
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Diego Fernández Lázaro | + 1664 word(s) | 1664 | 2020-12-01 09:59:31 | | | |
| 2 | Karina Chen | -432 word(s) | 1232 | 2021-01-15 05:03:29 | | |
Video Upload Options
Muscular alterations as a consequence of hypoxic situations contribute not only to a decrease in life expectancy but also to a lower quality of life and health status. Our perspective, based on the results of this systematic review, is that Electromyography (EMG) is a suitable tool for monitoring the different skeletal muscle responses and has sufficient sensitivity to detect the muscle changes produced by hypoxic stimuli. Therefore, surface EMG (sEMG) maybe provide a practical point-of-care diagnostic test for medical diagnoses as well as a tool to improve sports performance. integrated EMG (iEMG) studies the physiology and pathology of denervation, re-innervation, and various myopathies. It also analyzes deep musculature such as muscular behavior, temporal activity patterns, fatigue, and muscular activation. sEMG is suitable for providing information about global muscle behavior, temporal activity patterns, muscle fatigue, and the activation level of the superficial musculature.
1. Introduction
Hypoxia is defined as the reduction of oxygen (O2) content or pressure at the cellular level. Hypoxemic hypoxia is one of the main approaches to improving muscular performance. It has two subtypes: hypobaric hypoxia, characterized by an atmospheric pressure lower than 760 mm Hg and a fraction of inspired O2 (FiO2) of 20.9%; and normobaric hypoxia, with a barometric pressure of 760 mm Hg and a FiO2 of less than 20.9%. In terms of exposure time, hypoxia is classified as acute, chronic, or intermittent. Intermittent hypoxia characterizes a state in which subjects are exposed to alternating cycles of hypoxia and normoxia. These artificial hypoxic conditions (hypobaric or normobaric) can be simulated by devices such as mixed gas masks, chambers, tents or rooms, and reduced-oxygen breathing devices [1]. Two common techniques that simulate altitude training in elite athletes are intermittent hypoxic exposure (IHE) and intermittent hypoxic training (IHT). IHE is implemented through lengths of passive stays in a hypoxic environment or through breathing in an environment with reduced oxygen concentration, whereas IHT consists of training sessions under hypoxic conditions [2].
Electromyography (EMG) is an indirect diagnostic device to evaluate the electrical activity produced in muscles by a nerve impulse that generates a potential for action in the membrane of myocytes in situations of rest or activation phase [3][4]. In general, EMG can be classified according to the test protocol conducted on the individual being evaluated: resting EMG (determines basal muscular electrical activity), voluntary EMG (assesses muscular response after the action), and EMG with evoked potentials (evaluates motor units) [5].
EMG is a type of recording equipment composed of several elements: electrodes, amplifiers, and a registration system. It has two types of electrodes: internal or needle electrodes (deep EMG or integrated EMG (iEMG), and surface electrodes (kinesiological or surface EMG (sEMG)). The EMG signal is emitted by the electrodes and is collected in the amplifier, which detects potential difference and eliminates interference. Next, the signal is quantified by means of a recording system that expresses the signal entity compared to a previously obtained reference value. There are two primary methods of signal amplification: monopolar and bipolar configurations. Moreover, there are different types of recording systems that collect information, such as graphic recording, oscilloscopic recording, permanent records on paper, or permanent records by photographic means [3][5][6][7].
EMG has multiple applications, not least as a diagnostic tool. In some cases, patients are diagnosed after the onset of the first symptoms that follow a lengthy preclinical phase. Delayed diagnosis may cause health problems and notably reduce the quality of life. In this context, EMG provides a relatively simple and accessible diagnosis, one that yields information about the state of the peripheral nerves and muscles. EMG may also be useful in the early diagnosis of neuromuscular disease, distinguishing the specific type(s) of pathology and its effect on the axons or the nerve myelin. In other words, EMG may act as a record of muscle electrical activity; therefore, it constitutes an extension of physical examination that can evaluate the integrity of the motor system [1][5][7][8].
2. Application of Electromyography for a Sustainable Lifestyle
2.1. Quality of Health and Quality of Life
The application of EMG in rehabilitation medicine may prove especially useful. EMG allows clinicians to study muscular physiology and diagnose neuromuscular diseases (Figure 1). Furthermore, EMG can be used to detect spasms, muscular hyperactivity, muscular imbalances, and the resting and occlusal positions of the jaw [5]. Moreover, it allows for the analysis of muscular movement (i.e., muscle walking), to determine the activation time of the muscle, the beginning and end of the articular position, and the degree of muscular activation that marks the muscular effort that is necessary to generate the action of gesture and intermuscular coordination [4]. These parameters are important when assessing pathologies with movement disorders from neurological origin, post-surgical care after a joint prosthesis, and in case of instability and/or injuries of the ligaments [9][10][11][12]. Additionally, EMG allows for the assessment of motor unit potentials, identification of neuromuscular alterations, [13] and differentiation of neuropathic and/or myopathy processes [4] (Figure 2).
Figure 1. Application of electromyography in sports rehabilitation.
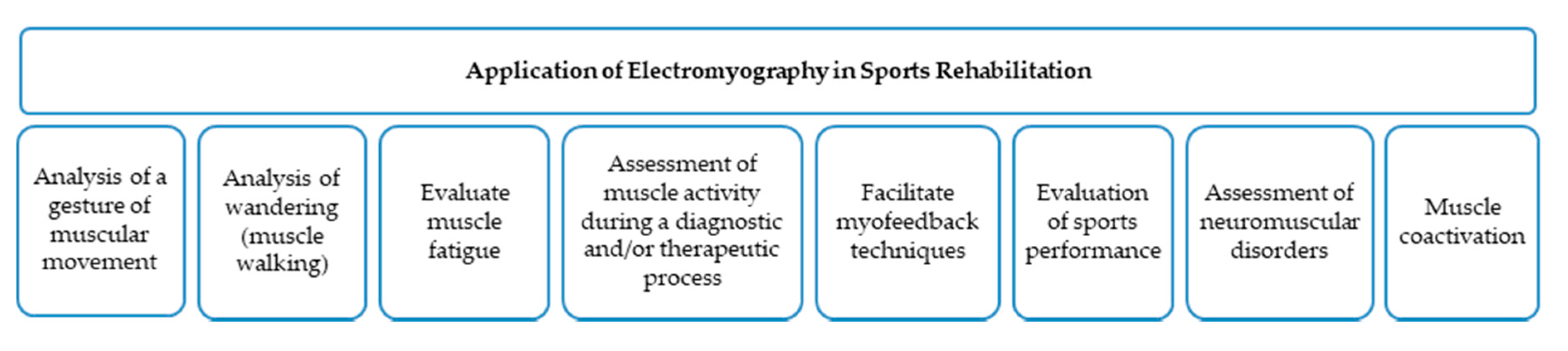
Figure 2. Main pathologies diagnosed by electromyography.
2.2. Physical Performance
EMG can analyze dynamic situations that may be of special interest in assessments of sports performance. Potential uses of EMG in physical performance include improvements in the effectiveness of a gesture, co-activation, fatigue, myofeedback techniques, diagnosis, and treatment of muscle injuries.
The effectiveness of a gesture implies the correct use of muscular work in terms of effort economy, profitability, and injury prevention. During training, improvements can be made in muscular activity. In particular, the execution of a task can be improved in terms of muscular activation and/or in terms of muscular fatigue based on the analysis of the frequencies of the electromyographic traces obtained. In other words, EMG improves the effectiveness of an action by saving effort and improving the prevention of muscular injuries [4].
Co-activation also involves simultaneous activity in agonist and antagonist muscles [14]. This is very important when assessing the quality of movement because alterations in coercion are related to immaturity of the neuromuscular system [4]. Furthermore, it is possible to evaluate fatigue with EMG by studying its evolution and potentially providing a solution with an appropriate treatment [15]. This is of special interest for sports and occupational medicine because it could improve sports performance and productivity [4]. EMG facilitates myofeedback techniques that are widely used in physiotherapy with the aim of postural re-education and proprioception work [16]. EMG gives the opportunity to assess muscle activity during a diagnostic and/or therapeutic process in sports medicine. Moreover, it analyzes muscular activation, which allows for the comparison of healthy and pathological states. Lastly, EMG provides information about muscular coordination and the relationship between agonist and antagonist muscles [16].
3. Perspectives
Muscular alterations as a consequence of hypoxic situations contribute not only to a decrease in life expectancy but also to a lower quality of life and health status. Our perspective, based on the results of this systematic review, is that EMG is a suitable tool for monitoring the different skeletal muscle responses and has sufficient sensitivity to detect the muscle changes produced by hypoxic stimuli. Therefore, sEMG maybe provide a practical point-of-care diagnostic test for medical diagnoses as well as a tool to improve sports performance. iEMG studies the physiology and pathology of denervation, re-innervation, and various myopathies. It also analyzes deep musculature such as muscular behavior, temporal activity patterns, fatigue, and muscular activation. sEMG is suitable for providing information about global muscle behavior, temporal activity patterns, muscle fatigue, and the activation level of the superficial musculature.
References
- Fernandez-Lazaro, D.; Diaz, J.; Caballero, A.; Cordova, A. Strength and endurance training in hypoxia: Effect on muscular hypertrophy. Biomedica 2019, 39, 212–220.
- Millet, G.P.; Roels, B.; Schmitt, L.; Woorons, X.; Richalet, J.P. Combining hypoxic methods for peak performance. Sports Med. 2010, 40, 1–25.
- Córdova Martínez, A.; Nuin, I.; Fernández-Lázaro, D.; Latasa Zudaire, I.A.; Rodríguez Falces, J. Electromyographic activity (EMG) during pedaling, its usefulness in the diagnosis of fatigue in cyclists. Med. Dep. 2017, 34, 217–223.
- Massó, N.; Rey, F.; Romero, D.; Gual, G.; Costa, L.; Germán, A. Applications of surface electromyography in sport. Med. Esport. 2010, 45, 127–136.
- Caballero, K.; Duque, L.M.; Ceballos, S.; Ramírez, J.C.; Peláez, A. Basic concepts for electromyographic analysis. Ces. Odontol. 2002, 15, 41–50.
- Tankisi, H.; Burke, D.; Cui, L.; de Carvalho, M.; Kuwabara, S.; Nandedkar, S.D.; Rutkove, S.B.; Stålberg, E.; Van Putten, M.J.; Fuglsang-Frederiksen, A. Standards of instrumentation of EMG. Neurophysiol. 2020, 131, 243–258.
- Rojas Martínez, M.; Mañanas Villanueva, M.Á. Multichannel surface electromyography as a non-invasive tool in neuromuscular rehabilitation. In Proceedings of the 4th CEA Bioengineering Symposium 2012: Brain Computer Interface and Rehabilitation Technologies [conference proceedings on the Internet]; 29th May 2012, Valladolid, Spain:. Valladolid: University of Valladolid; 2012 [cited 2020 Sep 2]. p. 73-9. Available from https://upcommons.upc.edu/handle/2117/17970.
- Cordova Martinez, A.; Pascual Fernandez, J.; Fernandez Lazaro, D.; Alvarez Mon, M. Muscular and heart adaptations of execise in hypoxia. Is training in slow hypoxy healthy? Clin. 2017, 148, 469–474.
- Benedetti, M. Muscle activation intervals and EMG envelope in clinical gait analysis. IEEE Eng. Med. Biol. Mag. 2001, 20, 33–44.
- Benedetti, M.G.; Catani, F.; Bilotta, T.; Marcacci, M.; Mariani, E.; Giannini, S. Muscle activation pattern and gait biomechanics after total knee replacement. Biomech. 2003, 18, 871–876.
- Benoit, D.L.; Lamontagne, M.; Cerulli, G.; Liti, A. The clinical significance of electromyography normalisation techniques in subjects with anterior cruciate ligament injury during treadmill walking. Gait Posture 2003, 18, 56–63.
- Frigo, C.; Crenna, P. Multichannel SEMG in clinical gait analysis: A review and state-of-the-art. Biomech. 2009, 24, 236–245.
- Meekins, G.D.; So, Y.; Quan, D. American Association of Neuromuscular & Electrodiagnostic Medicine evidenced‐based review: Use of surface electromyography in the diagnosis and study of neuromuscular disorders. Muscle Nerve 2008, 38, 1219–1224.
- Balestra, G.; Frassinelli, S.; Knaflitz, M.; Molinari, F. Time-frequency analysis of surface myoelectric signals during athletic movement. IEEE Eng. Med. Biol. Mag. 2001, 20, 106–115.
- Nordander, C.; Hansson, G.-Å.; Rylander, L.; Asterland, P.; BystrÖm, J.U.; Ohlsson, K.; Balogh, I.; Skerfving, S. Muscular rest and gap frequency as EMG measures of physical exposure: The impact of work tasks and individual related. Ergonomics 2000, 43, 1904–1919.
- So, R.; Ng, J.; Lam, R.; Lo, C.; Ng, G. EMG wavelet analysis of quadriceps muscle during repeated knee extension movement. Sci. Sports Exerc. 2009, 41, 788–796.




