1000/1000
Hot
Most Recent

Techniques for noncontact measurement of vital signs using camera imaging technologies have been attracting increasing attention. For noncontact physiological assessments, computer vision-based methods appear to be an advantageous approach that could be robust, hygienic, reliable, safe, cost effective and suitable for long distance and long-term monitoring. In addition, video techniques allow measurements from multiple individuals opportunistically and simultaneously in groups.
The monitoring of human vital signs, for example respiratory rate (RR), blood oxygen saturation (SpO2 ), heart rate (HR), heart rate variability (HRV) and blood pressure (BP) plays a significant role in modern clinical care of patients in hospitals and at home [1]. Applications include medical diagnosis, training programs, fitness assessment, lie detection and stress measurement [2]. There are various instruments for measuring these vital signs, such as electrocardiograms (ECGs), pulse oximeters, nasal thermocouples, respiratory belt transducers and piezoelectric transducers [3]. These instruments require direct physical contact with the human body as they use contact-based, sensor modalities, straps, probes or electrodes [4]. These instruments may cause skin infection, injury, or harmful reactions on patients especially premature babies, aged people or burns victims who have fragile skin [5]. Moreover, there is a risk of entanglement or strangulation of infants who are attached to monitors by means of wires and leads [6]. These instruments are also not appropriate for long term monitoring as they may cause discomfort, irritation and a cumulative risk of fungal and bacterial infection [7]. In addition, a reduced amplitude of chest wall expansion can affect the respiratory rate (RR) input signal from the impedance lead [8]. Furthermore, cost is an important issue as the monitoring electrodes and leads are only intended and certified for a single use, followed by disposal [9]. Placement of the sensors with self-adhesive pads leads to difficulties with wet, oily, dirty or hairy subjects which is a limitation of these technologies in emergency situations [10]. Accuracy is another issue with conventional contact methods since they are sensitive to artefacts produced by the subject’s movement [11]. Therefore, to minimise these limitations, there is a need for an alternative method where vital signs can be measured without any physical contact.
As presented in Figure 1, there are several noncontact means based on magnetic induction, the Doppler effect, thermal imaging and video camera imaging which can be an effective alternative means of monitoring vital signs with acceptable reliability and accuracy [12]. These methods depend on the observation of physical and physiological variations including skin colour, temperature, impedance changes, head motion, arterial pulse motion, and importantly, thoracic and abdominal motion due to the activity of both the respiratory and cardiovascular systems. Magnetic induction-based methods can detect the impedance changes caused by blood and air volume variations due to the mechanical action of the heart, diaphragm and thorax. The basic principle is to induce eddy currents in the tissue and to calculate the re-inducted magnetic field externally; the impedance changes can then be observed remotely to extract vital signs [13]. The method uses a simple arrangement based on multiple coils [14] or a single coil [15] integrated into a mattress [16], bed [17] or seat [18]. However, the method is highly susceptible to relative movements between coil and body.

Figure 1. Contactless measuring methods. (a) The Doppler effect; (b) thermal imaging; (c) video camera imaging.
The Doppler effect is an active noncontact method that can detect subtle chest movements due to cardiorespiratory activity. In this method, vital signs are extracted using a Doppler radar [19][20], or laser sensors [21] as well as digital signal processing (DSP) techniques [22] where the phase shift between the transmitted waves and the reflected received waves from a region of interest (ROI) are calculated. There are three types of Doppler-based methods—Doppler with electromagnetics [23][24], lasers [25][26], and ultrasonics[27][28][29].
Thermal imaging [30][31] is a passive noncontact method that can detect the radiation emitted from particular parts of the human body in the infrared (IR) range of the electromagnetic spectrum to measure the physiological signal using a thermal camera [32][33][34]. Thermal imaging-based methods extract vital signs by measuring temperature changes around the nostril area [35][36][37][38] as well as heat differences due to pulsating blood flow in the main superficial arteries at various regions such as the carotid artery in the neck [39][40] and temporal artery in the forehead [41][42]. However, both Doppler- and thermal imaging-based approaches are susceptible to noise and motion artefacts and constrain the movement of the subjects due to the high cost of the sensor, preventing saturation sampling of the environment. Their relatively low resolution limits the detection range and specificity to one subject. Moreover, these methods need exposed ROI and specialized hardware, making them costly [4]. They are also constrained to short-term monitoring and monitoring a single subject at a time. Additionally, Doppler-based methods may have biological effects on humans [43] with unknown future population risks if broadly adopted.
Using video camera imaging, a series of image and signal processing techniques are required to extract vital signs from the image. Figure 2 shows the basic framework, which includes data acquisition, ROI detection, raw signal extraction, noise artefact removal and vital sign extraction.
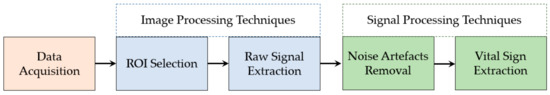
Figure 2. Block diagram of contactless monitoring system
Cardiorespiratory activity causes subtle motion in various parts of the human body that can be measured from video to extract vital signs. Numerous researchers have introduced different techniques to monitor vital signs using information extracted from motion. Nakazima et al. [44] proposed a contactless method based on optical flow analysis to extract RR from the video of whole body motion captured by a CCD (charge-coupled device) camera. Another optical flow analysis-based respiratory monitoring system was introduced by Frigola et al. [45] using videos of a subject’s chest movement recorded by video camera. Optical flow-based techniques have been found to be susceptible to motion artefacts caused by the subject’s movement, ambient light and unclear ROI. Computational complexity is a consideration for optical flow-based analysis compared to other processing options.
Photoplethysmography (PPG) is a non-invasive, low-cost, passive, optical technique first proposed by Hertzman et. al. in 1937 [46]. It can monitor three vital signs: HR, RR and SpO2. PPG is used extensively in biomedical, clinical and non-clinical fields due to its simple design and relatively low cost. PPG measures variations in the optical properties of transmitted or reflected light from the human skin caused by blood volume changes during cardiorespiratory activity. Blood absorbs light more than the adjacent tissue which causes subtle optical property variations of the skin because of the haemoglobin in blood. Generally, PPG can function either in a transmissive or a reflective mode; however, the first mode is limited to regions such as the ear lobes and fingertips. In the PPG technique, a dedicated light source is required to illuminate a part of the body and an optical sensor or photodetector connected to the skin is needed to sense the optical properties of the skin. Imaging photoplethysmography (iPPG) is basically remote or non-contact PPG; whereas for skin-contact, a PPG sensor and illuminator replace the camera. To detect PPG signals remotely, many researchers have considered a video camera as an optical sensor. Some studies have used a dedicated light source and others have considered just ambient light as a source of light. Nevertheless, a dedicated light source increases the hardware setup of experiments as well as starts to become invasive to the participant, particularly infants.
Because of its contactless sensing mode, iPPG can offer a comfortable method to monitor elderly people, infants, and patients with chronic pain, burnt skin, under dialysis, during and after surgery.
In nonclinical sectors such as home health care, fitness monitoring, sleep monitoring, polygraph, living skin detection, stress monitoring, driver monitoring, security, war zone, natural calamity, and animal research, the iPPG may play an important future role by monitoring vital signs.
Computer vision-based methods for vital signs measurement have been attracting increasing attention over the past few years. This paper gives a review of recent works in camera imaging-based methods, especially colour-based methods. First, numerous works based on motion- and colour-based methods have been discussed. Then, different aspects of colour-based methods, for example, motion artefacts, illumination variations, alternate sensors, different subjects, different vital signs, multiple ROIs, long distance and multiple persons have been reviewed. Additionally, potential applications of iPPG in both clinical and non-clinical sectors have been described. Moreover, we tried to identify the research gaps and challenges of the existing studies and gave some indications for future research. We believe that this paper will be a pathway for new researchers to understand and explore the gaps and challenges found in recent studies.