Patient-specific three-dimensional (3D) printed models have been increasingly used in cardiology and cardiac surgery, in particular, showing great value in the domain of congenital heart disease (CHD). CHD is characterized by complex cardiac anomalies with disease variations between individuals; thus, it is difficult to obtain comprehensive spatial conceptualization of the cardiac structures based on the current imaging visualizations. 3D printed models derived from patient’s cardiac imaging data overcome this limitation by creating personalized 3D heart models, which not only improve spatial visualization, but also assist preoperative planning and simulation of cardiac procedures, serve as a useful tool in medical education and training, and improve doctor–patient communication.
- three-dimensional printing
- congenital heart disease
- medical education
1. Introduction
2. Image Post-Processing and Segmentation Process for Three-Dimensional (3D) Printing in Congenital Heart Disease (CHD)
The first step to generate a 3D printed heart model is to undergo a series of image post-processing and segmentation of volumetric data, which are commonly acquired with cardiac CT or MRI imaging. While high-resolution original datasets are important for accurately isolating the desired anatomy of interest and pathology from surrounding structures, segmentation of cardiac structures remains challenging due to complexity of cardiac features, especially in the CHD cases. Different software is used for segmentation, with Mimics (Materialise HQ, Leuven, Belgium) being the most commonly used commercial software and 3D Slicer (Brigham and Women’s Hospital, Boston, Mass) as the most common open-source tool. Several review articles have provided excellent description of details about the steps required from data acquisition to image post-processing and segmentation [11][12][13][14][11,12,13,14]. Figure 1 shows the steps to create 3D printed models from data acquisition to image post-processing and segmentation.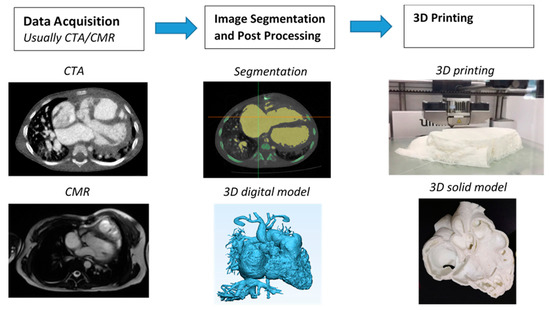
3. Accuracy of 3D Printed Heart Models
The most important part of creating 3D printed models is to ensure that 3D models accurately delineate anatomical structures and pathologies since the model accuracy is essential for treatment planning [15]. Current research evidence indicates that 3D printed heart models are generally accurate [16], and this has been validated by other studies, either based on case reports/series or single- or multi-center studies [17][18][19][20][21][22][23][17,18,19,20,21,22,23]. In most of the studies, model accuracy is determined by the degree of agreement between the measured dimensions of the 3D printed model and the dimensions of original source images, usually using cardiac CT, MRI, and sometimes using rotational angiography or echocardiography [16][17][18][22][16,17,18,22], or intraoperative findings [19]. Currently, there is no standardized method to measure the dimensions of the 3D printed heart models. Most of the studies carried out measurement using calipers on the physical 3D printed models [17][20][21][17,20,21]. Only a few studies conducted measurement on the standard tessellation language (STL) file [18] and conducted CT scan on the 3D printed model for measurement [16]. The authors claimed it is easier to replicate the exact plane for measurement comparison, hence improving the accuracy of the results [16][18][16,18].4. 3D Printed Models in Medical Education and Training
3D printed heart models have been shown to serve as a novel teaching tool in medical education and training and this is confirmed by RCT available in the literature [22][23][24][25][22,23,24,25]. Three of them reported the usefulness of 3D printed models of different types of CHD in medical education [22][23][24][22,23,24]. Table 1 shows details of these three studies and other single- and multi-center reports.| Authors | Study Design | Sample Size and Participants | Types of CHD | Key Findings |
|---|---|---|---|---|
| Loke et al. 2017 [22] | RCT: study group was presented with 3D printed models, while control group with 2D images | 35 pediatric residents:18 in study group and 17 in control group | Tetralogy of Fallot (ToF) | 3D printed models resulted in significantly higher satisfaction scores than 2D images (p = 0.03). 3D printed models improved residents’ self-efficacy scores in managing ToF, although this did not reach significant difference when compared to 2D images (p = 0.39). |
| Su et al., 2018 [23] | RCT: study group participated in teaching seminar including 3D printed models, while control group only attended teaching seminar without having 3D models | 63 medical students: 32 in study group and 31 in control group | Ventricular septal defect (VSD) | Significant improvement in VSD learning and structure conceptualization in the study group compared to the control group (p < 0.05). |
| White et al., 2018 [24] | RCT: study group was given 3D printed models in addition to lectures, while control group received only the lectures | 60 pediatric residents:31 in study group and 29 in control group | VSD and ToF | 3D printed models of CHD improved residents’ knowledge and confidence in managing complex CHD such as ToF but did not seem to improve simple CHD such as VSD. |
| Olivieri et al., 2016 [26] | Single-center report of 3D printed models for training and simulation | 10 3D printed models, 70 clinicians participated in the training sessions | Cardiac and vascular anomalies | 3D printed models can be used as a simulation training tool for multidisciplinary intensive care providers by enhancing their anatomic knowledge and clinical management of CHD patients. |
| Hoashi et al., 2018 [27] | Single-center experience | 20 cases | DORV and other cardiac anomalies | 3D printed heart models improved understanding of the relationship between intraventricular communications and great vessels. Further, 3D printed models allowed simulation of cardiac surgeries by creating intracardiac pathways, thus providing benefits to inexperienced cardiac surgeons. |
| Valverde et al., 2017 [21] | Multi-center study consisting of 10 international centers | 40 patients with complex CHD | DORV (50%) and other cardiac anomalies | 3D models were accurate in replicating anatomy. 3D models refined the surgical approach in nearly 50% cases. 3D models resulted in significant change in the surgical plan in 24% of cases. |
| Zhao et al., 2018 [28] | Single-center experience | 25 patients with 8 in 3D printing group and 17 in control group | DORV | 3D printed models showed high accuracy in measurements of aortic diameters and the size of VSD when compared to original CT data. 3D printed models significantly reduced ICU time and mechanical ventilation time (p < 0.05). |
| Ryan et al., 2018 [29] | Single-center experience | Of 928 cardiothoracic surgeries, 164 3D models were printed for various purposes | DORV, ToF and other cardiac anomalies | 3D printed models reduced mean time in the operating room and 30-day readmission and mortality rates when compared to the standard of care. |
