Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Daniela Dumitrescu | + 1545 word(s) | 1545 | 2021-11-04 06:52:02 | | | |
| 2 | Beatrix Zheng | Meta information modification | 1545 | 2021-11-05 03:27:15 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Dumitrescu, D. Preoperative Planning for Superior Mesenteric Artery Aneurysm. Encyclopedia. Available online: https://encyclopedia.pub/entry/15733 (accessed on 07 February 2026).
Dumitrescu D. Preoperative Planning for Superior Mesenteric Artery Aneurysm. Encyclopedia. Available at: https://encyclopedia.pub/entry/15733. Accessed February 07, 2026.
Dumitrescu, Daniela. "Preoperative Planning for Superior Mesenteric Artery Aneurysm" Encyclopedia, https://encyclopedia.pub/entry/15733 (accessed February 07, 2026).
Dumitrescu, D. (2021, November 04). Preoperative Planning for Superior Mesenteric Artery Aneurysm. In Encyclopedia. https://encyclopedia.pub/entry/15733
Dumitrescu, Daniela. "Preoperative Planning for Superior Mesenteric Artery Aneurysm." Encyclopedia. Web. 04 November, 2021.
Copy Citation
Surgical procedures on various artery aneurysms are difficult to perform and require careful preparation. We have developed a software platform, CardioCTNav, that can help in planning such procedures. The planning consists of a 3D rendering of the area of interest, virtual angiography, automated measurements, and virtual stent simulation.
artery aneurysm
planning software
automated measurements
stent simulation
1. Introduction
A mesenteric artery aneurysm is an aneurysm that occurs in either the inferior or superior mesenteric arteries that irrigate visceral organs like the stomach. Mesenteric artery aneurysms are rare, with a prevalence of 5–8% of all aneurysms, and have an annual incidence of between 0.01% and 0.2% [1]. Superior mesenteric artery aneurysms are the third most common true visceral aneurysms, often affecting the proximal 5 cm of the artery [2] and accounting for 14% of all visceral aneurysms [3]. They occur predominantly in men who are in the 5th decade of life. Aneurysmal degeneration of the superior mesenteric artery does not occur frequently, but when it does, it may result in mesenteric ischemia or rupture [4], which can initiate a potentially life-threatening condition [3]. In about 25% of cases, visceral aneurysms present as surgical emergencies [1], although the disease is often asymptomatic. They are an incidental finding in almost half of the patients [5]. Around 22% of patients with visceral aneurysms are diagnosed after rupture. Variable clinical manifestations pose the risk of misdiagnosis with a high mortality of 8.5–25% [6][7].
There is no known cause for aneurysm, but there are several risk factors that are known of that include: family history, male gender, an age > 65, history of smoking, high blood pressure, high cholesterol, atherosclerosis, or having a connective tissue disorder like Marfans or Ehlers-Danlos syndrome.
The diagnosis of a superior mesenteric artery aneurysm is made by computed tomographic angiography (CTA) or magnetic resonance (MR) and sometimes via an abdominal ultrasound examination. The suspicion of an aneurysm can be raised by a calcified wall on X-rays. In addition, the changes in the surrounding tissues and organs, like the signs of chronic pancreatitis or other events, might reveal the cause of the condition. By evaluating laboratory findings, imaging, and clinical symptoms, the factors influencing condition management should be determined and additional vascular changes might be discovered.
Imaging has a very important role not only in diagnosis but also in treatment planning because on these images is possible to determine multiple parameters for surgery like aneurysmal size, neck, access vessels, etc. Image processing software and virtual planning methods are already of great importance in medical practice. A long list could be made of either free-of-charge medical imaging software platforms, e.g., [8][9], semi-commercial, e.g., [10], or commercial ones. Characteristics used for the evaluation of such platforms could be the functionalities it offers (3D rendering, segmentation, measurements, virtual simulations, etc.), the price (from free-of-charge to very expensive), the training curve, hardware requirements, etc.
2. Analysis on Results
2.1. The Characterization of the Aneurysm and of the Anatomy on Real Patient CT Data
We applied the suggested pre-operatory planning procedure on CT data from a male patient aged 74. The scans were performed using a Siemens Somatom go. Top 128 slice machine [11], with contrast substance (ULTRAVIST 370 I.V.). The series used for planning took 647 slices at a distance of 0.99 mm each. The reconstructed 3D image had 655 × 512 × 647 voxels.
The results can be seen in, Figure 2, Figure 3, Figure 4, Figure 5, Figure 6, Figure 7, Figure 8 and Figure 9 and Table 1:
-
3D reconstruction—various tissues,
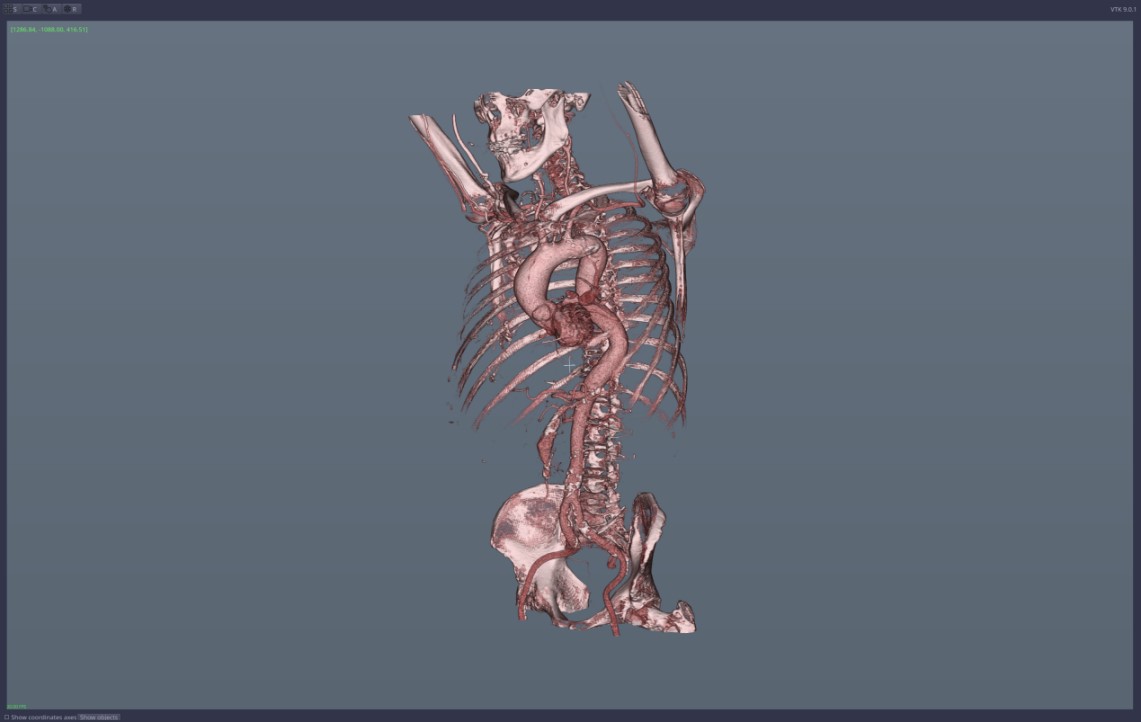
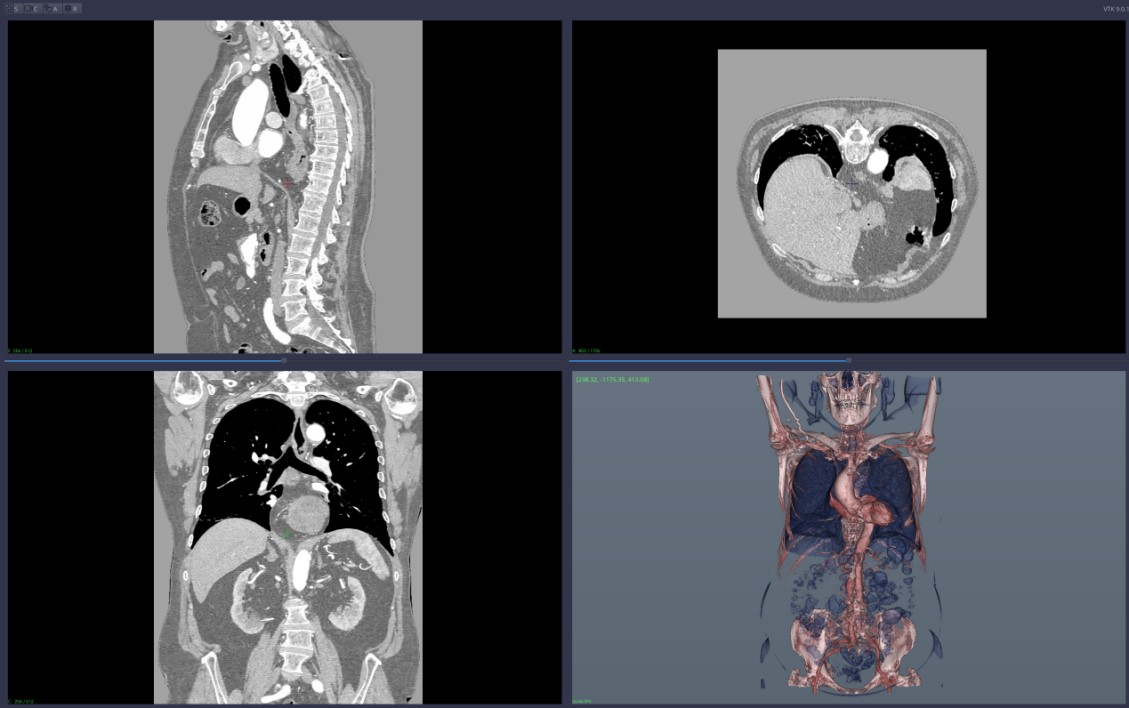 Figure 1: arteries and mesenteric artery aneurysm,
Figure 1: arteries and mesenteric artery aneurysm,-
Figure 2
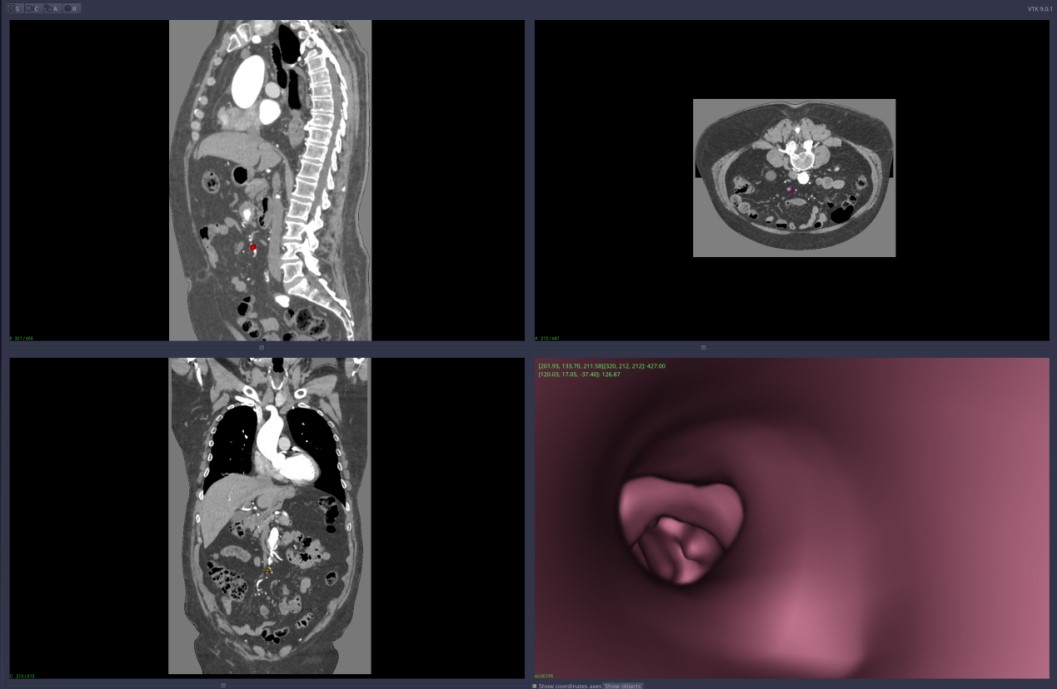
-
Virtual angiography—Figure 3,
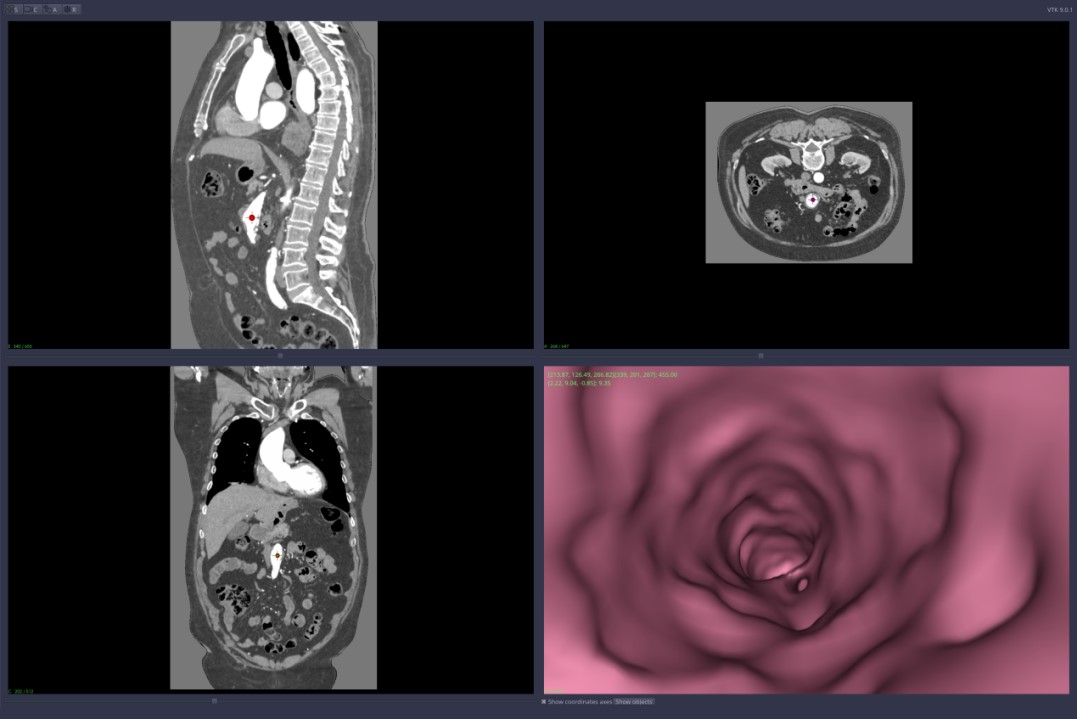
-
Figure 4,
-
Figure 5
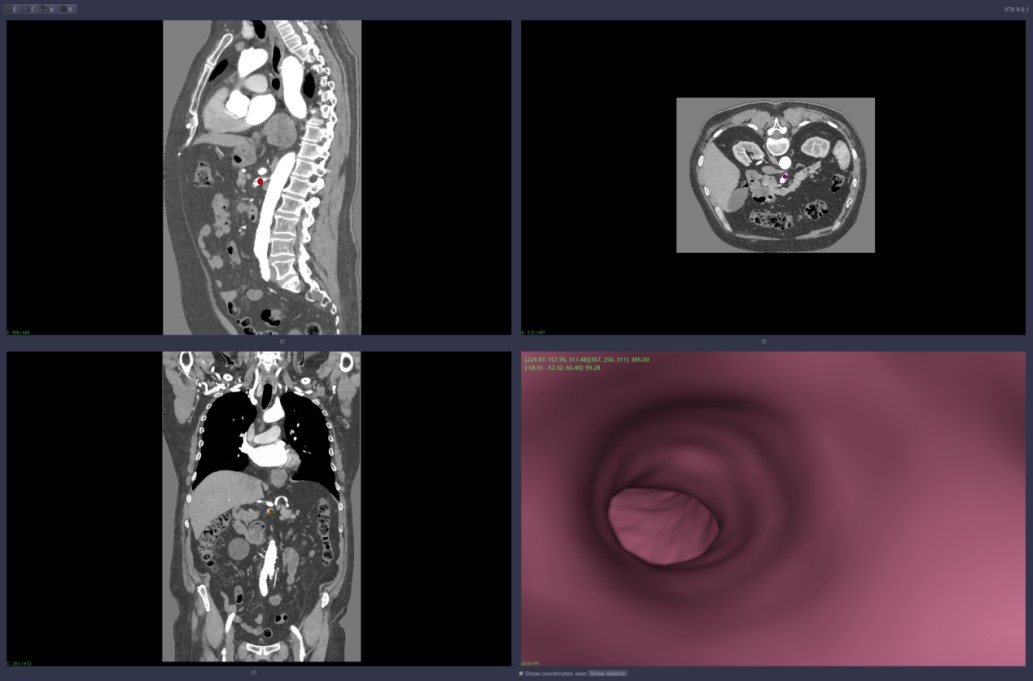
-
Figure 6
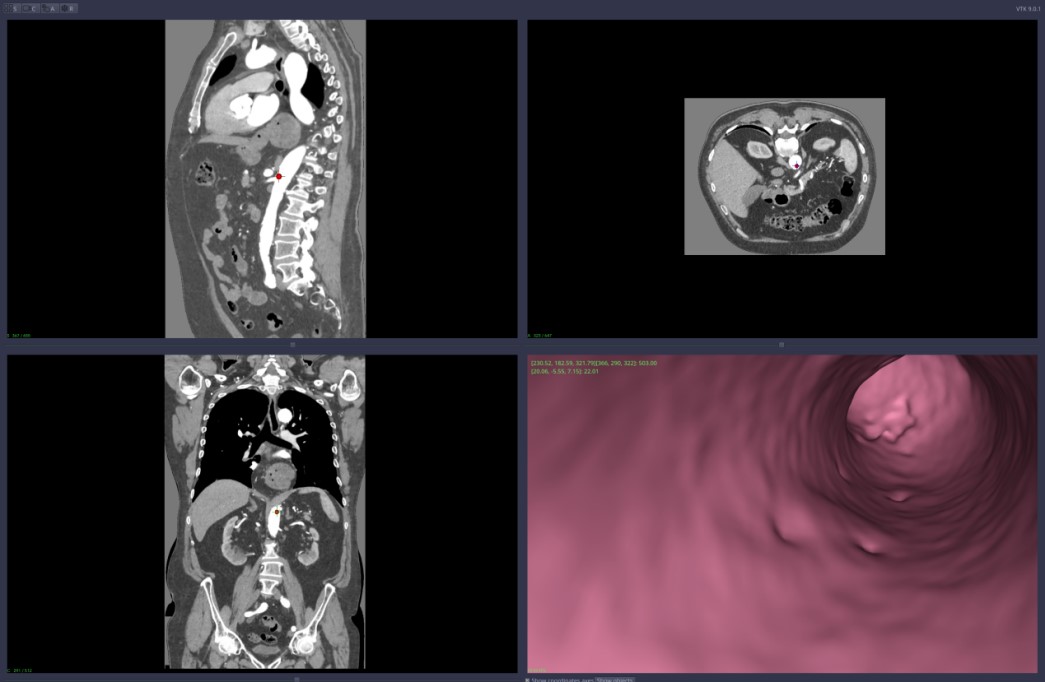
-
and Figure 7
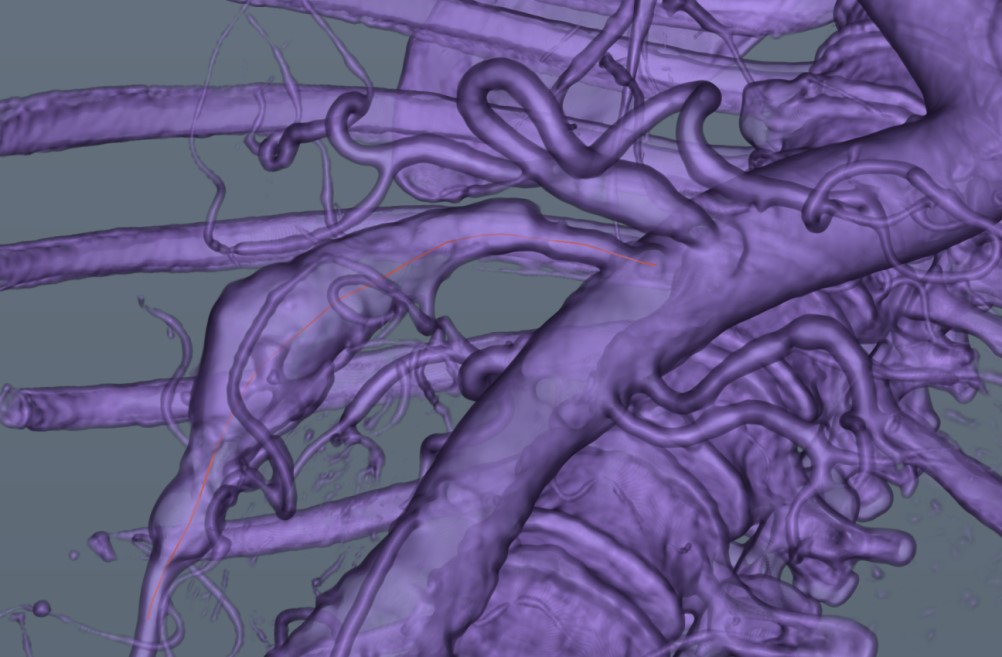
-
Measurements—Figure 8
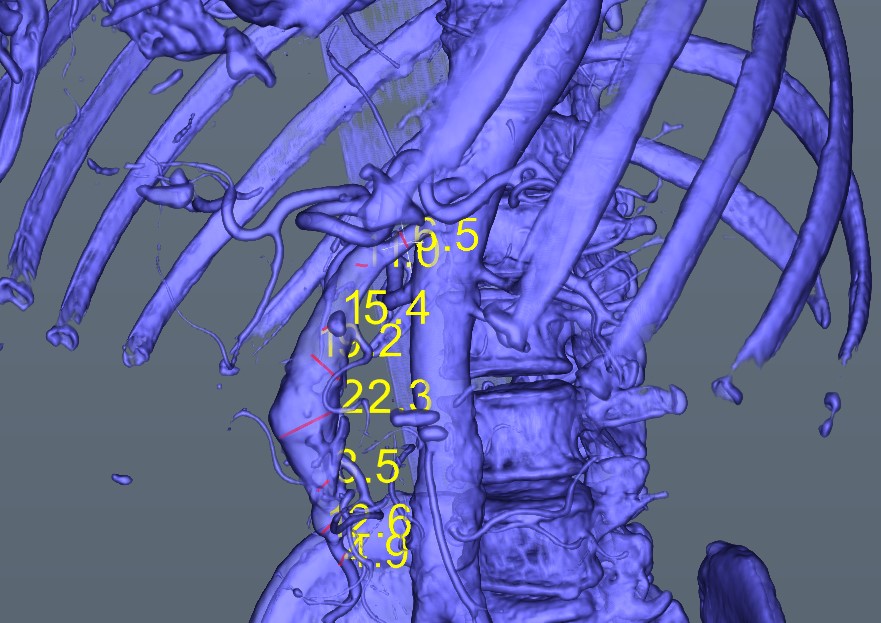
-
and Table 1
-
Table 1. Automated measurements along the aneurysm, opposite the direction of the blood flow, starting and ending with “healthy” zones.
Entry Point—Healthy Zone Aneurysm Zone Exit Point—Healthy Zone 4.9 12.6 13.5 22.3 19.2 15.4 11.0 6.5 -
Stent simulation (diameter, length)—Figure 9.
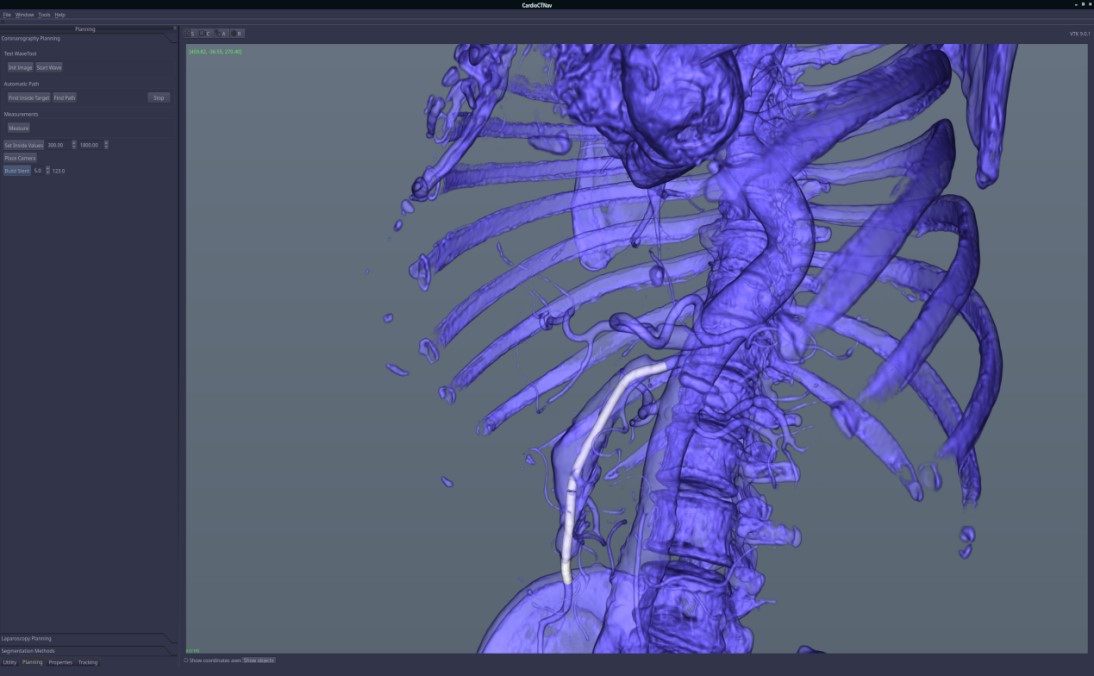
As you can determine from those figures, this particular aneurysm included the whole main part of the superior mesenteric artery, was fusiform in shape and involved all small intestinal branches, which makes the cases difficult to repair.
In addition, the stent graft required to cover the whole dilated area was 5 mm in diameter and 123 mm in length. We used as an example those stents available for renal artery stenting (for example, the Herculink Elite® stent made by Abbott Vascular, Santa Clara, CA, USA, with dimensions of 7.0 × 15 mm, 135 mm).
2.2. Planning Follow-Up for Surgery Procedures
Our vascular surgeon considered two main methods to repair a mesenteric aneurysm: open surgery or endovascular repair [12]. In the following paragraphs, we will briefly explain both methods. When considering a course of action, the vascular surgeon will decide the best method for a particular patient based on multiple factors, like the presence of collaterals, patient frailty, etc. However, both methods require a tubular prosthetic material to be introduced inside the aneurysm that has to be specially tailored to the patient’s physiology.
2.2.1. Open Surgery with Aneurysmectomy and Bypass or Interposition Graft
This method of revascularization is recommended as the first choice if bowel ischemia is present in patients undergoing an operation for rupture, or if preoperative symptoms or evaluation suggested mesenteric ischemia. More recent reports have shown good long-term results with an aneurysmectomy and bypass, or with an interposition graft [13][14].
The surgery consists of the interposition of two covered polyester stent grafts (two 7.0 × 57 mm Jostent peripheral stent grafts made by Jomed, Helsingborg, Sweden) with reimplantation of multiple side branches into the polyester interposition graft (see Figure 10). The polyester graft must have a good size to match the dilated proximal and distal native SMA at the area of the anastomosis; this also makes reimplantation of the side branches easier than using an autologous vein graft [15][16].
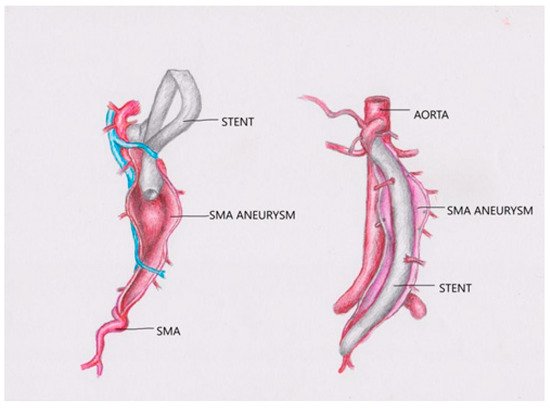
Figure 10. Endovascular repair illustration.
A clear 3D reconstruction and precise preoperative planning help the surgeon to determine exactly whether this procedure is adequate, to evaluate the type of stent technology needed for repair, and, most importantly, to reduce the time necessary when performing the procedure.
2.2.2. Endovascular Aneurysm Repair (EVAR) of Superior Mesenteric Artery Aneurysm
Endovascular treatment is safer than open surgery in patients with multiple comorbidities, such as severe cardiac or pulmonary disease. However, it should not be used when the cause of the aneurysm is suspected to be infectious. Alternative options include covered stent placement, coil embolization, liquid embolic agents, and thrombin injections [6]. Surgical options include an aneurysmectomy with grafting and/or transposition, aneurysmorrhaphy, and ligation [17].
The vascular interventional radiologist must consider several vascular factors, in addition to bowel viability, when reviewing a CT scan before the treatment of an SMA aneurysm. A femoral arterial approach is the most common, although a radial approach may be more direct when the aortic-mesenteric angle established in CT angiography is acute. Determining the number of aneurysms is important because individuals may have more than one aneurysm. The presence or absence of aneurysmal wall calcification can help to determine the patient’s risk of rupture. Stone et al. [18] found that all ruptures in their study occurred in noncalcified aneurysms. An aneurysm with a small neck, distal to the SMA origin, can be treated safely with coil embolization. The aneurysm must be packed tightly with coils to promote thrombosis. With a wide-necked aneurysm, stent-assisted coil placement, in which a bare-metal stent is deployed in the parent vessel and coils are delivered into the aneurysm sac via a microcatheter passed through the interstices of the stent, is an option.
The location of the aneurysm in the SMA must be considered, because it may be difficult to place a stent in an aneurysm near the point of origin owing to the lack of an adequate landing zone [6]. The stent should extend at least 1 cm proximally and distally to the aneurysm [6]. Large aneurysms may not be conducive to the use of a covered stent owing to instability in a large lumen and/or inadequate landing zones. The diameter and length of the stent can usually be determined accurately from the preoperative CT angiogram and may be compared with the diagnostic angiogram obtained before endovascular intervention. Self-expanding stents are available in various sizes of 5–16 mm and may require different sizes of sheaths, ranging from 5 F to 10 F [6].
For vessels with a smaller diameter, lower-profile stents are available and can be placed over a 0.018-inch wire. Covered stents are preferred, to completely exclude the aneurysm and prevent an endoleak, but bare metal stents can also be used successfully [19]. The stent should extend past the aneurysm neck without covering too many jejunal or ileal branches [17]. Branches arising from the aneurysm itself also must be considered. The tortuosity of the vessel at pre-procedure CT angiography should also be noted because self-expanding covered stents are effective in tortuous vessels but balloon-expandable stents may be used in proximal straight segments [6]. CT angiography with MPR and 3D rendering helps to delineate the proximity of branch vessels to the aneurysm. Studies by [17] have reported covering up to three jejunoileal branches without bowel ischemia. Careful consideration of clinical presentation, gastrointestinal and/or vascular multidetector CT findings, and patient comorbidities is crucial for proper patient selection and treatment.
Another option for the side branches is to use fenestrated endovascular aortic aneurysm repair (f-EVAR), which gives more options for the endovascular treatment of pararenal aortic aneurysms. The devices are individually customized to the patient’s vascular anatomy, especially to the morphology of the visceral vessels. In a typical fenestrated endovascular device design, the superior mesenteric artery (SMA) is involved, either having a large non-strut fenestration or a single wide scallop (10 mm in diameter).
References
- Ullery, B.W.; Lee, G.K.; Lee, J.T. Shuttering of the superior mesenteric artery during fenestrated endovascular aneurysm repair. J. Vasc. Surg. 2014, 60, 900–907.
- Yongcheng, X.; Yukun, L. The Fate of the Superior Mesenteric Artery in Fenestrated Endovascular Repair of Complex Abdominal Aortic Aneurysms. Vasc. Endovasc. Rev. 2019, 2, 38–39.
- Greenberg, R.K.; Haulon, S.; Lyden, S.P.; Srivastava, S.D.; Turc, A.; Eagleton, M.J.; Sarac, T.P.; Ouriel, K. Endovascular management of juxtarenal aneurysms with fenestrated endovascular grafting. J. Vasc. Surg. 2004, 39, 279–287.
- Tkalčić, L.; Budiselić, B.; Kovačević, M.; Knežević, S.; Kovačić, S.; Miletić, D.; Tomulić, V.; Kuhelj, D. Endovascular Management of Superior Mesenteric Artery (SMA) Aneurysm—Adequate Access is Essential for Success—Case Report. Pol. J. Radiol. 2017, 82, 379–383.
- Balderi, A.; Antonietti, A.; Ferro, L.; Peano, E.; Pedrazzini, F.; Fonio, P.; Grosso, M. Endovascular treatment of visceral artery aneurysms and pseudoaneurysms: Our experience. La Radiol. Med. 2012, 117, 815–830.
- Hemp, J.H.; Sabri, S.S. Endovascular Management of Visceral Arterial Aneurysms. Tech. Vasc. Interv. Radiol. 2015, 18, 14–23.
- Cochennec, F.; Riga, C.; Allaire, E.; Cheshire, N.; Hamady, M.; Jenkins, M.; Kobeiter, H.; Wolfe, J.; Becquemin, J.; Gibbs, R. Contemporary Management of Splanchnic and Renal Artery Aneurysms: Results of Endovascular Compared with Open Surgery from Two European Vascular Centers. Eur. J. Vasc. Endovasc. Surg. 2011, 42, 340–346.
- 3D Slicer Image Computing Platform. Available online: https://www.slicer.org/ (accessed on 10 October 2021).
- The Medical Imaging Interaction Toolkit (MITK). Available online: https://www.mitk.org (accessed on 10 October 2021).
- OsiriX Viewer. Available online: http://www.osirix-viewer.com (accessed on 10 October 2021).
- Siemens Somatom Go Top. Available online: https://www.siemens-healthineers.com/computed-tomography/single-source-ct-scanner/somatom-go-top (accessed on 1 November 2021).
- Carr, S.C.; Mahvi, D.M.; Hoch, J.R.; Archer, C.W.; Turnipseed, W.D. Visceral artery aneurysm rupture. J. Vasc. Surg. 2001, 33, 806–811.
- Ghariani, M.Z.; Georg, Y.; Ramirez, C.; Lebied, E.; Gaudric, J.; Chiche, L.; Kieffer, E.; Koskas, F. Long-Term Results of Surgical Treatment of Aneurysms of Digestive Arteries. Ann. Vasc. Surg. 2013, 27, 954–958.
- Sachdev, U.; Baril, D.T.; Ellozy, S.H.; Lookstein, R.A.; Silverberg, D.; Jacobs, T.S.; Carroccio, A.; Teodorescu, V.J.; Marin, M.L. Management of aneurysms involving branches of the celiac and superior mesenteric arteries: A comparison of surgical and endovascular therapy. J. Vasc. Surg. 2006, 44, 718–724.
- Arghami, A.; Krajewski, A.C.; Gloviczki, P.; Leduc, C.; Lin, P.T. Open staged repair of splenic and extensive superior mesenteric artery aneurysms. J. Vasc. Surg. 2019, 69, 1252–1256.
- Carr, S.C.; Pearce, W.H.; Vogelzang, R.L.; McCarthy, W.J.; Nemcek, A.A.; Yao, J.S. Current management of visceral artery aneurysms. Surgery 1996, 120, 627–634.
- Jiang, J.; Ding, X.; Su, Q.; Zhang, G.; Wang, Q.; Jian, W.; Wang, Z.; Hu, S. Therapeutic management of superior mesenteric artery aneurysms. J. Vasc. Surg. 2011, 53, 1619–1624.
- Stone, W.M.; Abbas, M.; Cherry, K.J.; Fowl, R.J.; Gloviczki, P. Superior mesenteric artery aneurysms: Is presence an indication for intervention? J. Vasc. Surg. 2002, 36, 234–237.
- Geana, R.C.; Pavel, P.; Nayyerani, R.; Kulcsar, I.; Tulin, A.; Honciuc, O.; Balescu, I.; Bacalbasa, N.; Stiru, O.; Iliescu, V.A.; et al. Successfully superior mesenteric artery stenting in operated type A aortic dissection complicated with delayed mesenteric malperfusion. SAGE Open Med. Case Rep. 2021, 9, 2050313X211021184.
More
Information
Contributor
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
1.1K
Entry Collection:
Hypertension and Cardiovascular Diseases
Revisions:
2 times
(View History)
Update Date:
05 Nov 2021
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No




