| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Martial CAILLAUD | + 1365 word(s) | 1365 | 2020-10-12 08:13:38 | | | |
| 2 | Vicky Zhou | Meta information modification | 1365 | 2020-10-20 10:37:28 | | |
Video Upload Options
Peripheral neuropathies (PN) can be triggered after metabolic diseases, traumatic peripheral nerve injury, genetic mutations, toxic substances, and/or inflammation. PN is a major clinical problem, affecting many patients and with few effective therapeutics. Recently, interest in natural dietary compounds, such as polyphenols, in human health has led to a great deal of research, especially in PN. Curcumin is a polyphenol extracted from the root of Curcuma longa. This molecule has long been used in Asian medicine for its anti-inflammatory, antibacterial, and antioxidant properties. However, like numerous polyphenols, curcumin has a very low bioavailability and a very fast metabolism. This part provides an overview of curcumin in the treatment of PN (anti-inflammatory, antioxidant, anti-endoplasmic reticulum stress (anti-ER-stress), neuroprotection, and glial protection). Finally, because PN are associated with numerous pathologies (e.g., cancers, diabetes, addiction, inflammatory disease...), this part is likely to interest a large audience.
1. Introduction
Peripheral neuropathies (PN) can be inherited or acquired as a result of a pathological process or trauma [1]. Causes of acquired PN can have multiple origins such as autoimmune, toxic, alcoholic, diabetic, cancerous, chemo-induced, and traumatic, including crushing, constriction, stretching, and complete nerve sectioning [2][3][4][5][6]. However, the precise ethology of some neuropathies is sometimes not identified. Clinicians refer to these conditions as idiopathic neuropathies. PN may affect a single nerve (mononeuropathy), two or more nerves in different areas (multiple mononeuropathy), or many nerves (polyneuropathy). Carpal tunnel syndrome and facial paralysis are examples of mononeuropathy. Most people with PN have polyneuropathy affecting longer nerve fibers (length-dependent polyneuropathy)[7].
The symptomatology is very diverse depending on the type of nerve fibers affected. In the case of sensory fiber damage, symptoms are dependent on the caliber and size of the nerve fibers. These symptoms are generally progressive numbness, tingling in the feet or hands which may extend to the legs and arms, or even sharp, throbbing, icy or burning pain, stinging sensations and extreme sensitivity to touch. In the case of motor fiber damage, the most common symptoms are a lack of motor coordination and falls, muscle weakness or paralysis. If autonomic nerves are affected, signs and symptoms may include: heat intolerance and alterations in sweating, dermal problems, intestinal, bladder or digestive problems, but also changes in blood pressure, which can lead to dizziness[1][2].
The major clinical problem in PN, in addition to the difficulties in diagnosing and understanding pathological mechanisms, is that they are poorly treated with currently available therapeutics.
2. Use Curcumin in Treatment of PN
Recently, interest in the role of dietary antioxidants, such as polyphenols, in human health has led to a great deal of research on their potential as possible treatment of many inflammatory diseases. Among these polyphenols, curcumin which has long been used in traditional Asian cuisine and medicine, is an attractive molecule. However, curcumin has a very low bioavailability and a very fast metabolism. Thus, very high doses are required to achieve therapeutic effects given the uncertainty that curcumin will reach the target organ.
Curcumin [1,7-bis(4-hydroxy-3-methoxyphenyl)-1,6-heptadiene-3,5-dione], also known as diferuloylmethane, is a polyphenol present in the rhizome of Curcuma longa[8]. Curcuma longa powder is a spice known as turmeric and used in the preparation of curry. Turmeric powder is an orange-yellow crystalline compound that is used as a food coloring agent [8]. Traditionally, turmeric powder has been used in Asian countries as a medicinal preparation to combat several diseases because of its antioxidant, anti-inflammatory, antimicrobial, anticancer, and neuroprotective properties [8][9][10][11][12]. Over the past 50 years, it has been shown that most of the effects of Curcuma longa are primarily due to curcumin, with potential beneficial properties against diabetes, allergies, arthritis, neuropathies, and other chronic diseases[13]. However, there are other components of Curcuma longa that, together with curcumin, form the curcuminoid group[14]. These are demethoxycurcumin and bis-demethoxycurcumin. The curcuminoid group constitutes about 5% of the total components of Curcuma longa and curcumin is the most abundant of this group with 77% [14].
Curcumin is a lipophilic molecule that is rapidly metabolized, leading to low bioavailability. Thus, several studies propose the use of new formulations of curcumin such as emulsions or nanoparticles to improve systemic bioavailability. These approaches are very interesting in the context of several PN in which nerves are affected (diabetes, alcohol, chemotherapy, genetic mutations.)[15]. Moreover, these approaches allow to decrease and better control the dose of curcumin used, although it has no proven toxicity. In this respect, there is growing evidence that curcumin nanoparticles have a better effect on oxidative stress than conventional curcumin[15]. Other authors propose in the case of localized lesions, as in the case of traumatic lesion, transection or local inflammation, the use of biofunctionalized conduit with curcumin or local administration at the site of the lesion[16]. Thus, the use of these new approaches (nanoparticles, tubes.) allows a progressive diffusion of curcumin in the target organism or organ. This makes it possible to avoid the “one shot” effect produced by a conventional injection. This diffusion is all the more interesting as it allows a better reduction of inflammation and oxidative stress, which are processes that last over time and can be chronic. Thus, curcumin because of its anti-inflammatory, antioxidant, anti-ER-stress, and neuro-protective properties is the perfect candidate for the treatment of PN[9].
In addition, its lipophilic nature allows it to be integrated into the myelin sheath, thus exerting a powerful antioxidant effect. The role of curcumin on the ER is not very clear at the moment. In our opinion, it represents a major challenge for the future. Indeed, a growing number of studies show the key role of this organelle in the development of numerous PN (diabetes, alcohol, chemotherapy, genetic mutations.). Thus, because of its numerous biological properties, curcumin reduces tissue damage or improves tissue repair (nerve, muscle, DRG) in many PN. These effects are also reflected at the behavioral level by reducing the signs of pain, improving sensory and motor recovery. However, despite a large number of pre-clinical studies (both in vitro and in vivo) on the subject and a large amount of laboratory evidence of curcumin’s efficacy, studies in humans are sorely lacking. Indeed, to date, only four clinical studies have been specifically conducted in humans in the field of PN. These studies, although encouraging, are sometimes carried out on too few subjects and therefore make it difficult to objectify the use of curcumin clinically for PN[17][18][19][20]. However, the large number of studies on inflammatory pain represents hope for the future use of this molecule for the treatment of neuropathies. We therefore believe that the advent of new curcumin formulations represents a key milestone in the treatment of PN in humans.
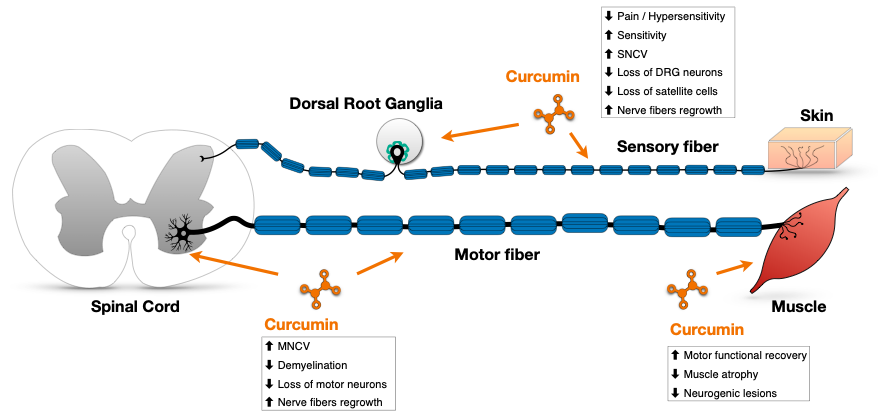
Figure1. A suggested model summarizing the sites of action of curcumin in peripheral neuropathies as reported in the literature: Curcumin reduces neuropathic pain and improves sensitivity in in vivo models of PN, by improving sensory nerve conduction velocity (SNCV), reducing the loss of neurons and satellite cells in dorsal roots ganglia (DRG), and promoting the regrowth of sensory nerve fibers. In addition, curcumin improves motor functions in in vivo models of PN, by improving motor nerve conduction velocity (MNCV), reducing nerve fibers demyelination, loss of motor neurons in spinal cord, muscle atrophy and neurogenic lesions, and improving motor nerves fibers regrowth.
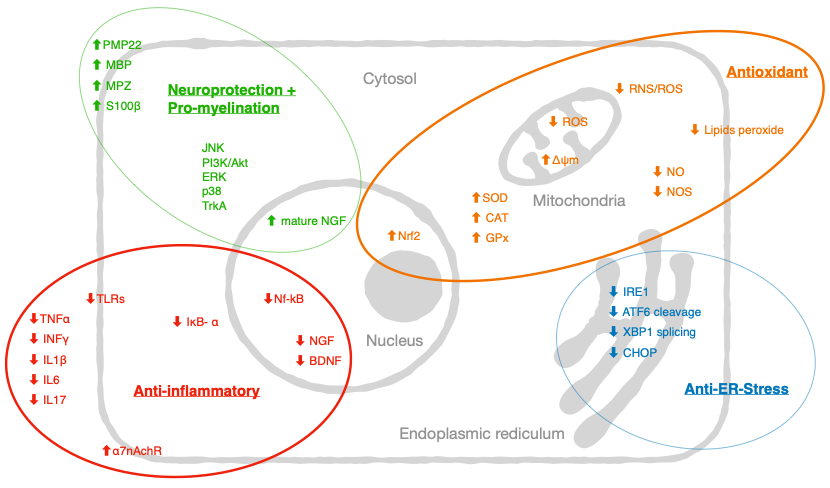
Figure 2. A proposed model summarizing the molecular targets of curcumin in peripheral neuropathies reported in the literature: Tumor necrosis factors (TNFα), interferon (INF-γ), interleukins (IL-1α, IL-1β, IL-6, IL_10), granulocyte-macrophage colony-stimulating factor (GM-CSF), monocyte chemoattractant protein-1 (MCP-1), and macrophage inflammatory protein (MIP-1α), Toll-like receptor (TLR, TLR1, TLR3, TLR4, and TLR7), nuclear factor-kappa B (NF-κB), NF-κB inhibitor-α (IκB-α), nerve growth factor (NGF), brain derived neurotrophic factor (BDNF), lipooxygenase (LOX), cyclooxygenase (COX), nitric oxide synthase (NOS), superoxide dismutase (SOD), catalase (CAT), glutathione peroxidase (GPx), transient receptor potential cation channel subfamily-M-2 (TRMP2), nuclear factor erythroid 2–related factor 2 (Nrf2), reactive oxygen species (ROS), reactive nitrogen species (RNS), peripheral myelin protein 22 (PMP22), myelin protein zero (MPZ), myelin basic protein (MBP), extracellular signal regulated kinase (ERK), c-Jun-N-terminal kinase (JNK), α7-nicotinic acetylcholine receptors (α7-nAchR), tropomyosin receptor kinase A (TrkA), phosphoinositide 3-kinase (PI3K), activating transcription factor 3 (ATF3), ER-residing protein endoplasmic oxidoreductin-1 (Ero-1β), activating transcription factor 6 (ATF6) cleavage, X-Box binding protein 1 (XBP1) splicing, and C/EBP homologous protein (CHOP).
References
- Richard A C Hughes; Regular review: Peripheral neuropathy. BMJ 2002, 324, 466-469, 10.1136/bmj.324.7335.466.
- Istvan Katona; Joachim Weis; Diseases of the peripheral nerves. Handbook of Clinical Neurology 2017, 145, 453-474, 10.1016/b978-0-12-802395-2.00031-6.
- Sindhu Ramchandren; Charcot-Marie-Tooth Disease and Other Genetic Polyneuropathies. CONTINUUM: Lifelong Learning in Neurology 2017, 23, 1360-1377, 10.1212/con.0000000000000529.
- Fabrice Billet; Martial Caillaud; Laurence Richard; Jean-Michel Vallat; Alexis Desmoulière; Peripheral nerve regeneration and intraneural revascularization. Neural Regeneration Research 2018, 14, 24-33, 10.4103/1673-5374.243699.
- Nathan P. Staff; Jill C. Fehrenbacher; Martial Caillaud; M. Imad Damaj; Rosalind A. Segal; Sandra Rieger; Pathogenesis of paclitaxel-induced peripheral neuropathy: A current review of in vitro and in vivo findings using rodent and human model systems. Experimental Neurology 2020, 324, 113121, 10.1016/j.expneurol.2019.113121.
- Jordi Bruna; Paola Alberti; Aina Calls-Cobos; Martial Caillaud; M. Imad Damaj; Xavier Navarro; Methods for in vivo studies in rodents of chemotherapy induced peripheral neuropathy. Experimental Neurology 2020, 325, 113154, 10.1016/j.expneurol.2019.113154.
- C N Martyn; R A Hughes; Epidemiology of peripheral neuropathy.. Journal of Neurology, Neurosurgery & Psychiatry 1997, 62, 310-318, 10.1136/jnnp.62.4.310.
- Maria L.A.D. Lestari; Gunawan Indrayanto; Curcumin. Profiles of Drug Substances, Excipients and Related Methodology 2013, 39, 113-204, 10.1016/b978-0-12-800173-8.00003-9.
- Gianni Belcaro; Morio Hosoi; Luciano Pellegrini; Giovanni Appendino; Edmondo Ippolito; Andrea Ricci; Andrea Ledda; Mark Dugall; Maria Rosaria Cesarone; Claudia Maione; et al.Giovanna CiammaichellaDomenico GenovesiStefano Togni A Controlled Study of a Lecithinized Delivery System of Curcumin (Meriva®) to Alleviate the Adverse Effects of Cancer Treatment. Phytotherapy Research 2013, 28, 444-450, 10.1002/ptr.5014.
- Gail B. Mahady; S L Pendland; G Yun; Z Z Lu; Turmeric (Curcuma longa) and curcumin inhibit the growth of Helicobacter pylori, a group 1 carcinogen.. Anticancer Research 2003, 22, 1.
- Bharat B. Aggarwal; Anushree Kumar; Alok C Bharti; Anticancer potential of curcumin: preclinical and clinical studies.. Anticancer Research 2003, 23, 1.
- Dawn Chin; Patricia Huebbe; Kathrin Pallauf; Gerald Rimbach; Neuroprotective Properties of Curcumin in Alzheimer’s Disease – Merits and Limitations. Current Medicinal Chemistry 2013, 20, 3955-3985, 10.2174/09298673113209990210.
- 11. Aggarwal, B.B., Surh, Y.-J., Shishodia, S.; The Molecular Targets and Therapeutic Uses of Curcumin in Health and Disease. Advances in Experimental Medicine and Biology; Springer 2006, 595, 1, 10.1007/978-0-387-46401-5.
- Santosh K. Sandur; Manoj K. Pandey; Bokyung Sung; Kwang Seok Ahn; Akira Murakami; Gautam Sethi; Pornngarm Limtrakul; Vladimir Badmaev; Bharat B. Aggarwal; Curcumin, demethoxycurcumin, bisdemethoxycurcumin, tetrahydrocurcumin and turmerones differentially regulate anti-inflammatory and anti-proliferative responses through a ROS-independent mechanism. Carcinogenesis 2007, 28, 1765-1773, 10.1093/carcin/bgm123.
- Martial Caillaud; Zeina Msheik; Gautier M-A Ndong-Ntoutoume; Laetitia Vignaud; Laurence Richard; Frédéric Favreau; Pierre-Antoine Faye; Franck Sturtz; Robert Granet; Jean-Michel Vallat; et al.Vincent SolAlexis DesmoulièreFabrice Billet Curcumin–cyclodextrin/cellulose Nanocrystals Improve the Phenotype of Charcot-Marie-Tooth-1A Transgenic Rats Through the Reduction of Oxidative Stress. Free Radical Biology and Medicine 2020, 1, 1, 10.1016/j.freeradbiomed.2020.09.019.
- Martial Caillaud; Benjamin Chantemargue; Laurence Richard; Laetitia Vignaud; Frédéric Favreau; Pierre-Antoine Faye; Philippe Vignoles; Franck Sturtz; Patrick Trouillas; Jean-Michel Vallat; et al.Alexis DesmoulièreFabrice Billet Local low dose curcumin treatment improves functional recovery and remyelination in a rat model of sciatic nerve crush through inhibition of oxidative stress. Neuropharmacology 2018, 139, 98-116, 10.1016/j.neuropharm.2018.07.001.
- Martial Caillaud; Yu Par Aung Myo; Bryan D. McKiver; Urszula Osinska Warncke; Danielle Thompson; Jared Mann; Egidio Del Fabbro; Alexis Desmoulière; Fabrice Billet; M. Imad Damaj; et al. Key Developments in the Potential of Curcumin for the Treatment of Peripheral Neuropathies. Antioxidants 2020, 9, 950, 10.3390/antiox9100950.
- Francesco Di Pierro; Roberto Settembre; Safety and efficacy of an add-on therapy with curcumin phytosome and piperine and/or lipoic acid in subjects with a diagnosis of peripheral neuropathy treated with dexibuprofen. Journal of Pain Research 2013, 6, 497-503, 10.2147/JPR.S48432.
- Sara Asadi; Mohammad Saeed Gholami; Fereydoun Siassi; Mostafa Qorbani; Kianoosh Khamoshian; Gity Sotoudeh; Nano curcumin supplementation reduced the severity of diabetic sensorimotor polyneuropathy in patients with type 2 diabetes mellitus: A randomized double-blind placebo- controlled clinical trial.. Complementary Therapies in Medicine 2019, 43, 253-260, 10.1016/j.ctim.2019.02.014.
- Joshua Burns; Pathma D. Joseph; Kristy J. Rose; Monique M. Ryan; Robert A. Ouvrier; Effect of Oral Curcumin on Déjérine-Sottas Disease. Pediatric Neurology 2009, 41, 305-308, 10.1016/j.pediatrneurol.2009.04.030.