Your browser does not fully support modern features. Please upgrade for a smoother experience.
Please note this is a comparison between Version 1 by Claudia Von Arx and Version 3 by Dean Liu.
Male breast cancer (MBC) is a rare disease. Genetic factors predispose to male breast cancer. Germline and/or genetic and/or epigenetic alterations at the somatic level identify a subset of male breast cancer that could differ from female breast cancer (FBC).
- male breast cancer
- BRCA1/2
1. Introduction
MBC is a rare disease [1]. Current evidence about treatment is derived from small single institutional experiences. The knowledge of genetic drivers of MBC could drive prospective clinical trials of more specific and targeted therapies.
2. Management
2.1. Imaging
MBC patients usually presents with signs of locally advanced tumor (nipple and/or skin involvement); this is due to the smaller breast size in men, and probably the later manifestation of breast symptoms. MBC is commonly located in the subareolar region while in FBC, it is commonly in the upper-outer quadrant. Malignant calcifications are less frequent in men than in women, and their mammographic features (i.e., scattered and punctuate) would be considered benign in women. Cystic lesions are rare, which is different from what occurs in women, and they should be considered as suspicious of malignancy. Lobular tissue is not commonly present in male breasts and for this reason cysts are uncommon. For instance, in men papillary carcinomas are generally detected as cysts with a complex pattern at US-imaging. MBC can be erroneously diagnosed for asymmetric/unilateral gynecomastia; however, the first is often eccentric to the nipple while the latter is central and concentric to the nipple [2][41].2.2. Histopathology
The most frequent histology of MBCs is invasive ductal carcinoma, which occurs in 85–95% of patients. Ductal carcinoma in situ is diagnosed in 5–10% of male with BC [1]. Regarding immunohistochemistry phenotypes, MBC seems to be more likely to express hormone receptors than FBC. In small retrospective studies, 82% of the included MBCs were positive for estrogen receptors (ER)s and 75% showed positivity for progestin receptors (PRs) [1]. A recent large retrospective analysis of 489 male patients confirmed these findings [3][42]. ERs were evaluable in 419 tumors, with 92% of tumors being positive; PR status was assessable in 399 tumors and was positive in 89.2% of cases. The concurrent evaluation of both hormone receptors shows ER+/PR+ = 86%; ER+/PR− = 6%; ER−/PR+ = 3.3%; and ER−/PR− = 4.8%. More than 95% of the tumors showed positivity in at least one hormone receptor. However, tumor subtypes seem to be distributed differently from that seen for women and varies according to race/ethnicity. In fact, as reported by Mc Gregor and colleagues, among 606 patients with different ethnic origins triple-negative or ER-positive/PR-negative tumors are more frequent in non-Hispanic black men for which is also reported a poorer outcome [4][43]. In the EORTC International Male Breast Cancer Program, 1483 MBCs were retrospectively analyzed over 20 years. For tumors without metastases, ductal invasive carcinomas were reported in 84.8% of cases, with grade 2 in 51.5%; ER-positivity in 99.3%; PR positivity in 81.9%; AR positivity in 96.9% and low expression of Ki67 in 61.1%. The most common subtypes in MBC were the luminal A-like (41.9%) and luminal B-like/HER-2-negative (48.6%), whereas less frequent were the HER-2-positive (8.7%) and triple-negative (0.3%) subtypes [5][39]. Men aged less than 50 years old had poorer outcomes. In tumors with high ER positivity, with high PR positivity, and high AR positivity, significantly longer overall survival (OS) and recurrent-free survival (RFS) was reported. While HER2 expression, Ki67, IHC subtypes or grade were no associated to OS/RFS [6][44]. Gargiulo et al. also reported a high prevalence of positive hormonal receptor status (88.4% ER+; 81.4% PR+) in MBC, with HER2-positive and triple-negative tumor prevalence being 26.8% and 7.0%, respectively [7][5]. HER2 expression has been reported to range between 2% and 27% in MBC. Humphries et al. showed a very low expression of HER2 in MBC, accounting for <10%. In the series by Gargiulo et al., a higher expression was reported, probably attributable to the non-systematic evaluation [1][7][8][1,5,45]. Other biomarkers were recently evaluated in 134 MBCs. Cyclin D1 and bcl-2 are frequently expressed (75% and 77%, respectively) in MBCs. BRST2 and p21 are expressed in 56% and 48% of MBCs, respectively; p53 is expressed only in 15% of these tumors and basal phenotype is uncommon [6][44]. Furthermore, it has been demonstrated that there is an association between high grade, high mitotic count and HER2 amplification and/or overexpression, high Ki67, p53 accumulation, high p21 expression, low PR expression, and low bcl-2 expression. A decreased 5-years survival were statistically associated to PR negativity and p53 accumulation; they were also independent markers of patient prognosis [9][46]. Histopathological features seem to be related to the tumor mutational status. An Italian multicenter study evaluating 382 male patients with BCs, including 50 BRCA carriers, reported that MBCs in BRCA2 carriers showed a statistically higher tumor grade, PR negativity, and HER2 positivity. Carriers of BRCA2 pathogenetic variants develop more frequently secondary primary tumors (OR = 11.42, 95% CI 1.79–73.08). BRCA2-related MBCs have a specific phenotype characterized by high-grade tumors, PR-negative status and consequently a more aggressive behavior [10][47]. MBC is often diagnosed at an advanced stage. T4 disease represented 20–25% of cancers [11][48]. The pT3–T4 stage significantly increases according to age, with the highest percentage (42%) in men over 70 years old [11][48]. Axillary nodal involvement is present in approximately 50% of MBC [3][11][12][42,48,49] and significantly correlates with the pathological tumor size [3][42].2.3. Treatments
Treatment options, schedules, and duration of therapies in MBC for both localized and metastatic disease are usually derived from recommendations and guidelines for FBC. Treatment includes the integration of surgery, radiotherapy, and systemic therapies. Modified radical mastectomy is the preferred surgical approach for MBCs, used in approximately 70% of patients. Less favored approaches are represented by radical mastectomy, especially in older patients, total mastectomy, and lumpectomy with or without radiation [11][48]. Sarmiento et al. reported, in a large population-based cohort, an evaluation on 16,498 MBCs from the National Cancer Database and showed an improved survival related to treatments, particularly surgery. Increasing age, black race, government insurance, more comorbidities, and higher tumor stages were associated with decreased survival [12][49]. More recently, Yadav et al. confirmed the association between a worse prognosis and advanced age, black ethnicity, comorbidities, high grade and stages, and poor access to health care [13][50]. They reported a negative association with mastectomy, differently from the study of Sarmiento. Yadav et al. found that more male patients underwent total mastectomy compared to breast-conserving treatment, which is the preferred option for surgical treatment in females. They showed an association between radical mastectomy and poor clinical outcomes, possibly due to a selection bias because of higher stage associated to larger tumors size and/or node involvement in this cohort. Further evaluation is needed [14][51]. Moreover, in MBC, like in FBC, sentinel lymph node (SLN) biopsy is a reliable tool for the identification of nodal metastases, as shown by two different experiences in a European and USA Center [15][16][52,53]. No strong evidence exists on the use of radiation after mastectomy. Current recommendations suggest adhering to the guidelines for FBC, as shown by a recent single institutional experience [1][17][1,54]. Hormonal therapy (HT) represents the gold standard treatment for hormone receptor-positive MBC. Adjuvant HT is represented by tamoxifen for 5 years. Tamoxifen is associated to a decreased risk of recurrence, accounting by 51%, comparable with FBC treatment [18][55]. In male, about 80% of the circulating estrogen is produced by the aromatase pathway and 20% by the testes [19][56]. However, the role of adjuvant aromatase inhibitors (AIs) has been little studied in male patients [20][57]. Eggermann et al., compared adjuvant tamoxifen vs AIs [21][58].They reported a statistically significant worse outcome in AI cohort for both mortality risk and overall survival [21][58]. In high-risk patients because of young age, high tumor grade and/or axillary nodal involvement, adjuvant chemotherapy is generally recommended. Currently, anthracycline-based schedules are preferred while in elderly patients, use of the CMF scheme has been described. However, adjuvant chemotherapy conferred a not statistically significant lower time to recurrence and improvement in overall survival [18][55]. No data exist about the adjuvant use of trastuzumab in MBC, and only one case report speculates about its efficacy in metastatic disease [22][59]. Considering that there is no biological reason for trastuzumab showing different activity in MBC than FBC patients, this treatment, and pertuzumab, might be considered for HER-2-positive MBC. Tamoxifen remains the gold standard treatment for male patients. The 5-year OS is similar for tamoxifen-treated FBC and MBC patients (85.1% and 89.2% respectively; p = 0.972) [23][60]. Luteinizing hormone-releasing hormone (LHRH) agonists and orchiectomy are other available therapies. AI associated or not to LHRH agonist was evaluated in a retrospective series, reporting a response rate of 26.1% and a disease control rate of 56.5% [24][25][61,62]. In comparison with AI-treated FBC, MBC had a significantly poor outcome (5-year OS was 85.0% in FBC vs. 73.3% in MBC; p = 0.028) [23][60]. HT is indeed associated with a multitude of side effects in men. The most common adverse event related to tamoxifen is hot flashes. Decreased libido, weight gain, and malaise have been described. Less common are rash and erectile dysfunction. Alteration of hepatic function, lung embolism, thrombophlebitis, myalgia, depression, visual deficit, and diarrhea are uncommon [26][63]. Reported toxicities of AI use include decreased libido, leg swelling, and depression for anastrozole while edema and hot flashes have been reported after use of letrozole [27][64]. In metastatic MBC, chemotherapy has been offered as second- or third-line therapy after relapse of HT in ER-negative patients. Few and small studies highlight the role of chemotherapy in this setting of patients; the poor efficacy might be related to the old schedules used in those studies [28][65]. IMore recently, in the phase III OlympiAD trial germline BRCA1/2 metastatic BC patients were randomized to olaparib, a PARP inhibitor, versus a standard chemotherapy (capecitabine or eribulin, or vinorelbine). The study demonstrated a statistically significant advantage in median progression-free survival (mPFS) in patients treated with olaparib (mPFS = 7.0 months) vs patient treated with chemotherapy (mPFS = 4.2 months). Of note, in this study, about 2% of the enrolled population, respectively 5 out 205 patient in the olaparib group and 2 out of 97 in the contol group were male [29][66].3. Cancer Genetic Counseling
In the clinical setting, professionals involved in the diagnosis and treatment of MBC patients should refer them to cancer genetic counseling services. Cancer genetic counseling should foresee risk assessment, adequate genetic testing, and an appropriate oncological preventive program for MBC patients and their at-risk healthy family members according to the specific genetic predisposition [30][31][67,68].3.1. Risk Assessment
Genetic testing should be offered at diagnosis of breast cancer in a male patient, independently of a positive oncological family history [32][69]. However, the assessment of the ‘a priori’ probability of identifying a pathogenetic variant is an important component of pre-test counseling. Different probabilistic tools are available for risk assessment. Among these, one of the most widely validated is BRCAPRO [33][34][70,71]. Several studies have validated this model relative to FBC [35][36][72,73], but few data exist about MBC. In a recent Italian trial, Different prediction models were evaluated for their performance in 102 MBC patients with mutations in BRCA1/2 genes, diagnosed between 1991 and 2007. Thirty-nine out 102 patients (38%) of the patients reported a breast and ovarian cancer diagnosis in first- and/or second-degree relatives. Family history (FH) seems to be a better predictor of pathogenetic variants. Thus, pathogenetic variant carriers account for 15.4% (6/39) of MBC patients with a positive FH and 6.4% (4/63) of those without. Comparing different risk estimation models, only the BRCAPRO version 5.0 showed the best performance with a good sensitivity, specificity, and negative and positive predictive value [37][74]. More recently, BRCAPRO version 6.0 has been specifically validated as a counseling tool, showing a high performance in determining the ‘a priori’ risk of having a pathogenic variant of MBCs with or without positive FH [38][75]. The BOADICEA (Breast and Ovarian Analysis of Disease Incidence and Carrier Estimation Algorithm) program is an upcoming tool in European countries [39][76]. Since 2008, it has been updated and extended, considering the risks of MBC [40][77]. Previously, two studies compared BOADICEA, BRCAPRO, and other risk estimation models relative to MBC. However, they considered both FBC and MBC, the number of MBC cases evaluated was scarce, and inconsistent results were shown [41][42][43][78,79,80]. More recently, a comparison of BOADICEA, BRCAPRO, and the Myriad probabilistic models was performed in 307 male patients with BC and tested for BRCA1/2. Fifty-eight of these patients were BRCA1/2 carriers. BOADICEA was effective in predicting the total number of BRCA1/2 carriers, and there were non-significant differences in carriers-prediction performance between the BRCAPRO and the BOADICEA. Conversely, Myriad underestimated the number of carriers in almost 70% of the cases and therefore has not been considered a good carriers-predictive model for MBC patients [44][81].3.2. Genetic Testing
Genetic testing should be offered within pre- and post-test counseling sessions according to the implications of the genetic test itself and the results [30][45][46][67,82,83]. Genetic testing for BRCA1/2 and PALB2 should be the first choice for mutational analysis. BRCA2 and PALB2 own similar clinical phenotype, i.e., a higher risk of solid tumors in children carriers of homozygotes pathogenetic variants. In addition, there is also an increase risk of developping BC in women. BRCA1/2 and PALB2 pathogenetic carriers in heterozygosis have also higher relative risk for pancreatic cancer [47][48][49][84,85,86]. BRCA2 and PALB2 share an analogue function and cancer predisposing spectrum; therefore, PALB2 genetic testing should be proposed to MBC patients belonging to families with BRCA1/2-negative or no informative genetic test results and to families in which a typical tumor of the BRCA2 spectrum are diagnosed. Other genes, i.e., TP53 and PTEN, should be considered if the family history is suggestive of minor syndromes, such as Li–Fraumeni and Cowden, respectively [32][69]. Moreover, mutational analysis of moderate-/low-penetrance genes should be considered if the genetic test is negative or not informative of pathogenetic variants in BRCA1/2. MBC patients should be counseled for the potential hereditary risk for relatives. Carriers of BRCA2 pathogenetic variants should be advised on the risk of Fanconi anemia and/or brain tumors in minor children if BRCA2 variants has been revealed in both maternal and paternal lines [50][51][52][87,88,89]. The most common pathogenetic variant situation would be in Iceland or in Ashkenazi Jews and no reports of Fanconi in double hits in Iceland or of c.5946delT have been described.Figure 1
summarizes the genetic testing process for MBC.
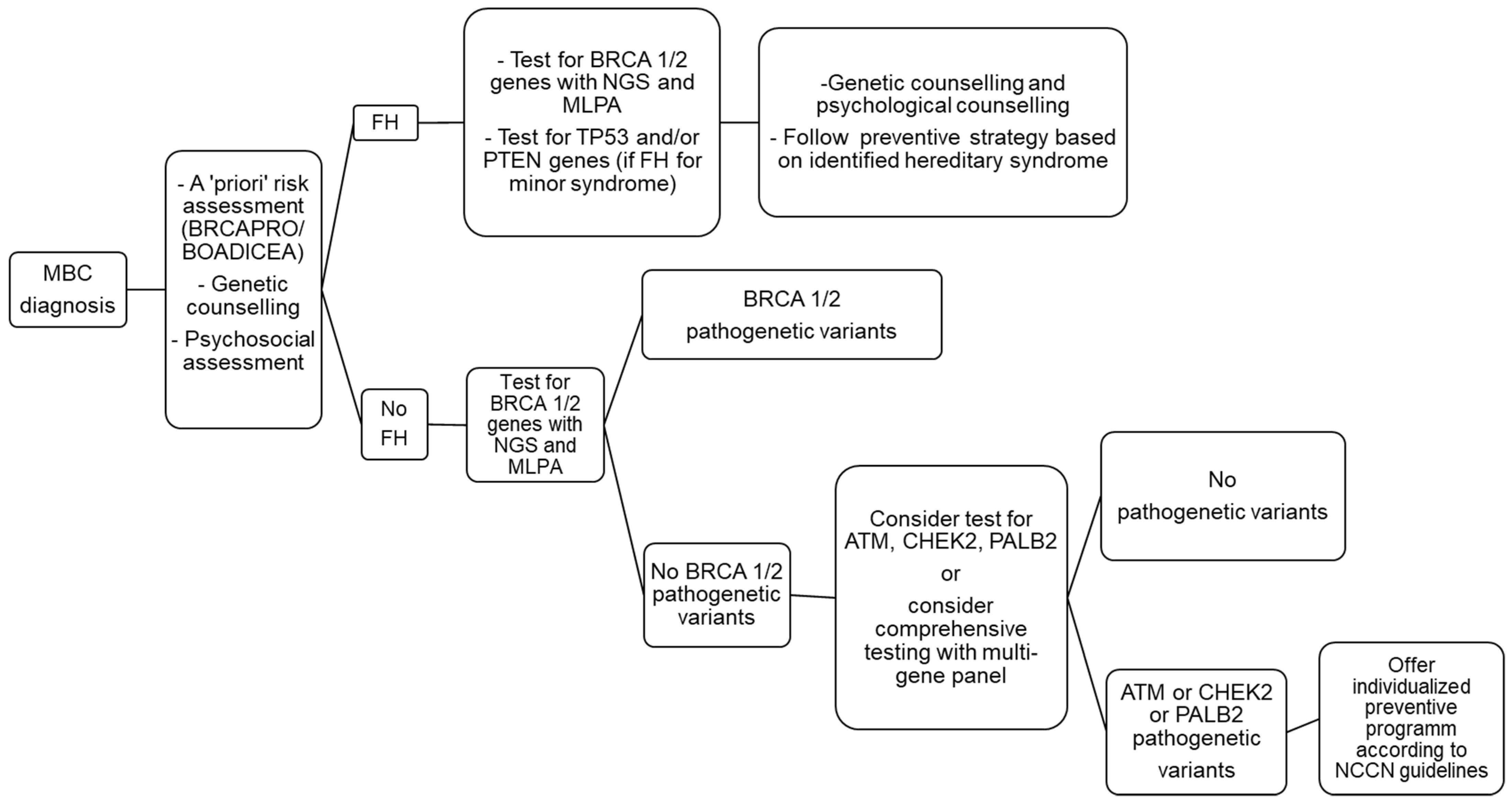
Figure 1. Genetic testing flow chart after a diagnosis of breast cancer (BC) in a male patient.
