| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Chioma Izzi-Engbeaya | + 904 word(s) | 904 | 2020-10-19 11:18:50 | | | |
| 2 | Lily Guo | Meta information modification | 904 | 2020-10-26 10:40:54 | | | | |
| 3 | Lily Guo | Meta information modification | 904 | 2020-10-29 02:15:21 | | | | |
| 4 | Lily Guo | Meta information modification | 904 | 2020-10-30 06:47:35 | | |
Video Upload Options
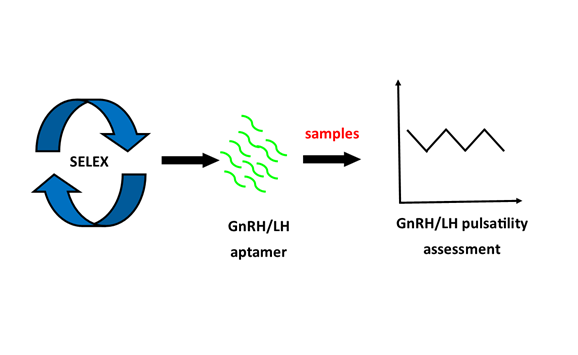
Aptamers are a novel technology enabling the continuous measurement of analytes in blood and other body compartments, without the need for repeated sampling and the associated reagent costs of traditional antibody-based methodologies. Aptamers are short single-stranded synthetic RNA or DNA that recognise and bind to specific targets. The conformational changes that can occur upon aptamer-ligand binding are transformed into chemical, fluorescent, color changes and other readouts. Aptamers have been developed to detect and measure a variety of targets in vitro and in vivo. Gonadotropin-releasing hormone (GnRH) is a pulsatile hypothalamic hormone, that is essential for normal fertility but difficult to measure in the peripheral circulation. However, pulsatile GnRH release results in pulsatile luteinizing hormone (LH) release from the pituitary gland. As such, LH pulsatility is the clinical gold standard method to determine GnRH pulsatility in humans. Aptamers have recently been shown to successfully bind to and measure GnRH and LH and this review focuses on this specific area. However, due to the adaptability of aptamers, and their suitability for incorporation into portable devices, aptamer-based technology is likely to be used more widely in the future.
1. Introduction
Gonadotropin-releasing hormone (GnRH) is decapeptide secreted into the hypophyseal portal system by specialised hypothalamic neurons, to reach its site of action at the pituitary gland. GnRH acts on pituitary gonadotropes to stimulate the production and secretion of gonadotropins (luteinizing hormone (LH) and follicle stimulating hormone (FSH))[1]. LH and FSH stimulate the secretion of sex steroids from the gonads (primarily testosterone from the testes and oestrogen/progesterone from the ovaries)[2]. Apart from during the pre-ovulatory phase of the menstrual cycle, GnRH and LH secretion are inhibited by sex steroids (i.e., negative feedback)[3]. However, during the pre-ovulatory phase of the menstrual cycle, oestrogen exerts positive feedback on GnRH and LH secretion, leading to increased LH secretion and the production of the LH surge required for ovulation[3].
GnRH, LH and FSH all exhibit pulsatile secretory patterns, which are pivotal to their biological functions[3], including stimulation of gonadal sex steroid secretion. GnRH has a short half-life of 2-8 min in the peripheral circulation[4], with very low levels (i.e., ≤5pg/ml) detected in plasma[5]. Therefore, it is challenging to measure GnRH in the peripheral circulation. As LH pulses are temporally coupled with GnRH pulses and LH is stable in the blood[6], LH levels and pulses are commonly measured and used as the clinical gold standard surrogate markers of GnRH secretion.
GnRH and LH pulsatility change during different reproductive stages and at different phases of the menstrual cycle. Pre-pubertally, LH levels are low and very few LH pulses are detectable. However, as puberty progresses, LH pulse frequency increases in response to increased GnRH pulsatility[7]. In adulthood, LH pulses occur approximately every 2 h in healthy men[8]. In healthy women, LH pulses occur every 1-2 h in the follicular phase and every 4 h in the luteal phase[2]. When reproductive senescence occurs in menopausal women, LH levels are markedly elevated (resulting from the absence of negative feedback due to oestrogen deficiency), and approximately one LH pulse occurs each hour[9].
The detection and quantification of hormones (e.g. LH) have been reliant on antibody-based techniques for many decades. However, problems with these methods include suboptimal inter-assay reliability and reproducibility, high cost of reagents, high sample volumes required (limiting the number of samples that can be taken from a single subject) and the time-consuming nature of antibody-based assays[10]. To overcome these problems, alternative methods of analyte detection and quantification have been developed. One such method is based on the use of aptamers (i.e. synthetic ligand-binding oligonucleotides). In line with advancements in this technology, the development of aptamer-based assays has accelerated over the last two decades, such that their use is likely to become more widespread.
In this review, we highlight the major types of aptamers in development and outline possible applications for aptamer-based technology in the assessment of GnRH/LH pulsatility.
2. Potential Applications of GnRH/LH Aptamers
As aptamers have been used in conjunction with modified implantable electrodes (i.e., gold-coated electrodes functionalized with cocaine-specific aptamers) to measure cocaine in vivo in rat brains; a similar approach could be used to measure GnRH in the hypothalamus in animals. This would provide invaluable information such as changes in GnRH pulsatility during different stages of reproductive maturity and senescence, and in rodent models of human reproductive orders such as Polycystic Ovarian Syndrome (PCOS, the most common reproductive disorder affecting pre-menopausal women). Furthermore, incorporation of LH aptamers into intravenous or subcutaneous sensors would facilitate detailed characterisation of LH secretion and pulsatility in rodents, sheep and other mammals, which have been limited by factors such as blood volumes, technical challenges, as well as antibody-based assays with low specificity and inadequate sensitivity.
Furthermore, the development of the recently described robotic LH-aptamer system to include wireless connection to a portable transdermal sensor (similar to continuous glucose monitors currently in use for diabetes management) would revolutionize reproductive endocrinology research, due to the reduced costs and quantity of (previously inaccessible) information this technology would enable researchers to obtain. In addition, the availability of an inexpensive portable method of assessing LH pulsatility would facilitate timely and accurate diagnosis of patients presenting to clinicians with reproductive disorders, particularly as currently these patients’ reproductive hormones are assessed using single timepoint blood tests. Thus, GnRH and LH aptamers could have significant and beneficial impacts on research and in healthcare.
References
- Eli Hazum; P. Michael Conn; Molecular Mechanism of Gonadotropin Releasing Hormone (GnRH) Action. I. The GnRH Receptor*. Endocrine Reviews 1988, 9, 379-386, 10.1210/edrv-9-4-379.
- Marques, P.; Skorupskaite, K.; George, J.T.; Anderson, R.A. . Physiology of GNRH and Gonadotropin Secretion; Feingold, K.R.; Anawalt, B.; Boyce, A.; Chrousos, G.; Dungan, K.; Grossman, A., Eds.; Endotext: South Dartmouth, MA, USA, 2000; pp. https://www.ncbi.nlm.nih.gov/books/NBK279070.
- E. Knobil; T M Plant; L. Wildt; P E Belchetz; G. Marshall; Control of the rhesus monkey menstrual cycle: permissive role of hypothalamic gonadotropin-releasing hormone. Science 1980, 207, 1371-1373, 10.1126/science.6766566.
- David J. Handelsman; Ronald S. Swerdloff; Pharmacokinetics of Gonadotropin-Releasing Hormone and Its Analogs. Endocrine Reviews 1986, 7, 95-105, 10.1210/edrv-7-1-95.
- Carol A. Huseman; Robert P. Kelch; Gonadotropin Responses and Metabolism of Synthetic Gonadotropin-Releasing Hormone (GnRH) during Constant Infusion of GnRH in Men and Boys with Delayed Adolescence*. The Journal of Clinical Endocrinology & Metabolism 1978, 47, 1325-1331, 10.1210/jcem-47-6-1325.
- I. J. Clarke; J. T. Cummins; Increased Gonadotropin-Releasing Hormone Pulse Frequency Associated with Estrogen-Induced Luteinizing Hormone Surges in Ovariectomized Ewes*. Endocrinology 1985, 116, 2376-2383, 10.1210/endo-116-6-2376.
- Robert Boyar; Jordan Finkelstein; Howard Roffwarg; Sheldon Kapen; Elliot Weitzman; Leon Hellman; Synchronization of Augmented Luteinizing Hormone Secretion with Sleep during Puberty. New England Journal of Medicine 1972, 287, 582-586, 10.1056/nejm197209212871203.
- Chioma Izzi-Engbeaya; Sophie Jones; Yoshibye Crustna; Pratibha C Machenahalli; Deborah Papadopoulou; Manish Modi; Christos Panayi; Jessica Starikova; Pei Chia Eng; Maria Phylactou; et al.Edouard MillsLisa YangRisheka RatnasabapathyMark SykesIsabella PlumptreBen CoumbeVictoria C WingEwa PacuszkaPaul BechJames MinnionGeorge TharakanTricia TanJohannes VeldhuisAli AbbaraAlexander N ComninosWaljit S Dhillo Effects of Glucagon-like Peptide-1 on the Reproductive Axis in Healthy Men. The Journal of Clinical Endocrinology & Metabolism 2020, 105, 1119-1125, 10.1210/clinem/dgaa072.
- Julia K Prague; Margaritis Voliotis; Sophie Clarke; Alexander N Comninos; Ali Abbara; Channa N Jayasena; Rachel E Roberts; Lisa Yang; Johannes D Veldhuis; Krasimira Tsaneva-Atanasova; et al.Craig A McArdleWaljit S Dhillo Determining the relationship between hot flushes and LH pulses in menopausal women using mathematical modelling. The Journal of Clinical Endocrinology & Metabolism 2019, 104, 3628-3636, 10.1210/jc.2018-02797.
- Michael G. Weller; Quality Issues of Research Antibodies. Analytical Chemistry Insights 2016, 11, ACI.S31614-27, 10.4137/aci.s31614.