Preeclampsia is an obstetric pathology that, surprisingly, resembles the pathology of COVID-19. Both diseases are characterized by significant alterations in the renin-angiotensin system (RAS). RAS-mediated mechanisms may explain their primary clinical-pathological features, which are suggestive of an underlying microvascular dysfunction, with induction of vasculopathy, coagulopathy, and inflammation.
- COVID-19
- SARS-CoV-2
- preeclampsia
1. Introduction
2. Pathogenesis of Preeclampsia and COVID-19
In both pathologies, wresearchers were able to identify two main phases. In PE, a placental dysfunction is followed by maternal syndrome (systemic vascular inflammation). First, placental ischemia occurs most commonly because of vascular damage due to anomalous placentation or intraplacental malperfusion. In the next step, the hypoxic placenta then liberates bioactive mediators including sFlt-1, reactive oxygen species, and inflammatory cytokines (e.g., TNF-α, IL-1, -6, and -8) into the maternal circulation, which has been determined to be responsible for the consequent endothelial damage and related clinical manifestations [11]. In COVID-19 infection, the virus triggers an interstitial pneumonia. This causes alveolar hypoxia, which can quickly evolve into a severe respiratory distress syndrome. Moreover, inflammatory cells and cytokines can enter the bloodstream and play a relevant role in ED and in a multiple organ dysfunction syndrome (“cytokine storm syndrome”) [12]. Endotheliitis, in turn, is an important precursor of a generalized hypercoagulable state that results in macro- and microvascular thrombosis in the pulmonary vascular system and beyond [13]. In conclusion, placental/alveolar hypoxia could lead to PE and severe COVID-19, respectively, through an angiogenic imbalance and subsequent exacerbated systemic inflammatory reaction due to RAS activation, as explained below in detail and in Figure 1.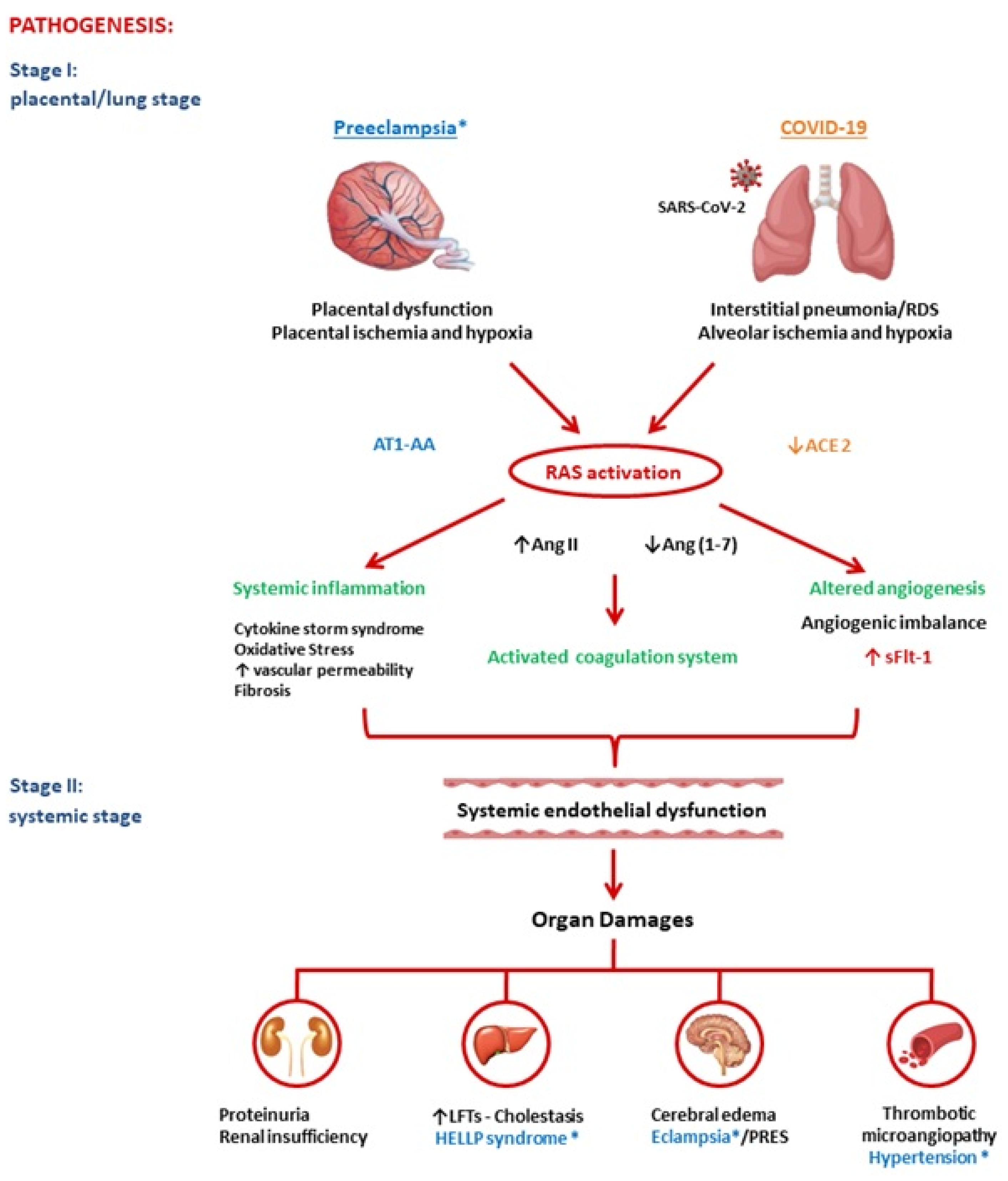
2.1. Renin-Angiotensin System
The RAS has been identified as playing a key role in the pathogenesis of both diseases. The classical RAS as it appeared in the mid-1970s is a hormone system that regulates blood pressure and fluid-electrolyte balance. When renal blood flow is reduced, an enzymatic cascade is activated: the juxtaglomerular cells in the kidneys transform the precursor prorenin into renin that converts angiotensinogen, released by the liver, into angiotensin I (Ang I). Ang I is subsequently turned into Ang II by the angiotensin-converting enzyme (ACE) located on the surface of, mostly, lung vascular endothelial cells. Ang II leads to an increase in blood pressure through the vasoconstriction and the secretion of the hormone aldosterone from the adrenal cortex. This increases the volume of extracellular fluid in the body. In the renal tubules, aldosterone provokes the reabsorption of sodium, and therefore of water into the blood, simultaneously causing the excretion of potassium, to maintain electrolyte balance. Since then, a broader view on RAS has gradually emerged [14][15]. Local tissue RAS systems have been recognized in most organs. Recently, evidence for an intracellular RAS has been reported. The new expanded view of RAS therefore covers endocrine, paracrine, and intracrine functions. Other RAS peptides have been shown to have biological actions, for example, the Ang (1–7) generated from angiotensin I (Ang I) or Ang II by ACE2 and other peptidases. This seems to play an important role in offsetting many of Ang II’s actions (Figure 2). Lung tissue has high RAS activity and is the main site of Ang II synthesis. The local RAS is also present in the placenta and is one of the major extrarenal RAS sites during pregnancy [16]. Various organ systems have a predilection for the involvement in COVID-19 and PE, and each of these organ systems can be a site of a tissue-based RAS, such as the brain, heart, and kidneys [15]. The RAS undergoes important changes in response to pregnancy and plays a crucial role in placentation. It is upregulated in normal pregnant women and downregulated in women with PE. Although Ang II levels are enhanced during pregnancy, normotensive pregnant women are refractory to its vasopressor effects. Trophoblasts are rich in angiotensin type 1 receptors (AT1Rs) and thus respond to changes in Ang II concentrations that occur during pregnancy. While plasma Ang I, Ang II, Ang (1–7), and plasma renin activity are all noted to decrease in the circulation of preeclamptic women and in the chorionic villi of preeclamptic placentas, Ang II peptide, angiotensinogen, and AT1R mRNA levels are observed to increase, showing an excessive pressor response to Ang II, which is also due to the presence of agonistic autoantibodies to the angiotensin type 1 receptor (AT1-AA). These antibodies have been reported to facilitate the interaction of Ang II with its receptor and may play a role in increasing vascular sensitivity to Ang II in preeclamptic women [17]. In COVID-19, ACE2 acts as a functional SARS-CoV-2 receptor, which leads to the downregulation of ACE2, which catalyzes and inactivates Ang II and produces Ang (1–7), a potent vasodilator. This serves as a negative regulator of the RAS. Recently, Liu et al. have also revealed that serum Ang II levels were directly proportional to the viral load and extent of lung damage in COVID-19 [18].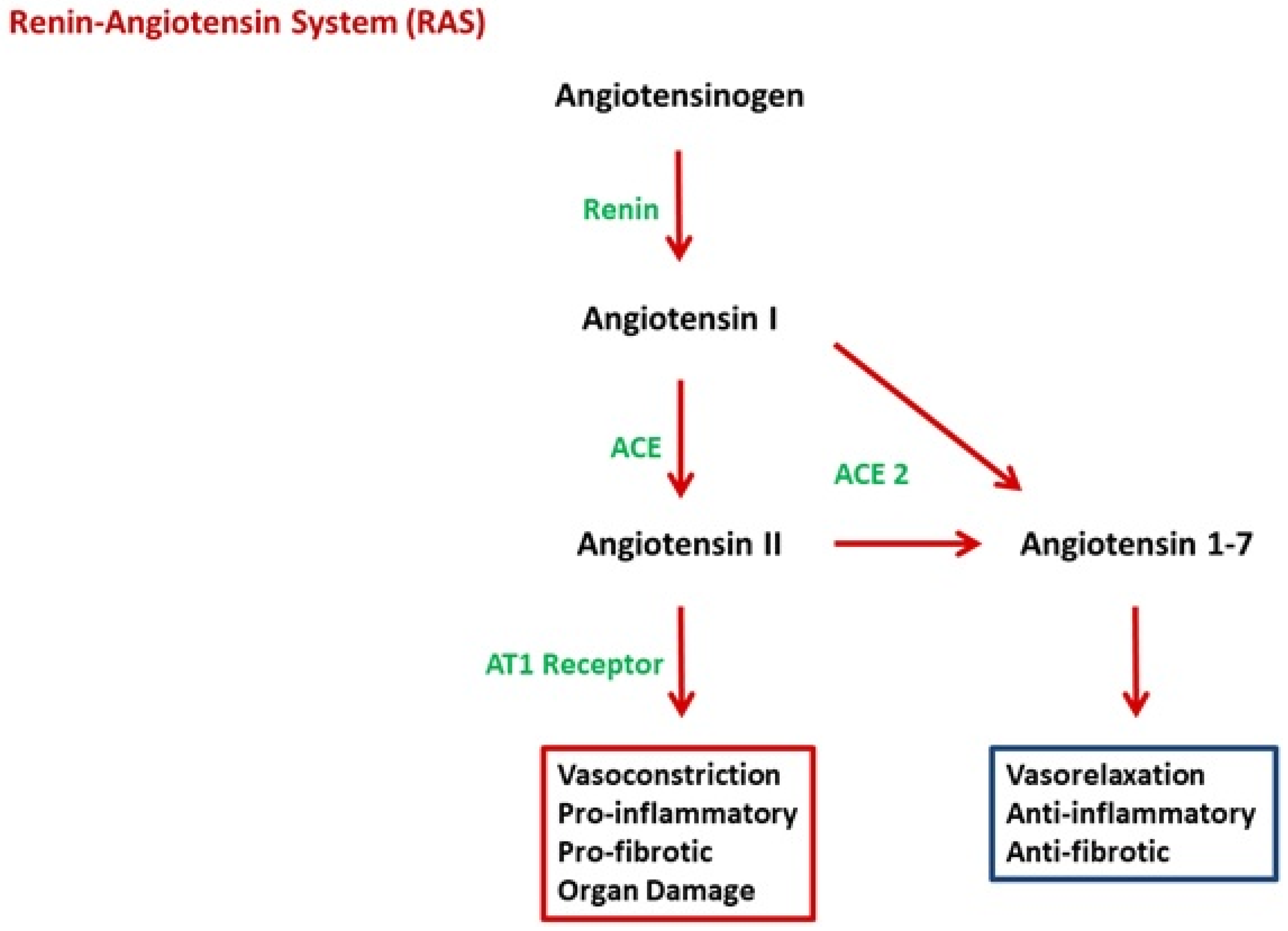
2.2. Angiotensin II
Ang II is a key vasoactive hormone. Recently, a large number of experimental studies have shown that it mediates several events of the inflammatory processes via binding to AT1Rs located in the heart, lungs, blood vessels, kidneys, adrenal glands, and placenta. It also plays an essential role in myocardial hypertrophy, fibrosis, inflammation, vascular remodeling, angiogenesis, atherosclerosis, and microvascular thrombosis and therefore ED [19]. Ang II-mediated mechanisms may explain the primary clinical-pathological features of COVID-19 and PE [20]. Indeed, both PE and COVID-19 could be due to an excess of Ang II or AT1 receptor activation. ACE2 knockout mice have showed more severe lung damage caused by increased hydrostatic pressure, reduced perfusion, and severe pulmonary edema [21]. Activation of coagulation and prothrombotic events is a well-known phenomenon in PE and COVID-19 [22][23]. Fibrosis is one of the most salient pathologic features of preeclamptic placentas [24]. Autopsy of the lungs after severe COVID-19 showed fibrin deposition [25]. The novel observation that Ang II modulates T-cell responses suggests a possible role for the peptide in autoimmune diseases. In COVID-19, as in PE, it has been shown that CD4 T lymphocytes are quickly activated to become pathogenic T helper-1 cells. This subsequently triggers a “cytokine storm” through increased expression of interleukin-6 (IL-6) and many other cytokines [26]. In the late 1990s, Wallukat et al. proposed that PE is a pregnancy-induced autoimmune disease in which abnormalities in placentation result from circulating autoantibodies, which, in turn, react to and activate the AT1R (AT1-AA). However, it has been hypothesized that AT1-AA may appear in a variety of pathological circumstances related to vascular damage; for example, parvovirus B19 also causes the generation of AT1-AA during pregnancy [17].2.3. Link between RAS and sFlt-1
The RAS is an important mediator of angiogenesis. Recent studies have demonstrated sFlt-1 is regulated by AT1 receptor signaling, along with multiple genes [27]. Ang II has also been shown to regulate angiogenesis [28].2.4. sFlt1 and Endothelial Dysfunction
sFlt-1 (sVEGFR-1) has been determined to be an anti-angiogenic factor expressed as an alternate junction variant of VEGFR-1 that lacks both the transmembrane and cytoplasmic domains. sFlt-1 antagonizes VEGF and PlGF (pro-angiogenic factors) in the circulation by binding and preventing interaction with their endothelial receptors, creating an anti-angiogenic state and ED [29], Figure 3. Clinical tests and experimental research have suggested that endothelial cell damage reduces the synthesis of vasorelaxant agents, increases the production of vasoconstrictors, impairs the synthesis of endogenous anticoagulants, and increases procoagulant production [30]. VEGF and PlGF are important in both angiogenesis and the maintenance of endothelial cell health at baseline [31].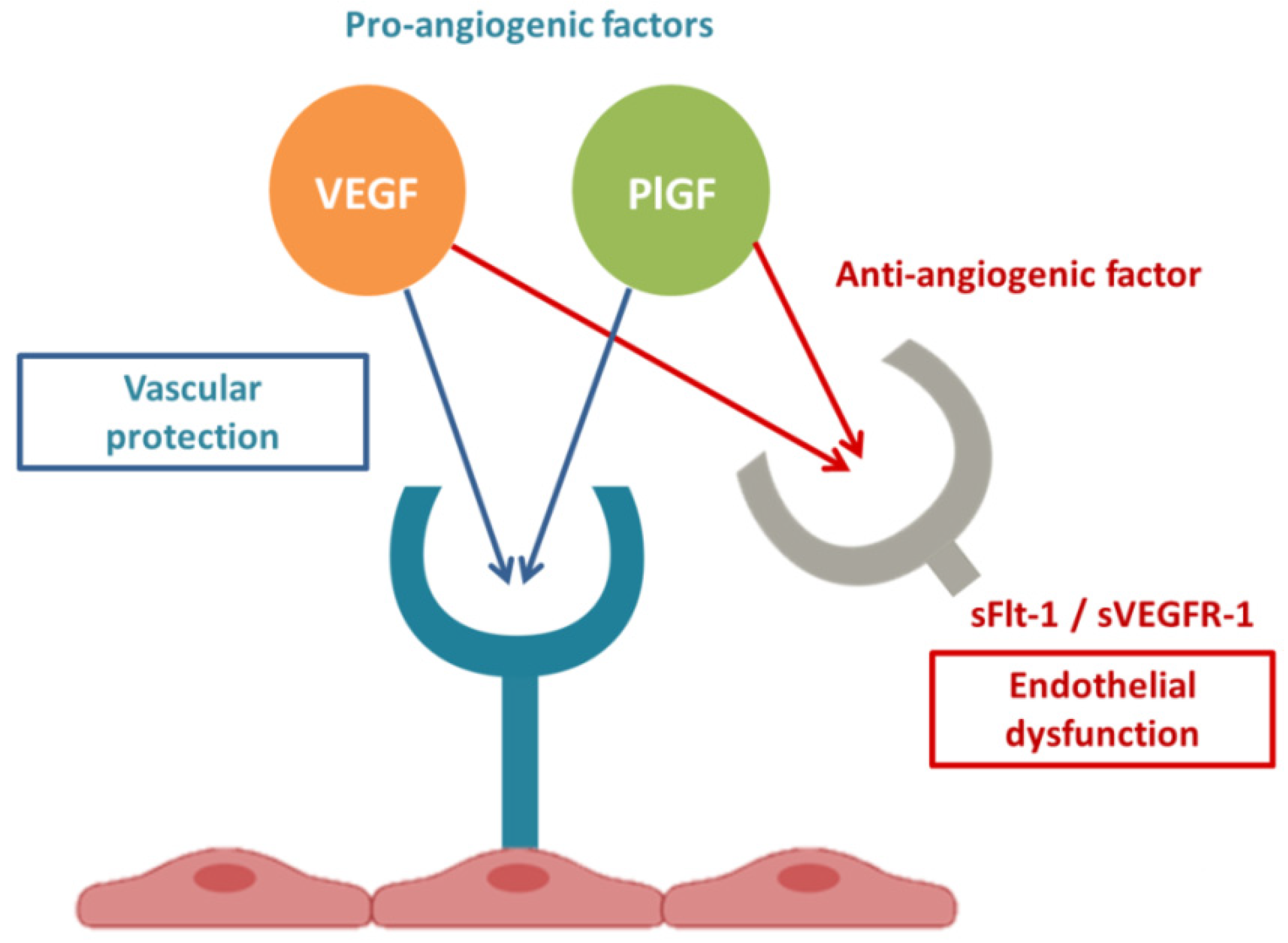
PE and COVID-19 have common pathogenic pathways. Both diseases are characterized by significant alterations in the RAS with an imbalanced proportion of anti-angiogenic and pro-angiogenic soluble plasmatic factors. In summary, both PE and COVID-19 appear to be due to a state of ED secondary to increased Ang II and ensuing excessive levels of circulating anti-angiogenic factors, such as sFlt1. COVID-19 and PE are defined to be diseases that begin, respectively, in the lungs and in the placenta, and both end in the endothelium. In conclusion, SARS-CoV-2 infection could be defined an angiogenic- pneumo-syndrome.
PE and COVID-19 have common pathogenic pathways. Both diseases are characterized by significant alterations in the RAS with an imbalanced proportion of anti-angiogenic and pro-angiogenic soluble plasmatic factors. In summary, both PE and COVID-19 appear to be due to a state of ED secondary to increased Ang II and ensuing excessive levels of circulating anti-angiogenic factors, such as sFlt1. COVID-19 and PE are defined to be diseases that begin, respectively, in the lungs and in the placenta, and both end in the endothelium. In conclusion, SARS-CoV-2 infection could be defined an angiogenic- pneumo-syndrome.
References
- Guo, Y.R.; Cao, Q.D.; Hong, Z.S.; Tan, Y.Y.; Chen, S.D.; Jin, H.J.; Tan, K.S.; Wang, D.Y.; Yan, Y. The origin, transmission and clinical therapies on coronavirus disease 2019 (COVID-19) outbreak—An update on the status. Mil. Med. Res. 2020, 7, 11.
- Cheng, H.; Wang, Y.; Wang, G.Q. Organ-protective effect of angiotensin-converting enzyme 2 and its effect on the prognosis of COVID-19. J. Med. Virol. 2020, 92, 726–730.
- Roberts, J.M.; August, P.A.; Bakris, G.; Barton, J.R.; Bernstein, I.M.; Druzin, M.; Gaiser, R.R.; Granger, J.P.; Jeyabalan, A.; Johnson, D.D.; et al. Hypertension in pregnancy. Report of the American College of Obstetricians and Gynecologists’ Task Force on Hypertension in Pregnancy. Obstet. Gynecol. 2013, 122, 1122–1131.
- Mayrink, J.; Costa, M.L.; Cecatti, J.G. Preeclampsia in 2018: Revisiting Concepts, Physiopathology, and Prediction. Sci. World J. 2018, 2018, 6268276.
- Mendoza, M.; Garcia-Ruiz, I.; Maiz, N.; Rodo, C.; Garcia-Manau, P.; Serrano, B.; Lopez-Martinez, R.M.; Balcells, J.; Fernandez-Hidalgo, N.; Carreras, E.; et al. Pre-eclampsia-like syndrome induced by severe COVID-19: A prospective observational study. BJOG 2020, 127, 1374–1380.
- Papageorghiou, A.T.; Deruelle, P.; Gunier, R.B.; Rauch, S.; García-May, P.K.; Mhatre, M.; Usman, M.A.; Abd-Elsalam, S.; Etuk, S.; Simmons, L.E.; et al. Preeclampsia and COVID-19: Results from the INTERCOVID prospective longitudinal study. Am. J. Obstet. Gynecol. 2021, 225, 289.e1–289.e17.
- Stepan, H.; Hund, M.; Andraczek, T. Combining Biomarkers to Predict Pregnancy Complications and Redefine Preeclampsia: The Angiogenic-Placental Syndrome. Hypertension 2020, 75, 918–926.
- Giardini, V.; Carrer, A.; Casati, M.; Contro, E.; Vergani, P.; Gambacorti-Passerini, C. Increased sFLT-1/PlGF ratio in COVID-19: A novel link to angiotensin II-mediated endothelial dysfunction. Am. J. Hematol. 2020, 95, E188–E191.
- Giardini, V.; Ornaghi SAcampora, E.; Vasarri, M.V.; Arienti, F.; Gambacorti-Passerini, C.; Casati, M.; Carrer, A.; Vergani, P. Letter to the Editor: SFlt-1 and PlGF Levels in Pregnancies Complicated by SARS-CoV-2 Infection. Viruses 2021, 13, 2377.
- Murphy, S.R.; Cockrell, K. Regulation of soluble fms-like tyrosine kinase-1 production in response to placental ischemia/hypoxia: Role of angiotensin II. Physiol. Rep. 2015, 3, e12310.
- Staff, A.C. The two-stage placental model of preeclampsia: An update. J. Reprod. Immunol. 2019, 134–135, 1–10.
- Lippi, G.; Sanchis-Gomar, F.; Henry, B.M. COVID-19: Unravelling the clinical progression of nature’s virtually perfect biological weapon. Ann. Transl. Med. 2020, 8, 693.
- Varga, Z.; Flammer, A.J.; Steiger, P.; Haberecker, M.; Andermatt, R.; Zinkernagel, A.S.; Mehra, M.R.; Schuepbach, R.A.; Ruschitzka, F.; Moch, H. Endothelial cell infection and endotheliitis in COVID-19. Lancet 2020, 395, 1417–1418.
- Patel, S.; Rauf, A.; Khan, H.; Abu-Izneid, T. Renin-angiotensin-aldosterone (RAAS): The ubiquitous system for homeostasis and pathologies. Biomed. Pharmacother. 2017, 94, 317–325.
- Santos, R.A.S.; Oudit, G.Y.; Verano-Braga, T.; Canta, G.; Steckelings, U.M.; Bader, M. The renin-angiotensin system: Going beyond the classical paradigms. Am. J. Physiol. Heart Circ. Physiol. 2019, 316, H958–H970.
- Verdonk, K.; Visser, W.; Van Den Meiracker, A.H.; Danser, A.H. The renin-angiotensin-aldosterone system in pre-eclampsia: The delicate balance between good and bad. Clin. Sci. 2014, 126, 537–544.
- Walther, T.; Stepan, H. Agonist autoantibodies against the angiotensin AT1 receptor in renal and hypertensive disorders. Curr. Hypertens. Rep. 2007, 9, 128–132.
- Liu, Y.; Yang, Y.; Zhang, C.; Huang, F.; Wang, F.; Yuan, J.; Wang, Z.; Li, J.; Li, J.; Feng, C.; et al. Clinical and biochemical indexes from 2019-nCoV infected patients linked to viral loads and lung injury. Sci. China Life Sci. 2020, 63, 364–374.
- Benigni, A.; Cassis, P.; Remuzzi, G. Angiotensin II revisited: New roles in inflammation, immunology and aging. EMBO Mol. Med. 2010, 2, 247–257.
- Miesbach, W. Pathological Role of Angiotensin II in Severe COVID-19. TH Open 2020, 4, e138–e144.
- Wang, L.; Li, Y.; Qin, H.; Xing, D.; Su, J.; Hu, Z. Crosstalk between ACE2 and PLGF regulates vascular permeability during acute lung injury. Am. J. Transl. Res. 2016, 8, 1246–1252.
- Egan, K.; Kevane, B.; Ní Áinle, F. Elevated venous thromboembolism risk in preeclampsia: Molecular mechanisms and clinical impact. Biochem. Soc. Trans. 2015, 43, 696–701.
- Bikdeli, B.; Madhavan, M.V.; Jimenez, D.; Chuich, T.; Dreyfus, I.; Driggin, E.; Nigoghossian, C.; Ageno, W.; Madjid, M.; Guo, Y.; et al. Global COVID-19 Thrombosis Collaborative Group, Endorsed by the ISTH, NATF, ESVM, and the IUA, Supported by the ESC Working Group on Pulmonary Circulation and Right Ventricular Function. COVID-19 and Thrombotic or Thromboembolic Disease: Implications for Prevention, Antithrombotic Therapy, and Follow-Up: JACC State-of-the-Art Review. J. Am. Coll. Cardiol. 2020, 75, 2950–2973.
- Ohmaru-Nakanishi, T.; Asanoma, K.; Fujikawa, M.; Fujita, Y.; Yagi, H.; Onoyama, I.; Hidaka, N.; Sonoda, K.; Kato, K. Fibrosis in Preeclamptic Placentas Is Associated with Stromal Fibroblasts Activated by the Transforming Growth Factor-β1 Signaling Pathway. Am. J. Pathol. 2018, 188, 683–695.
- Carsana, L.; Sonzogni, A.; Nasr, A.; Rossi, R.S.; Pellegrinelli, A.; Zerbi, P.; Rech, R.; Colombo, R.; Antinori, S.; Corbellino, M.; et al. Pulmonary post-mortem findings in a series of COVID-19 cases from northern Italy: A two-centre descriptive study. Lancet Infect. Dis. 2020, 20, 1135–1140.
- Mehta, P.; McAuley, D.F.; Brown, M.; Sanchez, E.; Tattersall, R.S.; Manson, J.J.; HLH Across Speciality Collaboration, UK. COVID-19: Consider cytokine storm syndromes and immunosuppression. Lancet 2020, 395, 1033–1034.
- Irani, R.A.; Xia, Y. The functional role of the renin-angiotensin system in pregnancy and preeclampsia. Placenta 2008, 29, 763–771.
- Anton, L.; Merrill, D.C.; Neves, L.A.; Gruver, C.; Moorefield, C.; Brosnihan, K.B. Angiotensin II and angiotensin-(1-7) decrease sFlt1 release in normal but not preeclamptic chorionic villi: An in vitro study. Reprod. Biol. Endocrinol. 2010, 8, 135.
- Maynard, S.E.; Min, J.Y.; Merchan, J.; Lim, K.H.; Li, J.; Mondal, S.; Libermann, T.A.; Morgan, J.P.; Sellke, F.W.; Stillman, I.E.; et al. Excess placental soluble fms-like tyrosine kinase 1 (sFlt1) may contribute to endothelial dysfunction, hypertension, and proteinuria in preeclampsia. J. Clin. Investig. 2003, 111, 649–658.
- Roberts, J.M. Objective evidence of endothelial dysfunction in preeclampsia. Am. J. Kidney Dis. 1999, 33, 992–997.
- He, Y.; Smith, S.K.; Day, K.A.; Clark, D.E.; Licence, D.R.; Charnock-Jones, D.S. Alternative splicing of vascular endothelial growth factor (VEGF)-R1 (FLT-1) pre-mRNA is important for the regulation of VEGF activity. Mol. Endocrinol. 1999, 13, 537–545.
- Shanes, E.D.; Mithal, L.B.; Otero, S.; Azad, H.A.; Miller, E.S.; Goldstein, J.A. Placental Pathology in COVID-19. Am. J. Clin. Pathol.
- Zeisler, H.; Llurba, E.; Chantraine, F.; Vatish, M.; Staff, A.C.; Sennström, M.; Olovsson, M.; Brennecke, S.P.; Stepan, H.; Allegranza, D.; et al. Predictive Value of the sFlt-1:PlGF Ratio in Women with Suspected Preeclampsia. N. Engl. J. Med. 2016, 374, 13–22.
- Negro, A.; Fama, A.; Penna, D.; Belloni, L.; Zerbini, A.; Giuri, P.G. SFLT-1 levels in COVID-19 patients: Association with outcome
- Dupont, V.; Kanagaratnam, L.; Goury, A.; Poitevin, G.; Bard, M.; Julien, G.; Bonnivard, M.; Champenois, V.; Noel, V.; Mourvillier,
- Shapiro, N.I.; Schuetz, P.; Yano, K.; Sorasaki, M.; Parikh, S.M.; Jones, A.E.; Trzeciak, S.; Ngo, L.; Aird, W.C. The association of
- Dumnicka, P.; Sporek, M.; Mazur-Laskowska, M.; Ceranowicz, P.; Kuz ́niewski, M.; Droz ̇dz ̇, R.; Ambroz ̇y, T.; Olszanecki, R.; Kus ́nierz-Cabala, B. Serum Soluble Fms-Like Tyrosine Kinase 1 (sFlt-1) Predicts the Severity of Acute Pancreatitis. Int. J. Mol. Sci.
- Maynard, S.E.; Karumanchi, S.A. Angiogenic factors and preeclampsia. Semin. Nephrol. 2011, 31, 33–46.
- van Veen, T.R.; Panerai, R.B.; Haeri, S.; Griffioen, A.C.; Zeeman, G.G.; Belfort, M.A. Cerebral autoregulation in normal pregnancy
- van Veen, T.R.; Panerai, R.B.; Haeri, S.; Griffioen, A.C.; Zeeman, G.G.; Belfort, M.A. Cerebral autoregulation in normal pregnancy and preeclampsia. Obstet. Gynecol. 2013, 122, 1064–1069.
