
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Dror Paley | + 1845 word(s) | 1845 | 2021-07-12 07:40:45 | | | |
| 2 | Nora Tang | + 227 word(s) | 2072 | 2021-07-16 10:31:06 | | |
Video Upload Options
Limb lengthening for achondroplasia is controversial. Modern techniques of limb lengthening, using distraction osteogenesis, have been able to add significant length to the lower and upper limbs of children and adults with achondroplasia and hypochondroplasia. The long-term results of these treatments have remained unknown.
1. Introduction
Limb lengthening for achondroplasia is controversial [1][2][3]. Modern techniques of limb lengthening, using distraction osteogenesis, have been able to add significant length to the lower and upper limbs of children and adults with achondroplasia and hypochondroplasia [1][2][3][4][5][6]. There has been concern that while the increased stature may be obtained, the patients will eventually develop degeneration of their joints or other long-term complications [2][3]. The purpose of this study is to determine what are the long-term results of extensive limb lengthening (ELL) in achondroplasia and hypochondroplasia.
From 1987 to 1997, all the cases of ELL performed by the author were by two-segment lengthenings; bilateral tibial lengthening [4] (double-level lengthening with external fixation in most cases) followed by single-level bilateral femoral lengthening (Figure 1).

Since 1997, the author switched to simultaneous 4-segment lengthening of both femurs and both tibias at the same time using external fixation [5] The femurs were lengthened to a maximum goal of 8 cm and the tibias to 7 cm, for a total gain in height of 15 cm. This method was later modified to do bilateral femoral lengthening with implantable lengthening nails simultaneous with bilateral tibial lengthening with external fixation Since 2014, with the advent of shorter and smaller diameter implantable lengthening nails, 4-segment femur and tibia all implantable nail lengthenings were performed (Figure 2, right)
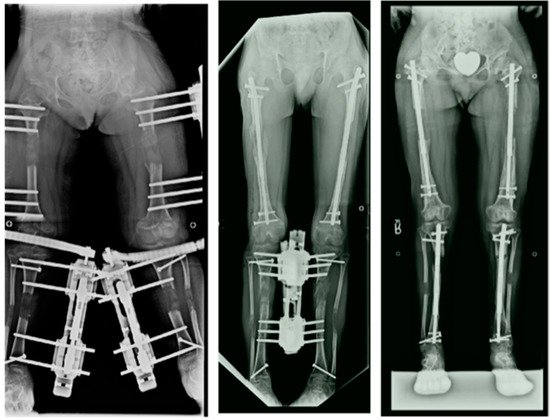
The age of starting the first lengthening was 12 yrs. In 1997, we also began to lengthen at age 7 yrs. for girls and 8 years for boys and referred to this as the juvenile-onset (age of first lengthening 7–11 yrs.). Patients who presented for the first lengthening at age 18 or over were referred to as adult-onset lengthening.
The cumulative goal of serial lengthenings was to bring the child to low normal height for their sex at skeletal maturity. To achieve this in achondroplasia for both boys and girls usually required between 30 and 40 cm total height gain by skeletal maturity. With two-segment lengthenings, total height gain was usually 25 cm with one bilateral tibial (15 cm) followed by one bilateral femoral lengthening (10 cm). If the 4-segment lengthening began at the juvenile age group, the lengthening goal was 5–6 cm lengthening in the femurs and 4–5 cm lengthening in the tibias for a total height gain of 10 cm.
4-segment limits the total lengthening per bone segment to no more than 8 cm, and 2-segment lengthening lengthens segments up to 15 cm in the tibia through double-level bone cuts and 10 cm through a single bone cut. This reduces pain, risk of nerve injury, and muscle contractures [7]. In the juvenile age group, there is also the consideration of growth inhibition following lengthening. It is felt that this will reduce the risk of growth inhibition at a young age.
2. Materials and Methods
This study was a retrospective x-ray and records review of all achondroplastic and hypochondroplastic patients treated by ELL by the author since 1987. Of those, only the ones whose follow-up is known until skeletal maturity and beyond and who completed all the serial lengthenings planned were included in this study. Of these patients, 75 completed all lengthenings planned and were followed into adulthood. Thirteen were lost to follow-up after completing all planned lengthenings and 18 have not completed all planned lengthenings and are currently under treatment or follow-up between lengthenings.
There were 48 females and 27 males. The clinical diagnosis was achondroplasia in 66 and hypochondroplasia in 9. The total amount of lengthening performed was an average of 27 cm (range 12–40 cm) for achondroplasia and an average of 17 cm (range 10–25 cm) for hypochondroplasia.
3. Results
Lengthening was performed as either 2-segment, bilateral femoral or bilateral tibial; or 4-segment, simultaneous bilateral femoral and tibial. 2-segment tibial followed by 2-segment femoral lengthening was done in 14 patients. Three patients had both 4-segment and 2-segment lengthenings at different times. Of the 4-segment lengthenings, 14 had three 4-segment lengthenings, 38 had two 4-segment lengthenings, and 12 had one 4-segment lengthening (Table 1).
| Type | 2-S × 2 | 2-S + 4-S | 4-S × 1 | 4-S × 2 | 4-S × 3 |
|---|---|---|---|---|---|
| Patients | 14 | 3 | 14 | 38 | 12 |
2-segment lengthenings were done either with external fixators (exfix) 9 times or with implantable lengthening nails (infix) four times. 4-segment lengthenings were done either with external fixators for both femurs and both tibias (all exfix) 107 times, external fixators on both tibias and implantable lengthening nails for both femurs (hybrid exfix-infix) five times, or both femurs and both tibias with implantable lengthening nails (all infix) 16 times. but two cases which were done with infix)
The average age at final follow-up was 26 years old (range 17–43 years). This represented a follow-up average of 13 years in the adult-onset group, vs. 10 years in the combined adolescent- and juvenile-onset groups (range 2–33 years) (Table 2).
| ELL Onset Age | Juvenile (7–11 yrs.) | Adolescent (12–17 yrs.) | Adult (18 yrs. & Older) |
|---|---|---|---|
| Patient # | 31 | 38 | 6 |
| M/F | 13/18 | 12/26 | 2/4 |
| Follow-up Age (yrs.) | 24 | 27 | 33 |
| Follow-up Age Range (range) | 17–35 | 17–46 | 23–43 |
While there were various complications during lengthening [4][8], for the purpose of this end-result study, we only tabulated the ones that led to permanent sequelae. One female patient, aged 16, developed paraparesis upon waking up from anesthesia at the time of removal of the external fixators after a successful second 2-segment lower-limb lengthening (total length gain was 25 cm). The paraparesis was treated by decompression and fusion and did improve, although she was left with some permanent lower-limb weakness. A second patient developed RSD after humeral lengthening.
Two of these were treated by periacetabular osteotomy immediately after completing lengthenings. A third patient went on to develop arthritis of one hip which will likely require a total hip replacement. No other patients developed degenerative joints of hips, knees, or ankles. Five patients developed spinal stenosis requiring surgery, either prior to, during treatment, or at a later date remote from the lengthening.
Patients started lengthening between ages 6–11 (juvenile-onset 31), 12–17 years (adolescent-onset 38), or 18 years and older (adult-onset 6) (Table 2 and Table 3).
| Juvenile/Adolescent | Achondroplasia | Method | Hyopchondroplasia | Method |
|---|---|---|---|---|
| ELL Goal | 30–40 cm | 15–25 cm | ||
| Age 7–11 yrs | F 5 cm + T 5 cm | 4-S | ±F-5 cm + T-5 cm | 4-S |
| Age12–13 yrs | F 5–8 cm + T 5–8 cm | 4-S | F 8 cm ± T 8 cm | 2-S or 4-S |
| Age 14–15 yrs | H 10–12 cm | 2-S | H 10 cm | 2-S |
| Age 15–16 yrs | F 5–8 cm + T 5–8 cm | 4-S | T 8 cm if previous F 2-S | 2-S if 2-S prior |
All patients had completed high school, and many went on to higher education. All patients had returned to normal activities of daily living. Many were also participating in sporting activities. The parents of the one patient who committed suicide were emphatic that his depression was not related to his previous lengthening surgery, which they felt was a very positive event in his life.
4. Discussions
Most focused on the short-term results and specific lengthening complications. 2015 from Korea [9] reported on 28 achondroplastic patients who underwent lengthening as adolescents (bilateral tibias followed by bilateral femurs). from the UK [10] reported on 10 achondroplastic children who lengthened a total average of 20 cm with good final results. Lee and Chow from Hong Kong [11] published on 8 patients with an average gain of 5.2 cm in the femurs and 5.8 cm gain in the tibias.
The average male height in achondroplasia is 132 cm with the low end of height range being 118 cm and the high end 146 cm [12][13]. The low end of normal height range for a male is 160 cm. The difference between the low-end, average, and high-end height for a male with achondroplasia vs. the low-end normal height for a male is 42 cm, 28 cm, and 14 cm respectively.
The average female height in achondroplasia is 125 cm with the low end of height range being 114 cm and the high end 138 cm. The low end of normal height range for a female is 150 cm. The difference between the low-end, average, and high-end height for a female with achondroplasia vs. the low-end normal height for a female is 36 cm, 25 cm, and 12 cm respectively.
Using Schiedel and Rodl’s [14] metanalysis as the range of height gain from lengthening from most studies (5.7–20.5 cm) suggests that few if any, achondroplastic patients achieve low normal height for their sex with the methods used by most authors (2-segment: bilateral femoral and bilateral tibial lengthening) [9][15][10][16][17][11]. It is clear that both the adolescent-onset as well as the juvenile-onset strategies gained sufficient height to reach the low normal height for their sex. ELL can add sufficient height to restore achondroplastic patients to normal adult heights for each sex in the majority of cases. and Peretti et al. recognized that the goal of lengthening should be to aim for a low normal height for the sex of the patient [18][19].
There are no published growth charts for hypochondroplasia. In this author’s experience, the final adult height in hypochondroplasia is 10–15 cm taller than in achondroplasia. In this study, the average length gain in hypochondroplasia was 16.8 cm All of these patients reached normal adult height for their sex.
Although we did not do quality of life (QOL) or psychologic analysis, prior studies of QOL have shown that despite frequent complications and despite the limited height gain as previously described, the QOL improved with ELL [20]. Batibay et al. showed that despite complications with lower limb lengthening the QOL scores improved significantly if humeral lengthening was also performed [21]. Fernandes et al. showed that limb-lengthening surgery helped patients in Spain integrate into society better than in the USA, where such surgery was less common [22]. Their patients were motivated by a combination of being able to overcome some physical shortcomings related to their short stature and short limbs and, at the same time, improving their social life.
The 4-segment lengthening method is currently our preferred lengthening strategy to achieve maximum total length gain in the shortest possible time without exceeding 8 cm lengthening in any single bone segment. While this strategy was originally used with 4-segment external fixation application, it can also be done with 4-segment implantable limb-lengthening devices or with hybrid 4-segment lengthening; two segments with external and two segments with internal devices. This is to reduce the risk of fat embolism syndrome from reaming 4 bones at one time. Most recently, the extramedullary lengthening with Precice nail or Precice plate has allowed us to use implantable lengthening nails in the femurs and lengthening plates in the tibias (Figure 3)
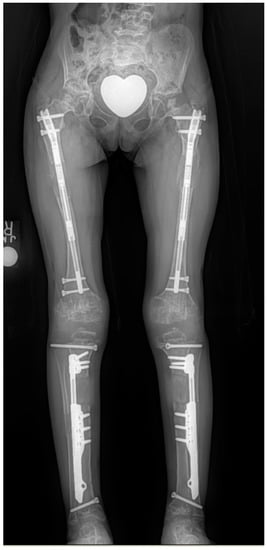
Since extra-medullary application does not involve reaming, two intramedullary nails and two extramedullary nails or plates can be placed at one time. When the goal is to gain less total length, a 2-segment strategy may be preferable to a 4-segment strategy. This is more applicable to ELL for hypochondroplasia, where the lengthening goal is only 16 cm on average. In contrast, when the lengthening goal is 25–40 cm as in achondroplasia, the 4-segment strategy is preferred.
This study confirms that ELL planning should consider the total height gains desired based on prediction of adult height using the achondroplasia growth charts [12][13][18]. To achieve the desired gain in height, the adolescent-onset strategy should be chosen if the goal is under 30 cm. The juvenile-onset strategy also has the advantage of not allowing the achondroplastic or hypochondroplastic child to fall too far behind their peers in height. Lengthening younger than age 7 in girls and 8 in boys risks growth inhibition and also is limited in total amount of length gain [23].
Drug therapy for achondroplasia is in clinical trials. The height gain from these new drugs will likely depend on the age the drugs are started. (e.g., girls achieve half their lower- and upper-limb growth by age 3 yrs. ; by age 1, both boys and girls have one-third of their total adult limb lengths). For this reason, it is likely that stature lengthening for children with achondroplasia will still be needed, but to a lesser extent, and only at skeletal maturity. This may involve one 2- or 4-segment lengthening with fully implantable lengthening devices.
References
- Paley, D. Current Techniques of Limb Lengthening. J. Pediatr. Orthop. 1988, 8, 73–92.
- Herzenberg, J.; Paley, D. Methods and strategies in limb lengthening and realignment for skeletal dysplasia. In Limb Lengthening: For Whom, When & How? Laron, Z., Mastragostino, S., Romano, C., Eds.; Freund Publishing, Ltd.: Tel Aviv, Israel, 1995; pp. 181–199.
- Herzenberg, J.E.; Paley, D. Stature lengthening: Skeletal dysplasia. In Limb Lengthening and Reconstruction Surgery; Rozbruch, S.R., Ilizarov, S., Eds.; Informa Healthcare: New York, NY, USA, 2007; pp. 575–596.
- Burghardt, R.D.; Yoshino, K.; Kashiwagi, N.; Yoshino, S.; Bhave, A.; Paley, D.; Herzenberg, J.E. Bilateral double level tibial lengthening in dwarfism. J. Orthop. 2015, 12, 242–247.
- Paley, D. Progress in and from Limb Lengthening. Current Progress in Orthopedics Tree Life Media; Kothari Medical Sub-scription Services, Pvt. Ltd.: Mumbai, India, 2014; pp. 55–80.
- Paley, D.; Harris, M.; Debiparshad, K.; Prince, D. Limb Lengthening by Implantable Limb Lengthening Devices. Tech. Orthop. 2014, 29, 72–85.
- Venkatesh, K.P.; Modi, H.N.; Devmurari, K.; Yoon, J.Y.; Anupama, B.R.; Song, H.R. Femoral lengthening in achondroplasia. Magnitude of Lengthening in Relation to Patterns of Callus, Stiffness of Adjacent Joints and Fracture. J. Bone Jt. Surg. Br. Vol. 2009, 91, 1612–1617.
- Paley, D. Problems, obstacles, and complications of limb lengthening by the Ilizarov technique. Clin. Orthop. Relat. Res. 1990, 250, 81–104.
- Park, K.W.; Garcia, R.A.N.; Rejuso, C.A.; Choi, J.W.; Song, H.R. Limb Lengthening in Patients with Achondroplasia. Yonsei Med. J. 2015, 56, 1656–1662.
- Donaldson, J.; Aftab, S.; Bradish, C. Achondroplasia and limb lengthening: Results in a UK cohort and review of the literature. J. Orthop. 2015, 12, 31–34.
- Lie, W.H.; Chow, W. Limb lengthening in short-stature patients using monolateral and circular external fixators. Hong Kong Med. J. 2009, 15, 280–284.
- Horton, W.A.; Rotter, J.I.; Rimoin, D.L.; Scott, C.I.; Hall, J.G. Standard growth curves for achondroplasia. J. Pediatr. 1978, 93, 435–438.
- Paley, D.; Matz, A.L.; Kurland, D.B.; Lamm, B.M.; Herzenberg, J.E. Multiplier Method for Prediction of Adult Height in Patients with Achondroplasia. J. Pediatr. Orthop. 2005, 25, 539–542.
- Schiedel, F.; Rödl, R. Lower limb lengthening in patients with disproportionate short stature with achondroplasia: A systematic review of the last 20 years. Disabil. Rehabil. 2012, 34, 982–987.
- Madhuri, V.; Chilbule, S.K.; Dutt, V. Limb lengthening in achondroplasia. Indian J. Orthop. 2016, 50, 397–405.
- Yasui, N.; Kawabata, H.; Kojimoto, H.; Ohno, H.; Matsuda, S.; Araki, N.; Shimomura, Y.; Ochi, T. Lengthening of the Lower Limbs in Patients with Achondroplasia and Hypochondroplasia. Clin. Orthop. Relat. Res. 1997, 344, 298–306.
- Aldegheri, R.; Dall’Orca, C. Limb Lengthening in Short Stature Patients. J. Pediatr. Orthop. Part B 2001, 10, 238–247.
- Vilarrubias, J.M.; Ginebreda, I.; Jimeno, E. Lengthening of the lower limbs and correction of lumbar hyperlordosis in achondro-plasia. Clin. Orthop. Relat. Res. 1990, 250, 143–149.
- Peretti, G.; Memeo, A.; Paronzini, A.; Marzorati, S. Staged Lengthening in the Prevention of Dwarfism in Achondroplastic Children. J. Pediatr. Orthop. Part B 1995, 4, 58–64.
- Kim, S.J.; Balce, G.C.; Agashe, M.V.; Song, S.H.; Song, H.R. Is Bilateral Lower Limb Lengthening Appropriate for Achondroplasia? Midterm Analysis of the Complications and Quality of Life. Clin. Orthop. Relat. Res. 2012, 470, 616–621.
- Batıbay, S.G.; Balcı, H.İ.; Bayram, S.; Chodza, M.; Göksoy, Ş.; Hürmeydan, Ö.M.; Kardelen, A.D.; Şen, C.; Kocaoğlu, M. Quality of Life Evaluation Following Limb Lengthening Surgery in Patients with Achondroplasia. Indian J. Orthop. 2020, 54, 39–46.
- Fernández, S.; Branscombe, N.R.; Gómez, Á.; Morales, J.F. Influence of the social context on use of surgical-lengthening and group-empowering coping strategies among people with dwarfism. Rehabil. Psychol. 2012, 57, 224–235.
- Song, S.-H.; Kim, S.E.; Agashe, M.V.; Lee, H.; Refai, M.A.; Park, Y.E.; Choi, H.J.; Park, J.H.; Song, H.R. Growth disturbance after lengthening of the lower limb and quantitative assessment of physeal closure in skeletally immature patients with achondroplasia. J. Bone Jt. Surg. Br. Vol. 2012, 94, 556–563.




