Your browser does not fully support modern features. Please upgrade for a smoother experience.

Submitted Successfully!
Thank you for your contribution! You can also upload a video entry or images related to this topic.
For video creation, please contact our Academic Video Service.
| Version | Summary | Created by | Modification | Content Size | Created at | Operation |
|---|---|---|---|---|---|---|
| 1 | Stefania Arasi | + 2012 word(s) | 2012 | 2021-05-24 07:52:22 | | | |
| 2 | Vivi Li | + 487 word(s) | 2499 | 2021-05-26 10:13:44 | | |
Video Upload Options
We provide professional Academic Video Service to translate complex research into visually appealing presentations. Would you like to try it?
Cite
If you have any further questions, please contact Encyclopedia Editorial Office.
Arasi, S. Heiner Syndrome and Milk Hypersensitivity. Encyclopedia. Available online: https://encyclopedia.pub/entry/10101 (accessed on 08 February 2026).
Arasi S. Heiner Syndrome and Milk Hypersensitivity. Encyclopedia. Available at: https://encyclopedia.pub/entry/10101. Accessed February 08, 2026.
Arasi, Stefania. "Heiner Syndrome and Milk Hypersensitivity" Encyclopedia, https://encyclopedia.pub/entry/10101 (accessed February 08, 2026).
Arasi, S. (2021, May 26). Heiner Syndrome and Milk Hypersensitivity. In Encyclopedia. https://encyclopedia.pub/entry/10101
Arasi, Stefania. "Heiner Syndrome and Milk Hypersensitivity." Encyclopedia. Web. 26 May, 2021.
Copy Citation
Infants affected by Heiner syndrome (HS) display chronic upper or lower respiratory tract infections, including otitis media or pneumonia. Clinically, gastrointestinal signs and symptoms, anemia, recurrent fever and failure to thrive can be also present. Chest X-rays can show patchy infiltrates miming pneumonia. Clinical manifestations usually disappear after a milk-free diet. The pathogenetic mechanism underlying HS remains unexplained, but the formation of immune complexes and the cell-mediated reaction have been proposed. Patients usually outgrow this hypersensitivity within a few years.
allergy
anemia
cow’s milk
children
immunology
non-IgE-mediated food allergy
pneumonia
pulmonary hemosiderosis
pulmonary infiltrates
1. Introduction
Heiner syndrome (HS) is a rare food-induced hypersensitivity disease characterized by chronic respiratory symptoms with X-ray (XR) infiltrates, and the resolution of signs and symptoms after the removal of milk proteins. Other clinical manifestations include poor growth, gastrointestinal signs and symptoms, iron deficiency anemia and pulmonary hemosiderosis (PH). Precipitins to cow’s milk (CM) were also considered a useful aid in recognizing hypersensitivity to CM [1]. The literature concerning HS is restricted to a few case reports or series, although the disease has always been described at infant or pediatric age [2]. The definition of the disease is lacking and the diagnosis is often delayed, since its presentation is uncommon with dissimilar manifestations.
2. Age at Onset
The clinical onset of the disease has been described typically by the age of 1 month to 48 months, but it can develop even during the first 5 days of life, as reported by Torres et al. [3]. However, it can also appear later (the oldest patient was 5 years old) [4]. Nevertheless, there was a frequent delay in diagnosing this disease, due to its various modes of presentation and lack of standardized diagnostic criteria. The past medical history of affected children was always unremarkable. A family history of allergic disorders was often present. Differently from immediate-onset IgE-mediated CM allergy, HS did not display signs and symptoms before several days or weeks after CM consumption.
3. Etiology
Although HS is more likely to be induced by homogenized CM, the disease also may occur in some infants fed with CM-derived formula. Furthermore, it has been speculated that it can be related to non-IgE-mediated allergy to food proteins differently from CM at an older age (e.g., soy, egg, pork, wheat and peanut) [5][6]. In this context, a single case of PH hemosiderosis due to buckwheat has also been reported [7].
4. Clinical Characteristics
Respiratory features of the disease included persistent cough, dyspnea, tachypnea, wheezing, occasional sputum production and rales. The peculiarity of pneumonia in these case series was the refractoriness of antibiotic treatments. Of note, in most cases, the additional administration of anti-inflammatory drugs probably might have resolved hypersensitivity pneumonia or idiopathic PH (IPH). The most commonly described systemic clinical manifestations were intermittent fever, progressive anorexia and FTT. Inflammatory markers were usually found to be high. Eosinophilia and severe iron deficiency anemia were frequently described at blood count examination. Gastrointestinal manifestations were reported in about half of the patients and included frequent vomiting or diarrhea. Rarely, lymph node hypertrophy with hepatomegaly, splenomegaly and hypertrophied tonsils or adenoids were labeled [8]. Noticeably, lymphonodular hyperplasia in biopsy was found in a child with HS-manifesting hematochezia [9].
Clinically, the disease can be complicated with cardiopulmonary involvement, such as alveolar hypoventilation, massive acute PH, pulmonary hypertension and cor pulmonale, or nephrological ones, such as crescentic glomerulonephritis [10][11]. These characteristics contributed drastically to morbidity and emerged in situations of overdue diagnosis and management. In particular, a delayed manifestation of the disease is episodic hemoptysis, which may represent a PH with repeated episodes of intra-alveolar bleeding, hemosiderin deposition in alveolar macrophages, followed by the development of pulmonary fibrosis and severe anemia [10]. PH may occur as a primary disease of the lung (also called IPH) or secondary to cardiac diseases, bleeding disorders, collagen-vascular diseases or systemic vasculitis. IPH, if not treated, leads to progressive pulmonary fibrosis and may be lethal [12].
5. Pathogenesis and Immunological Implications
The exact mechanism that triggers HS is not fully understood. Feasibly, the formation of immune complexes is strongly suspected (Gell and Coombs type III reaction) and the cell-mediated reaction (Gell and Coombs type IV reaction) may contribute to the development of this challenging disease.
Some cases showed positive skin tests [13][8], high serum total IgE levels [8], high milk-specific IgE antibodies [11][5] or circulating immune complexes [13]. A significant increase of histamine and ECP in BAL several hours after a milk OFC was reported [3]. In one case report, deposits of immunoglobulins, complement, fibrin and milk protein antigens diffusely scattered were described on immunofluorescence studies of lung tissue biopsies [2]. It is probable that a cause concurring to HS is the aspiration of milk, in particular among patients with an uncoordinated swallowing mechanism, tracheal/esophageal anomaly or gastroesophageal reflux. However, in the paper of Boat et al., this condition was ruled out [8]. Concerning the data on delayed immunity, in some cases a delayed skin test response to intradermal test [13][8] or a lymphocyte response [10] was reported. Other authors postulated that milk antigens might trigger an immune complex reaction resulting in multiorgan abnormalities, such as pulmonary, gastrointestinal and renal ones. In fact, pulmonary and gastrointestinal signs and symptoms were frequently associated [14] and granular immuno-deposits have been demonstrated along the glomerular basement membrane in a child with crescentic glomerulonephritis and PH [11].
Most studies, mainly the oldest ones, characteristically found high titers of precipitins (likely immunoglobulins of class G) against bovine milk proteins in the patients’ sera, by using the Ouchterlony double-immunodiffusion technique [4][15][8][14]. However, it is not sufficiently explicable why some children develop precipitating antibodies to ingested protein and other children do not. Moreover, it is not known if these precipitins play a causative role in the disease. Children with precipitins usually have an increased incidence of recurrent respiratory tract diseases, anemia and hepatosplenomegalia. However, precipitating IgG antibodies to milk are not pathognomonic of the disease, since they have been found among around 1% of healthy children in the absence of clinical manifestations [4], and in 4% to 6% of children with chronic disorders, including celiac disease, cystic fibrosis, IgA deficiency, Down’s syndrome, Wisckott–Aldrich syndrome and Hurler’s syndrome [8]. Additionally, methods used for detecting precipitins are obsolete and reports on them are timeworn. Therefore, the role of these antibodies should be critically considered.
6. Pulmonary Modifications and Immunofluorescence Studies
Chest roentgenograms displayed variable patchy and transient infiltrates, frequently associated with areas of atelectasis, consolidation, reticular opacities, pleural thickening or hilar lymphadenopathy. The lung biopsy obtained in patients who had hemoptysis showed an abnormal accumulation of hemosiderin in the lungs, which resulted in alveolar hemorrhage or PH [2]. Among patients with anemia and hemoptysis, PH was verified by the demonstration of iron-laden macrophages by using Prussian Blue staining of bronchial aspirates or morning gastric washes [10].
7. Diagnostic Criteria
As described in detail above, in order to better stratify the level of evidence for the diagnosis, we are herein proposing the first structured diagnostic approach for the diagnosis of HS to the best of our knowledge. We auspicate that this approach may allow clinicians to stratify patients with a clinical history consistent with the suspicion of HS in probable (criteria A + B) or convincing (criteria A + B + C) HS (Figure 1). According to our criteria, only 6 out of 61 patients had a convincing clinical diagnosis of HS, in 25 patients the clinical diagnosis was probable and in the others the HS diagnosis was doubtful (Table 1). Due to the heterogeneity in the methodologies applied for laboratory tests and missing reporting/lack of data, we decided to exclude laboratory parameters from the diagnostic criteria. We suggest in the future that milk-specific IgG tests with current diagnostic methods (i.e., immunoenzymatic), in the case of suspected HS, could be studied. Nevertheless, further points remain questionable in our proposed diagnostic approach. First, some cases of occurrence of signs and symptoms during exclusive maternal breastfeeding were reported (e.g., in three out of seven cases in Heiner et al. [13], leading to the question of whether or not minimal quantities of CM passing in breast milk are capable of inducing a clinical response through an IgG-mediated mechanism in the infant). As a second observation, one case of resolution of signs and symptoms without dietary restriction has been described (one out of seven patients from Heiner et al.). Again, a real, controlled OFC of milk was reported only in 6 cases [13][8][14] and a recurrence of clinical manifestations was reported in a further 6 cases (although without details on exact timing of the symptoms’ onset) based only on clinical history [15][17][8][11][5][18], for a total of 12 cases. Moreover, in some cases [11][5] pharmacological therapy was associated to the CM elimination diet, making it difficult to differentiate the effect of each single treatment. Spontaneous resolution of signs and symptoms also occurred in some cases of HS [1]. Furthermore, some studies did not report on the follow-up and specifically on the outcome of any CM reintroduction. In conclusion, even if in a few cases a convincing diagnosis can be made using specific criteria, certainty is lacking due to the incomplete clinical and imaging monitoring of the OFC and the lack of control cases.
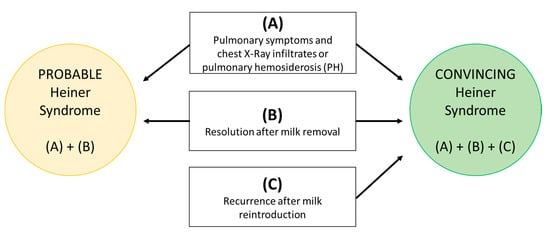
Figure 1. Proposed approach for Heiner syndrome diagnosis.
Table 1. Characteristics of the included studies of Heiner syndrome.
| Authors, Year | Country | n. Cases | Age at Onset (Months) | Signs/Symptoms | Lung Radiologic Infiltrates |
Pulmonary Hemosiderosis |
Hemosiderosis Diagnosis | Milk Precipitins |
Delayed Hypersensitivity | Allergic Sensitization to Milk [sIgE and/or skin prick test (SPT)] |
Improvement Upon Milk Avoidance | Recurrence Upon Milk Reintroduction |
|
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | Heiner, 1960 | USA | 7 | 1–17 | chronic cough (7/7); wheezing (7/7); chronic rhinitis (7/7); frequent fever (7/7); frequent earache (6/7); diarrhea (6/7); vomiting (5/7); hemoptysis (4/7) |
yes, recurrent |
yes (5/7) | gastric or bronchial aspirates (4/7); pulmonary needle biopsy (1/7) | yes | intradermal test (ID) late response pos (4/7) | ID +ve (7/7) | yes (6/6) | yes (2/6) |
| 2 | Holland, 1962 | USA | 22 | 4–12 | respiratory disease; failure to thrive (FTT); anemia; splenomegaly; hepatomegaly |
non specified (NS) | NS | NS | yes | NS | NS | yes (22/24 on milk-free diet) | NS |
| 3 | Chang, 1969 | USA | 1 | 9 | FTT ; anemia; chronic recurrent lung disease |
yes | NS | NS | yes | NS | NS | yes | doubtful, based on clinical history (CH) |
| 4 | Archer, 1971 | England | 1 | 13 | iron-deficiency anemia; lethargy; pallor; bloody vomit; severe cardiac failure; hemoptysis |
yes | yes | needle biopsy | no | NS | SPT –ve | yes | doubtful, based on CH |
| 5 | Boat, 1975 | USA | 6 | 7–48 | idiopathic chronic or recurrent pulmonary disease; upper respiratory symptoms; FTT (3/6); frequent regurgitation and watery stools (1/6). SOF (1/6): Iron deficiency (5/6); Anemia (4/6); Eosinophilia (4/6); right ventricular hypertrophy (3/6); adenoid hypertrophy (3/6) | yes (6/6) | yes (5/6) | gastric washing or bronchoalveolar lavage (BAL) |
yes (6/6) | 4 ID delayed response |
total IgE –ve (6/6); SPT +ve (5/6) | yes (5/6); 1/6 loss of data | yes (1/6) |
| 6 | Stafford, 1977 | USA | 7 | 8–48 | wheezing (5/9); chronic rhinitis (3/9); large adenoids/tonsils (4/9); anemia (4/9); gastrointestinal symptoms (4/9); eosinophilia (6/9) | yes (7/9) | yes (3/9) | gastric washing and BAL | yes (9/9) | lymphocyte response (3/3) |
SPT +ve (6/9), sIgE +ve (5/8) | NS | NS |
| 7 | Fossati, 1992 | Italy | 1 | 7 years | anemia; respiratory symptoms | yes | yes | NS | yes | NS | NS | yes | NS |
| 8 | Torres, 1996 | Spain | 1 | 0 (5 days) | vomiting with blood; respiratory failure; restrictive miocardiopathy; anemia; eosinophilia | yes (chest X-Ray, CXR) | yes | BAL | NS | NS | neg | yes | symptoms not reported |
| 9 | Moissidis, 2005 | USA | 8 | 4–29 | cough (7/9); wheezing (3/9); dyspnea (1/9); hemoptysis (2/9); nasal congestion (3/9); recurrent otitis media (OM) (3/9); recurrent fever (4/9); gastrointestinal symptoms (5/9); in 7/8; hematochezia (1/9); FTT (2/9); eosinophilia in 5/8 | yes (9/9) | yes (1/9) | NS | yes (6/6) | NS | sIgE (1/3), SPT (1/2) | yes (8/9) | positive challenge (3/3) |
| 10 | Sigua, 2013 | USA | 1 | 12 | persistent cough; progressive anorexia; intermittent fever; weight loss; iron deficiency anemia | yes (CXR) | no | BAL | yes | NS | sIgE –ve | yes | doubtful, based on CH |
| 11 | Yavuz, 2014 | Turkey | 1 | 36 | respiratory distress; hemoptysis; recurrent bronchitis; FTT; iron deficiency anemia; eosinophilia; increased inflammatory index; | yes (CXR, CT) | yes | BAL | NS | NS | sIgE +ve | yes | doubtful, based on CH |
| 12 | Mourad, 2015 | USA | 1 | 17 | severe anemia; respiratory distress | yes (CXR) | yes | BAL | IgG | NS | sIgE +ve | yes | doubtful, based on CH |
| 13 | Alsukhon, 2017 | USA | 1 | 2 | FTT; recurrent diarrhea; persistent cough; tachypnea; high inflammatory markers | yes (CXR) | NS | NS | IgG4 | NS | sIgE –ve | yes | NS |
| 14 | Ojuawo, 2019 | Nigeria | 1 | 4 | FTT; cough; dyspnea; wheeze; rhinitis; gastrointestinal symptoms; anemia | yes (CXR) | NS | NS | NS | NS | NS | yes | NS doubtful, based on CH |
| 15 | Koc, 2019 | Turkey | 1 | 6 | massive hemoptysis; hematemesis; deep anemia | yes (CXR, CT) | yes | gastric washing | NS | NS | NS | yes | NS |
| 16 | Liu, 2020 | China | 1 | 4 | respiratory failure; hematochezia; diarrhea; elevated WBC and C-reactive protein | yes (CXR, CT) | no | sputum or fasting gastric fluid | NS | NS | –ve | yes | NS |
Abbreviations: BAL, bronchoalveolar lavage; CH, clinical history; CT, computerized tomography; CXR, chest X-Ray; ID, intradermal test; NS, non specified; SPT, skin prick test; –ve, negative; +ve, positive.
8. Differential Diagnosis
In the differential diagnosis (DD) bronchial asthma, chronic aspiration, acute and chronic lower respiratory tract infections, including fungal ones, cystic fibrosis, foreign body, hypersensitivity pneumonitis, bronchopulmonary aspergillosis, secondary PH and IPH should be considered [14]. Cystic fibrosis essentially can be excluded by a normal chloride level on the sweat test and second line tests if there is a strong suspicion. Infectious causes should be ruled out with tuberculin skin test and available microbial tests, and empiric antibiotic treatments characteristically are inefficacious. Thereafter, a vasculitis or autoimmune disorder can be considered. The characteristic pulmonary hemorrhage attacks cannot be enlightened by modest bronchial asthma. The lack of chronic inhalant exposure and BAL examination can rule out hypersensitivity pneumonitis. Bronchopulmonary aspergillosis is unlikely if skin reactivity to Aspergillus antigens is negative or precipitating serum antibodies to A. fumigatus are absent. No hemorrhagic focus nor foreign bodies can be found on bronchoscopy. In particular, DD should consider IPH, that includes the classic triad hemoptysis, radiologic lung infiltrate and iron deficiency anemia, having a more severe course and prognosis [19]. Moreover, IPH occurs in older children, and it is rarely associated with gastrointestinal symptoms [20] (Table 2).
Table 2. Differential diagnosis between Heiner syndrome (HS) and idiopathic pulmonary hemosiderosis (IPH).
| HS | IPH | |
|---|---|---|
| Age | infants or young children | older children/adults |
| Hemosiderosis | often | always |
| GI symptoms | often | rarely |
| Precipitins | yes | no |
| Response to diet | yes | no |
| Prognosis | good | variable |
9. Natural History
The disease’s effects were reversible by stopping CM consumption. In fact, signs and symptoms could last within a time range of 5 to 21 days after the CM withdrawal. Before CM reintroduction, some children showed spontaneous tolerance to pasteurized or boiled CM [4]. Reoccurrence of clinical manifestations was reported with CM reintroduction [13][15][17][3][14][5]. However, it is believed that patients usually definitively outgrow this hypersensitivity, and they can tolerate CM within a few years [14][21][22].
10. Treatment
Clinical improvement with strict elimination of CM proteins sustains the diagnosis of HS. Infants may be fed by a milk substitute, such as extensively hydrolyzed protein formula, soy-based formula or synthesized free amino acid formula. Improvement of signs and symptoms occurs in few days and X-ray images in weeks. When a confirmatory CM reintroduction was performed [14], respiratory clinical manifestations also occurred in days or weeks. An early exclusion of the triggering food from the diet is crucial, since chronic PH induces pulmonary fibrosis which can be fatal [17]. However, recovery may occur also without exclusion of the culprit food (e.g., 1/7 in Heiner’s report [13]).
Even if the most striking criterion of HS is the dramatic response to the exclusion diet, initially, in some cases, appropriate treatment, e.g., bronchodilators, antihistamines, systemic or inhaled steroids and iron, may be needed. A short cycle of oral corticosteroids remains the first-line therapy for acute attacks. In more severe cases of HS, other immunomodulatory treatments may be helpful, such as hydroxychloroquine, azathioprine or cyclophosphamide. On the contrary, antibiotic therapy seems not to be useful.
References
- Heiner, D.C.; Sears, J.W.; Kniker, W.T. Multiple precipitins to cow’s milk in chronic respiratory disease. A syndrome including poor growth, gastrointestinal symptoms, evidence of allergy, iron deficiency anemia, and pulmonary hemosiderosis. Am. J. Dis. Child 1962, 103, 634–654.
- Lee, S.K.; Kniker, W.T.; Cook, C.D.; Heiner, D.C. Cow’s milk-induced pulmonary disease in children. Adv. Pediatr. 1978, 25, 39–57.
- Torres, M.J.; Girón, M.D.; Corzo, J.L.; Rodriguez, F.; Moreno, F.; Perez, E.; Blanca, M.; Martinez-Valverde, A. Release of in-flammatory mediators after cow’s milk intake in a newborn with idiopathic pulmonary hemosiderosis. J. Allergy Clin. Immunol. 1996, 98, 1120–1123.
- Holland, N.H.; Hong, R.; Davis, N.C.; West, C.D. Significance of precipitating antibodies to milk proteins in the serum of infants and children. J. Pediatr. 1962, 61, 181–195.
- Mourad, A.A.; Parekh, H.; Bahna, S.L. A 17-month-old patient with severe anemia and respiratory distress. Allergy Asthma Proc. 2015, 36, 506–511.
- Heiner, D.C.; University of California Los Angeles, Torrance, CA, USA. Personal Verbal Communication, 2015.
- Agata, H.; Kondo, N.; Fukutomi, O.; Takemura, M.; Tashita, H.; Kobayashi, Y.; Shinoda, S.; Nishida, T.; Shinbara, M.; Orii, T. Pulmonary hemosiderosis with hypersensitivity to buckwheat. Ann. Allergy Asthma Immunol. 1997, 78, 233–237.
- Boat, T.F.; Polmar, S.H.; Whitman, V.; Kleinerman, J.I.; Stern, R.C.; Doeshuk, C.F. Hyperactivity to cow milk in young children with pulmonary hemosiderosis and cor pulmonale secondary to nasopharyngeal obstruction. J. Pediatr. 1975, 87, 23–29.
- Liu, X.-Y.; Huang, X.-R.; Zhang, J.-W.; Xiao, Y.-M.; Zhang, T. Hematochezia in a Child with Heiner Syndrome. Front. Pediatr. 2020, 7, 551.
- Stafford, H.A.; Polmar, S.H.; Boat, T.F. Immunologic Studies in Cow’s Milk-induced Pulmonary Hemosiderosis. Pediatr. Res. 1977, 11, 898–903.
- Yavuz, S.; Karabay-Bayazıt, A.; Yılmaz, M.; Gönlüşen, G.; Anarat, A. Crescentic glomerulonephritis in a child with Heiner syndrome. Turk. J. Pediatr. 2014, 56, 661–664.
- Soergel, K.H.; Sommers, S.C. Idiopathic pulmonary haemosiderosis and related syndromes. Am. J. Med. 1962, 32, 499–511.
- Heiner, D.C.; Sears, J.W. Chronic respiratory disease associated with multiple circulating precipitins to cow’s milk. Am. J. Dis. Child. 1960, 100, 500–502.
- Moissidis, I.; Chaidaroon, D.; Vichyanond, P.; Bahna, S.L. Milk-induced pulmonary disease in infants (Heiner syndrome). Pediatr. Allergy Immunol. 2005, 16, 545–552.
- Chang, C.H.; Wittig, H.J. Heiner’s syndrome. Radiology 1969, 92, 507–508.
- Alsukhon, J.; Leonov, A.; Elisa, A.; Koon, G. P327 Food-induced pulmonary hemosiderosis. Ann. Allergy Asthma Immunol. 2017, 119, S77.
- Archer, J. Idiopathic Pulmonary Hemosiderosis Treated with a Milk-free Diet. Proc. Roy. Soc. Med. 1971, 64, 1217–1218.
- Ojuawo, A.B.; Ojuawo, O.B.; Aladesanmi, A.O.; Adio, M.O.; Abdulkadir, M.B.; Mokuolu, O.A. Heiner Syndrome: An uncommon cause of failure to thrive. Malawi Med. J. 2019, 31, 227–229.
- Saha, B.K. Idiopathic pulmonary hemosiderosis: A state of the art review. Respir. Med. 2021, 176, 106234.
- Taytard, J.; Nathan, N.; De Blic, J.; Fayon, M.; Epaud, R.; Deschildre, A.; Troussier, F.; Lubrano, M.; Chiron, R.; Reix, P.; et al. New insights into pediatric idiopathic pulmonary hemosiderosis: The French RespiRare® cohort. Orphanet J. Rare Dis. 2013, 8, 161.
- Lee, E.J.; Heiner, D.C. Allergy to Cow Milk. Pediatrics Rev. 1986, 7, 7.
- Williams, S.; Craver, R.D. Cow’s milk-induced pulmonary hemosiderosis. J. State Med Soc. Off. Organ State Med Soc. 1989, 141, 19–22.
More
Information
Subjects:
Nutrition & Dietetics
Contributor
MDPI registered users' name will be linked to their SciProfiles pages. To register with us, please refer to https://encyclopedia.pub/register
:
View Times:
1.8K
Revisions:
2 times
(View History)
Update Date:
23 Jun 2021
Notice
You are not a member of the advisory board for this topic. If you want to update advisory board member profile, please contact office@encyclopedia.pub.
OK
Confirm
Only members of the Encyclopedia advisory board for this topic are allowed to note entries. Would you like to become an advisory board member of the Encyclopedia?
Yes
No
${ textCharacter }/${ maxCharacter }
Submit
Cancel
Back
Comments
${ item }
|
More
No more~
There is no comment~
${ textCharacter }/${ maxCharacter }
Submit
Cancel
${ selectedItem.replyTextCharacter }/${ selectedItem.replyMaxCharacter }
Submit
Cancel
Confirm
Are you sure to Delete?
Yes
No




