Hematopoietic cell transplant (HCT), used for treatment of many malignant and non-malignant pediatric diseases, is associated with serious complications, limiting this therapy’s benefit. Acute kidney injury (AKI), seen often after HCT, can occur at different stages of the transplant process and contributes to morbidity and mortality after HCT. The etiology of AKI is often multifactorial, including kidney hypo-perfusion, nephrotoxicity from immunosuppressive and antimicrobial agents, and other transplant-related complications such as transplant-associated thrombotic microangiopathy and sinusoidal obstructive syndrome. Early recognition of AKI is crucial to prevent further AKI and associated complications. Initial management includes identifying the etiology of AKI, preventing further kidney hypo-perfusion, adjusting nephrotoxic medications, and preventing fluid overload. Some patients will require further support with kidney replacement therapy to manage fluid overload and AKI.
- hematopoietic cell transplant
- kidney injury
- renal replacement therapy
- thrombotic microangiopathy
- continuous kidney replacement therapy
1. Acute Kidney Injury
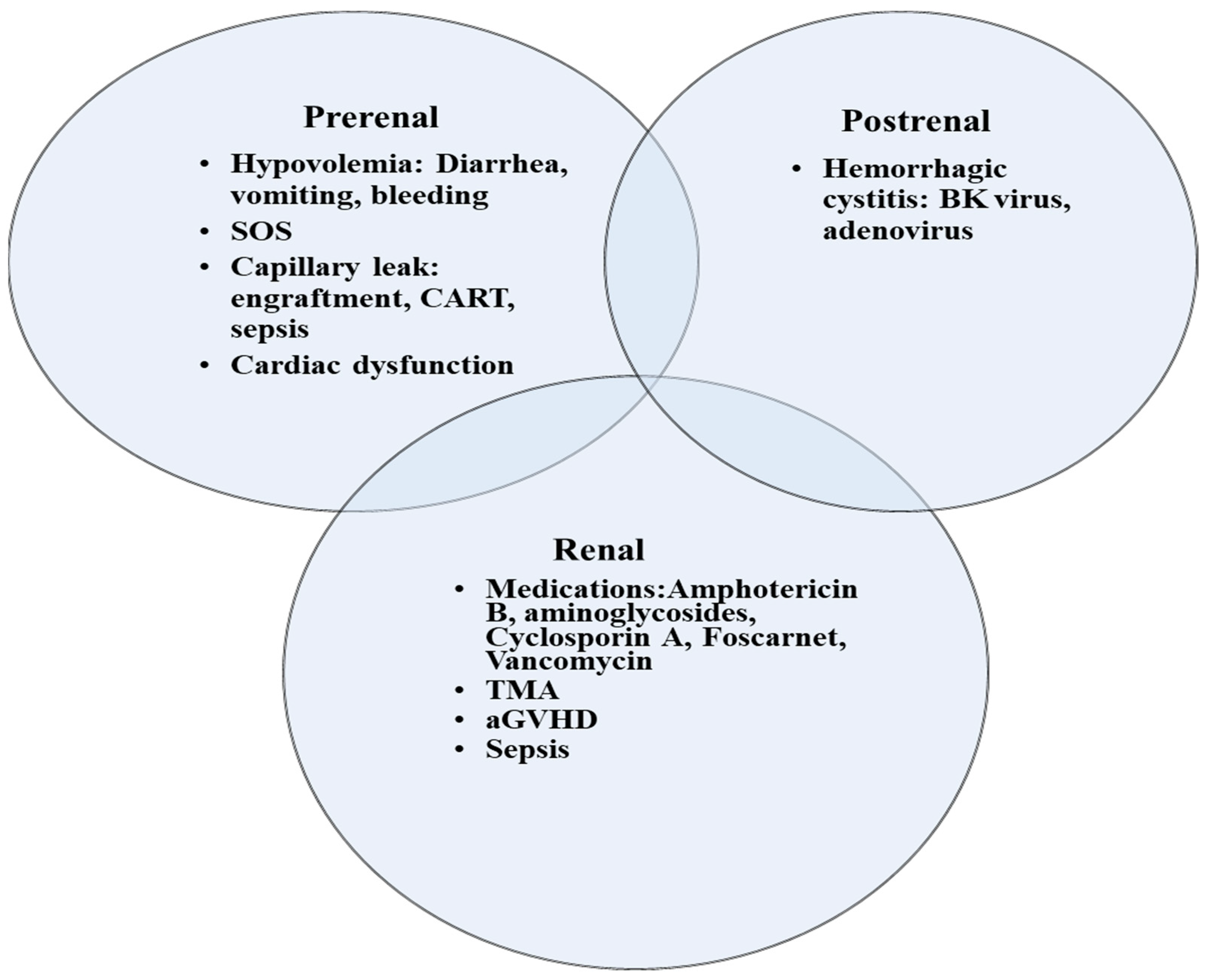
2. Special Disease Conditions Post HCT That Are Associated with AKI
2.1. Transplant-Associated Thrombotic Microangiopathy
2.2. Sinusoidal Obstruction Syndrome
-
Consumptive and transfusion-refractory thrombocytopenia;
-
Weight gain on 3 consecutive days despite the use of diuretics, or a weight gain of >5% above baseline weight within 72 h;
-
Increase in bilirubin from baseline on 3 consecutive days, or bilirubin ≥ 2 mg/dL within 72 h;
-
Hepatomegaly (best if supported by imaging) above baseline value;
-
Ascites (best if supported by imaging) above baseline.
2.3. Fluid Overload
2.4. CAR T-Cell Therapy
3. Continuous Kidney Replacement Therapy
4. Transition from CKRT to IHD/Discontinuation of CKRT
5. Outcomes of KRT
6. Biomarkers of AKI in Children with HCT
| Biomarker | Characteristic | Detection Time | Peak | AUC for AKI Detection | Limitations |
|---|---|---|---|---|---|
| Glomerular injury | |||||
| Cystatin C | 13-kDa protein that is present in all nucleated cells, protease inhibitor | 2–48 h | 6–8 h | Influenced by inflammation, muscle mass, and high-dose steroids | |
| Renal tubular injury | |||||
| NGAL | 25-kDa protein of the family of lipocalins with bacteriostatic function | 2–24 h | 6–12 h | 0.8 (0.72–0.87) | False elevation in sepsis and malignancy |
| NAG | >130-kDa proximal tubular lysosomal enzyme | 2–4 h | 0.6 | Elevated in diabetes and albuminuria | |
| KIM 1 | 38.7-kDa type I transmembrane glycoprotein | 1–24 h | 0.85 | Slow rise and non-specific May be elevated in the settings of chronic proteinuria and inflammatory diseases |
|
| Interleukin-18 | 24-kDa cytokine | 4–48 h | 12 h | 0.75 | Low sensitivity/specificity |
| L-FABP | 14-kDa lipid binding protein | 12–72 h | May lose its specificity when liver disease is present | ||
| TIMP 2 | 21-kDa protein, endogenous inhibitor of metalloproteinase activities, involved in G1 cycle arrest | 1–12 h | 0.8 | Proteinuria interferes with the test results Elevated in diabetes |
|
| IGFBP7 | 29-kDa protein, IGF-1 receptor antagonist, involved in G1 cycle arrest | 0.76 | |||
7. Tubular Injury Markers
8. Chronic Kidney Disease
This entry is adapted from the peer-reviewed paper 10.3390/curroncol30030253
References
- Raina, R.; Abu-Arja, R.; Sethi, S.; Dua, R.; Chakraborty, R.; Dibb, J.T.; Basu, R.K.; Bissler, J.; Felix, M.B.; Brophy, P.; et al. Acute kidney injury in pediatric hematopoietic cell transplantation: Critical appraisal and consensus. Pediatr. Nephrol. 2022, 37, 1179–1203.
- Elbahlawan, L.; Bissler, J.; Morrison, R.R. Continuous Renal Replacement Therapy: A Review of Use and Application in Pediatric Hematopoietic Stem Cell Transplant Recipients. Front. Oncol. 2021, 11, 632263.
- Satwani, P.; Bavishi, S.; Jin, Z.; Jacobson, J.S.; Baker, C.; Duffy, D.; Lowe, L.; Morris, E.; Cairo, M.S. Risk factors associated with kidney injury and the impact of kidney injury on overall survival in pediatric recipients following allogeneic stem cell transplant. Biol. Blood Marrow Transplant. 2011, 17, 1472–1480.
- Ando, M.; Ohashi, K.; Akiyama, H.; Sakamaki, H.; Morito, T.; Tsuchiya, K.; Nitta, K. Chronic kidney disease in long-term survivors of myeloablative allogeneic haematopoietic cell transplantation: Prevalence and risk factors. Nephrol. Dial. Transplant. 2010, 25, 278–282.
- Prókai, Á.; Csohány, R.; Sziksz, E.; Pap, D.; Balicza-Himer, L.; Boros, S.; Magda, B.; Vannay, Á.; Kis-Petik, K.; Fekete, A.; et al. Calcineurin-inhibition Results in Upregulation of Local Renin and Subsequent Vascular Endothelial Growth Factor Production in Renal Collecting Ducts. Transplantation 2016, 100, 325–333.
- Wanchoo, R.; Bayer, R.L.; Bassil, C.; Jhaveri, K.D. Emerging Concepts in Hematopoietic Stem Cell Transplantation-Associated Renal Thrombotic Microangiopathy and Prospects for New Treatments. Am. J. Kidney Dis. 2018, 72, 857–865.
- Catherine Joseph, J.R.A.; Benjamin, L. Laskin, sangeeta hingorani. Hematopoietic cell transplant associated kidney injury. In Onco-Nephrology; Elsevier: Amsterdam, The Netherlands, 2020; pp. 89–98.
- Van Benschoten, V.; Roy, C.; Gupta, R.; Ouellette, L.; Hingorani, S.; Li, A. Incidence and Risk Factors of Transplantation-Associated Thrombotic Microangiopathy: A Systematic Review and Meta-Analysis. Transplant. Cell Ther. 2022, 28, 266.e261–266.e268.
- Jodele, S.; Dandoy, C.E.; Lane, A.; Laskin, B.L.; Teusink-Cross, A.; Myers, K.C.; Wallace, G.; Nelson, A.; Bleesing, J.; Chima, R.S.; et al. Complement blockade for TA-TMA: Lessons learned from a large pediatric cohort treated with eculizumab. Blood 2020, 135, 1049–1057.
- Coppell, J.A.; Richardson, P.G.; Soiffer, R.; Martin, P.L.; Kernan, N.A.; Chen, A.; Guinan, E.; Vogelsang, G.; Krishnan, A.; Giralt, S.; et al. Hepatic veno-occlusive disease following stem cell transplantation: Incidence, clinical course, and outcome. Biol. Blood Marrow Transplant. 2010, 16, 157–168.
- Bonifazi, F.; Barbato, F.; Ravaioli, F.; Sessa, M.; Defrancesco, I.; Arpinati, M.; Cavo, M.; Colecchia, A. Diagnosis and Treatment of VOD/SOS After Allogeneic Hematopoietic Stem Cell Transplantation. Front. Immunol. 2020, 11, 489.
- Mohty, M.; Malard, F.; Abecassis, M.; Aerts, E.; Alaskar, A.S.; Aljurf, M.; Arat, M.; Bader, P.; Baron, F.; Bazarbachi, A.; et al. Sinusoidal obstruction syndrome/veno-occlusive disease: Current situation and perspectives-a position statement from the European Society for Blood and Marrow Transplantation (EBMT). Bone Marrow Transplant. 2015, 50, 781–789.
- Mahadeo, K.M.; McArthur, J.; Adams, R.H.; Radhi, M.; Angelo, J.; Jeyapalan, A.; Nicol, K.; Su, L.; Rabi, H.; Auletta, J.J.; et al. Consensus Report by the Pediatric Acute Lung Injury and Sepsis Investigators and Pediatric Blood and Marrow Transplant Consortium Joint Working Committees on Supportive Care Guidelines for Management of Veno-Occlusive Disease in Children and Adolescents: Part 2-Focus on Ascites, Fluid and Electrolytes, Renal, and Transfusion Issues. Biol. Blood Marrow Transplant. 2017, 23, 2023–2033.
- Alobaidi, R.; Basu, R.K.; DeCaen, A.; Joffe, A.R.; Lequier, L.; Pannu, N.; Bagshaw, S.M. Fluid Accumulation in Critically Ill Children. Crit. Care Med. 2020, 48, 1034–1041.
- Alobaidi, R.; Morgan, C.; Basu, R.K.; Stenson, E.; Featherstone, R.; Majumdar, S.R.; Bagshaw, S.M. Association Between Fluid Balance and Outcomes in Critically Ill Children: A Systematic Review and Meta-analysis. JAMA Pediatr. 2018, 172, 257–268.
- Goldstein, S.L.; Currier, H.; Graf, C.; Cosio, C.C.; Brewer, E.D.; Sachdeva, R. Outcome in children receiving continuous venovenous hemofiltration. Pediatrics 2001, 107, 1309–1312.
- Raymakers-Janssen, P.; Lilien, M.R.; Tibboel, D.; Kneyber, M.C.J.; Dijkstra, S.; van Woensel, J.B.M.; Lemson, J.; Cransberg, K.; van den Heuvel-Eibrink, M.M.; Wosten-van Asperen, R.M. Epidemiology and Outcome of Critically Ill Pediatric Cancer and Hematopoietic Stem Cell Transplant Patients Requiring Continuous Renal Replacement Therapy: A Retrospective Nationwide Cohort Study. Crit. Care Med. 2019, 47, e893–e901.
- Elbahlawan, L.; Morrison, R.; Li, Y.; Huang, S.; Cheng, C.; Avent, Y.; Madden, R. Outcome of Acute Respiratory Failure Secondary to Engraftment in Children After Hematopoietic Stem Cell Transplant. Front. Oncol. 2020, 10, 584269.
- Gutgarts, V.; Jain, T.; Zheng, J.; Maloy, M.A.; Ruiz, J.D.; Pennisi, M.; Jaimes, E.A.; Perales, M.A.; Sathick, J. Acute Kidney Injury after CAR-T Cell Therapy: Low Incidence and Rapid Recovery. Biol. Blood Marrow Transplant. 2020, 26, 1071–1076.
- Bagshaw, S.M.; Wald, R.; Adhikari, N.K.J.; Bellomo, R.; da Costa, B.R.; Dreyfuss, D.; Du, B.; Gallagher, M.P.; Gaudry, S.; Hoste, E.A.; et al. Timing of Initiation of Renal-Replacement Therapy in Acute Kidney Injury. N. Engl. J. Med. 2020, 383, 240–251.
- Zarbock, A.; Kellum, J.A.; Schmidt, C.; Van Aken, H.; Wempe, C.; Pavenstädt, H.; Boanta, A.; Gerß, J.; Meersch, M. Effect of Early vs Delayed Initiation of Renal Replacement Therapy on Mortality in Critically Ill Patients With Acute Kidney Injury: The ELAIN Randomized Clinical Trial. Jama 2016, 315, 2190–2199.
- Mendu, M.L.; Ciociolo, G.R., Jr.; McLaughlin, S.R.; Graham, D.A.; Ghazinouri, R.; Parmar, S.; Grossier, A.; Rosen, R.; Laskowski, K.R.; Riella, L.V.; et al. A Decision-Making Algorithm for Initiation and Discontinuation of RRT in Severe AKI. Clin. J. Am. Soc. Nephrol. 2017, 12, 228–236.
- Liu, C.; Peng, Z.; Dong, Y.; Li, Z.; Andrijasevic, N.M.; Albright, R.C., Jr.; Kashani, K.B. Predicting successful continuous renal replacement therapy liberation in critically ill patients with acute kidney injury. J. Crit. Care 2021, 66, 6–13.
- Elbahlawan, L.; Morrison, R.R. Continuous renal replacement therapy in children post-hematopoietic stem cell transplantation: The present and the future. Curr. Stem. Cell Res. Ther. 2012, 7, 381–387.
- Charlton, J.R.; Portilla, D.; Okusa, M.D. A basic science view of acute kidney injury biomarkers. Nephrol. Dial. Transplant. 2014, 29, 1301–1311.
- Nickolas, T.L.; Schmidt-Ott, K.M.; Canetta, P.; Forster, C.; Singer, E.; Sise, M.; Elger, A.; Maarouf, O.; Sola-Del Valle, D.A.; O’Rourke, M.; et al. Diagnostic and prognostic stratification in the emergency department using urinary biomarkers of nephron damage: A multicenter prospective cohort study. J. Am. Coll. Cardiol. 2012, 59, 246–255.
- Augustynowicz, M.; Bargenda-Lange, A.; Kałwak, K.; Zwolińska, D.; Musiał, K. Markers of acute kidney injury in children undergoing hematopoietic stem cell transplantation. Adv. Clin. Exp. Med. 2019, 28, 1111–1118.
- Shao, X.; Tian, L.; Xu, W.; Zhang, Z.; Wang, C.; Qi, C.; Ni, Z.; Mou, S. Diagnostic value of urinary kidney injury molecule 1 for acute kidney injury: A meta-analysis. PLoS ONE 2014, 9, e84131.
- Susantitaphong, P.; Siribamrungwong, M.; Doi, K.; Noiri, E.; Terrin, N.; Jaber, B.L. Performance of urinary liver-type fatty acid-binding protein in acute kidney injury: A meta-analysis. Am. J. Kidney Dis. 2013, 61, 430–439.
- Suzuki, G.; Ichibayashi, R.; Yamamoto, S.; Nakamichi, Y.; Watanabe, M.; Honda, M. Clinical significance of urinary L-FABP in the emergency department. Int. J. Emerg. Med. 2019, 12, 24.
- Suzuki, G.; Ichibayashi, R.; Yamamoto, S.; Serizawa, H.; Nakamichi, Y.; Watanabe, M.; Honda, M. Urinary liver-type fatty acid-binding protein variation as a predictive value of short-term mortality in intensive care unit patients. Ren. Fail. 2021, 43, 1041–1048.
- Zeng, X.F.; Li, J.M.; Tan, Y.; Wang, Z.F.; He, Y.; Chang, J.; Zhang, H.; Zhao, H.; Bai, X.; Xie, F.; et al. Performance of urinary NGAL and L-FABP in predicting acute kidney injury and subsequent renal recovery: A cohort study based on major surgeries. Clin. Chem. Lab. Med. 2014, 52, 671–678.
- Gauer, S.; Sichler, O.; Obermüller, N.; Holzmann, Y.; Kiss, E.; Sobkowiak, E.; Pfeilschifter, J.; Geiger, H.; Mühl, H.; Hauser, I.A. IL-18 is expressed in the intercalated cell of human kidney. Kidney Int. 2007, 72, 1081–1087.
- Gonzalez, F.; Vincent, F. Biomarkers for acute kidney injury in critically ill patients. Minerva Anestesiol 2012, 78, 1394–1403.
- Kashani, K.; Al-Khafaji, A.; Ardiles, T.; Artigas, A.; Bagshaw, S.M.; Bell, M.; Bihorac, A.; Birkhahn, R.; Cely, C.M.; Chawla, L.S.; et al. Discovery and validation of cell cycle arrest biomarkers in human acute kidney injury. Crit. Care 2013, 17, 1–12.
- Xie, Y.; Ankawi, G.; Yang, B.; Garzotto, F.; Passannante, A.; Breglia, A.; Digvijay, K.; Ferrari, F.; Brendolan, A.; Raffaele, B.; et al. Tissue inhibitor metalloproteinase-2 (TIMP-2) • IGF-binding protein-7 (IGFBP7) levels are associated with adverse outcomes in patients in the intensive care unit with acute kidney injury. Kidney Int. 2019, 95, 1486–1493.
- Levey, A.S.; Eckardt, K.U.; Dorman, N.M.; Christiansen, S.L.; Cheung, M.; Jadoul, M.; Winkelmayer, W.C. Nomenclature for Kidney Function and Disease: Executive Summary and Glossary from a Kidney Disease: Improving Global Outcomes (KDIGO) Consensus Conference. Kidney Dis. Basel. 2020, 6, 309–317.
- Hingorani, S.; Guthrie, K.A.; Schoch, G.; Weiss, N.S.; McDonald, G.B. Chronic kidney disease in long-term survivors of hematopoietic cell transplant. Bone Marrow Transplant. 2007, 39, 223–229.
- Hingorani, S. Chronic kidney disease after pediatric hematopoietic cell transplant. Biol. Blood Marrow Transplant. 2008, 14, 84–87.
- Prasad, M.; Jain, N.G.; Radhakrishnan, J.; Jin, Z.; Satwani, P. Risk factors for chronic kidney disease following acute kidney injury in pediatric allogeneic hematopoietic cell transplantation. Bone Marrow Transplant. 2021, 56, 1665–1673.
- Hingorani, S.R.; Seidel, K.; Lindner, A.; Aneja, T.; Schoch, G.; McDonald, G. Albuminuria in hematopoietic cell transplantation patients: Prevalence, clinical associations, and impact on survival. Biol. Blood Marrow Transplant. 2008, 14, 1365–1372.
- Hingorani, S. Renal Complications of Hematopoietic-Cell Transplantation. N. Engl. J. Med. 2016, 374, 2256–2267.
- Flynn, J.T.; Kaelber, D.C.; Baker-Smith, C.M. Subcommittee on screening and management of high blood pressure in children. Clinical Practice Guideline for Screening and Management of High Blood Pressure in Children and Adolescents. Pediatrics. Pediatrics 2017, 140, e20171904.
