
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Berend Beumer | + 5299 word(s) | 5299 | 2021-07-26 10:23:08 | | | |
| 2 | Nora Tang | -1750 word(s) | 3549 | 2021-07-27 07:40:31 | | |
Video Upload Options
For patients with early-stage hepatocellular carcinoma, it is important to know whether liver transplantation offers a survival benefit over liver resection. Patients receiving transplantation often have different characteristics in terms of their cancer stage and liver function compared to those being resected. This makes a comparison of the two treatment modalities challenging. This article presents a critical appraisal of the currently available literature. We not only provide a summary of the main results of individual articles but also describe their strengths and weaknesses, the relationships among them, and their trends. As a result, we suggest the regression discontinuity design for future studies that uses thresholds of a treatment guideline to help ensure that the groups are more comparable.
1. Introduction
2. Liver Resection vs. Liver Transplantation: Current Status
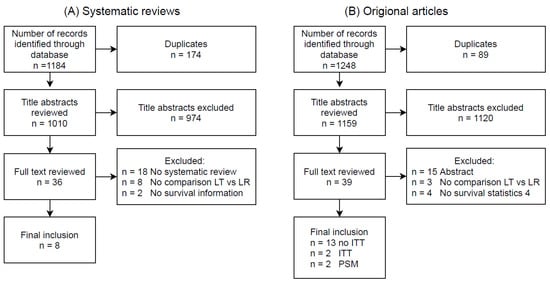
| Author | Year of Publication | Population | 5-Year OS | |||||
|---|---|---|---|---|---|---|---|---|
| Number of Studies | Number of Patients | Pooled OR (95%CI) |
p-Value | I2 | Conclusion | |||
| Non Intention-To-Treat | ||||||||
| Rahman [10] | 2012 | Non-ITT | 8 | 1769 | 0.62 (0.50–0.76) | <0.001 | 0 | In favour of LT |
| Dhir [9] | 2012 | Within MC | 10 | 1763 | 0.58 (0.36–0.94) | 0.027 | 78 | In favour of LT |
| Dhir [9] | 2012 | Within MC. Well compensated cirrhosis | 6 | 994 | 0.54 (0.38–0.77) | 0.001 | 32 | In favour of LT |
| Schoenberg [11] | 2017 | Within MC. No Child-Pugh class C | 8 | 1221 | 0.60 (0.45–0.78) | <0.001 | 70 | In favour of LT |
| Xu [12] | 2014 | 15 | 4102 | 0.54 (0.44–0.67) * | - | 40 | In favour of LT | |
| Zheng [13] | 2014 | 45 | 8288 | 0.56 (0.46–0.69) * | <0.001 | 65 | In favour of LT | |
| Intention-to-treat | ||||||||
| Rahman [10] | 2012 | ITT | 4 | 1310 | 1.19 (0.78–1.80) | 0.042 | 65 | In favour of LR |
| Dhir [9] | 2012 | ITT. Within MC | 6 | 1118 | 0.60 (0.29–1.24) | 0.166 | 83 | In favour of LT |
| Dhir [9] | 2012 | ITT. Within MC. Well compensated cirrhosis | 3 | 412 | 0.52 (0.30–0.91) | 0.022 | 31 | In favour of LT |
| Proneth [14] | 2014 | ITT | 7 | 1572 | 0.84 (0.48–1.48) | 0.055 | 84 | In favour of LT |
| Menahem [15] | 2017 | ITT | 9 | 1428 | 0.60 (0.32–1.02) | 0.060 | 80 | In favour of LT |
3. Novel Perspectives to Determine Outcome after LT vs. LR
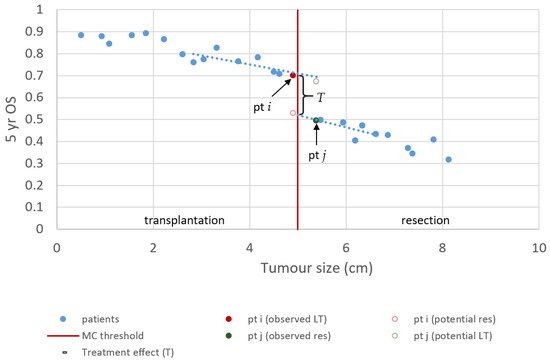
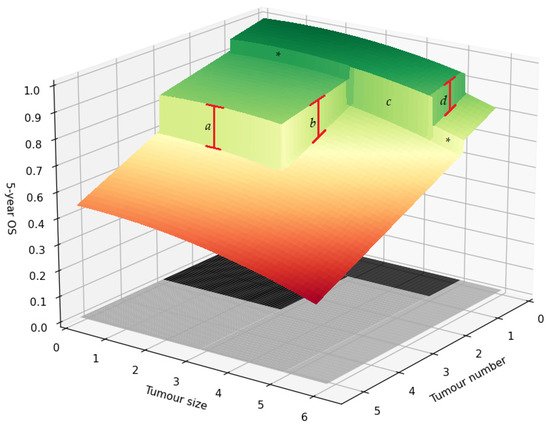
4. Conclusions
References
- European Association for The Study of The Liver. EASL clinical practice guidelines: Management of hepatocellular carcinoma. J. Hepatol. 2018, 69, 182–236.
- Heimbach, J.K.; Kulik, L.M.; Finn, R.S.; Sirlin, C.B.; Abecassis, M.M.; Roberts, L.R.; Zhu, A.X.; Murad, M.H.; Marrero, J.A. AASLD guidelines for the treatment of hepatocellular carcinoma. Hepatology 2018, 67, 358–380.
- Bhoori, S.; Schiavo, M.; Russo, A.; Mazzaferro, V. First-line treatment for hepatocellular carcinoma: Resection or transplantation? Transplant. Proc. 2007, 39, 2271–2273.
- Sala, M.; Fuster, J.; Llovet, J.M.; Navasa, M.; Solé, M.; Varela, M.; Pons, F.; Rimola, A.; García-Valdecasas, J.C.; Bru, C. High pathological risk of recurrence after surgical resection for hepatocellular carcinoma: An indication for salvage liver transplantation. Liver Transplant. 2004, 10, 1294–1300.
- Cherqui, D.; Laurent, A.; Mocellin, N.; Tayar, C.; Luciani, A.; Van Nhieu, J.T.; Decaens, T.; Hurtova, M.; Memeo, R.; Mallat, A. Liver resection for transplantable hepatocellular carcinoma: Long-term survival and role of secondary liver transplantation. Ann. Surg. 2009, 250, 738–746.
- Di Sandro, S.; Bagnardi, V.; Cucchetti, A.; Lauterio, A.; De Carlis, R.; Benuzzi, L.; Danieli, M.; Botta, F.; Centonze, L.; Najjar, M. From a philosophical framework to a valid prognostic staging system of the new “comprehensive assessment” for transplantable hepatocellular carcinoma. Cancers 2019, 11, 741.
- Cunningham, S.C.; Tsai, S.; Marques, H.P.; Mira, P.; Cameron, A.; Barroso, E.; Philosophe, B.; Pawlik, T.M. Management of early hepatocellular carcinoma in patients with well-compensated cirrhosis. Ann. Surg. Oncol. 2009, 16, 1820–1831.
- Belghiti, J.; Fuks, D. Liver resection and transplantation in hepatocellular carcinoma. Liver Cancer 2012, 1, 71–82.
- Dhir, M.; Lyden, E.R.; Smith, L.M.; Are, C. Comparison of outcomes of transplantation and resection in patients with early hepatocellular carcinoma: A meta-analysis. HPB 2012, 14, 635–645.
- Rahman, A.; Assifi, M.M.; Pedroso, F.E.; Maley, W.R.; Sola, J.E.; Lavu, H.; Winter, J.M.; Yeo, C.J.; Koniaris, L.G. Is resection equivalent to transplantation for early cirrhotic patients with hepatocellular carcinoma? A meta-analysis. J. Gastrointest. Surg. 2012, 16, 1897–1909.
- Schoenberg, M.B.; Bucher, J.N.; Vater, A.; Bazhin, A.V.; Hao, J.; Guba, M.O.; Angele, M.K.; Werner, J.; Rentsch, M. Resection or transplant in early hepatocellular carcinoma: A systematic review and meta-analysis. Dtsch. Ärzteblatt Int. 2017, 114, 519.
- Xu, X.-S.; Liu, C.; Qu, K.; Song, Y.-Z.; Zhang, P.; Zhang, Y.-L. Liver transplantation versus liver resection for hepatocellular carcinoma: A meta-analysis. Hepatobiliary Pancreat. Dis. Int. 2014, 13, 234–241.
- Zheng, Z.; Liang, W.; Milgrom, D.P.; Zheng, Z.; Schroder, P.M.; Kong, N.S.; Yang, C.; Guo, Z.; He, X. Liver transplantation versus liver resection in the treatment of hepatocellular carcinoma: A meta-analysis of observational studies. Transplantation 2014, 97, 227–234.
- Akcam, A.T.; Saritas, A.G.; Ulku, A.; Rencuzogullari, A. Oncological Outcomes of Hepatic Resection vs Transplantation for Localized Hepatocellular Carcinoma. Transplant. Proc. 2019, 51, 1147–1152.
- Aksoy, S.O.; Unek, T.; Sevinc, A.I.; Arslan, B.; Sirin, H.; Derici, Z.S.; Ellidokuz, H.; Sagol, O.; Agalar, C.; Astarcioglu, I. Comparison of Resection and Liver Transplant in Treatment of Hepatocellular Carcinoma. Exp. Clin. Transplant. 2020, 18, 712–718.
- Benjamin, A.J.; Baker, T.B.; Talamonti, M.S.; Bodzin, A.S.; Schneider, A.B.; Winschester, D.J.; Roggin, K.K.; Bentrem, D.J.; Suss, N.R.; Baker, M.S. Liver transplant offers a survival benefit over margin negative resection in patients with small unifocal hepatocellular carcinoma and preserved liver function. Surgery 2018, 163, 582–586.
- Grigorie, R.; Alexandrescu, S.; Smira, G.; Ionescu, M.; Hrehoreţ, D.; Braşoveanu, V.; Dima, S.; Ciurea, S.; Boeţi, P.; Dudus, I.; et al. Curative Intent Treatment of Hepatocellular Carcinoma-844 Cases Treated in a General Surgery and Liver Transplantation Center. Chirurgia (Buchar. Rom. 1990) 2017, 112, 289–300.
- Harimoto, N.; Yoshizumi, T.; Fujimoto, Y.; Motomura, T.; Mano, Y.; Toshima, T.; Itoh, S.; Harada, N.; Ikegami, T.; Uchiyama, H.; et al. Surgery for Hepatocellular Carcinoma in Patients with Child-Pugh B Cirrhosis: Hepatic Resection Versus Living Donor Liver Transplantation. World J. Surg. 2018, 42, 2606–2616.
- Kanneganti, M.; Mahmud, N.; Kaplan, D.E.; Taddei, T.H.; Goldberg, D.S. Survival Benefit of Liver Transplantation for Hepatocellular Carcinoma. Transplantation 2020, 104, 104–112.
- Krenzien, F.; Schmelzle, M.; Struecker, B.; Raschzok, N.; Benzing, C.; Jara, M.; Bahra, M.; Öllinger, R.; Sauer, I.M.; Pascher, A.; et al. Liver Transplantation and Liver Resection for Cirrhotic Patients with Hepatocellular Carcinoma: Comparison of Long-Term Survivals. J. Gastrointest. Surg. 2018, 22, 840–848.
- Lee, S.H.; Lee, J.S.; Na, G.H.; You, Y.K.; Kim, D.G. Immunohistochemical markers for hepatocellular carcinoma prognosis after liver resection and liver transplantation. Clin. Transplant. 2017, 31, e12852.
- Li, C.; Liu, J.Y.; Peng, W.; Wen, T.F.; Yan, L.N.; Yang, J.Y.; Li, B.; Wang, W.T.; Xu, M.Q. Liver resection versus transplantation for multiple hepatocellular carcinoma: A propensity score analysis. Oncotarget 2017, 8, 81492–81500.
- Li, Y.; Ruan, D.Y.; Jia, C.C.; Zhao, H.; Wang, G.Y.; Yang, Y.; Jiang, N. Surgical resection versus liver transplantation for hepatocellular carcinoma within the Hangzhou criteria: A preoperative nomogram-guided treatment strategy. Hepatobiliary Pancreat. Dis. Int. 2017, 16, 480–486.
- Lv, J.Y.; Zhang, N.N.; Du, Y.W.; Wu, Y.; Song, T.Q.; Zhang, Y.M.; Qu, Y.; Liu, Y.X.; Gu, J.; Wang, Z.Y.; et al. Comparison of liver transplantation and liver resection for hepatocellular carcinoma patients with portal vein tumor thrombus type i and type II. Yonsei Med. J. 2021, 62, 29–40.
- Zhang, K.; Chen, R.; Gong, X.; Gao, Y. Survival outcomes of liver transplantation versus liver resection among patients with hepatocellular carcinoma: A SEER-based longitudinal study. J. Formos. Med. Assoc. 2019, 118, 790–796.
- Eilard, M.S.; Naredi, P.; Helmersson, M.; Hemmingsson, O.; Isaksson, B.; Lindell, G.; Sandström, P.; Strömberg, C.; Rizell, M. Survival and prognostic factors after transplantation, resection and ablation in a national cohort of early hepatocellular carcinoma. HPB 2020, 23, 394–403.
- Proneth, A.; Zeman, F.; Schlitt, H.J.; Schnitzbauer, A.A. Is resection or transplantation the ideal treatment in patients with hepatocellular carcinoma in cirrhosis if both are possible? A systematic review and metaanalysis. Ann. Surg. Oncol. 2014, 21, 3096–3107.
- Menahem, B.; Lubrano, J.; Duvoux, C.; Mulliri, A.; Alves, A.; Costentin, C.; Mallat, A.; Launoy, G.; Laurent, A. Liver transplantation versus liver resection for hepatocellular carcinoma in intention to treat: An attempt to perform an ideal meta-analysis. Liver Transplant. 2017, 23, 836–844.
- Meyerovich, G.; Goykhman, Y.; Nakache, R.; Nachmany, I.; Lahat, G.; Shibolet, O.; Menachem, Y.; Katchman, H.; Wolf, I.; Geva, R.; et al. Resection vs Transplant Listing for Hepatocellular Carcinoma: An Intention-to-Treat Analysis. Transplant. Proc. 2019, 51, 1867–1873.
- Michelakos, T.; Xourafas, D.; Qadan, M.; Pieretti-Vanmarcke, R.; Cai, L.; Patel, M.S.; Adler, J.T.; Fontan, F.; Basit, U.; Vagefi, P.A.; et al. Hepatocellular Carcinoma in Transplantable Child-Pugh A Cirrhotics: Should Cost Affect Resection vs Transplantation? J. Gastrointest. Surg. 2019, 23, 1135–1142.
- Jiang, L.; Liao, A.; Wen, T.; Yan, L.; Li, B.; Yang, J. Living donor liver transplantation or resection for C hild-P ugh A hepatocellular carcinoma patients with multiple nodules meeting the Milan criteria. Transpl. Int. 2014, 27, 562–569.
- Harada, N.; Shirabe, K.; Ikeda, Y.; Korenaga, D.; Takenaka, K.; Maehara, Y. Surgical management of hepatocellular carcinoma in Child-Pugh class B cirrhotic patients: Hepatic resection and/or microwave coagulation therapy versus living donor liver transplantation. Ann. Transplant. 2012, 17, 11–20.
- Kaido, T.; Morita, S.; Tanaka, S.; Ogawa, K.; Mori, A.; Hatano, E.; Uemoto, S. Long-term outcomes of hepatic resection versus living donor liver transplantation for hepatocellular carcinoma: A propensity score-matching study. Dis. Markers 2015, 2015, 425926.
- Hoehn, R.S.; Wilson, G.C.; Wima, K.; Hohmann, S.F.; Midura, E.F.; Woodle, E.S.; Abbott, D.E.; Singhal, A.; Shah, S.A. Comparing living donor and deceased donor liver transplantation: A matched national analysis from 2007 to 2012. Liver Transplant. 2014, 20, 1347–1355.
- Vagefi, P.A.; Ascher, N.L.; Freise, C.E.; Dodge, J.L.; Roberts, J.P. Use of living donor liver transplantation varies with the availability of deceased donor liver transplantation. Liver Transplant. 2012, 18, 160–165.
- Shen, J.-Y.; Li, C.; Wen, T.-F.; Yan, L.-N.; Li, B.; Wang, W.-T.; Yang, J.-Y.; Xu, M.-Q.; Highness, T.N. Liver transplantation versus surgical resection for HCC meeting the Milan criteria: A propensity score analysis. Medicine 2016, 95, e5756.
- Shen, J.Y.; Li, C.; Wen, T.F.; Yan, L.N.; Li, B.; Wang, W.T.; Yang, J.Y.; Xu, M.Q.; Wen, J. Transplantation versus hepatectomy for HCC beyond the Milan criteria: A propensity score analysis. Int. J. Surg. 2017, 44, 33–42.
- Liu, J.B.; Baker, T.B.; Suss, N.R.; Talamonti, M.S.; Roggin, K.K.; Winchester, D.J.; Baker, M.S. Orthotopic liver transplantation provides a survival advantage compared with resection in patients with hepatocellular carcinoma and preserved liver function. Surgery 2017, 162, 1032–1039.
- Taefi, A.; Abrishami, A.; Nasseri-Moghaddam, S.; Eghtesad, B.; Sherman, M. Surgical resection versus liver transplant for patients with hepatocellular carcinoma. Cochrane Database Syst. Rev. 2013, CD006935.
- Earl, T.M.; Chapman, W.C. Hepatocellular carcinoma: Resection versus transplantation. Semin. Liver Dis. 2013, 33, 282–292.
- Mazzaferro, V.; Citterio, D.; Bhoori, S.; Bongini, M.; Miceli, R.; De Carlis, L.; Colledan, M.; Salizzoni, M.; Romagnoli, R.; Antonelli, B. Liver transplantation in hepatocellular carcinoma after tumour downstaging (XXL): A randomised, controlled, phase 2b/3 trial. Lancet Oncol. 2020, 21, 947–956.
- Thistlethwaite, D.L.; Campbell, D.T. Regression-discontinuity analysis: An alternative to the ex post facto experiment. J. Educ. Psychol. 1960, 51, 309.
- De Carlis, L.; Di Sandro, S.; Centonze, L.; Lauterio, A.; Buscemi, V.; De Carlis, R.; Ferla, F.; Sguinzi, R.; Okolicsanyi, S.; Belli, L.; et al. Liver-allocation policies for patients affected by HCC in Europe. Curr. Transplant. Rep. 2016, 3, 313–318.
- Bor, J.; Moscoe, E.; Mutevedzi, P.; Newell, M.-L.; Bärnighausen, T. Regression discontinuity designs in epidemiology: Causal inference without randomized trials. Epidemiology 2014, 25, 729.
- Mazzaferro, V.; Regalia, E.; Doci, R.; Andreola, S.; Pulvirenti, A.; Bozzetti, F.; Montalto, F.; Ammatuna, M.; Morabito, A.; Gennari, L. Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N. Engl. J. Med. 1996, 334, 693–700.
- Linden, A.; Adams, J.L. Combining the regression discontinuity design and propensity score-based weighting to improve causal inference in program evaluation. J. Eval. Clin. Pract. 2012, 18, 317–325.
- Imbens, G.; Kalyanaraman, K. Optimal bandwidth choice for the regression discontinuity estimator. Rev. Econ. Stud. 2012, 79, 933–959.
- Oldenburg, C.E.; Moscoe, E.; Bärnighausen, T. Regression discontinuity for causal effect estimation in epidemiology. Curr. Epidemiol. Rep. 2016, 3, 233–241.
- Hernán, M.A.; Robins, J.M. Causal Inference: What If; Chapman & Hall/CRC: Boca Raton, FL, USA, 2020.
- VanderWeele, T.J.; Hernan, M.A. Causal inference under multiple versions of treatment. J. Causal Inference 2013, 1, 1–20.




