Recently, tissue engineering and regenerative medicine studies have evaluated smart biomaterials as implantable scaffolds and their interaction with cells for biomedical applications. Porous materials have been used in tissue engineering as synthetic extracellular matrices, promoting the attachment and migration of host cells to induce the in vitro regeneration of different tissues. Biomimetic 3D scaffold systems allow control over biophysical and biochemical cues, modulating the extracellular environment through mechanical, electrical, and biochemical stimulation of cells, driving their molecular reprogramming. In this review, first we outline the main advantages of using polysaccharides as raw materials for porous scaffolds, as well as the most common processing pathways to obtain the adequate textural properties, allowing the integration and attachment of cells. The second approach focuses on the tunable characteristics of the synthetic matrix, emphasizing the effect of their mechanical properties and the modification with conducting polymers in the cell response. The use and influence of polysaccharide-based porous materials as drug delivery systems for biochemical stimulation of cells is also described. Overall, engineered biomaterials are proposed as an effective strategy to improve in vitro tissue regeneration and future research directions of modified polysaccharide-based materials in the biomedical field are suggested.
- biomaterials
- porous materials
- biomimetic
- multi-stimulation
- tissue engineering
- conductive polymers
1. Introduction
[1]
in vitro
in vivo
[9]
[14]
[17]
[18]
[19]
[20]
2. Processing Strategies for Polysaccharide-Based Aerogels
2.1. Processing Strategies for Polysaccharide-Based Aerogels
[22]
[21]
[21]
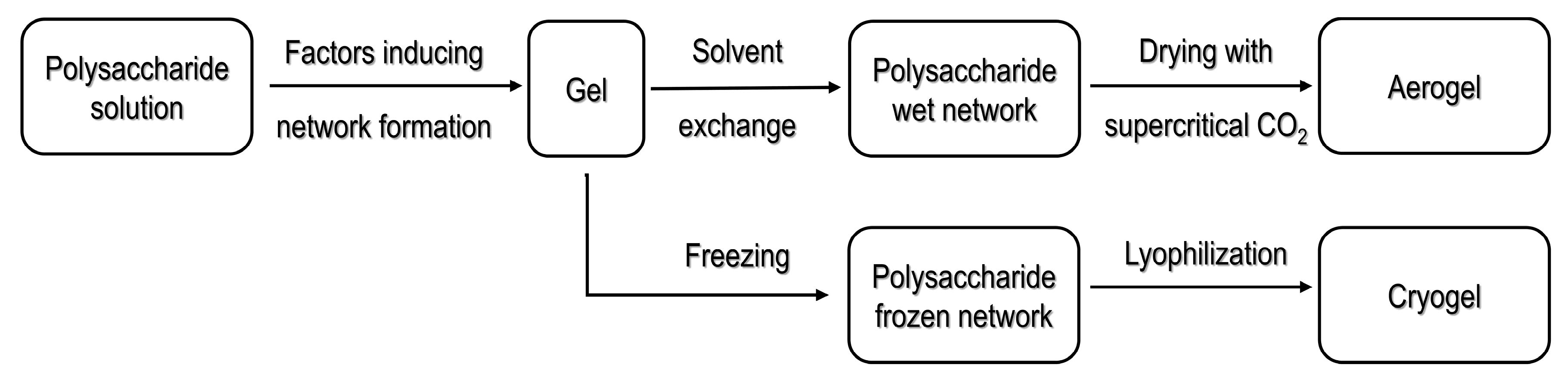
Figure 1.
[23] under Creative Commons attribution license.
3. Polysaccharide-Based Porous Materials for Tissue Engineering
[18]
[18]
[20]
3.1. Polysaccharide-Based Porous Materials as Extracellular Matrices
[24]
[26]
[27]
[28]
[29]
[30]
2
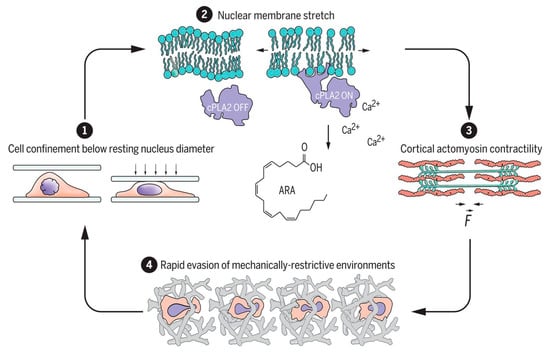
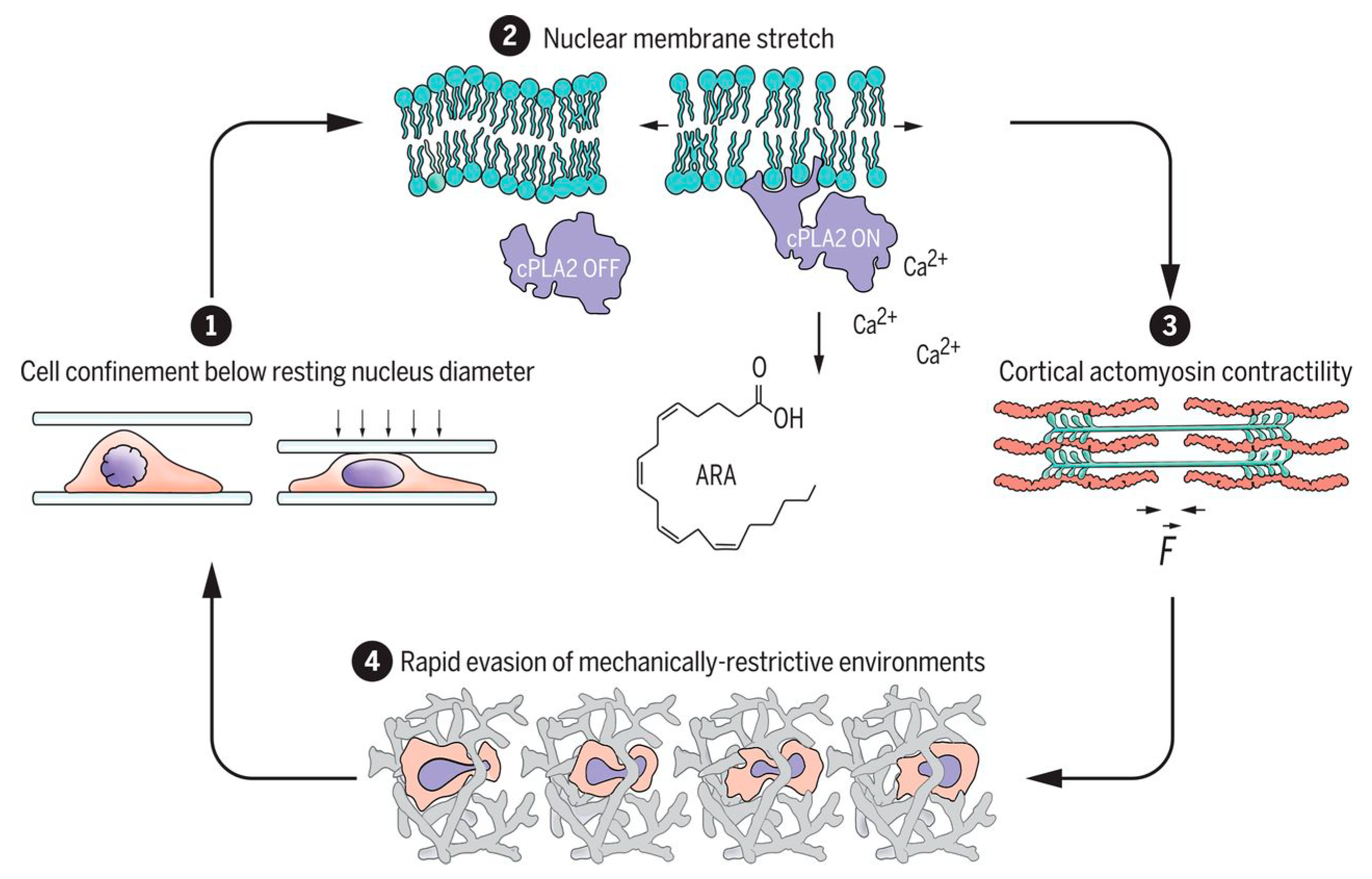
Figure 2.
2
[33] under Science Copyright Clearance Center (CCC) license.
3.2. Influence of the Mechanical Properties of the Scaffold in Cells and Tissues Behavior
in vivo
in vitro
in vivo
[31]
[40]
[32]
[39]
[41]
[42]
[43]
[7]
[40]
[44]
[31]
[9]
[38]
[42]
[38]
2+
[39]
[40]
[49]
[49]
3.3. Polysaccharide-Based Porous Materials as Scaffolds for Electrical Stimulation of Cells
[50]
[55]
[56]
[57]
[58]
[52]
[59]
[60]
[50]

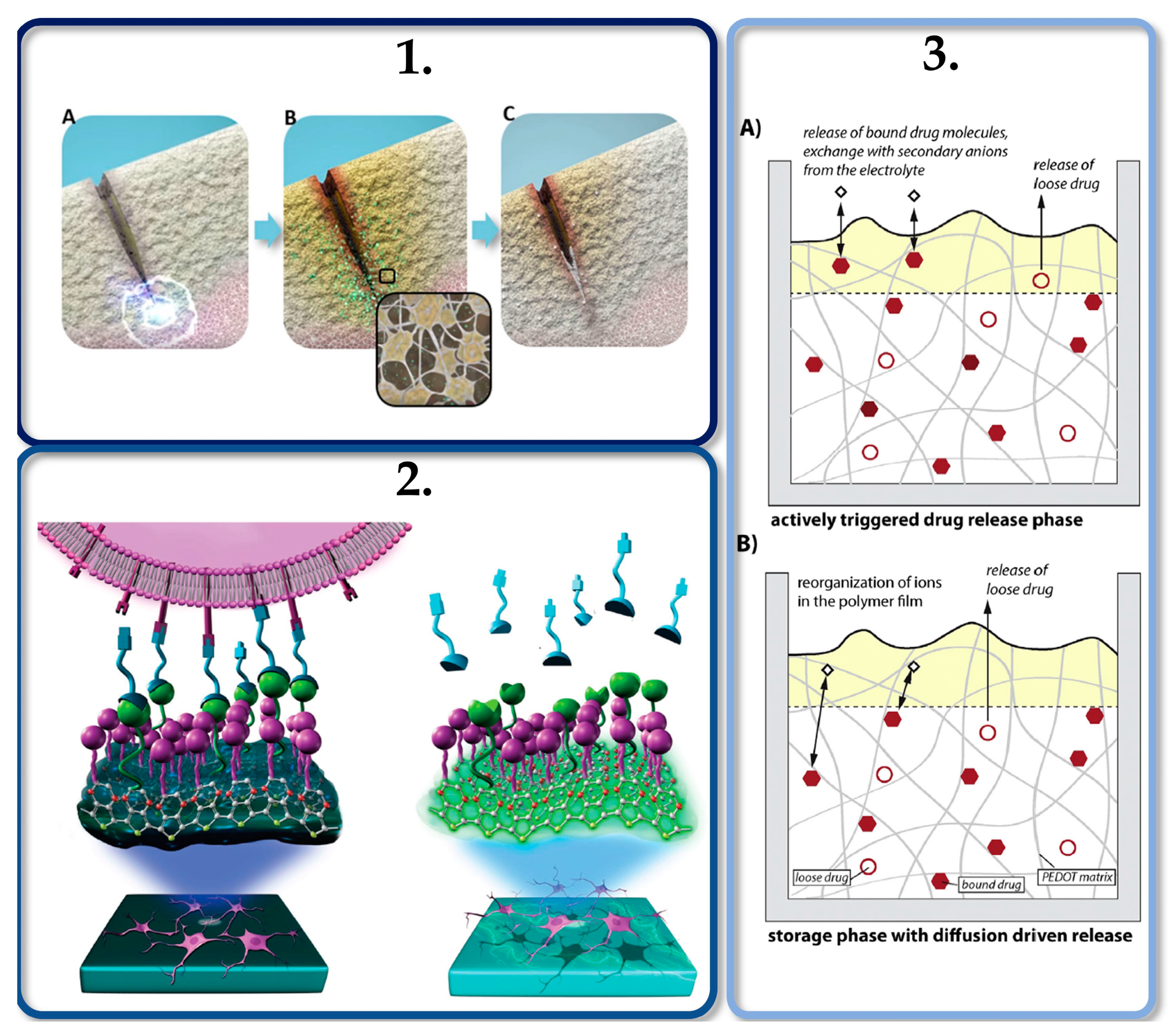
Figure 3.
a
b
c
[26][66] under Elsevier Copyright Clearance Center (CCC) licenses.
[70]
[72]
[29]
3.4. Polysaccharide-Based Porous Materials as Drug-Delivery Systems
[73]
[74]
[6]
in vivo
[80]
3.4.1. Diffusive Phenomena on the Controlled Release of Drugs on Polysaccharide-Based Aerogels
2
[81]
[75]
2
[75]
[82]
[73]
[81]
3.4.2. Controlled Drug Release by Electrical Stimulation Employing Conductive Porous Materials
[83]
[85]
in situ
ex situ
[87]
[86]
in vivo
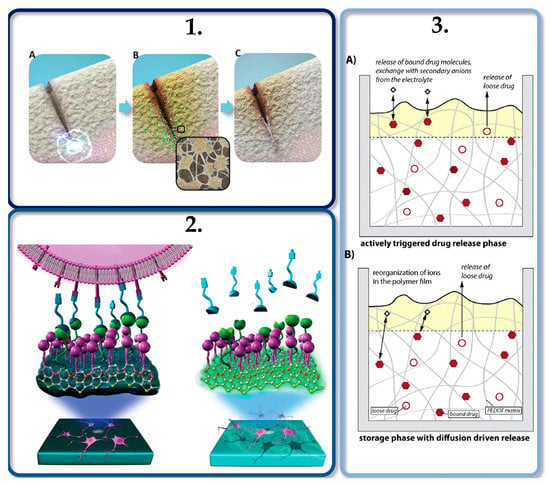
Figure 4.
1
A
B
C
[95]
2
3
A
B
References
- Brahatheeswaran Dhandayuthapani; Yasuhiko Yoshida; Toru Maekawa; D. Sakthi Kumar; Polymeric Scaffolds in Tissue Engineering Application: A Review. International Journal of Polymer Science 2011, 2011, 1-19, 10.1155/2011/290602.
- Scott Stratton; Namdev B. Shelke; Kazunori Hoshino; Swetha Rudraiah; Sangamesh G. Kumbar; Bioactive polymeric scaffolds for tissue engineering. Bioactive Materials 2016, 1, 93-108, 10.1016/j.bioactmat.2016.11.001.
- Marco Santoro; Sarita R. Shah; Jennifer L. Walker; Antonios G. Mikos; Poly(lactic acid) nanofibrous scaffolds for tissue engineering. Advanced Drug Delivery Reviews 2016, 107, 206-212, 10.1016/j.addr.2016.04.019.
- Hyerim Jo; Myeongbu Sim; Semin Kim; Sumi Yang; Youngjae Yoo; Jin-Ho Park; T. H. Yoon; Min‐Gon Kim; Jae Young Lee; Electrically conductive graphene/polyacrylamide hydrogels produced by mild chemical reduction for enhanced myoblast growth and differentiation. Acta Biomaterialia 2016, 48, 100-109, 10.1016/j.actbio.2016.10.035.
- Salvador D. Aznar-Cervantes; Ana Pagan Bernabeu; Jose G. Martinez; Antonia Bernabeu-Esclapez; Toribio F. Otero; Luis Meseguer-Olmo; Juan I. Paredes; Jose L. Cenis; Electrospun silk fibroin scaffolds coated with reduced graphene promote neurite outgrowth of PC-12 cells under electrical stimulation. Materials Science and Engineering: C 2017, 79, 315-325, 10.1016/j.msec.2017.05.055.
- Carlos A. García-González; Tatiana Budtova; Luisa Durães; Can Erkey; Pasquale Del Gaudio; Pavel Gurikov; Matthias M. Koebel; Falk Liebner; Monica Neagu; Irina Smirnova; et al. An Opinion Paper on Aerogels for Biomedical and Environmental Applications.. Molecules 2019, 24, 1815, 10.3390/molecules24091815.
- K.T. Shalumon; Han-Tsung Liao; Chang-Yi Kuo; Chak-Bor Wong; Chien-Ju Li; Mini P.A.; Jyh-Ping Chen; Rational design of gelatin/nanohydroxyapatite cryogel scaffolds for bone regeneration by introducing chemical and physical cues to enhance osteogenesis of bone marrow mesenchymal stem cells. Materials Science and Engineering: C 2019, 104, 109855, 10.1016/j.msec.2019.109855.
- Dzmitry Afanasenkau; Daria Kalinina; Vsevolod Lyakhovetskii; Christoph Tondera; Oleg Gorsky; Seyyed Moosavi; Natalia Pavlova; Natalia Merkulyeva; Allan V. Kalueff; Ivan R. Minev; et al.Pavel Musienko Rapid prototyping of soft bioelectronic implants for use as neuromuscular interfaces. Nature Biomedical Engineering 2020, 4, 1-13, 10.1038/s41551-020-00615-7.
- Akhilesh K. Gaharwar; Irtisha Singh; Ali Khademhosseini; Engineered biomaterials for in situ tissue regeneration. Nature Reviews Materials 2020, 5, 1-20, 10.1038/s41578-020-0209-x.
- Maliheh Jahromi; Shahnaz Razavi; Abbas Bakhtiari; The advances in nerve tissue engineering: From fabrication of nerve conduit to in vivo nerve regeneration assays. Journal of Tissue Engineering and Regenerative Medicine 2019, 13, 2077-2100, 10.1002/term.2945.
- Hang Lin; JiHee Sohn; He Shen; Mark T. Langhans; Rocky S. Tuan; Bone marrow mesenchymal stem cells: Aging and tissue engineering applications to enhance bone healing. Biomaterials 2019, 203, 96-110, 10.1016/j.biomaterials.2018.06.026.
- Irina Alexandra Paun; M. Zamfirescu; Catalin Romeo Luculescu; Adriana Maria Acasandrei; Cosmin Catalin Mustaciosu; Mona Mihailescu; Maria Dinescu; Electrically responsive microreservoires for controllable delivery of dexamethasone in bone tissue engineering. Applied Surface Science 2016, 392, 321-331, 10.1016/j.apsusc.2016.09.027.
- Víctor Santos-Rosales; Inés Ardao; Carmen Alvarez-Lorenzo; Nilza Ribeiro; J. M. Oliveira; C.A. García-González; Sterile and Dual-Porous Aerogels Scaffolds Obtained through a Multistep Supercritical CO₂-Based Approach.. Molecules 2019, 24, 871, 10.3390/molecules24050871.
- J.-K Francis Suh; Howard W.T Matthew; Application of chitosan-based polysaccharide biomaterials in cartilage tissue engineering: a review. Biomaterials 2000, 21, 2589-2598, 10.1016/s0142-9612(00)00126-5.
- Zahia Hamidouche; Eric Haÿ; Pascal Vaudin; Pierre Charbord; Roland Schüle; Pierre J. Marie; Olivia Fromigué; FHL2 mediates dexamethasone‐induced mesenchymal cell differentiation into osteoblasts by activating Wnt/β‐catenin signaling‐dependent Runx2 expression. The FASEB Journal 2008, 22, 3813-3822, 10.1096/fj.08-106302.
- Irving L. Weissman; Sean J. Morrison; Michael F. Clarke; Irving L. Weissman; Stem cells, cancer, and cancer stem cells. Nature 2001, 414, 105-111, 10.1038/35102167.
- J. Sammons; N. Ahmed; M. El-Sheemy; H T Hassan; The Role of BMP-6, IL-6, and BMP-4 in Mesenchymal Stem Cell–Dependent Bone Development: Effects on Osteoblastic Differentiation Induced by Parathyroid Hormone and Vitamin D3. Stem Cells and Development 2004, 13, 273-280, 10.1089/154732804323099208.
- Iwona M. Wojak-Ćwik; Łucja Rumian; Małgorzata Krok-Borkowicz; Ricarda Hess; Ricardo Bernhardt; Piotr Dobrzyński; Stephanie Möller; Matthias Schnabelrauch; Vera Hintze; Dieter Scharnweber; et al.Elżbieta Pamuła Synergistic effect of bimodal pore distribution and artificial extracellular matrices in polymeric scaffolds on osteogenic differentiation of human mesenchymal stem cells. Materials Science and Engineering: C 2019, 97, 12-22, 10.1016/j.msec.2018.12.012.
- Umber Cheema; S.-Y. Yang; Vivek Mudera; G Goldspink; R.A. Brown; 3-D in vitro model of early skeletal muscle development. Cell Motility and the Cytoskeleton 2003, 54, 226-236, 10.1002/cm.10095.
- Hongkun He; Marianna Sofman; Alex J-S Wang; Caroline C. Ahrens; Wade Wang; Linda G. Griffith; Paula T. Hammond; Engineering Helical Modular Polypeptide-Based Hydrogels as Synthetic Extracellular Matrices for Cell Culture. Biomacromolecules 2019, 21, 566-580, 10.1021/acs.biomac.9b01297.
- Mehrez E. El-Naggar; Sarah I. Othman; Ahmed A. Allam; Osama M. Morsy; Synthesis, drying process and medical application of polysaccharide-based aerogels. International Journal of Biological Macromolecules 2020, 145, 1115-1128, 10.1016/j.ijbiomac.2019.10.037.
- C.A. García-González; M. Alnaief; I. Smirnova; Polysaccharide-based aerogels—Promising biodegradable carriers for drug delivery systems. Carbohydrate Polymers 2011, 86, 1425-1438, 10.1016/j.carbpol.2011.06.066.
- Kathirvel Ganesan; Tatiana Budtova; Lorenz Ratke; Pavel Gurikov; Victor Baudron; Imke Preibisch; Philipp Niemeyer; Irina Smirnova; Barbara Milow; Review on the Production of Polysaccharide Aerogel Particles. Materials 2018, 11, 2144, 10.3390/ma11112144.
- Achilleas D. Theocharis; Spyros S. Skandalis; Chrysostomi Gialeli; Nikos K. Karamanos; Extracellular matrix structure. Advanced Drug Delivery Reviews 2016, 97, 4-27, 10.1016/j.addr.2015.11.001.
- Fergal J. O'brien; Biomaterials & scaffolds for tissue engineering. Materials Today 2011, 14, 88-95, 10.1016/s1369-7021(11)70058-x.
- Ricardo Starbird-Perez; Carlos A. García-González; Irina Smirnova; Wolfgang H. Krautschneider; Wolfgang Bauhofer; Synthesis of an organic conductive porous material using starch aerogels as template for chronic invasive electrodes. Materials Science and Engineering: C 2014, 37, 177-183, 10.1016/j.msec.2013.12.032.
- Gleeson, J. P.; O'Brien, F. J. . Advances in Composite Materials for Medicine and Nanotechnology; Attaf, Brahim, Eds.; Intech Open Access: Croatia, 2011; pp. 39-59.
- Carlos A. García-González; Angel Concheiro; Carmen Alvarez-Lorenzo; Processing of Materials for Regenerative Medicine Using Supercritical Fluid Technology. Bioconjugate Chemistry 2015, 26, 1159-1171, 10.1021/bc5005922.
- Karla Ramírez-Sánchez; Aura Ledezma-Espinoza; Andrés Sánchez-Kopper; Esteban Avendano; Monica Prado; Ricardo Starbird-Perez; Polysaccharide κ-Carrageenan as Doping Agent in Conductive Coatings for Electrochemical Controlled Release of Dexamethasone at Therapeutic Doses. Molecules 2020, 25, 2139, 10.3390/molecules25092139.
- Haoxiang Chen; Juchang Zhong; Jian Wang; Ruiying Huang; Xiaoyin Qiao; Honghui Wang; Zhikai Tan; Enhanced growth and differentiation of myoblast cells grown on E-jet 3D printed platforms. International Journal of Nanomedicine 2019, 14, 937-950, 10.2147/ijn.s193624.
- Basak E. Uygun; Sarah E. Stojsih; Howard W. T. Matthew; Effects of Immobilized Glycosaminoglycans on the Proliferation and Differentiation of Mesenchymal Stem Cells. Tissue Engineering Part A 2009, 15, 3499-3512, 10.1089/ten.tea.2008.0405.
- Valeria Venturini; Fabio Pezzano; Frederic Català Castro; Hanna-Maria Häkkinen; Senda Jiménez-Delgado; Mariona Colomer-Rosell; Monica Marro; Queralt Tolosa-Ramon; Sonia Paz-López; Miguel A. Valverde; et al.Julian WeghuberPablo Loza-AlvarezMichael KriegStefan WieserVerena Ruprecht The nucleus measures shape changes for cellular proprioception to control dynamic cell behavior. Science 2020, 370, eaba2644, 10.1126/science.aba2644.
- A. J. Lomakin; C. J. Cattin; D. Cuvelier; Z. Alraies; M. Molina; G. P. F. Nader; N. Srivastava; P. J. Sáez; J. M. Garcia-Arcos; I. Y. Zhitnyak; et al.A. BhargavaM. K. DriscollE. S. WelfR. FiolkaR. J. PetrieN. S. De SilvaJ. M. González-GranadoN. ManelA. M. Lennon-DuménilD. J. MüllerM. Piel The nucleus acts as a ruler tailoring cell responses to spatial constraints. Science 2020, 370, eaba2894, 10.1126/science.aba2894.
- Yusuke Nagai; Hidenori Yokoi; Keiko Kaihara; Keiji Naruse; The mechanical stimulation of cells in 3D culture within a self-assembling peptide hydrogel. Biomaterials 2012, 33, 1044-1051, 10.1016/j.biomaterials.2011.10.049.
- Niamh Fahy; Mauro Alini; Martin Stoddart; Mechanical stimulation of mesenchymal stem cells: Implications for cartilage tissue engineering. Journal of Orthopaedic Research 2017, 36, 52-63, 10.1002/jor.23670.
- Angelo S. Mao; David J. Mooney; Regenerative medicine: Current therapies and future directions. Proceedings of the National Academy of Sciences 2015, 112, 14452-14459, 10.1073/pnas.1508520112.
- John A. Pedersen; Melody A. Swartz; Mechanobiology in the Third Dimension. Annals of Biomedical Engineering 2005, 33, 1469-1490, 10.1007/s10439-005-8159-4.
- Vanessa Terraciano; Nathaniel Hwang; Lorenzo Moroni; Hyung Bin Park; Zijun Zhang; Joseph Mizrahi; Dror Seliktar; Jennifer Elisseeff; Differential Response of Adult and Embryonic Mesenchymal Progenitor Cells to Mechanical Compression in Hydrogels. Stem Cells 2007, 25, 2730-2738, 10.1634/stemcells.2007-0228.
- W. Zhang; C.W. Kong; M.H. Tong; W.H. Chooi; Nan Huang; R.A. Li; Barbara P. Chan; Maturation of human embryonic stem cell-derived cardiomyocytes (hESC-CMs) in 3D collagen matrix: Effects of niche cell supplementation and mechanical stimulation. Acta Biomaterialia 2017, 49, 204-217, 10.1016/j.actbio.2016.11.058.
- J. Matthew Barnes; Laralynne Przybyla; Valerie M. Weaver; Tissue mechanics regulate brain development, homeostasis and disease. Journal of Cell Science 2016, 130, 71-82, 10.1242/jcs.191742.
- Chao Liu; Xin Cui; Thomas M. Ackermann; Vittoria Flamini; Weiqiang Chen; Alesha B. Castillo; Osteoblast-derived paracrine factors regulate angiogenesis in response to mechanical stimulation. Integrative Biology 2015, 8, 785-794, 10.1039/c6ib00070c.
- Nina Bono; D. Pezzoli; L. Lévesque; C. Loy; Gabriele Candiani; G. B. Fiore; Diego Mantovani; Unraveling the role of mechanical stimulation on smooth muscle cells: A comparative study between 2D and 3D models. Biotechnology and Bioengineering 2016, 113, 2254-2263, 10.1002/bit.25979.
- Elham Hasanzadeh; Ghassem Amoabediny; Nooshin Haghighipour; Nasim Gholami; Javad Mohammadnejad; Shahrokh Shojaei; Nasim Salehi-Nik; The stability evaluation of mesenchymal stem cells differentiation toward endothelial cells by chemical and mechanical stimulation. In Vitro Cellular & Developmental Biology - Plant 2017, 53, 818-826, 10.1007/s11626-017-0165-y.
- Aban Shuaib; Daniyal Motan; Pinaki Bhattacharya; Alex McNabb; Timothy M. Skerry; Damien Lacroix; Heterogeneity in The Mechanical Properties of Integrins Determines Mechanotransduction Dynamics in Bone Osteoblasts. Scientific Reports 2019, 9, 1-14, 10.1038/s41598-019-47958-z.
- N Wang; J P Butler; D E Ingber; Mechanotransduction across the cell surface and through the cytoskeleton. Science 1993, 260, 1124-1127, 10.1126/science.7684161.
- H. Maldonado; C. Calderon; F. Burgos-Bravo; O. Kobler; W. Zuschratter; O. Ramirez; S. Härtel; P. Schneider; A.F.G. Quest; Rodrigo Herrera-Molina; et al.Lisette Leyton Astrocyte-to-neuron communication through integrin-engaged Thy-1/CBP/Csk/Src complex triggers neurite retraction via the RhoA/ROCK pathway. Biochimica et Biophysica Acta (BBA) - Molecular Cell Research 2017, 1864, 243-254, 10.1016/j.bbamcr.2016.11.006.
- Hyun Jung Lee; Miguel F. Diaz; Katherine M. Price; Joyce A. Ozuna; Songlin Zhang; Eva M. Sevick-Muraca; John P. Hagan; Pamela L. Wenzel; Fluid shear stress activates YAP1 to promote cancer cell motility. Nature Communications 2017, 8, 14122, 10.1038/ncomms14122.
- Xueran Chen; Shangrong Zhang; Zhen Wang; Fengsong Wang; Xinwang Cao; Quan Wu; Chenggang Zhao; Huihui Ma; Fang Ye; Hongzhi Wang; et al.Zhiyou Fang Supervillin promotes epithelial-mesenchymal transition and metastasis of hepatocellular carcinoma in hypoxia via activation of the RhoA/ROCK-ERK/p38 pathway. Journal of Experimental & Clinical Cancer Research 2018, 37, 128, 10.1186/s13046-018-0787-2.
- A. Glücksmann; Studies on bone mechanics in vitro. I. Influence of pressure on orientation of structure. The Anatomical Record 1938, 72, 97-113, 10.1002/ar.1090720109.
- Greeshma Thrivikraman; Sunil Kumar Boda; Sunil Kumar Boda; Unraveling the mechanistic effects of electric field stimulation towards directing stem cell fate and function: A tissue engineering perspective. Biomaterials 2017, 150, 60-86, 10.1016/j.biomaterials.2017.10.003.
- Jaatinen, L. The Effect of an Applied Electric Current on Cell Proliferation, Viability, Morphology, Adhesion,and Stem Cell Differentiation. Ph.D. Thesis, Tampere University of Technology, Tampere, Finland, 2017.
- T. Taghian; D. A. Narmoneva; A. B. Kogan; Modulation of cell function by electric field: a high-resolution analysis. Journal of The Royal Society Interface 2015, 12, 20150153, 10.1098/rsif.2015.0153.
- Wang, L.; Liu, Y.; Jin, H.; Steinacker, J. Electrical stimulation induced Hsp70 response in C2C12 cells. Exerc. Immunol. Rev. 2010, 16, 86–97.
- Laleh Ghasemi-Mobarakeh; Molamma P Prabhakaran; Mohammad Morshed; Mohammad Hossein Nasr-Esfahani; Hossein Baharvand; Sahar Kiani; Salem S Al-Deyab; Seeram Ramakrishna; Application of conductive polymers, scaffolds and electrical stimulation for nerve tissue engineering. Journal of Tissue Engineering and Regenerative Medicine 2011, 5, e17-e35, 10.1002/term.383.
- Peter C. Sherrell; Brianna C. Thompson; Jonathan K. Wassei; Amy A. Gelmi; Michael J. Higgins; Richard B. Kaner; Gordon G. Wallace; Maintaining Cytocompatibility of Biopolymers Through a Graphene Layer for Electrical Stimulation of Nerve Cells. Advanced Functional Materials 2013, 24, 769-776, 10.1002/adfm.201301760.
- Ilyas S. Aleem; Idris Aleem; Nathan Evaniew; Jason W. Busse; Michael Yaszemski; Arnav Agarwal; Thomas Einhorn; Mohit Bhandari; Efficacy of Electrical Stimulators for Bone Healing: A Meta-Analysis of Randomized Sham-Controlled Trials. Scientific Reports 2016, 6, 31724, 10.1038/srep31724.
- Jenny W.H. Lou; Austin J. Bergquist; Abdulaziz Aldayel; Jennifer Czitron; David F. Collins; Interleaved neuromuscular electrical stimulation reduces muscle fatigue. Muscle & Nerve 2016, 55, 179-189, 10.1002/mus.25224.
- Wei Zhu; Tao Ye; Se-Jun Lee; Haitao Cui; Shida Miao; Xuan Zhou; Danmeng Shuai; Lijie Grace Zhang; Enhanced neural stem cell functions in conductive annealed carbon nanofibrous scaffolds with electrical stimulation. Nanomedicine: Nanotechnology, Biology and Medicine 2018, 14, 2485-2494, 10.1016/j.nano.2017.03.018.
- Xiaoning Yuan; Derya E. Arkonac; Pen-Hsiu Grace Chao; Gordana Vunjak-Novakovic; Electrical stimulation enhances cell migration and integrative repair in the meniscus. Scientific Reports 2014, 4, nd, 10.1038/srep03674.
- Tai, G.; Reid, B.; Cao, L.; Zhao, M. Electrotaxis and wound healing: Experimental methods to study electricfields as a directional signal for cell migration. Methods Mol. Biol. 2009, 571, 77–97.
- Piyush Bajaj; Bobby Reddy; Larry Millet; Chunan Wei; Pinar Zorlutuna; Gang Bao; Rashid Bashir; Patterning the differentiation of C2C12 skeletal myoblasts. Integrative Biology 2010, 3, 897-909, 10.1039/c1ib00058f.
- Weibo Guo; Xiaodi Zhang; Xin Yu; Shu Wang; Jichuan Qiu; Wei Tang; Linlin Li; Hong Liu; Zhong Lin Wang; Self-Powered Electrical Stimulation for Enhancing Neural Differentiation of Mesenchymal Stem Cells on Graphene–Poly(3,4-ethylenedioxythiophene) Hybrid Microfibers. ACS Nano 2016, 10, 5086-5095, 10.1021/acsnano.6b00200.
- Jing Wang; Lingling Tian; Nuan Chen; Seeram Ramakrishna; Xiumei Mo; The cellular response of nerve cells on poly-l-lysine coated PLGA-MWCNTs aligned nanofibers under electrical stimulation. Materials Science and Engineering: C 2018, 91, 715-726, 10.1016/j.msec.2018.06.025.
- Filipa Pires; Quirina Ferreira; Carlos A.V. Rodrigues; J. Morgado; Frederico Castelo Ferreira; Neural stem cell differentiation by electrical stimulation using a cross-linked PEDOT substrate: Expanding the use of biocompatible conjugated conductive polymers for neural tissue engineering. Biochimica et Biophysica Acta (BBA) - General Subjects 2015, 1850, 1158-1168, 10.1016/j.bbagen.2015.01.020.
- C. Boehler; C. Kleber; N. Martini; Y. Xie; I. Dryg; T. Stieglitz; U.G. Hofmann; M. Asplund; Actively controlled release of Dexamethasone from neural microelectrodes in a chronic in vivo study. Biomaterials 2017, 129, 176-187, 10.1016/j.biomaterials.2017.03.019.
- Roy Zamora-Sequeira; Inés Ardao; Ricardo Starbird-Perez; C.A. García-González; Conductive nanostructured materials based on poly-(3,4-ethylenedioxythiophene) (PEDOT) and starch/κ-carrageenan for biomedical applications. Carbohydrate Polymers 2018, 189, 304-312, 10.1016/j.carbpol.2018.02.040.
- Hao, H.B.; Yuan, L.; Fu, Z.B.; Wang, C.Y.; Yang, X.; Zhu, J.; Qu, J.; Chen, H.; Schiraldi, D. Biomass-basedmechanically-strong and electrically-conductive polymer aerogels and their application for supercapacitors.ACS Appl. Mater. Interfaces 2016, 8, 9917–9924.
- Insang You; Unyong Jeong; Electromechanical Decoupling by Porous Aerogel Conducting Polymer. Matter 2019, 1, 24-25, 10.1016/j.matt.2019.06.008.
- Xuetong Zhang; Dongwu Chang; Jiren Liu; Yunjun Luo; Conducting polymer aerogels from supercritical CO2 drying PEDOT-PSS hydrogels. Journal of Materials Chemistry 2009, 20, 5080, 10.1039/c0jm00050g.
- Christopher Bertucci; Ryan Koppes; Courtney Dumont; Abigail N. Koppes; Neural responses to electrical stimulation in 2D and 3D in vitro environments. Brain Research Bulletin 2019, 152, 265-284, 10.1016/j.brainresbull.2019.07.016.
- Priscila Hernandez-Suarez; Karla Ramirez; Fernando Alvarado; E. Avendano; Karla Ramírez Sánchez; Electrochemical characterization of poly(3,4-ethylenedioxythiophene)/κ-carrageenan as a biocompatible conductive coat for biologic applications. MRS Communications 2018, 9, 218-223, 10.1557/mrc.2018.189.
- Eimear M. Ryan; Carmel B. Breslin; Formation of polypyrrole with dexamethasone as a dopant: Its cation and anion exchange properties. Journal of Electroanalytical Chemistry 2018, 824, 188-194, 10.1016/j.jelechem.2018.07.052.
- V.S.S. Gonçalves; Pavel Gurikov; J. Poejo; A.A. Matias; S. Heinrich; C.M.M. Duarte; I. Smirnova; Alginate-based hybrid aerogel microparticles for mucosal drug delivery. European Journal of Pharmaceutics and Biopharmaceutics 2016, 107, 160-170, 10.1016/j.ejpb.2016.07.003.
- Clara López-Iglesias; Joana Barros; Inés Ardao; Fernando J. Monteiro; Carmen Alvarez-Lorenzo; José L. Gómez-Amoza; Carlos A. García-González; Vancomycin-loaded chitosan aerogel particles for chronic wound applications. Carbohydrate Polymers 2018, 204, 223-231, 10.1016/j.carbpol.2018.10.012.
- C.A. García-González; Irina Smirnova; Use of supercritical fluid technology for the production of tailor-made aerogel particles for delivery systems. The Journal of Supercritical Fluids 2013, 79, 152-158, 10.1016/j.supflu.2013.03.001.
- Leticia Goimil; Víctor Santos-Rosales; Araceli Delgado; Carmen Évora; R. Reyes; A. Abel Lozano-Pérez; Salvador D. Aznar-Cervantes; Jose Luis Cenis; Francisco J. Otero Espinar; Angel Concheiro; et al.Carmen Alvarez-LorenzoC.A. García-González scCO2-foamed silk fibroin aerogel/poly(ε-caprolactone) scaffolds containing dexamethasone for bone regeneration. Journal of CO2 Utilization 2019, 31, 51-64, 10.1016/j.jcou.2019.02.016.
- Pedro F. Costa; Ana M. Puga; Luis Diaz-Gomez; Angel Concheiro; Dirk H. Busch; Carmen Alvarez-Lorenzo; Additive manufacturing of scaffolds with dexamethasone controlled release for enhanced bone regeneration. International Journal of Pharmaceutics 2015, 496, 541-550, 10.1016/j.ijpharm.2015.10.055.
- Qihai Liu; Lian Cen; Heng Zhou; Shuo Yin; Guangpeng Liu; Wei Liu; Yilin Cao; Lei Cui; The Role of the Extracellular Signal-Related Kinase Signaling Pathway in Osteogenic Differentiation of Human Adipose-Derived Stem Cells and in Adipogenic Transition Initiated by Dexamethasone. Tissue Engineering Part A 2009, 15, 3487-3497, 10.1089/ten.tea.2009.0175.
- M. Danckwerts; A. Fassihi; Implantable Controlled Release Drug Delivery Systems: A Review. Drug Development and Industrial Pharmacy 1990, 17, 1465-1502, 10.3109/03639049109026629.
- Chizhu Ding; Zibiao Li; A review of drug release mechanisms from nanocarrier systems. Materials Science and Engineering: C 2017, 76, 1440-1453, 10.1016/j.msec.2017.03.130.
- Paola Franco; Iolanda De Marco; Supercritical CO2 adsorption of non-steroidal anti-inflammatory drugs into biopolymer aerogels. Journal of CO2 Utilization 2020, 36, 40-53, 10.1016/j.jcou.2019.11.001.
- Leticia Goimil; Mara E.M. Braga; Ana M.A. Dias; José L. Gómez-Amoza; Angel Concheiro; Patricia Diaz-Rodriguez; Hermínio C. De Sousa; Carlos A. García-González; Supercritical processing of starch aerogels and aerogel-loaded poly(ε-caprolactone) scaffolds for sustained release of ketoprofen for bone regeneration. Journal of CO2 Utilization 2017, 18, 237-249, 10.1016/j.jcou.2017.01.028.
- K Krukiewicz; Tailorable drug capacity of dexamethasone-loaded conducting polymer matrix. IOP Conference Series: Materials Science and Engineering 2018, 369, 012002, 10.1088/1757-899x/369/1/012002.
- Susanne Löffler; Silke Seyock; Rolf Nybom; Gunilla B. Jacobson; Agneta Richter-Dahlfors; Electrochemically triggered release of acetylcholine from scCO2 impregnated conductive polymer films evokes intracellular Ca2+ signaling in neurotypic SH-SY5Y cells. Journal of Controlled Release 2016, 243, 283-290, 10.1016/j.jconrel.2016.10.020.
- Richard Balint; Nigel J. Cassidy; Sarah H. Cartmell; Conductive polymers: Towards a smart biomaterial for tissue engineering. Acta Biomaterialia 2014, 10, 2341-2353, 10.1016/j.actbio.2014.02.015.
- B. Alshammary; Frank C. Walsh; P. Herrasti; Carlos Ponce De Leon; Electrodeposited conductive polymers for controlled drug release: polypyrrole. Journal of Solid State Electrochemistry 2015, 20, 839-859, 10.1007/s10008-015-2982-9.
- Katarzyna Krukiewicz; Barbara Gniazdowska; Tomasz Jarosz; Artur P. Herman; Slawomir Boncel; Roman Turczyn; Effect of immobilization and release of ciprofloxacin and quercetin on electrochemical properties of poly(3,4-ethylenedioxypyrrole) matrix. Synthetic Metals 2019, 249, 52-62, 10.1016/j.synthmet.2019.02.001.
- Naader Alizadeh; Ehsan Shamaeli; Electrochemically controlled release of anticancer drug methotrexate using nanostructured polypyrrole modified with cetylpyridinium: Release kinetics investigation. Electrochimica Acta 2014, 130, 488-496, 10.1016/j.electacta.2014.03.055.
- C. Boehler; Felix Oberueber; Maria Asplund; Tuning drug delivery from conducting polymer films for accurately controlled release of charged molecules.. Journal of Controlled Release 2019, 304, 173-180, 10.1016/j.jconrel.2019.05.017.
- Darren Svirskis; Manisha Sharma; Yang Yu; Sanjay Garg; Electrically switchable polypyrrole film for the tunable release of progesterone. Therapeutic Delivery 2013, 4, 307-313, 10.4155/tde.12.166.
- Lucas Leprince; Audrey Dogimont; Delphine Magnin; Sophie Demoustier-Champagne; Dexamethasone electrically controlled release from polypyrrole-coated nanostructured electrodes. Journal of Materials Science: Materials in Electronics 2010, 21, 925-930, 10.1007/s10856-010-4008-6.
- Grace Stevenson; Simon E. Moulton; Peter C. Innis; Gordon G. Wallace; Polyterthiophene as an electrostimulated controlled drug release material of therapeutic levels of dexamethasone. Synthetic Metals 2010, 160, 1107-1114, 10.1016/j.synthmet.2010.02.035.
- Jin Qu; Yongping Liang; Mengting Shi; Baolin Guo; Y. Gao; Zhanhai Yin; Biocompatible conductive hydrogels based on dextran and aniline trimer as electro-responsive drug delivery system for localized drug release. International Journal of Biological Macromolecules 2019, 140, 255-264, 10.1016/j.ijbiomac.2019.08.120.
- Jin Qu; Xin Zhao; Peter X. Ma; Baolin Guo; Injectable antibacterial conductive hydrogels with dual response to an electric field and pH for localized “smart” drug release. Acta Biomaterialia 2018, 72, 55-69, 10.1016/j.actbio.2018.03.018.
- Raquel Núñez-Toldrà; Fabian Vasquez-Sancho; Nathalie Barroca; Gustau Catalan; Investigation of The Cellular Response to Bone Fractures: Evidence for Flexoelectricity. Scientific Reports 2020, 10, 1-10, 10.1038/s41598-019-57121-3.
- Hsing-An Lin; Bo Zhu; Yu-Wei Wu; Jun Sekine; Aiko Nakao; Shyh-Chyang Luo; Yoshiro Yamashita; Hsiao-Hua Yu; Dynamic Poly(3,4-ethylenedioxythiophene)s Integrate Low Impedance with Redox-Switchable Biofunction. Advanced Functional Materials 2018, 28, nd, 10.1002/adfm.201703890.