
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Amélie Marsot | + 2355 word(s) | 2355 | 2021-07-01 12:29:56 | | | |
| 2 | Lindsay Dong | + 51 word(s) | 2406 | 2021-07-27 04:48:33 | | |
Video Upload Options
Aminoglycosides are a class of antibiotics used as treatment for Gram-negative infections in patients hospitalized in intensive care units (ICUs). Life-threatening infections, often caused by Gram-negative bacteria [1,2], may lead to pathophysiological conditions, such as sepsis, influencing the pharmacokinetics (PK) of many drugs including antibiotics [3]. Antibiotic dosing regimens have been developed with the help of population pharmacokinetic (PopPK) modeling and simulation [11]. Multiple studies have established PopPK models to characterize PK parameters and to gain a better understanding of the variability of aminoglycoside clinical response based on ICU patients’ characteristics. These studies have used nonlinear mixed effects modeling to target and quantify the contribution of specific demographic and pathophysiological characteristics that may influence the aminoglycoside PK profile.
1. Introduction
2. Population PK Modeling of Aminoglycosides in the Intensive Care Unit
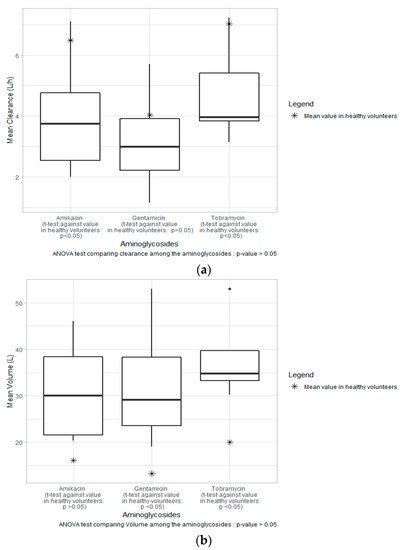
To treat severe infections, the administration of aminoglycosides in special populations has led to an increase in interest in aminoglycoside pharmacokinetics. Noticeably, a considerable number of PopPK models have been developed for ICU patients in the last decade [7][8][9][10][11][12][13][14][15][16][17][18]. In fact, Marsot et al. suggested in their review that single-compartment models could lead to an inaccurate estimation of aminoglycoside Vd [19]. Although median CL and Vd values were comparable across aminoglycosides, as shown in Figure 1, the parameter values tended to vary from one study to another for each drug. As described previously, ICU patients are prone to present additional comorbidities, such as cardiovascular dysfunction, sepsis, burns, or use of vasopressors, and/or develop complications, such as acute kidney injury (AKI) or, conversely, augmented renal clearance (ARC). These complications usually lead to divergence in PK values as compared to healthy patients [20]. As per Figure 1a, based on a similar dosing regimen, median CL values for all three drugs in this present study were generally lower as compared to values in healthy volunteers: 6.48 L/h, 4.03 L/h, and 7.02 L/h for amikacin, gentamicin, and tobramycin, respectively [21][22][23][24].
2.1. Major Covariates
2.1.1. Renal Function
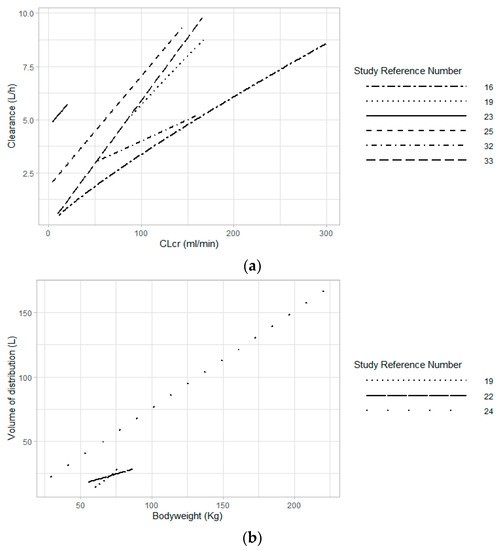
2.1.2. Bodyweight and Body Size
2.2. External Validation and Application
External validation is one of the strictest approaches in model testing and consists of applying a new dataset within a final model to determine the accuracy and reproducibility of the model and in which conditions it would be applicable. Different strategies and steps are possible in order to adequately evaluate models from the literature.
The conception of a meta-model for each aminoglycoside may also be feasible by including the characteristics (covariates, error models, initial estimates) from the best-performing models following external validation with an independent dataset. The development of this meta-model is, therefore, derived from the independent dataset while also being based on previously published PK models.
2.3. Simulation of Dosing Regimens
Firstly, amikacin dosing recommendations in critically ill patients without RRT were simulated in two articles [7][10]. In Boidin et al., an optimal initial amikacin dose of 3.5 g showed a better PTA for Cmax ≥ 64 mg/L and AUC0–24 ≥ 600 mg*h/L compared to the conventional 30 mg/kg of corrected bodyweight (CBW), considering an MIC of 8 mg/L [7]. It was suggested that an increase in the dosing interval up to 36 or 48 h might be feasible in critically ill patients with normal to moderate renal function. In fact, several recommendations were simulated on the basis of different values of the two significant covariates in their respective PopPK model, CLCG (10 mL/min to 250 mL/min), and BSA (1.5 m2 to 2.5 m2). As for Aréchiga-Alvarado et al., different daily dosing recommendations were simulated on the basis of three different MICs (4 mg/L, 8 mg/L, and 16 mg/L) and CLCR ranging from 60 mL/min to 200 mL/min [10]. Considering an MIC of 8 mg/L, a 30 mg/kg daily dose would be able to show a TAR over 80% and 75% for patients with CLCR lower than 140 mL/min and greater than 140 mL/min, respectively. As for amikacin dosing recommendations in critically ill patients RRT, two studies showed similar results in terms of optimal dosing regimens. In fact, Roger et al. and Carrié et al. suggested, respectively, that a dose of 25 mg/kg every 48 h and a dose ranging from 25 mg/kg and 30 mg/kg every 36 to 48 h were the most appropriate in order to maximize TAR for Cmax/MIC ≥ 8 and AUC0–24 ≥ 70 or AUC0–24 ≥ 75 with an MIC of 8 mg/L [8][9].
Secondly, gentamicin and tobramycin dosing recommendations in critically ill patients without RRT were simulated in five different articles [25][13][17][41][18]. Three out of the five studies established similar dosing recommendations with an initial starting dose of 6 to 7 mg/kg or a daily dose of 7 mg/kg [25][13][14]. The other study from Conil et al. provided a graphical representation of TAR for Cmax > 10 mg/L, Ctrough at 24h < 1 mg/L, and AUC between 80 and 125 mg*h/L according to different fixed dose regimens [17]. Their main takeaway was that these targets were not reached simultaneously in more than 45% of patients. Furthermore, only half of the population was able to attain the target for AUC with daily fixed dosages of 375 and 400 mg. The other study from Aarons et al. simulated dosing regimens on the basis of CLCR values [41]. All dosing regimens proposed were presented as a sequence: a fixed dose administered for the first 48 h with a dosing interval ranging from 8 h to 24 h depending on the CLCR. Following the first 48 h, a maintenance dose was to be administered as per the same dosing interval. The first period of 48 h was chosen according to the authors’ assumption that aminoglycoside concentration was to be detectable and, thus, have the possibility of dose adaptation [41]. As for patients under RRT, Teigen et al. demonstrated that, on the basis of PK/PD targets of Cmax ≥ 8 mg/L and AUC48 between 140 and 24 0 mg·h/L, three fixed starting doses (300 mg, 240 mg, 220 mg) prior to dialysis are related to a better TAR compared to post-dialysis administration [40]. Furthermore, Roberts et al. showed that a dosing of gentamicin 6 mg/kg every 48 h and administered 30 min prior to RRT (EDD-f in this situation) was able to achieve PK/PD targets compared to daily 7 mg/kg administration [15].
Results from simulations based on inter- and extrapolation should be interpreted cautiously considering the high variability observed in the estimation of PK parameters for all aminoglycosides.
3. Conclusions
References
- Bland, C.M.; Pai, M.P.; Lodise, T.P. Reappraisal of Contemporary Pharmacokinetic and Pharmacodynamic Principles for Informing Aminoglycoside Dosing. Pharmacother. J. Hum. Pharmacol. Drug Ther. 2018, 38, 1229–1238.
- Craig, W.A. Optimizing Aminoglycoside Use. Crit. Care Clin. 2011, 27, 107–121.
- Eliopoulos, G.M.; Drusano, G.L.; Ambrose, P.G.; Bhavnani, S.M.; Bertino, J.S.; Nafziger, A.N.; Louie, A. Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally. Clin. Infect. Dis. 2007, 45, 753–760.
- Germovsek, E.; Barker, C.I.; Sharland, M. What do I need to know about aminoglycoside antibiotics? Arch. Dis. Child.-Educ. Pract. Ed. 2017, 102, 89.
- Kumar, A.; Roberts, D.; Wood, K.E.; Light, B.; Parrillo, J.E.; Sharma, S.; Suppes, R.; Feinstein, D.; Zanotti, S.; Taiberg, L.; et al. Duration of hypotension before initiation of effective antimicrobial therapy is the critical determinant of survival in human septic shock. Crit. Care Med. 2006, 34, 1589–1596.
- Kanji, S.; Hayes, M.; Ling, A.; Shamseer, L.; Chant, C.; Edwards, D.J.; Edwards, S.; Ensom, M.H.H.; Foster, D.R.; Hardy, B.; et al. Reporting Guidelines for Clinical Pharmacokinetic Studies: The ClinPK Statement. Clin. Pharmacokinet. 2015, 54, 783–795.
- Boidin, C.; Bourguignon, L.; Cohen, S.; Roger, C.; Lefrant, J.-Y.; Roberts, J.A.; Allaouchiche, B.; Lepape, A.; Friggeri, A.; Goutelle, S. Amikacin Initial Dose in Critically Ill Patients: A Nonparametric Approach To Optimize a Priori Pharmacokinetic/Pharmacodynamic Target Attainments in Individual Patients. Antimicrob. Agents Chemother. 2019, 63, e00993-19.
- Roger, C.; Wallis, S.C.; Muller, L.; Saissi, G.; Lipman, J.; Lefrant, J.-Y.; Roberts, J.A. Influence of Renal Replacement Modalities on Amikacin Population Pharmacokinetics in Critically Ill Patients on Continuous Renal Replacement Therapy. Antimicrob. Agents Chemother. 2016, 60, 4901.
- Carrié, C.; Delzor, F.; Roure, S.; Dubuisson, V.; Petit, L.; Molimard, M.; Breilh, D.; Biais, M. Population Pharmacokinetic Study of the Suitability of Standard Dosing Regimens of Amikacin in Critically Ill Patients with Open-Abdomen and Negative-Pressure Wound Therapy. Antimicrob. Agents Chemother. 2020, 64, e02098-19.
- Aréchiga-Alvarado, N.A.; Medellín-Garibay, S.E.; Milán-Segovia, R.d.C.; Ortiz-Álvarez, A.; Magaña-Aquino, M.; Romano-Moreno, S. Population Pharmacokinetics of Amikacin Administered Once Daily in Patients with Different Renal Functions. Antimicrob. Agents Chemother. 2020, 64, e02178-19.
- Petitcollin, A.; Dequin, P.F.; Darrouzain, F.; Vecellio, L.; Boulain, T.; Garot, D.; Paintaud, G.; Ternant, D.; Ehrmann, S. Pharmacokinetics of high-dose nebulized amikacin in ventilated critically ill patients. J. Antimicrob. Chemother. 2016, 71, 3482–3486.
- Hodiamont, C.J.; Juffermans, N.P.; Bouman, C.S.C.; de Jong, M.D.; Mathôt, R.A.A.; van Hest, R.M. Determinants of gentamicin concentrations in critically ill patients: A population pharmacokinetic analysis. Int. J. Antimicrob. Agents 2017, 49, 204–211.
- Bos, J.C.; Prins, J.M.; Mistício, M.C.; Nunguiane, G.; Lang, C.N.; Beirão, J.C.; Mathôt, R.A.A.; van Hest, R.M. Population Pharmacokinetics with Monte Carlo Simulations of Gentamicin in a Population of Severely Ill Adult Patients from Sub-Saharan Africa. Antimicrob. Agents Chemother. 2019, 63, e02328-18.
- Hodiamont, C.J.; Janssen, J.M.; de Jong, M.D.; Mathôt, R.A.; Juffermans, N.P.; van Hest, R.M. Therapeutic Drug Monitoring of Gentamicin Peak Concentrations in Critically Ill Patients. Ther. Drug Monit. 2017, 39, 522–530.
- Roberts, J.A.; Field, J.; Visser, A.; Whitbread, R.; Tallot, M.; Lipman, J.; Kirkpatrick, C.M.J. Using population pharmacokinetics to determine gentamicin dosing during extended daily diafiltration in critically ill patients with acute kidney injury. Antimicrob. Agents Chemother. 2010, 54, 3635–3640.
- Gomes, A.; van der Wijk, L.; Proost, J.H.; Sinha, B.; Touw, D.J. Pharmacokinetic modeling of gentamicin in treatment of infective endocarditis: Model development and validation of existing models. PLoS ONE 2017, 12, e0177324.
- Conil, J.-M.; Georges, B.; Ruiz, S.; Rival, T.; Seguin, T.; Cougot, P.; Fourcade, O.; Pharmd, G.H.; Saivin, S. Tobramycin disposition in ICU patients receiving a once daily regimen: Population approach and dosage simulations. Br. J. Clin. Pharmacol. 2011, 71, 61–71.
- Hennig, S.; Standing, J.F.; Staatz, C.E.; Thomson, A.H. Population Pharmacokinetics of Tobramycin in Patients with and without Cystic Fibrosis. Clin. Pharmacokinet. 2013, 52, 289–301.
- Marsot, A.; Guilhaumou, R.; Riff, C.; Blin, O. Amikacin in Critically Ill Patients: A Review of Population Pharmacokinetic Studies. Clin. Pharmacokinet. 2017, 56, 127–138.
- Bagshaw, S.M.; Uchino, S.; Bellomo, R.; Morimatsu, H.; Morgera, S.; Schetz, M.; Tan, I.; Bouman, C.; Macedo, E.; Gibney, N.; et al. Septic Acute Kidney Injury in Critically Ill Patients: Clinical Characteristics and Outcomes. Clin. J. Am. Soc. Nephrol. 2007, 2, 431.
- Lode, H.; Grunert, K.; Koeppe, P.; Langmaack, H. Pharmacokinetic and Clinical Studies with Amikacin, a New Aminoglycoside Antibiotic. J. Infect. Dis. 1976, 134, S316–S322.
- Demczar, D.J.; Nafziger, A.N.; Bertino, J.S., Jr. Pharmacokinetics of gentamicin at traditional versus high doses: Implications for once-daily aminoglycoside dosing. Antimicrob. Agents Chemother. 1997, 41, 1115–1119.
- Garraffo, R.; Drugeon, H.B.; Dellamonica, P.; Bernard, E.; Lapalus, P. Determination of optimal dosage regimen for amikacin in healthy volunteers by study of pharmacokinetics and bactericidal activity. Antimicrob. Agents Chemother. 1990, 34, 614–621.
- Green, T.P.; Mirkin, B.L.; Peterson, P.K.; Sinaiko, A.R.; Ramsay, N.K.C.; O’Dea, R.F. Tobramycin Serum Level Monitoring in Young Patients with Normal Renal Function. Clin. Pharmacokinet. 1984, 9, 457–468.
- Rea, R.S.; Capitano, B.; Bies, R.; Bigos, K.L.; Smith, R.; Lee, H. Suboptimal Aminoglycoside Dosing in Critically Ill Patients. Ther. Drug Monit. 2008, 30, 674–681.
- Lim, A.K.H.; Mathanasenarajah, G.; Larmour, I. Assessment of aminoglycoside dosing and estimated glomerular filtration rate in determining gentamicin and tobramycin area under the curve and clearance. Intern. Med. J. 2015, 45, 319–329.
- Chin, P.K.L.; Florkowski, C.M.; Begg, E.J. The performances of the Cockcroft-Gault, Modification of Diet in Renal Disease Study and Chronic Kidney Disease Epidemiology Collaboration equations in predicting gentamicin clearance. Ann. Clin. Biochem. 2013, 50, 546–557.
- Pai, M.P.; Nafziger, A.N.; Bertino, J.S. Simplified Estimation of Aminoglycoside Pharmacokinetics in Underweight and Obese Adult Patients. Antimicrob. Agents Chemother. 2011, 55, 4006.
- Sunder, S.; Jayaraman, R.; Mahapatra, H.S.; Sathi, S.; Ramanan, V.; Kanchi, P.; Gupta, A.; Daksh, S.K.; Ram, P. Estimation of renal function in the intensive care unit: The covert concepts brought to light. J. Intensive Care 2014, 2, 31.
- Ruiz, S.; Minville, V.; Asehnoune, K.; Virtos, M.; Georges, B.; Fourcade, O.; Conil, J.-M. Screening of patients with augmented renal clearance in ICU: Taking into account the CKD-EPI equation, the age, and the cause of admission. Ann. Intensive Care 2015, 5, 49.
- Bragadottir, G.; Redfors, B.; Ricksten, S.-E. Assessing glomerular filtration rate (GFR) in critically ill patients with acute kidney injury—True GFR versus urinary creatinine clearance and estimating equations. Crit. Care 2013, 17, R108.
- Grootaert, V.; Willems, L.; Debaveye, Y.; Meyfroidt, G.; Spriet, I. Augmented Renal Clearance in the Critically Ill: How to Assess Kidney Function. Ann. Pharmacother. 2012, 46, 952–959.
- Ciarimboli, G.; Lancaster, C.S.; Schlatter, E.; Franke, R.M.; Sprowl, J.A.; Pavenstädt, H.; Massmann, V.; Guckel, D.; Mathijssen, R.H.J.; Yang, W.; et al. Proximal tubular secretion of creatinine by organic cation transporter OCT2 in cancer patients. Clin. Cancer Res. 2012, 18, 1101–1108.
- Zarowitz, B.J.; Robert, S.; Peterson, E.L. Prediction of Glomerular Filtration Rate Using Aminoglycoside Clearance in Critically Ill Medical Patients. Ann. Pharmacother. 1992, 26, 1205–1210.
- Mangoni, A.A.; Jackson, S.H.D. Age-related changes in pharmacokinetics and pharmacodynamics: Basic principles and practical applications. Br. J. Clin. Pharm. 2004, 57, 6–14.
- Triggs, E.; Charles, B. Pharmacokinetics and Therapeutic Drug Monitoring of Gentamicin in the Elderly. Clin. Pharmacokinet. 1999, 37, 331–341.
- Bauer, L.A.; Blouin, R.A. Gentamicin Pharmacokinetics. J. Am. Geriatr. Soc. 1982, 30, 309–311.
- Matzke, G.R.; Jameson, J.J.; Halstenson, C.E. Gentamicin Disposition in Young and Elderly Patients with Various Degrees of Renal Function. J. Clin. Pharmacol. 1987, 27, 216–220.
- Velissaris, D.; Karamouzos, V.; Marangos, M.; Pierrakos, C.; Karanikolas, M. Pharmacokinetic changes and dosing modification of aminoglycosides in critically ill obese patients: A literature review. J. Clin. Med. Res. 2014, 6, 227–233.
- Teigen, M.M.B.; Duffull, S.; Dang, L.; Johnson, D.W. Dosing of Gentamicin in Patients with End-Stage Renal Disease Receiving Hemodialysis. J. Clin. Pharmacol. 2006, 46, 1259–1267.
- Aarons, L.; Vozeh, S.; Wenk, M.; Weiss, P.; Follath, F. Population pharmacokinetics of tobramycin. Br. J. Clin. Pharm. 1989, 28, 305–314.
- Pai, M.P. Anti-infective Dosing for Obese Adult Patients: A Focus on Newer Drugs to Treat Methicillin-resistant Staphylococcus aureus Acute Bacterial Skin and Skin Structure Infections. Clin. Ther. 2016, 38, 2032–2044.
- Schneider, A.G.; Baldwin, I.; Freitag, E.; Glassford, N.; Bellomo, R. Estimation of fluid status changes in critically ill patients: Fluid balance chart or electronic bed weight? J. Crit. Care 2012, 27, 745.e7–745.e712.
- Alghanem, S.S.; Touw, D.J.; Thomson, A.H. Pharmacokinetic/pharmacodynamic analysis of weight- and height-scaled tobramycin dosage regimens for patients with cystic fibrosis. J. Antimicrob. Chemother. 2019, 74, 2311–2317.
- Crass, R.L.; Pai, M.P. Optimizing Estimated Glomerular Filtration Rate to Support Adult to Pediatric Pharmacokinetic Bridging Studies in Patients with Cystic Fibrosis. Clin. Pharmacokinet. 2019, 58, 1323–1332.
- Maskin, L.P.; Attie, S.; Setten, M.; Rodriguez, P.O.; Bonelli, I.; Stryjewski, M.E.; Valentini, R. Accuracy of Weight and Height Estimation in an Intensive Care Unit. Anaesth. Intensive Care 2010, 38, 930–934.
- Bloomfield, R.; Steel, E.; MacLennan, G.; Noble, D.W. Accuracy of weight and height estimation in an intensive care unit: Implications for clinical practice and research. Crit. Care Med. 2006, 34, 2153–2157.
- Gao, Z.; Chen, Y.; Guan, M.-X. Mitochondrial DNA mutations associated with aminoglycoside induced ototoxicity. J. Otol. 2017, 12, 1–8.




