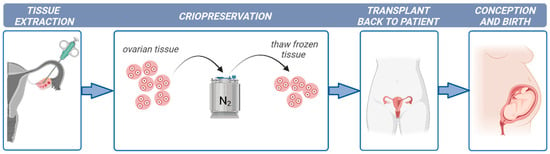
Ovarian tissue cryopreservation is gaining importance as a successful method to restore fertility to girls and young women at high risk of sterility. However, there are concerns regarding the safety of transplantation after ovarian tissue cryopreservation due to the high risk of reintroducing cancer cells and causing disease recurrence. In these cases, the development of culture systems that support oocyte development from the primordial follicle stage is required.
- cancer
- cryopreservation
- fertility preservation
1. Introduction
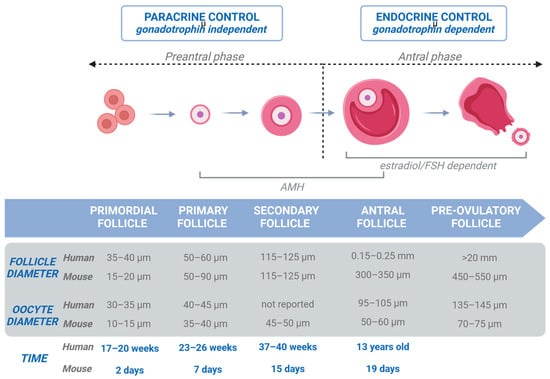
2. Folliculogenesis in Human Ovaries
3. Culture Systems
3.1. Two-Dimensional Culture Systems
3.2. Three-Dimensional Culture Systems
3.3. Critical Cell–Cell and Cell–Matrix Interactions for Improved Oocyte Survival and Growth
4. Organ-on-a-Chip Technology
Although the activation of growth of primordial follicles has been achieved, a limited number of follicles progress to secondary follicles [67]. Decent results were obtained in primates using expandable matrixes in 3D systems but the fertilization ability of the oocytes obtained was low and no blastocyst development was observed [68,69]. One of the reasons for the limited success of this technology can be found in the lack of more appropriate and physiological culture systems because it does not recapitulate the heterogeneous nature of the ECM in the ovary, with the medulla being much softer than the cortex. The ECM is believed to not only provide a 3D network to support the ovarian tissue architecture but also to regulate (together with hormones and nutrients) cell-ECM and cell–cell interactions that are important for follicle development. Choi et al. [70] revealed the crucial role of mechanical heterogeneity in the ovary in regulating follicle development by producing ovarian microtissues by encapsulating early secondary preantral follicles in microcapsules consisting of a softer, biodegradable collagen (0.5%) hydrogel core and a harder, slowly degradable alginate (2%) hydrogel shell. Folliculogenesis mainly depends upon hormones and nutrients, and their disturbance can cause abnormal follicle growth. Hence, a precise culture system that ensures the diffusion of nutrients and gases within the tissue, maximizing the retention of essential growth factors of oocyte maturation, is needed.
Considering the aforementioned aspects, a pioneering technology known as Organ-on-a-Chip (OOC) offers the means to replicate tissue architecture and emulate fluidic conditions in an in vitro setting. Broadly, these systems facilitate the miniaturization of experimental models, resulting in several advantages such as reduced working volumes, quicker reaction times, cost-effectiveness, and enhanced precision and control over experimental designs. This innovative approach holds significant promise in advancing research capabilities and improving the efficiency of experimental processes within the field.
OOC platforms, which are founded on microfluidic devices, facilitate three-dimensional organized cell culture by employing various types of ECMs. This methodology aims to emulate tissue architecture and replicate the cellular environment, mechanisms, and physiological responses of organs in an in vitro setting. The microenvironment is established through dynamic interactions among cells, fluids, and the ECM, influencing cellular processes and functions via biophysical and biochemical signals. A distinctive advantage of OOC lies in its ability to operate under flow conditions, enabling the continual replenishment of media, a process that mirrors in vivo blood supply or interstitial flow. Consequently, fluid flow ensures a consistent and adjustable supply of nutrients and oxygen, along with the supplementation of stage-specific growth factors. This dynamic environment sustains physical interactions while preventing cellular stress induced by the formation and accumulation of reactive oxygen substances [74,75].
Another pertinent aspect of this technology is the capability to tailor the devices based on design specifications including shaped microchannels, compartments, and reservoirs or the materials used to make the devices such as polydimethylsiloxane (PDMS; most prevalent), thermoplastics, or glass. Careful consideration is essential in material selection, as the inherent physicochemical properties of certain materials may impose limitations, including transparency, cost, flexibility or rigidity, and gas permeability, as well as considerations about time-consuming fabrication processes. The choice of material is contingent upon factors such as the intended application of the device, volume requirements, and production costs.
5. Conclusions
This entry is adapted from the peer-reviewed paper 10.3390/ijms25031510
