Pregnancy, alone, being associated with a state of immune alterations, exposes the maternal immune system to many challenges. Pregnant women, being a highly vulnerable group, need to be administered vaccines as early as possible; however, there is a lot of vaccine hesitancy among the population regarding immunization of pregnant women, who are avoided in the initial phases of most clinical trials. A look at available studies on the mechanisms of immune response in pregnant women and further, the reports of vaccine efficacy and outcomes among pregnant women against COVID-19 and EVD would definitely yield many insights that could be useful in the surveillance and planning of vaccination strategies for pregnant women against impending pathogenic RNA viruses.
- Covid-19
- Ebola
- Pregnancy
- Immune response
- Vaccination
1. Impact of COVID-19 and EVD on Pregnancy
2. Maternal and Neonatal Outcomes Associated with COVID-19 and EVD
| (a) | |||||||||||||
| Year of Study | Country | Study Approach | Case Type | Sample Size | Pre-Existing Medical Conditions | Need for Hospitalization | Maternal Mortality | Obstetric Complication | Perinatal Outcome | Reference | |||
| 2020 | 22 countries | Retrospective cohort study | Pregnant women with confirmed SARS-CoV-2 infection | 388 | Not available | ICU admission (11.1%) Mechanical Ventilation (9.3%) | 0.80% | Miscarriage (19.4%) Termination of pregnancy (1.1%) | Termination of pregnancy (1.1%) Pre-term birth (26.3%) Still birth (2.3%) Neonatal death (2%) SARS-CoV-2 positive (0.4%) | [10] | |||
| 2020 | United Kingdom | Prospective observational cohort study | pregnant women with confirmed SARS-CoV-2 infection | 427 | Asthma (7%) Hypertension (3%), Diabetes (3%) | Critical care (10%) | 1% | Pregnancy loss (1%) | Stillbirth (1%) Neonatal death (1%) Loss of Pregnancy (1%) SARS-CoV-2 positive (2%) | [11] | |||
| 2020 | Singapore | Prospective Cohort Study | Pregnant women with diagnosis of COVID-19 | 16 | Asthma (12.5%) HCV carriers (6.25%) | ICU admission (6.25%) | NIL | Spontaneous miscarriage (22.2%) | Neonatal death (6.25%) | [12] | |||
| 2020 | China | Retrospective Cohort study | Pregnant women who gave a single live birth between January 13 and March 18, 2020 | 65 | Not available | Higher need for Caesarean section (80%) | NIL | Gestational diabetes (3%) Gestational hypertension (11%) Pre-eclampsia (1%) | Pre-term birth (14%) Diarrhea (1.7%) Fever (5.17%) | [13] | |||
| 2020 | Iran | Prospective Cohort Study | Pregnant women with diagnosis of COVID-19 | 56 | Diabetes (16.1%) Hypertension (10.7%) Hypothyroidy (19.6%) | ICU admission (10.7%) Mechanical Ventilation (6.15%) Higher need for Caesarean section (67.3%) | NIL | Pre-eclampsia | Pre-term birth (34.5%) Perinatal death (3.6%) | [14] | |||
| 2020 | France | Retrospective Cohort study | Pregnant women with diagnosis of COVID-19 having a code for hospitalization for COVID-19 | 874 | Diabetes (1.3%) Hypertension (1.9%) | ICU admission (5.9%) Higher need for Caesarean section (33%) | 0.20% | Pre-eclampsia (4.8%) Gestational hypertension (2.3%) Postpartum hemorrhage (10%) | Pre-term birth (11.3%) | [15] | |||
| 2020 | Democratic Republic of the Congo | Case Study | Pregnant woman with confirmed SARS-CoV-2 infection | 1 | NIL | Caesarean section | NIL | Thrombotic vasculopathy in the placenta, Inflammatory appearance in the pelvic organs | SARS-CoV-2-infected Neonate, Perinatal death | [16] | |||
| 2020 | China | Retrospective Case Control study | Pregnant woman with confirmed SARS-CoV-2 infection, pregnant women with suspected infection and Control groups | 11 | Gestational diabetes (18.75%) Gestational hypertension (18.75%) Hypothyroidism (12.5%) | Caesarean section (87.5%) | NIL | Pre-eclampsia (6.25%) | Pre-term birth (18.8%), Low birth weight (17.6%) | [17] | |||
| 2020 | China | Case Study | Pregnant woman who was exposed to SARS-CoV-2 | 1 | NIL | Hospitalization Caesarean section | NIL | NIL | SARS-CoV-2-infected Neonate | [18] | |||
| 2020 | USA | Case Series | Pregnant women with suspected COVID-19 infection | 92 | NIL | Hospitalization (1.1%) | NIL | low morbidity | One fetal demise, but not sure whether it is due to COVID-19 | [19] | |||
| 2020 | Sweden | Case Series | Critically ill pregnant or newly delivered women positive for COVID-19 | 5 | Gestational diabetes (2 out of 5) Gestational Hypothyroidism (1 out of 5) Situs Inversus (1 out of 5) | Hospitalization for an average of 20 days (4 out of 5) Intubation (4 out of 5) | NIL | Severe respiratory distress syndromeCardiac arrest (1 out of 5) | NIL | [20] | |||
| 2020 | USA | Retrospective cohort study | Possible exposure or infection and positive COVID-19 test | 1609 | Chronic pulmonary disease (12.6%) Cardiac arrhythmia (10.4%) Hypertension (6.5%) Hypothyroidism (5%) Diabetes (3%) | Hospitalization (60.5%) | 0.20% | Not available | NIL | [21] | |||
| 2020 | USA | Retrospective cohort study | Pregnant and post-partum patients with SARS-CoV-2 infection | 2352 | Chronic pulmonary disease (12%) Hypertension (6.9%) Thyroid disease (3.9%) Diabetes (3.8%) | ICU admission (3.7%) | 0.20% | Post-partum hemorrhage (2.6%) Other infections (2.3%) Hypertensive disorders of pregnancy (10.1%) | Fetal/neonatal death (2.5%) Miscarriage (1.2%) Stillbirth (0.5%) Preterm birth (17.7%) | [22] | |||
| 2020 | USA | Observational Cohort study | Women who delivered and had SARS-CoV-2 infection during pregnancy | 252 | Gestational diabetes (3%) Chronic hypertension (5%) | Hospitalization (6%) | NIL | Pre-eclampsia (11%) Chorioamnionitis (10%) Excessive blood loss (7%) | Neonatal SARS-CoV-2 infection (3%) | [23] | |||
| 2020 | Iran | Retrospective case Control study | Pregnant women with COVID-19 positive test and a positive chest X-ray result | 110 | Hypertension (5.45%) Diabetes (9.09%) Asthma (5.45%) | ICU admission (6.9%) Requirement for invasive ventilation (1.7%) | NIL | Abortion (21.42%) Post-partum hemorrhage (5%) Pre-term birth (25%) | Still birth (5%) Fetal distress (10%) Low birth weight (10%) NICU admission (10%) | [24] | |||
| 2021 | 18 countries | Cohort study | Pregnant women with diagnosis of COVID-19 | 706 | Hypertension (3.7%), Diabetes (4.7%), Chronic respiratory disease (3.5%), Endocrine dysfunction (10.6%) | ICU admission (8.4%) | 1.60% | Hypertension Pre-eclampsia Anemia Infections | Pre-term birth (22.5%) Low birth weight (20.5%) SARS-CoV-2 positive (57.1%) | [25] | |||
| (b) | |||||||||||||
| Year of Study | Country | Study Approach | Case Type | Sample Size | Maternal Age | Gestational Age of Infection | Comorbidity | Clinical Presentation | Need for Hospitalization/ICU Admission | Maternal Mortality | Obstetric Morbidity | Perinatal Outcome | Reference |
| 1995 | Kikwit | Cohort Study | Ebola positive Pregnant women | 15 | 24–38 (mean age 32) | First trimester (27%), second trimester (40%) and third trimester (33%) | Not available | Fever (100%), asthenia (100%), abdominal pain (100%), conjunctivitis (100%), anorexia (100%), diarrhea (100%), arthralgia (100%), dysphagia (100%), headache (100%) | Admitted to General Hospital | 95.5% death | Genital bleeding (100%) | Abortion (67%), curettage performed due to incomplete abortion (20%), still birth (6.7%) | [26] |
| 2000 | North Uganda | Case study | Ebola positive Pregnant women | 1 | 31 | 28 weeks | Placenta had a moderate amount of malarial parasite pigment | Conjunctival injection, diffuse abdominal tenderness, and slight pulmonary rales | Admitted to ETU | Maternal survival | Placenta had mild subchorionitis | Still birth | [27] |
| 2012 | Congo | Case study | Ebola positive Pregnant women | 1 | 29 | 7 months | Not available | Fever, vomiting, dysphagia and diarrhea, drowsiness and wheezing, Dyspnea, coma stage 1b, light exophthalmos, cold limbs and sub icterus | Admitted to ETU | Maternal death | Dystocia | Death of neonate | [28] |
| 2014 | Liberia | Case Study | Ebola positive Pregnant women | 1 | 31 | Third trimester | Not available | vomiting, diarrhea, bleeding, and semi consciousness | Admitted to ETU | Maternal death | Not available | Intrauterine fetal death | [29] |
| 2014 | Guinea | Case Study | Ebola positive Pregnant woman | 1 | 40 | 4th month | Not available | abdominal pain, diarrhea and fever | Admitted to ETU | Maternal survival | Vaginal bleeding | Still birth | [30] |
| 2014 | Southern Guinea | Case study | Ebola positive Pregnant women | 2 | 20’s | 7 months | Malaria (50%) | Asthenia, fever, and vomiting, Anasarca (50%) | Admitted to ETU | Maternal survival (100%) | Absence of uterine contraction, cervical dilation (50%) and fetal heartbeat, hypertonic uterus (50%), post-partum hemorrhage (50%), suspected chorioamnionitis (50%) | Still birth (100%) | [31] |
| 2014 | Sierra Leone | Case study | Ebola positive Pregnant women | 1 | 34 | 36 | Not available | Headache, cough, and arthralgia | Admitted to ETU | Maternal survival | Hydropic Placenta | Still birth | [32] |
| 2014 | Sierra Leone | Cohort Study | Ebola positive Pregnant women | 55 | Mean age 25 | Not available | Not available | Fever (86.8%), fatigue or weakness (81.1%), nausea or vomiting (64.2%), headache (66%), muscle or joint pain (58.5%), vaginal bleeding (32.1%), unexplained bleeding (20.8%), and sore throat (13.2%) | Admitted to ETU | Not available | Vaginal bleeding (32%) | Not available | [33] |
| 2014 | Sierra Leone | Cohort Study | Ebola positive Pregnant women | 67 | Mean age 23 | 28–37 weeks | Not available | Fever (86.8%), abdominal pain (75.5%), fatigue (81.1%), nausea (64.2%) | Admitted to ETU | Maternal death (79%) | Vaginal bleeding (32%), obstetric hemorrhage (29.8%) and eclampsia (1.5%) | Spontaneous abortion (20.9%), Fetal death (5 out of 6), Still birth (8) | [34] |
| 2014 | Sierra Leone | Case study | qPCR negative, IgG positive | 1 | 19 | 36 weeks | Sickle cell anemia | Symptom free | Admitted to ETU | Maternal survival | Not available | Intrauterine fetal death, heavily macerated baby | [35] |
| 2014–15 | Liberia and Sierra Leone | Retrospective Cohort study | Ebola positive Pregnant women | 13 | 20-32 | Not available | Not available | Abdominal pain (85%) and nausea/vomiting (69%), Bleeding (30%), Hiccups (8%) and non-hemorrhagic rash (8%) | Admitted to ETU | 46% death | Not available | Preterm delivery (15%), Perinatal death (15%), Abortion (15%), Termination of pregnancy (7.6%), | [36] |
| 2014–2015 | Sierra Leone | Case series | Ebola positive Pregnant women (83.3%), Ebola survivor (16.6%) | 6 | 18-38 | Third trimester | Not available | Muscle pain (16.6%), headache (16.6%), diarrhea (16.6%), vomiting (16.6%) | Admitted to ETU | Maternal death (66.6%) | Postpartum hemorrhage (50%), hypovolemic shock (16.6%) | Neonate death (83.3%), still birth (16.6%) | [37] |
| 2015 | Sierra Leone | Case Study | Ebola positive Pregnant woman | 1 | 22 | 5 months | Not available | Anorexia, muscle pain, and joint pain | Admitted to ETU | Maternal survival | Leaking fluid | Intrauterine fetal death | [30] |
| 2015 | Sierra Leone | Case Study | IgG, IgM positive | 1 | 20 | Not available | Severe back pain, loss of appetite, and intense fatigue | Delivery attended by village traditional birth attendant | Maternal survival | Leakage of bloody fluid from vagina | Still birth | [38] | |
| 2016 | Guinea | Case Study | Ebola positive Pregnant women | 1 | 25 | 28th week | Not available | Hyperthermia, asthenia, and conjunctival infection | Admitted to ETU | Maternal death post delivery | Severe vaginal bleeding with signs of coagulopathy | Survived after treatment | [39] |
3. Effects of COVID-19 and EVD on Placenta and Vertical Transmission
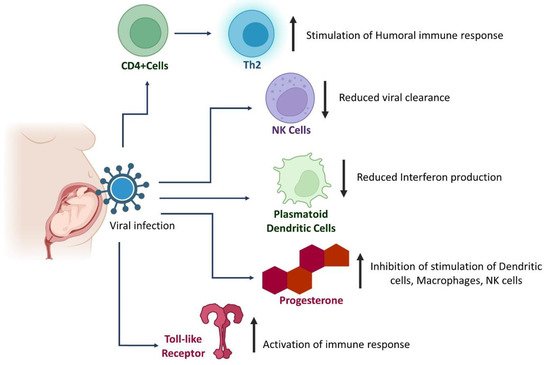
4. Alterations in Immune Response in Pregnant Women with SARS-CoV-2 and EBOV Infections
This entry is adapted from 10.3390/pathogens11070800
References
- Paixao, E.S.; Harron, K.; Campbell, O.; Teixeira, M.G.; Costa, M.D.C.N.; Barreto, M.L.; Rodrigues, L.C. Dengue in pregnancy and maternal mortality: A cohort analysis using routine data. Sci. Rep. 2018, 8, 9938.
- Susich, M.; Packer, C.H.; Chaiken, S.R.; Garg, B.; Caughey, A.B. 1115 A comparison of maternal and neonatal outcomes in acute and chronic hepatitis B. Am. J. Obstet. Gynecol. 2021, 224, S687.
- Kreitchmann, R.; Li, S.X.; Melo, V.H.; Coelho, D.F.; Watts, D.H.; João, E.; Coutinho, C.M.; Alarcon, J.O.; Siberry, G.K. Predictors of adverse pregnancy outcomes in women infected with HIV in Latin America and the Caribbean: A cohort study. BJOG Int. J. Obstet. Gynaecol. 2014, 121, 1501–1508. Available online: https://obgyn.onlinelibrary.wiley.com/doi/10.1111/1471-0528.12680 (accessed on 26 May 2022).
- Foeller, M.E.; Valle, C.C.R.D.; Foeller, T.M.; Oladapo, O.T.; Roos, E.; Thorson, A.E. Pregnancy and breastfeeding in the context of Ebola: A systematic review. Lancet Infect. Dis. 2020, 20, e149–e158.
- World Health Organization. Guidelines for the Management of Pregnant and Breastfeeding Women in the Context of Ebola Virus Disease; World Health Organization: Geneva, Switzerland, 2020. Available online: https://apps.who.int/iris/handle/10665/330851 (accessed on 26 May 2022).
- Kotlar, B.; Gerson, E.; Petrillo, S.; Langer, A.; Tiemeier, H. The impact of the COVID-19 pandemic on maternal and perinatal health: A scoping review. Reprod. Health 2021, 18, 10.
- Lokken, E.M.; Taylor, G.G.; Huebner, E.M.; Vanderhoeven, J.; Hendrickson, S.; Coler, B.; Sheng, J.S.; Walker, C.L.; McCartney, S.A.; Kretzer, N.M.; et al. Higher severe acute respiratory syndrome coronavirus 2 infection rate in pregnant patients. Am. J. Obstet. Gynecol. 2021, 225, 75.e1–75.e16.
- Sutton, D.; Fuchs, K.; D’Alton, M.; Goffman, D. Universal Screening for SARS-CoV-2 in Women Admitted for Delivery. N. Engl. J. Med. 2020, 382, 2163–2164.
- Liu, H.; Wang, L.-L.; Zhao, S.-J.; Kwak-Kim, J.; Mor, G.; Liao, A.-H. Why are pregnant women susceptible to COVID-19? An immunological viewpoint. J. Reprod. Immunol. 2020, 139, 103122.
- Maternal and Perinatal Outcomes of Pregnant Women with SARS-CoV-2 Infection—2021—Ultrasound in Obstetrics & Gynecology—Wiley Online Library. Available online: https://obgyn.onlinelibrary.wiley.com/doi/10.1002/uog.23107 (accessed on 26 May 2022).
- Characteristics and Outcomes of Pregnant Women Admitted to Hospital with Confirmed SARS-CoV-2 infection in UK: National Population Based Cohort Study | The BMJ. Available online: https://www.bmj.com/content/369/bmj.m2107 (accessed on 26 May 2022).
- Mattar, C.N.; Kalimuddin, S.; Sadarangani, S.P.; Tagore, S.; Thain, S.; Thoon, K.C.; Hong, E.Y.; Kanneganti, A.; Ku, C.W.; Chan, G.M.; et al. Pregnancy Outcomes in COVID-19: A Prospective Cohort Study in Singapore. Ann. Acad. Med. Singapore 2020, 49, 857–869.
- Yang, R.; Mei, H.; Zheng, T.; Fu, Q.; Zhang, Y.; Buka, S.; Yao, X.; Tang, Z.; Zhang, X.; Qiu, L.; et al. Pregnant women with COVID-19 and risk of adverse birth outcomes and maternal-fetal vertical transmission: A population-based cohort study in Wuhan, China. BMC Med. 2020, 18, 330.
- Abedzadeh-Kalahroudi, M.; Sehat, M.; Vahedpour, Z.; Talebian, P. Maternal and neonatal outcomes of pregnant patients with COVID-19: A prospective cohort study. Int. J. Gynecol. Obstet. 2021, 153, 449–456.
- Epelboin, S.; Labrosse, J.; De Mouzon, J.; Fauque, P.; Gervoise-Boyer, M.-J.; Levy, R.; Sermondade, N.; Hesters, L.; Bergère, M.; Devienne, C.; et al. Obstetrical outcomes and maternal morbidities associated with COVID-19 in pregnant women in France: A national retrospective cohort study. PLoS Med. 2021, 18, e1003857.
- Birindwa, E.K.; Mulumeoderhwa, G.M.; Nyakio, O.; Mbale, G.-Q.M.; Mushamuka, S.Z.; Materanya, J.M.; Kahasha, P.M.; Bisimwa, Y.K.; Kampara, F.M.; Irenge, J.M.; et al. A case study of the first pregnant woman with COVID-19 in Bukavu, eastern Democratic Republic of the Congo. Matern. Health Neonatol. Perinatol. 2021, 7, 6.
- Li, N.; Han, L.; Peng, M.; Lv, Y.; Ouyang, Y.; Liu, K.; Yue, L.; Li, Q.; Sun, G.; Chen, L.; et al. Maternal and Neonatal Outcomes of Pregnant Women with Coronavirus Disease 2019 (COVID-19) Pneumonia: A Case-Control Study. Clin. Infect. Dis. 2020, 71, 2035–2041.
- Long, R.; Wu, D.; Lin, X.; Lv, D.; Wang, R.; Jin, L.; Liao, S.; Liu, W.; Deng, D. COVID-19 and Pregnancy: A Case Study. Glob. Chall. 2021, 5, 2000074.
- Fox, N.S.; Melka, S. COVID-19 in Pregnant Women: Case Series from One Large New York City Obstetrical Practice. Am. J. Perinatol. 2020, 37, 1002–1004.
- A Case Series on Critically Ill Pregnant or Newly Delivered Patients with Covid-19, Treated at Karolinska University Hospital, Stockholm. Available online: https://www.hindawi.com/journals/criog/2021/8868822/ (accessed on 26 May 2022).
- Qeadan, F.; Mensah, N.A.; Tingey, B.; Stanford, J.B. The risk of clinical complications and death among pregnant women with COVID-19 in the Cerner COVID-19 cohort: A retrospective analysis. BMC Pregnancy Childbirth 2021, 21, 305.
- Association of SARS-CoV-2 Infection with Serious Maternal Morbidity and Mortality from Obstetric Complications | Infectious Diseases | JAMA | JAMA Network. Available online: https://jamanetwork.com/journals/jama/fullarticle/2788985 (accessed on 26 May 2022).
- Pregnancy Outcomes Among Women with and Without Severe Acute Respiratory Syndrome Coronavirus 2 Infection | Global Health | JAMA Network Open | JAMA Network. Available online: https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2773105 (accessed on 26 May 2022).
- Taghavi, S.-A.; Heidari, S.; Jahanfar, S.; Amirjani, S.; Aji-Ramkani, A.; Azizi-Kutenaee, M.; Bazarganipour, F. Obstetric, maternal, and neonatal outcomes in COVID-19 compared to healthy pregnant women in Iran: A retrospective, case-control study. Middle East. Fertil. Soc. J. 2021, 26, 17.
- Maternal and Neonatal Morbidity and Mortality Among Pregnant Women with and Without COVID-19 Infection: The INTERCOVID Multinational Cohort Study | Neonatology | JAMA Pediatrics | JAMA Network. Available online: https://jamanetwork.com/journals/jamapediatrics/fullarticle/2779182 (accessed on 26 May 2022).
- Mupapa, K.; Mukundu, W.; Bwaka, M.A.; Kipasa, M.; De Roo, A.; Kuvula, K.; Kibadi, K.; Massamba, M.; Ndaberey, D.; Colebunders, R.; et al. Ebola Hemorrhagic Fever and Pregnancy. J. Infect. Dis. 1999, 179, S11–S12.
- Muehlenbachs, A.; Vázquez, O.D.L.R.; Bausch, D.G.; Schafer, I.J.; Paddock, C.D.; Nyakio, J.P.; Lame, P.; Bergeron, E.; McCollum, A.M.; Goldsmith, C.S.; et al. Ebola Virus Disease in Pregnancy: Clinical, Histopathologic, and Immunohistochemical Findings. J. Infect. Dis. 2016, 215, 64–69.
- Kratz, T.; Roddy, P.; Oloma, A.T.; Jeffs, B.; Ciruelo, D.P.; De La Rosa, O.; Borchert, M. Ebola Virus Disease Outbreak in Isiro, Democratic Republic of the Congo, 2012: Signs and Symptoms, Management and Outcomes. PLoS ONE 2015, 10, e0129333.
- Akerlund, E.; Prescott, J.; Tampellini, L. Shedding of Ebola Virus in an Asymptomatic Pregnant Woman. N. Engl. J. Med. 2015, 372, 2467–2469.
- Dilemmas in Managing Pregnant Women with Ebola: 2 Case Reports | Clinical Infectious Diseases | Oxford Academic. Available online: https://academic.oup.com/cid/article/62/7/903/2462754 (accessed on 26 May 2022).
- Baggi, F.M.; Taybi, A.; Kurth, A.; Van Herp, M.; Di Caro, A.; Wölfel, R.; Günther, S.; Decroo, T.; Declerck, H.; Jonckheere, S. Management of pregnant women infected with Ebola virus in a treatment centre in Guinea, June 2014. Eurosurveillance 2014, 19, 20983.
- Oduyebo, T.; Pineda, D.; Lamin, M.; Leung, A.; Corbett, C.; Jamieson, D. A Pregnant Patient with Ebola Virus Disease. Obstet. Gynecol. 2015, 126, 1273–1275.
- Mpofu, J.J.; Soud, F.; Lyman, M.; Koroma, A.P.; Morof, D.; Ellington, S.; Kargbo, S.S.; Callaghan, W. Clinical presentation of pregnant women in isolation units for Ebola virus disease in Sierra Leone, 2014. Int. J. Gynecol. Obstet. 2019, 145, 76–82.
- Lyman, M.; Mpofu, J.J.; Soud, F.; Oduyebo, T.; Ellington, S.; Schlough, G.W.; Koroma, A.P.; McFadden, J.; Morof, D. Maternal and perinatal outcomes in pregnant women with suspected Ebola virus disease in Sierra Leone, 2014. Int. J. Gynecol. Obstet. 2018, 142, 71–77.
- Okoror, L.; Kamara, A.; Kargbo, B.; Bangura, J.; Lebby, M. Transplacental Transmission: A Rare Case of Ebola Virus Transmission. Infect. Dis. Rep. 2018, 10, 53–55.
- Henwood, P.C.; Bebell, L.M.; Roshania, R.; Wolfman, V.; Mallow, M.; Kalyanpur, A.; Levine, A.C. Ebola Virus Disease and Pregnancy: A Retrospective Cohort Study of Patients Managed at 5 Ebola Treatment Units in West Africa. Clin. Infect. Dis. 2017, 65, 292–299.
- Pavlin, B.I.; Hall, A.; Hajek, J.; Raja, M.A.; Sharma, V.; Ramadan, O.P.; Mishra, S.; Rangel, A.; Kitching, A.; Roper, K.; et al. Atypical clinical presentation of Ebola virus disease in pregnancy: Implications for clinical and public health management. Int. J. Infect. Dis. 2020, 97, 167–173.
- Bower, H.; Brault, A.; Chege, E.; Saffa, G.; Seneca, D.; Salzer, J.S.; Grass, J.E.; Stroeher, U.; Belser, J.; Decroo, T.; et al. Delivery of an Ebola Virus-Positive Stillborn Infant in a Rural Community Health Center, Sierra Leone, 2015. Am. J. Trop. Med. Hyg. 2016, 94, 417–419.
- First Newborn Baby to Receive Experimental Therapies Survives Ebola Virus Disease | The Journal of Infectious Diseases | Oxford Academic. Available online: https://academic.oup.com/jid/article/215/2/171/2877903 (accessed on 26 May 2022).
- Resta, L.; Vimercati, A.; Cazzato, G.; Mazzia, G.; Cicinelli, E.; Colagrande, A.; Fanelli, M.; Scarcella, S.; Ceci, O.; Rossi, R. SARS-CoV-2 and Placenta: New Insights and Perspectives. Viruses 2021, 13, 723.
- Linehan, L.; O’Donoghue, K.; Dineen, S.; White, J.; Higgins, J.R.; Fitzgerald, B. SARS-CoV-2 placentitis: An uncommon complication of maternal COVID-19. Placenta 2021, 104, 261–266.
- Huynh, A.; Sehn, J.K.; Goldfarb, I.T.; Watkins, J.; Torous, V.; Heerema-McKenney, A.; Roberts, D.J. SARS-CoV-2 Placentitis and Intraparenchymal Thrombohematomas Among COVID-19 Infections in Pregnancy. JAMA Netw. Open 2022, 5, e225345.
- Shook, L.L.; Brigida, S.; Regan, J.; Flynn, J.P.; Mohammadi, A.; Etemad, B.; Siegel, M.R.; Clapp, M.A.; Li, J.Z.; Roberts, D.J.; et al. SARS-CoV-2 Placentitis Associated with B.1.617.2 (Delta) Variant and Fetal Distress or Demise. J. Infect. Dis. 2022, 225, 754–758.
- Lu-Culligan, A.; Chavan, A.R.; Vijayakumar, P.; Irshaid, L.; Courchaine, E.M.; Milano, K.M.; Tang, Z.; Pope, S.D.; Song, E.; Vogels, C.B.; et al. Maternal respiratory SARS-CoV-2 infection in pregnancy is associated with a robust inflammatory response at the maternal-fetal interface. Med 2021, 2, 591–610.e10.
- Bordt, E.A.; Shook, L.L.; Atyeo, C.; Pullen, K.M.; De Guzman, R.M.; Meinsohn, M.-C.; Chauvin, M.; Fischinger, S.; Yockey, L.J.; James, K.; et al. Maternal SARS-CoV-2 infection elicits sexually dimorphic placental immune responses. Sci. Transl. Med. 2021, 13.
- Bebell, L.M.; Oduyebo, T.; Riley, L.E. Ebola virus disease and pregnancy: A review of the current knowledge of Ebola virus pathogenesis, maternal, and neonatal outcomes. Birth Defects Res. 2017, 109, 353–362. Available online: https://onlinelibrary.wiley.com/doi/full/10.1002/bdra.23558 (accessed on 25 May 2022).
- Cribiù, F.M.; Erra, R.; Pugni, L.; Rubio-Perez, C.; Alonso, L.; Simonetti, S.; Croci, G.A.; Serna, G.; Ronchi, A.; Pietrasanta, C.; et al. Severe SARS-CoV-2 placenta infection can impact neonatal outcome in the absence of vertical transmission. J. Clin. Investig. 2021, 131, e145427.
- Olgun, N.S. Viral Infections in Pregnancy: A Focus on Ebola Virus. Curr. Pharm. Des. 2018, 24, 993–998.
- Kliman, H.J. From Trophoblast to Human Placenta; p. 23, 2006. Available online: https://medicine.yale.edu/obgyn/kliman/placenta/research/trophoblast%20to%20placenta%20eor_163163_284_18220_v1.pdf (accessed on 1 July 2022).
- Ouyang, Y.; Bagalkot, T.; Fitzgerald, W.; Sadovsky, E.; Chu, T.; Martínez-Marchal, A.; Brieño-Enríquez, M.; Su, E.J.; Margolis, L.; Sorkin, A.; et al. Term Human Placental Trophoblasts Express SARS-CoV-2 Entry Factors ACE2, TMPRSS2, and Furin. mSphere 2021, 6, e00250-21. Available online: https://journals.asm.org/doi/10.1128/mSphere.00250-21 (accessed on 26 May 2022).
- Vivanti, A.J.; Vauloup-Fellous, C.; Prevot, S.; Zupan, V.; Suffee, C.; Do Cao, J.; Benachi, A.; De Luca, D. Transplacental transmission of SARS-CoV-2 infection. Nat. Commun. 2020, 11, 3572.
- Dong, L.; Tian, J.; He, S.; Zhu, C.; Wang, J.; Liu, C.; Yang, J. Possible Vertical Transmission of SARS-CoV-2 From an Infected Mother to Her Newborn. JAMA 2020, 323, 1846–1848.
- Fenizia, C.; Biasin, M.; Cetin, I.; Vergani, P.; Mileto, D.; Spinillo, A.; Gismondo, M.R.; Perotti, F.; Callegari, C.; Mancon, A.; et al. Analysis of SARS-CoV-2 vertical transmission during pregnancy. Nat. Commun. 2020, 11, 5128.
- Atyeo, C.; Pullen, K.M.; Bordt, E.A.; Fischinger, S.; Burke, J.; Michell, A.; Slein, M.D.; Loos, C.; Shook, L.L.; Boatin, A.A.; et al. Compromised SARS-CoV-2-specific placental antibody transfer. Cell 2020, 184, 628–642.e10.
- Yuan, J.; Qian, H.; Cao, S.; Dong, B.; Yan, X.; Luo, S.; Zhou, M.; Zhou, S.; Ning, B.; Zhao, L. Is there possibility of vertical transmission of COVID-19: A systematic review. Transl. Pediatr. 2021, 10, 423–434.
- Tolu, L.B.; Ezeh, A.; Feyissa, G.T. Vertical transmission of Severe Acute Respiratory Syndrome Coronavirus 2: A scoping review. PLoS ONE 2021, 16, e0250196.
- Pace, R.M.; Williams, J.E.; Järvinen, K.M.; Belfort, M.B.; Pace, C.D.W.; Lackey, K.A.; Gogel, A.C.; Nguyen-Contant, P.; Kanagaiah, P.; Fitzgerald, T.; et al. COVID-19 and human milk: SARS-CoV-2, antibodies, and neutralizing capacity. medRxiv 2020.
- Krogstad, P.; Contreras, D.; Ng, H.; Tobin, N.; Chambers, C.D.; Bertrand, K.; Bode, L.; Aldrovandi, G.M. No infectious SARS-CoV-2 in breast milk from a cohort of 110 lactating women. Pediatr. Res. 2022, 1–6.
- Medina-Rivera, M.; Centeno-Tablante, E.; Finkelstein, J.L.; Rayco-Solon, P.; Peña-Rosas, J.P.; Garcia-Casal, M.N.; Rogers, L.; Ridwan, P.; Martinez, S.S.; Andrade, J.; et al. Presence of Ebola virus in breast milk and risk of mother-to-child transmission: Synthesis of evidence. Ann. N. Y. Acad. Sci. 2020, 1488, 33–43.
- Nordenstedt, H.; Bah, E.I.; De La Vega, M.-A.; Barry, M.; N’Faly, M.; Barry, M.; Crahay, B.; DeCroo, T.; Van Herp, M.; Ingelbeen, B. Ebola Virus in Breast Milk in an Ebola Virus–Positive Mother with Twin Babies, Guinea, 2015. Emerg. Infect. Dis. 2016, 22, 759–760.
- Rapid Outbreak Sequencing of Ebola Virus in Sierra Leone Identifies Transmission Chains Linked to Sporadic Cases | Virus Evolution | Oxford Academic. Available online: https://academic.oup.com/ve/article/2/1/vew016/1753554 (accessed on 26 May 2022).
- Keita, A.K.; Vidal, N.; Toure, A.; Diallo, M.S.K.; Magassouba, N.; Baize, S.; Mateo, M.; Raoul, H.; Mely, S.; Subtil, F.; et al. A 40 months follow-up of Ebola virus disease survivors in Guinea (Postebogui) reveals longterm detection of Ebola viral RNA in semen and breast milk. Open Forum Infect. Dis. 2019, 6, ofz482.
- Ebola Virus Localization in the Macaque Reproductive Tract during Acute Ebola Virus Disease—ScienceDirect. Available online: https://www.sciencedirect.com/science/article/pii/S0002944017309501?via%3Dihub (accessed on 26 May 2022).
- Liu, W.J.; Sesay, F.R.; Coursier, A.; Knust, B.; Marrinan, J.E.; Whitmer, S.; McDonald, S.L.R.; Gaillard, P.; Liu, Y.; Su, Q.; et al. Comprehensive Clinical and Laboratory Follow-up of a Female Patient with Ebola Virus Disease: Sierra Leone Ebola Virus Persistence Study. Open Forum Infect. Dis. 2019, 6, ofz068.
- Khoiwal, K.; Kalita, D.; Kumari, R.; Dhundi, D.; Shankar, R.; Kumari, R.; Gaurav, A.; Bahadur, A.; Panda, P.K.; Tomy, A.; et al. Presence of SARS-CoV -2 in the lower genital tract of women with active COVID-19 infection: A prospective study. Int. J. Gynecol. Obstet. 2022, 157, 744–747.
- Barber, E.; Kovo, M.; Leytes, S.; Sagiv, R.; Weiner, E.; Schwartz, O.; Mashavi, M.; Holtzman, K.; Bar, J.; Engel, A.; et al. Evaluation of SARS-CoV-2 in the Vaginal Secretions of Women with COVID-19: A Prospective Study. J. Clin. Med. 2021, 10, 2735.
- Qiu, L.; Liu, X.; Xiao, M.; Xie, J.; Cao, W.; Liu, Z.; Morse, A.; Xie, Y.; Li, T.; Zhu, L. SARS-CoV-2 Is Not Detectable in the Vaginal Fluid of Women with Severe COVID-19 Infection. Clin. Infect. Dis. 2020, 71, 813–817.
- Frontiers | Cesarean Section or Vaginal Delivery to Prevent Possible Vertical Transmission from a Pregnant Mother Confirmed With COVID-19 to a Neonate: A Systematic Review | Medicine. Available online: https://www.frontiersin.org/articles/10.3389/fmed.2021.634949/full (accessed on 26 May 2022).
- Lopian, M.; Kashani-Ligumsky, L.; Czeiger, S.; Cohen, R.; Schindler, Y.; Lubin, D.; Olteanu, I.; Neiger, R.; Lessing, J.B.; Somekh, E. Safety of vaginal delivery in women infected with COVID-19. Pediatr. Neonatol. 2020, 62, 90–96.
- Ferrazzi, E.; Frigerio, L.; Savasi, V.; Vergani, P.; Prefumo, F.; Barresi, S.; Bianchi, S.; Ciriello, E.; Facchinetti, F.; Gervasi, M.; et al. Vaginal Delivery in SARS-CoV-2-infected Pregnant Women in Northern Italy: A Retrospective Analysis. Obstet. Anesthesia Dig. 2021, 41, 82.
- Martínez-Perez, O.; Vouga, M.; Melguizo, S.C.; Acebal, L.F.; Panchaud, A.; Muñoz-Chápuli, M.; Baud, D. Association Between Mode of Delivery Among Pregnant Women with COVID-19 and Maternal and Neonatal Outcomes in Spain. JAMA 2020, 324, 296–299.
- Mor, G.; Cardenas, I. The Immune System in Pregnancy: A Unique Complexity. Am. J. Reprod. Immunol. 2010, 63, 425–433.
- Frontiers | Innate Immune Responses to Acute Viral Infection During Pregnancy | Immunology. Available online: https://www.frontiersin.org/articles/10.3389/fimmu.2020.572567/full (accessed on 26 May 2022).
- Frontiers | Immune Response to COVID-19 During Pregnancy | Immunology. Available online: https://www.frontiersin.org/articles/10.3389/fimmu.2021.675476/full (accessed on 26 May 2022).
- Seery, V.; Raiden, S.C.; Algieri, S.C.; Grisolía, N.A.; Filippo, D.; De Carli, N.; Di Lalla, S.; Cairoli, H.; Chiolo, M.J.; Meregalli, C.N.; et al. Blood neutrophils from children with COVID-19 exhibit both inflammatory and anti-inflammatory markers. eBioMedicine 2021, 67, 103357.
- Maternal-Fetal Immune Responses in Pregnant Women Infected with SARS-CoV-2 | Nature Communications. Available online: https://www.nature.com/articles/s41467-021-27745-z (accessed on 26 May 2022).
- Andrikopoulou, M.; Madden, N.; Wen, T.; Aubey, J.J.; Aziz, A.; Baptiste, C.D.; Breslin, N.; D’Alton, M.E.; Fuchs, K.M.; Goffman, D.; et al. Symptoms and Critical Illness Among Obstetric Patients with Coronavirus Disease 2019 (COVID-19) Infection. Obstet. Gynecol. 2020, 136, 291–299.
- Juttukonda, L.J.; Wachman, E.M.; Boateng, J.; Jain, M.; Benarroch, Y.; Taglauer, E.S. Decidual immune response following COVID-19 during pregnancy varies by timing of maternal SARS-CoV-2 infection. J. Reprod. Immunol. 2022, 151, 103501.
