Cardiovascular disease (CVD) remains the primary cause of mortality and morbidity worldwide
[1]. The principal risk factor for developing CVD is relatively high plasma level of low-density lipoprotein cholesterol (LDLc)
[2][3][4]. Numerous epidemiological and clinical investigations have revealed that plasma level of high-density lipoprotein cholesterol (HDLc) correlates inversely with the risk of CVD
[5][6]. This association has been described by anti-atherogenic capacities of HDL, comprising its role in reverse cholesterol transport (RCT), in which cholesterol from peripheral tissues is transferred to the liver for excretion in bile and its ability to receive cholesterol from macrophages in the artery wall
[7][8]. However, Mendelian randomization studies
[9][10] and pharmacological interventional studies
[11][12] do not support the concept that HDLc directly reduces the risk of CVD
[8]. In addition, a retrospective analysis of large epidemiological studies showed that high HDLc concentration is associated with higher risk for CVD
[13][14]. These results support the hypothesis that HDL metabolism and functionality is more important than HDLc levels for CVD risk prediction
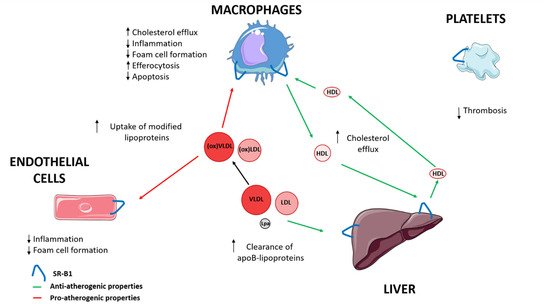
[14]. Acton et al. identified the scavenger receptor B class 1 (SR-B1) as a high-affinity HDL receptor, which facilitates the selective uptake of cholesterol esters (CE) in HDL into the liver
[15]. This receptor is also implicated in the plasma clearance of LDL, very low-density lipoprotein (VLDL) and lipoprotein(a) (Lp(a)), lipoproteins with pro-atherogenic properties
[16][17][18][19]. Therefore, SR-B1 is involved in cholesterol homeostasis, lipoprotein metabolism and atherosclerosis
[4]. In addition, SR-B1 plays a relevant role in HDL-mediated cellular signaling
[20], and might play a crucial role in the pathogenesis of non-alcoholic fatty liver disease (NAFLD)
[21], since this receptor is linked to dyslipidemia
[22].