. Curr. Drug Metab. 2005, 6, 495–501.
- Ko, E.Y.; Sabanegh, E.S.; Agarwal, A. Male infertility testing: Reactive oxygen species and antioxidant capacity. Fertil. Steril. 2014, 102, 1518–1527.
- Zareba, P.; Colaci, D.S.; Afeiche, M.; Gaskins, A.J.; Jørgensen, N.; Mendiola, J.; Swan, S.H.; Chavarro, J.E. Semen quality in relation to antioxidant intake in a healthy male population. Fertil. Steril. 2013, 100, 1572–1579.
- Young, S.; Eskenazi, B.; Marchetti, F.; Block, G.; Wyrobek, A. The association of folate, zinc and antioxidant intake with sperm aneuploidy in healthy non-smoking men. Hum. Reprod. 2008, 23, 1014–1022.
- Tchounwou, P.B.; Yedjou, C.G.; Patlolla, A.K.; Sutton, D.J. Heavy Metal Toxicity and the Environment. Mol. Clin. Environ. Toxicol. 2012, 101, 133–164.
- Mukherjee, A.; Sengupta, M.K.; Hossain, M.A.; Ahamed, S.; Das, B.; Nayak, B.; Lodh, D.; Rahman, M.M.; Chakraborti, D. Arsenic contamination in groundwater: A global perspective with emphasis on the Asian scenario. J. Health Popul. Nutr. 2006, 24, 142–163.
- Hamurcu, M.; Özcan, M.M.; Dursun, N.; Gezgin, S. Mineral and heavy metal levels of some fruits grown at the roadsides. Food Chem. Toxicol. 2010, 48, 1767–1770.
- Radwan, M.A.; Salama, A.K. Market basket survey for some heavy metals in Egyptian fruits and vegetables. Food Chem. Toxicol. 2006, 44, 1273–1278.
- Muñoz, O.; Bastias, J.M.; Araya, M.; Morales, A.; Orellana, C.; Rebolledo, R.; Velez, D. Estimation of the dietary intake of cadmium, lead, mercury, and arsenic by the population of Santiago (Chile) using a Total Diet Study. Food Chem. Toxicol. 2005, 43, 1647–1655.
- Almela, C.; Algora, S.; Benito, V.; Clemente, M.J.; Devesa, V.; Súñer, M.A.; Vélez, D.; Montoro, R. Heavy Metal, Total Arsenic, and Inorganic Arsenic Contents of Algae Food Products. J. Agric. Food Chem. 2002, 50, 918–923.
- Almutairi, M.; Alsaleem, T.; Jeperel, H.; Alsamti, M.; Alowaifeer, A.M. Determination of inorganic arsenic, heavy metals, pesticides and mycotoxins in Indian rice (Oryza sativa) and a probabilistic dietary risk assessment for the population of Saudi Arabia. Regul. Toxicol. Pharmacol. 2021, 125, 104986.
- Hruska, K.S.; Furth, P.A.; Seifer, D.B.; Sharara, F.I.; Flaws, J.A. Environmental Factors in Infertility. Clin. Obstet. Gynecol. 2000, 43, 821–829.
- Wirth, J.J.; Mijal, R.S. Adverse Effects of Low Level Heavy Metal Exposure on Male Reproductive Function. Syst. Biol. Reprod. Med. 2010, 56, 147–167.
- Najafi, T.F.; Roudsari, R.L.; Namvar, F.; Ghanbarabadi, V.G.; Talasaz, Z.H.; Esmaeli, M. Air Pollution and Quality of Sperm: A Meta-Analysis. Iran. Red Crescent Med. J. 2015, 17, e26930.
- Abarikwu, S.O. Causes and risk factors for male-factor infertility in Nigeria: A review. Afr. J. Reprod. Health 2013, 17, 150–166.
- Sengupta, P.; Nwagha, U.; Dutta, S.; Krajewska-Kulak, E.; Izuka, E. Evidence for decreasing sperm count in African population from 1965 to 2015. Afr. Health Sci. 2017, 17, 418–427.
- Thompson, J.; Bannigan, J. Cadmium: Toxic effects on the reproductive system and the embryo. Reprod. Toxicol. 2008, 25, 304–315.
- Rogers, J.M. Tobacco and pregnancy: Overview of exposures and effects. Birth Defects Res. Part C Embryo Today Rev. 2008, 84, 1–15.
- Ren, T.; Chen, X.; Ge, Y.; Zhao, L.; Zhong, R. Determination of heavy metals in cigarettes using high-resolution continuum source graphite furnace atomic absorption spectrometry. Anal. Methods 2017, 9, 4033–4043.
- Bjørklund, G.; Chirumbolo, S.; Dadar, M.; Pivina, L.; Lindh, U.; Butnariu, M.; Aaseth, J. Mercury exposure and its effects on fertility and pregnancy outcome. Basic Clin. Pharmacol. Toxicol. 2019, 125, 317–327.
- Lavranos, G.; Balla, M.; Tzortzopoulou, A.; Syriou, V.; Angelopoulou, R. Investigating ROS sources in male infertility: A common end for numerous pathways. Reprod. Toxicol. 2012, 34, 298–307.
- Martynowicz, H.; Skoczyńska, A.; Karczmarek-Wdowiak, B.; Andrzejak, R. Effects of cadmium on testis function. Med. Pr. 2005, 56, 167–174.
- Lettieri, G.; D’Agostino, G.; Mele, E.; Cardito, C.; Esposito, R.; Cimmino, A.; Giarra, A.; Trifuoggi, M.; Raimondo, S.; Notari, T.; et al. Discovery of the Involvement in DNA Oxidative Damage of Human Sperm Nuclear Basic Proteins of Healthy Young Men Living in Polluted Areas. Int. J. Mol. Sci. 2020, 21, 4198.
- De Guglielmo, V.; Puoti, R.; Notariale, R.; Maresca, V.; Ausió, J.; Troisi, J.; Verrillo, M.; Basile, A.; Febbraio, F.; Piscopo, M. Alterations in the properties of sperm protamine-like II protein after exposure of Mytilus galloprovincialis (Lamarck 1819) to sub-toxic doses of cadmium. Ecotoxicol. Environ. Saf. 2019, 169, 600–606.
- Hales, B.F.; Robaire, B. Review—Paternal exposure to drugs and environmental chemicals: Effects on progeny outcome. J. Androl. 2001, 22, 927–936.
- Qiao, Z.-D.; Dai, J.-B.; Wang, Z.-X. The hazardous effects of tobacco smoking on male fertility. Asian J. Androl. 2015, 17, 954–960.
- Ashiru, O.; Odusanya, O.O. Fertility and occupational hazards: Review of the literature. Afr. J. Reprod. Health 2009, 13, 159–165.
- Sheiner, E.K.; Sheiner, E.; Hammel, R.D.; Potashnik, G.; Carel, R. Effect of Occupational Exposures on Male Fertility: Literature Review. Ind. Health 2003, 41, 55–62.
- Bonde, J.P. Male reproductive organs are at risk from environmental hazards. Asian J. Androl. 2010, 12, 152–156.
- Jensen, T.K.; Bonde, J.P.; Joffe, M. The influence of occupational exposure on male reproductive function. Occup. Med. 2006, 56, 544–553.
More
Information
Subjects:
Reproductive Biology
Contributor
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
1.5K
Revisions:
2 times
(View History)
Update Date:
26 Oct 2021
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No





