Avalanche accidents are common in mountain regions and approximately 100 fatalities are counted in Europe each year. The average mortality rate is about 25% and survival chances are mainly determined by the degree and duration of avalanche burial, the patency of the airway, the presence of an air pocket, snow characteristics, and the severity of traumatic injuries. The most common cause of death in completely buried avalanche victims is asphyxia followed by trauma. Hypothermia accounts for a minority of deaths; however, hypothermic cardiac arrest has a favorable prognosis and prolonged resuscitation and extracorporeal rewarming are indicated.
- avalanche
- avalanche burial
- cardiac arrest
- emergency medicine
- hypothermia
1. Introduction and Epidemiology
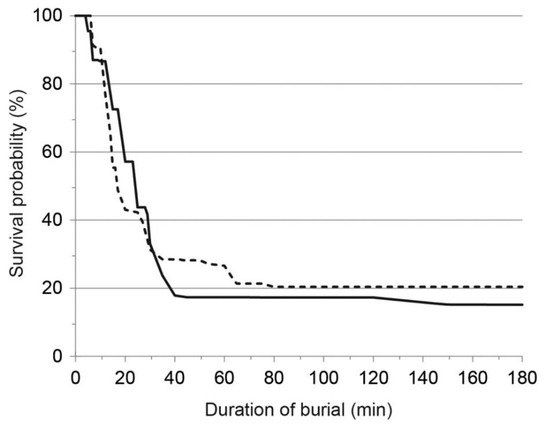
2. Pathophysiology
3. On-Site Management
3.1. Guidelines for On-Site Management
3.2. Companion and Organized Rescue
3.3. Extrication, Initial Assessment and Monitoring
3.4. Trauma Management
3.5. Airway Management and Ventilation
This entry is adapted from the peer-reviewed paper 10.3390/ijerph181910234
References
- Techel, F.; Jarry, F.; Kronthaler, G.; Mitterer, S.; Nairz, P.; Pavšek, M.; Valt, M.; Darms, G. Avalanche fatalities in the European Alps: Long-term trends and statistics. Geogr. Helvetica 2016, 71, 147–159.
- Brugger, H.; Durrer, B.; Elsensohn, F.; Paal, P.; Strapazzon, G.; Winterberger, E.; Zafren, K.; Boyd, J. Resuscitation of avalanche victims: Evi-dence-based guidelines of the international commission for mountain emergency medicine (ICAR MEDCOM): Intended for physi-cians and other advanced life support personnel. Resuscitation 2013, 84, 539–546.
- Atkins, D. 10 years of avalanche rescues in the United States, 2003/04 to 2012/13. Avalanche Rev. 2015, 33, 22–24.
- Schweizer, J.; Lütschg, M. Characteristics of human-triggered avalanches. Cold Reg. Sci. Technol. 2001, 33, 147–162.
- Rainer, B.; Frimmel, C.; Sumann, G.; Brugger, H.; Kinzl, J.F.; Lederer, W. Correlation between avalanche emergencies and avalanche danger forecast in the alpine region of Tyrol. Eur. J. Emerg. Med. 2008, 15, 43–47.
- Strapazzon, G.; Schweizer, J.; Chiambretti, I.; Brodmann Maeder, M.; Brugger, H.; Zafren, K. Effects of Climate Change on Ava-lanche Accidents and Survival. Front Physiol. 2021, 12, 639433.
- Strapazzon, G.; Paal, P.; Schweizer, J.; Falk, M.; Reuter, B.; Schenk, K.; Gatterer, H.; Grasegger, K.; Cappello, T.D.; Malacrida, S.; et al. Effects of snow properties on humans breathing into an artificial air pocket–An experimental field study. Sci. Rep. 2017, 7, 17675.
- Brugger, H.; Durrer, B.; Adler-Kastner, L.; Falk, M.; Tschirky, F. Field management of avalanche victims. Resuscitation 2001, 51, 7–15.
- Haegeli, P.; Falk, M.; Brugger, H.; Etter, H.-J.; Boyd, J. Comparison of avalanche survival patterns in Canada and Switzerland. Can. Med. Assoc. J. 2011, 183, 789–795.
- Van Tilburg, C.; Grissom, C.K.; Zafren, K.; McIntosh, S.; Radwin, M.I.; Paal, P.; Haegeli, P.; Smith, W.W.R.; Wheeler, A.R.; Weber, D.; et al. Wilderness Medical Society Practice Guidelines for Prevention and Management of Avalanche and Nonavalanche Snow Burial Accidents. Wilderness Environ. Med. 2017, 28, 23–42.
- Falk, M.; Brugger, H.; Adler-Kastner, L. Avalanche survival chances. Nature 1994, 368, 21.
- Procter, E.; Strapazzon, G.; Cappello, T.D.; Zweifel, B.; Würtele, A.; Renner, A.; Falk, M.; Brugger, H. Burial duration, depth and air pocket explain avalanche survival patterns in Austria and Switzerland. Resuscitation 2016, 105, 173–176.
- Strapazzon, G.; Brugger, H.; Paal, P.; Brown, D. Reconsidering the air pocket around mouth and nose as a positive outcome predictor in completely buried avalanche victims. Resuscitation 2020, 152, 208–209.
- Strapazzon, G.; Putzer, G.; Cappello, T.D.; Falla, M.; Braun, P.; Falk, M.; Glodny, B.; Pinggera, D.; Helbok, R.; Brugger, H. Effects of hypothermia, hypoxia, and hypercapnia on brain oxygenation and hemodynamic parameters during simulated avalanche burial: A porcine study. J. Appl. Physiol. 2021, 130, 237–244.
- Brugger, H.; Etter, H.J.; Boyd, J.; Falk, M. Causes of death from avalanche. Wilderness Environ. Med. 2009, 20, 93–96.
- Paal, P.; Strapazzon, G.; Braun, P.; Ellmauer, P.P.; Schroeder, D.C.; Sumann, G.; Werner, A.; Wenzel, V.; Falk, M.; Brugger, H. Factors affecting survival from avalanche burial—A randomised prospective porcine pilot study. Resuscitation 2013, 84, 239–243.
- Brugger, H.; Sumann, G.; Meister, R.; Adler-Kastner, L.; Mair, P.; Gunga, H.C.; Schobersberger, W.; Falk, M. Hypoxia and hypercapnia during respiration into an artificial air pocket in snow: Implications for avalanche survival. Resuscitation 2003, 58, 81–88.
- Strapazzon, G.; Gatterer, H.; Falla, M.; Cappello, T.D.; Malacrida, S.; Turner, R.; Schenk, K.; Paal, P.; Falk, M.; Schweizer, J.; et al. Hypoxia and hypercapnia effects on cerebral oxygen saturation in avalanche burial: A pilot human experimental study. Resuscitation 2020, 158, 175–182.
- Boyd, J.; Brugger, H.; Shuster, M. Prognostic factors in avalanche resuscitation: A systematic review. Resuscitation 2010, 81, 645–652.
- Lott, C.; Truhlář, A.; Alfonzo, A.; Barelli, A.; González-Salvado, V.; Hinkelbein, J.; Nolan, J.P.; Paal, P.; Perkins, G.D.; Thies, K.-C.; et al. European Resuscitation Council Guidelines 2021: Cardiac arrest in special circumstances. Resuscitation 2021, 161, 152–219.
- Eidenbenz, D.; Techel, F.; Kottmann, A.; Rousson, V.; Carron, P.-N.; Albrecht, R.; Pasquier, M. Survival probability in avalanche victims with long burial (≥60 min): A retrospective study. Resuscitation 2021.
- Paal, P.; Gordon, L.; Strapazzon, G.; Brodmann Maeder, M.; Putzer, G.; Walpoth, B.; Wanscher, M.; Brown, D.; Holzer, M.; Broessner, G.; et al. Accidental hypothermia-an update: The content of this review is endorsed by the International Commission for Mountain Emergency Medicine (ICAR MEDCOM). Scand. J. Trauma Resusc. Emerg. Med. 2016, 24, 111.
- Locher, T.; Walpoth, B.H. Differential diagnosis of circulatory failure in hypothermic avalanche victims: Retrospective analysis of 32 avalanche accidents. Praxis 1996, 85, 1275–1282.
- Oberhammer, R.; Beikircher, W.; Hörmann, C.; Lorenz, I.; Pycha, R.; Adler-Kastner, L.; Brugger, H. Full recovery of an avalanche victim with profound hypothermia and prolonged cardiac arrest treated by extracorporeal re-warming. Resuscitation 2008, 76, 474–480.
- Mittermair, C.; Foidl, E.; Wallner, B.; Brugger, H.; Paal, P. Extreme Cooling Rates in Avalanche Victims: Case Report and Narrative Review. High Alt. Med. Biol. 2021, 22, 235–240.
- Hohlrieder, M.; Brugger, H.; Schubert, H.M.; Pavlic, M.; Ellerton, J.; Mair, P. Pattern And Severity of Injury in Avalanche Victims. High Alt. Med. Biol. 2007, 8, 56–61.
- Brugger, H.; Durrer, B.; Adler-Kastner, L. On-site triage of avalanche victims with asystole by the emergency doctor. Resuscitation 1996, 31, 11–16.
- Brugger, H.; Durrer, B. On-Site Treatment of Avalanche Victims ICAR-MEDCOM-Recommendation. High Alt. Med. Biol. 2002, 3, 421–425.
- Soar, J.; Perkins, G.; Abbas, G.; Alfonzo, A.; Barelli, A.; Bierens, J.J.; Brugger, H.; Deakin, C.D.; Dunning, J.; Georgiou, M.; et al. European Resuscitation Council Guidelines for Resuscitation 2010 Section 8. Cardiac arrest in special circumstances: Electrolyte abnormalities, poisoning, drowning, accidental hypothermia, hyperthermia, asthma, anaphylaxis, cardiac surgery, trauma, pregnancy, electrocution. Resuscitation 2010, 81, 1400–1433.
- Vanden Hoek, T.L.; Morrison, L.J.; Shuster, M.; Donnino, M.; Sinz, E.; Lavonas, E.J.; Jeejeebhoy, F.M.; Gabrielli, A. Part 12: Cardiac arrest in special situations: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Circulation 2010, 122, S829–S861.
- Soar, J.; Bossaert, L.L.; Monsieurs, K.; Nikolaou, N.I.; Truhlář, A.; Zideman, D.A.; Maconochie, I.K.; Nolan, J.P.; Greif, R.; Perkins, G.D.; et al. European Resuscitation Council Guidelines for Resuscitation 2015: Section 1. Executive summary. Resuscitation 2015, 95, 1–80.
- Mair, P.; Frimmel, C.; Vergeiner, G.; Hohlrieder, M.; Moroder, L.; Hoesl, P.; Voelckel, W. Emergency medical helicopter operations for ava-lanche accidents. Resuscitation 2013, 84, 492–495.
- Wallner, B.; Moroder, L.; Brandt, A.; Mair, P.; Erhart, S.; Bachler, M.; Putzer, G.; Turner, R.; Strapazzon, G.; Falk, M.; et al. Extrication Times During Avalanche Companion Rescue: A Randomized Single-Blinded Manikin Study. High Alt. Med. Biol. 2019, 20, 245–250.
- Grasegger, K.; Strapazzon, G.; Procter, E.; Brugger, H.; Soteras, I. Avalanche Survival After Rescue With the RECCO Rescue System: A Case Report. Wilderness Environ. Med. 2016, 27, 282–286.
- Strapazzon, G.; Beikircher, W.; Procter, E.; Brugger, H. Msc Electrical Heart Activity Recorded During Prolonged Avalanche Burial. Circulation 2012, 125, 646–647.
- Strapazzon, G.; Procter, E.; Paal, P.; Brugger, H. Pre-hospital core temperature measurement in accidental and therapeutic hy-pothermia. High Alt. Med. Biol. 2014, 15, 104–111.
- Pasquier, M.; Paal, P.; Kosinski, S.; Brown, D.; Podsiadlo, P.; DaRocha, T. Esophageal Temperature Measurement. N. Engl. J. Med. 2020, 383, e93.
- Strapazzon, G.; Procter, E.; Putzer, G.; Avancini, G.; Cappello, T.D.; Überbacher, N.; Hofer, G.; Rainer, B.; Rammlmair, G.; Brugger, H. Influence of low ambient temperature on epitympanic temperature measurement: A prospective randomized clinical study. Scand. J. Trauma Resusc. Emerg. Med. 2015, 23, 90.
- Spahn, D.R.; Bouillon, B.; Cerny, V.; Duranteau, J.; Filipescu, D.; Hunt, B.J.; Komadina, R.; Maegele, M.; Nardi, G.; Riddez, L.; et al. The European guideline on management of major bleeding and coagulopathy following trauma: Fifth edition. Crit. Care 2019, 23, 98.
- Sumann, G.; Moens, D.; Brink, B.; Brodmann Maeder, M.; Greene, M.; Jacob, M.; Koirala, P.; Zafren, K.; Ayala, M.; Musi, M.; et al. Multiple trauma management in mountain environments—A scoping review: Evidence based guidelines of the International Commission for Mountain Emergency Medicine (ICAR MedCom). Intended for physicians and other advanced life support personnel. Scand. J. Trauma Resusc. Emerg. Med. 2020, 28, 1–22.
- Papenhausen, M.; Burke, L.; Antony, A.; Phillips, J. Severe hypothermia with cardiac arrest: Complete neurologic recovery in a 4-year-old child. J. Pediatr. Surg. 2001, 36, 1590–1592.
- Osborne, L.; El-Din, A.S.K.; Smith, J.E. Survival after prolonged cardiac arrest and accidental hypothermia. BMJ 1984, 289, 881–882.
- Gillen, J.P.; Vogel, M.F.; Holterman, R.K.; Skiendzielewski, J.J. Ventricular fibrillation during orotracheal intubation of hypothermic dogs. Ann. Emerg. Med. 1986, 15, 412–416.
- Danzl, D.F.; Pozos, R.S.; Auerbach, P.S.; Glazer, S.; Goetz, W.; Johnson, E.; Jui, J.; Lilja, P.; Marx, J.A.; Miller, J.; et al. Multicenter hypothermia survey. Ann. Emerg. Med. 1987, 16, 1042–1055.
- Soar, J.; Böttiger, B.W.; Carli, P.; Couper, K.; Deakin, C.D.; Djärv, T.; Lott, C.; Olasveengen, T.; Paal, P.; Pellis, T.; et al. European Resuscitation Council Guidelines 2021: Adult advanced life support. Resuscitation 2021, 161, 115–151.
- Gruber, E.; Oberhammer, R.; Balkenhol, K.; Strapazzon, G.; Procter, E.; Brugger, H.; Falk, M.; Paal, P. Basic life support trained nurses ventilate more efficiently with laryngeal mask supreme than with facemask or laryngeal tube suction-disposable--a prospective, randomized clinical trial. Resuscitation 2014, 85, 499–502.
